Submitted:
27 April 2026
Posted:
28 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
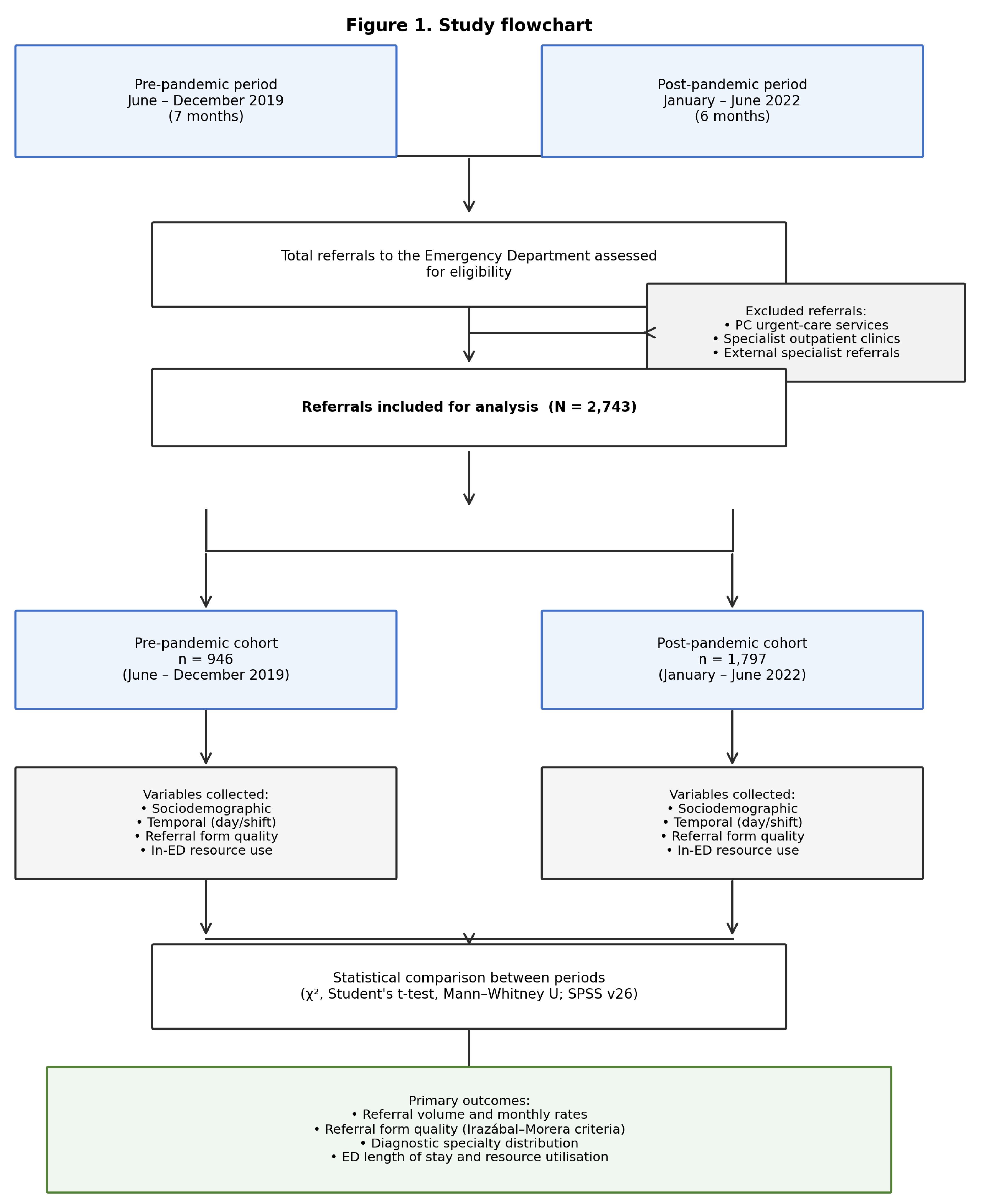
2.2. Study Periods and Population
- Pre-pandemic period: 1 June - 31 December 2019 (7 months), preceding the onset of the COVID-19 pandemic in Spain.
- Post-pandemic period: 1 January - 30 June 2022 (6 months), after the main pandemic waves had subsided but while the healthcare system was still operating under the influence of pandemic-related structural changes.
2.3. Variables
2.4. Data Collection and Ethics
2.5. Statistical Analysis
3. Results
3.1. Referral Volume and Sociodemographic Characteristics
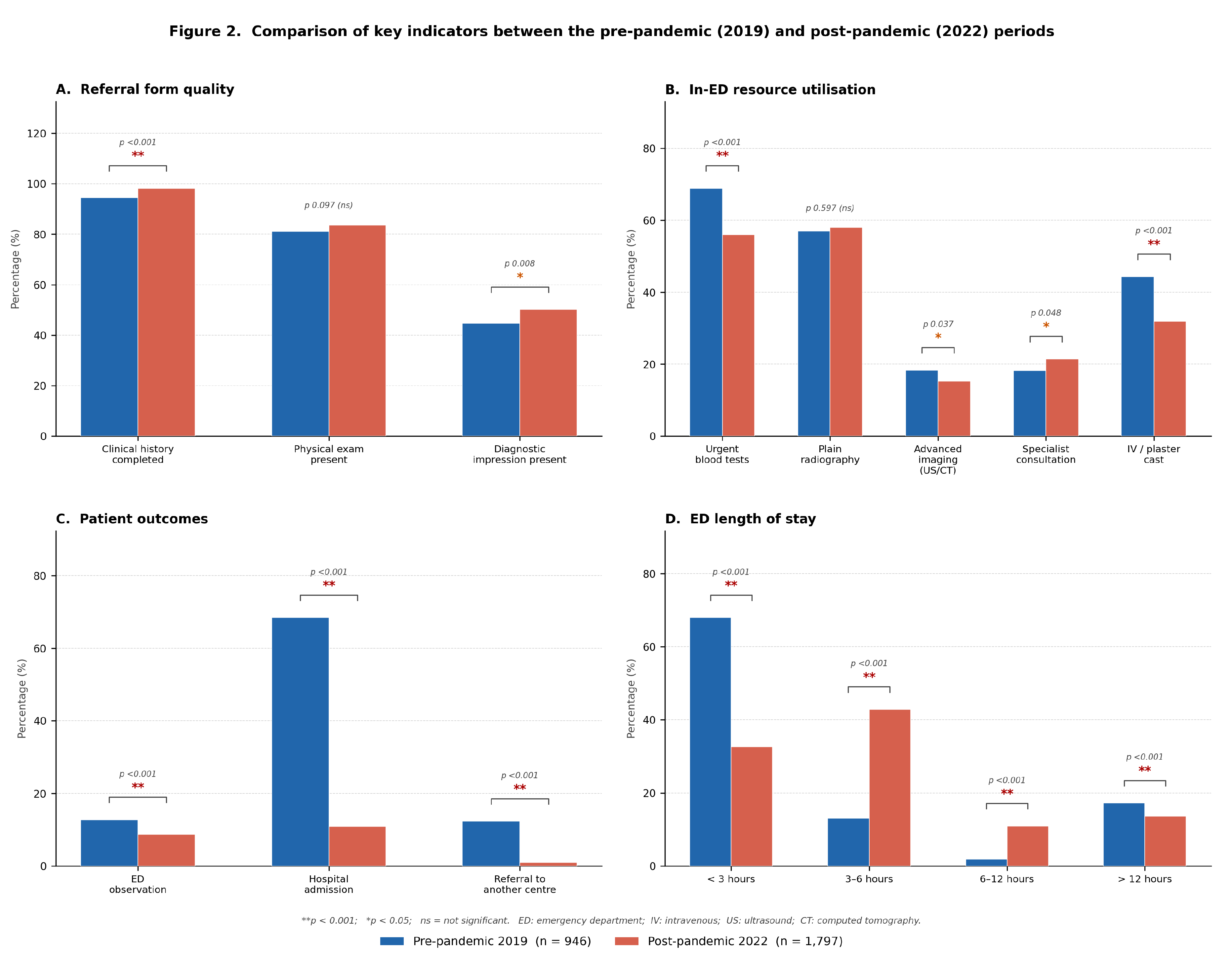
3.2. Referral Form Quality
3.3. Diagnostic Specialty Distribution
- Orthopedics: increased from 5.8% to 18.4%, nearly tripling, consistent with a surge in physical activity after the end of confinement.
- Pulmonology + COVID-19: 12.9% in 2019, rising to 22.0% in 2022 when COVID-19-specific referrals (7.7%) are combined with pulmonology (14.3%).
- Gastroenterology: decreased from 17.2% to 9.1%.
- Hematology: decreased from 7.1% to 2.7%.
- Infectious Diseases: decreased markedly from 5.7% to 0.5%.
- Ophthalmology: increased from 3.0% to 6.1%.
- Vascular Surgery: appeared as a new category in 2022 (1.1%).
3.4. Emergency Department Length of Stay
3.5. In-ED Resource Utilisation and Outcomes
- Urgent blood tests: 68.9% vs. 56.0%; .
- Advanced imaging (ultrasound or CT): 18.3% vs. 15.2%; .
- Intravenous treatment or plaster cast: 44.3% vs. 31.9%; .
- ED observation: 12.7% vs. 8.7%; .
- Hospital admission: 68.4% vs. 10.9%; .
- Referral to another centre: 12.3% vs. 0.9%; .
4. Discussion
4.1. Increase in Referral Volume
4.2. Improvement in Referral Form Quality
4.3. Changes in ED Resource Utilization
4.4. Temporal Patterns
4.5. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| COVID-19 | Coronavirus Disease 2019 |
| CT | Computed Tomography |
| ED | Emergency Department |
| ENT | Ear, Nose and Throat (Otorhinolaryngology) |
| EU | European Union |
| GP | General Practitioner |
| IV | Intravenous |
| NHS | National Health System |
| PC | Primary Care |
| SD | Standard Deviation |
| SPSS | Statistical Package for the Social Sciences |
| US | Ultrasound |
| WHO | World Health Organization |
References
- Espinosa Sabina, L.; Castilla Pérez, M.d.P. Estudio descriptivo de las derivaciones urgentes a una unidad de salud mental. Rev. De. La Asoc. Española De. Neuropsiquiatría No DOI assigned for this article. 2002, 111–123. [Google Scholar] [CrossRef]
- Márquez Cabeza, J.J.; et al. Análisis de las derivaciones hospitalarias desde un servicio de urgencias de Atención Primaria durante un año. Med. De. Fam. SEMERGEN Authors: verify full author list in Dialnet record 3747456. 2007, 33, 341–348. [Google Scholar] [CrossRef]
- Bermejo Higuera, J.C.; Carabias Maza, R.; Díaz-Albo Hermida, E.; Muñoz Alustiza, C.; Villacieros Durbán, M. Derivaciones al Servicio de Urgencias del hospital en una población de ancianos residentes: Estudio retrospectivo sobre sus causas y adecuación. Gerokomos No DOI assigned; indexed in IBECS and SciELO. 2010, 21, 114–117. [Google Scholar] [CrossRef]
- Lang, T.; Davido, A.; Diakite, B.; Agay, E.; Viel, J.F.; Flicoteaux, B. Non-urgent care in the hospital medical emergency department in France: how much and which health need does it reflect? J. Epidemiol. Community Health 1996, 50, 456–462. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Jiménez, J.; Becerra, Ó.; Boneu, F.; Bugués, L.; Pàmies, S. Análisis de la casuística de los pacientes derivables desde urgencias a atención primaria. Gac. Sanit. 2006, 20, 40–46. [Google Scholar] [CrossRef] [PubMed]
- Manzano Fernández, S.; Pastor Pérez, F.J.; Salar Alcaraz, M.; Pascual Figal, D.A. Resultados de una consulta telefónica entre cardiología y atención primaria previa a la derivación de casos dudosos a urgencias hospitalarias. Atención Primaria 2022, 54, 102303. [Google Scholar] [CrossRef] [PubMed]
- Meneses, A.S.d. Gerenciamento emergencial de recursos da Atenção Primária à Saúde no enfrentamento à pandemia da COVID-19. SciELO Prepr. Preprint; not peer-reviewed at time of citation. 2020. [Google Scholar] [CrossRef]
- Solera Albero, J.; Tárraga López, P.J. La Atención Primaria de Salud: más necesaria que nunca en la crisis del Coronavirus. J. Negat. No Posit. Results 2020, 5, 468–472. [Google Scholar] [CrossRef]
- Kuitunen, I.; Ponkilainen, V.T.; Launonen, A.P.; Reito, A.; Hevonkorpi, T.P.; Paloneva, J.; et al. The effect of national lockdown due to COVID-19 on emergency department visits. Scand. J. Trauma Resusc. Emerg. Med. 2020, 28, 114. [Google Scholar] [CrossRef] [PubMed]
- Montero-Pérez, F.J.; Jiménez Murillo, L.M. Impacto de la primera ola pandémica COVID-19 sobre los indicadores asistenciales y de calidad de un servicio de urgencias de hospital. Emergencias No DOI assigned by journal; available via Emergencias journal portal. 2021, 33, 345–353. [Google Scholar] [PubMed]
- Irazábal Olabarrieta, L.; Gutiérrez Ruiz, B. ?`Funciona la comunicación entre los niveles primario y secundario? Atención Primaria No DOI assigned; pre-DOI era publication. 1996, 17, 376–381. [Google Scholar] [PubMed]
- Morera, J.; Custodi, J.; Sanchez, K.; Miaja, F. Análisis de la calidad de la información transmitida entre atención primaria y atención especializada. Medifam No DOI assigned; pre-DOI era publication. Verify author given names. 1991, 1, 132–140. [Google Scholar]
- López-Villegas, A.; Bautista-Mesa, R.J.; Baena-López, M.Á.; Garzón-Miralles, A.; Castellano-Ortega, M.Á.; Leal-Costa, C.; et al. Impact of the COVID-19 Pandemic on Healthcare Activity in the Regional Hospitals of Andalusia (Spain). J. Clin. Med. 2022, 11, 363. [Google Scholar] [CrossRef] [PubMed]
- Bouzas Senande, E.; López Olmeda, C.; Cerrada Cerrada, E.; Olalla Linares, J.; Menéndez, J.L. Adecuación de las derivaciones desde atención primaria al servicio de urgencias hospitalario en el Área 9 de Madrid. Emergencias No DOI assigned; available as open-access PDF via journal portal. 2005, 17, 215–219. [Google Scholar]
| Variable | 2019 () | 2022 () | p-value |
|---|---|---|---|
| (%) | (%) | ||
| Sex | |||
| Female | 515 (54.4) | 968 (53.9) | 0.775 |
| Male | 431 (45.6) | 829 (46.1) | |
| PC centre of origin | |||
| PC Centre 1 | 255 (27.0) | 428 (23.8) | <0.001 |
| PC Centre 2 | 180 (19.0) | 214 (11.9) | |
| PC Centre 3 | 159 (16.8) | 278 (15.5) | |
| PC Centre 4 | 158 (16.7) | 350 (19.5) | |
| PC Centre 5 | 71 (7.5) | 96 (5.3) | |
| PC Centre 6 | 33 (3.5) | 196 (10.9) | |
| PC Centre 7 | 23 (2.4) | 107 (6.0) | |
| PC Centre 8 | 9 (1.0) | 49 (2.7) | |
| Other centres | 58 (6.1) | 79 (4.4) | |
| Day of the week | |||
| Monday | 214 (22.6) | 360 (20.0) | 0.026 |
| Tuesday | 161 (17.0) | 390 (21.7) | |
| Wednesday | 223 (23.6) | 401 (22.3) | |
| Thursday | 168 (17.8) | 340 (18.9) | |
| Friday | 180 (19.0) | 306 (17.0) | |
| Work shift | |||
| Morning (08:00–15:00) | 543 (57.4) | 993 (55.3) | 0.283 |
| Afternoon (15:00–21:00) | 403 (42.6) | 804 (44.7) | |
| Variable | 2019 () | 2022 () | p-value |
|---|---|---|---|
| (%) | (%) | ||
| Reason for referral | |||
| Specialist assessment | 878 (92.8) | 1,668 (92.9) | 0.282 |
| Request for complementary test | 68 (7.0) | 128 (7.1) | |
| Request for admission | 1 (0.1) | 0 (0.0) | |
| Appointment request | 1 (0.1) | 0 (0.0) | |
| Referral form completeness | |||
| Clinical history present | 894 (94.5) | 1,765 (98.2) | <0.001 |
| Physical examination present | 768 (81.2) | 1,504 (83.7) | 0.097 |
| Diagnostic impression present | 423 (44.7) | 899 (50.1) | 0.008 |
| Specialty | 2019 () | 2022 () | p-value |
|---|---|---|---|
| (%) | (%) | ||
| Gastroenterology | 163 (17.2) | 164 (9.1) | <0.001 |
| Cardiology | 147 (15.5) | 248 (13.8) | |
| Pulmonology | 122 (12.9) | 257 (14.3) | |
| COVID-19 | 0 (—) | 139 (7.7) | |
| Neurology | 98 (10.4) | 104 (5.8) | |
| Hematology | 67 (7.1) | 48 (2.7) | |
| ENT (Otorhinolaryngology) | 61 (6.4) | 75 (4.2) | |
| Orthopedics | 55 (5.8) | 330 (18.4) | |
| Infectious Diseases | 54 (5.7) | 9 (0.5) | |
| Urology | 51 (5.4) | 83 (4.6) | |
| Ophthalmology | 28 (3.0) | 109 (6.1) | |
| Dermatology | 38 (4.0) | 36 (2.0) | |
| Endocrinology | 17 (1.8) | 21 (1.2) | |
| Maxillofacial Surgery | 15 (1.6) | 0 (0.0) | |
| Nephrology | 5 (0.5) | 35 (1.1) | |
| Psychiatry | 8 (0.8) | 22 (1.2) | |
| General Surgery | 7 (0.7) | 62 (3.5) | |
| Gynecology | 3 (0.3) | 12 (0.7) | |
| Rheumatology | 3 (0.3) | 15 (0.8) | |
| Allergology | 0 (0.0) | 8 (0.4) | |
| Vascular Surgery | 0 (0.0) | 21 (1.1) | |
| Social Work | 2 (0.2) | 0 (0.0) |
| Variable | 2019 () | 2022 () | p-value |
|---|---|---|---|
| (%) | (%) | ||
| ED length of stay | |||
| <3 hours | 642 (67.9) | 588 (32.7) | <0.001 |
| 3–6 hours | 123 (13.0) | 769 (42.8) | |
| 6–12 hours | 18 (1.9) | 195 (10.9) | |
| >12 hours | 163 (17.2) | 245 (13.6) | |
| Complementary investigations and treatments | |||
| Urgent blood tests | 652 (68.9) | 1,011 (56.0) | <0.001 |
| Plain radiography | 539 (57.0) | 1,043 (58.0) | 0.597 |
| Advanced imaging (US or CT) | 173 (18.3) | 273 (15.2) | 0.037 |
| Urgent specialist consultation | 172 (18.2) | 384 (21.4) | 0.048 |
| IV treatment or plaster cast | 419 (44.3) | 573 (31.9) | <0.001 |
| Outcomes | |||
| ED observation area admission | 120 (12.7) | 157 (8.7) | <0.001 |
| Hospital admission | 647 (68.4) | 196 (10.9) | <0.001 |
| Referral to another centre | 116 (12.3) | 16 (0.9) | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




