Submitted:
10 April 2026
Posted:
13 April 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Literature Review
Data Sources
Method
Simulation Framework
Data Foundation and Assumptions
Historical Population Reconstruction (2000-2019)
Forward Interpolation (2021-2024)
Disability Count Calculation
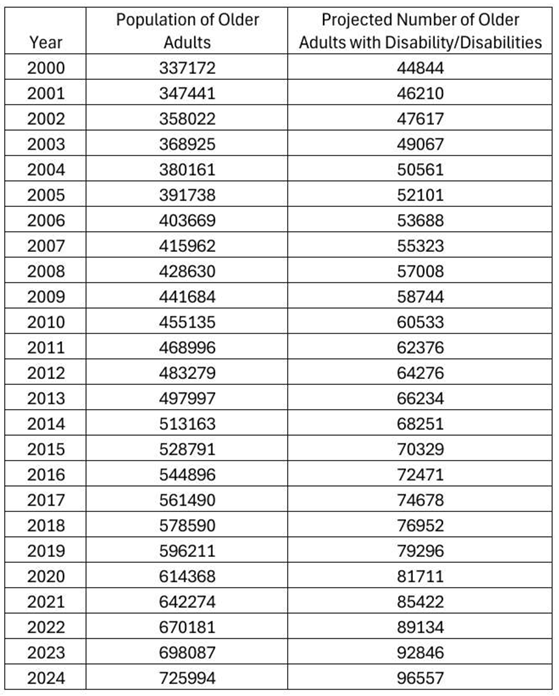 |
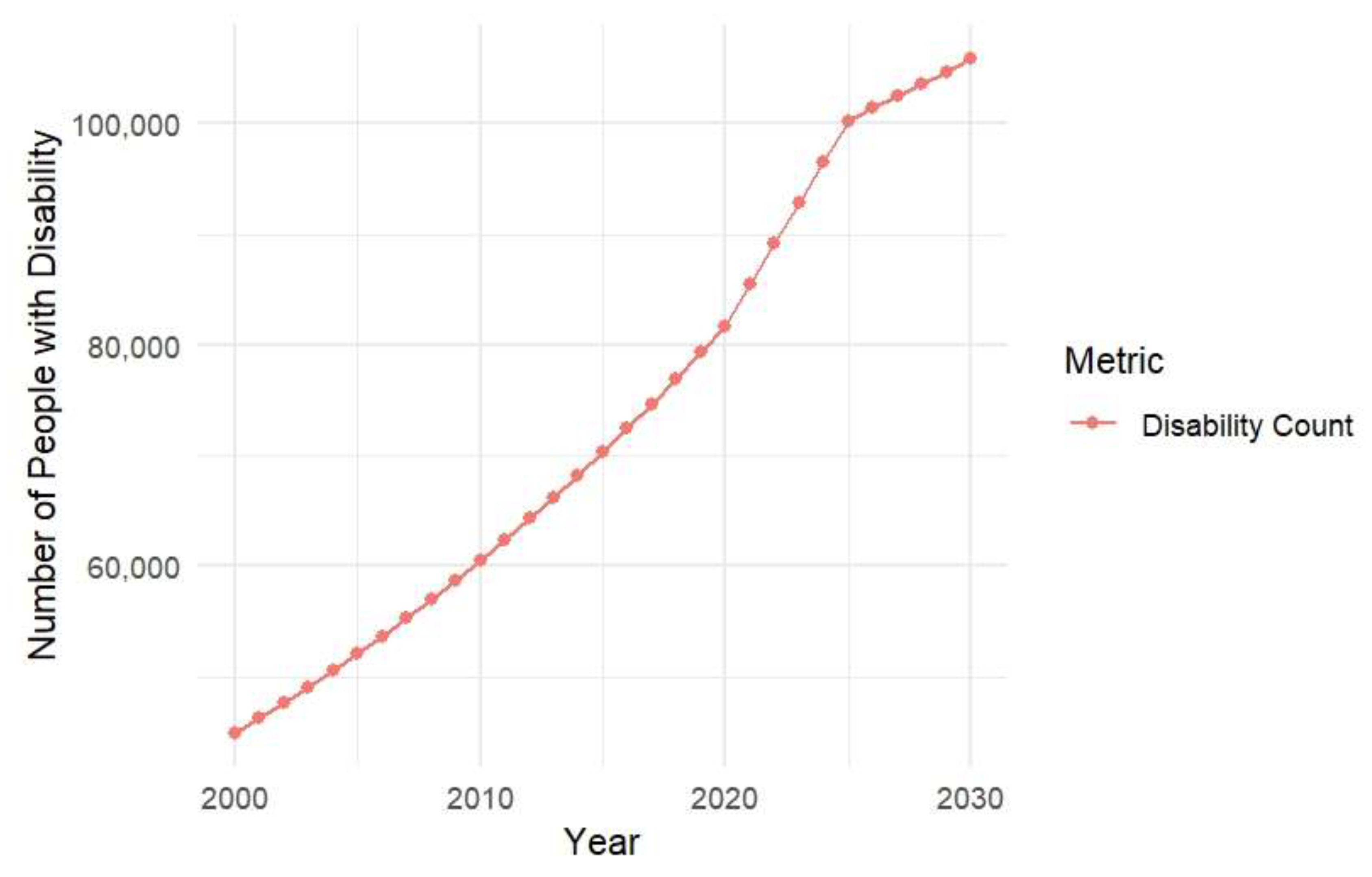
Historical Rate Adjustment
Backward Projection
Results
Method for Forecasting the Number of Older Adults Requiring Assisted Living Arrangements
ARIMA Model Selection and Specification
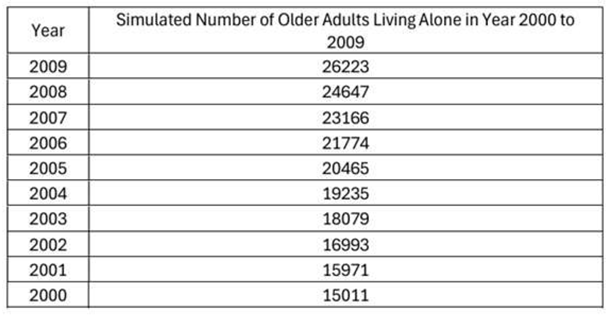 |
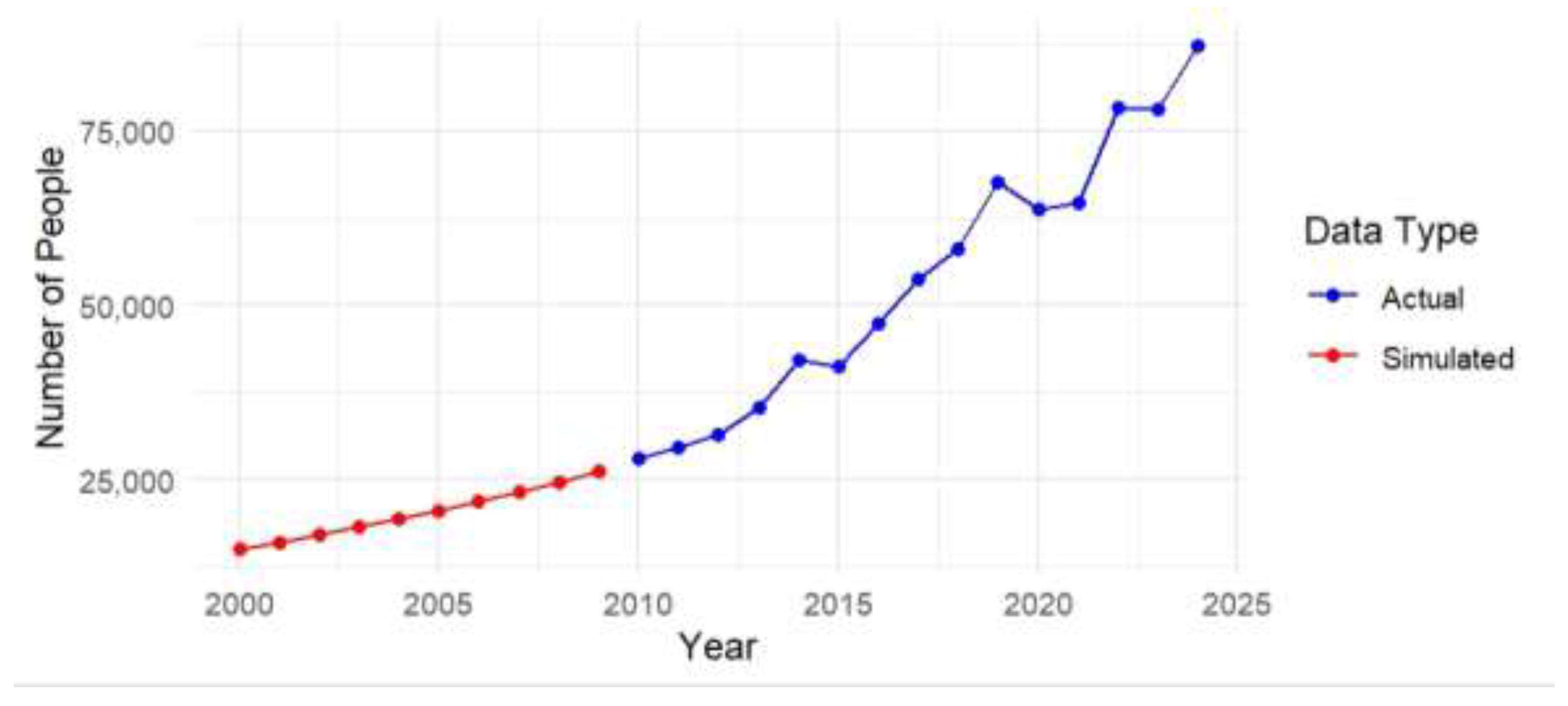
Results
Forecast Results for Number of Older Adults Requiring Assisted Living Arrangements (2025 to 2035)
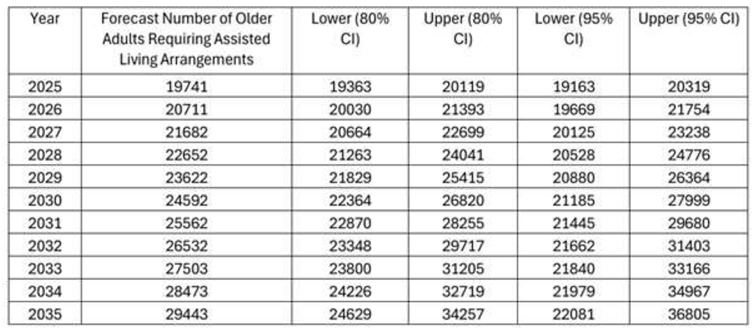 |
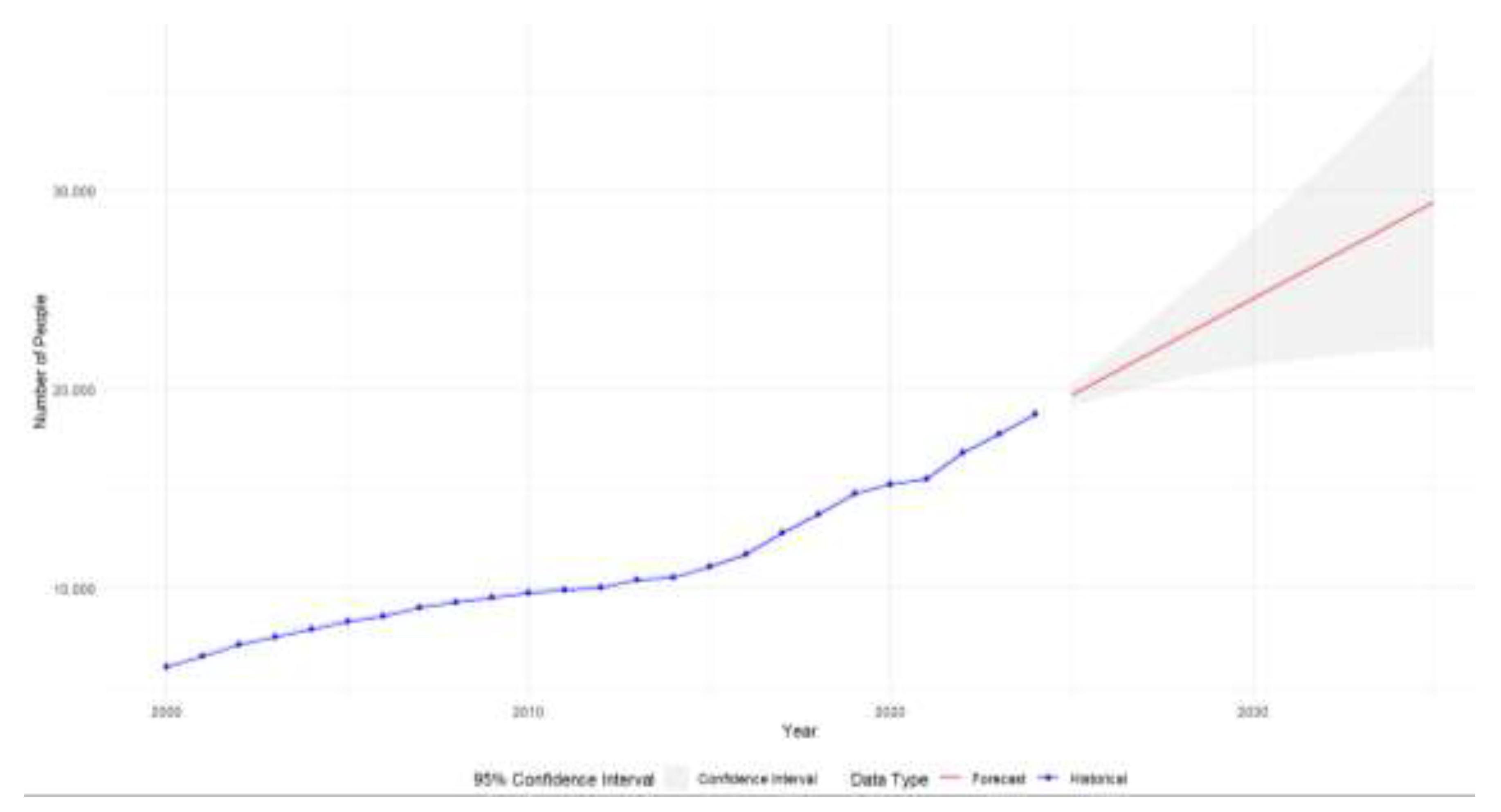
Model Performance
Discussion
Informal Care Availability and Conservative Projections
Underestimation of Structural Shifts
Limitations
Future Research Directions
Conclusion
Funding
Conflicts of Interest
References
- Andrew Kingston, Adelina Comas-Herrera, Carol Jagger for the MODEM project* 2018 Forecasting the care needs of the older population in England over the next 20 years: estimates from the Population Ageing and Care Simulation (PACSim) modelling study. [CrossRef]
- Aranco, N., I; rrarán, P.; Stampini, M. Prevalence of care dependence among older persons in 26 Latin American and the Caribbean countries; Inter-American Bank Development, 2022. [Google Scholar] [CrossRef]
- Brasher, M.S. Filial Norms, Altruism, and Reciprocity: Financial Support to Older Parents in China. Population Ageing 2022, 15, 259–277. [Google Scholar] [CrossRef]
- Duke-NUS Medical School. Filial piety norms: Caught between two worlds. Duke-NUS Medical School. 25 April 2021. Available online: https://www.duke-nus.edu.sg/newshub/media-coverage/filial-piety-norms-caught-between-two-worlds-(straits-times-premium).
- Fuino, M.; Wagner, J. Old-age care prevalence in Switzerland: drivers and future development. Eur. Actuar. J. 2018, 8, 321–362. [Google Scholar] [CrossRef]
- Gong, Jinquan, &; et al. Nowcasting and forecasting the care needs of the older population in China: analysis of data from the China Health and Retirement Longitudinal Study (CHARLS). The Lancet Public Health 2022, 7(Issue 12), e1005–e1013. [Google Scholar] [CrossRef] [PubMed]
- Ożegalska-Łukasik, N. Filial Piety Revisited—Family Care and Filial Obligation in China at the Time of the COVID-19 Pandemic. Social Sciences 2025, 14(12), 696. [Google Scholar] [CrossRef]
- Rozario, P. A.; Hong, S. I. Foreign Domestic Workers and Eldercare in Singapore: Who Hires Them? Journal of Aging & Social Policy 2019, 31(3), 197–210. [Google Scholar] [CrossRef] [PubMed]
- Thompson, J.; Malhotra, R.; Love, S.; Ostbye, T.; Chan, A.; Matchar, D. Projecting the number of older Singaporeans with activity of daily living limitations requiring human assistance through 2030. Annals of the Academy of Medicine, Singapore 2014, 43(1), 51–56. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y; Zhao, X; Feng, Q; Liu, L; Yao, Y; Shi, J. Psychological assistance during the coronavirus disease 2019 outbreak in China. Journal of Health Psychology 2020, 25(6), 733–737. [Google Scholar] [CrossRef] [PubMed]
- Yeoh, B. S. A.; Huang, S. Foreign Domestic Workers and Home-Based Care for Elders in Singapore. Journal of Aging & Social Policy 2009, 22(1), 69–88. [Google Scholar] [CrossRef] [PubMed]
- Zhang, J.; Wang, Z.; Sun, Y.; et al. Projections of households, living arrangements, and demand of care needs for disabled older adults in China. China popul. dev. stud. 9, 1–16. [CrossRef]
| 1 | https://www.sgenable.sg/about-us/our-impact/disability-in-singapore |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




