Submitted:
21 April 2026
Posted:
22 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction: Toward a Paradigm Refinement
2. Three Persistent Misconceptions in Applying Thermodynamics to Body Weight Regulation
2.1. Calories Cannot Be Eaten – Nor Oxidized
2.2. The Irrelevance of Einstein’s E=mc² to Human Metabolism
2.3. The First Law of Thermodynamics Concerns Only Energy, Not Mass
2.4. Why These Distinctions Matter
3. The Inefficiency of the Two-Step Conversion Process in EBM
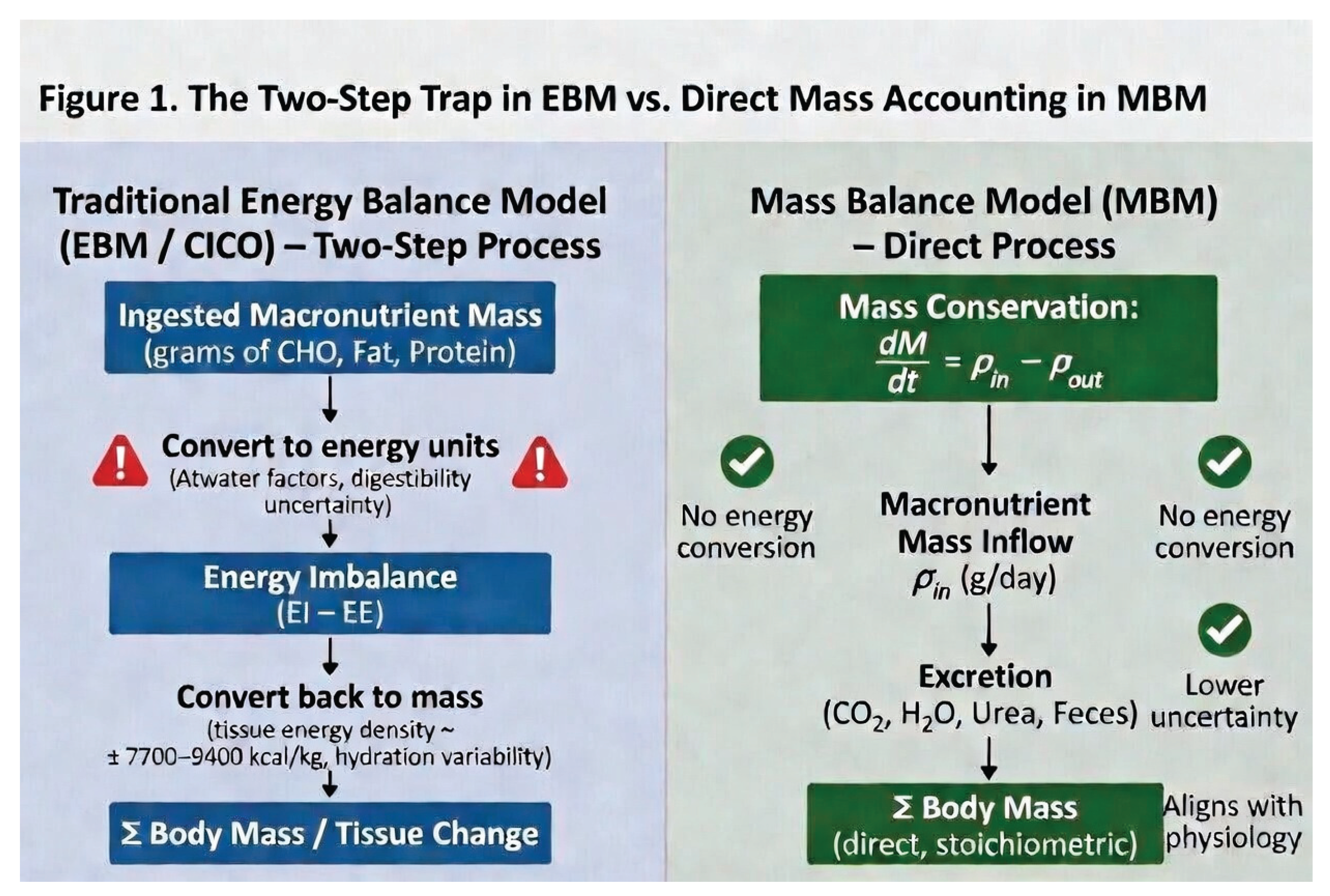
4. Clarification in Response to Recent Feedback
5. Conclusion
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
Ethics approval and consent to participate
Consent for publication
Availability of data
References
- Hall, K.D.; Farooqi, I.S.; Friedman, J.M.; Klein, S.; Loos, R.J.F.; Mangelsdorf, D.J.; O'Rahilly, S.; Ravussin, E.; Redman, L.M.; Ryan, D.H.; Speakman, J.R.; Tobias, D.K. The energy balance model of obesity: beyond calories in, calories out. Am J Clin Nutr 2022, 115(5), 1243–1254. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Nutrition and Metabolic Management Branch of China International Exchange and Promotive Association for Medical and Health Care; Clinical Nutrition Branch of Chinese Nutrition Society; Chinese Diabetes Society; Chinese Society for Parenteral and Enteral Nutrition; Chinese Clinical Nutritionist Center of Chinese Medical Doctor Association. Guidelines for medical nutrition treatment of overweight/obesity in China (2021). Asia Pac J Clin Nutr. 2022, 31(3), 450–482. [Google Scholar] [CrossRef] [PubMed]
- Hassapidou, M.; Vlassopoulos, A.; Kalliostra, M.; Govers, E.; Mulrooney, H.; Ells, L.; Salas, X.R.; Muscogiuri, G.; Darleska, T.H.; Busetto, L.; Yumuk, V.D.; Dicker, D.; Halford, J.; Woodward, E.; Douglas, P.; Brown, J.; Brown, T. European Association for the Study of Obesity Position Statement on Medical Nutrition Therapy for the Management of Overweight and Obesity in Adults Developed in Collaboration with the European Federation of the Associations of Dietitians. Obes Facts 2023, 16(1), 11–28. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Raynor, H.A.; Morgan-Bathke, M.; Baxter, S.D.; Halliday, T.; Lynch, A.; Malik, N.; Garay, J.L.; Rozga, M. Position of the Academy of Nutrition and Dietetics: Medical Nutrition Therapy Behavioral Interventions Provided by Dietitians for Adults With Overweight or Obesity, 2024. J Acad Nutr Diet. 2024, 124(3), 408–415. [Google Scholar] [CrossRef] [PubMed]
- Arencibia-Albite, F. Serious analytical inconsistencies challenge the validity of the energy balance theory. Heliyon Erratum in: Heliyon. 2020 Sep 14;6(9):e04609. doi: 10.1016/j.heliyon.2020.e04609. PMID: 32685707; PMCID: PMC7355950. 2020, 6(7), e04204. [Google Scholar] [CrossRef] [PubMed]
- Arencibia-Albite, F. The energy balance theory is an inconsistent paradigm. J Theor Biol. 2022, 550, 111240. [Google Scholar] [CrossRef] [PubMed]
- Manninen, A.H. Chronic positive mass balance is the actual etiology of obesity: A living review. Global Transl Med. 2023, 2(1), 222. [Google Scholar] [CrossRef]
- Manninen, A.H. Mass balance and energy balance in body weight regulation: A response to Theodorakis’ comments. Global Transl Med. 2025, 4(3), 119–120. [Google Scholar] [CrossRef]
- Arencibia-Albite, F. Empirical Evaluation of the Mass Balance Model in Human Bodyweight Regulation PREPRINT (Version 1) available at Research Square. 13 January 2026. [CrossRef]
- Arencibia-Albite, F. Quantitative Foundations of Energy Balance Are Not Empirically Reliable Under Ideal Conditions. PREPRINT (Version 1) available at Research Square. 16 January 2026. [CrossRef]
- Ludwig, D.S.; Aronne, L.J.; Astrup, A.; de Cabo, R.; Cantley, L.C.; Friedman, M.I.; Heymsfield, S.B.; Johnson, J.D.; King, J.C.; Krauss, R.M.; Lieberman, D.E.; Taubes, G.; Volek, J.S.; Westman, E.C.; Willett, W.C.; Yancy, W.S.; Ebbeling, C.B. The carbohydrate-insulin model: a physiological perspective on the obesity pandemic. Am J Clin Nutr. 2021, 114(6), 1873–1885. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



