1. Introduction
Disease-related malnutrition (DRM) represents a significant public health challenge affecting millions of patients worldwide, particularly those with chronic conditions, oncological diseases, and age-related decline. DRM in various clinical settings is associated with increased morbidity, mortality, prolonged hospital stays, rehospitalizations and reduced quality of life. The economic burden is substantial, with malnourished patients requiring more healthcare resources and experiencing poorer treatment outcomes [
1,
2].
Oral nutritional supplements (ONS) serve as a cornerstone intervention for managing disease-related malnutrition. These specialized medical nutrition products provide energy, protein, essential nutrients and pharmaconutrients designed for patients who cannot meet their nutritional needs through regular diet alone, either temporarily or permanently [
3]. In the European Union, ONS are regulated under the category of Foods for Special Medical Purposes (FSMP), primarily governed by Regulation (EU) No. 609/2013 on foods for specific groups and further specified by Commission Delegated Regulation (EU) 2016/128 [
4,
5]. FSMP is defined as " food specially processed or formulated and intended for the dietary management of patients, including infants, to be used under medical supervision; it is intended for the exclusive or partial feeding of patients with a limited, impaired or disturbed capacity to take, digest, absorb, metabolize or excrete ordinary food or certain nutrients contained therein, or metabolites, or with other medically-determined nutrient requirements, whose dietary management cannot be achieved by modification of the normal diet alone” [
5].
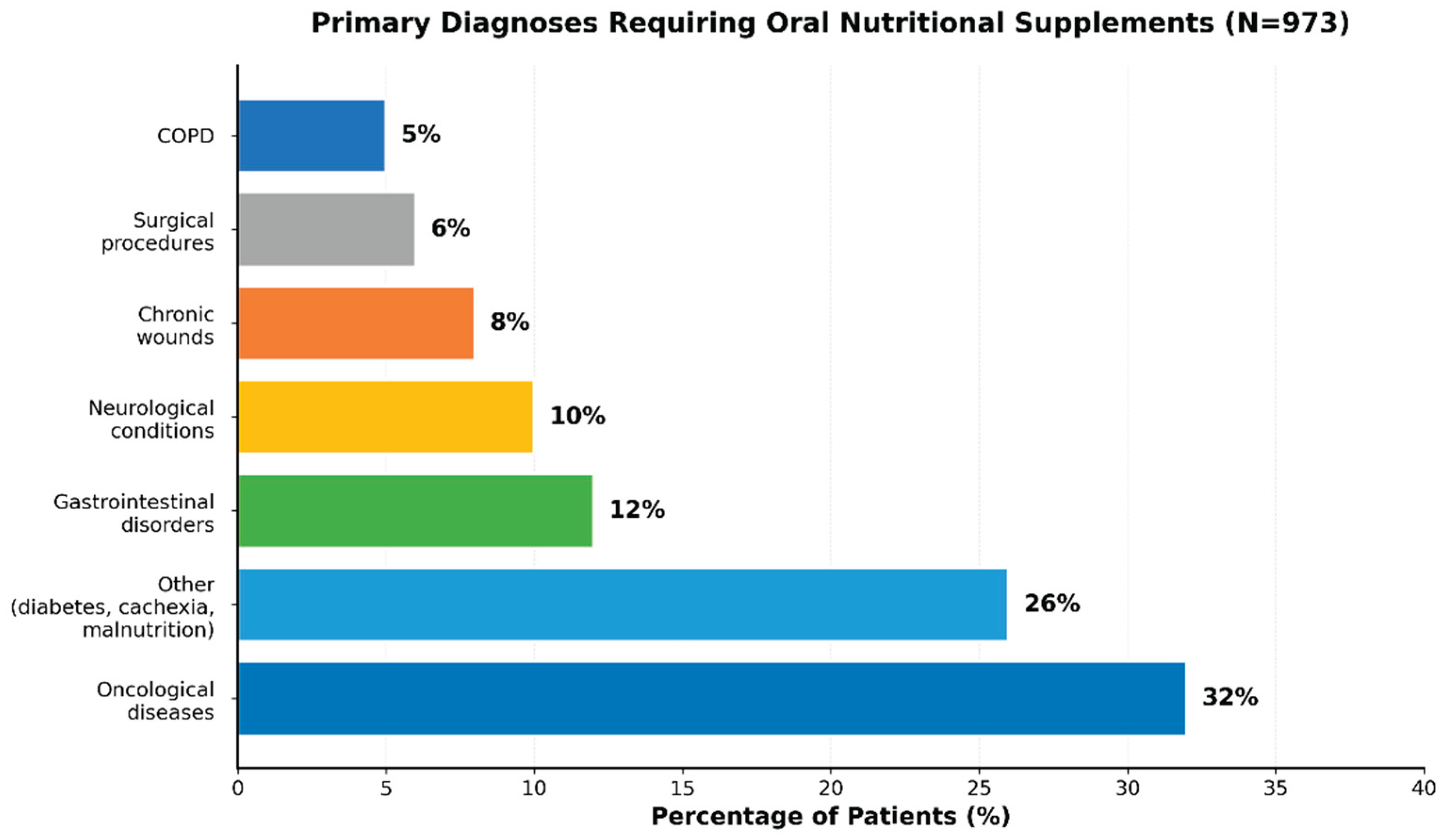
Clinical evidence demonstrates that appropriate ONS use improves nutritional status, supports recovery, reduces complications, and enhances patient outcomes across various conditions including cancer, gastrointestinal diseases, chronic obstructive pulmonary disease (COPD), neurological diseases, geriatric medicine, and perioperative care [
6,
7,
8,
9]. However, the effectiveness of ONS depends not only on appropriate clinical prescription but also on patient adherence and accessibility [
10]. Reimbursement of ONS by the national healthcare fund is shown to facilitate ONS consumption and increase adherence in many studies [
10,
11]. In healthcare systems where ONS require patient co-payment, the step from prescription to actual use becomes critical barrier to adherence [
9,
10]. It involves several stakeholders requiring coherent collaborative practice: specialists who diagnose malnutrition and prescribe treatment, clinical dietitians who advise on nutrition support therapy, general practitioners who coordinate care, pharmacists who dispense and advise, and patients who must understand and follow the therapy [
3,
12].
The current healthcare landscape emphasizes integrated care models and collaborative practice, recognizing that optimal patient outcomes require coordinated efforts across disciplines rather than isolated clinical encounters [
3,
13]. However, the ONS provision pathway often operates as a fragmented sequence rather than a cohesive system [
14]. Understanding the dynamics of this care continuum—particularly the key touchpoint at the pharmacy where prescribed therapy is first presented to the patient—is essential for optimizing nutritional outcomes and ensuring that patient populations at nutritional risk receive required therapeutic nutrition [
15]. The management of disease-related malnutrition requires coordinated efforts across healthcare disciplines. While specialists, clinical dietitians and general practitioners possess clinical expertise to identify nutritional needs and prescribe appropriate interventions, they typically lack direct insight into what occurs at the pharmacy dispensing encounter—the moment when medical recommendations transform into treatment decisions [
9]. Conversely, pharmacists interact directly with patients but often lack comprehensive clinical context about the prescribing rationale and patient-specific considerations. Research reveals that 87.2% of pharmacists identify lack of expertise in nutrition counseling as the main barrier to providing nutritional support, with inadequate knowledge and unavailability of educational materials limiting their practice [
15]. Pharmacists occupy a distinct position in the patient care pathway, often representing the final point of contact before a prescription is dispensed. This role places them in a meaningful position to support adherence to oral nutritional supplement (ONS) therapy; however, their contribution to nutritional care remains relatively underexplored in both clinical practice and research literature. From a pharmaceutical care perspective, the role of the pharmacist extends beyond dispensing and explanation of co-payment. At the point of supply, pharmacists should assess whether patients understand the therapeutic purpose of ONS, are able to incorporate it into daily routines, and are likely to adhere to the recommended regimen. They are also often the first to identify practical barriers such as affordability concerns, anticipated poor palatability, treatment fatigue, or caregiver dependence, which may not be fully apparent during prescribing. This unique position makes pharmacists emergent gatekeepers of ONS therapy, yet their role in nutritional care remains underexplored and under-supported in both clinical practice and research literature [
9,
10,
12]
This study examines the ONS provision pathway in Croatia’s co-payment healthcare system, focusing on patient acceptance patterns, barriers to adherence, and the pivotal role of pharmacist-patient interactions in determining treatment outcomes. Croatia provides an instructive case study as a European Union member state with a mainly public healthcare system where some categories of ONS require substantial patient co-payment, creating financial barriers like those experienced in many healthcare systems globally.
The research investigates fundamental questions about the ONS care pathway:
What factors influence patients’ willingness to accept and collect prescribed ONS at the pharmacy dispensing encounter?
What proportion of patients experience barriers—financial, informational, or psychological—that prevent them from obtaining prescribed nutrition therapy?
How do pharmacist-patient interactions influence acceptance decisions, and what role do pharmacists currently play in supporting nutritional therapy?
What gaps exist in the communication pathway from prescriber through pharmacist to patient, and how might enhanced collaborative practice optimize this crucial stage in the care pathway?
Given that pharmacists often represent the final opportunity to educate and support patients before treatment is initiated or discontinued, their role and the patient experience at this point are critical for treatment success. Identifying gaps at this stage of the care continuum also creates opportunities for targeted interventions through stronger collaborative practice models between prescribers and pharmacists.