Submitted:
22 April 2026
Posted:
24 April 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Research Aims
Methodology
Study Design
Study Population
Sample Size Calculation
Sampling Strategy
Data Collection Tools
- General Health Questionnaire (GHQ-30):
- 2.
- Demographic and Socioeconomic Questionnaire:
Data Collection Procedure
Statistical Analysis
Ethical Considerations
Results
Sample Characteristics
Lifestyle Habits and Experiences
Prevalence of Psychological Distress and Symptom Clusters
Bivariate Associations
Multivariable Logistic Regression
Discussion
Conclusions and Recommendations
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- World Health Organization. Adolescent mental health [Internet]. World Health Organization: Geneva, 2021; Available online: https://www.who.int/news-room/fact-sheets/detail/adolescent-mental-health.
- Patel, V.; Saxena, S.; Lund, C.; Thornicroft, G.; Baingana, F.; Bolton, P.; Chisholm, D.; Collins, P.Y.; Cooper, J.L.; Eaton, J.; et al. The Lancet Commission on global mental health and sustainable development. Lancet 2018, 392, 1553–1598. [Google Scholar] [CrossRef] [PubMed]
- Goldberg, D.P.; Williams, P. A user’s guide to the General Health Questionnaire; NFER-Nelson: Windsor, 1988. [Google Scholar]
- Goodman, R.; Ford, T.; Simmons, H.; Gatward, R.; Meltzer, H. Using the Strengths and Difficulties Questionnaire (SDQ) to screen for child psychiatric disorders in a community sample. Br. J. Psychiatry 2000, 177, 534–539. [Google Scholar] [CrossRef] [PubMed]
- Jackson, C. The General Health Questionnaire. Int Rev Psychiatry 2007, 19(3), 207–15. [Google Scholar] [CrossRef]
- Hankins, M. The reliability of the twelve-item general health questionnaire (GHQ-12) under realistic assumptions. BMC Public Heal. 2008, 8, 355–355. [Google Scholar] [CrossRef]
- Abdel-Rasoul, G.M.; Abou Salem, M.E.; Mechael, A.A.; Hendy, O.M.; El-Batanouny, M.M. Risk factors associated with stress, anxiety and depression among Egyptian adolescents: A cross-sectional study. Egypt J Community Med. 2016, 34(1), 21–33. [Google Scholar]
- El-Rufaie, O.E.F.; Daradkeh, T.K. Validation of the Arabic versions of the Thirty- and Twelve-Item General Health Questionnaires in Primary Care Patients. Br. J. Psychiatry 1996, 169, 662–664. [Google Scholar] [CrossRef]
- Abdel-Rasoul, G.; Awadalla, N.J. Psychological distress in Arab adolescents: A review. East Mediterr Health J. 2016, 22(12), 887–94. [Google Scholar]
- Gordon, J.M.; Gaffney, K.; Slavitt, H.C.; Williams, A.; Lauerer, J.A. Integrating infant mental health practice models in nursing. J. Child Adolesc. Psychiatr. Nurs. 2020, 33, 7–23. [Google Scholar] [CrossRef]
- AlYousefi, N.A.; AlYousefi, R.A.; AlYousefi, F.A.; et al. Depression and its associated factors among adolescents in Saudi Arabia. J Family Community Med. 2021, 28(1), 1–7. [Google Scholar] [CrossRef]
- Khan, A.A.; Al-Dabal, B.K.; Al-Ghamdi, S.A.; et al. Prevalence of depression, anxiety and obsessive-compulsive disorders among secondary school students in Al-Hasa Region, Saudi Arabia. J Family Community Med. 2021, 28(1), 8–14. [Google Scholar] [CrossRef]
- Ministry of Education; Saudi Arabia. Statistical yearbook 2023; Ministry of Education: Riyadh, 2023. [Google Scholar]
- Baksheev, G.N.; Robinson, J.; Cosgrave, E.M.; Baker, K.; Yung, A.R. Validity of the 12-item General Health Questionnaire (GHQ-12) in detecting depressive and anxiety disorders among high school students. Psychiatry Res. 2011, 187, 291–296. [Google Scholar] [CrossRef] [PubMed]
- Farhood, L.F.; Dimassi, H. Validation of an Arabic Version of the GHQ-28 against the Beck Depression Inventory for Screening for Depression in War-Exposed Civilians. Psychol. Rep. 2015, 116, 470–484. [Google Scholar] [CrossRef] [PubMed]
- Van Meter, A.R.; Moreira, A.L.R.; Youngstrom, E.A. Meta-Analysis of Epidemiologic Studies of Pediatric Bipolar Disorder. J. Clin. Psychiatry 2011, 72, 1250–1256. [Google Scholar] [CrossRef] [PubMed]
- Walker, M.; Mann, R.A. Exploration of mindfulness in relation to compassion, empathy and reflection within nursing education. Nurse Educ. Today 2016, 40, 188–190. [Google Scholar] [CrossRef]
- Huppert, F.A.; Corney, R.; Bramwell, G.; St Leger, S. Measuring psychological well-being: a validated instrument for use in primary care. Br J Gen Pract. 1989, 39(320), 298–302. [Google Scholar]
- Birmaher, B.; Axelson, D.; Goldstein, B.; Strober, M.; Gill, M.K.; Hunt, J.; Houck, P.; Ha, W.; Iyengar, S.; Kim, E.; et al. Four-Year Longitudinal Course of Children and Adolescents With Bipolar Spectrum Disorders: The Course and Outcome of Bipolar Youth (COBY) Study. Am. J. Psychiatry 2009, 166, 795–804. [Google Scholar] [CrossRef]
- Youngstrom, E.A. Definitional issues in bipolar disorder across the life cycle. Clin. Psychol. Sci. Pr. 2009, 16, 140–160. [Google Scholar] [CrossRef]
- Al-Yousefi, N.A.; Al-Yousefi, R.A.; Badri, M.; et al. Predictors of adolescents’ mental health problems in Saudi Arabia. J Family Community Med. 2017, 24(2), 106–12. [Google Scholar] [CrossRef]
- Mahsoon, A.; Sharif, L.; Banakhar, M.; Alasmee, N.; Almowallad, E.; Jabali, R.; Bahamil, A.; Assur, S. Parental Support, Beliefs about Mental Illness, and Mental Help-Seeking among Young Adults in Saudi Arabia. Int. J. Environ. Res. Public Heal. 2020, 17, 5615. [Google Scholar] [CrossRef]
- Hermosilla, F.; Sanders, R.; González-Mohíno, F.; Yustres, I.; González-Rave, J.M. Effects of Dry-Land Training Programs on Swimming Turn Performance: A Systematic Review. Int. J. Environ. Res. Public Heal. 2021, 18, 9340. [Google Scholar] [CrossRef]
- Al-Haqwi, A.I.; Tamim, H.; Jarallah, J.S.; et al. Exploring the predictors of depression among Saudi adolescents. Saudi Med J. 2021, 42(6), 673–80. [Google Scholar] [CrossRef] [PubMed]
- Finlay-Jones, R.A.; Murphy, E. Severity of Psychiatric Disorder and the 30-Item General Health Questionnaire. Br. J. Psychiatry 1979, 134, 609–616. [Google Scholar] [CrossRef] [PubMed]
- Sharp, D.J.; Lipscombe, J.; Calnan, M.; Azam, U.; Sampson, F.; Vail, L.; et al. Shortened General Health Questionnaire: a valid tool for depression screening in primary care? Br J Gen Pract. 1997, 47(423), 144–8. [Google Scholar]
- Agenda Julio-Septiembre 2015. Rev. de Psiquiatr. y Salud Ment. 2015, 8, 195. [CrossRef]
- Goldberg, D.P.; Hillier, V.F. A scaled version of the General Health Questionnaire. Psychol. Med. 1979, 9, 139–145. [Google Scholar] [CrossRef]
- Tait, R.J.; French, D.J.; Hulse, G.K. Validity and Psychometric Properties of the General Health Questionnaire-12 in Young Australian Adolescents. Aust. New Zealand J. Psychiatry 2003, 37, 374–381. [Google Scholar] [CrossRef]
- Montazeri, A.; Harirchi, A.M.; Shariati, M.; Garmaroudi, G.; Ebadi, M.; Fateh, A. The 12-item General Health Questionnaire (GHQ-12): translation and validation study of the Iranian version. Heal. Qual. Life Outcomes 2003, 1, 1–66. [Google Scholar] [CrossRef]
- Dwekat, E.; Al-Amer, R.M.; Al-Daraawi, H.; Saleh, M.Y.N. Prevalence and Correlates of Depression and Anxiety Among Jordanian Adolescents: A Cross-Sectional Study. Youth Soc. 2021, 55, 103–121. [Google Scholar] [CrossRef]
- Al-Gelban, K.S. Depression, anxiety and stress among Saudi adolescent school boys. Perspect. Public Heal. 2007, 127, 33–37. [Google Scholar] [CrossRef]
- Al-Shehri, M.M.; Harazi, N.M.; Elmagd, M.H.A.; T, M.A.; Alshmemri, M. Prevalence of Depression, Anxiety and Stress among Secondary School Students in Jeddah City. Asean J. Psychiatry 2022, 23. [Google Scholar] [CrossRef]
- Bischops, A.C.; Radev, S.T.; Köthe, U.; Chen, S.; Geldsetzer, P.; Sarker, M.; et al. Data resource profile: the global school-based student health survey—behavioural risk and protective factors among adolescents. Int J Epidemiol. 2023, 52(2), e102-9. [Google Scholar] [CrossRef] [PubMed]
- Amu, H.; Seidu, A.-A.; Agbemavi, W.; Afriyie, B.O.; Ahinkorah, B.O.; Ameyaw, E.K.; Kissah-Korsah, K. Psychosocial distress among in-school adolescents in Mozambique: a cross-sectional study using the Global School-Based Health Survey data. Child Adolesc. Psychiatry Ment. Heal. 2020, 14, 1–9. [Google Scholar] [CrossRef]
- World Health Organization. Report of the second global school-based student health survey (2016) in Myanmar; World Health Organization: Geneva, 2016. [Google Scholar]
- Salk, R.H.; Hyde, J.S.; Abramson, L.Y. Gender differences in depression in representative national samples: Meta-analyses of diagnoses and symptoms. Psychol. Bull. 2017, 143, 783–822. [Google Scholar] [CrossRef] [PubMed]
- Owens, J.; Au, R.; Carskadon, M.; Millman, R.; Wolfson, A.; Braverman, P.K.; Adelman, W.P.; Breuner, C.C.; et al.; ADOLESCENT SLEEP WORKING GROUP; COMMITTEE ON ADOLESCENCE Insufficient Sleep in Adolescents and Young Adults: An Update on Causes and Consequences. Pediatrics 2014, 134, e921–e932. [Google Scholar] [CrossRef] [PubMed]
- Shochat, T.; Cohen-Zion, M.; Tzischinsky, O. Functional consequences of inadequate sleep in adolescents: A systematic review. Sleep Med. Rev. 2014, 18, 75–87. [Google Scholar] [CrossRef]
- Yoo, S.-S.; Gujar, N.; Hu, P.; Jolesz, F.A.; Walker, M.P. The human emotional brain without sleep — a prefrontal amygdala disconnect. Curr. Biol. 2007, 17, R877–R878. [Google Scholar] [CrossRef]
- Moore, E.S.; E Norman, R.E.; Suetani, S.; Thomas, H.J.; Sly, P.D.; Scott, J.G. Consequences of bullying victimization in childhood and adolescence: A systematic review and meta-analysis. World J. Psychiatry 2017, 7, 60–76. [Google Scholar] [CrossRef]
- Currie, D. Growing up unequal: gender and socioeconomic differences in young people’s health and well-being. Health Behaviour in School-aged Children (HBSC) study: international report from the 2013/2014 survey; World Health Organization: Geneva, 2016. [Google Scholar]
- AlBuhairan, F.; Abou Abbas, O.; El Sayed, D.; Badri, M.; Alshahri, S.; De Vries, N. The relationship of bullying and physical violence to mental health and academic performance: a cross-sectional study among adolescents in the Kingdom of Saudi Arabia. Int J Pediatr Adolesc Med. 2017, 4(2), 61–5. [Google Scholar] [CrossRef]
- Al-Ketbi, A.; Elkonaisi, I.; Abdullahi, A.S.; Elbarazi, I.; Abu Hamada, B.; Grivna, M. Bullying victimization in schools in the United Arab Emirates: a cross-sectional study. BMC Public Heal. 2024, 24, 1–15. [Google Scholar] [CrossRef]
- Biddle, S.J.H.; Asare, M. Physical activity and mental health in children and adolescents: a review of reviews. Br. J. Sports Med. 2011, 45, 886–895. [Google Scholar] [CrossRef]
- Nguyen Ho, P.T.; Ha, P.B.; Tong, T.; Bramer, W.M.; Hofman, A.; Lubans, D.R.; et al. Mechanisms linking physical activity with psychiatric symptoms across the lifespan: a systematic review. Sports Med. 2023, 53(11), 2171–90. [Google Scholar] [CrossRef]
- Reiss, F. Socioeconomic inequalities and mental health problems in children and adolescents: A systematic review. Soc. Sci. Med. 2013, 90, 24–31. [Google Scholar] [CrossRef]
- Copeland, W.E.; Wolke, D.; Shanahan, L.; Costello, E.J. Adult functional outcomes of common childhood psychiatric problems: a prospective, longitudinal study. JAMA Psychiatry 2015, 72(9), 892–9. [Google Scholar] [CrossRef]
- Bas, G. Relation between student mental health and academic achievement revisited: a meta-analysis. In Health and academic achievement findings; IntechOpen: London, 2021. [Google Scholar]
| Socio-Demographic data | No | % |
| Age in years | ||
| 15 | 51 | 9.5% |
| 16 | 130 | 24.3% |
| 17 | 245 | 45.8% |
| 18 | 109 | 20.4% |
| Gender | ||
| Male | 363 | 67.9% |
| Female | 172 | 32.1% |
| The study year | ||
| 1st secondary school year | 96 | 17.9% |
| 2nd secondary school year | 164 | 30.7% |
| 3rd secondary school year | 275 | 51.4% |
| School type | ||
| Governmental | 366 | 68.4% |
| Private | 169 | 31.6% |
| Do you have a history of psychological/mental conditions? | ||
| Yes | 6 | 1.1% |
| No | 529 | 98.9% |
| Do you take any medications regularly? | ||
| Yes, neurological or psychiatric medications | 4 | .7% |
| Yes, medications for other diseases | 55 | 10.3% |
| None | 476 | 89.0% |
| Monthly income | ||
| < 5000 SR | 67 | 12.5% |
| 5000-10000 SR | 76 | 14.2% |
| 10000-15000 SR | 40 | 7.5% |
| > 15000 SR | 89 | 16.6% |
| I prefer not to answer | 263 | 49.2% |
| Father education | ||
| Illiterate | 13 | 2.4% |
| Primary education | 20 | 3.7% |
| Preparatory education | 42 | 7.9% |
| Secondary education | 136 | 25.4% |
| University education | 213 | 39.8% |
| Post-graduate degree | 111 | 20.7% |
| Mother education | ||
| Illiterate | 23 | 4.3% |
| Primary education | 23 | 4.3% |
| Preparatory education | 65 | 12.1% |
| Secondary education | 137 | 25.6% |
| University education | 236 | 44.1% |
| Post-graduate degree | 51 | 9.5% |
| Number of brothers and sisters | ||
| None | 8 | 1.5% |
| 1-2 | 92 | 17.2% |
| 3-4 | 224 | 41.9% |
| 5+ | 211 | 39.4% |
| Items | No | % |
| Daily sleep hours | ||
| < 4 hours/day | 33 | 6.2% |
| 4-6 hours/day | 242 | 45.2% |
| 7-9 hours/day | 201 | 37.6% |
| > 9 hours/day | 59 | 11.0% |
| Physical activity level | ||
| < 60 minutes per week | 143 | 26.7% |
| 60-400 minutes per week | 158 | 29.5% |
| > 400 minutes per week | 59 | 11.0% |
| I do not engage in any physical activity | 175 | 32.7% |
| Have you been subjected to any kind of bullying from your schoolmates during the past three years? | ||
| I have not been subjected to any type of bullying. | 415 | 77.6% |
| Yes, I have been subjected to verbal or psychological bullying. | 109 | 20.4% |
| Yes, I was subjected to physical and psychological bullying. | 7 | 1.3% |
| Yes, I was subjected to physical bullying. | 4 | .7% |
| Academic performance | ||
| Range | 20-100 | |
| Mean ± SD | 94.5 ± 8.0 | |
| Factors | Psychological distress | p-value | ||||
| No | Yes | |||||
| No | % | No | % | |||
| Age in years | 15 | 26 | 51.0% | 25 | 49.0% | .002* |
| 16 | 37 | 28.5% | 93 | 71.5% | ||
| 17 | 60 | 24.5% | 185 | 75.5% | ||
| 18 | 35 | 32.1% | 74 | 67.9% | ||
| Gender | Male | 118 | 32.5% | 245 | 67.5% | .028* |
| Female | 40 | 23.3% | 132 | 76.7% | ||
| School type | Governmental | 99 | 27.0% | 267 | 73.0% | .064 |
| Private | 59 | 34.9% | 110 | 65.1% | ||
| Do you have a history of psychological/mental conditions? | Yes | 1 | 16.7% | 5 | 83.3% | .487^ |
| No | 157 | 29.7% | 372 | 70.3% | ||
| Monthly income | < 5000 SR | 10 | 14.9% | 57 | 85.1% | .001* |
| 5000-10000 SR | 23 | 30.3% | 53 | 69.7% | ||
| 10000-15000 SR | 15 | 37.5% | 25 | 62.5% | ||
| > 15000 SR | 39 | 43.8% | 50 | 56.2% | ||
| I prefer not to answer | 71 | 27.0% | 192 | 73.0% | ||
| Father education | Illiterate | 2 | 15.4% | 11 | 84.6% | .652 |
| Primary education | 5 | 25.0% | 15 | 75.0% | ||
| Preparatory education | 10 | 23.8% | 32 | 76.2% | ||
| Secondary education | 43 | 31.6% | 93 | 68.4% | ||
| University education | 68 | 31.9% | 145 | 68.1% | ||
| Post-graduate degree | 30 | 27.0% | 81 | 73.0% | ||
| Mother education | Illiterate | 6 | 26.1% | 17 | 73.9% | .525 |
| Primary education | 7 | 30.4% | 16 | 69.6% | ||
| Preparatory education | 19 | 29.2% | 46 | 70.8% | ||
| Secondary education | 38 | 27.7% | 99 | 72.3% | ||
| University education | 78 | 33.1% | 158 | 66.9% | ||
| Post-graduate degree | 10 | 19.6% | 41 | 80.4% | ||
| Number of brothers and sisters | None | 2 | 25.0% | 6 | 75.0% | .906 |
| 1-2 | 26 | 28.3% | 66 | 71.7% | ||
| 3-4 | 64 | 28.6% | 160 | 71.4% | ||
| 5+ | 66 | 31.3% | 145 | 68.7% | ||
| Daily sleep hours | < 4 hours/day | 3 | 9.1% | 30 | 90.9% | .001* |
| 4-6 hours/day | 54 | 22.3% | 188 | 77.7% | ||
| 7-9 hours/day | 84 | 41.8% | 117 | 58.2% | ||
| > 9 hours/day | 17 | 28.8% | 42 | 71.2% | ||
| Physical activity level | < 60 minutes per week | 44 | 30.8% | 99 | 69.2% | .001* |
| 60-400 minutes per week | 63 | 39.9% | 95 | 60.1% | ||
| > 400 minutes per week | 20 | 33.9% | 39 | 66.1% | ||
| I do not engage in any physical activity | 31 | 17.7% | 144 | 82.3% | ||
| Have you been subjected to any bullying from your schoolmates during the past three years? | I have not been subjected to any bullying. | 145 | 34.9% | 270 | 65.1% | .001*^ |
| Yes, I have been subjected to verbal or psychological bullying. | 11 | 10.1% | 98 | 89.9% | ||
| Yes, I was subjected to physical and psychological bullying. | 1 | 14.3% | 6 | 85.7% | ||
| Yes, I was subjected to physical bullying. | 1 | 25.0% | 3 | 75.0% | ||
| Predictors | p-value | ORA | 95% CI | |
| Lower | Upper | |||
| Age in years | .485 | 1.14 | 0.79 | 1.62 |
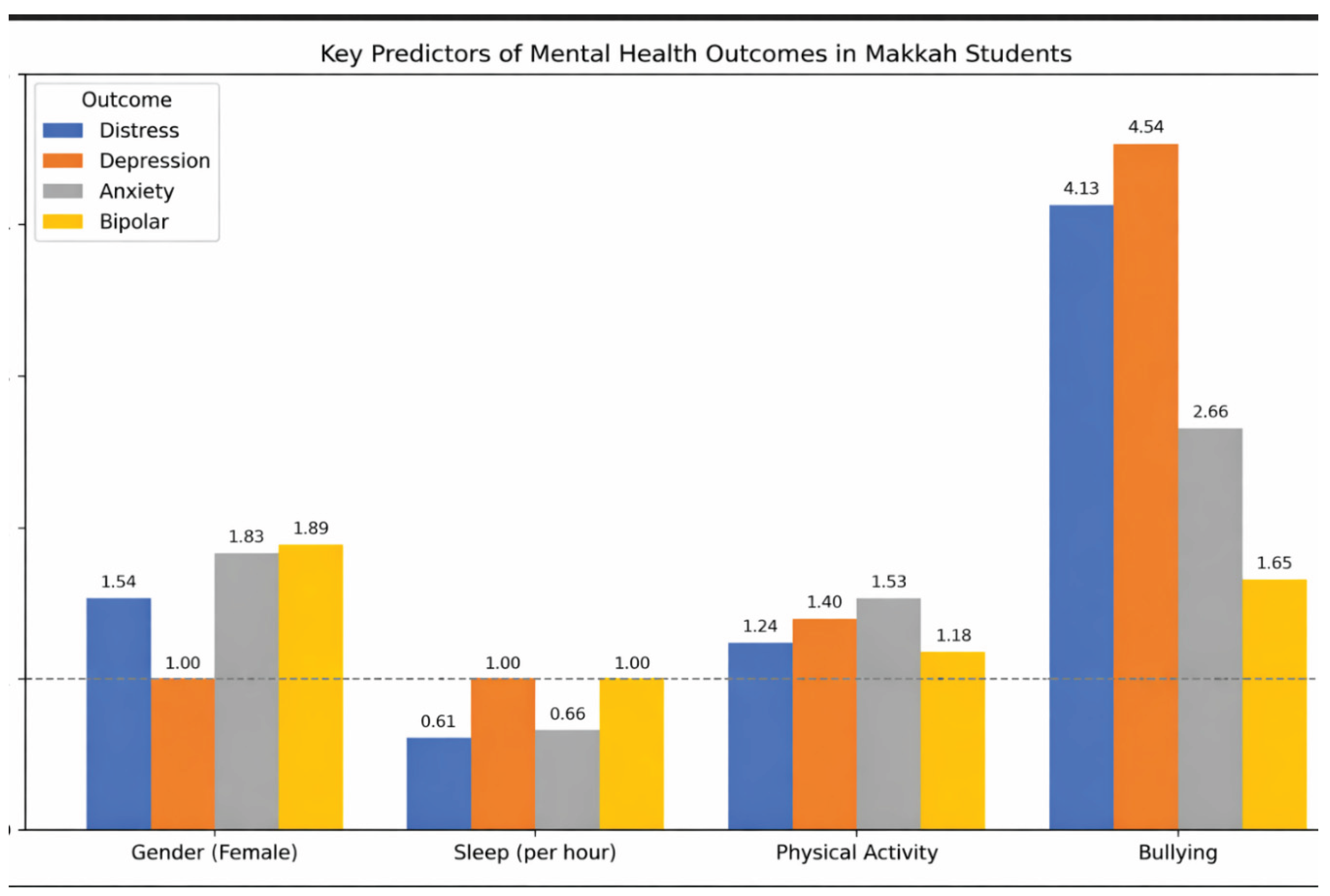
| Female vs. Male gender | .049* | 1.54 | 1.01 | 2.60 |
| Higher academic year | .444 | 1.18 | 0.77 | 1.79 |
| Private school vs. Governmental | .924 | 0.97 | 0.57 | 1.65 |
| History of psychological/mental conditions | .771 | 1.41 | 0.14 | 14.50 |
| Receive any medications | .198 | 0.63 | 0.31 | 1.27 |
| Higher family income | .841 | 0.98 | 0.85 | 1.15 |
| Higher father’s education | .859 | 1.02 | 0.82 | 1.26 |
| Higher mother’s education | .464 | 1.07 | 0.89 | 1.29 |
| Number of brothers/sisters | .545 | 0.92 | 0.70 | 1.21 |
| Academic performance (high grades) | .202 | 0.98 | 0.94 | 1.01 |
| Daily sleep hours | .001* | 0.61 | 0.47 | 0.80 |
| Physical activity engagement per week | .015* | 1.24 | 1.04 | 1.48 |
| Subjected to any kind of bullying from your schoolmates | .001* | 4.13 | 2.19 | 7.78 |
| Predictors | p-value | ORA | 95% CI | |
| Lower | Upper | |||
| Age in years | .547 | .90 | .63 | 1.28 |
| Female vs. Male gender | .768 | .93 | .57 | 1.52 |
| Higher academic year | .388 | 1.20 | .79 | 1.82 |
| Private school vs. Governmental | .132 | .67 | .39 | 1.13 |
| History of psychological/mental conditions | .048* | 11.56 | 1.99 | 134.45 |
| Receive any medications | .041* | .55 | .31 | .98 |
| Higher family income | .199 | 1.10 | .95 | 1.27 |
| Higher father’s education | .286 | .90 | .73 | 1.10 |
| Higher mother’s education | .996 | 1.00 | .83 | 1.20 |
| Number of brothers/sisters | .934 | 1.01 | .78 | 1.32 |
| Academic performance (high grades) | .501 | 1.01 | .98 | 1.04 |
| Daily sleep hours | .111 | .81 | .63 | 1.05 |
| Physical activity engagement per week | .001* | 1.40 | 1.18 | 1.66 |
| Subjected to any kind of bullying from your schoolmates | .001* | 4.54 | 2.88 | 7.17 |
| Predictors | p-value | ORA | 95% CI | |
| Lower | Upper | |||
| Age in years | .047* | .69 | .47 | 1.00 |
| Female vs. Male gender | .019* | 1.83 | 1.10 | 3.05 |
| Higher academic year | .024* | 1.68 | 1.07 | 2.64 |
| Private school vs. Governmental | .816 | .93 | .52 | 1.67 |
| History of psychological/mental conditions | .185 | 3.80 | .53 | 27.38 |
| Receive any medications | .007* | .45 | .25 | .81 |
| Higher family income | .823 | .98 | .85 | 1.14 |
| Higher father’s education | .032* | .80 | .65 | .98 |
| Higher mother’s education | .625 | .95 | .78 | 1.16 |
| Number of brothers/sisters | .852 | 1.03 | .77 | 1.36 |
| Academic performance (high grades) | .743 | 1.00 | .97 | 1.02 |
| Daily sleep hours | .003* | .66 | .51 | .87 |
| Physical activity engagement per week | .001* | 1.53 | 1.29 | 1.83 |
| Subjected to any kind of bullying from your schoolmates | .001* | 2.66 | 1.65 | 4.29 |
| Predictors | p-value | ORA | 95% CI | |
| Lower | Upper | |||
| Age in years | .700 | .93 | .66 | 1.33 |
| Female vs. Male gender | .007* | 1.89 | 1.19 | 3.00 |
| Higher academic year | .406 | 1.19 | .79 | 1.79 |
| Private school vs. Governmental | .070 | .60 | .35 | 1.04 |
| History of psychological/mental conditions | .928 | .92 | .16 | 5.20 |
| Receive any medications | .026* | .54 | .31 | .93 |
| Higher family income | .770 | .98 | .85 | 1.12 |
| Higher father’s education | .373 | .91 | .75 | 1.11 |
| Higher mother’s education | .815 | 1.02 | .85 | 1.23 |
| Number of brothers/sisters | .820 | .97 | .75 | 1.26 |
| Academic performance (high grades) | .313 | 1.01 | .99 | 1.04 |
| Daily sleep hours | .066 | .79 | .62 | 1.02 |
| Physical activity engagement per week | .040* | 1.18 | 1.01 | 1.39 |
| Subjected to any kind of bullying from your schoolmates | .033* | 1.65 | 1.04 | 2.60 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




