Submitted:
20 March 2026
Posted:
23 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
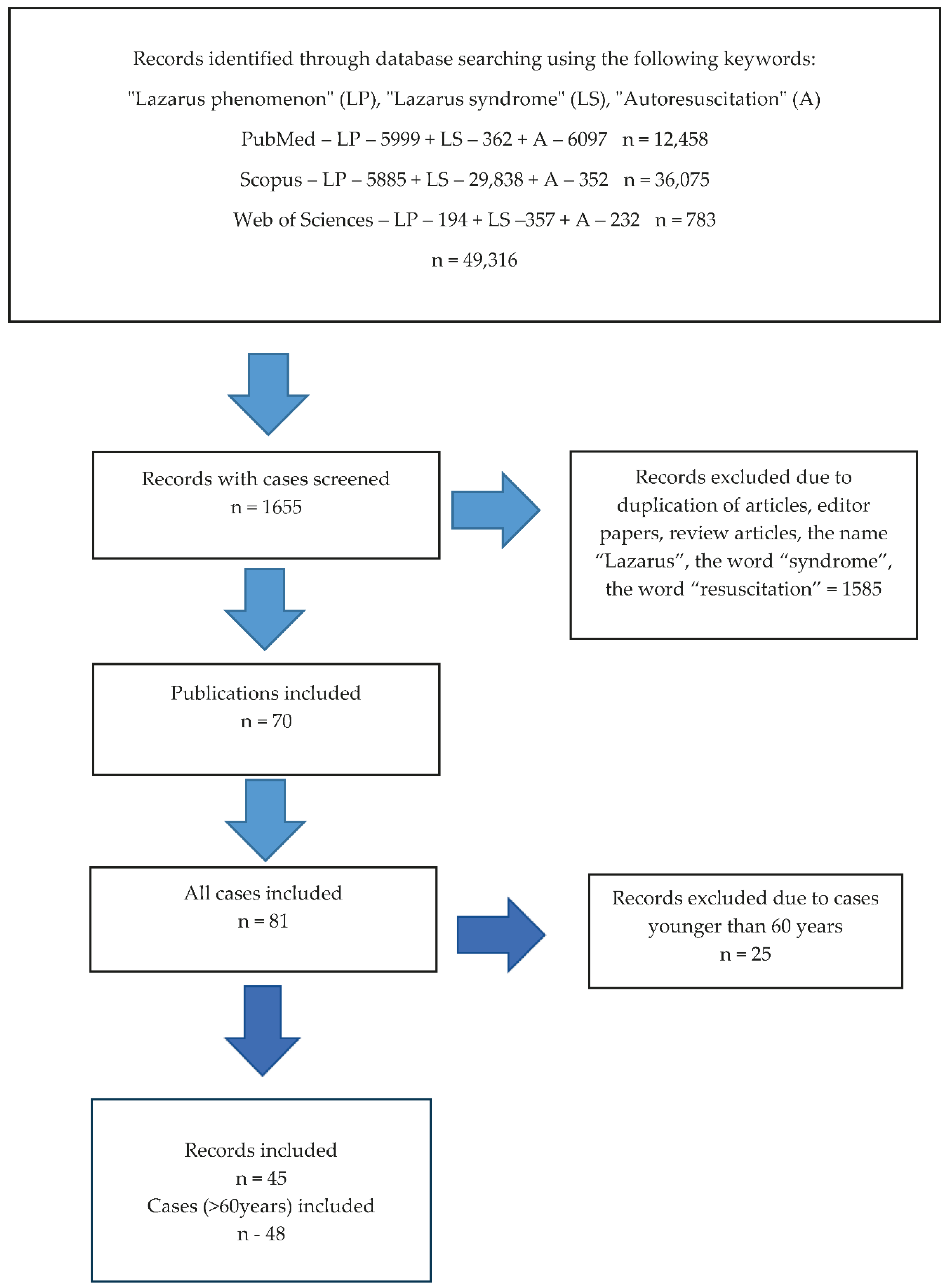
2. The Methods
| Analysed categories among 48 cases | Number of missing data |
|---|---|
| Causes of cardiac arrest (C or NC) | 6 |
| Place of cardiac arrest (IH or OH) | 16 |
| Time of CPR | 7 |
| Rhythm during CPR before occurrence of the LP | 4 |
| Time from cessation of cardiopulmonary resuscitation to the occurrence of the LP | 7 |
| Return of consciousness | 8 |
| Survival | 13 |
3. Results
4. Discussion
5. Conclusions
6. Limitations of the Study
References
- Linko, K.; Honkavaara, P.; Salmenpera, M. RECOVERY AFTER DISCONTINUED CARDIOPULMONARY RESUSCITATION. Lancet 1982, 319, 106–107. [Google Scholar] [CrossRef] [PubMed]
- Bray, JG, Jr. : The Lazarus phenomenon revisited. Anesthesiology 1993, 78, 991. [Google Scholar] [CrossRef]
- Wijdicks, EF; Diringer, MN. Electrocardiographic activity after terminal cardiac arrest in neurocatastrophes. Neurology 2004, 62, 673–4. [Google Scholar] [CrossRef]
- Schlichtig, R; Miro, A. : Auto-PEEP during CPR. An “occult” cause of electromechanical dissociation? Chest 1991, 99, 492–493. [Google Scholar]
- Kämäräinen, A.; Virkkunen, I.; Holopainen, L.; Erkkilä, E.-P.; Yli-Hankala, A.; Tenhunen, J. Spontaneous defibrillation after cessation of resuscitation in out-of-hospital cardiac arrest: A case of Lazarus phenomenon. Resuscitation 2007, 75, 543–546. [Google Scholar] [CrossRef] [PubMed]
- Gutierrez, SG S; Montoro, VD; Gómez JMG, GM. Dynamic hyperinflation, a case report. Pediatrics International 2020, 62(5), 647–649. [Google Scholar] [CrossRef] [PubMed]
- Berlin, D. Hemodynamic Consequences of Auto-PEEP. J. Intensiv. Care Med. 2012, 29, 81–86. [Google Scholar] [CrossRef]
- Brieler, J.; Breeden, M.A.; Tucker, J. Cardiomyopathy: An Overview. Am. Fam. Physician 2017, 96, 640–646. [Google Scholar]
- Morgan, R.W.; Fitzgerald, J.C.; Weiss, S.L.; Nadkarni, V.M.; Sutton, R.M.; Berg, R.A. Sepsis-associated in-hospital cardiac arrest: Epidemiology, pathophysiology, and potential therapies. J. Crit. Care 2017, 40, 128–135. [Google Scholar] [CrossRef]
- Hirlekar, G.; Karlsson, T.; Aune, S.; Ravn-Fischer, A.; Albertsson, P.; Herlitz, J.; Libungan, B. Survival and neurological outcome in the elderly after in-hospital cardiac arrest. Resuscitation 2017, 118, 101–106. [Google Scholar] [CrossRef]
- Zorko, D.J.; Shemie, J.; Hornby, L.; Singh, G.; Matheson, S.; Sandarage, R.; Wollny, K.; Kongkiattikul, L.; Dhanani, S. Autoresuscitation after circulatory arrest: an updated systematic review. Can. J. Anaesth. 2023, 70, 699–712. [Google Scholar] [CrossRef]
- Grześkowiak, M.; Gaczkowska, A.; Kluzik, A.; Rzeźniczek, P.; Pytliński, A. Remarks on autoresuscitation—Polish analysis of Lazarus syndrome. Can. J. Anaesth. 2023, 71, 302–303. [Google Scholar] [CrossRef]
- Rzeźniczek, P.; Gaczkowska, A.D.; Kluzik, A.; Cybulski, M.; Bartkowska-Śniatkowska, A.; Grześkowiak, M. Lazarus Phenomenon or the Return from the Afterlife—What We Know about Auto Resuscitation. J. Clin. Med. 2023, 12, 4704. [Google Scholar] [CrossRef]
- Einav, S.; Cortegiani, A.; Marcus, E.-L. Cardiac arrest in older adult patients. Curr. Opin. Anaesthesiol. 2021, 34, 40–47. [Google Scholar] [CrossRef]
- Heuser, N.; Rupp, D.; Glass, S.; Sassen, M.C.; Morin, A.; Volberg, C. Influences on the duration and success of out-of-hospital resuscitation of geriatric patients over 80 years of age - a retrospective evaluation. BMC Emerg. Med. 2024, 24, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Rajan, S.; Folke, F.; Hansen, S.M.; Hansen, C.M.; Kragholm, K.; Gerds, T.A.; Lippert, F.K.; Karlsson, L.; Møller, S.; Køber, L.; et al. Incidence and survival outcome according to heart rhythm during resuscitation attempt in out-of-hospital cardiac arrest patients with presumed cardiac etiology. Resuscitation 2017, 114, 157–163. [Google Scholar] [CrossRef] [PubMed]
- Havranek, S.; Fingrova, Z.; Rob, D.; Smalcova, J.; Kavalkova, P.; Franek, O.; Smid, O.; Huptych, M.; Dusik, M.; Linhart, A.; et al. Initial rhythm and survival in refractory out-of-hospital cardiac arrest. Post-hoc analysis of the Prague OHCA randomized trial. Resuscitation 2022, 181, 289–296. [Google Scholar] [CrossRef]
- Molaschi, M; Ponzetto, M; Romin, R; Berrino, E; Fabris, F. Modificazioni dell’elettrocardiogramma nell’anziano. Limiti tra normalità e patologia [Changes in the electrocardiogram in the elderly patient. The limits between normality and pathology]. Recenti Prog Med;Italian 1995, 86(1), 32–6. [Google Scholar] [PubMed]
- Basile, G.; Cucinotta, M.D.; Figliomeni, P.; Balbo, C.L.; Maltese, G.; Lasco, A. Electrocardiographic Changes in Centenarians: A Study on 42 Subjects and Comparison with the Literature. Gerontology 2011, 58, 216–220. [Google Scholar] [CrossRef] [PubMed]
- Ngcobo, Nokwanda N. Influence of Ageing on the Pharmacodynamics and Pharmacokinetics of Chronically Administered Medicines in Geriatric Patients: A Review. Clinical Pharmacokinetics 2025, 64, 335–367. [Google Scholar] [CrossRef]
- Klotz, U. Pharmacokinetics and drug metabolism in the elderly. Drug Metab. Rev. 2009, 41, 67–76. [Google Scholar] [CrossRef] [PubMed]
- Klotz, U. Pharmacokinetics and drug metabolism in the elderly. Drug Metab. Rev. 2009, 41, 67–76. [Google Scholar] [CrossRef] [PubMed]
| Year . | Diseases before CA and place of CA (if known) | Age (years) |
Sex | Time of CPR (in min) | ECG rhythm before occurrence of the LP | Occurrence of the LP after cessation of CPR (min) |
Return of consciousness |
Survival (in days) |
|---|---|---|---|---|---|---|---|---|
|
Cases of Lazarus phenomenon among patients aged 79 - 60 years |
||||||||
| 1982 [1] | C - MI | 67 | M | 20 | A | < 9 | ND |
15 |
| C - MI 68 F ND A 20 Yes 90 | ||||||||
| 1991 [2] | NC, Co, IH 64 M 20 PEA 15 ND < 1 | |||||||
| 1991 [3] | NC, OH 75 F 20 A 5 No < 1 |
|||||||
| 1993 [4] | NC 75 M 23 A 5 No < 9 |
|||||||
| 1994 [5] | C, Co, IH 70 M 34 A 8 Yes 21 |
|||||||
| 1996 [6] | C, MI, IH 66 M 30 VF < 5 Yes S |
|||||||
| 1998 [7] | C, MI, IH 67 F 43 A 5 Yes 9 |
|||||||
| 1999 [8] | NC, Co, IH | 76 | M | 30 | A | 5 | No |
1 |
| 2001 [9] |
NC, Co, IH | 66 | M | 18 | A |
10 |
Yes | 13 |
| 2002 [10] | NC, Co, OH | 65 | M | 35 | A | 20 | No |
5 |
|
2005 [11] |
NC | 63 | F | 12 | A | 10 | Yes | 12 |
| 2006 [12] | C, MI, OH | 78 | M | 25 | A | < 9 | No |
< 1 |
| 2012 [13] | C, MI, OH | 65 | M | 55 |
A |
40 |
No | 13 |
|
2013 [14] |
NC, IH |
62 |
M |
40 |
PEA |
5 |
ND |
< 2 |
| 2015 [15] | NK, Co | 67 | M | 47 | PEA | 5 | Yes |
1 |
| 2016 [16] | NC | 69 | F | 25 | PEA | 10 | ND |
S |
| 2017 [17] | NC, OH | 69 | M | 40 | A | 180 | No |
10 |
| 2017 [18] |
NC, |
63 | M | 12 | PEA | 3 | Yes | > 1 |
|
NC, |
61 | F | 18 | PEA | 8 | No | < 1 | |
|
2017 [19] |
C, MI, Co | 66 | M | 45 |
PEA |
5 | Yes | 9 |
|
2020 [20] |
NC, OH | 79 | F | 9 | PEA | 14 | No | < 1 |
|
2021 [21] |
NC, Co, IH | 79 | F | 10 | A | 20 | ND |
14 |
|
2021 [22] |
IH | 66 | F | 32 | PEA | 5 | ND | ND |
|
2023 [23] |
C, OH 67 F 60 PEA 60 Yes S |
|||||||
|
2025 [24] |
C, OH 78 M 40 VF 3 ND < 1 |
|||||||
|
Cases of Lazarus phenomenon among patients aged ≥80 years | ||||||||
|
1982 [25] |
C, MI | 80 | M | 20 |
A |
5 | Yes |
35 |
| 1982 [26] | C, MI | 84 | M | 10 | A | 5 | No |
1 |
| 1993 [27] | NC, Co, IH | 87 | F | > 15 | ND | ND | ND |
12 |
| 1998 [28] | NC, Co | 80 | M | 30 | PEA | 5 | No |
2 |
| 2001 [29] | NC, Co, IH | 93 | F | 6 | ND | 5 | No |
ND |
|
2003 [30] |
NC, Co, IH | 81 | M | 25 | A | 2 | Yes | 31 |
|
2004 [31] |
C, MI, OH | 81 | F | 13 | A | < 9 | No |
< 1 |
|
2004 [32] |
NC, Co, IH | 94 | F | 40 | PEA | 3 | ND |
21 |
| 2005 [33] | C, MI, OH | 83 | F | 17 | A | 33 | No |
< 1 |
| 2006 [34] | C, OH | 83 | M | 60 | PEA | 7 | Yes |
ND |
|
2007 [35] |
NC, Co, IH | 85 | M | DNR | PEA | 6 | No |
2 |
|
2010 [36] |
NC, Co, OH | 84 | M | 15 | PEA | 5 | Yes | S |
| 2011 [37] | NC, Co, OH | 83 | M | 90 | A | 10 | No |
12 |
| 2013 [38] | NC, Co, IH | 89 | F | 18 | A | 5 | No |
< 16 |
| 2017 [39] | NK | 97 | F | 16 | A | 3 | No |
< 1 |
| NK | 91 | F | 16 | PEA | 3 | No |
< 1 |
|
| 2018 [40] | C, Co | 97 | M | DNR | A | ND | No |
< 1 |
|
2019 [41] |
C | 86 | F | DNR | A | 4 | Yes | S |
|
2019 [42] |
C, Co, OH | 86 | F | 40 | A | 15 | No | 3 |
|
2023 [43] NC, Co 88 M 20 PEA 60 No < 1 | ||||||||
|
2025 [44] C, OH 94 F DNR A 10 Yes S | ||||||||
|
2025 [45] C, Co, OH 88 F DNR A < 9 Yes S | ||||||||
| Analysed data | Group No 1 (n=26) | Group No 2 (n=22) |
|---|---|---|
| Causes of cardiac arrest | C – 10 NC - 14 | C - 10 NC - 8 |
| Place of CA | IH – 9 OH - 8 | IH – 7 OH - 8 |
| Gender | F – 10 M - 16 | F – 12 M - 10 |
| ECG rhythm during CPR before occurrence of LP | A – 14 PEA – 10, VF - 2 | A – 13 PEA - 7 |
| Return of consciousness | Y – 9 N - 9 | Y – 7 N - 13 |
| Time of CPR (in minutes) | n=25 mean – 29.72 median – 30.00 min-9.00 max-60,00 lower quartile – 20.00 upper quartile – 40.00 SD – 14.03 |
n=16 mean – 27.25 median – 19.00 min-6.00 max-9.00 lower quartile – 15.50 upper quartile – 35.00 SD – 21.60 |
| Time of cessation of CPR to the occurrence of the LP (in minutes) | n=23 mean – 20.04 median – 8.00 min-3.00 max-180.00 lower quartile – 5.00 upper quartile – 20.00 SD – 37.31 |
n=18 mean – 10.33 median – 5.00 min-2.00 max-60.00 lower quartile – 4.00 upper quartile – 10.00 SD – 14.29 |
| Time of survival (in days) | n=19 mean – 11.35 median – 9.00 min-0.002 max-90.00 lower quartile – 0.79 upper quartile – 13.00 SD – 20.12 |
n=16 mean – 7.57 median – 1.50 min-0.001 max-35.00 lower quartile – 0.21 upper quartile – 12.00 SD – 11.59 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




