Submitted:
13 April 2026
Posted:
14 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Sampling Procedure
2.3. Data Collection Procedures
2.4. Confidentiality and Data Security
2.5. Measures
2.5.1. Sociodemographic Questionnaire
2.5.2. SF-36 Health Survey
2.5.3. Patient Health Questionnaire-9 (PHQ-9)
2.6. Statistical Analysis
3. Results
3.1. Sample Characteristics
3.2. Depressive Symptoms
3.3. Health-Related Quality of Life
3.4. Preliminary Analyses
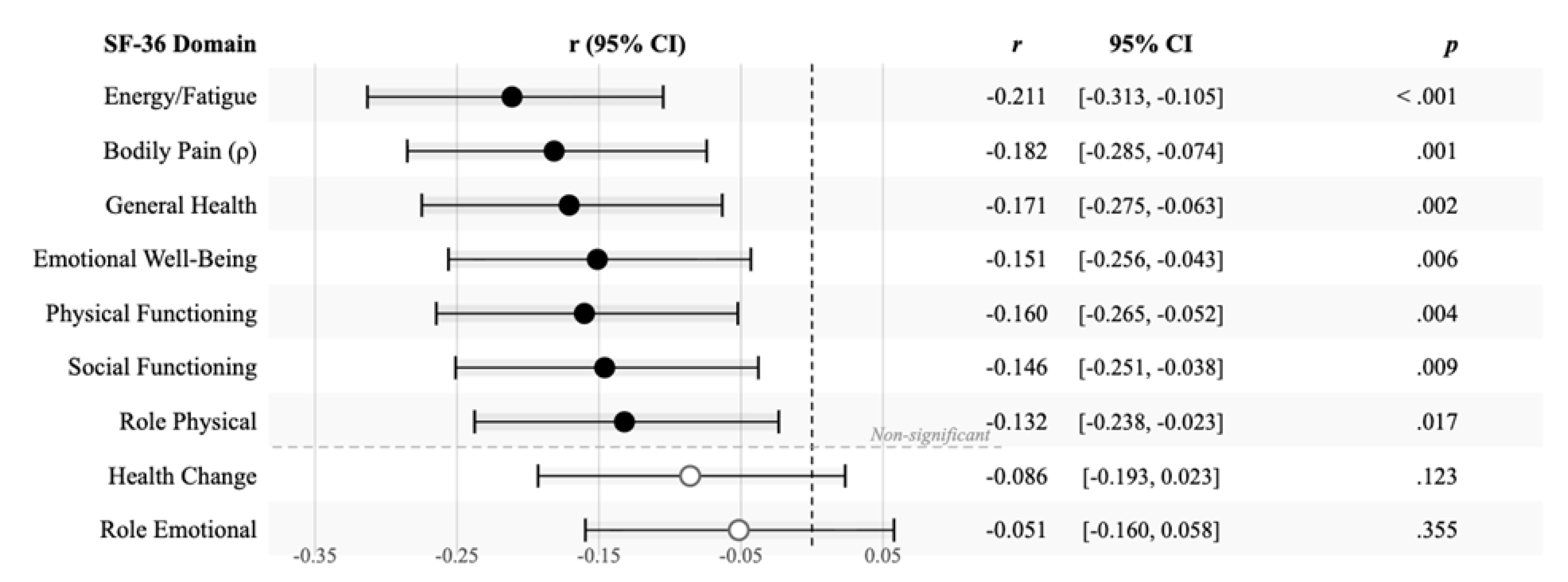
3.5. Associations Between Depressive Symptoms and Quality of Life
3.6. Hierarchical Linear Regression: Predictors of Depressive Symptom Severity
3.7. Binary Logistic Regression: Predictors of Clinically Significant Depression
3.8. Convergence Across Regression Approaches
4. Discussion
4.1. Prevalence and Severity of Depressive Symptoms
4.2. Gender Differences
4.3. Quality of Life: Physical Versus Psychosocial Divergence
4.4. Depression and Quality of Life: Energy/Fatigue as the Central Link
4.5. Trauma, Safety Threats, and the Primacy of Current Stressors
4.6. Education, Employment, Social Support, and Family Context
4.7. The Self-Rated Health Paradox
4.8. Clinical and Public Health Implications
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| HQoL PHQ-9 |
Health Related Quality of Life Patient Health Questionnaire-9 |
| WHO | World Health Organization |
| UNHCR | United Nations High Commissioner for Refugees |
| PTSD | Post-Traumatic Stress Disorder |
| QoL | Quality of life |
References
- United Nations High Commissioner for Refugees (UNHCR). Convention and Protocol Relating to the Status of Refugees; UNHCR: Geneva, Switzerland, 2010; Available online: https://www.unhcr.org/3b66c2aa10 (accessed on 25 April 2024).
- World mental health report: transforming mental health for all Licence: CC BY-NC-SA 3.0 IGO. World Health Organization: Geneva, 2022; Available online: https://www.who.int/teams/mental-health-and-substance-use/world-mental-health-report (accessed on 25 April 2026).
- United Nations High Commissioner for Refugees (UNHCR). Global Trends: Forced Displacement 2022. UNHCR, 2022. Available online: https://www.unhcr.org/global-trends-report-2022 (accessed on 25 April 2024).
- UN Refugees. Available online: https://www.unrefugees.com (accessed on 25 April 2024).
- Jankovic, J.A.; Trivuncic, B.; Durasinovic, V. The demographic picture, assessment of legal status and needs, and traumatic experiences of refugees in transit through Serbia; IAN: Belgrade, Serbia, 2015. [Google Scholar]
- AIDA. Asylum Information Database: Country Report Serbia; European Council on Refugees and Exiles, 2016. [Google Scholar]
- Muhieddine, D.; Farhat, T.; Ibrahim, S.; Al-Yahya, M.; Al-Sheyab, N.; Zeng, W.; Halasa-Rappel, Y.; Jarawan, E.; Diab, J.L.; Hashoush, M.; et al. World Bank Consortium: The Big Questions in Forced Displacement and Health—Jordan Country Report, 2022. Available online: https://documents1.worldbank.org (accessed on 25 April 2024).
- Hollifield, M.; Warner, T.D.; Krakow, B.; Westermeyer, J. Mental health effects of stress over the life span of refugees. J. Clin. Med. 2018, 7, 25. [Google Scholar] [CrossRef]
- Sengoelge, M.; Nissen, A.; Solberg, Ø. Post-migration stressors and health-related quality of life in refugees from Syria resettled in Sweden. Int. J. Environ. Res. Public Health 2022, 19, Article number. [Google Scholar] [CrossRef]
- Khaled, S.M.; Gray, R. Depression in migrant workers and nationals of Qatar: An exploratory cross-cultural study. Int. J. Soc. Psychiatry 2019, 65, 354–367. [Google Scholar] [CrossRef]
- Mucci, N.; Traversini, V.; Giorgi, G.; Tommasi, E.; De Sio, S.; Arcangeli, G. Migrant workers and psychological health: A systematic review. Sustainability 2020, 12, 1–28. [Google Scholar] [CrossRef]
- Lindert, J.; Ehrenstein, O.S.V.; Priebe, S.; Mielck, A.; Brähler, E. Depression and anxiety in labor migrants and refugees: A systematic review and meta-analysis. Soc. Sci. Med. 2009, 69, 246–257. [Google Scholar] [CrossRef] [PubMed]
- Georgiadou, E.; Zbidat, A.; Schmitt, G.; Erim, Y. Prevalence of mental distress among Syrian refugees in Germany. Front. Psychiatry 2018, 9, 393. [Google Scholar] [CrossRef]
- Acarturk, C.; Cetinkaya, M.; Senay, I.; Gulen, B.; Aker, T.; Hinton, D. Prevalence and predictors of PTSD and depression among Syrian refugees. J. Nerv. Ment. Dis. 2018, 206, 40–45. [Google Scholar] [CrossRef]
- Naja, W.J.; Aoun, M.P.; El Khoury, E.L.; Abdallah, F.J.B.; Haddad, R.S. Prevalence of depression in Syrian refugees and the influence of religiosity. Compr. Psychiatry 2016, 68, 78–85. [Google Scholar] [CrossRef]
- Bogic, M.; Ajdukovic, D.; Bremner, S.; Franciskovic, T.; Galeazzi, G.M.; Kucukalic, A.; Lecic-Tosevski, D.; Morina, N.; Popovski, M.; Schützwohl, M.; et al. Factors associated with mental disorders in long-settled war refugees. Br. J. Psychiatry 2012, 200, 216–223. [Google Scholar] [CrossRef]
- Porter, M.; Haslam, N. Predisplacement and postdisplacement factors associated with mental health of refugees. JAMA 2005, 294, 602–612. [Google Scholar] [CrossRef] [PubMed]
- Hosseini, A.; Kakuma, R.; Ghazinour, M.; Davern, M.; Evans, W.P.; Minas, H. Migration experience, resilience and depression: A study of Iranian immigrants living in Australia. Int. J. Cult. Ment. Health 2017, 10, 108–120. [Google Scholar] [CrossRef]
- Yao, X.; Yang, Y.; Lu, D.; Chen, S.; Liu, T.; Qi, L.; Shang, S.; Gan, Y.; Wang, Y.; Bao, X.; et al. Central symptoms of depression and their associations with health-related quality of life among migrant older adults with children: A network analysis. Geriatr. Nurs. 2025, 63, 415–421. [Google Scholar] [CrossRef]
- van der Boor, C.F.; Amos, R.; Nevitt, S.; Dowrick, C.; White, R.G. Systematic review of factors associated with quality of life of asylum seekers and refugees in high-income countries. Confl. Health 2020, 14, 48. [Google Scholar] [CrossRef]
- Matanov, A.; Giacco, D.; Bogic, M.; Ajdukovic, D.; Franciskovic, T.; Galeazzi, G.M.; Kucukalic, A.; Lecic-Tosevski, D.; Morina, N.; Popovski, M.; et al. Subjective quality of life in war-affected populations. BMC Public Health 2013, 13, 624. [Google Scholar] [CrossRef] [PubMed]
- Al Masri, F.; Müller, M.; Nebl, J.; Greupner, T.; Hahn, A.; Straka, D. Quality of life among Syrian refugees in Germany: A cross-sectional pilot study. Arch. Public Health 2021, 79, 213. [Google Scholar] [CrossRef] [PubMed]
- Hynie, M. The social determinants of refugee mental health in the post-migration context: A critical review. Can. J. Psychiatry 2018, 63, 297–303. [Google Scholar] [CrossRef] [PubMed]
- Maharaj, V.; Tomita, A.; Thela, L.; Mhlongo, M.; Burns, J.K. Food insecurity and risk of depression among refugees and immigrants in South Africa. J. Immigr. Minor. Health 2017, 19, 631–637. [Google Scholar] [CrossRef]
- Spiritus-Beerden, E.; Verelst, A.; Devlieger, I.; Langer Primdahl, N.; Botelho Guedes, F.; Chiarenza, A.; De Maesschalck, S.; Durbeej, N.; Garrido, R.; Gaspar de Matos, M.; et al. Mental health of refugees and migrants during the COVID-19 pandemic: The role of experienced discrimination and daily stressors. Int. J. Environ. Res. Public Health 2021, 18, 6354. [Google Scholar] [CrossRef]
- Hombrados-Mendieta, I.; Millán-Franco, M.; Gómez-Jacinto, L.; Gonzalez-Castro, F.; Martos-Méndez, M.J.; García-Cid, A. Positive influences of social support on sense of community, life satisfaction and the health of immigrants in Spain. Front. Psychol. 2019, 10, 2555. [Google Scholar] [CrossRef]
- Harvard Program in Refugee Trauma. Harvard Trauma Questionnaire (HTQ). Available online: https://hprt-cambridge.org/screening/harvard-trauma-questionnaire/ (accessed on 25 April 2024).
- Ware, J.E.; Snow, K.K.; Kosinski, M.; Gandek, B. SF-36 Health Survey Manual and Interpretation Guide; Nimrod Press: Boston, MA, USA, 1993. [Google Scholar]
- RAND Corporation. 36-Item Short Form Survey (SF-36). Available online: https://www.rand.org/health-care/surveys_tools/mos/36-item-short-form.html (accessed on 25 April 2024).
- Patient Health Questionnaire (PHQ-9). Available online: https://patient.info/doctor/patient-health-questionnaire-phq-9 (accessed on 25 April 2024).
- AboAbat, A.; Qannam, H.; Bjorner, J.B.; Al-Tannir, M. Psychometric validation of a Saudi Arabian version of the SF-36v2 health survey and norm data for Saudi Arabia. J. Patient Rep. Outcomes 2020, 4, 67. [Google Scholar] [CrossRef]
- Patient Health Questionnaire (PHQ-9). Available online: https://patient.info/doctor/patient-health-questionnaire-phq-9 (accessed on 25 April 2024).
- Sawaya, H.; Atoui, M.; Hamadeh, A.; Zeinoun, P.; Nahas, Z. Adaptation and initial validation of the Patient Health Questionnaire-9 (PHQ-9) and the Generalized Anxiety Disorder-7 (GAD-7) in an Arabic-speaking Lebanese psychiatric outpatient sample. Psychiatry Res. 2016, 239, 245–252. [Google Scholar] [CrossRef]
- Bedaso, A.; Duko, B. Epidemiology of depression among displaced people: A systematic review and meta-analysis. Psychiatry Res. 2022, 311, 114493. [Google Scholar] [CrossRef]
- Verhülsdonk, I.; Shahab, M.; Molendijk, M. Prevalence of psychiatric disorders among refugees and migrants in immigration detention: A systematic review with meta-analysis. BJPsych Open 2021, 7, e204. [Google Scholar] [CrossRef]
- Foo, S.Q.; Tam, W.W.; Ho, C.S.; Tran, B.X.; Nguyen, L.H.; McIntyre, R.S.; Ho, R.C. Prevalence of depression among migrants: A systematic review and meta-analysis. Int. J. Environ. Res. Public Health 2018, 15, 1986. [Google Scholar] [CrossRef]
- Blackmore, R.; Boyle, J.A.; Fazel, M.; Ranasinha, S.; Gray, K.M.; Fitzgerald, G.; Misso, M.; Gibson-Helm, M. The prevalence of mental illness in refugees and asylum seekers: A systematic review and meta-analysis. PLoS Med. 2020, 17, e1003337. [Google Scholar] [CrossRef]
- Naal, H.; Nabulsi, D.; El Arnaout, N.; Abdouni, L.; Dimassi, H.; Harb, R.; Saleh, S. Prevalence of depression symptoms and associated sociodemographic and clinical correlates among Syrian refugees in Lebanon. BMC Public Health 2021, 21, 217. [Google Scholar] [CrossRef]
- Mollica, R.F.; McInnes, K.; Poole, C.; Tor, S. Dose-effect relationships of trauma to symptoms of depression and post-traumatic stress disorder among Cambodian survivors of mass violence. Br. J. Psychiatry 1998, 173, 482–488. [Google Scholar] [CrossRef] [PubMed]
- Fenta, H.; Hyman, I.; Noh, S. Determinants of depression among Ethiopian immigrants and refugees in Toronto. J. Nerv. Ment. Dis. 2004, 192, 363–372. [Google Scholar] [CrossRef] [PubMed]
- Awang, S.; Mohamad, S.; Awaluddin, S. Humanitarian disaster: Mental health disorders at primary healthcare clinic. Disaster Emerg. Med. J. 2022, 7, 1–10. [Google Scholar] [CrossRef]
- Steel, Z.; Chey, T.; Silove, D.; Marnane, C.; Bryant, R.A.; van Ommeren, M. Association of torture and other potentially traumatic events with mental health outcomes among populations exposed to mass conflict and displacement: A systematic review and meta-analysis. JAMA 2009, 302, 537–549. [Google Scholar] [CrossRef]
- Poole, D.N.; Hedt-Gauthier, B.; Liao, S.; Raymond, N.; Bärnighausen, T. Major depressive disorder prevalence and risk factors among Syrian asylum seekers in Greece. BMC Public Health 2018, 18, 908. [Google Scholar] [CrossRef]
- Reile, R.; Saavaste, J.; Opikova, G.; Lai, T.; Haagsma, J. Health-Related Quality of Life Among Ukrainian War Refugees Compared to the General Population in Estonia. Int J Public Health 2026, 71, 1608807. [Google Scholar] [CrossRef]
- Essex, R.; Govintharjah, P.; Issa, R.; Kalocsányiová, E.; Lakika, D.; Markowski, M.; Smith, J.; Thompson, T. Health-related quality of life amongst refugees: A meta-analysis of studies using the SF-36. J. Immigr. Minor. Health 2024, 26, 925–935. [Google Scholar] [CrossRef] [PubMed]
- Laban, C.J.; Komproe, I.H.; Gernaat, H.B.P.E.; de Jong, J.T.V.M. The impact of a long asylum procedure on quality of life, disability and physical health in Iraqi asylum seekers in the Netherlands. Soc. Psychiatry Psychiatr. Epidemiol. 2008, 43, 507–515. [Google Scholar] [CrossRef] [PubMed]
- Buhmann, C.; Mortensen, E.L.; Lundstrøm, S.; Ryberg, J.; Nordentoft, M.; Ekstrøm, M. Symptoms, quality of life and level of functioning of traumatized refugees at a psychiatric trauma clinic in Copenhagen. Torture 2014, 24, 25–39. [Google Scholar] [CrossRef]
- Strømme, E.M.; Igland, J.; Haj-Younes, J.; Kumar, B.N.; Fadnes, L.T.; Hasha, W.; Diaz, E. Chronic pain and mental health problems among Syrian refugees: Associations, predictors and use of medication over time: A prospective cohort study. BMJ Open 2021, 11, e046454. [Google Scholar] [CrossRef]
- Yao, C.; Zhang, Y.; Lu, P.; Xiao, B.; Sun, P.; Tao, J.; Cheng, Y.; Kong, L.; Xu, D.; Fang, M. Exploring the bidirectional relationship between pain and mental disorders: A comprehensive Mendelian randomization study. J. Headache Pain 2023, 24, 82. [Google Scholar] [CrossRef]
- Kirmayer, L.J. Cultural variations in the clinical presentation of depression and anxiety: Implications for diagnosis and treatment. J. Clin. Psychiatry 2001. [Google Scholar]
- Powell, T.M.; Shin, O.J.; Li, S.J.; Hsiao, Y. Post-traumatic stress, social and physical health: A mediation and moderation analysis of Syrian refugees and Jordanians in a border community. PLoS ONE 2020, 15, e0241036. [Google Scholar] [CrossRef]
- Bogic, M.; Njoku, A.; Priebe, S. Long-term mental health of war refugees: A systematic literature review. BMC Int. Health Hum. Rights 2015, 15, 29. [Google Scholar] [CrossRef]
- Mässing, A.; Cardeña, E. The relation between postmigration stressors and trauma treatment outcomes: A scoping review. Eur. J. Psychotraumatol. 2025, 16, 2570929. [Google Scholar] [CrossRef] [PubMed]
- Kemna, S.; Bringmann, M.; Karnouk, C.; Hoell, A.; Tschorn, M.; Kamp-Becker, I.; Padberg, F.; Übleis, A.; Hasan, A.; Falkai, P.; et al. Predictors of symptom change in the mental health of refugees and asylum seekers (MEHIRA) study examining the effects of a stepped and collaborative care model – A multicentered rater-blinded randomized controlled trial. J Affect Disor. 2025, 370, 45–53. [Google Scholar] [CrossRef]
- Nemani, A.; Kananian, S.; Starck, A.; Kip, A.; Churbaji, D.; Morina, N.; Nater-Mewes, R.; Weise, C.; Preiß, H.; Ehring, T.; et al. Carrying what came after: Post-migration difficulties and depression among refugees and asylum seekers. Confl. Health 2025, 19, 86. [Google Scholar] [CrossRef]
- Handiso, D.W.; Paul, E.; Boyle, J.; Shawyer, F.; Mengistu, Y.; Enticott, J. Course of depression and anxiety among refugees and asylum seekers: A systematic review and meta-analysis of longitudinal studies. Int. J. Ment. Health Addict. 2024. [Google Scholar] [CrossRef]
- Anbesaw, T.; Kassa, M.A.; Yimam, W.; Kassaw, A.B.; Belete, M.; Abera, A.; Abebe, G.; Yimer, N.; Melkam, M.; Ayano, G. Factors associated with depression among war-affected populations in Northeast Ethiopia. BMC Psychiatry 2024, 24, 376. [Google Scholar] [CrossRef] [PubMed]
- AbuZarifa, M.; Zaqout, K.; AlHabbash, S.; AbuDraz, A.; AbuZarifa, M.; Zimmo, M. Prevalence and risk factors of depression among individuals affected by the Gaza war in 2024: A cross-sectional study. Middle East Curr. Psychiatry 2025, 32, 51. [Google Scholar] [CrossRef]
- Lai, H.; Due, C.; Ziersch, A. The relationship between employment and health for people from refugee and asylum-seeking backgrounds: A systematic review of quantitative studies. SSM Popul. Health 2022, 18, 101075. [Google Scholar] [CrossRef]
- McKee-Ryan, F.M.; Song, Z.; Wanberg, C.R.; Kinicki, A.J. Psychological and physical well-being during unemployment: A meta-analytic study. J. Appl. Psychol. 2005, 90, 53–76. [Google Scholar] [CrossRef]
- Paul, K.I.; Moser, K. Unemployment impairs mental health: Meta-analyses. J. Vocat. Behav. 2009, 74, 264–282. [Google Scholar] [CrossRef]
- Schweitzer, R.; Melville, F.; Steel, Z.; Lacherez, P. Trauma, post-migration living difficulties and social support as predictors of psychological adjustment in resettled Sudanese refugees. Aust. N. Z. J. Psychiatry 2006, 40, 179–187. [Google Scholar] [CrossRef]
- Li, S.S.Y.; Liddell, B.J.; Nickerson, A. The relationship between post-migration stress and psychological disorders in refugees and asylum seekers. Curr. Psychiatry Rep. 2020, 22, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Pozuelo, J.R.; Bradenbrink, R.; Stierna, M.F.; Sterck, O. Depression, violence and socioeconomic outcomes among refugees in East Africa: Evidence from a multicountry representative survey. BMJ Ment. Health 2023, 26, e300773. [Google Scholar] [CrossRef] [PubMed]
- Edinoff, A.N.; Nix, C.A.; Hollier, J.; Sagrera, C.E.; Delacroix, B.M.; Abubakar, T.; Cornett, E.M.; Kaye, A.M.; Kaye, A.D. Benzodiazepines: Uses, dangers and clinical considerations. Neurol. Int. 2021, 13, 594–607. [Google Scholar] [CrossRef]
- Muradyan, D.; Giloyan, A.; Harutyunyan, T.; Petrosyan, V. Health-related quality of life and associated factors among older refugees from Nagorno-Karabakh residing in Kotayk province of Armenia. Front. Public Health 2026, 13, 1718203. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | n (%) or M ± SD |
|---|---|
| Demographics | |
| Gender | |
| Male | 285 (88) |
| Female | 39 (12) |
| Age (years) | 30.02 ± 7.34 |
| Relationship status [n = 323] | |
| Single | 132 (40.9) |
| In a relationship, living separately | 49 (15.2) |
| Cohabiting | 35 (10.8) |
| Married | 75 (23.2) |
| Divorced | 21 (6.5) |
| Widowed | 3 (0.9) |
| Other | 8 (2.5) |
| Children | |
| No | 141 (43.5) |
| Yes | 183 (56.5) |
| Education level | |
| No school/incomplete primary | 43 (13.3) |
| Primary school | 88 (27.2) |
| Vocational | 37 (11.4) |
| Secondary school | 115 (35.5) |
| Higher education | 32 (9.9) |
| University/postgraduate | 9 (2.8) |
| Current employment | |
| Unemployed | 312 (96.3) |
| Temporary | 7 (2.2) |
| Permanent | 5 (1.5) |
| Migration characteristics | |
| Country of origin | |
| Pakistan | 22 (6.8) |
| Afghanistan | 13 (4) |
| Syria | 158 (48.8) |
| Iran | 23 (7.1) |
| Iraq | 52 (16) |
| Other | 56 (17.3) |
| Duration of stay in Serbia | |
| Up to 3 months | 237 (73.1) |
| 3–6 months | 67 (20.7) |
| 6–12 months | 12 (3.7) |
| More than 1 year | 8 (2.5) |
| Living arrangement in Serbia [n = 323] | |
| Alone | 234 (72.4) |
| With parents | 4 (1.2) |
| With spouse | 11 (3.4) |
| With children only | 17 (5.3) |
| With family (spouse + children) | 19 (5.9) |
| With friends | 37 (11.5) |
| Other | 1 (0.3) |
| Reasons for migration (multiple response) | |
| Personal safety threats | 201 (62) |
| Poor family situation | 168 (51.9) |
| Employment | 95 (29.3) |
| Education | 26 (8) |
| Family reunion | 22 (6.8) |
| Marriage/partnership | 4 (1.2) |
| Natural disaster | 1 (0.3) |
| Other | 8 (2.5) |
| Nutrition and lifestyle | |
| Smoking status | |
| Daily smoker (≥1 cigarette/day) | 130 (40.1) |
| Occasional smoker | 75 (23.1) |
| Former smoker | 45 (13.9) |
| Non-smoker | 74 (22.8) |
| Health status | |
| Any chronic illness | 71 (21.9) |
| Self-rated physical health (1–10) | 6.67 ± 2.4 [n = 323] |
| Self-rated mental health (1–10) | 7.19 ± 2.29 |
| Stressful/traumatic experiences (multiple response) | |
| Exposure to torture | 167 (51.5) |
| Death threats | 82 (25.3) |
| Lack of food and water | 76 (23.5) |
| Forced separation from family | 74 (22.8) |
| Prison stay | 37 (11.4) |
| Participation in war | 33 (10.2) |
| Kidnapped | 19 (5.9) |
| Political persecution | 14 (4.3) |
| Murder of a close person | 2 (0.6) |
| Other traumatic experience | 17 (5.2) |
| Treatment since arriving in Serbia (multiple response) | |
| Treated with kindness | 211 (65.1) |
| Verbally insulted | 38 (11.7) |
| Treated unfairly by police | 27 (8.3) |
| Treated differently due to origin | 24 (7.4) |
| Shunned by community | 20 (6.2) |
| Physically attacked | 10 (3.1) |
| Called names due to origin/religion | 6 (1.9) |
| Sources of support (multiple response) | |
| RS institutions for migrant issues | 140 (43.2) |
| Migrant friends | 75 (23.1) |
| Lonely/without support | 75 (23.1) |
| Family | 36 (11.1) |
| Friends made in Serbia | 35 (10.8) |
| Surroundings (warm/helpful) | 21 (6.5) |
| Non-governmental organizations | 15 (4.6) |
| Mental health service use | |
| Current sedative use [n = 323] | |
| No | 273 (84.5) |
| Occasionally, as needed | 31 (9.6) |
| Yes, daily | 15 (4.6) |
| Don't know | 4 (1.2) |
| Ever used psychiatric/psychological help [n = 319] | |
| No, never | 242 (75.9) |
| Sometimes | 56 (17.6) |
| Often | 21 (6.6) |
| Currently need professional help [n = 320] | |
| No, I feel fine | 167 (52.2) |
| No, I can cope on my own | 63 (19.7) |
| Not sure | 22 (6.9) |
| Yes, but it is not available | 46 (14.4) |
| Yes, but I don't use it | 22 (6.9) |
| Panel A: Score Distribution and Severity | |||
| Measure | n | % / M ± SD | Range |
| PHQ-9 total score | 324 | 8.67 ± 5.91 | 0–25 |
| Severity classification | |||
| No symptoms (0) | 31 | 9.6 | |
| Minimal depression (1–4) | 59 | 18.2 | |
| Mild depression (5–9) | 100 | 30.9 | |
| Moderate depression (10–14) | 78 | 24.1 | |
| Moderately severe depression (15–19) | 40 | 12.3 | |
| Severe depression (20–27) | 16 | 4.9 | |
| Clinically significant (PHQ-9 ≥ 10) | 134 | 41.4 | |
| Panel B: Item Analysis (Cronbach's α = 0.875 [95% CI: 0.853, 0.894]) | |||
| Item | M ± SD | r(item-total) | α if deleted |
| 1. Diminished interest or pleasure | 1.11 ± 0.92 | 0.547 | 0.867 |
| 2. Feeling hopeless or empty | 1.19 ± 0.98 | 0.706 | 0.853 |
| 3. Sleep problems | 1.1 ± 0.97 | 0.666 | 0.856 |
| 4. Fatigue or low energy | 0.97 ± 0.99 | 0.702 | 0.853 |
| 5. Appetite changes | 0.95 ± 0.98 | 0.654 | 0.858 |
| 6. Negative self-perception | 1.2 ± 1 | 0.638 | 0.859 |
| 7. Difficulty concentrating | 1.17 ± 1.01 | 0.570 | 0.866 |
| 8. Psychomotor changes | 0.57 ± 0.74 | 0.624 | 0.862 |
| 9. Suicidal ideation | 0.4 ± 0.7 | 0.424 | 0.875 |
| Domain | M | SD | Mdn | IQR | Floor % | Ceil % | α | 95% CI |
| Physical Func. | 75.5 | 22.4 | 85.0 | 60–95 | 0.0 | 16.4 | 0.846 | [0.82, 0.87] |
| Role Physical | 64.6 | 33.8 | 75.0 | 50–100 | 11.4 | 34.6 | 0.673 | [0.61, 0.73] |
| Role Emotional | 53.9 | 38.8 | 66.7 | 33–100 | 22.2 | 33.3 | 0.671 | [0.60, 0.73] |
| Bodily Pain | 80.5 | 24.5 | 90.0 | 65–100 | 0.9 | 48.8 | 0.748 | [0.69, 0.80] |
| General Health | 54.6 | 16.2 | 55.0 | 45–65 | 0.0 | 0.3 | 0.494 | [0.40, 0.58] |
| Vitality | 54.6 | 17.2 | 55.0 | 45–65 | 0.0 | 1.9 | 0.447 | [0.34, 0.54] |
| Social Func. | 62.0 | 25.6 | 62.5 | 38–88 | 2.5 | 9.3 | 0.409 | [0.26, 0.53] |
| Mental Health | 53.6 | 16.9 | 56.0 | 40–64 | 0.0 | 0.0 | 0.552 | [0.47, 0.63] |
| Health Change | 57.2 | 26.3 | 50.0 | 50–75 | 3.1 | 15.1 | — | — |
| Panel A: Hierarchical Block Summary | ||||||
| Block | Variables | R² | ΔR² | F-change | p | |
| 1. Demographics | 1 | 0.011 | 0.011 | 3.53 | 0.061 | |
| 2. Migration/Trauma | 5 | 0.075 | 0.064 | 4.22 | 0.001 | |
| 3. Psychosocial | 2 | 0.115 | 0.040 | 6.90 | 0.001 | |
| 4. SF-36 QoL | 2 | 0.178 | 0.063 | 11.65 | < .001 | |
| Panel B: Final Model Coefficients | ||||||
| Variable | B | SE | β | t | p | |
| Demographics | ||||||
| Education level | -0.586 | 0.233 | -0.133 | -2.52 | 0.012 | * |
| Migration/Trauma | ||||||
| Personal safety threats | 2.070 | 0.671 | 0.171 | 3.08 | 0.002 | ** |
| Death threats | 1.152 | 0.717 | 0.086 | 1.61 | 0.109 | |
| Poor family situation | 1.267 | 0.647 | 0.108 | 1.96 | 0.051 | † |
| Lack of food/water | 1.655 | 0.724 | 0.121 | 2.29 | 0.023 | * |
| War participation | -2.361 | 1.006 | -0.123 | -2.35 | 0.020 | * |
| Psychosocial | ||||||
| Sedative use | 2.428 | 0.886 | 0.145 | 2.74 | 0.006 | ** |
| Support: migrant friends | -1.742 | 0.738 | -0.125 | -2.36 | 0.019 | * |
| SF-36 QoL | ||||||
| SF-36 Energy/Fatigue | -0.067 | 0.018 | -0.196 | -3.65 | < .001 | *** |
| SF-36 Bodily Pain | -0.033 | 0.013 | -0.137 | -2.57 | 0.011 | * |
| Overall model: R² = .178, Adjusted R² = .151, F(10, 302) = 6.56, p < .001 | ||||||
| Variable | B | SE | Wald | p | OR | 95% CI | |
|---|---|---|---|---|---|---|---|
| Education level | -0.268 | 0.096 | 7.85 | 0.005 | 0.77 | [0.63, 0.92] | ** |
| Personal safety threats | 0.745 | 0.265 | 7.89 | 0.005 | 2.11 | [1.25, 3.54] | ** |
| Death threats | 0.721 | 0.280 | 6.60 | 0.010 | 2.06 | [1.19, 3.56] | * |
| Support: migrant friends | -0.516 | 0.304 | 2.89 | 0.089 | 0.60 | [0.33, 1.08] | † |
| Support: friends in Serbia | 0.926 | 0.401 | 5.34 | 0.021 | 2.53 | [1.15, 5.54] | * |
| SF-36 Energy/Fatigue | -0.024 | 0.007 | 10.42 | 0.001 | 0.98 | [0.96, 0.99] | ** |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




