Submitted:
31 March 2026
Posted:
01 April 2026
You are already at the latest version
Abstract
Background: Motivational Interviewing (MI) is a behavioral approach widely used to improve oral health among adolescents. The integration of face-to-face MI with mobile application support has the potential to overcome limitations related to time and accessibility in conventional care. Objective: This study aimed to evaluate the effect of a combined MI intervention (face-to-face and app-based) on oral hygiene status, knowledge, and tooth-brushing behavior among adolescents. Methods: A randomized controlled trial (RCT) with a parallel-group design was conducted among 100 adolescents aged 13–15 years, who were randomly assigned to an intervention group receiving combined MI (face-to-face and app-based) and a control group receiving conventional face-to-face MI. The intervention was implemented over four months following structured MI stages, with assessments conducted at baseline and three follow-up points. Oral hygiene status was measured using the Oral Hygiene Index Simplified (OHI-S). Data were analyzed using Wilcoxon, Mann–Whitney, and effect sizes were calculated to assess the magnitude of change. Results: The intervention group demonstrated a significantly greater reduction in OHI-S scores compared with the control group. The mean OHI-S score decreased from 3.19 ± 1.16 to 1.37 ± 1.06 (p < 0.001), indicating a large effect size. Conclusion: The combined MI intervention resulted in greater improvements in adolescents’ oral hygiene status compared with conventional MI. These findings highlight the potential of a hybrid MI approach as an effective strategy for adolescent oral health promotion; however, causal interpretations should be made with caution.
Keywords:
1. Introduction
2. Materials and Methods

3. Results
3.1. Feasibility and Usability of the Motivational Interviewing (MI) During Application
| Media Quality | Agree (%) (n=100) |
Don’t agree (%) (n=10) |
|---|---|---|
| Accessible | ||
|
90 (90%) | 10 (10%) |
|
95(95%) | 5 (5%) |
|
3(3%) | 97 (97%) |
| Acceptance / Usability | ||
|
10 (100%) | 90 (90%) |
|
89 (89%) | 11 (11%) |
|
97 (97%) | 3 (3%) |
| Effectiveness | ||
|
100 (100%) | 0 (0%) |
|
2 (2%) | 98 (98%) |
|
92 (92%) | 8 (8%) |
|
90 (90%) | 10 (10%) |
| Efficiency | ||
|
96 (96%) | 4 (40%) |
|
100 (100%) | 0 (0%) |
| Appropriateness / Suitability | ||
| Do you think the MI application is useful as a supporting tool in managing your oral health problems? | 92 (92%) | 8 (8%) |
3.2. Effect of Combined Motivational Interviewing on Knowledge
| Variables | Mean ± SD | ||
|---|---|---|---|
| Group Intervention (given by MI) |
Group Control (without MI) |
||
| Knowledge | Pre-Test | 3.56±1.44 | 4.96±1.44 |
| Post Test 1 | 5.50±0.90 | 6.58±1.41 | |
| Post Test 2 | 6.32±1.15 | ||
| Post Test 3 | 7.40±1.27 | ||
| Mean Difference | 3.84±0.17 | 1.62±0.03 | |
| Z | -6.146 | -5,003 | |
| p -value | 0.000 | 0.003 | |
| Effect Size (r) | 0.87 | 0.71 | |
| 95% CI | 0.60; 1.00 | 0.44; 0.98 | |
3.3. Effect of Combined Motivational Interviewing on Tooth Brushing Behavior (TBP)
| Variables | Mean ± SD | ||
|---|---|---|---|
| Group Intervention (given MI) |
Group Control (without MI) |
||
| Tooth brushing behavior | Pre-Test | 10.18±2.16 | 12.14±1.92 |
| Post Test 1 | 11.20±2.05 | 13.40±2.82 | |
| Post Test 2 | 13.08±2.43 | ||
| Post Test 3 | 15.36±2.66 | ||
| Mean Difference | 5.18±0.5 | 1.26±0.9 | |
| Z | -6,168 | -3.160 | |
| Nilai p | 0.000* | 0.003** | |
| Effect Size (r) | 0.87 | 1.40 | |
| 95% CI | (0.60 – 1.00) | (0.30 – 0.84) | |
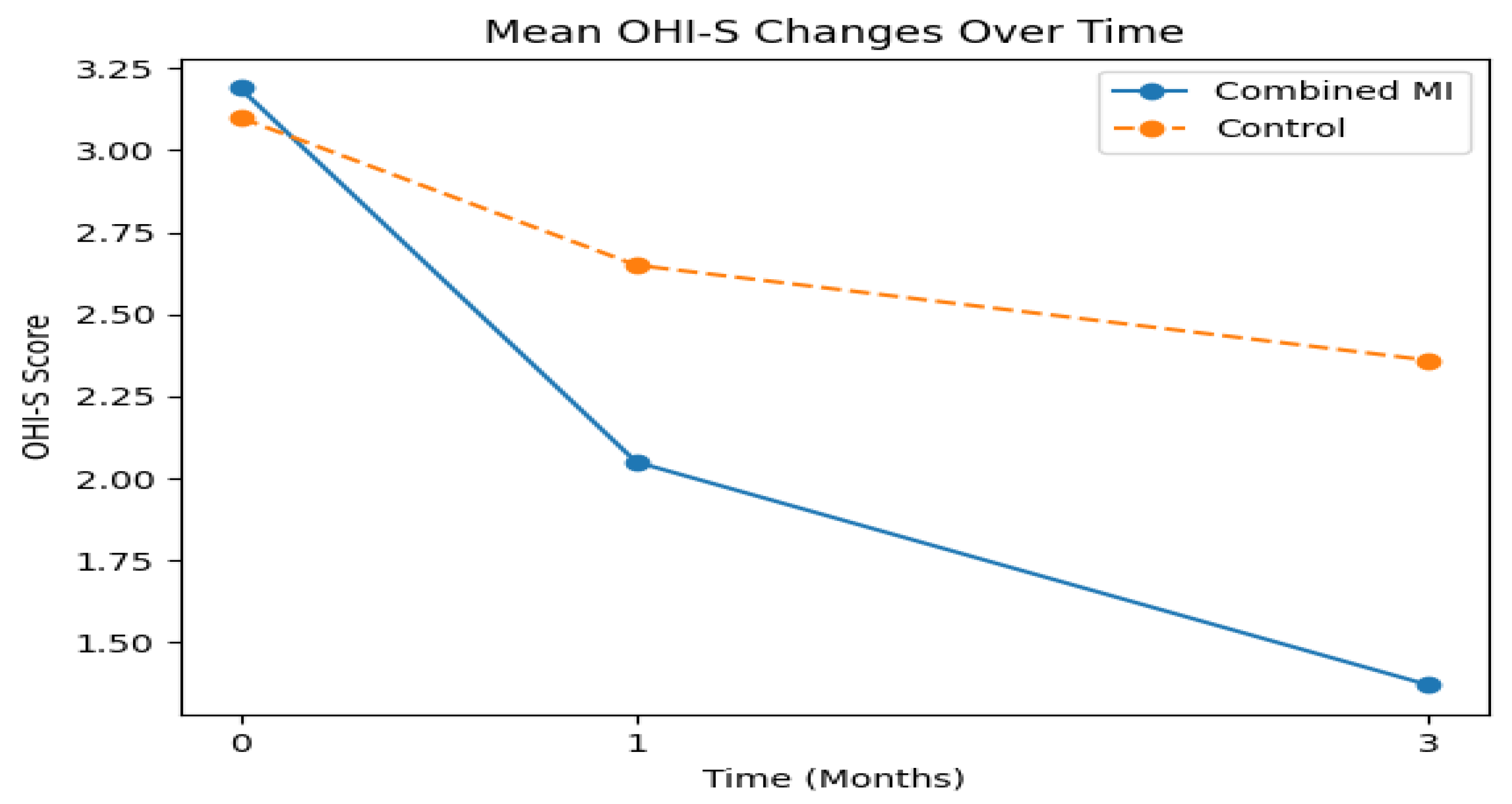
3.4. Effect of Combined Motivational Interviewing on Oral Hygiene Status (OHI-S)
| Variables | Mean ± SD | ||
|---|---|---|---|
| Group Intervention (without MI) | Group Control (without MI) |
||
| OHI-S Status | Pre-Test | 3.19±1.16 | 2.74±1.48 |
| Post Test 1 | 2.62±1.00 | 2.00±1.19 | |
| Post Test 2 | 1.87±1.01 | ||
| Post Test 3 | 1.37±1.06 | ||
| Mean Difference | -1.82±0.1 | -0.74±0.29 | |
| Z | -6,038 | -3,483 | |
| p -value | 0.000 | 0.000 | |
| Effect Size (r) | 0.85 | 0.49 | |
| 95% CI | (0.58 – 1.00) | (0.22 – 0.76) | |
| Variable | Group | Baseline (Mean ± SD) | p-Value | 1 Month (Mean ± SD) | p-Value | r | 3 Months (Mean ± SD) | p-Value | r |
|---|---|---|---|---|---|---|---|---|---|
|
Knowldge ± SD |
Intervention (n=50) | 3.56 ± 1.44 | 0.812† | 5.98 ± 1.30 | 0.021*δ | 0.21 | 7.40 ± 1.27 | 0.000*δ | 0.61 |
| Control (n=50) | 3.60 ± 1.38 | 4.85 ± 1.25 | 5.22 ± 1.35 | ||||||
| TBP ± SD | Intervention (n=50) | 10.18 ± 2.16 | 0.765† | 13.72 ± 2.40 | 0.018*δ | 0.20 | 15.36 ± 2.66 | 0.000*δ | 0.62 |
| Control (n=50) | 10.05 ± 2.20 | 10.92 ± 2.30 | 11.31 ± 2.45 | ||||||
| OHI-S ± SD | Intervention (n=50) | 3.19 ± 1.16 | 0.842† | 2.05 ± 1.10 | 0.032*δ | 0.20 | 1.37 ± 1.06 | 0.000*δ | 0.60 |
| Control (n=50) | 3.10 ± 1.20 | 2.65 ± 1.15 | 2.36 ± 1.18 |
4. Discussion
4.1. Implementation of Combined Motivational Interviewing
4.2. Effect of Combined Motivational Interviewing on Adolescent Oral Hygiene Status
4.2. Effect of Combined Motivational Interviewing on Tooth Brushing Practice (TBP)
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| OHI-S | Oral Hygiene Index Status |
| MI | Motivational Interview |
References
- Santoso, CMA; Bramantoro, T; Nguyen, MC; Nagy, A. Lifestyle and psychosocial correlates of oral hygiene practice among Indonesian adolescents. Eur J Oral Sci 2021, 129(1). [Google Scholar] [CrossRef]
- Ferizi, L; Bimbashi, V; Kelmendi, K. Dental Caries Prevalence and Oral Health Status among 15-Year- Old Adolescents in Kosovo. Acta Stomatol Croat 2022, 56(1), 42–9. [Google Scholar] [CrossRef] [PubMed]
- Lawal, FB; Fagbule, OF; Akinloye, SJ; Lawal, TA; Oke, GA. Impact of oral hygiene habits on oral health-related quality of life of in-school adolescents in Ibadan, Nigeria. Frontiers in Oral Health 2022, 3. [Google Scholar] [CrossRef] [PubMed]
- Borji-Navan, S; Maleki, N; Keramat, A. Efficacy of Digital Health Interventions Used for Adolescent’s Sexual Health: An Umbrella Review. Health Sci Rep. 2024, 7(12). [Google Scholar] [CrossRef] [PubMed]
- Lehtimaki, S; Martic, J; Wahl, B; Foster, KT; Schwalbe, N. Evidence on Digital Mental Health Interventions for Adolescents and Young People: Systematic Overview. JMIR Ment Health 2021, 8(4), e25847. [Google Scholar] [CrossRef]
- Naef, AN; Fischbock, N; Tezcan-Güntekin, H; Amelung, VE. Adolescents with type 1 diabetes’ perspectives on digital health interventions to enhance health literacy: a qualitative study. Front Public Health 2024, 12. [Google Scholar] [CrossRef]
- Aiman, H; Kilgariff, JK; Marks, D; Albiston, M. Does motivational interviewing have a role in dentistry? Br Dent J 2025, 238(3), 166–71. [Google Scholar] [CrossRef]
- Gao, X; Lo, ECM; McGrath, C; Ho, SMY. Face-to-face individual counseling and online group motivational interviewing in improving oral health: study protocol for a randomized controlled trial. Trials 2015, 16(1), 416. [Google Scholar] [CrossRef]
- Basheer, N A; Jodalli, P; Gowdar, IM; Almalki, SA. Effectiveness of Motivational Interviewing and cross platform messaging application in improving oral health knowledge, attitude and behaviours among pregnant women- A Randomized Controlled Trial. F1000Res 2024, 13, 871. [Google Scholar] [CrossRef]
- Zhang, M; Lan, J; Zhang, T; Sun, W; Liu, P; Wang, Z. Oral health and caries/gingivitis-associated factors of adolescents aged 12–15 in Shandong province, China: a cross-sectional Oral Health Survey. BMC Oral Health 2021, 21(1), 288. [Google Scholar] [CrossRef]
- Barahona-Cubillo, JB; Rojas-Brenes, C; Sánchez-Achío, T; Stradi-Granados, S; Barboza-Solís, C. Prevalence of Tooth Loss, Bleeding on Probing and Malocclusion as Oral Disease Indicators in Costa Rican Male Adolescents: a Cross Sectional Study. Odovtos - International Journal of Dental Sciences 2022, 465–79. [Google Scholar] [CrossRef]
- Firmino, RT; Granville-Garcia, AF; Paiva, SM; de Campos, PH; Oliveira, AV; Diniz, MB. Shame from Smiling and Speaking Due to Oral Health Problems in Brazilian Adolescents: A Nationwide Population-Based Study. Pesqui Bras Odontopediatria Clin Integr 2022, 22. [Google Scholar] [CrossRef]
- Simangwa, LD; Åstrøm, AN; Johansson, A; Minja, IK; Johansson, AK. Oral diseases and oral health related behaviors in adolescents living in Maasai population areas of Tanzania: a cross-sectional study. BMC Pediatr 2019, 19(1), 275. [Google Scholar] [CrossRef]
- Su, S; Zhang, J; Deng, R; Wang, W; Cui, T; Su, Y; et al. Oral health status and associated factors among 12 to 15-year-old Chinese adolescents in Southeast China: A cross-sectional study. Medicine 2024, 103(4), e37080. [Google Scholar] [CrossRef]
- Galicia-Diez Barroso, D; Abeijón-Malvaez, LD; Moreno Altamirano, GA; Irigoyen-Camacho, MEJ; Finlayson, TL; Borges-Yáñez, SA. Using the Expanded Andersen Model to Determine Factors Associated with Mexican Adolescents’ Utilization of Dental Services. Healthcare 2023, 11(24), 3159. [Google Scholar] [CrossRef] [PubMed]
- Guzman, A; Landers, SE; Nechitilo, M; Garbers, S; Catallozzi, M; Gold, MA; et al. Acceptability of a Phone App-Based Motivational Interviewing Intervention for Young Men’s Health. J Technol Behav Sci. 2020, 5(3), 258–65. [Google Scholar] [CrossRef]
- Adams, Z; Grant, M; Hupp, S; Scott, T; Feagans, A; Phillips, ML; et al. Acceptability of an mHealth App for Youth With Substance Use and Mental Health Needs: Iterative, Mixed Methods Design. JMIR Form Res 2021, 5(12), e30268. [Google Scholar] [CrossRef] [PubMed]
- Kaskova, LF; Drozda, II; Soltys, OM; Kilmukhametova, YH. THE IMPACT OF PREVENTIVE MEASURES ON ORAL HYGIENE IN 15-YEAR-OLD ADOLESCENTS. Ukrainian Dental Almanac 2022, (3), 35–8. [Google Scholar] [CrossRef]
- Sessiz, R; Ayan, G; Sezer, B; Tosun, İ. Evaluation of oral health and dental hygiene habits in adolescents with intellectual and developmental disabilities: a longitudinal pilot study. Quintessence Int. PubMed. 2025, 56(5), 402–10. [Google Scholar] [CrossRef] [PubMed]
- Wu, L; Gao, X; Lo, ECM; Ho, SMY; McGrath, C; Wong, MCM. Motivational Interviewing to Promote Oral Health in Adolescents. Journal of Adolescent Health 2017, 61(3), 378–84. [Google Scholar] [CrossRef]
- Uguz, HN; Çiftçi, V; Dogan, MC. Effectiveness of motivational interviewing on oral healthcare in pediatric patients. Journal of Clinical Pediatric Dentistry 2023. [Google Scholar] [CrossRef]
- Zhou, X; Bambling, M; Bai, X; Smith, AC; Edirippulige, S. Exploring factors affecting Chinese adolescents’ perceived usefulness and engagement with a stress management app: a qualitative study. Front Psychol 2023, 14. [Google Scholar] [CrossRef] [PubMed]
- Yoon, S; Tang, H; Tan, CM; Phang, JK; Kwan, YH; Low, LL. Acceptability of Mobile App–Based Motivational Interviewing and Preferences for App Features to Support Self-Management in Patients With Type 2 Diabetes: Qualitative Study. JMIR Diabetes 2024, 9, e48310. [Google Scholar] [CrossRef] [PubMed]
- Jiang, S; McGrath, C; Lo, EC; Ho, SM; Gao, X. Motivational interviewing to prevent early childhood caries: A randomized controlled trial. J Dent. 2020, 97, 103349. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




