Submitted:
06 April 2026
Posted:
07 April 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Introduction
Research Design
Data Collection
Results & Discussion
| Characteristic | n (%) | Mean |
|---|---|---|
| Age | - | 57 |
| Sex | ||
| Male | 254 (83,8) | - |
| Female | 49 (16,2) | - |
| Revascularization | ||
| Complete | 153 (50,4) | - |
| Incomplete | 150 (49,6) | - |
| Primary PCI | 125 (41,2) | - |
| Elective PCI | 178 (58,8) | - |
| Procedure | Revascularization | Description | Range (m) |
|---|---|---|---|
| 6MWT | Complete | Mean | 316 |
| Median | 328 | ||
| Standard Deviation | 70 | ||
| Incomplete | Mean | 290 | |
| Median | 300 | ||
| Standard Deviation | 77 |
| T-Test For Equality | ||||||
| df. | Sig. (2-tailed) | Mean Difference | 95% Confidence Interval of the Difference | |||
| Lower | Upper | |||||
| 6MWT | Equal Variances | 301 | 0.002 | 26.41 | 9.64 | 43.18 |
| Equal Variances Not Assumed | 297,1 | 0.002 | 26.41 | 9.62 | 43.19 | |
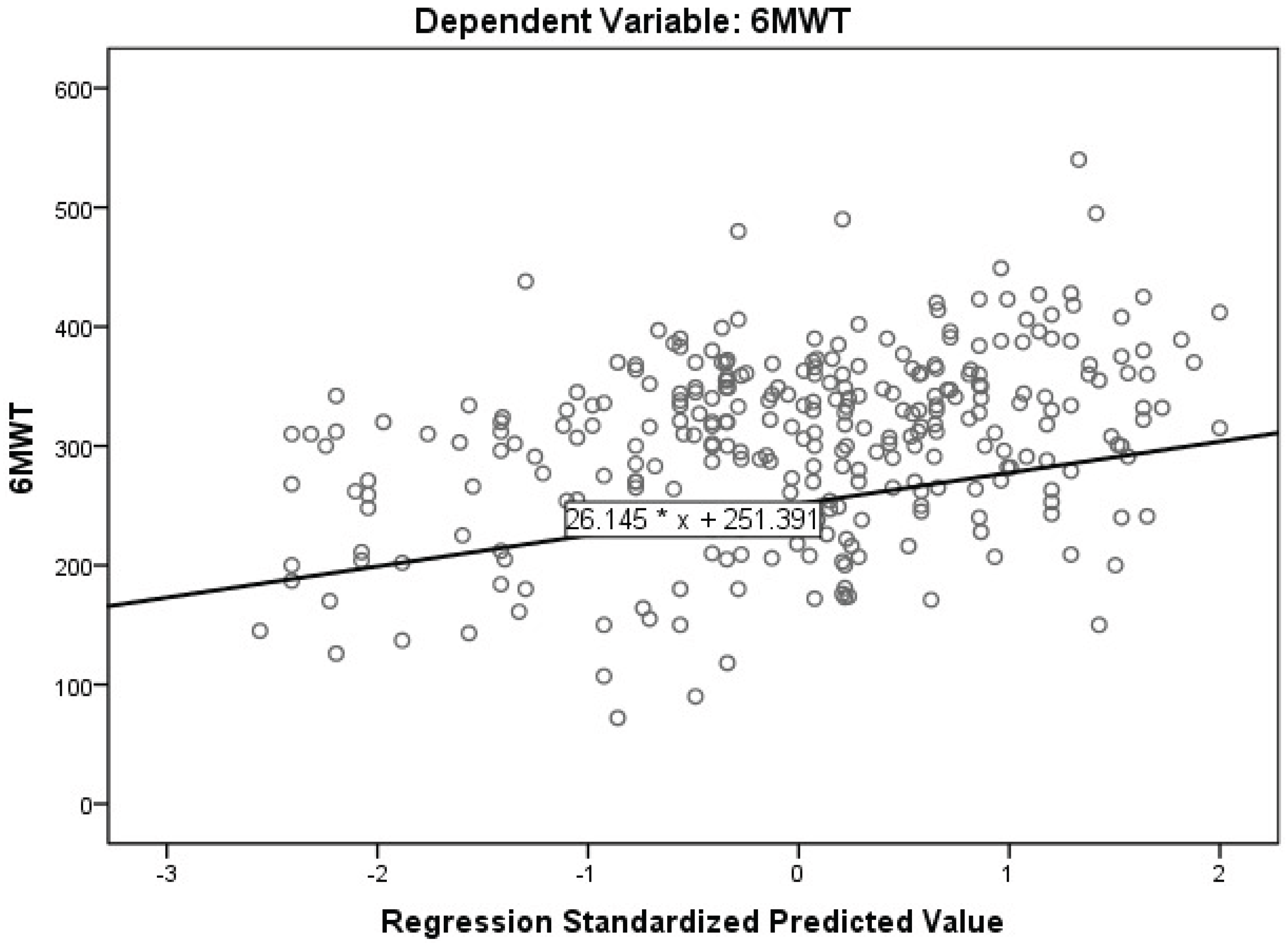
Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Ethical Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Clinical Trial
References
- Hari Jantung Sedunia (World Heart Day): Your Heart is Our Heart Too - Penyakit Tidak Menular Indonesia [Internet]. Available online: http://p2ptm.kemkes.go.id/kegiatan-p2ptm/pusat-/hari-jantung-sedunia-world-heart-day-your-heart-is-our-heart-too (accessed on 25 January 2025).
- Amini, M; Zayeri, F; Salehi, M. Trend analysis of cardiovascular disease mortality, incidence, and mortality-to-incidence ratio: results from global burden of disease study 2017. BMC Public Health 2021, 21, 401. [Google Scholar] [CrossRef] [PubMed]
- Gaidai, O; Cao, Y; Loginov, S. Global cardiovascular diseases death rate prediction. Curr Probl Cardiol 2023, 48, 101622. [Google Scholar] [CrossRef] [PubMed]
- Kim, Y. Health-related quality of life in patients with coronary artery disease undergoing percutaneous coronary intervention: A cross-sectional study. J Nurs Res 2021, 30, e186. [Google Scholar] [CrossRef] [PubMed]
- Pavasini, R; Biscaglia, S; Kunadian, V; Hakeem, A; Campo, G. Coronary artery disease management in older adults: revascularization and exercise training. Eur Heart J 2024, 45, 2811–23. [Google Scholar] [CrossRef] [PubMed]
- Mehta, SR; Wood, DA; Storey, RF; Mehran, R; Bainey, KR; Nguyen, H; et al. Complete revascularization with multivessel PCI for myocardial infarction. N Engl J Med 2019, 381, 1411–21. [Google Scholar] [CrossRef] [PubMed]
- Collet, J-P; Thiele, H; Barbato, E; Barthélémy, O; Bauersachs, J; Bhatt, DL; et al. 2020 ESC Guidelines for the management of acute coronary syndromes in patients presenting without persistent ST-segment elevation. Eur Heart J 2021, 42, 1289–367. [Google Scholar] [CrossRef] [PubMed]
- Neumann, F-J; Sousa-Uva, M; Ahlsson, A; Alfonso, F; Banning, AP; Benedetto, U; et al. 2018 ESC/EACTS Guidelines on myocardial revascularization. Eur Heart J 2019, 40, 87–165. [Google Scholar] [CrossRef] [PubMed]
- ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories. ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med 2002, 166, 111–7. [Google Scholar] [CrossRef] [PubMed]
- Ross, RM; Murthy, JN; Wollak, ID; Jackson, AS. The six minute walk test accurately estimates mean peak oxygen uptake. BMC Pulm Med 2010, 10, 31. [Google Scholar] [CrossRef] [PubMed]
- Dasari, TW; Patel, B; Wayangankar, SA; Alexander, D; Zhao, YD; Schlegel, J; et al. Prognostic value of 6-minute walk distance in patients undergoing percutaneous coronary intervention: A veterans affairs prospective study. Tex Heart Inst J 2020, 47, 10–4. [Google Scholar] [CrossRef] [PubMed]
- Fiorina, C; Vizzardi, E; Lorusso, R; Maggio, M; De Cicco, G; Nodari, S; et al. The 6-min walking test early after cardiac surgery. Reference values and the effects of rehabilitation programme. Eur J Cardiothorac Surg 2007, 32, 724–9. [Google Scholar] [CrossRef] [PubMed]
- Gaba, P; Gersh, BJ; Ali, ZA; Moses, JW; Stone, GW. Complete versus incomplete coronary revascularization: definitions, assessment and outcomes. Nat Rev Cardiol 2021, 18, 155–68. [Google Scholar] [CrossRef] [PubMed]
- Gao, Y; Yue, L; Miao, Z; Wang, F; Wang, S; Luan, B; et al. The effect and possible mechanism of cardiac rehabilitation in partial revascularization performed on multiple coronary artery lesions. Clin Interv Aging 2023, 18, 235–48. [Google Scholar] [CrossRef] [PubMed]
- Melotti, E; Belmonte, M; Gigante, C; Mallia, V; Mushtaq, S; Conte, E; et al. The role of multimodality imaging for percutaneous coronary intervention in patients with Chronic total occlusions. Front Cardiovasc Med 2022, 9, 823091. [Google Scholar] [CrossRef] [PubMed]
- Tjahjono, C; Arthamin, M. The role of cardiac rehabilitation in facilitating return to work after cardiovascular events. Med Res Arch 2024, 12. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




