Submitted:
20 April 2026
Posted:
22 April 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Methods
Step 1. Review Scope and Initial Program Theories
Step 2: Searching for Evidence
Eligibility Criteria
Information Sources and Search Strategy
Information Sources
Search Concepts and Strategy Development
Screening and Selection Process
Results
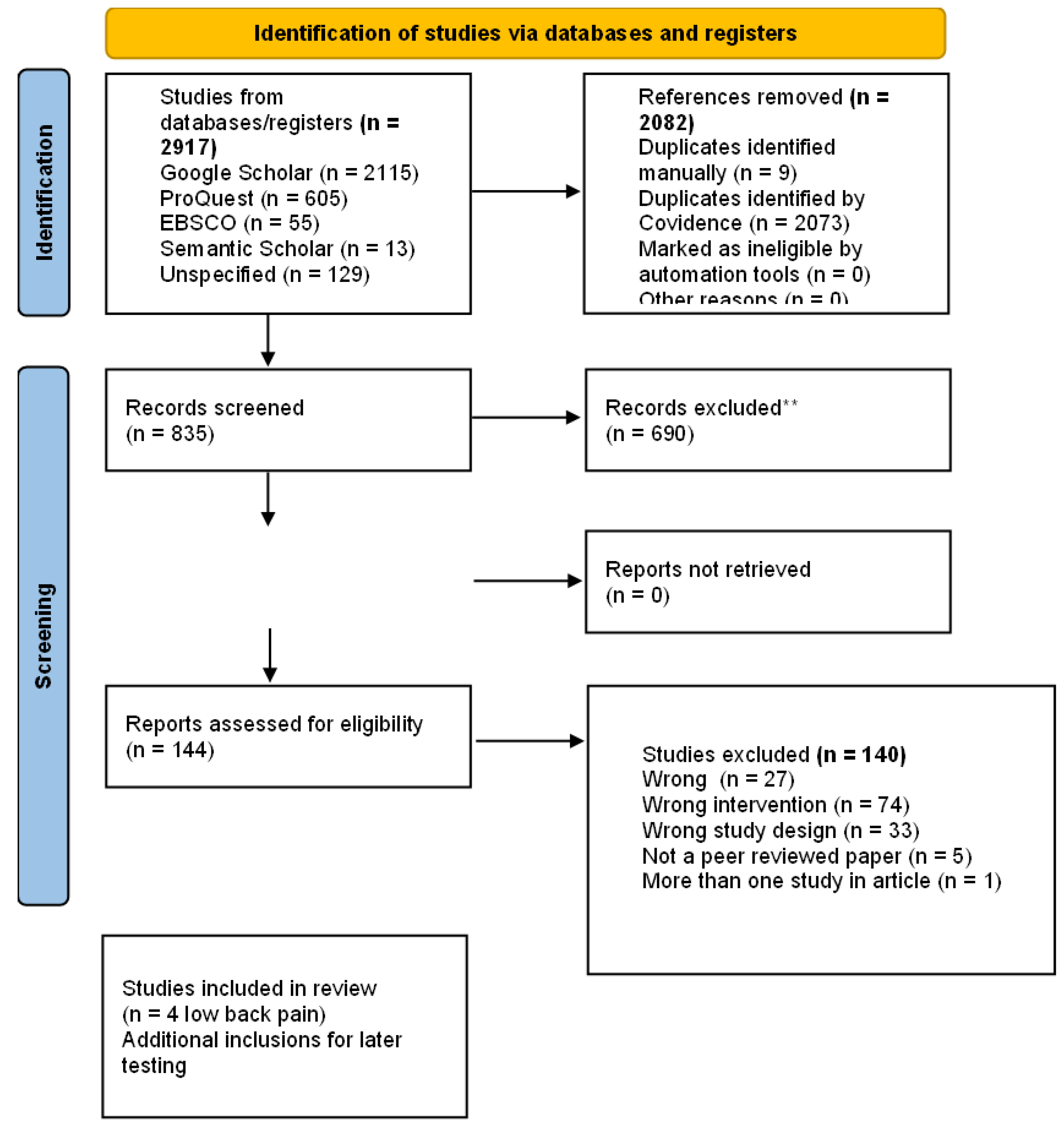
Search Output
| Medline terms used for data base searching |
| Population: (low back pain OR back pain OR lumbar pain OR nonspecific low back pain OR persistent low back pain OR chronic low back pain OR chronic musculoskeletal pain OR musculoskeletal pain OR chronic pain OR persistent pain OR arthritis OR rheumatoid arthritis OR osteoarthritis OR chronic disease OR long-term condition* OR cardiometabolic disease OR metabolic syndrome OR type 2 diabetes OR cancer survivor* OR cancer-related pain OR chronic respiratory disease OR COPD OR older adult* OR ageing OR frail* OR pre-frail OR physically inactive adult* OR sedentary adult*) Intervention: (snacktivity OR "exercise snack*" OR microbout* OR "movement break*" OR "activity break*" OR "sedentary break*" OR "brief physical activity" OR "intermittent physical activity" OR "accumulated physical activity" OR "micro exercise" OR "short bouts of exercise") Mechanisms and behavioural processes (self-efficacy OR mastery OR confidence OR fear OR "fear of movement" OR kinesiophobia OR pain-related fear OR threat appraisal OR motivation OR engagement OR adherence OR habit formation OR habit* OR automaticity OR autonomy OR capability OR identity OR psychological safety OR perceived burden OR meaning-making OR reframing OR behaviour change OR acceptability OR feasibility OR tolerance OR pacing OR symptom exacerbation) Study design (qualitative OR interview* OR focus group* OR mixed-method* OR process evaluation OR feasibility OR pilot OR observational OR realist OR experimental) |
Results
Sedentary Behaviour and Physical Activity Outcomes
Self-Reported Sitting Time
Objectively Measured Sedentary Time and Activity
Objectively Measured Physical Activity
Health-Related Outcomes
Pain and Disability
Sleep
Qualitative Findings: Factors Influencing Outcomes
Refinement of PTs
| PT | Status | Rationale | Refined IPT |
|---|---|---|---|
| IPT1 (Snacktivity supports engagement in physical activity and improves outcomes by reducing perceived threat and fear) | Partially supported → refine | Supported indirectly via indications of improvements in pain, perception of the condition, mood, social functioning. This means it is possible that fear or threat is reduced but not explicit from current evidence. | Snacktivity supports engagement by lowering the perceived burden and risk of activity, increasing psychological safety and feasibility rather than eliminating fear directly. |
| IPT2 (Snacktivity enhances self-efficacy through repeated mastery experiences.) | Strongly supported | Strongly supported by directly by habit outcomes indicators and changes in sitting, sedentary time and light physical activity changes and supported by psychosocial confidence/esteem/perc/perception of living with the condition indicators. | Repeated, achievable Snacktivity bouts generate mastery experiences that enhance self-efficacy and confidence, supporting sustained engagement through habit formation rather than performance gains. |
| IPT3 (Pain/soreness minimisation) | Supported → context-dependent | Evidence supports this indirectly by identifying benefits on disability, pain interference, adherence. However, not pain elimination | Brief, distributed activity reduces symptom exacerbation and functional interference, disrupting negative reinforcement cycles and enabling continued participation despite ongoing symptoms. |
| IPT4 (Education/coaching → meaning-making) | Strongly supported | Consistent combination of counselling based approached used and identification of emotional role functioning improvement, mood and energy change and confidence as well as life satisfaction indicators, combined with mechanism of education about sedentary risk, refarming productivity and social permission support this process theory. | Education and coaching components activate meaning-making and motivational mechanisms (e.g., reframing movement as legitimate, valuable, and achievable), increasing adherence and perceived value of activity. |
| IPT5 (Environment/routine → autonomy/habit) | Strongly supported | One of the clearest explanatory mechanisms is provided by this from qualitative evidence of factors which influence the program. This is supported by habit change identified in outcome domains and the direct benefits link to | Environments and routines that afford spontaneous movement provide cues, permission, and autonomy that support habit formation, amplifying intervention effectiveness. |
Demographics of Additional Samples
Mapped Results
Discussion
References
- Abu Zaitoon, R.; Said, N. B.; Snober, R. H.; Hussein, R. F.; Abdoon, A. H.; Abu Shehadeh, A. M.; Battat, M. M.; Sakleh, I. R. Low back pain prevalence and associated factors among nurses: A cross-sectional study from Palestine. BMC Public Health 2024, 24, 3076. [Google Scholar] [CrossRef]
- Agbangla, N. F.; Séba, M.-P.; Bunlon, F. Snacktivity™, giant games and immersive virtual reality exercises: A rapid narrative review of these new physical activity practices among older people living in nursing homes and long-term care facilities. Healthcare 2022, 10(10), 1897. [Google Scholar] [CrossRef]
- Akkarakittichoke, N.; Jensen, M. P.; Newman, A. K.; Waongenngarm, P.; Janwantanakul, P. Characteristics of office workers who benefit most from interventions for preventing neck and low back pain: A moderation analysis. Pain Reports 2022, 7(3), e1014. [Google Scholar] [CrossRef]
- Alammari, M. A.; Alammari, A. A.; Alammari, A. A.; Alammari, A.; Alammari, N. A.; Alabdali, M. Y. I. Psychosocial and occupational factors associated with low back pain among healthcare professionals: A systematic review. Cureus 2025. [Google Scholar] [CrossRef] [PubMed]
- Altuğ, F.; Ünal, A.; Kılavuz, G.; Kavlak, E.; Çitışlı, V.; Cavlak, U. Investigation of the relationship between kinesiophobia, physical activity level and quality of life in patients with chronic low back pain. Journal of Back and Musculoskeletal Rehabilitation 2016, 29, 527–531. [Google Scholar] [CrossRef]
- Alhowimel, A. S.; Alotaibi, M. A.; Alenazi, A. M.; Alqahtani, B. A.; Alshehri, M. A.; Alamam, D.; Alodaibi, F. A. Psychosocial predictors of pain and disability outcomes in people with chronic low back pain treated conservatively by guideline-based intervention: A systematic review. Journal of Multidisciplinary Healthcare 2021, 14, 3549–3559. [Google Scholar] [CrossRef]
- Alschuler, K. N.; Hoodin, F.; Murphy, S. L.; Rice, J.; Geisser, M. E. Factors contributing to physical activity in a chronic low back pain clinical sample: A comprehensive analysis using continuous ambulatory monitoring. Pain 2011, 152(11), 2521–2527. [Google Scholar] [CrossRef] [PubMed]
- Alzahrani, H.; Alshehri, M. A.; Alzhrani, M.; Alshehri, Y. S.; Al Attar, W. S. A. The association between sedentary behavior and low back pain in adults: A systematic review and meta-analysis of longitudinal studies. PeerJ 2022, 10, e13127. [Google Scholar] [CrossRef]
- André, M.; Lundberg, M. Thoughts on pain, physical activity, and body in patients with recurrent low back pain and fear: An interview study. Physical Therapy 2022, 102(2), 1–9. [Google Scholar] [CrossRef]
- Amorim, A.B.; Pappas, E.; Simic, M.; Ferreira, M.L.; Jennings, M.; Tiedemann, A.; Carvalho-E-Silva, A.P.; Caputo, E.; Kongsted, A.; Ferreira, P.H. Integrating Mobile-health, health coaching, and physical activity to reduce the burden of chronic low back pain trial (IMPACT): a pilot randomised controlled trial. BMC Musculoskelet Disord 2019, 20(1), 71. [Google Scholar] [CrossRef] [PubMed]
- Babir, F. J.; Islam, H.; McCreary, S.; Vaz, E.; Falkenhain, K.; Cranston, K.; Jung, M.; Singer, J.; Sandilands, R.; Marcotte-Chénard, A.; Stamatakis, E.; Richards, D. L.; Gibala, M. J.; Little, J. P. Technology-enabled exercise “snacks” are feasible to perform in a real-world setting: A randomized controlled trial. Scandinavian Journal of Medicine & Science in Sports 2025, 35(8), e70117. [Google Scholar] [CrossRef]
- Babir, F. J.; Marcotte-Chénard, A.; Sandilands, R. E.; Falkenhain, K.; Mulkewich, N.; Islam, H.; McCarthy, S. F.; Richards, D. L.; Madden, K.; Singer, J.; Riddell, M. C.; Jung, M. E.; Gibala, M. J.; Little, J. P. Exercise snacks are feasible to perform in the real world and improve physical capacity for adults living with non-insulin treated type 2 diabetes: A randomized trial. medRxiv (preprint) 2026. [Google Scholar] [CrossRef]
- Babir, F. J.; Islam, H.; McCreary, S.; Vaz, E.; Falkenhain, K.; Cranston, K.; Jung, M.; Singer, J.; Sandilands, R.; Marcotte-Chénard, A.; Stamatakis, E.; Richards, D. L.; Gibala, M. J.; Little, J. P. Technology-enabled exercise “snacks” are feasible to perform in a real-world setting: A randomized controlled trial. Scandinavian Journal of Medicine & Science in Sports 2025, 35, e70117. [Google Scholar] [CrossRef]
- Barone Gibbs, B.; Hergenroeder, A. L.; Perdomo, S. J.; Kowalsky, R. J.; Delitto, A.; Jakicic, J. M. Reducing sedentary behaviour to decrease chronic low back pain: The Stand Back randomised trial. Occupational and Environmental Medicine 2018, 75(5), 321–327. [Google Scholar] [CrossRef] [PubMed]
- Bandura, A. Self-efficacy: The exercise of control; W. H. Freeman, 1997. [Google Scholar]
- Boutevillain, L.; Dupeyron, A.; Rouch, C.; Richard, E.; Coudeyre, E. Facilitators and barriers to physical activity in people with chronic low back pain: A qualitative study. PLOS ONE 2017, 12(7), e0179826. [Google Scholar] [CrossRef]
- Buchbinder, R.; van Tulder, M.; Öberg, B.; Costa, L. M.; Woolf, A.; Schoene, M.; Croft, P. Low back pain: A call for action. The Lancet 2018, 391(10137), 2384–2388. [Google Scholar] [CrossRef]
- Bunzli, S.; Watkins, R.; Smith, A.; Schütze, R.; O’Sullivan, P. Lives on hold: A qualitative synthesis exploring the experience of chronic low back pain. Clinical Journal of Pain 2013, 29(10), 907–916. [Google Scholar] [CrossRef]
- Cheung, C. K. C.; Cheung, E. T. C.; Schoeb, V.; Opsommer, E.; Chong, D. Y. K.; Lee, J. L. C.; Kumlien, C.; Wong, A. Y. L. Lived experiences of older adults with chronic low back pain and implications on their daily life: A metasynthesis of qualitative research. Archives of Rehabilitation Research and Clinical Translation 2025, 7(2), 100456. [Google Scholar] [CrossRef]
- Cheng, S. W. M.; Alison, J. A.; Stamatakis, E.; Dennis, S.; McNamara, R.; Spencer, L.; McKeough, Z. Six-week behaviour change intervention to reduce sedentary behaviour in people with chronic obstructive pulmonary disease: A randomised controlled trial. Thorax 2022, 77, 231–238. [Google Scholar] [CrossRef] [PubMed]
- Christensen, M. N.; Johansen, S. K.; Sloth, S. R.; Madsen, E.; Carlsen, A.; Rathleff, M. S. Exploring self-management barriers and facilitators experienced by people with chronic musculoskeletal pain: A qualitative study (Preprint). European Journal of Pain 2023. [Google Scholar] [CrossRef]
- Comachio, J.; Beckenkamp, P. R.; Ho, E. K.-Y.; Abdel Shaheed, C.; Stamatakis, E.; Ferreira, M. L.; Lan, Q.; Mork, P. J.; Holtermann, A.; Wang, D. X. M.; Ferreira, P. H. Benefits and harms of exercise therapy and physical activity for low back pain: An umbrella review. Journal of Sport and Health Science 2025, 14, 101038. [Google Scholar] [CrossRef]
- Coole, C.; Drummond, A.; Watson, P. J.; Radford, K. What concerns workers with low back pain? Findings of a qualitative study of patients referred for rehabilitation. Journal of Occupational Rehabilitation 2010, 20(4), 472–480. [Google Scholar] [CrossRef] [PubMed]
- Curran, F.; Brennan, C.; Matthews, J.; O’Donoghue, G. A qualitative study of perceived barriers and facilitators to interrupting sedentary behavior among adults living with obesity. Obesity Science & Practice 2024, e721. [Google Scholar] [CrossRef]
- Daley, A. J.; Griffin, R. A.; Moakes, C. A.; Sanders, J. P.; Skrybant, M.; Ives, N.; Parretti, H. M.; Biddle, S. J. H.; Greaves, C.; Maddison, R.; Mutrie, N.; Esliger, D. W.; Sherar, L. B.; Edwardson, C. L.; Yates, T.; Frew, E.; Tearne, S.; Jolly, K.; Moakes, C. A. Snacktivity™ to promote physical activity and reduce future risk of disease in the population: Protocol for a feasibility randomised controlled trial and nested qualitative study. Pilot and Feasibility Studies 2023, 9, 45. [Google Scholar] [CrossRef]
- Daley, A. J.; Griffin, R. A.; Sanders, J.; Gokal, K.; Ives, N.; Skrbant, M.; Jarrett, H. M.; Edwardson, C. L.; Biddle, S. J. H.; Joll, K.; Greaves, C. J.; Greenfield, S. M.; Maddison, R.; Esliger, D. W.; Sherar, L. B.; Frew, E.; Murtre, N.; Mallor, B.; Yates, T.; Tearne, S.; Moakes, C. A. Snacktivity™ to promote physical activity in primary care, community health and public health settings: A feasibility randomised controlled trial. International Journal of Behavioral Medicine 2025, 32, 702–716. [Google Scholar] [CrossRef]
- Deci, E. L.; Ryan, R. M. The “what” and “why” of goal pursuits: Human needs and the self-determination of behavior. Psychological Inquiry 2000, 11(4), 227–268. [Google Scholar] [CrossRef]
- Ding, D.; Lawson, K. D.; Kolbe-Alexander, T. L.; Finkelstein, E. A.; Katzmarzyk, P. T.; van Mechelen, W.; Pratt, M. The economic burden of physical inactivity: A global analysis of major non-communicable diseases. The Lancet 2020, 388(10051), 1311–1324. [Google Scholar] [CrossRef] [PubMed]
- Ellingson, L. D.; Lansing, J. E.; Phillips, L. A.; Meyer, J. D. Efficacy of breaking up sedentary time on pain and mood in chronic low back pain. Medicine & Science in Sports & Exercise 2023, 55, 899. [Google Scholar] [CrossRef]
- Ellingson, L. D.; Connolly, M. L.; Lansing, J. E.; Phillips, L. A.; Meyer, J. D. Evaluating the effects of a sedentary time reduction intervention on pain, mood, and quality of life in chronic low back pain: A pilot randomized controlled trial. Journal of Behavioral Medicine 2026. [Google Scholar] [CrossRef]
- Ferreira, M. L.; de Luca, K.; Haile, L.; et al. Global, regional, and national burden of low back pain, 1990–2020, its attributable risk factors, and projections to 2050: A systematic analysis of the Global Burden of Disease Study 2021. The Lancet Rheumatology 2023, 5(6), e316–e329. [Google Scholar] [CrossRef]
- Foster, N. E.; Anema, J. R.; Cherkin, D.; Chou, R.; Cohen, S. P.; Gross, D. P.; Ferreira, P. H.; Fritz, J. M.; Koes, B. W.; Peul, W.; Turner, J. A.; Maher, C. G. Prevention and treatment of low back pain: Evidence, challenges, and promising directions. The Lancet 2018, 391(10137), 2368–2383. [Google Scholar] [CrossRef]
- Fyfe, J. J.; Dalla Via, J.; Jansons, P.; Scott, D.; Day, R. M. Feasibility and acceptability of a remotely delivered, home-based, pragmatic resistance ‘exercise snacking’ intervention in community-dwelling older adults: A pilot randomised controlled trial. BMC Geriatrics 2022, 22, 521. [Google Scholar] [CrossRef] [PubMed]
- Gokal, K.; Amos-Hirst, R.; Moakes, C. A.; Sanders, J. P.; Esliger, D. W.; Sherar, L. B.; Ives, N.; Biddle, S. J. H.; Edwardson, C.; Yates, T.; Frew, E.; Greaves, C.; Greenfield, S. M.; Jolly, K.; Skrybant, M.; Maddison, R.; Mutrie, N.; Parrett, H. M.; Daley, A. J. Views of the public about Snacktivity™: A small changes approach to promoting physical activity and reducing sedentary behaviour. BMC Public Health 2022, 22, 618. [Google Scholar] [CrossRef] [PubMed]
- Graham, J.; Murphy, C.; Montgomery, C.; Twomey, B.; Timmons, J.; Egan, B. Feasibility and effectiveness of exercise snacking in older adults: A pilot randomized controlled trial. PM&R 2025, 17, S2–S175. [Google Scholar] [CrossRef]
- Hartvigsen, J.; Hancock, M. J.; Kongsted, A.; Louw, Q.; Ferreira, M. L.; Genevay, S.; Hoy, D.; Karppinen, J.; Pransky, G.; Sieper, J.; Smeets, R. J.; Underwood, M. What low back pain is and why we need to pay attention. The Lancet 2018, 391(10137), 2356–2367. [Google Scholar] [CrossRef] [PubMed]
- Hergenroeder, A. L.; Quinn, T. D.; Perdomo, S. J.; Kline, C. E.; Barone Gibbs, B. Effect of a 6-month sedentary behavior reduction intervention on well-being and workplace health in desk workers with low back pain. Work: A Journal of Prevention, Assessment & Rehabilitation 2022, 71(4), 1003–1014. [Google Scholar] [CrossRef]
- Hu, Z.; Li, S.; Shi, X.; Huang, K.; Huang, H.; Yuan, X. Feasibility and acceptability of a remotely delivered, home-based “exercise snacking” to improve physical function in community-dwelling older adults: A 28-day pilot study. Frontiers in Medicine 2026, 13, 1755508. [Google Scholar] [CrossRef]
- Gardner, B.; Lally, P.; Wardle, J. Making health habitual: The psychology of “habit-formation” and general practice. British Journal of General Practice 2012, 62(605), 664–666. [Google Scholar] [CrossRef]
- Gallagher, K. M.; Payne, M.; Daniels, B.; Caldwell, A. R.; Ganio, M. S. Walking breaks can reduce prolonged standing-induced low back pain. Human Movement Science 2019, 66, 31–37. [Google Scholar] [CrossRef]
- GBD 2019 Diseases and Injuries Collaborators. Global burden of 369 diseases and injuries in 204 countries and territories, 1990–2019: A systematic analysis for the Global Burden of Disease Study 2019. The Lancet 2020, 396(10258), 1204–1222. [Google Scholar] [CrossRef]
- Geneen, L. J.; Moore, R. A.; Clarke, C.; Martin, D.; Colvin, L. A.; Smith, B. H. Physical activity and exercise for chronic pain in adults: An overview of Cochrane Reviews. Cochrane Database of Systematic Reviews 2017, CD011279. [Google Scholar] [CrossRef] [PubMed]
- George, S. Z.; Goossens, M. E. J. B.; Vlaeyen, J. W. S.; Fritz, J. M. Psychological factors, physical activity, and pain-related fear in low back pain: Implications for rehabilitation. Journal of Orthopaedic & Sports Physical Therapy 2022, 52(9), 515–525. [Google Scholar] [CrossRef]
- Chandran, O.; Shruthi, P.; Sukumar, S.; Kadavigere, R.; Chakravarthy, K.; Rao, C. R.; Chandrasekaran, B. Effects of physical activity breaks during prolonged sitting on vascular and executive function: A randomised cross-over trial. Journal of Taibah University Medical Sciences 2023, 18(5), 1065–1075. [Google Scholar] [CrossRef] [PubMed]
- Gokal, K.; Amos-Hirst, R.; Moakes, C. A.; Sanders, J. P.; Esliger, D. W.; Sherar, L. B.; Ives, N.; Biddle, S. J. H.; Edwardson, C.; Yates, T.; Frew, E.; Greaves, C.; Greenfield, S. M.; Jolly, K.; Skrybant, M.; Maddison, R.; Mutrie, N.; Parretti, H. M.; Daley, A. J. Views of the public about Snacktivity™: A small changes approach to promoting physical activity and reducing sedentary behaviour. BMC Public Health 2022, 22, 618. [Google Scholar] [CrossRef]
- Hartvigsen, J.; Hancock, M. J.; Kongsted, A.; Louw, Q.; Ferreira, M. L.; Genevay, S.; Hoy, D.; Karppinen, J.; Pransky, G.; Sieper, J.; Smeets, R. J.; Underwood, M. What low back pain is and why we need to pay attention. The Lancet 2018, 391(10137), 2356–2367. [Google Scholar] [CrossRef]
- Ho, E. K.-Y.; Chen, L.; Simic, M.; Ashton-James, C. E.; Comachio, J.; Wang, D. X. M.; Hayden, J. A.; Ferreira, M. L.; Ferreira, P. H. Psychological interventions for chronic, non-specific low back pain: Systematic review with network meta-analysis. BMJ 2022, 376, e067718. [Google Scholar] [CrossRef]
- Holden, M. A.; Haywood, K. L.; Potia, T. A.; Gee, M.; McLean, S. The role of exercise self-efficacy in people with chronic musculoskeletal pain: A systematic review. Rheumatology 2010, 49(5), 967–976. [Google Scholar] [CrossRef]
- Jansons, P.; Fyfe, J. J.; Dalla Via, J.; Daly, R. M.; Scott, D. Barriers and enablers associated with participation in a home-based pragmatic exercise snacking program in older adults delivered and monitored by Amazon Alexa: A qualitative study. Aging Clinical and Experimental Research 2023, 35, 561–569. [Google Scholar] [CrossRef]
- Jakicic, J. M.; Wing, R. R.; Butler, B. A.; Robertson, R. J. Prescribing exercise in multiple short bouts versus one continuous bout: Effects on adherence, cardiorespiratory fitness, and weight loss in overweight women. International Journal of Obesity and Related Metabolic Disorders 1995, 19, 893–901. [Google Scholar]
- Jenkins, E. M.; Nairn, L. N.; Skelly, L. E.; Little, J. P.; Gibala, M. J. Do stair climbing exercise “snacks” improve cardiorespiratory fitness? Applied Physiology, Nutrition, and Metabolism 2019, 44(6), 681–684. [Google Scholar] [CrossRef]
- Jones, M. D.; Clifford, B. K.; Stamatakis, E.; Gibbs, M. T. Exercise snacks and other forms of intermittent physical activity for improving health in adults and older adults: A scoping review of epidemiological, experimental and qualitative studies. Sports Medicine 2024, 54(4), 813–835. [Google Scholar] [CrossRef]
- Keefe, F. J.; Main, C. J.; George, S. Z. Advancing psychologically informed practice for patients with persistent musculoskeletal pain: Promise, pitfalls, and solutions. Physical Therapy 2018, 98(5), 398–407. [Google Scholar] [CrossRef]
- Krouwel, M.; Greenfield, S. M.; Chalkley, A.; Sanders, J. P.; Parretti, H. M.; Gokal, K.; Jolly, K.; Skrybant, M.; Biddle, S. J. H.; Greaves, C.; Maddison, R.; Mutrie, N.; Ives, N.; Esliger, D. W.; Sherar, L.; Edwardson, C. L.; Yates, T.; Frew, E.; Tearne, S.; Daley, A. J. Promoting participation in physical activity through Snacktivity™: A qualitative mixed methods study. PLOS ONE 2023, 18(9), e0291040. [Google Scholar] [CrossRef]
- Liang, I. J.; Francombe-Webb, J.; McGuigan, P. M.; Perkin, O. J.; Thompson, D.; Western, M. J. The acceptability of home-based exercise snacking and Tai-chi snacking amongst high- and low-function UK and Taiwanese older adults. Frontiers in Aging 2023, 4, 1180939. [Google Scholar] [CrossRef]
- Liang, I. J.; Perkin, O. J.; Williams, S.; McGuigan, P. M.; Thompson, D.; Western, M. J. The efficacy of 12-week progressive home-based strength and Tai-Chi exercise snacking in older adults: A mixed-method exploratory randomised controlled trial. Journal of Frailty & Aging 2024, 13(4), 572–581. [Google Scholar] [CrossRef]
- Lally, P.; van Jaarsveld, C. H. M.; Potts, H. W. W.; Wardle, J. How are habits formed: Modelling habit formation in the real world. European Journal of Social Psychology 2010, 40(6), 998–1009. [Google Scholar] [CrossRef]
- Lansing, J. E.; Ellingson, L. D.; DeShaw, K. J.; Cruz-Maldonado, G.; Hurt, T. R.; Meyer, J. D. A qualitative analysis of barriers and facilitators to reducing sedentary time in adults with chronic low back pain. BMC Public Health 2021, 21, 215. [Google Scholar] [CrossRef]
- Latza, U.; Karmaus, W.; Stürmer, T. alCohort study of occupational risk factors of low back pain in construction workers. Occupational and Environmental Medicine 2000, 57, 28–34. [Google Scholar] [CrossRef] [PubMed]
- Lynch, B. M.; Courneya, K. S.; Sethi, P.; Patrao, T. A.; Hawkes, A. L. A randomized controlled trial of a multiple health behavior change intervention delivered to colorectal cancer survivors: Effects on sedentary behavior. Cancer 2014, 120, 2665–2672. [Google Scholar] [CrossRef] [PubMed]
- Lynch, B. M.; Nguyen, N. H.; Moore, M. M.; Reeves, M. M.; Rosenberg, D. E.; Boyle, T.; Vallance, J. K.; Milton, S.; Friedenreich, C. M.; English, D. R. A randomized controlled trial of a wearable technology–based intervention for increasing moderate-to-vigorous physical activity and reducing sedentary behavior in breast cancer survivors: The ACTIVATE Trial. Cancer 2019, 125, 2846–2855. [Google Scholar] [CrossRef] [PubMed]
- Manaenkova, Z.; Santanna, E. Movement snacks as a non-pharmacological approach to symptom management and lifestyle adaptation in menopausal transition: A qualitative study. Frontiers 2025, 5(3), 150–158. [Google Scholar] [CrossRef]
- Maxwell-Smith, C.; Hince, D.; Cohen, P. A.; Bulsara, M. K.; Boyle, T.; Platell, C.; Tan, P.; Levitt, M.; Salama, P.; Tan, J.; Salfinger, S.; Makin, G.; Mohan, G. R. K. A.; Jiménez-Castuera, R.; Hardcastle, S. J. A randomized controlled trial of WATAAP to promote physical activity in colorectal and endometrial cancer survivors. Psycho-Oncology 2019, 28, 1420–1429. [Google Scholar] [CrossRef] [PubMed]
- McMillan, J.; Soundy, A. Exploration of How Uncertainty Tolerance, Emotion Regulation, and Hope Are Linked and Influenced in People with Chronic Low Back Pain: A Worked Example of a Social Constructivist Meta-Ethnography Study. Behavioral Sciences 2025, 15(10), 1399. [Google Scholar] [CrossRef] [PubMed]
- Mescouto, K.; Olson, R. E.; Hodges, P. W.; Setchell, J. A critical review of the biopsychosocial model of low back pain care: Time for a new approach? Disability and Rehabilitation 2022, 44(13), 3270–3284. [Google Scholar] [CrossRef]
- Michie, S.; Atkins, L.; West, R. The behaviour change wheel: A guide to designing interventions; Silverback Publishing, 2014. [Google Scholar]
- Mues, J. P.; Flohr, S.; Kurpiers, N. The influence of workplace-integrated exercise snacks on cognitive performance in sedentary middle-aged adults: A randomized pilot study. Sports 2025, 13(6), 186. [Google Scholar] [CrossRef]
- National Institute for Health and Care Excellence. Low back pain and sciatica in over 16s: Assessment and management (NICE Guideline NG59). 2016. updated 2020. Available online: https://www.nice.org.uk/guidance/ng59.
- Norha, J.; Sjöros, T.; Garthwaite, T.; Laine, S.; Saarenhovi, M.; Kallio, P.; Laitinen, K.; Houttu, N.; Vähä-Ypyä, H.; Sievänen, H.; Löyttyniemi, E.; Vasankari, T.; Knuuti, J.; Kalliokoski, K. K.; Heinonen, I. H. A. Effects of reducing sedentary behavior on cardiorespiratory fitness in adults with metabolic syndrome: A 6-month randomized controlled trial. Scandinavian Journal of Medicine & Science in Sports 2023, 33, 1452–1461. [Google Scholar] [CrossRef]
- Norha, J.; Sjöros, T.; Garthwaite, T.; Laine, S.; Laitinen, K.; Houttu, N.; Vähä-Ypyä, H.; Sievänen, H.; Löyttyniemi, E.; Vasankari, T.; Knuuti, J.; Kalliokoski, K. K.; Heinonen, I. H. A. Secondary analysis of a randomised controlled trial on reducing sedentary behaviour and its effects on quality of life and wellbeing. Scientific Reports 2025, 15, 36861. [Google Scholar] [CrossRef]
- Oppezzo, M. A.; Tremmel, J. A.; Kapphahn, K.; Desai, M.; Baiocchi, M.; Sanders, M.; Prochaska, J. J. Feasibility, preliminary efficacy, and acceptability of a Twitter-based social support group vs Fitbit-only to decrease sedentary behavior in women. Internet Interventions 2021, 25, 100426. [Google Scholar] [CrossRef]
- Patterson, K.; Davey, R.; Keegan, R.; Niyonsenga, T.; Mohanty, I.; Bowen, S.; Regan, E.; Lander, M.; van Berlo, S.; Freene, N. Testing the effect of a smartphone app on hospital admissions and sedentary behavior in cardiac rehabilitation participants: ToDo-CR randomized controlled trial. JMIR mHealth and uHealth 2023, 11, e48229. [Google Scholar] [CrossRef] [PubMed]
- Pawson, R.; Greenhalgh, T.; Harvey, G.; Walshe, K. Realist review—A new method of systematic review designed for complex policy interventions. Journal of Health Services Research & Policy 2005, 10, 21–34. [Google Scholar] [CrossRef]
- Perkin, O. J.; McGuigan, P. M.; Stokes, K. A. Exercise snacking to improve muscle function in healthy older adults: A pilot study. Journal of Aging Research 2019, 7516939. [Google Scholar] [CrossRef] [PubMed]
- Pincus, T.; Burton, A. K.; Vogel, S.; Field, A. P. A systematic review of psychological factors as predictors of chronicity/disability in prospective cohorts of low back pain. Spine 2002, 27(5), E109–E120. [Google Scholar] [CrossRef]
- Poppe, L.; De Bourdeaudhuij, I.; Verloigne, M.; Shadid, S.; Van Cauwenberg, J.; Compernolle, S.; Crombez, G. Efficacy of a self-regulation–based electronic and mobile health intervention targeting an active lifestyle in adults having type 2 diabetes and in adults aged 50 years or older: Two randomized controlled trials. Journal of Medical Internet Research 2019, 21(8), e13363. [Google Scholar] [CrossRef]
- Pronk, N. P.; Katz, A. S.; Lowry, M.; Payfer, J. R. Reducing occupational sitting time and improving worker health: The Take-a-Stand Project, 2011. Preventing Chronic Disease 2012, 9, 110323. [Google Scholar] [CrossRef]
- Qaseem, A.; Wilt, T. J.; McLean, R. M.; Forciea, M. A. Noninvasive treatments for acute, subacute, and chronic low back pain: A clinical practice guideline from the American College of Physicians. Annals of Internal Medicine 2017, 166(7), 514–530. [Google Scholar] [CrossRef]
- Roren, A.; Daste, C.; Coleman, M.; Rannou, F.; Freyssenet, D.; Moro, C.; Lefèvre-Colau, M.-M.; Nguyen, C. Physical activity and low back pain: A critical narrative review. Annals of Physical and Rehabilitation Medicine 2023, 66(2), 101650. [Google Scholar] [CrossRef]
- Sanders, J. P.; Gokal, K.; Thomas, J. J. C.; Rawstorn, J. C.; Sherar, L. B.; Maddison, R.; Greaves, C. J.; Esliger, D.; Daley, A. J.; on behalf of the Snacktivity Investigators. Development of a mobile health Snacktivity app to promote physical activity in inactive adults (SnackApp): Intervention mapping and user testing study. JMIR Formative Research 2023, 7, e41114. [Google Scholar] [CrossRef]
- Sallis, J. F.; Owen, N.; Fisher, E. B. Ecological models of health behavior. In Health behavior: Theory, research, and practice, 5th ed.; Glanz, K., Rimer, B. K., Viswanath, K., Eds.; Jossey-Bass, 2016; pp. 43–64. [Google Scholar]
- Sjöros, T.; Laine, S.; Garthwaite, T.; Vähä-Ypyä, H.; Löyttyniemi, E.; Koivumäki, M.; Houttu, N.; Laitinen, K.; Kalliokoski, K. K.; Sievänen, H.; Vasankari, T.; Knuuti, J.; Heinonen, I. H. A. Reducing sedentary time and whole-body insulin sensitivity in metabolic syndrome: A 6-month randomized controlled trial. Medicine & Science in Sports & Exercise 2023, 55(3), 342–353. [Google Scholar] [CrossRef]
- Sjöros, T.; Laine, S.; Garthwaite, T.; Vähä-Ypyä, H.; Koivumäki, M.; Eskola, O.; Löyttyniemi, E.; Houttu, N.; Laitinen, K.; Kalliokoski, K. K.; Sievänen, H.; Vasankari, T.; Knuuti, J.; Heinonen, I. H. A. The effects of a 6-month intervention aimed to reduce sedentary time on skeletal muscle insulin sensitivity: A randomized controlled trial. American Journal of Physiology – Endocrinology and Metabolism 2023, 325, E152–E162. [Google Scholar] [CrossRef] [PubMed]
- Stork, M. J.; Marcotte-Chénard, A.; Jung, M. E.; Little, J. P. Exercise in the workplace: Examining the receptivity of practical and time-efficient stair-climbing “exercise snacks”. Applied Physiology, Nutrition, and Metabolism 2024, 49, 30–40. [Google Scholar] [CrossRef] [PubMed]
- Stamatakis, E.; Gale, J.; Bauman, A.; Ekelund, U.; Hamer, M.; Ding, D.; Britton, A. Associations between vigorous intermittent lifestyle physical activity and mortality. Nature Medicine 2022, 28(12), 2521–2529. [Google Scholar] [CrossRef]
- Stawarz, K.; Liang, I. J.; Alexander, L.; Carlin, A.; Wijekoon, A.; Western, M. J. Exploring the potential of technology to promote exercise snacking for older adults who are prefrail in the home setting: User-centered design study. JMIR Aging 2023, 6, e41810. [Google Scholar] [CrossRef] [PubMed]
- Thomsen, T.; Aadahl, M.; Beyer, N.; Hetland, M. L.; Løppenthin, K.; Midtgaard, J.; Christensen, R.; Østergaard, M.; Jennum, P. J.; Esbensen, B. A. The efficacy of motivational counselling and SMS reminders on daily sitting time in patients with rheumatoid arthritis: A randomised controlled trial. Annals of the Rheumatic Diseases 2017, 76, 1603–1606. [Google Scholar] [CrossRef] [PubMed]
- Thomsen, T.; Aadahl, M.; Beyer, N.; Hetland, M. L.; Løppenthin, K. B.; Midtgaard, J.; Christensen, R.; Nielsen, S. M.; Østergaard, M.; Jennum, P.; Esbensen, B. A. Sustained long-term efficacy of motivational counseling and text message reminders on daily sitting time in patients with rheumatoid arthritis: Long-term follow-up of a randomized, parallel-group trial. Arthritis Care & Research 2020, 72(11), 1560–1570. [Google Scholar] [CrossRef]
- Thøgersen-Ntoumani, C.; Kritz, M.; Grunseit, A.; Chau, J.; Ahmadi, M.; Holtermann, A.; Koster, A.; Tudor-Locke, C.; Johnson, N.; Sherrington, C.; Paudel, S.; Maher, C.; Stamatakis, E. Barriers and enablers of vigorous intermittent lifestyle physical activity (VILPA) in physically inactive adults: A focus group study. International Journal of Behavioral Nutrition and Physical Activity 2023, 20, 78. [Google Scholar] [CrossRef]
- Tyldesley-Marshall, N.; Greenfield, S. M.; Parretti, H. M.; Gokal, K.; Greaves, C.; Jolly, K.; Maddison, R.; Daley, A. J. Snacktivity™ to promote physical activity: A qualitative study. International Journal of Behavioral Medicine 2022, 29, 553–564. [Google Scholar] [CrossRef]
- van Bakel, B. M. A.; Kroesen, S. H.; Bakker, E. A.; van Mierlo, R. V.; Güna, A.; Scheepmaker, A.; Aengevaeren, W. R. M.; Wiems, F. F.; Wondergem, R.; Pisters, M. F.; de Bruin, M.; Hopman, M. T. E.; Thijssen, D. H. J.; Eijsvogels, T. M. H. Effectiveness of an intervention to reduce sedentary behaviour as a personalised secondary prevention strategy for patients with coronary artery disease: Main outcomes of the SIT LESS randomised clinical trial. International Journal of Behavioral Nutrition and Physical Activity 2023, 20, 17. [Google Scholar] [CrossRef]
- Vlaeyen, J. W. S.; Linton, S. J. Fear-avoidance and its consequences in chronic musculoskeletal pain: A state of the art. Pain 2012, 153(6), 1144–1147. [Google Scholar] [CrossRef]
- Western, M. J.; Welsh, T.; Keen, K.; Bishop, V.; Perkin, O. J. Exercise snacking to improve physical function in pre-frail older adult memory clinic patients: A 28-day pilot study. BMC Geriatrics 2023, 23, 471. [Google Scholar] [CrossRef] [PubMed]
- Wong, G.; Greenhalgh, T.; Westhorp, G.; et al. RAMESES publication standards: realist syntheses. BMC Med 2013, 11, 21. [Google Scholar] [CrossRef]
- Wong, G.; Westhorp, G.; Manzano, A.; et al. RAMESES II reporting standards for realist evaluations. BMC Med 2016, 14, 96. [Google Scholar] [CrossRef] [PubMed]
- Wood, L.; Foster, N. E.; Dean, S. G.; Booth, V.; Hayden, J. A.; Booth, A. Contexts, behavioural mechanisms and outcomes to optimise therapeutic exercise prescription for persistent low back pain: A realist review. British Journal of Sports Medicine 2024, 58(4), 222–230. [Google Scholar] [CrossRef] [PubMed]
- Yin, M.; Deng, S.; Chen, Z.; Zhang, B.; Zheng, H.; Bai, M.; Li, H.; Zhang, X.; Deng, J.; Liu, Q.; Little, J. P.; Li, Y. Exercise snacks are a time-efficient alternative to moderate-intensity continuous training for improving cardiorespiratory fitness but not maximal fat oxidation in inactive adults: A randomized controlled trial. Applied Physiology, Nutrition, and Metabolism 2024. [Google Scholar] [CrossRef] [PubMed]
| IPT | Key Mechanisms producing better engagement, health and adherence outcomes |
|---|---|
| 1 | Low back pain threat and fear
|
Exercise format and threat
| |
Snacktivity and intermitted activity
| |
| 2 | Importance of self-efficacy in LBP
|
The value of mastery experiences
| |
Snacktivity logic
| |
| 3 | The importance of post exercise pain
|
Activity Dosing
| |
Snacktivity plausibility
| |
| 4 | The value of psychological and educational interventions
|
The value of education and coaching
| |
The compatibility with Snacktivity
| |
| 5 | Environment and physical activity
|
Habit formation
| |
Autonomy
| |
The compatibility with Snacktivity
|
| Studies | Evidence for reduced sitting & light physical activity | Evidence for habit formation outcomes (standing more or breaking up prolonged sitting) | Quality of life Outcomes | Pain | Confidence | Mood and Energy or Fatigue |
|---|---|---|---|---|---|---|
| Chronic conditions |
Reduce sitting and sedentary behaviour • 6/15 studies @Sig with OE (reductions between 42-51 mins/day) • 5/15 meaningful within group reductions • 3/15 no meaningful effect Light physical activity • 6/15 studies @Sig with OE • 5/15 studies no group effect but meaningful changes • 4/15 with no light physical activity change noticed |
Direct habit Indicators • 5/15 studies identified significant changes (setting/standing) with 4/15 @Sig OE. • 10/15 with any habit relevant evidence • 2/15 with no evidence Habit mechanisms • 5/15 with supportive mechanisms • 3/15 with adherence driven evidence • 3/15 with cue-based intervention • 3/15 explicitly theory |
• 4/15 (4/5) identify @Sig with SR • 3/15 used SF-36 to quantify with clinically meaningful change across both physical and mental sub-domains • 10/15 did not measure the domain |
• 2/15 (2/6) identify @Sig with SR • 2/15 used VAS and identify clinically meaningful change • 2/15 identified no significant effect (although 1/15 identified association of reduced pain with decrease body mass index or body fat) • 1/15 reported worsening of COPD scores and or pain • 9/15 did not measure pain |
• 8/15 with some sort of confidence signal (qualitative and quantitative combined) • 4/15 (4/8) @Sig SR. using validated scale. 3/15 with moderate and large effect • 4/15 identified qualitative evidence of improvement - mechanisms identified as exercises perceived as manageable, reduced apprehension of activity, feeling in control of progression, reduced psychological barriers • 7/15 did not measure confidence |
Mood • 4/15 (4/9) @Sig SR • 2/15 with sustained effects • 3/15 with qualitative evidence • 1/15 with limited benefit • 6/15 did not report mood Energy or Fatigue • 3/15 (3/9) @Sig SR • 4/15 (4/9) reported positive energy or reduced fatigue evidence e.g., sit to stand repetition, tolerance for repeated movement, less tired during daily activities • 6/15 did not measure energy or fatigue |
| Older adults |
Reduce sitting and sedentary behaviour • 2/8 studies @Sig with OE(reductions between 40-50 minutes) • 2/8 qualitative supporting evidence • 3/8 supportive but sitting measurement (e.g., sit to stand) Light physical activity • 1/8 studies @Sig OE • 3/8 meaningful SR within group |
Direct habit indicators • 4/8 studies identifying significant change 1/8 with @Sig OE. Habit mechanisms • 7/8 with supportive mechanisms • 5/8 evidence of adherence • 4/8 routine establishment • 4/8 environmental cues • 3/8 prompts • 4/8 intention to continue post intervention |
• No studies reported quality of life outcomes | • 1/8 (1/1) provided qualitative evidence of reduced knee and hip stiffness, perceived reduction in joint discomfort • 7/8 did not measure pain |
• 1/8 identified significant improvement within study • 5/8 identified qualitative evidence of improvements • Mechanisms included: exercise being manageable and empowering, functional gains meant more confidence, improved safety or less threat, sense of achievement, actives that are achievable, improved capability of daily tasks |
Mood • 3/8 (3/6) with @Sig SR • 2/8 with sustained effects • 1/8 with limited benefit • 4/8 with qualitative evidence of improved emotional stability, better mood with exercise, better emotional regulation, • enjoyment following session • 2/8 did not report on mood Energy or Fatigue • Direct measurement not identified • 5/8 identified support from indirect measures e.g., sit to stand improvements or step count |
| Inactive adults |
Reduce sitting and sedentary behaviour • 4/8 of SR evidence • 1/8 no between group difference Light physical activity • 1/8 studies @Sig OE • 4/8 SR meaningful within group evidence • |
Direct habit indicators • 5/8 studies with positive/supportive change from SR. • 5/8 of explicit sitting to movement substitution from SR • 3/8 supportive evidence around automaticity from SR Habit formation mechanisms • 7/8 with supportive mechanism identified • 6/8 adherence • 5/8 routine scheduling • 5/8 behavioural substitution • 4/8 prompts or technology reminders • 4/8 environmental or contextual cues • 4/8 low effort burden • 3/8 intension to continue |
• No studies reported quality of life outcomes | • 2/8 (2/2) pain discussed as a barrier • 6/8 did not measure pain |
• 1/8 (1/1) provided qualitative evidence • 4/8 (4/7) identified qualitative evidence of improvements • Mechanisms identified: reduce fear of injury, physical activity now considered achievable, improved perception of capability, snack are easy and flexible, change in understanding of what counts as exercise, ability to adhere to a high level, ease of integrating movement into routines, repeated use of familiar environment • 1/8 did not measure |
Mood • 1/8 (1/4) @Sig SR • 3/8 identified qualitative improvements around feeling well, improved mood and feeling better because of intervention or just after • 4/8 did not measure Energy or Fatigue • 2/8 indirect @Sig SR • 5/8 qualitative reports of positive energy and less fatigue during tasks and when exercising and more energy after exercise |
| Healthy adults |
Reduce sitting and sedentary behaviour • 3/8 positive significant evidence (2/8 @Sig with OE) Light physical activity • 2/5 with between group evidence (1/5 with OE @Sig) • 2/5 SR meaningful within group change |
Direct habit indicators • 1/5 with @Sig OE Habit formation mechanism • 4/5 with supportive mechanism identified • 3/5 prompts or technology reminders • 3/5 behavioural substitution • 2/5 environmental restructuring • 2/5 anchoring routines and context • 2/5 self-monitoring or feedback |
• No studies reported quality of life outcomes | • 1/5 (1/2) with @Sig SR • 1/5 identified @Sig OE • 3/5 did not measure pain |
• 1/5 @Sig SR. • 1/5 improvements in SR • 1/5 with mechanisms identifying better awareness and knowledge and attitudes towards physical activity • 2/5 did not measure confidence |
Mood • 2/5 @Sig SR • 1/5 identified @Sig preservation of cognitive stage • 2/5 did not measure mood Energy or Fatigue • 3/5 @Sig SR via indirect measure e.g., improvement in RPE during exercise • 1/5 reduced discomfort • 1/5 did not measure fatigue |
| PT | Context | Mechanism | Outcome |
| 1 |
|
|
Willingness to initiate movement
|
| 2 |
|
Mastery experiences from completion, not performance
|
|
| 3 |
|
|
|
| 4 |
|
|
|
| 5 |
|
|
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




