Submitted:
01 April 2026
Posted:
03 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. The Warburg Effect and Tumor Metabolism: The Central Role of NAD+/NADH
2.1. Glycolytic Dependence of Cancer Cells
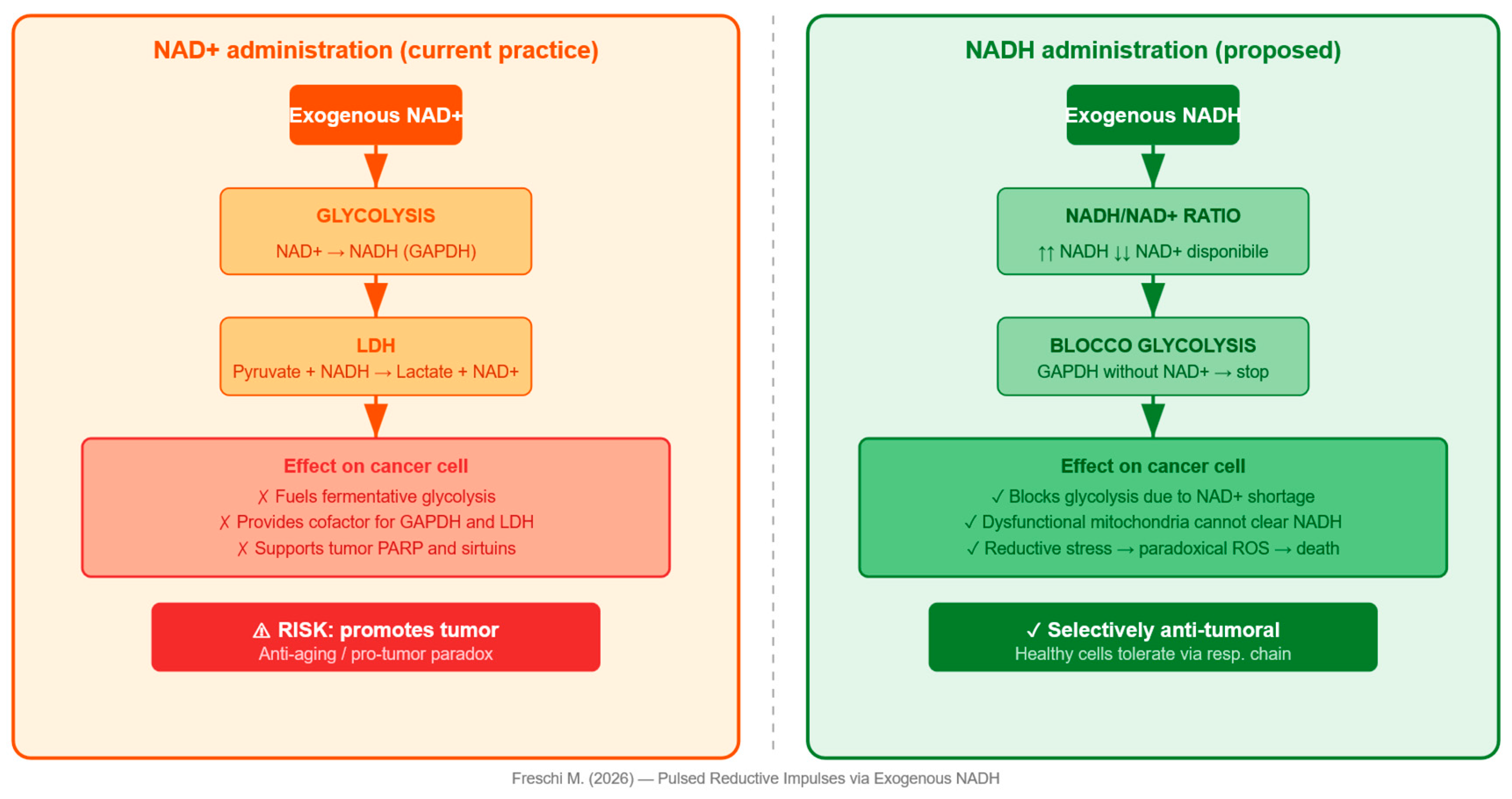
2.2. The NAD+ Paradox in Oncology vs Anti-Aging
2.3. Exogenous Reducing Equivalents vs NAD+: A Fundamental Distinction
3. Redox State and Tumor Microenvironment
3.1. The Oxidative-Inflammatory Environment as a Tumor Substrate
3.2. The Transmembrane Redox Interface
- (a)
- Transplasma membrane redox systems (ECTO-NOX): membrane proteins that transfer electrons from intracellular NADH to extracellular acceptors; in a reduced external environment, these systems are blocked, causing intracellular NADH accumulation [16].
- (b)
- Cysteine/cystine system (xCT/SLC7A11): the xCT transporter imports cystine (oxidized form), which is internally reduced to cysteine for glutathione synthesis. A reductive extracellular environment alters the cysteine/cystine ratio, modifying the intracellular glutathione pool [17].
- (c)
- Redox-sensitive receptors: EGFR, IGFR, and integrins possess extracellular domains with cysteine residues whose oxidation is required for dimerization and activation. A reductive environment suppresses these proliferative signals [18].
- (d)
- Direct ROS diffusion: hydrogen peroxide (H₂O₂) crosses the cell membrane, including through aquaporins, acting as a transmembrane redox messenger [19].
- (e)
- Lactate/pH gradients: lactate transport through MCT transporters is dependent on the pH gradient; alterations in the extracellular environment modify this gradient and the metabolic shuttle between cancer cells and stroma [20].
- (f)
- Intercellular communication: gap junctions (connexins) allow the direct passage of NADH, NAD+, glutathione, and second messengers between adjacent cells [21].
3.3. Reductive Stress: A Mirror Concept to Oxidative Stress
4. Limitations of Conventional Antioxidants
4.1. Lack of Targeting
4.2. Secondary Pro-Oxidation
4.3. Inadequate Compartmentalization
4.4. The Advantage of Reducing Equivalents as Electron Vehicles
5. Hypothesis: Cyclic Reductive Impulses via Exogenous Reducing Equivalents
5.1. Rationale for Intrinsic Metabolic Selectivity
- (a)
- Glycolytic blockade: NAD+ shortage arrests GAPDH, blocking glycolysis — the primary source of ATP for the cancer cell.
- (b)
- Blockade of mitochondrial substrate level phosphorylation (mSLP): the alpha-ketoglutarate dehydrogenase reaction, which converts alpha-ketoglutarate to succinyl-CoA in the glutaminolysis pathway, requires NAD+ as an electron acceptor. The depletion of NAD+ caused by NADH accumulation blocks this reaction, cutting off the substrate supply to succinyl-CoA ligase and halting mSLP-derived ATP production [42,43]. This means that the cancer cell cannot use glutamine as an alternative energy source to bypass the glycolytic blockade.
- (c)
- Metabolic congestion: NADH excess allosterically inhibits key Krebs cycle enzymes (isocitrate dehydrogenase, alpha-ketoglutarate dehydrogenase), halting intermediary metabolism.
- (d)
- Paradoxical ROS generation: excess electrons leak from the saturated and dysfunctional respiratory chain, generating superoxide that the cancer cell — already with antioxidant systems at their limit — cannot neutralize.
- (e)
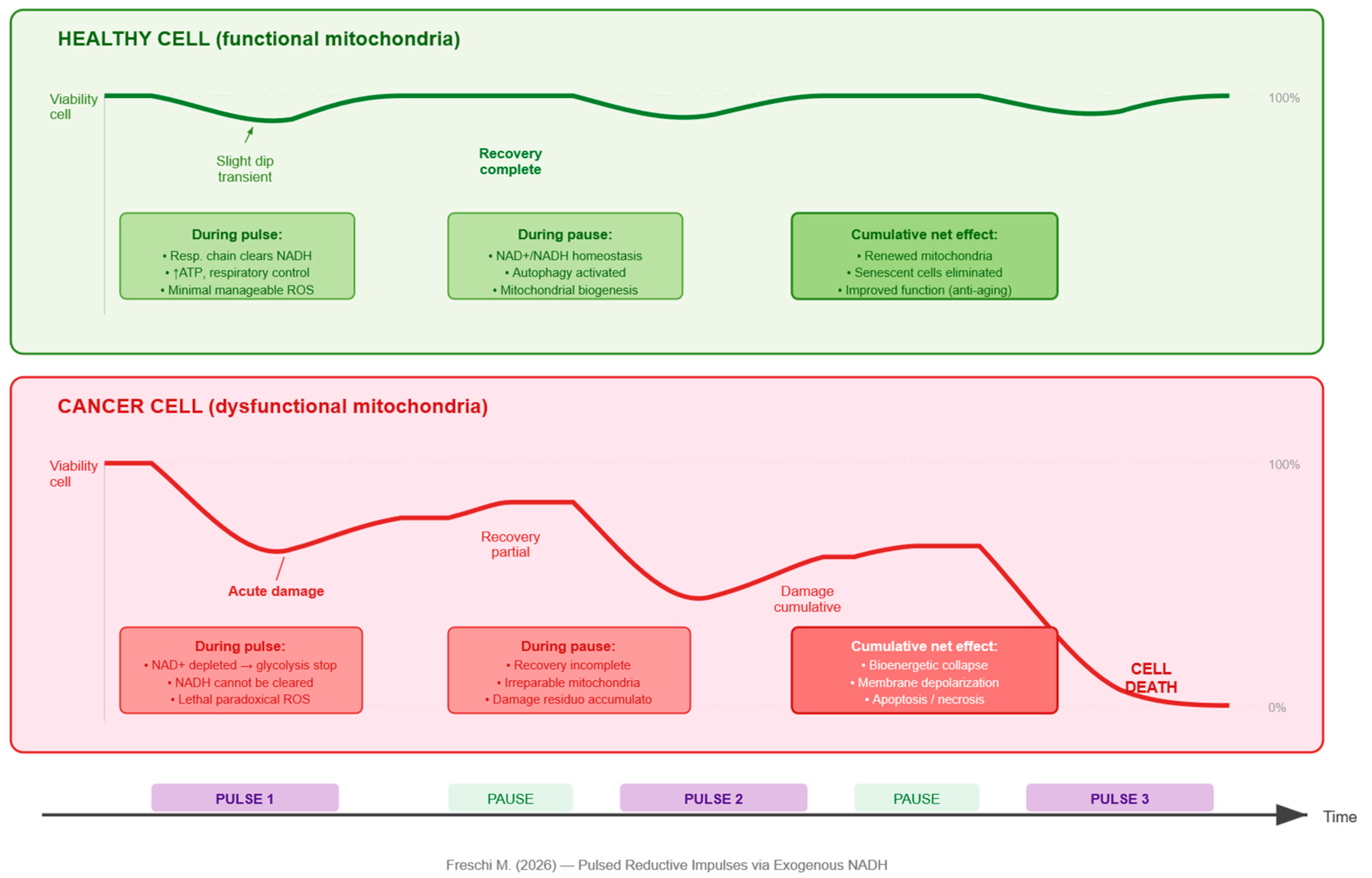
- Bioenergetic collapse: without ATP from glycolysis, without functional oxidative phosphorylation, and without mSLP from glutaminolysis, the cancer cell undergoes a total energy crisis with consequent plasma membrane depolarization and activation of cell death pathways. The cancer cell is thus subjected to a simultaneous blockade of all three known ATP-generating pathways.
5.2. Press-Pulse Logic Applied to Redox State
5.3. Synergy with Glucose Restriction
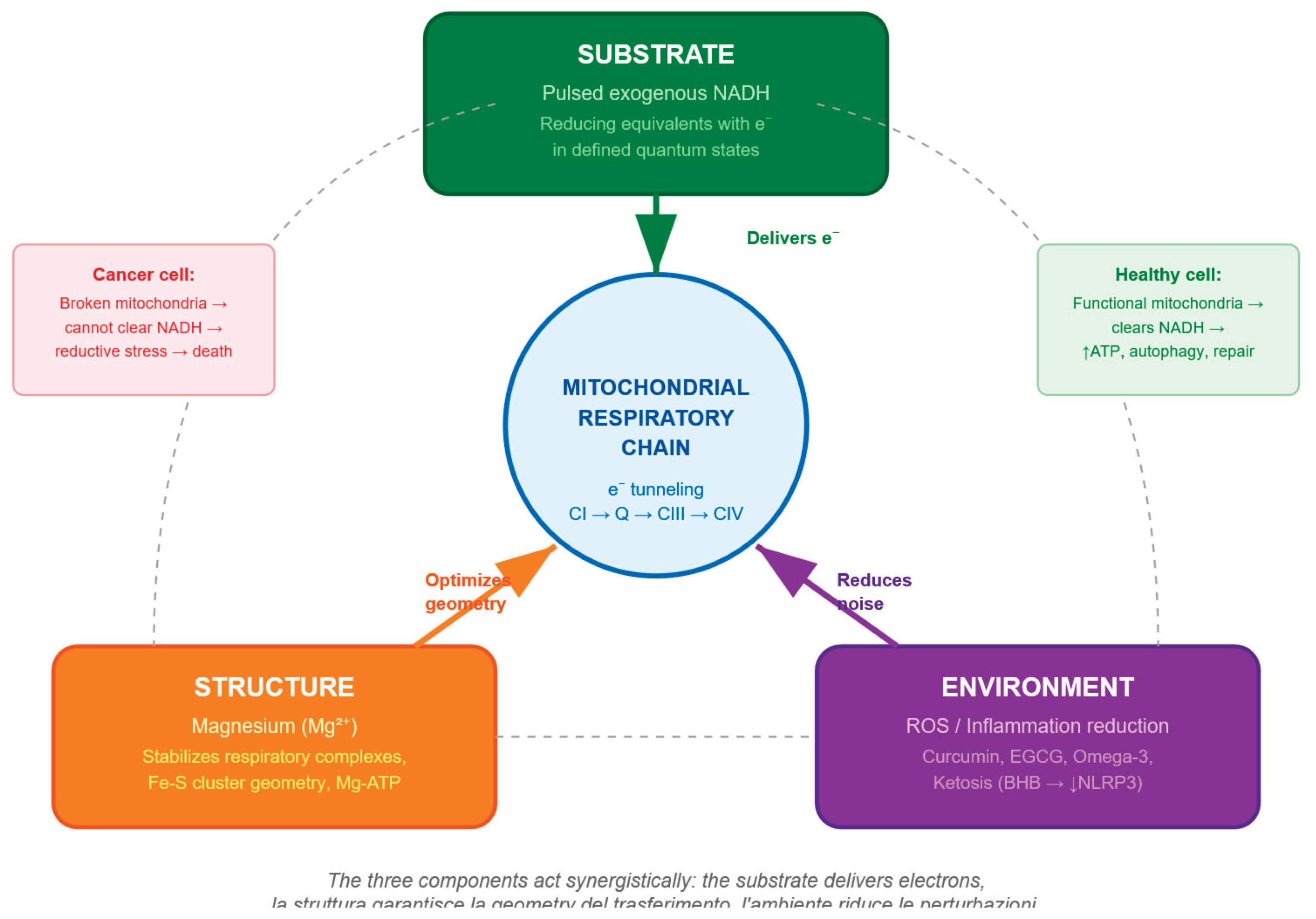
5.4. The Therapeutic Triad: Substrate, Structure, Environment
5.5. Dual-Compartment Rationale: Extracellular Blockade and Intracellular Stress
6. Proposed Experimental Protocol
6.1. Preclinical In Vitro Phase
- (a)
- Cell cultures of tumor lines (e.g., PC-3, LNCaP for prostate; HeLa; MCF-7 for breast) and healthy lines (e.g., RWPE-1 for prostate; MCF-10A for breast) exposed to increasing concentrations of exogenous NADH (0.1–10 mM) for variable durations (1–8 hours), followed by recovery periods in standard medium.
- (b)
- Primary endpoints: cell viability (MTT, trypan blue), intracellular NAD+/NADH ratio (enzymatic assays or NADH fluorescence), lactate production (indicator of glycolytic flux), ATP levels, ROS generation (DCFDA probe), mitochondrial membrane potential (JC-1).
- (c)
- Experimental groups: pulsed NADH (2h exposure + 22h recovery, repeated for 5 cycles) vs continuous NADH (same total dose distributed over 120h) vs control. This comparison is critical to validate the superiority of the pulse logic.
- (d)
- Combination: repeat the experiments in glucose-free medium (ketosis/fasting simulation) to verify the synergistic effect of glucose depletion and NADH overload.
6.2. Modalities for Reducing Equivalent Delivery
6.3. Pulse Protocol Parameters (Preliminary Clinical Proposal)
- • Pulse duration: 2–4 hours of slow intravenous infusion
- • Frequency: 2–3 sessions per week during intensive cycles
- • Cycle duration: 2–3 weeks
- • Inter-cycle pause: 4–6 weeks
- • Metabolic combination: sessions should ideally be conducted during fasting periods (≥16 hours) to maximize the metabolic vulnerability of cancer cells
- • Supplementation: magnesium glycinate/citrate (400–800 mg/day), reduced CoQ10 (ubiquinol, 200–400 mg/day)
- • Mandatory monitoring: plasma NAD+/NADH ratio, blood lactate, blood glucose, ketones, continuous ECG during infusion, electrolytes (Na+, K+, Mg²⁺), inflammatory markers (CRP, IL-6), complete blood count
6.4. Safety Criteria
- • Cardiac risk: acute alterations of the NAD+/NADH ratio may affect cardiomyocyte membrane potential. Continuous ECG monitoring during infusion is mandatory.
- • Metabolic risk: an excessive infusion rate could cause paradoxical lactic acidosis or excessively activate respiratory control, reducing ATP production in healthy cells. Gradual dose titration is recommended.
- • Electrolyte risk: reductive stress could transiently affect the Na+/K+-ATPase pump. Monitoring of electrolytes before, during, and after infusion is essential.
7. Anti-Cancer and Anti-Aging Convergence
7.1. Shared Mechanisms
7.2. The Nocturnal Window as a Physiological Reductive Impulse
7.3. Integrated Preventive Protocol
8. Limitations and Future Directions
8.1. Limitations of the Present Hypothesis
- (a)
- Absence of specific clinical data: no clinical trials exist that test pulsed NADH administration with the metabolic selectivity rationale described here. The experiences of the Hyperthermia Centre Hannover [7] and Birkmayer [8] use NADH in a different therapeutic framework (general support) without press-pulse logic.
- (b)
- Pharmacokinetics of exogenous NADH: the intracellular bioavailability of intravenously administered NADH is not fully characterized. NADH could be metabolized in plasma before reaching target cells. Dedicated pharmacokinetic studies are necessary.
- (c)
- Tumor heterogeneity: not all tumors exhibit the same degree of mitochondrial dysfunction. Tumors with partially preserved oxidative phosphorylation might better tolerate the reductive impulse. Patient selection based on metabolic imaging (FDG-PET, as an indicator of the Warburg effect) could improve selectivity.
- (d)
- Therapeutic window: the distance between the dose effective against cancer cells and the dose toxic to healthy cells — considering the respiratory control mechanism that also limits the clearance capacity of healthy cells — could be narrow. Only preclinical experimentation can define this window.
- (e)
- Interaction with conventional therapies: the effect of the reductive impulse on cells treated with chemotherapy, radiotherapy, or immunotherapy is unknown and requires specific study. Of particular interest would be the combination with PARP inhibitors (e.g., olaparib), which deplete intracellular NAD+ through a complementary mechanism.
- (f)
- Need for structural turnover: the administration of exogenous reducing equivalents does not repair damaged respiratory complexes. Its effect is to bypass metabolic bottlenecks and, through cyclic impulses, to stimulate the mitophagy and mitochondrial biogenesis that replace structurally compromised components.
8.2. Future Directions
- (a)
- Preclinical in vitro studies with the protocol described in Section 6.1 to validate the selectivity of the reductive impulse, with specific measurement of the simultaneous blockade of glycolysis, OxPhos, and mSLP.
- (b)
- Development of NADH formulations in liposomes or nanoparticles to improve intracellular delivery.
- (c)
- Combined study of pulsed NADH + fasting + PARP inhibitors to maximize NAD+ depletion in cancer cells through complementary mechanisms.
- (d)
- Experimental validation of the dual-compartment redox blockade concept: systematic comparison of extracellular-only perturbation (NADH) versus combined extracellular + intracellular perturbation using agents with different membrane permeability profiles, to determine whether dual-compartment approaches enhance selectivity and efficacy.
- (e)
- Quantum biology studies (see Appendix) to characterize the quantum states of electrons in exogenous vs endogenous NADH and their functional relevance.
- (f)
- Development of predictive response biomarkers based on tumor metabolic profile (NAD+/NADH ratio, complex I expression, LDH activity, succinate export as indicator of mSLP dependence).
- (g)
- Comparative evaluation of different modalities for exogenous reducing equivalent delivery (NADH, ubiquinol, H₂, and future catalytic redox vehicles) within the press-pulse protocol, with attention to the coherence of the quantum states of the delivered electrons.
- (h)
- Investigation of the potential immunometabolic effects of reductive impulses on tumor-associated macrophage polarization and T lymphocyte function in the tumor microenvironment.
9. Conclusions
Funding
Acknowledgments
Conflict of interest
AI Disclosure
Appendix A. Quantum Biology Perspectives
A.1. Preamble
A.2. Quantum Tunneling in the Respiratory Chain
A.3. Quantum coherence in biological systems
A.4. Quantum States of Electrons in Exogenous vs Endogenous Reducing Equivalents
A.5. Decoherence as a Component of Aging
A.6. Experimental Verification
- (a)
- Pulsed EPR spectroscopy and ENDOR: to compare the spin states and relaxation times (T1, T2) of electrons in fresh synthetic NADH vs NADH extracted from young tissues vs NADH extracted from aged tissues.
- (b)
- High-resolution oximetry (Oroboros O2k): to measure respiratory chain efficiency in mitochondria isolated from young vs aged tissues, before and after incubation with exogenous NADH.
- (c)
- Time-resolved fluorescence spectroscopy: to characterize the dynamics of enzyme-bound NADH in different age and pathology contexts.
References
- Warburg, O. On the origin of cancer cells. Science 1956, 123(3191), 309–314. [Google Scholar] [CrossRef]
- Seyfried, TN. Cancer as a Metabolic Disease: On the Origin, Management, and Prevention of Cancer; Wiley: Hoboken, NJ, 2012. [Google Scholar]
- López-Otín, C; Blasco, MA; Partridge, L; Serrano, M; Kroemer, G. Hallmarks of aging: An expanding universe. Cell. 2023, 186(2), 243–278. [Google Scholar] [CrossRef]
- Massudi, H; Grant, R; Braidy, N; et al. Age-associated changes in oxidative stress and NAD+ metabolism in human tissue. PLoS One 2012, 7(7), e42357. [Google Scholar] [CrossRef]
- Grant, R; Berg, J; Mestayer, R; et al. A pilot study investigating changes in the human plasma and urine NAD+ metabolome during a 6 hour intravenous infusion of NAD+. Front Aging Neurosci. 2019, 11, 257. [Google Scholar] [CrossRef] [PubMed]
- Yaku, K; Okabe, K; Hikosaka, K; Nakagawa, T. NAD metabolism in cancer therapeutics. Front Oncol. 2018, 8, 622. [Google Scholar] [CrossRef] [PubMed]
- Hyperthermia Centre Hannover. NADH Infusions — Cancer treatment and therapy. 2026.
- Birkmayer, JGD; Vrecko, C; Volc, D; Birkmayer, W. Nicotinamide adenine dinucleotide (NADH) — a new therapeutic approach to Parkinson’s disease. Comparison of oral and parenteral application. Acta Neurol Scand Suppl. 1993, 146, 32–35. [Google Scholar] [CrossRef] [PubMed]
- Seyfried, TN; Yu, G; Maroon, JC; D’Agostino, DP. Press-pulse: a novel therapeutic strategy for the metabolic management of cancer. Nutr Metab. 2017, 14, 19. [Google Scholar] [CrossRef]
- Vander Heiden, MG; Cantley, LC; Thompson, CB. Understanding the Warburg effect: the metabolic requirements of cell proliferation. Science 2009, 324(5930), 1029–1033. [Google Scholar] [CrossRef]
- Verdin, E. NAD+ in aging, metabolism, and neurodegeneration. Science 2015, 350(6265), 1208–1213. [Google Scholar] [CrossRef]
- Lucena-Cacace, A; Otero-Albiol, D; Jimenez-Garcia, MP; et al. NAMPT overexpression induces cancer stemness and defines a novel tumor signature for glioma prognosis. Oncotarget 2017, 8, 99514–99530. [Google Scholar] [CrossRef]
- Hasmann, M; Schemainda, I. FK866, a highly specific noncompetitive inhibitor of nicotinamide phosphoribosyltransferase, represents a novel mechanism for induction of tumor cell apoptosis. Cancer Res. 2003, 63(21), 7436–7442. [Google Scholar] [PubMed]
- Sabharwal, SS; Schumacker, PT. Mitochondrial ROS in cancer: initiators, amplifiers or an Achilles’ heel? Nat Rev Cancer 2014, 14(11), 709–721. [Google Scholar] [CrossRef] [PubMed]
- Mantovani, A; Allavena, P; Sica, A; Balkwill, F. Cancer-related inflammation. Nature 2008, 454(7203), 436–444. [Google Scholar] [CrossRef] [PubMed]
- Morré, DJ; Morré, DM. ECTO-NOX proteins: growth, cancer, and aging; Springer: New York, 2013. [Google Scholar]
- Lewerenz, J; Hewett, SJ; Huang, Y; et al. The cystine/glutamate antiporter system xc- in health and disease. Antioxid Redox Signal. 2013, 18(5), 522–555. [Google Scholar] [CrossRef]
- Paulsen, CE; Carroll, KS. Cysteine-mediated redox signaling: chemistry, biology, and tools for discovery. Chem Rev. 2013, 113(7), 4633–4679. [Google Scholar] [CrossRef]
- Bienert, GP; Schjoerring, JK; Jahn, TP. Membrane transport of hydrogen peroxide. Biochim Biophys Acta 2006, 1758(8), 994–1003. [Google Scholar] [CrossRef]
- Halestrap, AP; Wilson, MC. The monocarboxylate transporter family — role and regulation. IUBMB Life 2012, 64(2), 109–119. [Google Scholar] [CrossRef]
- Aasen, T; Mesnil, M; Naus, CC; et al. Gap junctions and cancer: communicating for 50 years. Nat Rev Cancer 2016, 16(12), 775–788. [Google Scholar] [CrossRef]
- Xiao, W; Bhatt, SR; Bhatt, DP. Reductive stress and the pathogenesis of human disease. FASEB J. 2020, 34(1), 87–103. [Google Scholar]
- Aon, MA; Cortassa, S; O’Rourke, B. Redox-optimized ROS balance: a unifying hypothesis. Biochim Biophys Acta 2010, 1797(6-7), 865–877. [Google Scholar] [CrossRef]
- Halliwell, B. The antioxidant paradox: less paradoxical now? Br J Clin Pharmacol. 2013, 75(3), 637–644. [Google Scholar] [CrossRef] [PubMed]
- Carr, AC; Frei, B. Toward a new recommended dietary allowance for vitamin C based on antioxidant and health effects in humans. Am J Clin Nutr. 1999, 69(6), 1086–1107. [Google Scholar] [CrossRef] [PubMed]
- Traber, MG; Atkinson, J. Vitamin E, antioxidant and nothing more. Free Radic Biol Med. 2007, 43(1), 4–15. [Google Scholar] [CrossRef] [PubMed]
- The Alpha-Tocopherol, Beta Carotene Cancer Prevention Study Group. The effect of vitamin E and beta carotene on the incidence of lung cancer and other cancers in male smokers. N Engl J Med. 1994, 330(15), 1029–1035. [CrossRef]
- Klein, EA; Thompson, IM, Jr.; Tangen, CM; et al. Vitamin E and the risk of prostate cancer: the Selenium and Vitamin E Cancer Prevention Trial (SELECT). JAMA 2011, 306(14), 1549–1556. [Google Scholar] [CrossRef]
- Murphy, MP; Smith, RAJ. Targeting antioxidants to mitochondria by conjugation to lipophilic cations. Annu Rev Pharmacol Toxicol. 2007, 47, 629–656. [Google Scholar] [CrossRef]
- Skulachev, VP. An attempt to prevent senescence: a mitochondrial approach. Biochim Biophys Acta 2009, 1787(5), 437–461. [Google Scholar] [CrossRef]
- Chance, B; Williams, GR. Respiratory enzymes in oxidative phosphorylation. III. The steady state. J Biol Chem. 1955, 217(1), 409–427. [Google Scholar] [CrossRef]
- Joiner, MC; van der Kogel, AJ. Basic Clinical Radiobiology, 5th ed.; CRC Press, 2018. [Google Scholar]
- de Baaij, JHF; Hoenderop, JGJ; Bindels, RJM. Magnesium in man: implications for health and disease. Physiol Rev. 2015, 95(1), 1–46. [Google Scholar] [CrossRef]
- Ohsumi, Y. Historical landmarks of autophagy research. Cell Res. 2014, 24(1), 9–23. [Google Scholar] [CrossRef]
- Youle, RJ; Narendra, DP. Mechanisms of mitophagy. Nat Rev Mol Cell Biol. 2011, 12(1), 9–14. [Google Scholar] [CrossRef] [PubMed]
- Hardie, DG; Ross, FA; Hawley, SA. AMPK: a nutrient and energy sensor that maintains energy homeostasis. Nat Rev Mol Cell Biol. 2012, 13(4), 251–262. [Google Scholar] [CrossRef] [PubMed]
- Campisi, J. Aging, cellular senescence, and cancer. Annu Rev Physiol. 2013, 75, 685–705. [Google Scholar] [CrossRef] [PubMed]
- Youm, YH; Nguyen, KY; Grant, RW; et al. The ketone metabolite β-hydroxybutyrate blocks NLRP3 inflammasome-mediated inflammatory disease. Nat Med. 2015, 21(3), 263–269. [Google Scholar] [CrossRef]
- Moser, CC; Keske, JM; Warncke, K; Farid, RS; Dutton, PL. Nature of biological electron transfer. Nature 1992, 355(6363), 796–802. [Google Scholar] [CrossRef]
- Marcus, RA; Sutin, N. Electron transfers in chemistry and biology. Biochim Biophys Acta 1985, 811(3), 265–322. [Google Scholar] [CrossRef]
- Engel, GS; Calhoun, TR; Read, EL; et al. Evidence for wavelike energy transfer through quantum coherence in photosynthetic systems. Nature 2007, 446(7137), 782–786. [Google Scholar] [CrossRef]
- Seyfried, TN; Lee, DC; Duraj, T; et al. The Warburg hypothesis and the emergence of the mitochondrial metabolic theory of cancer. J Bioenerg Biomembr. 2025. [Google Scholar] [CrossRef]
- Lee, DC; Ta, L; Mukherjee, P; et al. Amino acid and glucose fermentation maintain ATP content in mouse and human malignant glioma cells. ASN Neuro 2024, 16(1), 2422268. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



