Submitted:
21 March 2026
Posted:
23 March 2026
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Methodology
3. Literature Selection
4. Conceptual Synthesis
5. Scope and Limitations
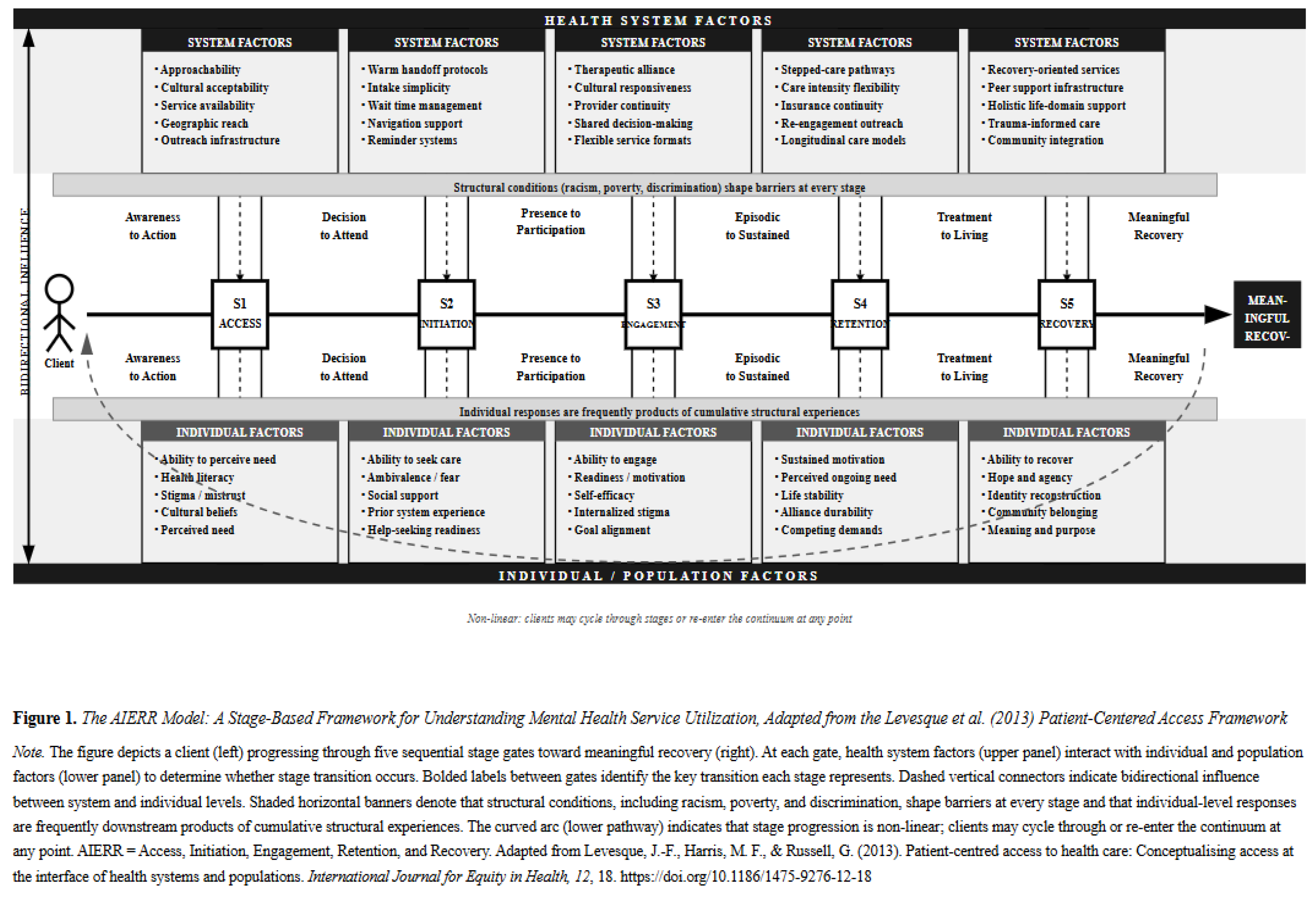
6. Model Characteristics
6.1. Stage 1: Access to Services
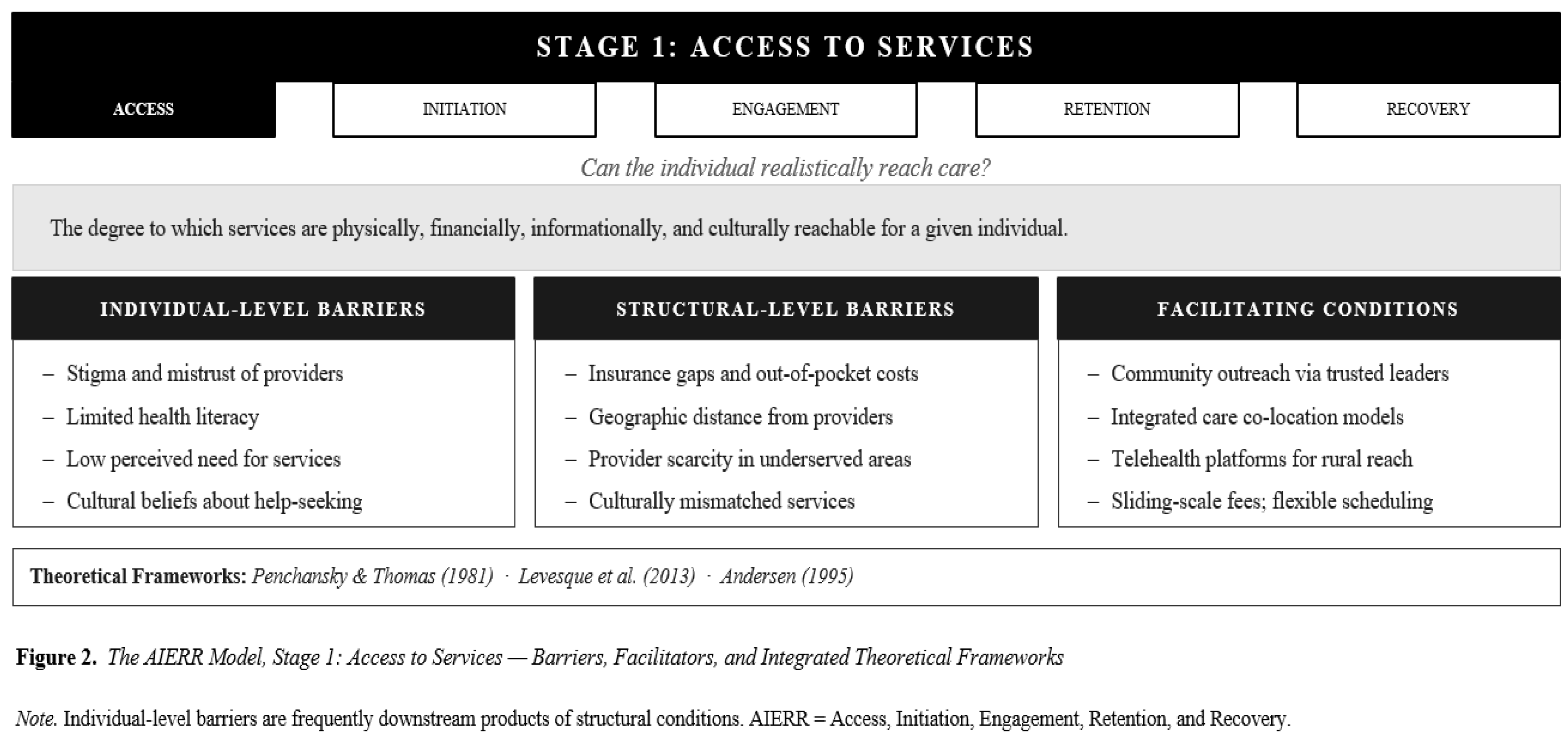
6.2. Stage 2: Initiation of Mental Health Services
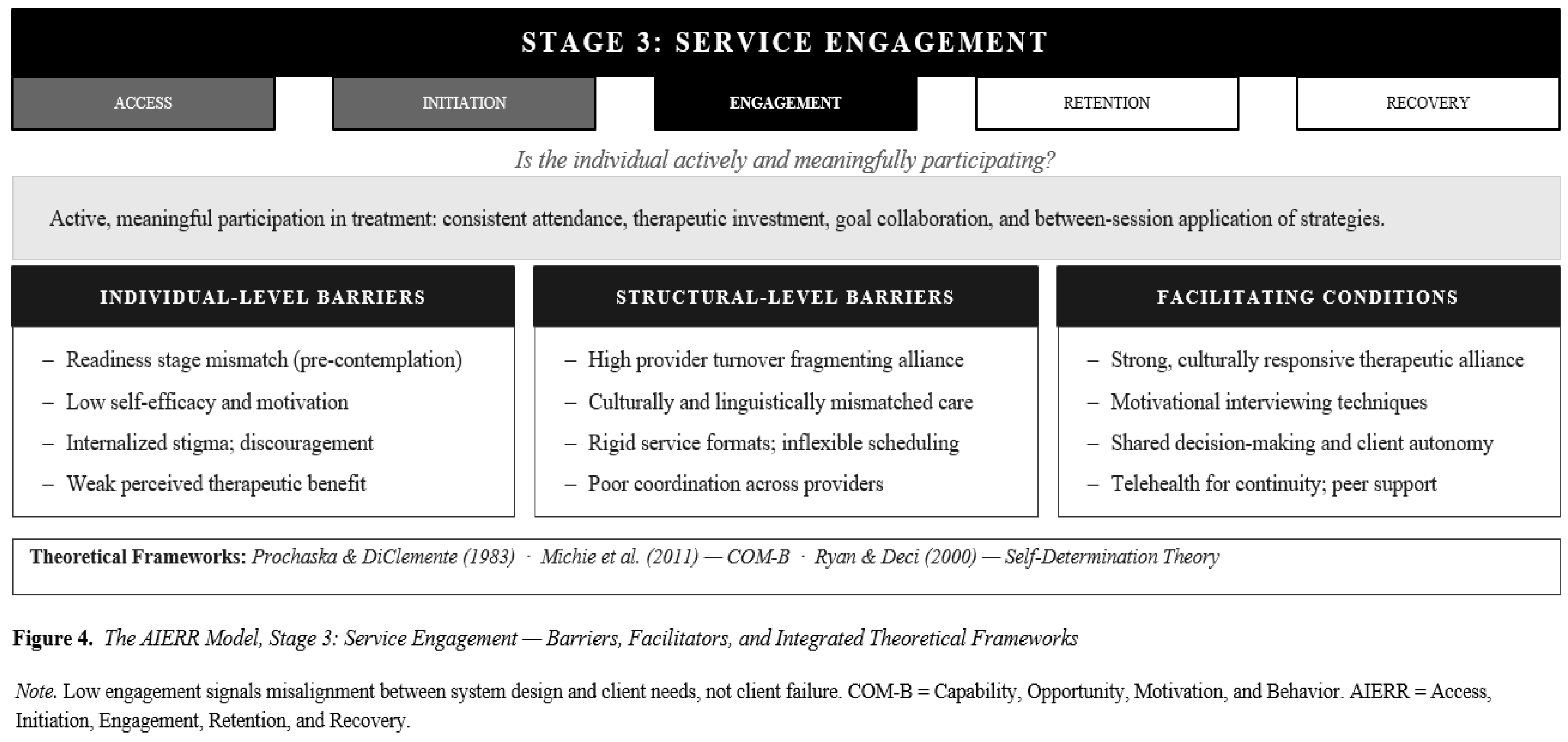
6.3. Stage 3: Service Engagement
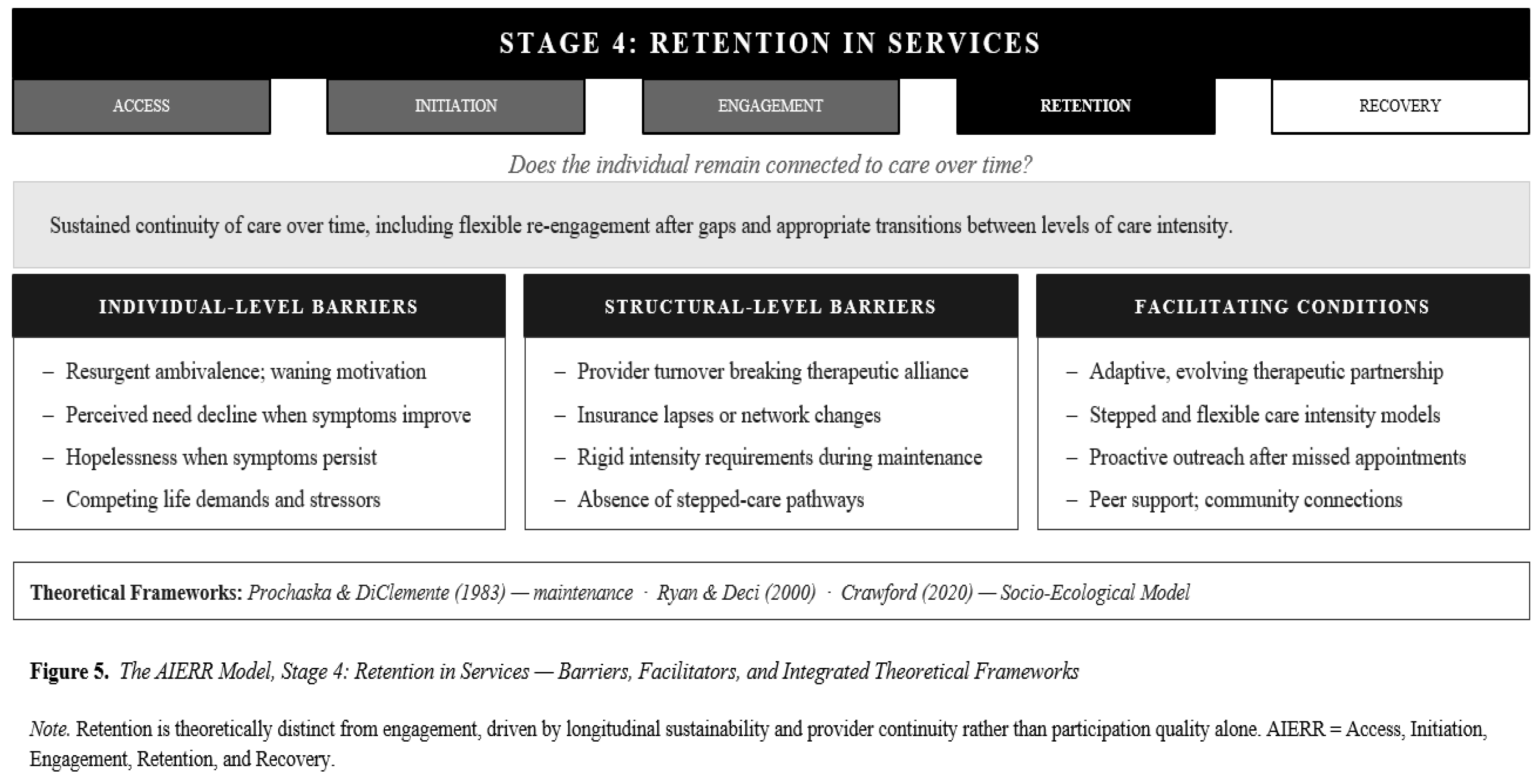
6.4. Stage 4: Retention of Services in Mental Health Care
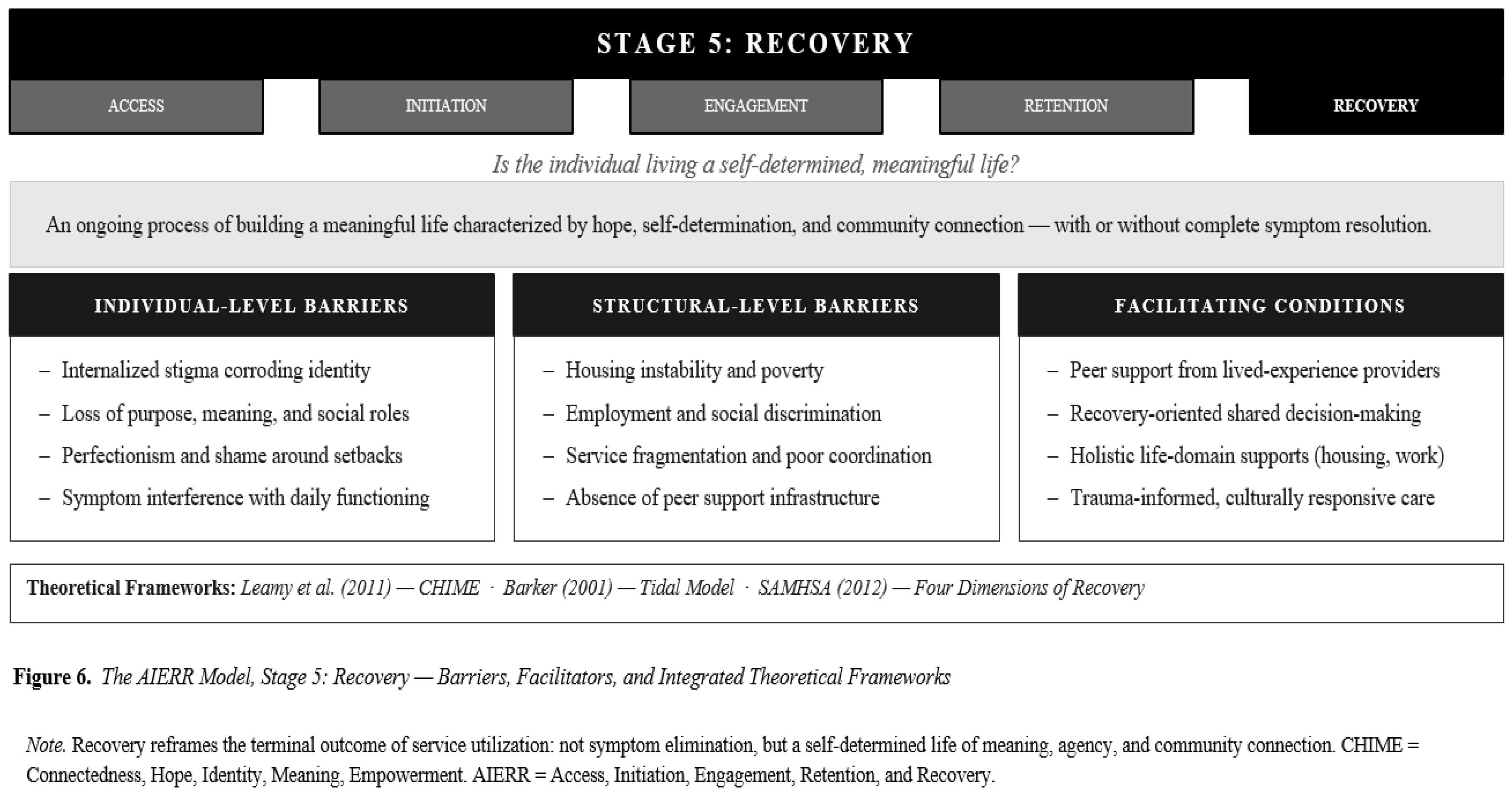
6.5. Stage 5: Recovery
7. Discussion
7.1. Implications for Research and Practice
7.2. Limitations
7.3. Future Directions
Author Contributions
Funding
Data Availability Statement
Human Subjects
Financial and Non-Financial Interests
Ethics Approval Statement
References
- Alegría, M.; Carson, N.; Flores, M.; Li, X.; Shi, P.; Lessios, A.S.; Polo, A.; Allen, M.; Fierro, M.; Interian, A.; et al. Activation, Self-management, Engagement, and Retention in Behavioral Health Care. JAMA Psychiatry 2014, 71, 557–565. [Google Scholar] [CrossRef] [PubMed]
- AlHarthy, S.H.; AL-MoundhrI, M.; Al-Mahmoodi, W.; Ibrahim, R.; Ayaad, O.; Al Baimani, K. Referral Process Enhancement: Innovative Approaches and Best Practices. Asian Pac. J. Cancer Prev. 2024, 25, 1691–1698. [Google Scholar] [CrossRef]
- Andersen, R.M. Revisiting the Behavioral Model and Access to Medical Care: Does it Matter? J. Health Soc. Behav. 1995, 36, 1–10. [Google Scholar] [CrossRef]
- Anderson, K.N.; Bautista, C.L.; Hope, D.A. Therapeutic alliance, cultural competence and minority status in premature termination of psychotherapy. Am. J. Orthopsychiatry 2019, 89, 104–114. [Google Scholar] [CrossRef]
- Anindhita, M.; Haniifah, M.; Putri, A.M.N.; Karnasih, A.; Agiananda, F.; Yani, F.F.; Haya, M.A.N.; Pakasi, T.A.; Widyahening, I.S.; Fuady, A.; et al. Community-based psychosocial support interventions to reduce stigma and improve mental health of people with infectious diseases: a scoping review. Infect. Dis. Poverty 2024, 13, 1–17. [Google Scholar] [CrossRef]
- Anthony, W.A. Recovery from mental illness: The guiding vision of the mental health service system in the 1990s. Psychosoc. Rehabilitation J. 1993, 16, 11–23. [Google Scholar] [CrossRef]
- Audet, C.T.; Everall, R.D. Therapist self-disclosure and the therapeutic relationship: a phenomenological study from the client perspective. Br. J. Guid. Couns. 2010, 38, 327–342. [Google Scholar] [CrossRef]
- Bardone-Cone, A.M.; White, J.P.; Thompson, K.A.; Zucker, N.; Watson, H.J.; Bulik, C.M. Examination of perfectionism and self-concept constructs across stages of eating disorder recovery in men: An exploratory study. Eat. Behav. 2022, 46, 101658–101658. [Google Scholar] [CrossRef]
- Frcn, P.B.P.R. The Tidal Model: developing an empowering, person-centred approach to recovery within psychiatric and mental health nursing. J. Psychiatr. Ment. Heal. Nurs. 2001, 8, 233–240. [Google Scholar] [CrossRef]
- Barrett, M.S.; Chua, W.-J.; Crits-Christoph, P.; Gibbons, M.B.; Casiano, D.; Thompson, D. Early withdrawal from mental health treatment: Implications for psychotherapy practice. Psychotherapy 2008, 45, 247–267. [Google Scholar] [CrossRef] [PubMed]
- Bauer, A.G.; Ruglass, L.M.; Shevorykin, A.; Saraiya, T.C.; Robinson, G.; Cadet, K.; Julien, L.; Chao, T.; Hien, D. Predictors of therapeutic alliance, treatment feedback, and clinical outcomes among African American women in treatment for co-occurring PTSD and SUD. J. Subst. Abus. Treat. 2022, 139, 108766–108766. [Google Scholar] [CrossRef] [PubMed]
- Benjet, C.; Borges, G.; Orozco, R.; Aguilar-Gaxiola, S.; Andrade, L.H.; Cia, A.; Hwang, I.; Kessler, R.C.; Piazza, M.; Posada-Villa, J.; et al. Dropout from treatment for mental disorders in six countries of the Americas: A regional report from the World Mental Health Surveys. J. Affect. Disord. 2022, 303, 168–179. [Google Scholar] [CrossRef]
- Bjørlykhaug, K.I.; Karlsson, B.; Hesook, S.K.; Kleppe, L.C. Social support and recovery from mental health problems: a scoping review. Nord. Soc. Work. Res. 2021, 12, 666–697. [Google Scholar] [CrossRef]
- Brancewicz, M.; Robakowska, M.; Śliwiński, M.; Rystwej, D. SMS and Telephone Communication as Tools to Reduce Missed Medical Appointments. Appl. Sci. 2025, 15, 9773. [Google Scholar] [CrossRef]
- Caple, V.; Maude, P.; Walter, R.; Ross, A. An exploration of loneliness experienced by people living with mental illness and the impact on their recovery journey: An integrative review. J. Psychiatr. Ment. Heal. Nurs. 2023, 30, 1170–1191. [Google Scholar] [CrossRef]
- Chapman, K.A.; Machado, S.S.; van der Merwe, K.; Bryson, A.; Smith, D. Exploring Primary Care Non-Attendance: A Study of Low-Income Patients. J. Prim. Care Community Heal. 2022, 13. [Google Scholar] [CrossRef]
- Clark, D.M.; Canvin, L.; Green, J.; Layard, R.; Pilling, S.; Janecka, M. Transparency about the outcomes of mental health services (IAPT approach): an analysis of public data. Lancet 2018, 391, 679–686. [Google Scholar] [CrossRef]
- Corrigan, P.W.; Druss, B.G.; Perlick, D.A. The Impact of Mental Illness Stigma on Seeking and Participating in Mental Health Care. Psychol. Sci. Public Interes. 2014, 15, 37–70. [Google Scholar] [CrossRef]
- Crawford, M. Ecological Systems Theory: Exploring the Development of the Theoretical Framework as Conceived by Bronfenbrenner. J. Public Heal. Issues Pr. 2020, 4. [Google Scholar] [CrossRef]
- Curtis, E.; Jones, R.; Tipene-Leach, D.; Walker, C.; Loring, B.; Paine, S.-J.; Reid, P. Why cultural safety rather than cultural competency is required to achieve health equity: a literature review and recommended definition. Int. J. Equity Health 2019, 18, 1–17. [Google Scholar] [CrossRef]
- Dang, B.N.; Westbrook, R.A.; Njue, S.M.; Giordano, T.P. Building trust and rapport early in the new doctor-patient relationship: a longitudinal qualitative study. BMC Med Educ. 2017, 17, 1–10. [Google Scholar] [CrossRef]
- Dawkins, B.; Renwick, C.; Ensor, T.; Shinkins, B.; Jayne, D.; Meads, D. What factors affect patients’ ability to access healthcare? An overview of systematic reviews. Trop. Med. Int. Heal. 2021, 26, 1177–1188. [Google Scholar] [CrossRef]
- de Jong, K.; Douglas, S.; Wolpert, M.; Delgadillo, J.; Aas, B.; Bovendeerd, B.; Carlier, I.; Compare, A.; Edbrooke-Childs, J.; Janse, P.; et al. Using Progress Feedback to Enhance Treatment Outcomes: A Narrative Review. Adm. Policy Ment. Heal. Ment. Heal. Serv. Res. 2024, 52, 210–222. [Google Scholar] [CrossRef]
- De-María, B.; Topa, G.; López-González, M.A. Cultural Competence Interventions in European Healthcare: A Scoping Review. Healthcare 2024, 12, 1040. [Google Scholar] [CrossRef]
- De-María, B.; Topa, G.; López-González, M.A. Cultural Competence Interventions in European Healthcare: A Scoping Review. Healthcare 2024, 12, 1040. [Google Scholar] [CrossRef]
- English, W.; Gott, M.; Robinson, J. The meaning of rapport for patients, families, and healthcare professionals: A scoping review. Patient Educ. Couns. 2022, 105, 2–14. [Google Scholar] [CrossRef] [PubMed]
- Fernández, D.; Vigo, D.; Sampson, N.A.; Hwang, I.; Aguilar-Gaxiola, S.; Al-Hamzawi, A.O.; Alonso, J.; Andrade, L.H.; Bromet, E.J.; de Girolamo, G.; et al. Patterns of care and dropout rates from outpatient mental healthcare in low-, middle- and high-income countries from the World Health Organization's World Mental Health Survey Initiative. Psychol. Med. 2020, 51, 2104–2116. [Google Scholar] [CrossRef] [PubMed]
- Fitzpatrick, P.J. Improving health literacy using the power of digital communications to achieve better health outcomes for patients and practitioners. Front. Digit. Heal. 2023, 5, 1264780. [Google Scholar] [CrossRef] [PubMed]
- Flückiger, C.; Del Re, A.C.; Wampold, B.E.; Horvath, A.O. The alliance in adult psychotherapy: A meta-analytic synthesis. Psychotherapy 2018, 55, 316–340. [Google Scholar] [CrossRef]
- Fortney, J.C.; Burgess, J.F.; Bosworth, H.B.; Booth, B.M.; Kaboli, P.J. A Re-conceptualization of Access for 21st Century Healthcare. J. Gen. Intern. Med. 2011, 26, 639–647. [Google Scholar] [CrossRef]
- Geyti, C.; Dalsgaard, E.-M.; Sandbæk, A.; Maindal, H.T.; Christensen, K.S. Initiation and cessation of mental healthcare after mental health screening in primary care: a prospective cohort study. BMC Fam. Pr. 2018, 19, 176. [Google Scholar] [CrossRef]
- Giansanti, D.; Pirrera, A. Integrating AI and Assistive Technologies in Healthcare: Insights from a Narrative Review of Reviews. Healthcare 2025, 13, 556. [Google Scholar] [CrossRef]
- Graffigna, G.; Barello, S.; Bonanomi, A.; Lozza, E. Measuring patient engagement: development and psychometric properties of the Patient Health Engagement (PHE) Scale. Front. Psychol. 2015, 6, 274–274. [Google Scholar] [CrossRef]
- Greene, J.A.; Bina, R.; Gum, A.M. Interventions to Increase Retention in Mental Health Services: A Systematic Review. Psychiatr. Serv. 2016, 67, 485–495. [Google Scholar] [CrossRef]
- Griffith, D.M.; Bergner, E.M.; Fair, A.S.; Wilkins, C.H. Using Mistrust, Distrust, and Low Trust Precisely in Medical Care and Medical Research Advances Health Equity. Am. J. Prev. Med. 2021, 60, 442–445. [Google Scholar] [CrossRef] [PubMed]
- Hall, J.A. Clinicians’ accuracy in perceiving patients: Its relevance for clinical practice and a narrative review of methods and correlates. Patient Educ. Couns. 2011, 84, 319–324. [Google Scholar] [CrossRef] [PubMed]
- Hodgkinson, S.; Godoy, L.; Beers, L.S.; Lewin, A. Improving Mental Health Access for Low-Income Children and Families in the Primary Care Setting. Pediatrics 2017, 139, e20151175. [Google Scholar] [CrossRef]
- Holdsworth, E.; Bowen, E.; Brown, S.; Howat, D. Client engagement in psychotherapeutic treatment and associations with client characteristics, therapist characteristics, and treatment factors. Clin. Psychol. Rev. 2014, 34, 428–450. [Google Scholar] [CrossRef] [PubMed]
- Hostutler, C.; Wolf, N.; Snider, T.; Butz, C.; Kemper, A.R.; Butter, E. Increasing Access to and Utilization of Behavioral Health Care Through Integrated Primary Care. Pediatrics 2023, 152. [Google Scholar] [CrossRef]
- Hulland, J. Conceptual review papers: revisiting existing research to develop and refine theory. AMS Rev. 2020, 10, 27–35. [Google Scholar] [CrossRef]
- Isaacs, A.; Bonsey, A.; Couch, D. Centralized Intake Models and Recommendations for Their Use in Non-Acute Mental Health Services: A Scoping Review. Int. J. Environ. Res. Public Heal. 2023, 20, 5747. [Google Scholar] [CrossRef]
- Jeitani, A.; Fahey, P.P.; Gascoigne, M.; Darnal, A.; Lim, D. Effectiveness of stepped care for mental health disorders: An umbrella review of meta-analyses. Pers. Med. Psychiatry 2024, 47–48, 100140–100140. [Google Scholar] [CrossRef]
- Jiao, S.; Slemon, A.; Guta, A.; Bungay, V. Exploring the conceptualization, operationalization, implementation, and measurement of outreach in community settings with hard-to-reach and hidden populations: A scoping review. Soc. Sci. Med. 2022, 309, 115232. [Google Scholar] [CrossRef]
- Kashgary, A.; Alsolaimani, R.; Mosli, M.; Faraj, S. The role of mobile devices in doctor-patient communication: A systematic review and meta-analysis. J. Telemed. Telecare 2016, 23, 693–700. [Google Scholar] [CrossRef] [PubMed]
- Killaspy, H.; Harvey, C.; Brasier, C.; Brophy, L.; Ennals, P.; Fletcher, J.; Hamilton, B. Community-based social interventions for people with severe mental illness: a systematic review and narrative synthesis of recent evidence. World Psychiatry 2022, 21, 96–123. [Google Scholar] [CrossRef]
- Kirby, J.B.; Nogueira, L.; Zhao, J.; Yabroff, K.R. Do Disruptions in Health Insurance Continue to Affect Access to Care Even After Coverage Is Regained? J. Gen. Intern. Med. 2022, 37, 2579–2581. [Google Scholar] [CrossRef] [PubMed]
- Kornhaber, R.; Walsh, K.; Duff, J.; Walker, K. Enhancing adult therapeutic interpersonal relationships in the acute health care setting: an integrative review. J. Multidiscip. Heal. 2016, ume 9, 537–546. [Google Scholar] [CrossRef]
- Kyle, M.A.; Frakt, A.B. Patient administrative burden in the US health care system. Heal. Serv. Res. 2021, 56, 755–765. [Google Scholar] [CrossRef]
- Leamy, M.; Bird, V.; Le Boutillier, C.; Williams, J.; Slade, M. Conceptual framework for personal recovery in mental health: systematic review and narrative synthesis. Br. J. Psychiatry 2011, 199, 445–452. [Google Scholar] [CrossRef] [PubMed]
- Levesque, J.-F.; Harris, M.F.; Russell, G. Patient-centred access to health care: conceptualising access at the interface of health systems and populations. Int. J. Equity Health 2013, 12, 18. [Google Scholar] [CrossRef]
- Lin, C.; Cousins, S.J.; Zhu, Y.; Clingan, S.E.; Mooney, L.J.; Kan, E.; Wu, F.; Hser, Y.-I. A scoping review of social determinants of health's impact on substance use disorders over the life course. J. Subst. Use Addict. Treat. 2024, 166, 209484. [Google Scholar] [CrossRef] [PubMed]
- Long, L.J.; Fitzgerald, H.E.; Parsons, E.; McSpadden, B.; Cobb, A.; Shumake, J.; Monfils, M.-H.; Telch, M.; Smits, J.A.; Otto, M.W. The Role of Hope in Recovery During Transdiagnostic Exposure-Based Therapy for Anxiety-, Obsessive–Compulsive and Trauma- and Stressor-related Disorders. Behav. Ther. 2025. [Google Scholar] [CrossRef]
- Madanian, S.; Nakarada-Kordic, I.; Reay, S.; Chetty, T. Patients' perspectives on digital health tools. PEC Innov. 2023, 2, 100171. [Google Scholar] [CrossRef]
- Manuel, J.I.; Covell, N.H.; Jackson, C.T.; Essock, S.M. Does Assertive Community Treatment Increase Medication Adherence for People With Co-occurring Psychotic and Substance Use Disorders? J. Am. Psychiatr. Nurses Assoc. 2011, 17, 51–56. [Google Scholar] [CrossRef]
- Mays, V.M.P.; Jones, A.L.; Delany-Brumsey, A.; Coles, C.; Cochran, S.D. Perceived Discrimination in Health Care and Mental Health/Substance Abuse Treatment Among Blacks, Latinos, and Whites. Med Care 2017, 55, 173–181. [Google Scholar] [CrossRef]
- Meier, P.S.; Donmall, M.C.; McElduff, P.; Barrowclough, C.; Heller, R.F. The role of the early therapeutic alliance in predicting drug treatment dropout. Drug Alcohol Depend. 2006, 83, 57–64. [Google Scholar] [CrossRef]
- Melillo, A.; Sansone, N.; Allan, J.; Gill, N.; Herrman, H.; Cano, G.M.; Rodrigues, M.; Savage, M.; Galderisi, S. Recovery-oriented and trauma-informed care for people with mental disorders to promote human rights and quality of mental health care: a scoping review. BMC Psychiatry 2025, 25, 1–22. [Google Scholar] [CrossRef] [PubMed]
- Michie, S.; Van Stralen, M.M.; West, R. The behaviour change wheel: A new method for characterising and designing behaviour change interventions. Implement. Sci. 2011, 6, 42. [Google Scholar] [CrossRef]
- Miller, R.; Hilsenroth, M.J.; Hewitt, P.L. Perfectionism and therapeutic alliance: a review of the clinical research. Res. Psychother. Psychopathol. Process. Outcome 2017, 20. [Google Scholar] [CrossRef]
- Nye, A.; Delgadillo, J.; Barkham, M. Efficacy of personalized psychological interventions: A systematic review and meta-analysis. J. Consult. Clin. Psychol. 2023, 91, 389–397. [Google Scholar] [CrossRef]
- O’cOnnell, T.S.; Bedford, K.J.A.; Thiede, M.; McIntyre, D. Synthesizing qualitative and quantitative evidence on non-financial access barriers: implications for assessment at the district level. Int. J. Equity Heal. 2015, 14, 1–13. [Google Scholar] [CrossRef]
- Olfson, M.; Mojtabai, R.; Sampson, N.A.; Hwang, I.; Druss, B.; Wang, P.S.; Wells, K.B.; Pincus, H.A.; Kessler, R.C. Dropout From Outpatient Mental Health Care in the United States. Psychiatr. Serv. 2009, 60, 898–907. [Google Scholar] [CrossRef]
- O’cOnnell, T.S.; Bedford, K.J.A.; Thiede, M.; McIntyre, D. Synthesizing qualitative and quantitative evidence on non-financial access barriers: implications for assessment at the district level. Int. J. Equity Heal. 2015, 14, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Pandey, M.; Maina, R.G.; Amoyaw, J.; Li, Y.; Kamrul, R.; Michaels, C.R.; Maroof, R. Impacts of English language proficiency on healthcare access, use, and outcomes among immigrants: a qualitative study. BMC Heal. Serv. Res. 2021, 21, 1–13. [Google Scholar] [CrossRef]
- Pasman, E.; Kollin, R.; Broman, M.; Lee, G.; Agius, E.; Lister, J.J.; Brown, S.; Resko, S.M. Cumulative barriers to retention in methadone treatment among adults from rural and small urban communities. Addict. Sci. Clin. Pr. 2022, 17, 1–10. [Google Scholar] [CrossRef] [PubMed]
- Patterson, M.S.; Francis, A.N.; Pew, S.H.; Liu, S.; Kang, Z.; Heinrich, K.M.; Prochnow, T. Exploring support provision for recovery from substance use disorder among members of a sober active community. Sci. Rep. 2025, 15, 1–10. [Google Scholar] [CrossRef]
- Penchansky, R.; Thomas, J.W. The concept of access: Definition and relationship to consumer satisfaction. Med. Care 1981, 19, 127–140. [Google Scholar] [CrossRef] [PubMed]
- Pescosolido, B.A.; Gardner, C.B.; Lubell, K.M. How people get into mental health services: Stories of choice, coercion and “muddling through” from “first-timers”. Soc. Sci. Med. 1998, 46, 275–286. [Google Scholar] [CrossRef]
- Prochaska, J.O.; DiClemente, C.C. Stages and processes of self-change of smoking: Toward an integrative model of change. J. Consult. Clin. Psychol. 1983, 51, 390–395. [Google Scholar] [CrossRef]
- Repper, J.; Carter, T. A review of the literature on peer support in mental health services. J. Ment. Heal. 2011, 20, 392–411. [Google Scholar] [CrossRef]
- Ridjic, D.; Mahmutovic, J. Rupture in the Psychotherapy Relationship Described Through the Prism of Different Psychoterapy Schools: Is There a Unique Place For Creating an Integrative Approach in the Resolution of Psychoterapy Rupture? Med Arch. 2025, 79, 406–406. [Google Scholar] [CrossRef] [PubMed]
- Rong, T.; Ristevski, E.; Carroll, M. Exploring community engagement in place-based approaches in areas of poor health and disadvantage: A scoping review. Heal. Place 2023, 81, 103026. [Google Scholar] [CrossRef] [PubMed]
- Rosenstock, I.M. Why people use health services. The Milbank Quarterly 2005, 83. [Google Scholar] [CrossRef]
- Ryan, R.M.; Deci, E.L. Self-determination theory and the facilitation of intrinsic motivation, social development, and well-being. Am. Psychol. 2000, 55, 68–78. [Google Scholar] [CrossRef]
- Sabety, A.H.; Jena, A.B.; Barnett, M.L. Changes in Health Care Use and Outcomes After Turnover in Primary Care. JAMA Intern. Med. 2020, 181, 186–194. [Google Scholar] [CrossRef] [PubMed]
- Sadusky, A.; Yared, H.; Patrick, P.; Berger, E. A systematic review of client’s perspectives on the cultural and racial awareness and responsiveness of mental health practitioners. Cult. Psychol. 2023, 30, 567–605. [Google Scholar] [CrossRef]
- Salzer, M.S.; Brusilovskiy, E.; Townley, G. National Estimates of Recovery-Remission From Serious Mental Illness. Psychiatr. Serv. 2018, 69, 523–528. [Google Scholar] [CrossRef]
- Schiaffino, M.K.; Ruiz, M.; Yakuta, M.; Contreras, A.; Akhavan, S.; Prince, B.; Weech-Maldonado, R. Culturally and Linguistically Appropriate Hospital Services Reduce Medicare Length of Stay. Ethn. Dis. 2020, 30, 603–610. [Google Scholar] [CrossRef]
- Schleider, J.L.; Zapata, J.P.; Rapoport, A.; Wescott, A.; Ghosh, A.; Kaveladze, B.; Szkody, E.; Ahuvia, I.L. Single-Session Interventions for Mental Health Problems and Service Engagement: Umbrella Review of Systematic Reviews and Meta-Analyses. Annu. Rev. Clin. Psychol. 2025, 21, 279–303. [Google Scholar] [CrossRef]
- Schwalbe, D. M.; Richardt, L.; Sodemann, M.; et al. Absent or not invited? A qualitative study of barriers and enablers of attendance at outpatient appointments in the Region of Southern Denmark. Research Square [Preprint] 2025. [Google Scholar] [CrossRef]
- Shekelle, P.G.; Begashaw, M.M.; Miake-Lye, I.M.; Booth, M.; Myers, B.; Renda, A. Effect of interventions for non-emergent medical transportation: a systematic review and meta-analysis. BMC Public Heal. 2022, 22, 1–12. [Google Scholar] [CrossRef] [PubMed]
- Shukla, M.; Schilt-Solberg, M.; Gibson-Scipio, W. Medical Mistrust: A Concept Analysis. Nurs. Rep. 2025, 15, 103. [Google Scholar] [CrossRef] [PubMed]
- Slade, M.; Amering, M.; Farkas, M.; Hamilton, B.; O'HAgan, M.; Panther, G.; Perkins, R.; Shepherd, G.; Tse, S.; Whitley, R. Uses and abuses of recovery: implementing recovery-oriented practices in mental health systems. World Psychiatry 2014, 13, 12–20. [Google Scholar] [CrossRef]
- Smirnoff, M.; Wilets, I.; Ragin, D.F.; Adams, R.; Holohan, J.; Rhodes, R.; Winkel, G.; Ricci, E.M.; Clesca, C.; Richardson, L.D. A paradigm for understanding trust and mistrust in medical research: The Community VOICES study. AJOB Empir. Bioeth. 2017, 9, 39–47. [Google Scholar] [CrossRef] [PubMed]
- Staiger, B. Disruptions to the Patient-Provider Relationship and Patient Utilization and Outcomes: Evidence from Medicaid Managed Care. J. Heal. Econ. 2021, 81, 102574–102574. [Google Scholar] [CrossRef]
- Stepleman, L.M.; Penwell-Waines, L.; Valvano, A. Integrated care psychologists and their role in patient transition from medical to psychiatric specialty care settings: a conceptual model. Heal. Psychol. Behav. Med. 2015, 3, 154–168. [Google Scholar] [CrossRef]
- Substance Abuse and Mental Health Services Administration. Behavioral health by race and ethnicity: Results from the 2021–2023 National Surveys on Drug Use and Health (SAMHSA Publication No. PEP24-07-022). Center for Behavioral Health Statistics and Quality, Substance Abuse and Mental Health Services Administration: Rockville, MD, 2024. Available online: https://www.samhsa.gov/data/sites/default/files/reports/rpt47097/2023-nsduh-race-eth-companion.pdf.
- Substance Abuse and Mental Health Services Administration. SAMHSA's working definition of recovery. 2012. Available online: https://library.samhsa.gov/product/samhsas-working-definition-recovery/pep12-recdef.
- Sung, B.; O’driscoll, F.; Gregory, A.; Grailey, K.; Franklin, H.; Poon, S.; Lawrence-Jones, A.; Shepherd, L.; McCrudden, C.; Klaber, B.; et al. Identifying barriers to outpatient appointment attendance in patient groups at risk of inequity: a mixed methods study in a London NHS trust. BMC Heal. Serv. Res. 2024, 24, 1–13. [Google Scholar] [CrossRef]
- Sweetman, J.; Knapp, P.; Varley, D.; Woodhouse, R.; McMillan, D.; Coventry, P. Barriers to attending initial psychological therapy service appointments for common mental health problems: A mixed-methods systematic review. J. Affect. Disord. 2021, 284, 44–63. [Google Scholar] [CrossRef]
- Swift, J.K.; Greenberg, R.P. Premature discontinuation in adult psychotherapy: A meta-analysis. J. Consult. Clin. Psychol. 2012, 80, 547–559. [Google Scholar] [CrossRef]
- Tarescavage, A.M.; Finn, J.A.; Marek, R.J.; Ben-Porath, Y.S.; van Dulmen, M.H. Premature termination from psychotherapy and internalizing psychopathology: The role of demoralization. J. Affect. Disord. 2015, 174, 549–555. [Google Scholar] [CrossRef]
- Thomsen, D.K.; Cowan, H.R.; McAdams, D.P. Mental illness and personal recovery: A narrative identity framework. Clin. Psychol. Rev. 2025, 116, 102546. [Google Scholar] [CrossRef] [PubMed]
- Thrower, N.E.; Berry, K.; Johnston, I.; Morris, L. Understanding the Factors That Contribute to Creating a Collaborative Psychological Formulation: A Qualitative Systematic Review. Clin. Psychol. Psychother. 2024, 31, e2998. [Google Scholar] [CrossRef] [PubMed]
- Tune, K.N.; Zachrison, K.S.; Pines, J.M.; Zheng, H.; Hayden, E.M. Estimating the Proportion of Telehealth-Able United States Emergency Department Visits. Ann. Emerg. Med. 2025, 85, 428–435. [Google Scholar] [CrossRef] [PubMed]
- Tzenios, N. The determinants of access to healthcare: A review of individual, structural, and systemic factors. Journal of Humanities and Applied Science Research 2019, 2(1), 1–14. Available online: https://journals.sagescience.org/index.php/JHASR/article/view/23/26.
- Walmsley, I. Coping With the Persistence of Stigma in Recovery: A Qualitative Examination of the Disclosure Experiences of People in Recovery From Problem Drug Use From the Perspective of Modified Labeling Theory. Contemp. Drug Probl. 2025, 53, 160–177. [Google Scholar] [CrossRef]
- Declercq, F.; Vanheule, S.; Deheegher, J. Alexithymia and posttraumatic stress: subscales and symptom clusters. J. Clin. Psychol. 2010, 66, 1076–1089. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).