Submitted:
26 March 2026
Posted:
27 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. ASD Counts from DDS
2.2. Denominators for Prevalence Calculation: NCES Total School Populations
2.2.1. Method D1
2.2.2. Method D2
2.3. Estimation of the Changepoint in Prevalence
2.3.1. Method C1
2.3.2. Method C2
2.4. Socioeconomic Indices
3. Results
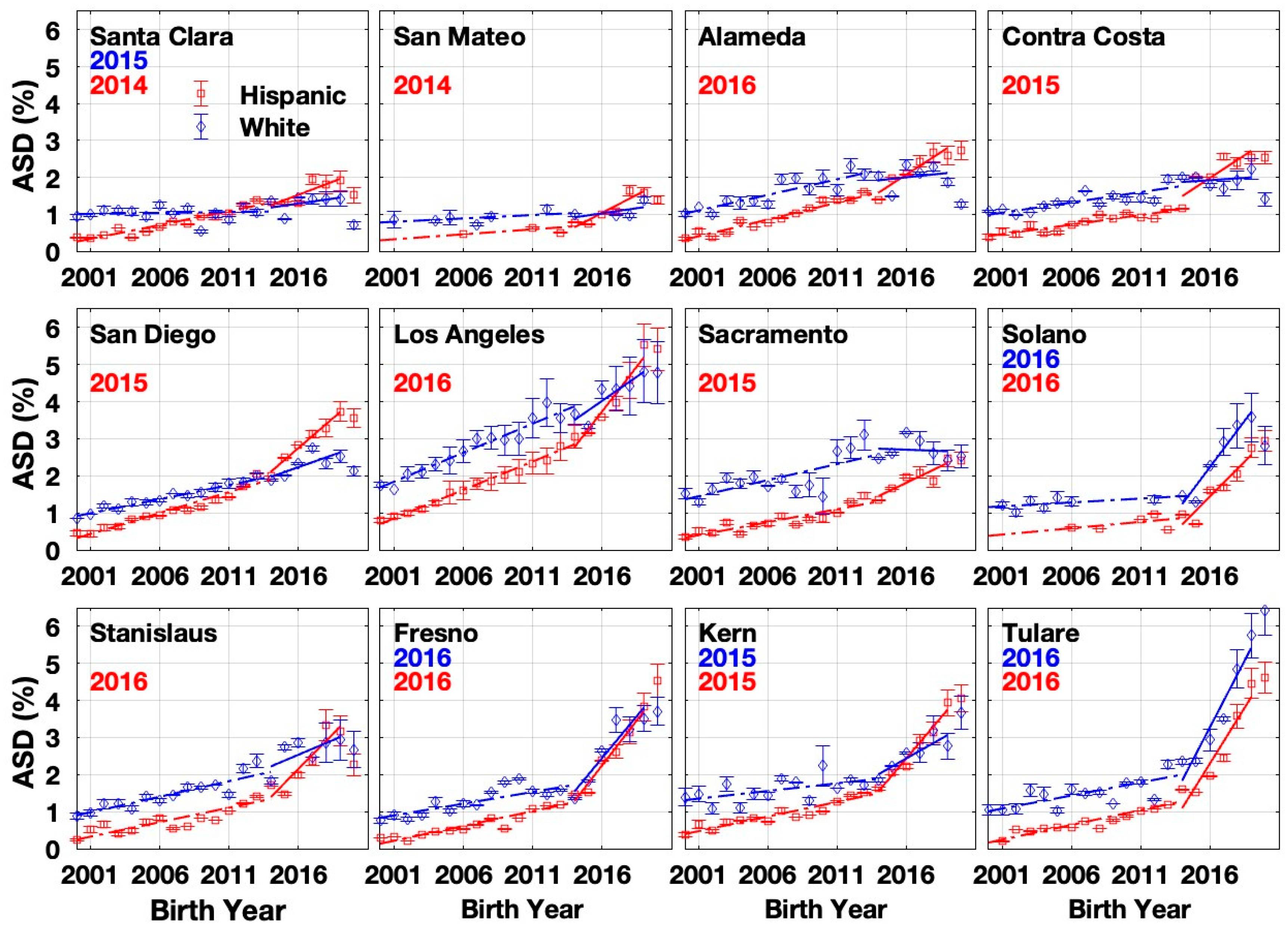
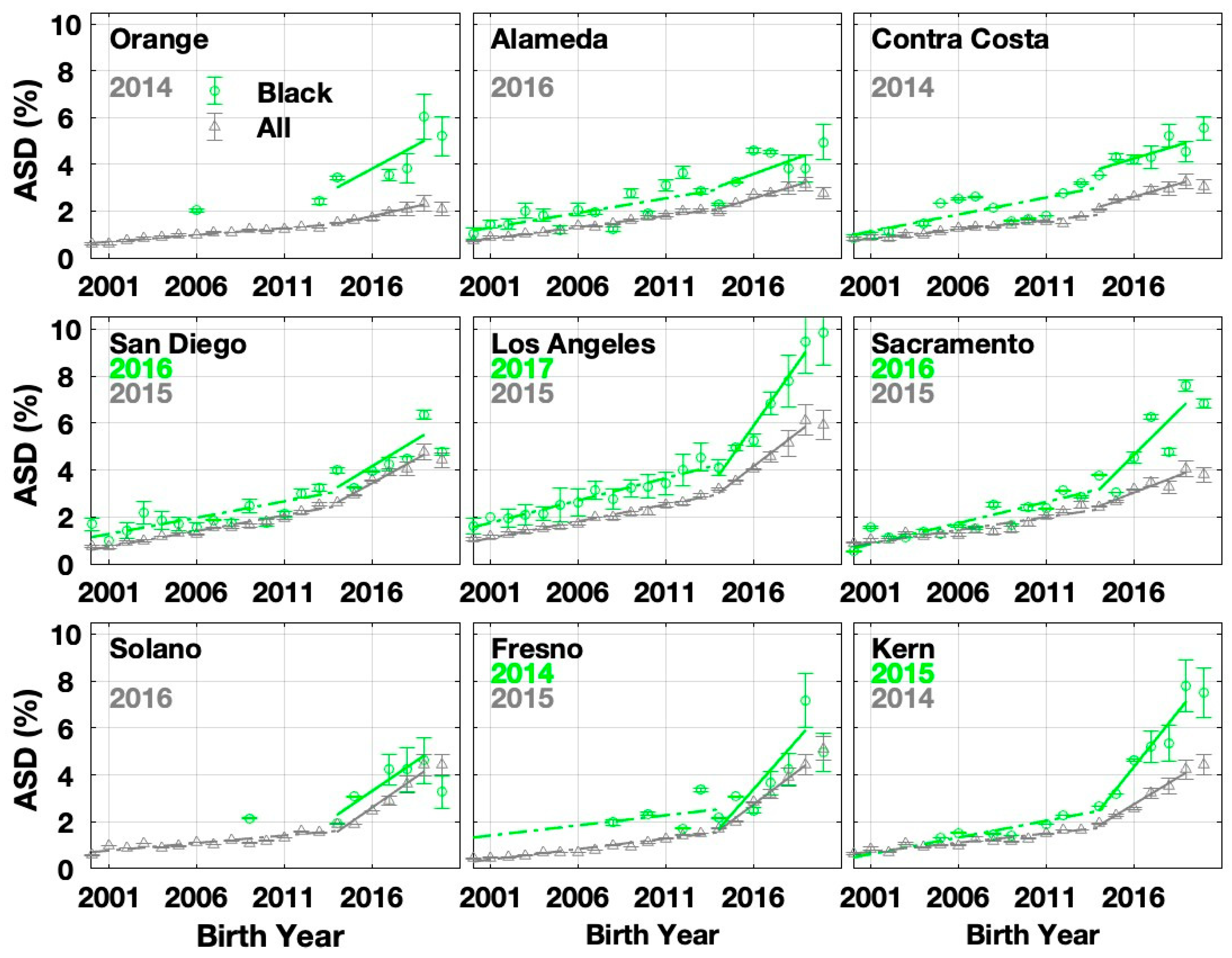
3.1. Autism Prevalence Trends by Race/Ethnicity and County
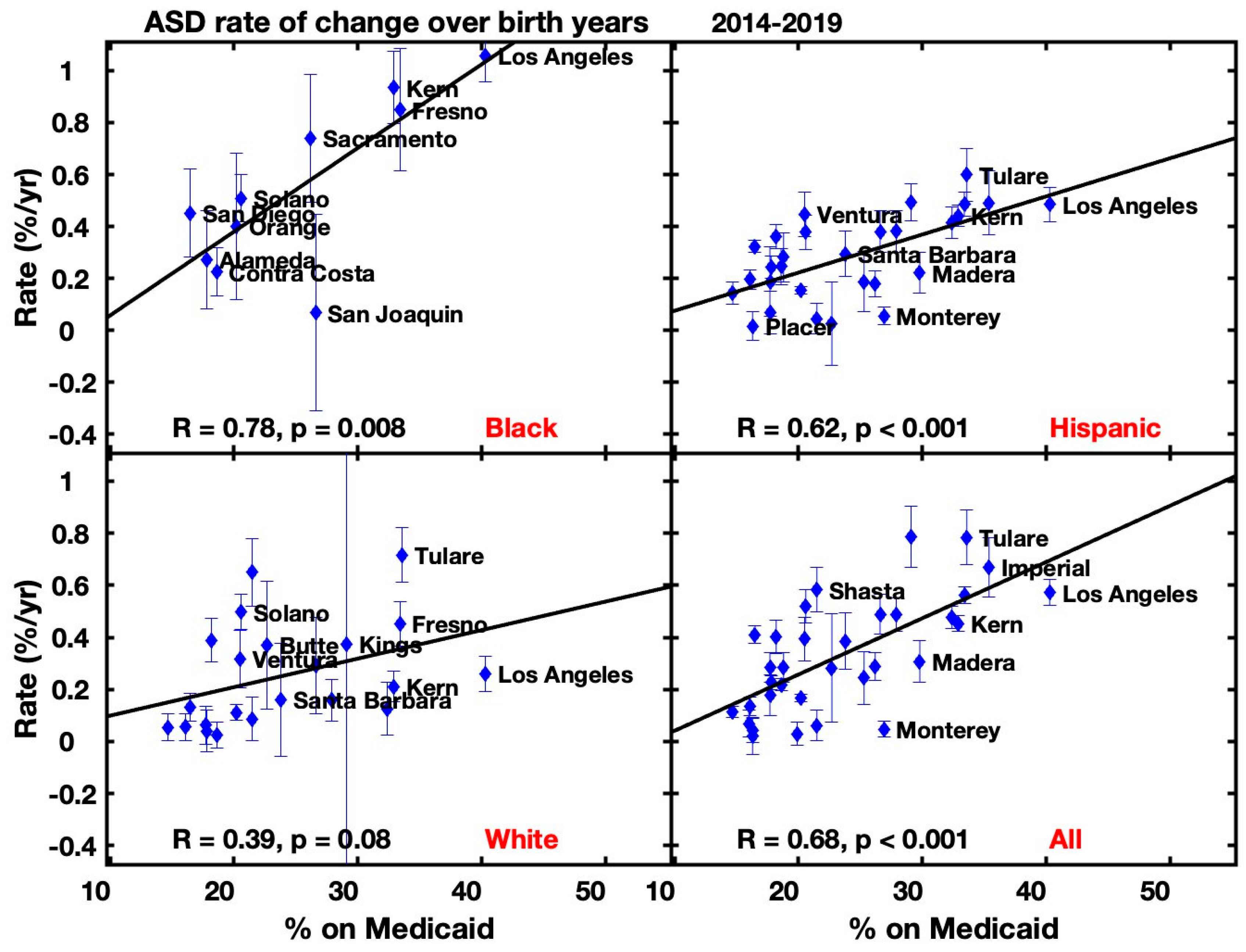
3.2. County-Level Correlations to Socioeconomic Indicators
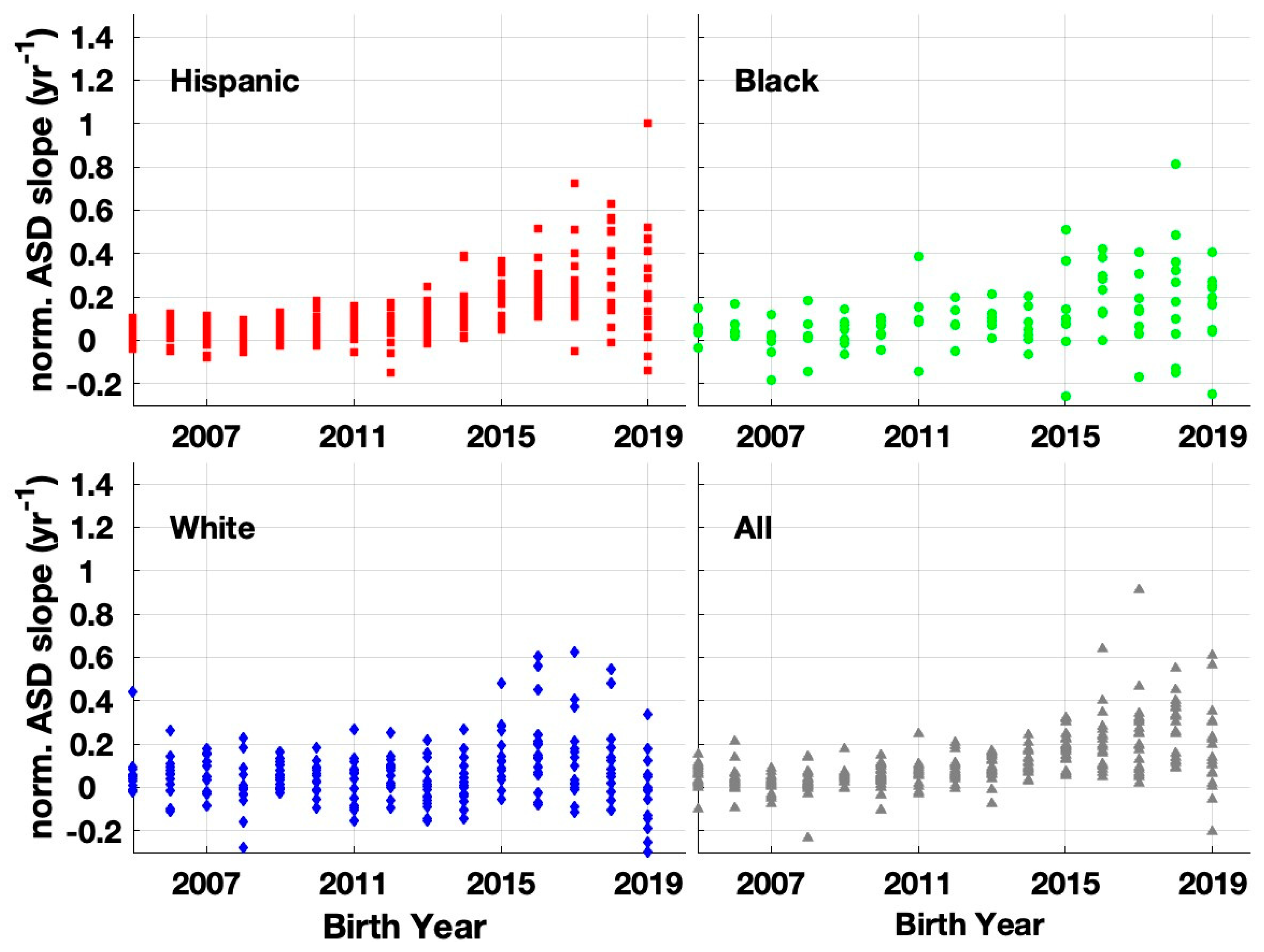
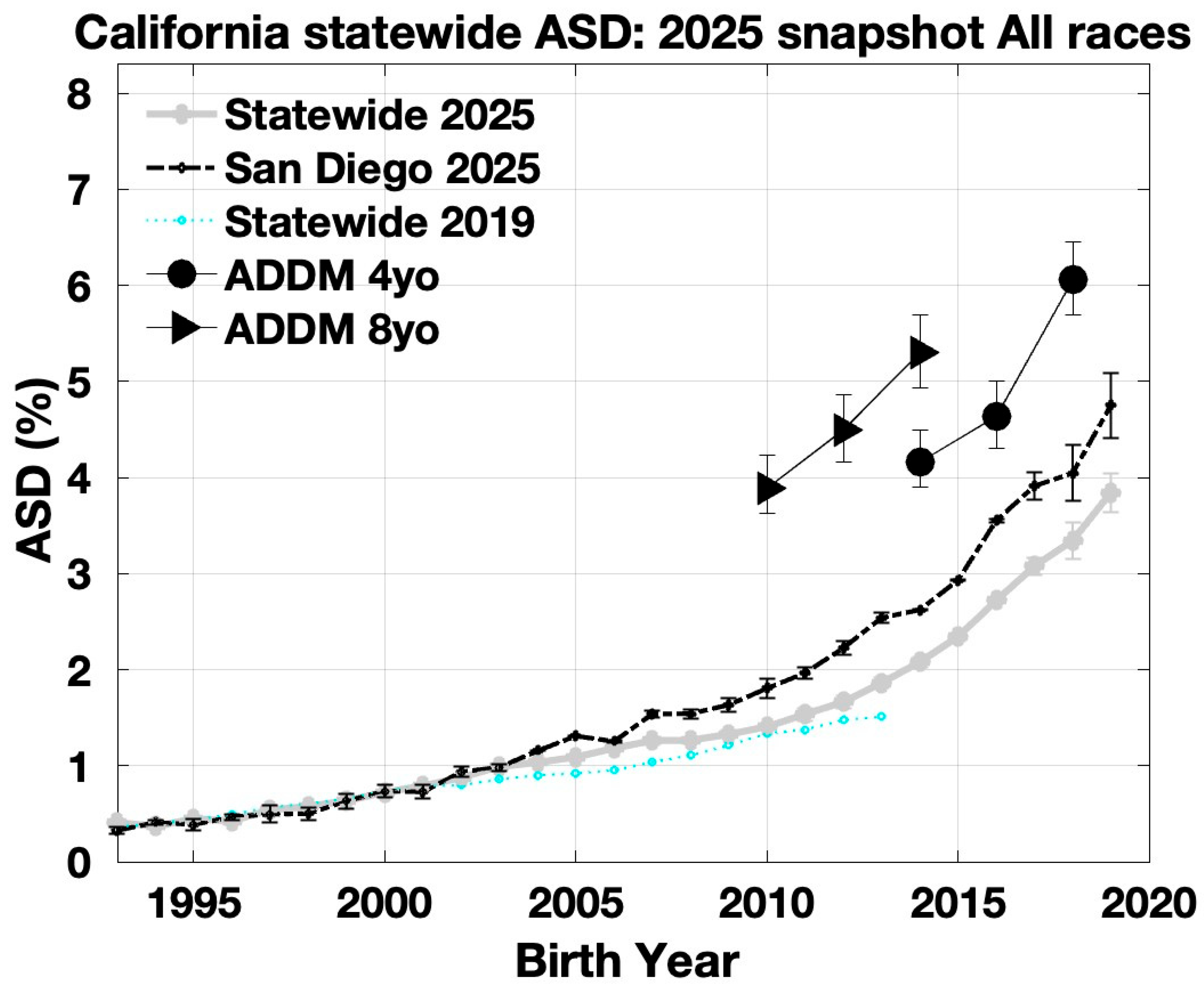
3.3. Statewide California ASD Prevalence Trends by Race/Ethnicity
4. Discussion
4.1. Accelerated Increase in ASD Growth rate with Changepoint Circa Birth Years 2015-2016
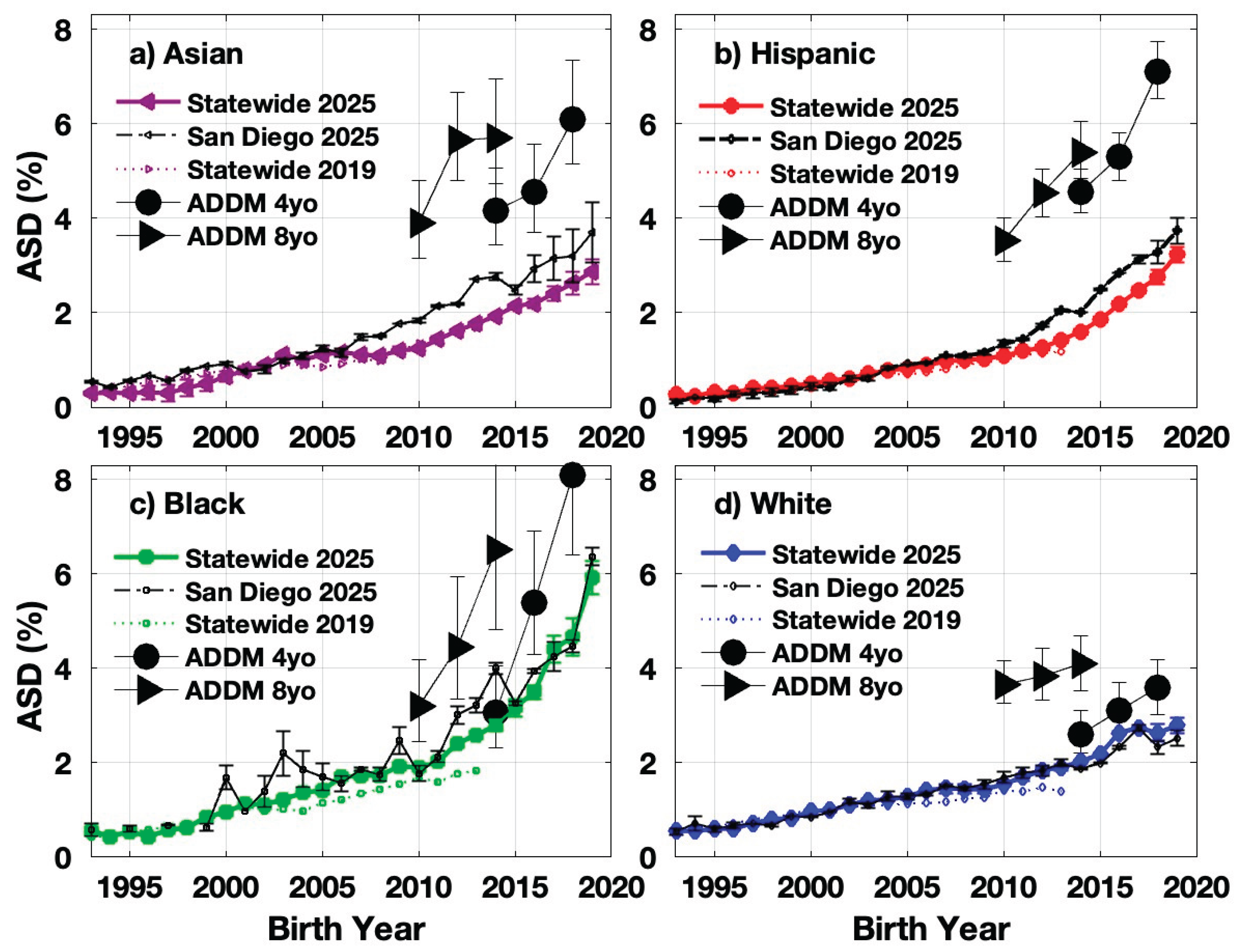
4.2. Divergence in ASD Trends by Race/Ethnicity
4.3. Divergence in ASD Trends by County
4.4. San Diego vs. Statewide ASD Prevalence
4.5. California DDS vs. ADDM
4.6. Limitations and Uncertainties
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ASD | Autism Spectrum Disorder |
| DDS | Department of Developmental Services |
| NCES | National Center for Education Statistics |
| PDD-NOS | Pervasive Developmental Disorder – Not Otherwise Specified |
| RSS | Residual Sum of Squares |
References
- American Psychiatric Association. 2013. Diagnostic and statistical manual of mental disorders. 5th ed. Washington: American Psychiatric Association.
- Hughes MM, Shaw KA, DiRienzo M, Durkin MS, Esler A, Hall-Lande J, Wiggins L, Zahorodny W, Singer A, Maenner MJ. The Prevalence and Characteristics of Children with Profound Autism, 15 Sites, United States, 2000-2016. Public Health Reports 2023,138(6): 1-10. doi.org/10.1177/00333549231163551.
- Rubenstein E, Schieve L, Wiggins L, Rice C, Van Naarden Braun K, Christensen D, Durkin M, Daniels J, Lee LC. Trends in documented co-occurring conditions in children with autism spectrum disorder, 2002-2010. Research in Developmental Disabilities 2018, 83:168-178.
- Nishimura Y, Kanda Y, Sone H, Aoyama H. Oxidative Stress as a Common Key Event in Developmental Neurotoxicity. Oxid Med Cell Longev. 2021, 6685204. Epub 2021/08/03. [CrossRef]
- Liu X, Lin J, Zhang H, Khan NU, Zhang J, Tang X, et al. Oxidative Stress in Autism Spectrum Disorder-Current Progress of Mechanisms and Biomarkers. Frontiers in Psychiatry 2022,13:813304. Epub 2022/03/19.
- Usui N, Kobayashi H, Shimada S. Neuroinflammation and oxidative stress in the pathogenesis of autism spectrum disorder. Int. J. Mol. Sci. 2023, 24(6):5487. [CrossRef]
- Hallmayer, J. et al. Genetic heritability and shared environmental factors among twin pairs with autism. Arch Gen Psychiatry 2011, 68:1095-1102.
- Shaw KA, Williams S, Patrick ME, Valencia-Prado M, Durkin MS, Howerton EM, et al. Prevalence and early identification of autism spectrum disorder among children aged 4 and 8 years – Autism and Developmental Disabilities Monitoring Network, 16 sites, United States, Morb Mortal Wkly Rep. 2025, 74(2):1-22.
- Centers for Disease Control and Prevention. Prevalence of Autism Spectrum Disorders --- Autism and Developmental Disabilities Monitoring Network, Six sites, United States, 2000. Morb Mortal Wkly Rep 2007, 56 (SS01): 1–11. http://www.cdc.gov/mmwr/preview/mmwrhtml/ss5810a1.htm.
- Nevison CD, Parker W. California autism prevalence by county and race/ethnicity: Declining trends among wealthy whites. J. Autism and Dev Disord 2020, 50(11): 4011-4021. [CrossRef]
- O’Sharkey K, Mitra S, Paik S, Chow T, Cockburn M, Ritz B. Trends in the Prevalence of Autism Spectrum Disorder in California: Disparities by Sociodemographic Factors and Region Between 1990–2018. J. Autism and Dev Disord. 2024. [CrossRef]
- Keaton, P. (National Center for Education Statistics). Personal communication, 2023.
- Chen, C.-S. (National Center for Education Statistics). Personal communication, 2023.
- McDonald ME, Paul JF. Timing of increased autistic disorder cumulative incidence. Environ Sci Technol. 2010, 44:2112-2118.
- Nevison CD, Blaxill M, Zahorodny W. California autism prevalence trends from 1931-2014 and comparison to national ASD data from IDEA and ADDM. J. Autism and Dev Disord 2018, 48:4103-4117.
- Pearl M, Matias S, Poon V, Windham G. Trends in birth prevalence of autism spectrum disorder (ASD) in California from 1990 to 2010, by race-ethnicity and income, International Society for Autism Research (INSAR), 2019 annual meeting, Poster 31748, Montreal, Canada, May 4, 2019.
- Data Commons. 2026. Ranking by median household income. All counties in California. https://datacommons.org/ranking/Median_Income_Household/County/geoId/06?h=geoId%2F06073&unit=%24. Accessed Jan 25, 2026.
- Georgetown University. 2023. Medicaid coverage in California counties, 2023. https://ccf.georgetown.edu/2025/02/06/medicaid-coverage-in-california-counties-2023/. McCourt School of Public Policy newsletter. Accessed Jan 24, 2026.
- Department of Health Care Services (DHCS). SB 75 – Full scope Medi-Cal for all children. https://www.dhcs.ca.gov/services/medi-cal/eligibility/Pages/SB-75.aspx. Accessed 3/11/2026.
- DOJ (Department of Justice). First defendant charged in autism fraud scheme. September 24, 2025. https://www.justice.gov/usao-mn/pr/first-defendant-charged-autism-fraud-scheme-0.
- Educate.Advocate. 2018. Special education finance hearing California, 2/28/2018. https://www.youtube.com/watch?v=utVER6Jczuk. Accessed 02/20/2026.
- Deoni S, Beauchemin J, Volpe A, D’Sa V. The COVID-19 Pandemic and Early Child Cognitive Development: A Comparison of Development in Children Born During the Pandemic and Historical References. 2021. https://www.medrxiv.org/content/10.1101/2021.08.10.21261846v2.full.pdf.
- Kisielinski K, Wagner S, Hirsch O, Klosterhalfen B, Prescher A. Possible toxicity of chronic carbon dioxide exposure associated with face mask use, particularly in pregnant women, children and adolescents – A scoping review. Heliyon 2023, 9, e14117.
- Walter D. Lengthy pandemic closures weakened already low-achieving California schools. Cal Matters. https://calmatters.org/commentary/2023/07/pandemic-poor-achievement-california-schools/.
- Fountain C, Bearman P. Risk as social context: Immigration policy and autism in California. Sociol Forum 2011, 26(2):215-240.
- Maenner MJ, Shaw KA, Bakian AV, Bilder DA, Durkin MS, Esler A, et al. Prevalence and Characteristics of Autism Spectrum Disorder Among Children Aged 8 Years - Autism and Developmental Disabilities Monitoring Network, 11 Sites, United States, 2018. Morb Mortal Wkly Rep. 2021, 70 (11):1–16.
- Maenner MJ, Warren Z, Williams AR, Amoakohene EA, Bakian AV, Bilder DA, et al. Prevalence and characteristics of autism spectrum disorder among children aged 8 years—Autism and Developmental Disabilities Monitoring Network, 11 sites, United States, 2020. Morb Mortal Wkly Rep. 2023, 72(2): 1–14. [CrossRef]
- Nevison CD, Zahorodny W. Race/Ethnicity-Resolved Time Trends in United States ASD Prevalence Estimates from IDEA and ADDM. J. Autism and Dev Disord 2019, 49(12): 4721-4730.
- Baio J, Wiggins L, Christensen DL, Maenner MJ, Daniels J, Warren Z, Kurzius-Spencer M, Zahorodny W, et al. Prevalence and Characteristics of Autism Spectrum Disorder Among Children Aged 8 Years — Autism and Developmental Disabilities Monitoring Network , 11 Sites , United States , 2014. Morb Mortal Wkly Rep. 2018, 67 (6): 1-23.
- Liu L, Wen W, Shrubsole MJ, Lipworth LE, Mumma MT, Ackerly BA, Shu XO, Blot WJ, Zheng W. 2024. Impacts of poverty and lifestyles on mortality: a cohort study in predominantly low-income Americans. Am J Prev Med. 2024, 67(1):15-23.
- US Department of Education (USDE), Educational Services for Immigrant Children and Those Recently Arrived to the United States, accessed March 10, 2026. https://www.ed.gov/sites/ed/files/policy/rights/guid/unaccompanied-children.pdf.
- California Department of Developmental Services. Changes in the Population of Persons with Autism and Pervasive Developmental Disorders in California’s Developmental Services System: 1987 through 1998., Sacramento, CA. 1999.
- California Department of Developmental Services. Autistic spectrum disorders. Changes in California Caseload. An Update: 1999 through 2002. Sacramento, CA. 2003.
- Centers for Disease Control and Prevention. Prevalence of autism spectrum disorder among children aged 8 years - autism and developmental disabilities monitoring network, 11 sites, United States, 2010. Morb Mortal Wkly Rep 2014, 63 Suppl 2 (2): 1–21. http://www.ncbi.nlm.nih.gov/pubmed/24670961.
- Leigh JP, Grosse SD, Cassady D, Melnikow J, Hertz-Picciotto I. Spending by California’s Department of Developmental Services for persons with autism across demographic and expenditure categories. PloS One 2016, 11(3), e0151970.
- Di Biasi, E. (California DDS). Personal communication, 2026.
| County | Yc | slope period 1 (%/yr) | slope period 2 (%/yr) | p value |
|---|---|---|---|---|
| Alameda | 2016 | 0.097 ± 0.007 | 0.186 ± 0.042 | 0.002 |
| Contra Costa | 2015 | 0.052 ± 0.006 | 0.246 ± 0.069 | 0.0002 |
| Fresno | 2016 | 0.084 ± 0.007 | 0.541 ± 0.050 | < 0.0001 |
| Imperial | 2015 | 0.323 ± 0.024 | 0.491 ± 0.124 | 0.0522 |
| Kern | 2015 | 0.079 ± 0.007 | 0.441 ± 0.041 | < 0.0001 |
| Kings | 2017 | 0.095 ± 0.018 | 0.662 ± 0.126 | < 0.0001 |
| Los Angeles | 2016 | 0.157 ± 0.006 | 0.572 ± 0.066 | < 0.0001 |
| Merced | 2014 | 0.041 ± 0.011 | 0.436 ± 0.044 | < 0.0001 |
| Monterey | 2016 | 0.047 ± 0.007 | 0.096 ± 0.036 | 0.0313 |
| Orange | 2014 | 0.039 ± 0.006 | 0.163 ± 0.012 | < 0.0001 |
| Sacramento | 2015 | 0.070 ± 0.008 | 0.179 ± 0.049 | 0.0028 |
| San Diego | 2015 | 0.113 ± 0.007 | 0.323 ± 0.024 | < 0.0001 |
| San Joaquin | 2016 | 0.117 ± 0.010 | 0.494 ± 0.073 | < 0.0001 |
| San Luis Obispo | 2015 | -0.052 ± 0.077 | 0.188 ± 0.133 | 0.3092 |
| San Mateo | 2016 | 0.029 ± 0.015 | 0.237 ± 0.046 | 0.0049 |
| Santa Barbara | 2016 | 0.074 ± 0.011 | 0.431 ± 0.056 | < 0.0001 |
| Santa Clara | 2016 | 0.074 ± 0.006 | 0.171 ± 0.063 | 0.0072 |
| Solano | 2016 | 0.023 ± 0.022 | 0.458 ± 0.069 | < 0.0001 |
| Sonoma | 2014 | 0.044 ± 0.010 | 0.348 ± 0.034 | < 0.0001 |
| Stanislaus | 2016 | 0.079 ± 0.011 | 0.477 ± 0.088 | < 0.0001 |
| Tulare | 2016 | 0.084 ± 0.008 | 0.749 ± 0.082 | < 0.0001 |
| Ventura | 2014 | 0.059 ± 0.008 | 0.402 ± 0.067 | < 0.0001 |
| Birth years | Correlation coefficient (p value) | |||||
| % on Medicaid | Asians | Black | Hispanic | White | All Races | |
| 2014-2019 | Mean | 0.64 (.01) | 0.66 (0.04) | 0.57 (0.001) | 0.39 (0.06) | 0.50 (0.01) |
| 2014-2019 | Rate | 0.48 (.07) | 0.78 (0.01) | 0.62 (0.001) | 0.37 (0.1) | 0.67 (0.001) |
| 2000-2014 | Mean | 0.26 (0.38) | 0.55 (0.15) | 0.27 (0.2) | 0.38 (0.06) | 0.18 (0.31) |
| 2000-2014 | Rate | 0.06 (0.84) | 0.12 (0.77) | 0.41 (0.05) | 0.24 (0.22) | 0.37 (0.04) |
| Median Income | ||||||
| 2014-2019 | Mean | -0.79 (.001) | -0.34 (.33) | -0.54 (0.01) | -0.63 (<.01) | -0.60 (<.01) |
| 2014-2019 | Rate | -0.55 (.04) | -0.69 (.03) | -0.47 (0.01) | -0.52 (.01) | -0.65 (.001) |
| 2000-2014 | Mean | -0.39 (.19) | -0.12 (.78) | -0.39 (0.06) | -0.59 (.01) | -0.37 (.03) |
| 2000-2014 | Rate | -0.22 (.46) | -0.07 (.82) | -0.32 (0.13) | -0.49 (.01) | -0.45 (.009) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




