Submitted:
03 April 2026
Posted:
07 April 2026
You are already at the latest version
Abstract
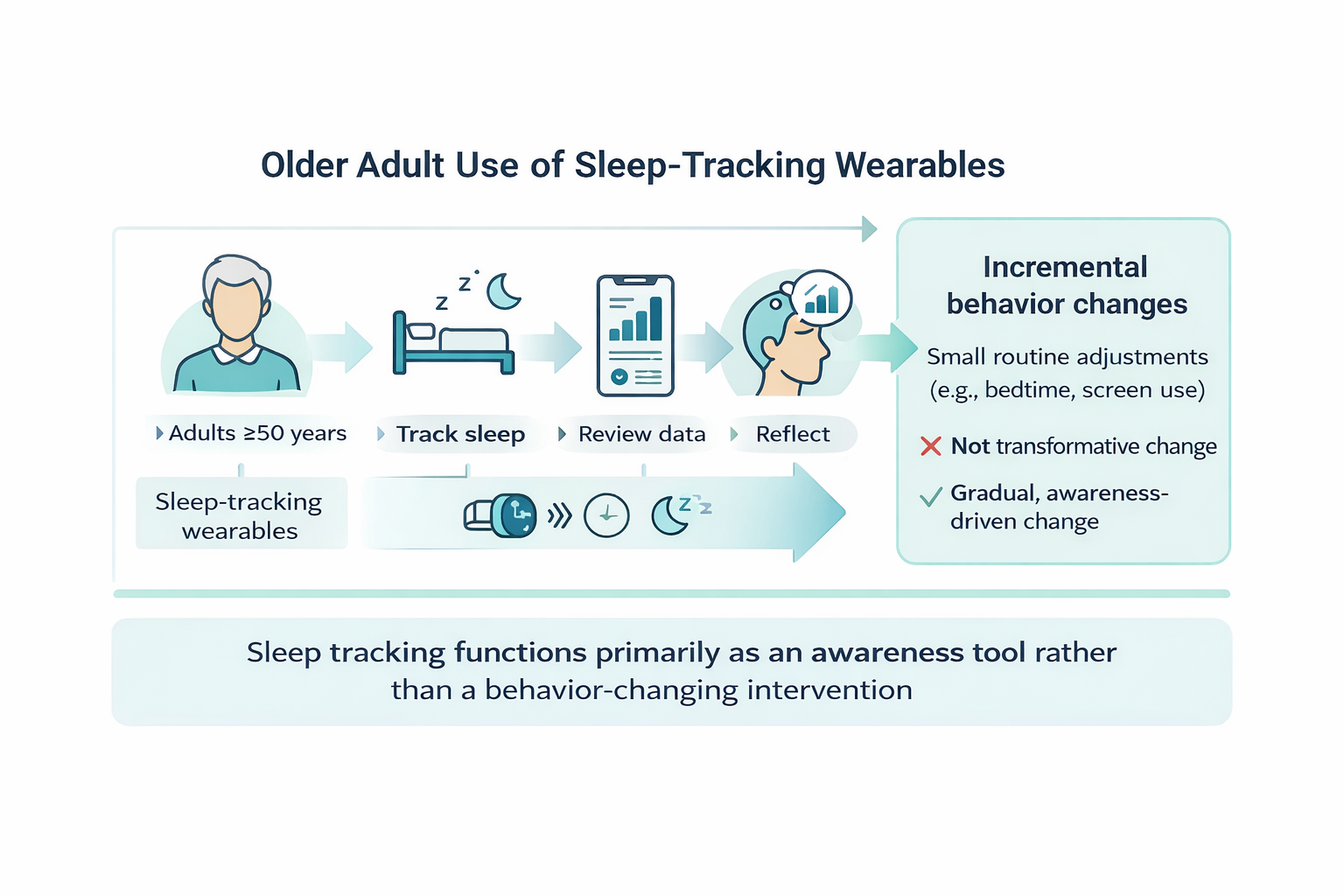
Keywords:
1. Introduction
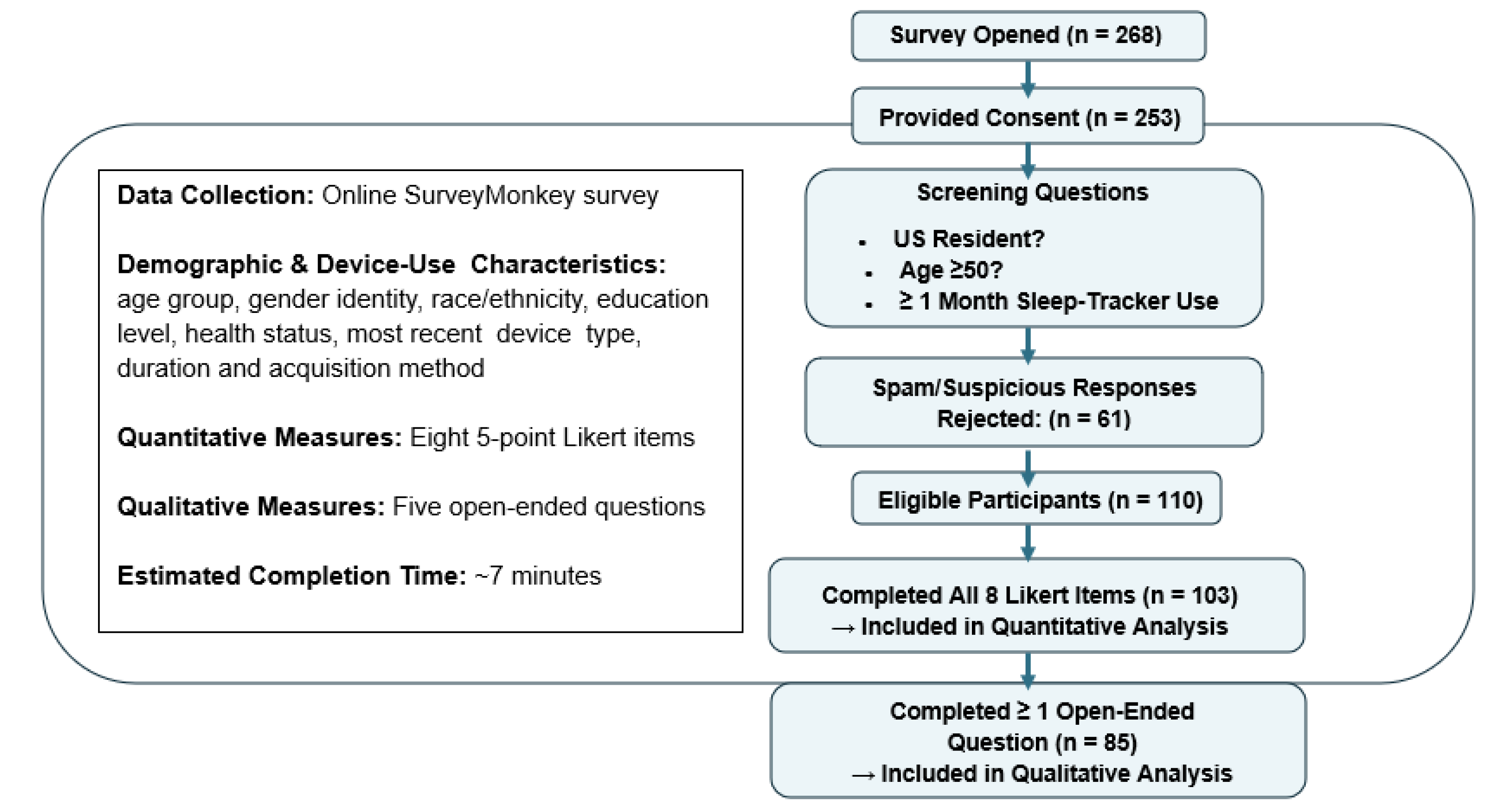
2. Methods
2.1. Study Design
2.2. Participants and Recruitment
2.3. Survey Design
2.4. Data Collection
2.5. Quantitative Analysis
2.6. Qualitative Analysis
2.7. Mixed-Methods Integration
3. Results
3.1. Participant Characteristics
3.2. Quantitative Findings
3.3. Qualitative Themes (Themes and Codes)
3.3.1. Theme 1: Sleep Tracking as a Reflective Daily Feedback System (n = 30)
3.3.2. Theme 2: Incremental Adjustment of Bedtime Routines (n = 46)
3.3.3. Theme 3: Selective Interpretation and Conditional Trust in Metrics (n = 35)
3.3.4. Theme 4: Design Friction and Desire for More Actionable Guidance (n = 32)
3.3.5. Thematic Synthesis
3.4. Integrated Findings
4. Discussion
4.1. Sleep Awareness
4.2. Digital Engagement
4.3. Incremental Habit Change
4.4. Interpreting Sleep Data
4.5. Daytime Functioning
4.6. Digital Companions
5. Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| MDPI | Multidisciplinary Digital Publishing Institute |
| DOAJ | Directory of open access journals |
| TLA | Three letter acronym |
Appendix A. IRB-Approved Survey Instrument

- Yes, I agree
- No
- Yes
- No
- Yes
- No
- Yes
- No
- Yes
- No
- If “No” → End Survey
- If “Yes” → Show Q5
- Fitbit
- Apple Watch
- Oura Ring
- Garmin
- WHOOP
- Samsung Galaxy Watch
- Prefer not to say
- Other: ________
- Fitbit
- Apple Watch
- Oura Ring
- Garmin
- WHOOP
- Samsung Galaxy Watch
- Prefer not to say
- Other: ________
- Less than 1 month
- 1–3 months
- 4–6 months
- 7–12 months
- More than 1 year
- Prefer not to say
- I purchased it myself
- It was gifted to me
- It was provided through a wellness program or employer
- It was provided for medical/health reasons
- Prefer not to say
- Other:
- Yes
- No
- Not sure
- Prefer not to say
- Activity tracking / steps
- Heart-rate monitoring
- Exercise / workout tracking
- Stress monitoring
- Blood oxygen (SpO₂) monitoring
- Notifications or communication
- Prefer not to say
- Other: ________
- 50-59
- 60-69
- 70-79
- 80-89
- 90+
- Prefer not to say
- Male
- Female
- Prefer not to say
- Asian
- Black or African American
- Hispanic or Latino
- Native American or Alaska Native
- Native Hawaiian or Pacific Islander
- White
- Prefer not to say
- Other: ______
- Less than high school
- High school diploma/GED
- Some college
- Associate degree
- Bachelor’s degree
- Graduate or professional degree
- Prefer not to say
- Excellent
- Very good
- Good
- Fair
- Poor
- Prefer not to say
- Yes
- No
Appendix Table B. Demographics and Device-Use Characteristics
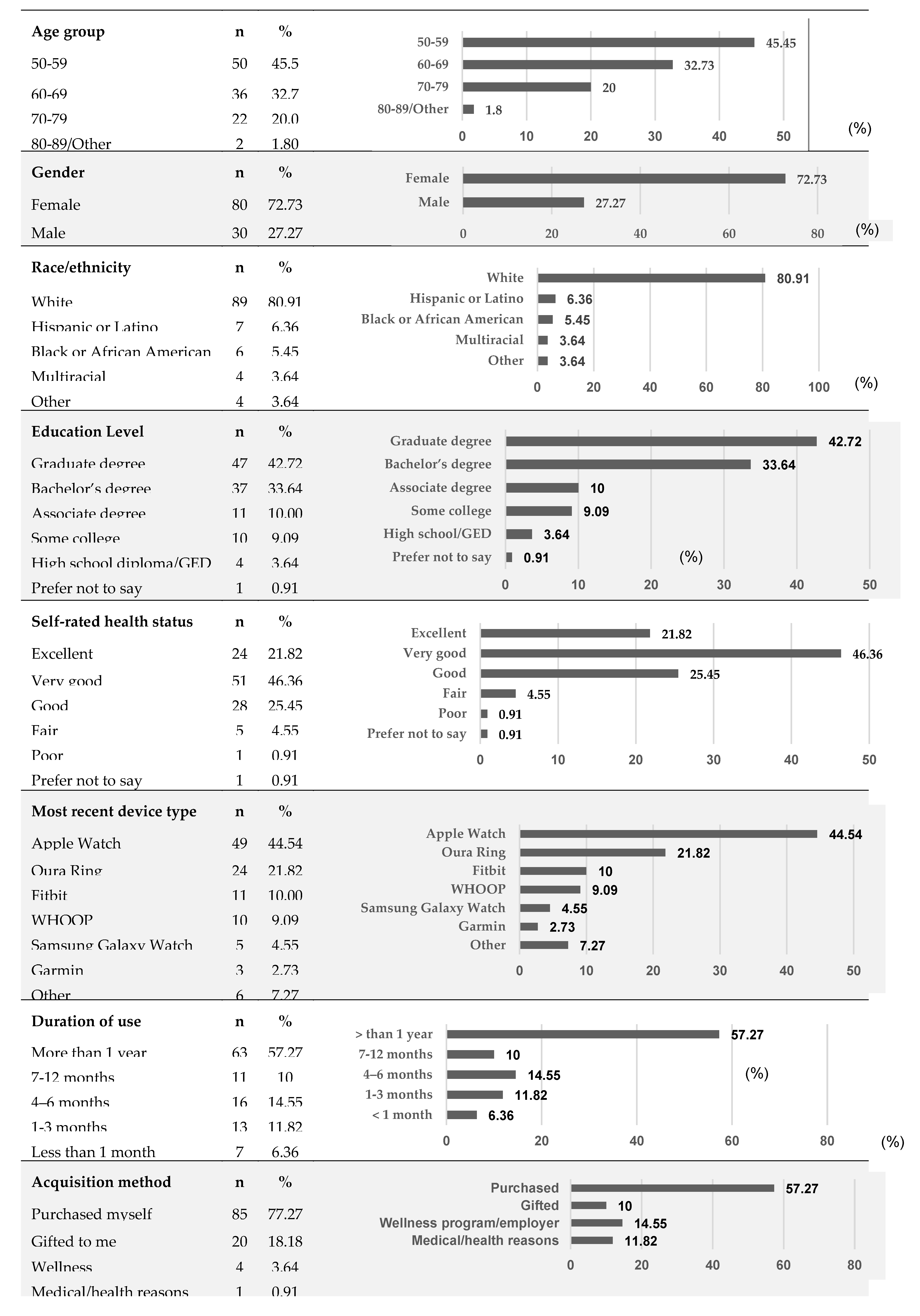
- Note. Values represent the number and percentage of participants within each category (N = 110). Percentages may not sum to exactly 100% due to rounding. Device-use characteristics refer to the participant’s most recently used sleep-tracking device.
Appendix Table C. Quantitative Analysis
| Outcome | Test | Mean (SD) | Median (IQR) | Neutral Reference | Test Statistic | p | Effect Size (r) |
| Behavior-change composite (mean of bedtime routine change + long-term improvement) | One-sample Wilcoxon signed-rank | 3.78 (0.87) | 4 (1.50) | 3 | V = 3578 | < .001 | 0.67 |
- Note. The Behavior-Change Composite is the mean of two Likert items assessing bedtime routine change and long-term sleep improvement.
Appendix Table D. Thematic Analysis of Open-Text Survey Responses
| Predictor | Test | Group Medians (IQR) | Test statistic | p | Effect |
| Gender | Mann–Whitney U | Female: 4 (1.00) , Male: 4 (1.25) | U = 712 | .024 | r = 0.223 |
| Age group | Kruskal–Wallis | 50–59: 4 (0.50), 0–69: 4 (1.63), 70–79: 4 (1.00), Other: 3 (0.00) | H(3) = 3.38 | .336 | η² = 0.004 |
| Education | Kruskal–Wallis | High School: 3 (0.25), Some college: 4 (0.50), Associate: 4 (0.50),, Bachelor’s: 4 (1.50), Graduate: 4 (1.00) | H(4) = 3.66 | .455 | η² < .001 |
| Self-rated health | Kruskal–Wallis | Excellent: 4 (1.38), Very Good: 4 (0.50), Good: 4 (1.00), Fair/Poor: 3.25 (0.88) | H(3) = 7.92 | .048 | η² = 0.050 |
| Race/ethnicity | Kruskal–Wallis | Black/AA: 4.25 (1.25), Hispanic/Latino: 4 (0.38), Multiracial: 3.5 (1.50), White: 4 (1.00), Other: 4.25 (1.25) | H(4) = 1.42 | .840 | η² < .001 |
| Device type | Kruskal–Wallis | Apple Watch: 4.0 (0.50), Fitbit: 3.75 (2.00), Garmin: 3.5 (1.25), Oura Ring: 4(1.25), Samsung Galaxy: 2.75 (1.13),Other: 4 (0.375) |
H(5) = 4.80 | .441 | η² < .001 |
| Duration of use | Kruskal–Wallis | <1 Month: 3.50 (0.50), 1–3 Months: 3.5 (0.50), 4–6 Months: 3.75 (0.50) 7–12 Months: 4 (0.75), >1 Year: 4 (1.00) |
H(4) = 2.72 | .606 | η² < .001 |
| Device acquisition | Kruskal–Wallis | Purchased: 4 (1.125), Gifted: 4 (1.00), Other: 4 (0.50) | H(2) = 0.38 | .825 | η² < .001 |
- Note. Values represent group medians (IQR). Mann–Whitney U tests were used for two-group comparisons and Kruskal–Wallis tests for multi-group comparisons. Bold p-values indicate statistical significance (p < .05). Effect sizes are reported as r (Mann–Whitney U) and η² (Kruskal–Wallis).
Appendix Table E. Joint Display of Quantitative Findings and Qualitative Themes
| Theme | Definition | Codes | n (%) of Respondents | Representative Quote(s) |
| Sleep Tracking as a Reflective Daily Feedback System | Participants described using sleep metrics as a routine, reflective check-in, typically conducted in the morning, allowing them to interpret data from previous night and increase awareness of sleep patterns over time. | Morning check-in, Reviewing sleep scores, Trend monitoring, Linking data to daytime readiness, Reflective self-monitoring | 30 (34.9%) | “I check the sleep score every morning and find it interesting and a reminder that going to bed earlier definitely makes a difference.” “A ‘sleep score’ is helpful when trying to assess how hard my daily workout should be.” |
|
Incremental Adjustment of Bedtime Routines |
Participants reported modest, practical adjustments to their bedtime routines, framed as small tweaks rather than major or sustained lifestyle change. | Earlier bedtime, Wind-down changes, Reduced screen use, Caffeine/alcohol reduction, Bedtime reminders, Minor routine tweaks | 46 (53.5%) | “I try to put my phone down sooner because I can see it affects my sleep score.” “”It nudges me to make better choices at night.” |
| Selective Interpretation and Conditional Trust in Metrics | Participants critically evaluated tracker outputs. Conditional trust was granted after weighing subjective sleep experiences alongside device metrics and discounting results that appeared discordant. | Accuracy skepticism, Sleep stage/quality doubt, Comparing metrics to subjective experience, Treating single-night irregularities as outliers, Selective metric use | 35 (40.7%) | “Sometimes the data doesn’t match how I actually feel. For example, it might say I had “great” sleep when I feel tired, or show multiple wake-ups that I don’t remember. That can make me question how reliable the metrics are.” “I use it as a guide, not gospel.” |
|
Design Friction and Desire for More Actionable Guidance |
Participants identified usability constraints and practical burdens, expressing a preference for more personalized and actionable recommendations rather than isolated scores or raw data. | Charging difficulties, Comfort/fit issues, Alerts interfering with sleep continuity, App/connectivity problems, Desire for tailored recommendations, Actionable coaching | 32 (37.2%) | “I would like my sleep tracker to give more personalized and practical insights instead of just showing raw data.” “It is very difficult to sleep with a device on my arm.” |
- Note. Thematic analysis was conducted on open-text survey responses provided by eligible participants (n = 86). Percentages represent the proportion of respondents whose comments reflected each theme. Responses could be coded to multiple themes. Quotes are illustrative examples.
References
- de Zambotti, M., Cellini, N., Goldstone, A., Colrain, I. M., & Baker, F. C. (2019). Wearable sleep technology in clinical and research settings. Medicine and Science in Sports and Exercise, 51(7), 1538–1557. [CrossRef]
- Del-Valle-Soto, C., López-Pimentel, J. C., Vázquez-Castillo, J., Nolazco-Flores, J. A., Velázquez, R., Varela-Aldás, J., & Visconti, P. (2024). A comprehensive review of behavior change techniques in wearables and IoT: Implications for health and well-being. Sensors (Basel, Switzerland), 24(8), 2429. [CrossRef]
- Dion, K., Porteous, M., Kendzerska, T., Nixon, A., Lee, E., de Zambotti, M., Garland, S. N., Singh, M., De Luca, G., Gillman, S., Baril, A.-A., Gallson, D., Robillard, R., & Canadian Sleep Research Consortium. (2025). Sleep, health care-seeking behaviors, and perceptions associated with the use of sleep wearables in Canada: Results from a nationally representative survey. Journal of Medical Internet Research, 27, e68816. [CrossRef]
- Ghazi, S. N., Behrens, A., Berner, J., Sanmartin Berglund, J., & Anderberg, P. (2025). Objective sleep monitoring at home in older adults: A scoping review. Journal of Sleep Research, 34(4), e14436. [CrossRef]
- Hoffmann, T., & Gualtieri, L. (2026). What’s your sleep number? Available online: https://generations.asaging.org/whats-your-sleep-number/ (accessed on 22 January 2026).
- Hui, S. A., & Grandner, M. A. (2015). Associations between poor sleep quality and stages of change of multiple health behaviors among participants of employee wellness program. Preventive Medicine Reports, 2, 292–299. [CrossRef]
- Kakulla, B. (2024). 2025 tech trends and adults 50-plus. Washington, DC: AARP Research. [CrossRef]
- Kakulla, B., David, P., Skufca, L., Boothe, J., & Garrett, K. (2025). Empowering independence with technology among adults age 50-plus. Washington, DC: AARP Research. [CrossRef]
- Kakulla, B., & AARP Research. (n.d.). Health and wellness apps: Considerable use among older adults but room to grow. Available online: https://www.aarp.org/pri/topics/health/prevention-wellness/health-app-users/ (accessed on 11 March 2026).
- Kononova, A., Li, L., Kamp, K., Bowen, M., Rikard, R., Cotten, S., & Peng, W. (2019). The use of wearable activity trackers among older adults: Focus group study of tracker perceptions, motivators, and barriers in the maintenance stage of behavior change. JMIR mHealth and uHealth, 7(4), e9832. [CrossRef]
- Lampkin, C. (2024a). Experiences with sleep: Views of adults ages 40 and older. Washington, DC: AARP Research. [CrossRef]
- Lampkin, C. (2024b). Healthy living and sleep: Views of adults ages 40 and older. Washington, DC: AARP Research. [CrossRef]
- Li, J., Vitiello, M. V., & Gooneratne, N. (2018). Sleep in normal aging. Sleep Medicine Clinics, 13(1), 1–11. [CrossRef]
- Liu, G.-H., Huang, Y.-H., Yuan, T.-C., Chen, Y.-P., Hsu, J.-L., Lee, S.-H., Lin, C.-M., Toh, C.-H., Fang, J.-T., Lin, S.-W., Chuang, L.-P., & Chen, N.-H. (2025). Associations of wearable-measured sleep and physical activity with memory performance in older adults: Cross-sectional study with actigraphy and MRI. JMIR Aging, 8(1), e80584. [CrossRef]
- Moore, K., O’Shea, E., Kenny, L., Barton, J., Tedesco, S., Sica, M., Crowe, C., Alamäki, A., Condell, J., Nordström, A., & Timmons, S. (2021). Older adults’ experiences with using wearable devices: Qualitative systematic review and meta-synthesis. JMIR mHealth and uHealth, 9(6), e23832. [CrossRef]
- Parsey, C. M., & Schmitter-Edgecombe, M. (2019). Using actigraphy to predict the ecological momentary assessment of mood, fatigue, and cognition in older adulthood: Mixed-methods study. JMIR Aging, 2(1), e11331. [CrossRef]
- Prochaska, J. O., & Velicer, W. F. (1997). The transtheoretical model of health behavior change. American Journal of Health Promotion, 12(1), 38–48. [CrossRef]
- Project Catalyst, & HomeLab. (2016). Building a better tracker: Older consumers weigh in on activity and sleep monitoring devices. Washington, DC: AARP Research. [CrossRef]
- Robbins, R., Weaver, M. D., Sullivan, J. P., Quan, S. F., Gilmore, K., Shaw, S., Benz, A., Qadri, S., Barger, L. K., Czeisler, C. A., & Duffy, J. F. (2024). Accuracy of three commercial wearable devices for sleep tracking in healthy adults. Sensors (Basel, Switzerland), 24(20), 6532. [CrossRef]
- Searles, M. E., Licata, A., Cucinotta, M., Kainec, K., & Spencer, R. M. C. (2026). Performance evaluation of consumer sleep-tracking wearables and nearables in healthy young and older adults. SLEEP Advances, 7(1), zpag006. [CrossRef]
- Sharma, N., Brinke, J. K., Gemert-Pijnen, J. E. W. C. V., & Braakman-Jansen, L. M. A. (2021). Implementation of unobtrusive sensing systems for older adult care: Scoping review. JMIR Aging, 4(4), e27862. [CrossRef]
- Willoughby, A. R., Golkashani, H. A., Ghorbani, S., Wong, K. F., Chee, N. I. Y. N., Ong, J. L., & Chee, M. W. L. (2024). Performance of wearable sleep trackers during nocturnal sleep and periods of simulated real-world smartphone use. Sleep Health, 10(3), 356–368. [CrossRef]
| Item | N |
M (SD) |
Median (IQR) | Top-box% | Netural % | Bottom-box % |
| Ease of use/understand | 103 | 4.14 (0.86) | 4 (1) | 84.5 | 10.7 | 4.9 |
| Perceived accuracy/reliability | 103 | 3.93 (0.78) | 4 (0) | 78.6 | 16.5 | 4.9 |
| Usefulness of sleep data | 103 | 4.27 (0.72) | 4 (1) | 89.3 | 9.7 | 1.0 |
| Benefits outweigh frustrations | 103 | 4.19 (0.82) | 4 (1) | 83.5 | 13.6 | 2.9 |
| Encourages healthier habits | 103 | 4.04 (0.93) | 4 (1) | 75.7 | 17.5 | 6.8 |
| Stress/anxiety from tracking | 103 | 2.62 (1.11) | 2 (2) | 27.1 | 18.5 | 54.4 |
| Positive bedtime routine change | 103 | 3.70 (1.03) | 4 (1) | 63.1 | 22.3 | 14.6 |
| Long-term sleep habit improvement | 103 | 3.85 (0.83) | 4 (1) | 72.8 | 22.3 | 4.9 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




