Submitted:
30 April 2026
Posted:
01 May 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Study sites
Study design and sample size
Data and measurements
Data handling and analysis
Ethical considerations
Results
3.1. Main findings
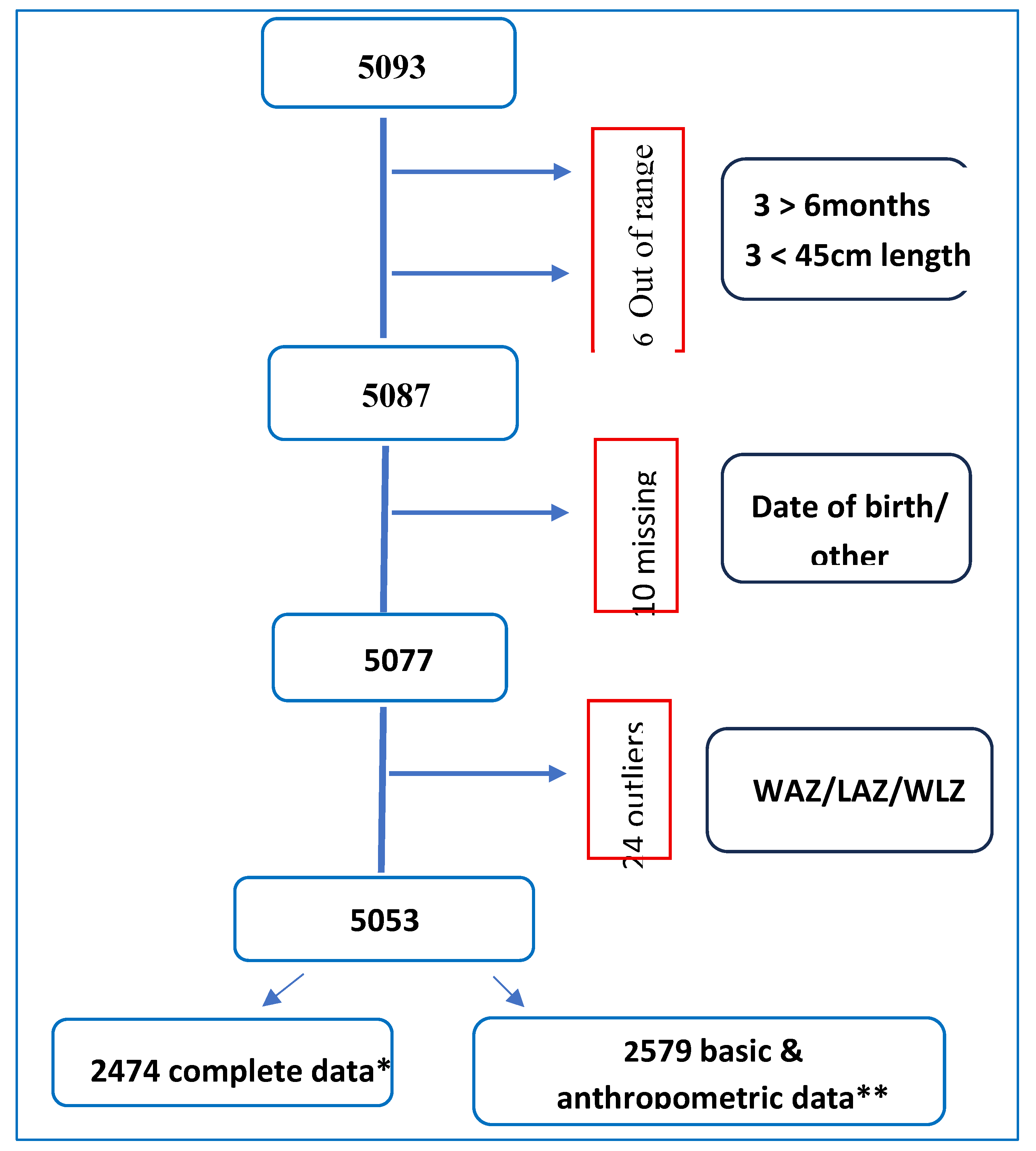
3.1.1. Flow of participants
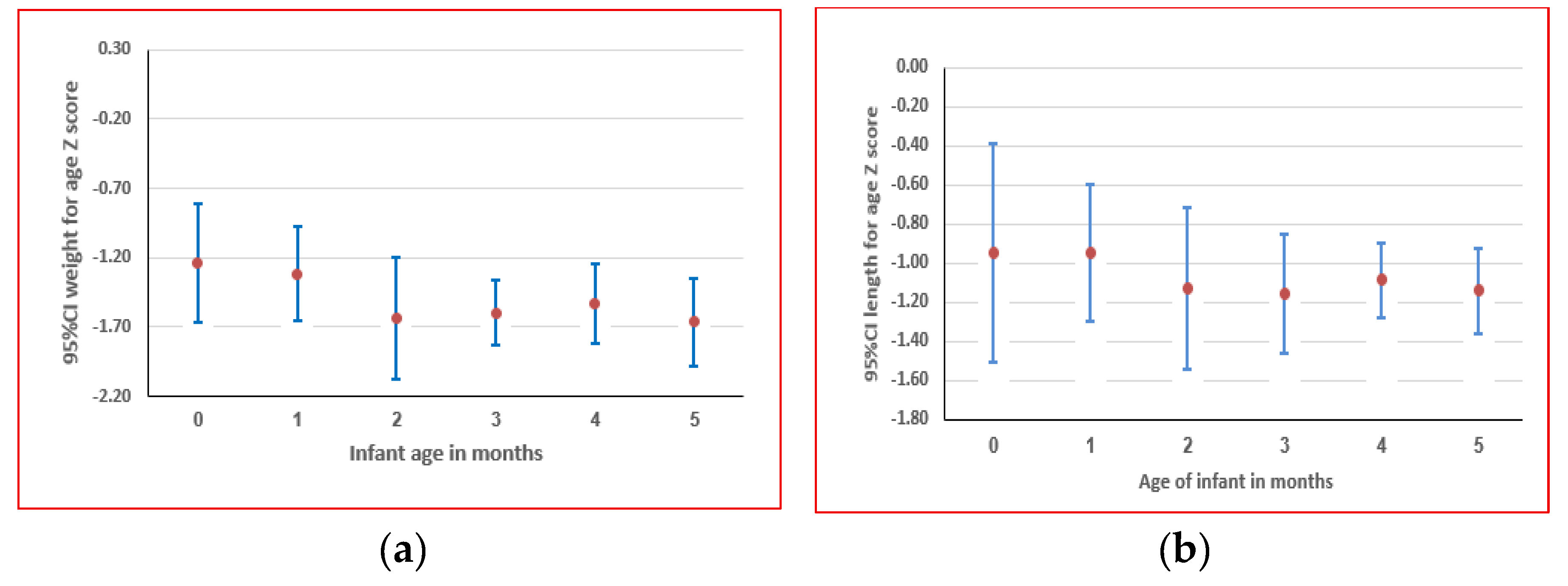
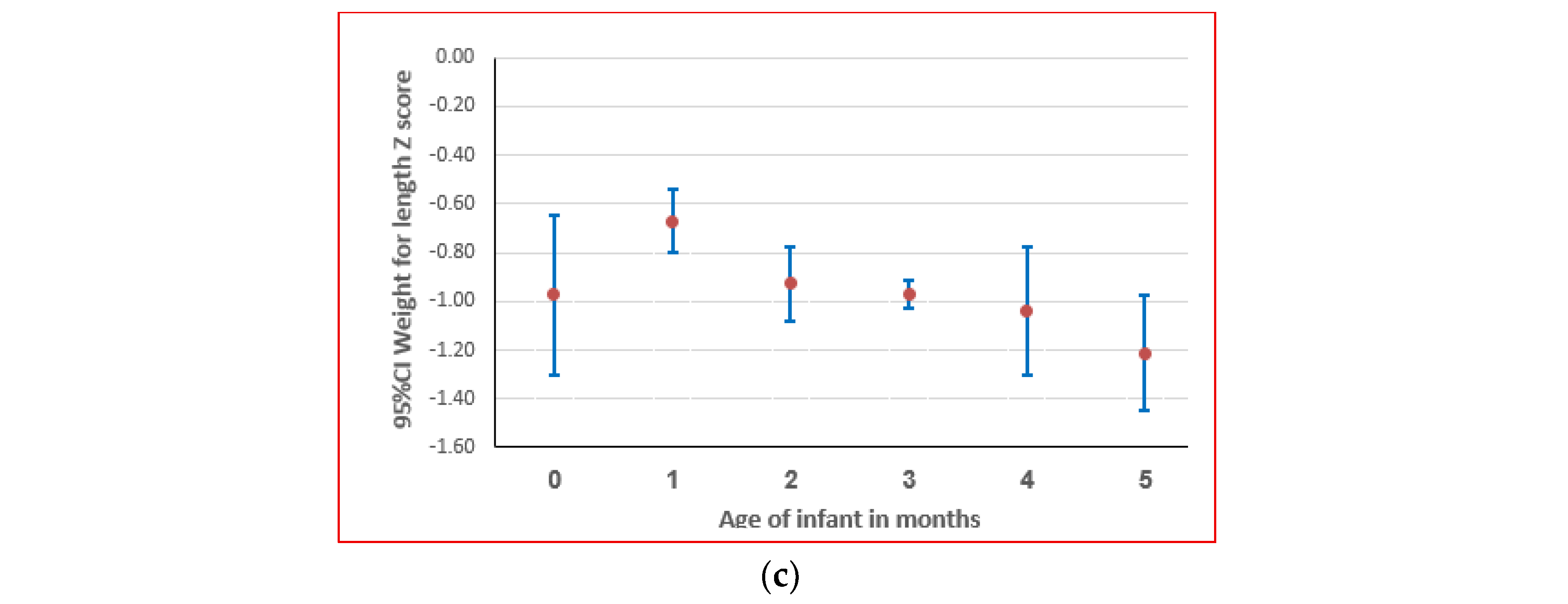
3.1.2. Sample demographic and anthropometric characteristics
3.1.3. Prevalence of different anthropometric deficits including composite indices by age
3.1.4. Prevalence of single and concurrent forms of anthropometric deficit
3.1.5. Prevalence of low MUAC
3.1.6. Which indicator best detects different anthropometric deficits?
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| < 3m | Less than 3 months |
| ≥ 3m | Three months and above |
| < 6m | Under six months |
| CIAF | Composite index of anthropometric failure |
| CISAF | Composite index of severe anthropometric failure |
| HC | Health center |
| HF | Health facility |
| Lahj HL | Lahj low land |
| Lahj LL | Lahj low land |
| LAZ | Length for age z score |
| MUAC | Mid upper arm circumference |
| SAM | Severe acute malnutrition |
| SD | Standard deviation |
| SES | Socio-economic status |
| UNICEF | United nations children fund |
| WHO | World Health Organization |
| WAZ | Weight for length z score |
| WLZ | Weight for age z score |
References
- Benjamin-Chung, J.; Mertens, A.; Colford, J.M.; Hubbard, A.E.; van der Laan, M.J.; Coyle, J.; Sofrygin, O.; Cai, W.; Nguyen, A.; Pokpongkiat, N.N. et al. Early-childhood linear growth faltering in low- and middle-income countries. Nature 2023, 621, 550–557. [CrossRef]
- Victora, C.G.; Bahl, R.; Barros, A.J.D.; França, G.V.A.; Horton, S.; Krasevec, J.; Murch, S.; Sankar, M.J.; Walker, N.; Rollins, N.C. Breastfeeding in the 21st century: epidemiology, mechanisms, and lifelong effect. Lancet 2016, 387(10017),475–490. [CrossRef]
- Patwari, A.K.; Kumar, S.; Beard, J. Undernutrition among infants less than 6 months of age: an underestimated public health problem in India. Matern. Child Nutr 2015, 11(1), 119–126. [CrossRef]
- Kerac, M.; Blencowe, H.; Grijalva-Eternod, C.; McGrath, M.; Shoham, J.; Cole, T.J.; Seal, A. Prevalence of wasting among under 6-month-old infants in developing countries and implications of new case definitions using WHO growth standards: a secondary data analysis. Arch. Dis. Child 2011, 96(11), 1008–1013. [CrossRef]
- Cashin, K.; Oot, L. Guide to Anthropometry: A Practical Tool for Program Planners, Managers, and Implementers, 1st ed.; FANTA/FHI 360: Washington, DC, USA, 2018; pp. 193–195.
- Nandy, S.; Irving, M.; Gordon, D.; Subramanian, S.V.; Smith, G.D. Poverty, child undernutrition and morbidity: new evidence from India. Bull. World Health Organ. 2005, 83, 210–216. Available from: https://iris.who.int/handle/10665/269373.
- Svedberg, P. How many people are malnourished? Annu. Rev. Nutr. 2011, 31, 263–283.
- McDonald, C.M.; Olofin, I.; Flaxman, S.; Fawzi, W.W.; Spiegelman, D.; Caulfield, L.E.; Black, R.E.; Ezzati, M.; Danaei, G. The effect of multiple anthropometric deficits on child mortality: Meta-analysis of individual data in 10 prospective studies from developing countries. Am. J. Clin. Nutr. 2013, 97, 896–901. [CrossRef]
- Mwangome, M.; Ngari, M.; Bwahere, P.; Kabore, P.; McGrath, M.; Kerac, M.; Berkley, J.A. Anthropometry at birth and at age of routine vaccination to predict mortality in the first year of life: A birth cohort study in Burkina Faso. PLoS One 2019, 14, e0213523. [CrossRef]
- Jyothi, S.D.; Bendre, S.L.; Desai, A.S. Mid-upper arm circumference cut-off for detection of severe acute malnutrition in infants aged between one and six months. Pediatr Rev Int J Pediatr Res 2020, 7, 430–436. Available online: https://pediatrics.medresearch.in/index.php/ijpr/article/view/643.
- Mwangome, M.; Ngari, M.; Fegan, G.; Mturi, N.; Shebe, M.; Bauni, E.; Berkley, J.A. Diagnostic criteria for severe acute malnutrition among infants aged under 6 mo. Am J Clin Nutr 2017, 105, 1415–1423. [CrossRef]
- Mwangome, M.K.; Fegan, G.; Mbunya, R.; Prentice, A.M.; Berkley, J.A. Reliability and accuracy of anthropometry performed by community health workers among infants under 6 months in rural Kenya. Trop. Med. Int. Health 2012, 17, 622–629. [CrossRef]
- Mwangome, M.K.; Fegan, G.; Fulford, T.; Prentice, A.M.; Berkley, J.A. Mid-upper arm circumference at age of routine infant vaccination to identify infants at elevated risk of death: a retrospective cohort study in the Gambia. Bull. World Health Organ. 2012, 90, 887–894. http://doi: 10.2471/BLT.12.109009.
- Mathenge, A.; Mwangome, M.; Fegan, G.; Mwaniki, M.; Shebe, M.; Newton, C.R.J.C.; Maitland, K.; Berkley, J.A. Assessment of severe malnutrition among hospitalised Kenyan infants under 6 months old – abstracts of the 10th CAPGAN Conference. Malawi Med. J. 2009, 21, 123–159.
- Bountogo, M.; Sié, A.; Zakane, A.; Compaoré, G.; Ouédraogo, T.; Lebas, E.; O’Brien, K.S.; Lietman, T.M.; Oldenburg, C.E. Neonatal anthropometric indicators of infant growth and mortality in Burkina Faso. Public Health Nutr. 2024, 27(1), e123. [CrossRef]
- World Health Organization. WHO Guideline on the Prevention and Management of Wasting and Nutritional Oedema (Acute Malnutrition) in Infants and Children under 5 Years; World Health Organization: Geneva, Switzerland, 2023. Available online: https://www.who.int/publications/i/item/9789240082830.
- Jima, B.R.; Hassen, H.Y.; Getnet, Y.; Bahwere, P.; Gebreyesus, S.H. Diagnostic performance of midupper arm circumference for detecting severe wasting among infants aged 1–6 months in Ethiopia. Am. J. Clin. Nutr. 2021, 113, 55–62. [CrossRef]
- Hoehn, C.; Lelijveld, N.; Mwangome, M.; Berkley, J.A.; McGrath, M.; Kerac, M. Anthropometric criteria for identifying infants under 6 months of age at risk of morbidity and mortality: a systematic review. Clin Med Insights Pediatr 2021,15:11795565211049904. [CrossRef]
- Yemen: Overview. Available online: https://www.worldbank.org/en/country/yemen/ove rview (accessed on 4 July 2025).
- Balkhy, HH. Mitigating the increasing threat of cholera in Yemen and other conflict-affected countries in the Eastern Mediterranean Region. East Mediterr Health J. 2025;31(7):423-425. [CrossRef]
- World Health Organization. Yemen health crisis at a glance; WHO Regional Office for the Eastern Mediterranean: Cairo, Egypt [no date]. Available online: https://www.emro.who.int/images/stories/yemen/yemen-health-crisis-overviewpdf.pdf(accessed on 4 July 2025).
- Internal Displacement Monitoring Centre (IDMC); Norwegian Refugee Council (NRC). 2025 Global Report on Internal Displacement (GRID); Internal Displacement Monitoring Centre: Geneva, Switzerland, 2025; Available online: https://www.internal-displacement.org/global-report/grid2025/.
- UNHCR Data Portal: Yemen. Available online: https://data.unhcr.org/en/country/yem (accessed on 4 July 2025).
- Talukdar, R.; Ravel, V.; Barman, D.; Kumar, V.; Dutta, S.; Kanungo, S. Prevalence of undernutrition among migrant, refugee, internally displaced children and children of migrated parents in lower-middle-income countries: a meta-analysis of published studies from last twelve years. Diabetes Metab. Syndr. 2024, 18(3), 102976. [CrossRef]
- Integrated Food Security Phase Classification (IPC). Yemen: Acute Food Insecurity (July 2024 - February 2025). IPC Global Platform; 2024. Available online: https://www.ipcinfo.org/fileadmin/user_upload/ipcinfo/docs/IPC_Yemen_Acute_Food_Insecurity_Jul2024_Feb2025_Report_English.pdf (accessed on 18 July 2025).
- Central Statistical Organization (CSO); United Nations Children’s Fund (UNICEF). Yemen Multiple Indicator Cluster Survey 2022-2023, Survey Findings Report; Central Statistical Organization and United Nations Children’s Fund: Yemen, 2023. Available online: https://mics.unicef.org/news/just-released-mics-yemen-survey-findings-report-and-snapshots (accessed on 4 July 2025).
- Fahmy, S.; Nofal, L.; Shehata, S.; El Kady, H.; Ibrahim, H. Updating indicators for scaling the socioeconomic level of families for health research. J. Egypt. Public Health Assoc. 2015, 90 (1), 1-7. [CrossRef]
- de Onis, M.; Onyango, A.W.; Van den Broeck, J.; Chumlea, W.C.; Martorell, R. Measurement and standardization protocols for anthropometry used in the construction of a new international growth reference. Food Nutr Bull. 2004; 25(1 Suppl):S27-S36. [CrossRef]
- World Health Organization. WHO Anthro for personal computers, version 3.2.2: Software for assessing growth and development of the world’s children; World Health Organization: Geneva, Switzerland, 2011. Available online: https://www.who.int/tools/child-growth-standards/software.
- Grijalva-Eternod, C.S.; Beaumont, E.; Rana, R.; Abate, N.; Barthorp, H.; McGrath, M.; Negesse, A.; Abera, M.; Abdissa, A.; Girma, T. et. al. Malnutrition in infants aged under 6 months attending community health centres: A cross-sectional survey. Nutrients 2021, 13(8), 2489. [CrossRef]
- Wright, C.M.; Macpherson, J.; Bland, R.; Ashorn, P.; Zaman, S.; Ho, F.K. Wasting and stunting in infants and young children as risk factors for subsequent stunting or mortality: Longitudinal analysis of data from Malawi, South Africa, and Pakistan. J. Nutr 2021, 151(7), 2022–2028. [CrossRef]
- Mertens, A.; Benjamin-Chung, J.; Colford, J.M.; Hubbard, A.E.; van der Laan, M.J.; Coyle, J.; Sofrygin, O.; Cai, W.; Jilek, W.; Rosete, S. et.al Child Growth Consortium. Child wasting and concurrent stunting in low- and middle-income countries. Nature 2023, 621(7979), 558–567. [CrossRef]
- World Health Organization. Yemen: Nutritional Surveillance; WHO Regional office for the Eastern Mediterranean: Cairo, Egypt, March 2025. Available online: https://www.emro.who.int/images/stories/yemen/Nutrition-Surveillance-March-2025.pdf (accessed on 4 July 2025).
- Mwangome, M.; Ngari, M.; Brals, D.; Bawhere, P.; Kabore, P.; McGrath, M.; Berkley, J.A. Stunting in the first year of life: Pathway analysis of a birth cohort. PLOS Glob. Public Health 2024, 4 (2), e0002908. [CrossRef]
- Ouattara, M.; Sié, A.; Bountogo, M.; Boudo, V.; Dah, C.; Lebas, E.; Hu, H.; Porco, T.C.; Arnold, B.F.; Lietman, T.M.; et al. Anthropometric differences in community- versus clinic-recruited infants participating in a trial of azithromycin for prevention of childhood mortality in Burkina Faso. Am. J. Trop. Med. Hyg. 2023, 109(5), 1187-1191. [CrossRef]
- Kerac, M.; Frison, S.; Connell, N.; Page, B.; McGrath, M. Informing the management of acute malnutrition in infants aged under 6 months (MAMI): risk factor analysis using nationally-representative demographic & health survey secondary data. PeerJ 2019, 6, e5848. [CrossRef]
- Khan, J.R.; Bakar, K.S.; Awan, N.; Muurlink, O.; Homaira, N. Accuracy of Mothers’ Perception of Birth Size to Predict Birth Weight Data in Bangladesh. Matern. Child Health J. 2024, 28(10), 1677-1684. [CrossRef]
- Banajeh, S.M.; Al-Sunbali, N.N.; Al-Sanahani, S.H. Clinical characteristics and outcome of children aged under 5 years hospitalized with severe pneumonia in Yemen. Ann. Trop. Paediatr. 1997, 17(4), 321–326. [CrossRef]
- Ezeofor, I.O.; Garcia, A.L.; Wright, C.M. Criteria for undernutrition screening in hospitalised infants under 6 months: a diagnostic accuracy study in a resource-poor setting. Arch. Dis. Child. 2020, 105, 524–529. [CrossRef]
- Mahmud, I.; Guesdon, B.; Kerac, M.; Grijalva-Eternod, C.S. Mortality risk in infants receiving therapeutic care for malnutrition: A secondary analysis. Matern. Child Nutr. 2024, 20 (3), e13635. [CrossRef]
- WHO Risk Stratification Working Group (WHO-RSWG). Infant-level and child-level predictors of mortality in low-resource settings: the WHO Child Mortality Risk Stratification Multi-Country Pooled Cohort. Lancet Glob. Health 2025, 13(5): e843-e858. [CrossRef]
- Hossain, S.; Mihrshahi, S. Effect of exclusive breastfeeding and other infant and young child feeding practices on childhood morbidity outcomes: Associations for infants 0–6 months in 5 South Asian countries using Demographic and Health Survey data. Int. Breastfeed. J. 2024, 19, 35. [CrossRef]
- Gomes, F.; Adu-Afarwuah, S.; Agustina, R.; Ali, H.; Arcot, A.; Arifeen, S.; Arnold, C.D.; Black, R.E.; Christian, P.; Dewey, K.G. et. al. Effect of prenatal multiple micronutrient supplementation compared with iron and folic acid supplementation on size at birth and subsequent growth through 24 mo of age: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2025, 122, 185–195. [CrossRef]
- Chowdhury, R.; Nitika; Choudhary, T.S.; Taneja, S.; Martines, J.; Bhandari, N.; Bahl, R. Diagnostic measures for severe acute malnutrition in Indian infants under 6 months of age: A secondary data analysis. BMC Pediatr. 2021, 21(1), 158. [CrossRef]
- Haidar, A.R.; Alselwi, A.G. Epidemiological study of determinants of low birth weight in Yemen: Systematic review. In Proceedings of Science Georgia International Conference on global practice of multidisciplinary scientific studies, Tbilisi, Georgia, 26-31 October 2025. Available from: https://www.researchgate.net/publication/398417518.
| Infant anthropometry (n= 5053) | Mean ± S.D | <-2 Z % (95% CI) | <-3 Z (95% CI) | |
|---|---|---|---|---|
| Weight (kg) | 4.8 ± 1.10 | |||
| Length (cm) | 57.23 ± 4.32 | |||
| WLZ score | -.91 ± 1.22 | 19.3 (15.1;24.3) | 4.2 (2.9;6.1) | |
| LAZ score | -1.07 ± 1.10 | 17.7 (13.8;22.5) | 3.9 (2.7;5.6) | |
| WAZ score | -1.50 ± 1.11 | 30.5 (21.8;40.7) | 9.1 (7.8;10.5) | |
| MUAC (cm) (n=5041) | 12.37 ± 1.13 | |||
| Anthropometric indicator n=5,053 | 0m (n=491) (95% CI) | 1m (n=1345) (95% CI) | 2m (n=1180) (95% CI) | 3m (n=896) (95% CI) | 4m (n=678) (95% CI) | 5m (n=463) (95% CI) |
|---|---|---|---|---|---|---|
| Wasted | 20% (12.9;29.5) |
13.1% (10.7;16.0) | 17.2% (11.5;24.9) | 20.4% (14.1;28.6) | 26% (19.9;33.0) | 29.8% (24.8;35.3) |
|
Severely wasted |
2.4% (1.5;4.0) |
2% (1.1;3.7) |
3.1% (1.7;5.5) |
5.5% (3.6;8.2) |
5.5% (2.7;10.7) |
11.4% (9.2;14.1) |
| Stunted | 21% (7.2;47.6) |
17.9% (11.7;26.4) | 18.9% (14.1;24.8) | 16.2% (11.3;22.7) | 15.3% (6.5;32.1) | 17.3% (7.0;36.6) |
|
Severely stunted |
6.3% (2.5;15.3) |
3.3% (2.3;4.6) |
3.1% (1.8;5.4) |
4.6% (2.3;8.8) |
4% (1.6;9.7) |
3.2% (0.7;13.9) |
| Underweight | 20.2% (9.0;39.1) |
26.3% (15.2;41.6) | 36.9% (22.5;54.0) | 30.8% (24.8;37.5) | 30.5% (24.1;37.8) | 36.3% (28.0;45.5) |
|
Severely underweight |
7.9% (2.3;24.1) |
6.7% (3.6;12.1) |
9.7% (7.6;12.3) |
9.3% (6.7;12.6) |
9.6% (5.3;16.7) |
14.5% (8.2;24.4) |
| All | ||||||
|
CIAF 40.9% (34.7;47.5) |
37.7% (24.0;53.6) | 37.4% (27.5;48.5) | 45.1% (34.9;55.7) | 40.6% (35.9;45.5) | 40.9% (28.5;54.4) | 44.7% (32.8;57.2) |
| CISAF 12% (10.8;13.4) | 11.6% (5.0;24.8) |
9.1% (5.9;13.8) |
12.1% (9.8;14.9) |
13.3% (9.8;17.8) |
12.7% (6.3;23.9) | 17.5% (10.1;28.7) |
| Anthropometric indicator | All n=5053 % (95% CI) |
< 3m n=3016 % (95% CI) |
≥ 3m n=2037 % (95% CI) |
p-value |
|---|---|---|---|---|
| Wasted only | 5.5 (2.2;13.1) | 6.0 (2.4;14.4) | 4.6 (1.8;11.3) | .267 |
| Wasted and underweight | 10.6 (5.4;19.6) | 7.0 (3.6;13.0) | 15.9 (9.2;25.8) | .011 |
| Wasted, underweight and stunted | 3.2 (2.3;4.5) | 2.8 (1.6;4.7) | 3.9 (2.1;7.1) | .346 |
| Stunted only | 5 (4.6;5.5) | 5 (3.9;6.3) | 5.1 (3.6;7.1) | .938 |
| Stunted and underweight | 9.5 (5.7;15.5) | 11.0 (6.4;18.3) | 7.2 (2.7;17.5) | .307 |
| Underweight only | 7.2 (3.3;14.9) | 8.6 (3.9;17.8) | 5 (2.1;11.5) | .045 |
| All n=5041 % (95% CI) |
0m n=489 % (95% CI) |
1m n=1344 % (95% CI) |
2m,n=1174 % (95% CI) |
3m n=895 % (95% CI) |
4m n=676 % (95% CI) |
5m n= 463 % (95% CI) |
|||
|---|---|---|---|---|---|---|---|---|---|
| MUAC <10.5 cm |
6 (2.4;14.3) |
33.1 (18.1;52.6) |
5.1 (2.4;10.5) |
2.1 (0.7;6.1) |
2.5 (1.0;5.8) |
1.3 (0.7;2.7) |
3.9 (1.9;7.8) |
||
| MUAC <11.0 cm |
10.9 (4.3;25.0) |
47.9 (27.6;68.8) |
12 (6.1;22.3) |
5.4 (1.7; 15.8) |
3.9 (1.7;8.9) |
2.5 (1.3;5.0) |
8.4 (5.5;12.6) |
||
| MUAC <11.5 cm |
18.6 (7.1;40.7) |
64.4 (38.6;83.9) |
23.4 (11.4;42.3) |
11.6 (3.7;30.9) |
7.8 (3.2;17.9) |
6.8 (2.9;15.1) |
11.9 (8.1;17.2) |
||
| n=5041 | Wasted n=972 |
Stunted n=893 |
Underweight n=1534 | CIAF n=2062 |
CISAF n=607 |
No CIAF n=2979 |
|---|---|---|---|---|---|---|
| MUAC <10.5 cm |
13.5 (7.6;22.7) |
12.7 (4.6;30.5) |
11 (4.1;26.6) |
10.3 (4.2;23.1) |
20.4 (10.1;36.9) |
3.1 (.8;10.9) |
| MUAC <11.0 cm |
22.3 (13.2;35.3) |
20.3 (7.0;46.3) |
19.1 (6.6;44.1) |
17.8 (7.0;38.4) |
33.1 (16.2;55.9) |
6.1 (1.8.;18.8) |
| MUAC <11.5 cm |
36.1 (20.2;55.8) |
29.9 (10.2;61.6) |
29.7 (10.1;61.3) |
28.8 (10.9;57.1) |
47 (26.0;69.1) |
11.5 (3.4;32.3) |
| WAZ <-2 | 71.6 (39.8;90.6) | 71.8 (63.6;78.8) | 100 (100:100) |
74.4 (58.2;85.8) | 92.1 (83.1;96.5) | 0 (0;0) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




