Submitted:
19 March 2026
Posted:
20 March 2026
You are already at the latest version
Abstract
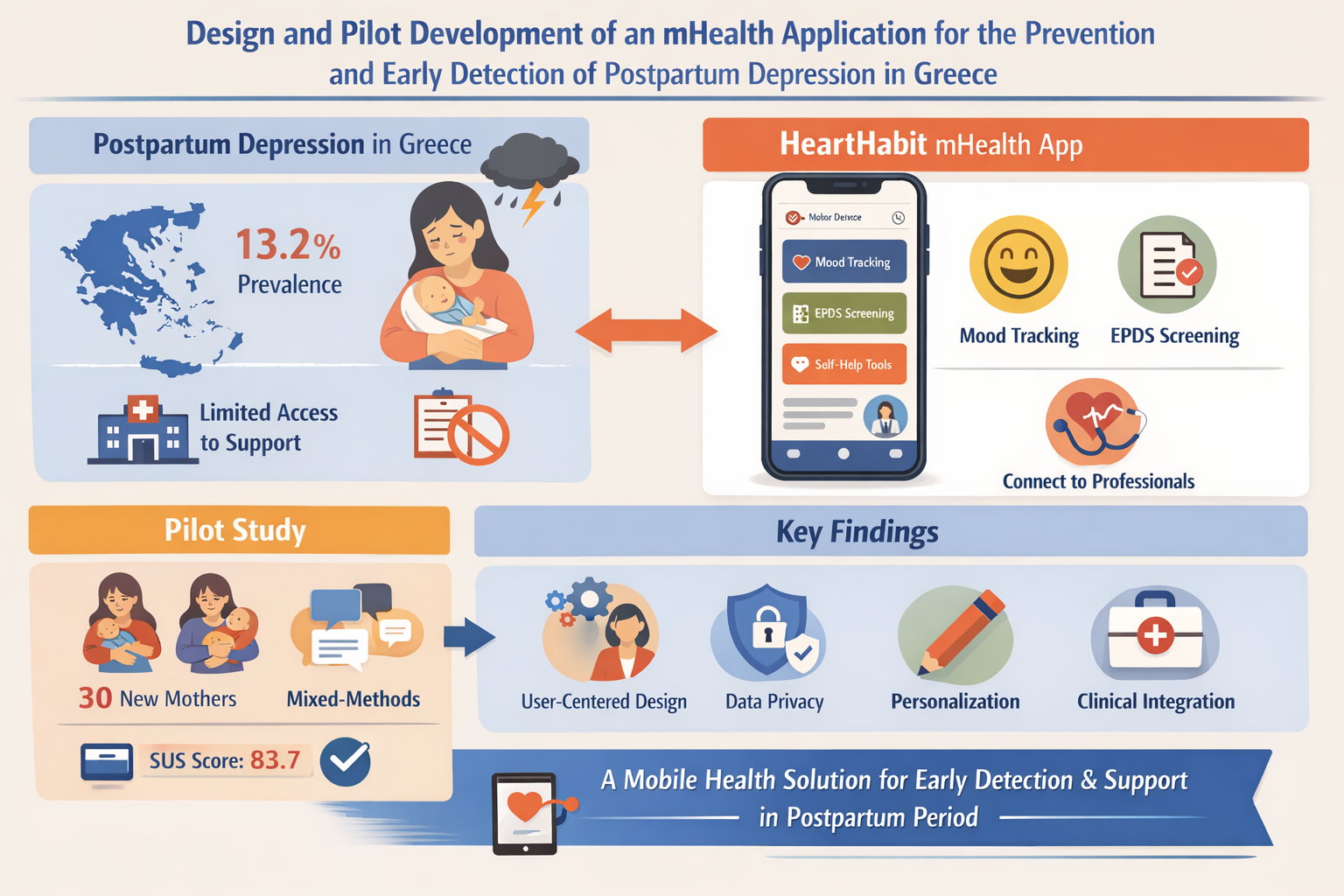
Keywords:
1. Introduction
2. Materials and Methods
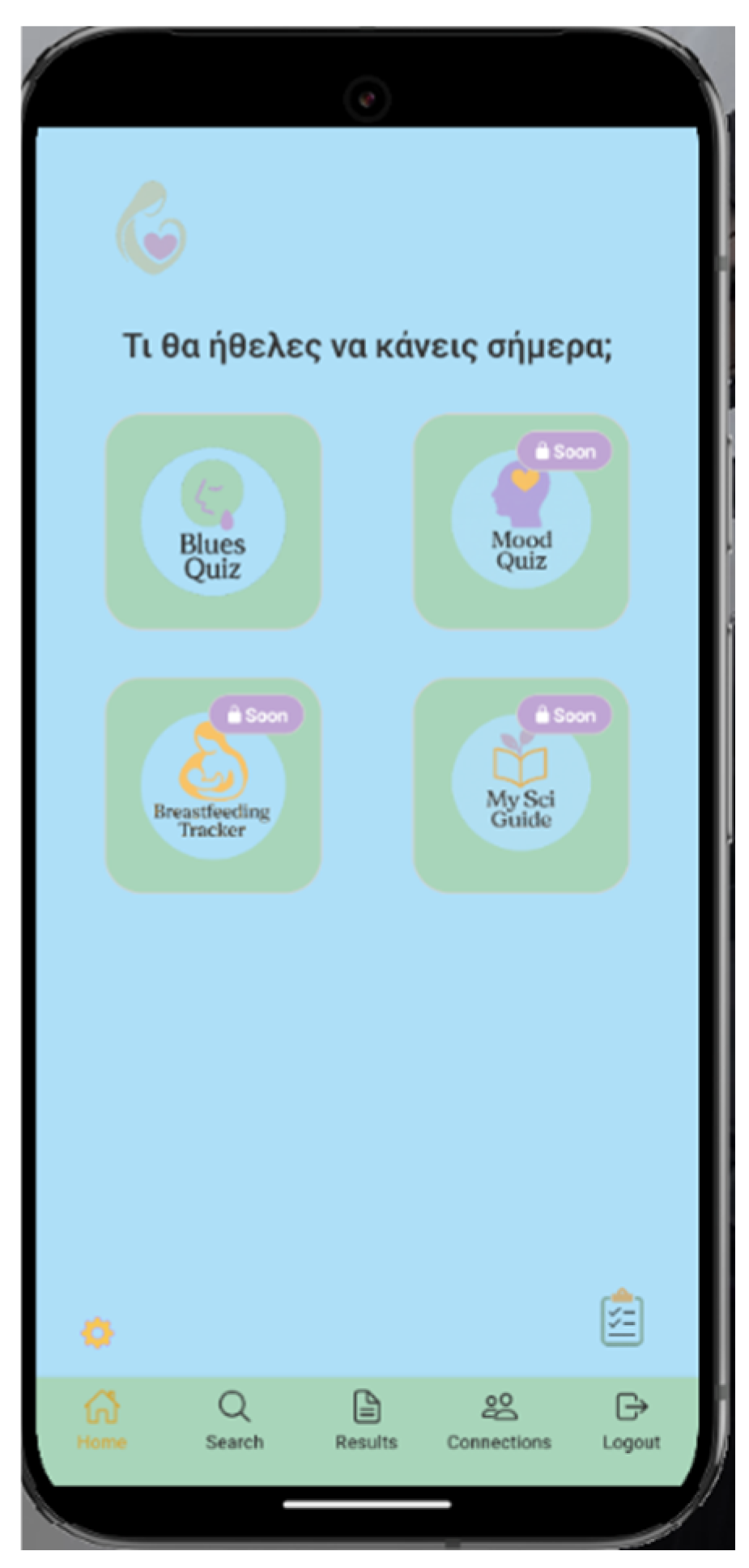
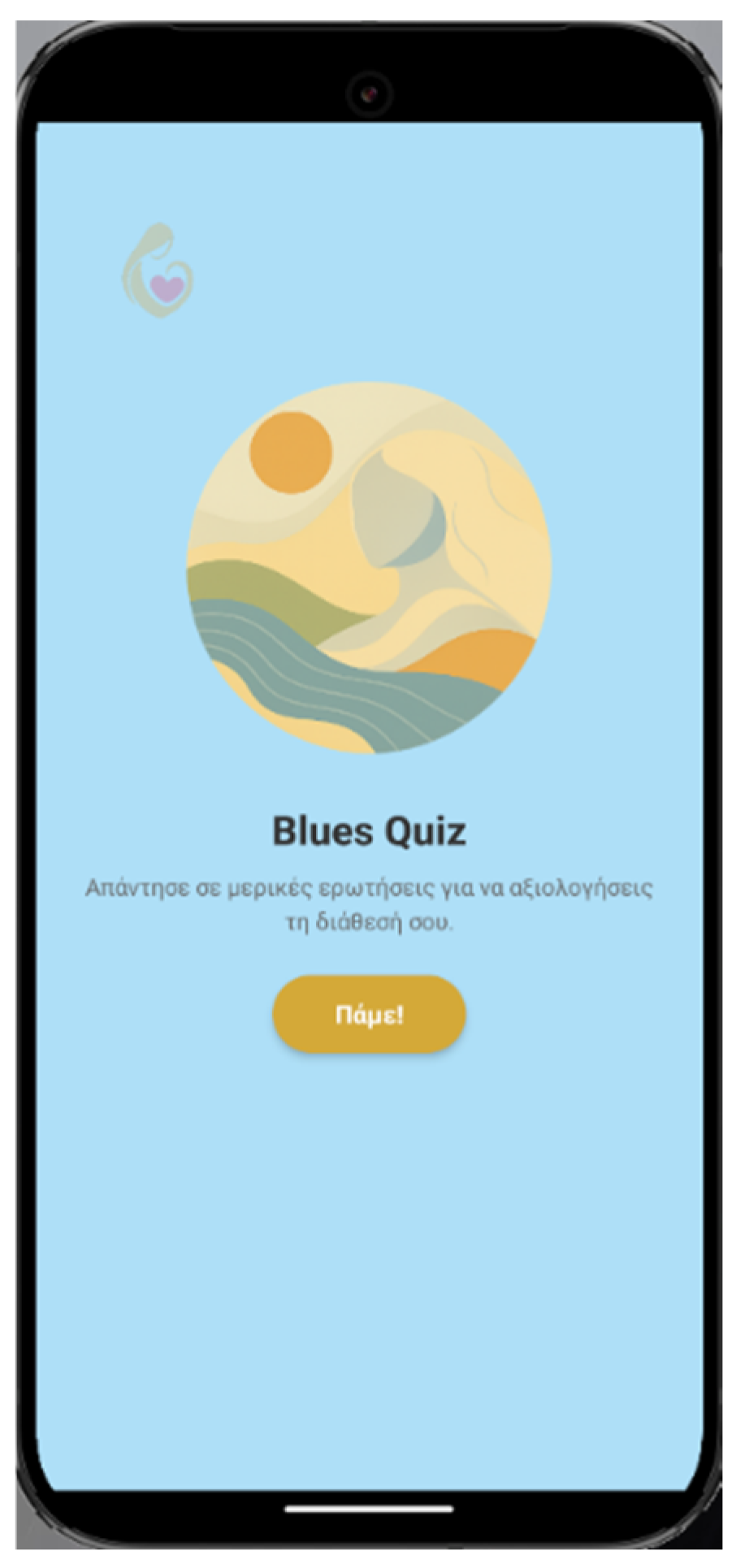
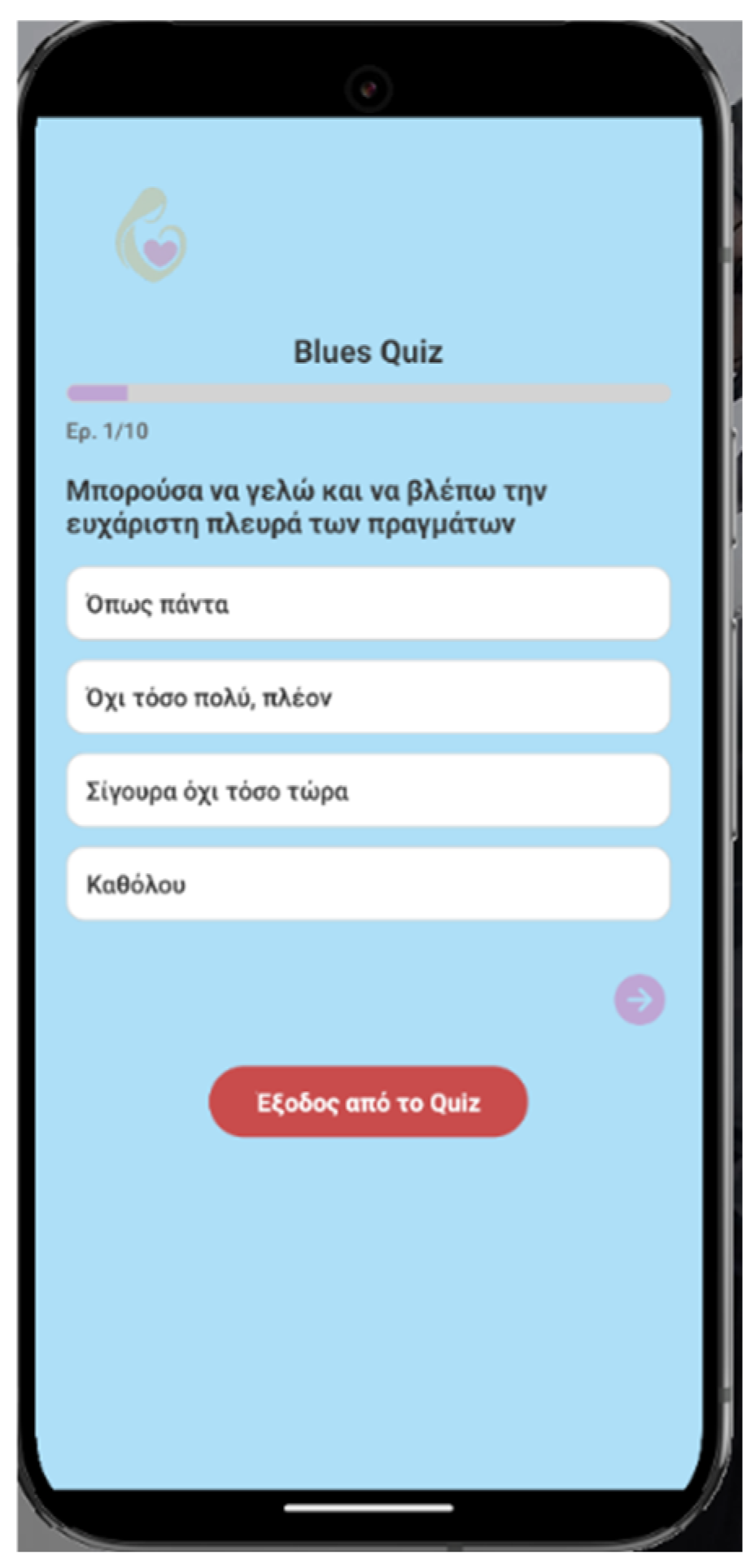
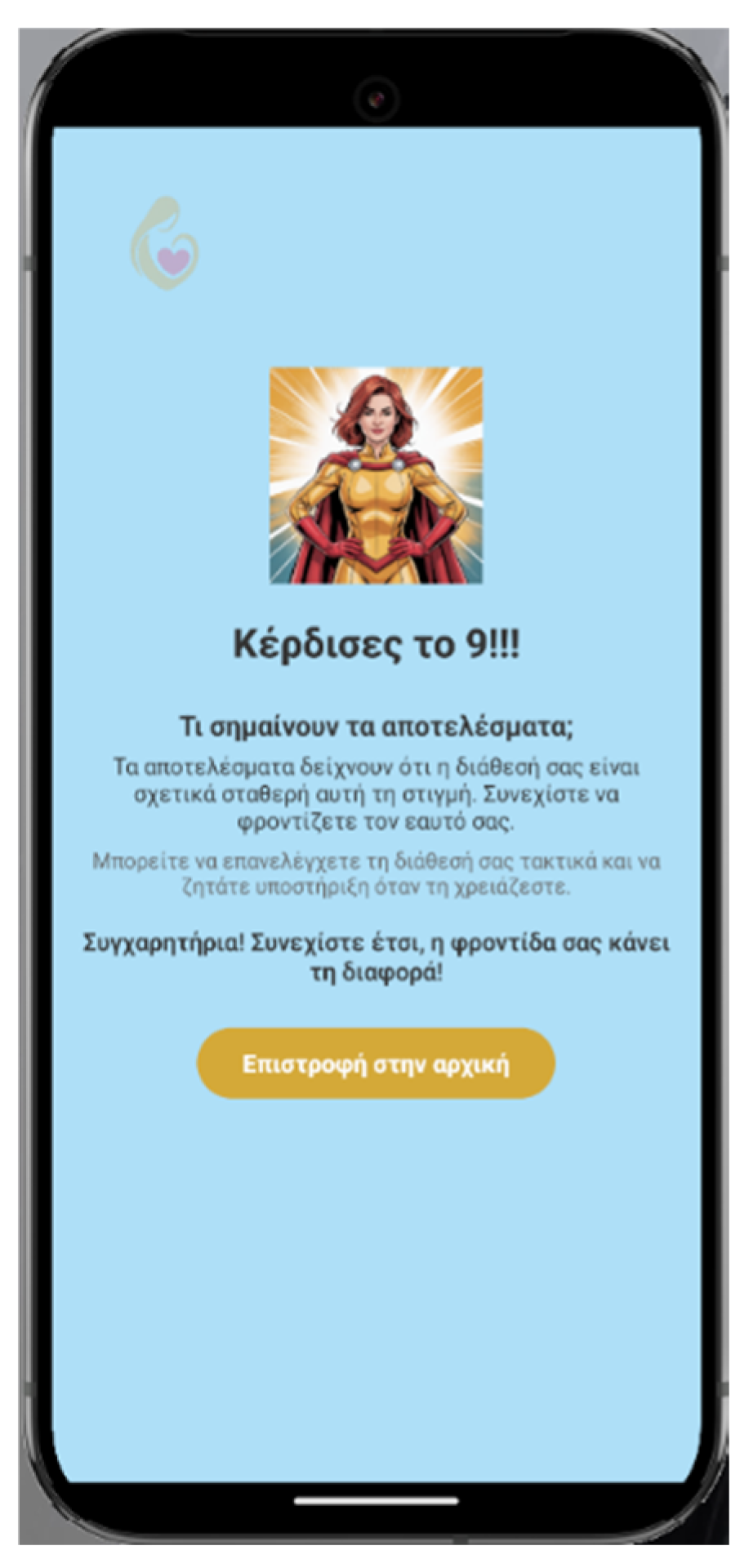
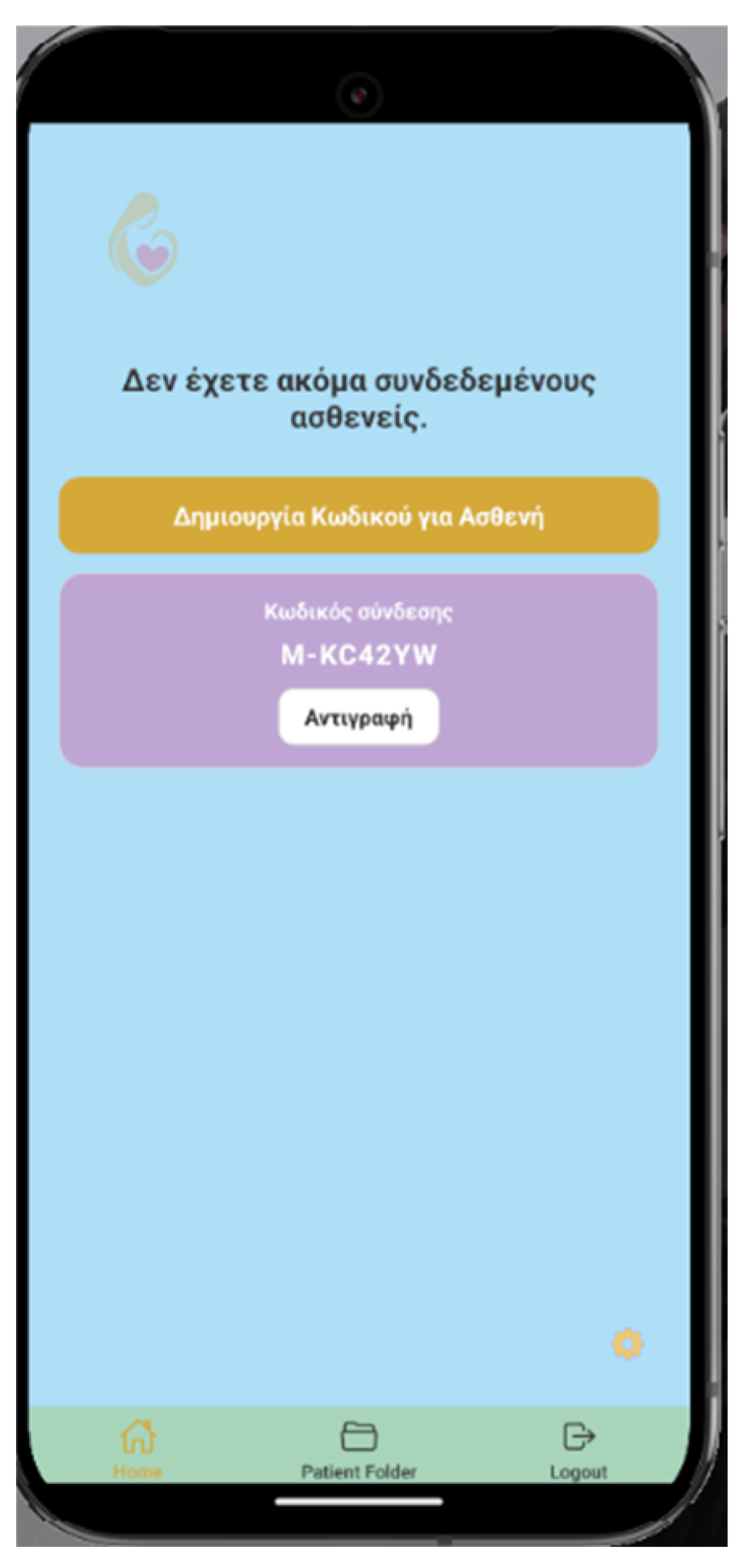
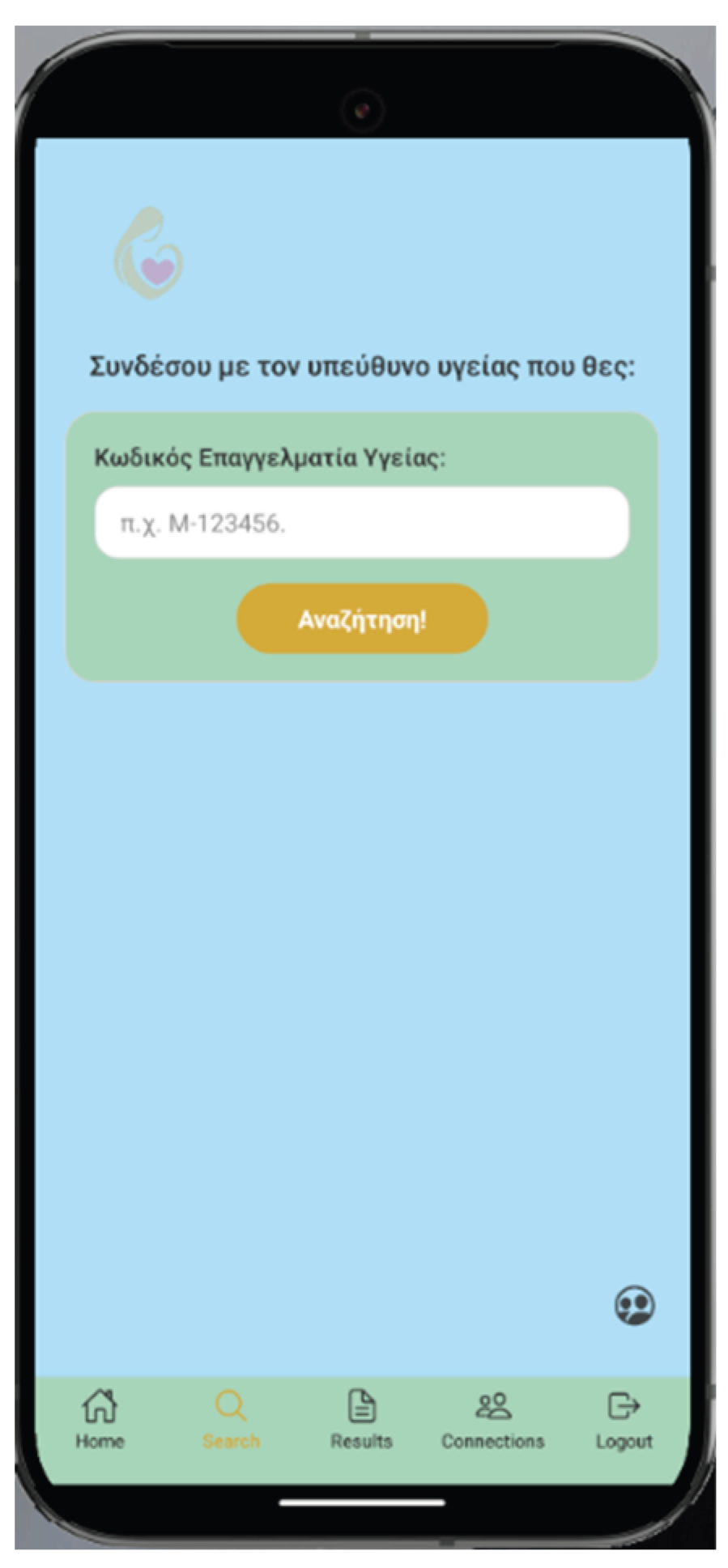
2.1. Smartphone Application “HeartHabit” – Alpha Version
2.2. Software and Equipment
2.3. Sample and Recruitment
2.4. Procedure of Pilot Evaluation
2.5. Data Analysis
2.6. Ethical Approval
3. Results
3.1. Participants’ Characteristics
3.2. Usability Evaluation
3.3. Quality and User Experience Evaluation
3.3.1. Engagement and Functionality
Practical Usability
Personalisation Features
Connectivity and Integration
Self-Regulation and Coping Support
3.3.2. Aesthetics
Soothing Visuals
User-Friendliness
Professional Design
3.3.3. Information Quality
Clarity of Information
Relevance of Content
Perceived Credibility
3.3.4. Privacy and Data Protection
Transparency and Data Governance
User Control and Data Autonomy
Anonymity and Identity Protection
4. Discussion
Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Amer, S. A.; Zaitoun, N. A.; Abdelsalam, H. A.; et al. Exploring predictors and prevalence of postpartum depression among mothers: Multinational study. BMC Public Health 2024, 24, 1308. [Google Scholar] [CrossRef]
- American Psychiatric Association. Diagnostic and statistical manual of mental disorders, 5th ed.; American Psychiatric Publishing, 2013. [Google Scholar]
- Anokye, R.; Acheampong, E.; Budu-Ainooson, A.; Obeng, E. I.; Akwasi, A. G. Prevalence of postpartum depression and interventions utilized for its management. Annals of General Psychiatry 2018, 17, 18. [Google Scholar] [CrossRef]
- Baumel, A.; Muench, F.; Edan, S.; Kane, J. M. Objective user engagement with mental health apps: Systematic search and panel-based usage analysis. Journal of Medical Internet Research 2019, 21(9), e14567. [Google Scholar] [CrossRef]
- Beck, K.; Beedle, M.; van Bennekum, A.; Cockburn, A.; Cunningham, W.; Fowler, M.; Grenning, J.; Highsmith, J.; Hunt, A.; Jeffries, R.; Kern, J.; Marick, B.; Martin, R. C.; Mellor, S.; Schwaber, K.; Sutherland, J.; Thomas, D. Manifesto for agile software development. 2001. https://agilemanifesto.org/.
- Bensenor, I. M.; Goulart, A. C.; Thomas, G. N.; Lip, G. Y. H.; NIHR Global Health Research Group on Atrial Fibrillation Management. Patient and public involvement and engagement (PPIE): First steps in the process of engagement in research projects in Brazil. Brazilian Journal of Medical and Biological Research 2022, 55, e12369. [Google Scholar] [CrossRef] [PubMed]
- Brooke, J. SUS: A “quick and dirty” usability scale. In Usability evaluation in industry; Jordan, P. W., Thomas, B., McClelland, I. L., Weerdmeester, B., Eds.; Taylor & Francis, 1996; pp. 189–194. [Google Scholar]
- Chan, G.; Alslaity, A.; Wilson, R.; Orji, R. Feeling Moodie: Insights from a usability evaluation to improve the design of mHealth apps. International Journal of Human–Computer Interaction 2023. [Google Scholar] [CrossRef]
- Chasiotis, G.; Stoyanov, S. R.; Karatzas, A.; Gravas, S. Greek validation of the user version of the Mobile Application Rating Scale (uMARS). Journal of International Medical Research 2023, 51(3), 03000605231161213. [Google Scholar] [CrossRef] [PubMed]
- Cox, J. L.; Holden, J. M.; Sagovsky, R. Detection of postnatal depression: Development of the 10-item Edinburgh Postnatal Depression Scale. British Journal of Psychiatry 1987, 150(6), 782–786. [Google Scholar] [CrossRef]
- Davis, F. D. Perceived usefulness, perceived ease of use, and user acceptance of information technology. MIS Quarterly 1989, 13(3), 319–340. [Google Scholar] [CrossRef]
- Deniz-Garcia, A.; Fabelo, H.; Rodriguez-Almeida, A.; Zamora-Zamorano, G.; Castro-Fernandez, M.; Alberiche Ruano, M.; Solvoll, T.; Granja, C.; Schopf, T.; Callico, G.; Soguero-Ruiz, C.; Wägner, A.; WARIFA Consortium. Quality, usability, and effectiveness of mHealth apps and the role of artificial intelligence: Current scenario and challenges. Journal of Medical Internet Research 2023, 25, e44030. [Google Scholar] [CrossRef]
- European Commission. Communication on a comprehensive approach to mental health (COM(2023) 298 final). 2023. https://health.ec.europa.eu/document/download/cef45b6d-a871-44d5-9d62-3cecc47eda89_en.
- Galletta, M. A. K.; Hashimoto, A. S.; de Almeida Estrambk, G.; Verardo, I. P. S.; Cantagalli, M. H. I.; Peres, S. V.; Francisco, R. P. V. Prevalence of postpartum depression in the COVID-19 pandemic and associated factors: Systematic review and meta-analysis. BMC Pregnancy and Childbirth 2026, 26(1), 157. [Google Scholar] [CrossRef]
- Regulation, General Data Protection. Regulation (EU) 2016/679 of the European Parliament and of the Council of 27 April 2016 on the protection of natural persons with regard to the processing of personal data and on the free movement of such data. Official Journal of the European Union. 2016. https://eur-lex.europa.eu/eli/reg/2016/679/oj.
- Huckvale, K.; Torous, J.; Larsen, M. E. Assessment of the data sharing and privacy practices of smartphone apps for depression and smoking cessation. JAMA Network Open 2019, 2(4), e192542. [Google Scholar] [CrossRef]
- Katsanos, C.; Tselios, N.; Xenos, M. Perceived usability evaluation of learning management systems: A first step towards standardization of the System Usability Scale in Greek. In Proceedings of the 16th Panhellenic Conference on Informatics, 2012; IEEE; pp. 302–307. [Google Scholar]
- Kendall-Tackett, K. A. Screening for perinatal depression: Barriers, guidelines, and measurement scales. Journal of Clinical Medicine 2024, 13(21), 6511. [Google Scholar] [CrossRef]
- Lazard, A. J.; Babwah Brennen, J.; Belina, S. App designs and interactive features to increase mHealth adoption: User expectation survey and experiment. JMIR mHealth and uHealth 2021, 9(11), e29815. [Google Scholar] [CrossRef]
- Leonardou, A.; Zervas, Y.; Papageorgiou, C.; Marks, M. N.; Tsartsara, E.; Antsaklis, A.; Christodoulou, G. N. Validation of the Edinburgh Postnatal Depression Scale and prevalence of postnatal depression at two months postpartum in a sample of Greek mothers. Journal of Reproductive and Infant Psychology 2009, 27(1), 28–39. [Google Scholar] [CrossRef]
- Lewkowitz, A.; Guillen, M.; Ursino, K.; Baker, R.; Lum, L.; Battle, C.; Ware, C.; Ayala, N.; Clark, M.; Ranney, M.; Miller, E.; Guthrie, K. Optimizing a novel smartphone app to prevent postpartum depression adapted from an evidence-based cognitive behavioral therapy program: Qualitative study. JMIR Human Factors 2024, 11, e63143. [Google Scholar] [CrossRef] [PubMed]
- Liu, X.; Wang, S.; Wang, G. Prevalence and risk factors of postpartum depression in women: A systematic review and meta-analysis. Journal of Clinical Nursing 2022, 31, 2665–2677. [Google Scholar] [CrossRef]
- Loughnan, S. A.; Butler, C.; Sie, A. A.; Grierson, A. B.; Chen, A. Z.; Hobbs, M. J.; Joubert, A. E.; Haskelberg, H.; Mahoney, A.; Holt, C.; Gemmill, A. W.; Milgrom, J.; Austin, M. P.; Andrews, G.; Newby, J. M. A randomised controlled trial of “MUMentum postnatal”: Internet-delivered cognitive behavioural therapy for anxiety and depression in postpartum women. Behaviour Research and Therapy 2019, 116, 94–103. [Google Scholar] [CrossRef]
- Mustafina, S. N.; Islam, M. N.; Mahjabin, M. R.; et al. Identifying key indicators to develop a novel mobile application for early screening of postpartum depression in developing countries. BMC Health Services Research 2025, 25, 287. [Google Scholar] [CrossRef] [PubMed]
- Panagiotakos, D. B.; Kouvari, M. Postpartum depression is associated with maternal sociodemographic and anthropometric characteristics, perinatal outcomes, breastfeeding practices, and Mediterranean diet adherence. Nutrients 2023, 15(17), 3853. [Google Scholar] [CrossRef] [PubMed]
- Slomian, J.; Honvo, G.; Emonts, P.; Reginster, J. Y.; Bruyère, O. Consequences of maternal postpartum depression: A systematic review of maternal and infant outcomes. Women’s Health 2019, 15, 1745506519844044. [Google Scholar] [CrossRef]
- Spitzer, R. L.; Kroenke, K.; Williams, J. B. W.; Löwe, B. A brief measure for assessing generalized anxiety disorder: The GAD-7. Archives of Internal Medicine 2006, 166(10), 1092–1097. [Google Scholar] [CrossRef]
- Stewart, D. E.; Vigod, S. N. Postpartum depression: Pathophysiology, treatment, and emerging therapeutics. Annual Review of Medicine 2019, 70, 183–196. [Google Scholar] [CrossRef] [PubMed]
- Stoyanov, S. R.; Hides, L.; Kavanagh, D. J.; Wilson, H.; et al. Development and validation of the user version of the Mobile Application Rating Scale (uMARS). JMIR mHealth and uHealth 2016, 4(2), e72. [Google Scholar] [CrossRef] [PubMed]
- Stoyanov, S. R.; Hides, L.; Kavanagh, D. J.; Zelenko, O.; Tjondronegoro, D.; Mani, M. Mobile App Rating Scale: A new tool for assessing the quality of health mobile apps. JMIR mHealth and uHealth 2015, 3(1), e27. [Google Scholar] [CrossRef] [PubMed]
- Tenaw, L. A.; Ngai, F. W.; Bessie, C. Effectiveness of psychosocial interventions in preventing postpartum depression among teenage mothers: Systematic review and meta-analysis of randomized controlled trials. Prevention Science 2024, 25, 1091–1103. [Google Scholar] [CrossRef]
- Torous, J.; Nicholas, J.; Larsen, M. E.; Firth, J.; Christensen, H. Clinical review of user engagement with mental health smartphone apps: Evidence, theory and improvements. Evidence-Based Mental Health 2018, 21(3), 116–119. [Google Scholar] [CrossRef]
- Vogazianos, P.; Motrico, E.; Domínguez-Salas, S.; Christoforou, A.; Hadjigeorgiou, E. Validation of the Generalized Anxiety Disorder Screener (GAD-7) in Cypriot pregnant and postpartum women. BMC Pregnancy and Childbirth 2022, 22, 841. [Google Scholar] [CrossRef]
- Wang, Z.; Liu, J.; Shuai, H.; Cai, Z.; Fu, X.; Liu, Y.; Xiao, X.; Zhang, W.; Krabbendam, E.; Liu, S.; Liu, Z.; Li, Z.; Yang, B. X. Mapping global prevalence of depression among postpartum women. Translational Psychiatry 2021, 11, 543. [Google Scholar] [CrossRef]
- World Health Organization. Comprehensive mental health action plan 2013–2030. 2021. https://www.who.int/publications/i/item/9789240031029.
- World Health Organization. Guide for integration of perinatal mental health in maternal and child health services. World Health Organization. 2022; https://www.who.int/publications/i/item/9789240057142.
- World Health Organization. Greece introduces a new 10-year national action plan for mental health to reform the provision of mental health services. European Observatory on Health Systems and Policies. 2023. https://eurohealthobservatory.who.int.
- World Wide Web Consortium. Understanding success criterion 1.4.3: Contrast (minimum). 2016. https://www.w3.org/TR/UNDERSTANDING-WCAG20/visual-audio-contrast-contrast.html.
| MARS Domain | Description |
| Engagement | Measures how well the app captures and maintains user interest, including entertainment value, interactivity, customization, and appropriateness for the target group. |
| Functionality | Evaluates how well the app works technically, including performance, ease of use, navigation, and gestural design. |
| Aesthetics | Assesses the visual design and appearance of the app, including layout, graphics, and overall visual appeal. |
| Information Quality | Evaluates the quality and credibility of the information provided, including accuracy, quality and quantity of content, and evidence base. |
| Characteristic | n | % |
| Age (years) | ||
| Mean (SD) | 31 (4.3) | |
| Range | 21–38 | |
| Nationality | ||
| Greek | 27 | 90 |
| Romanian | 2 | ≈7 |
| Albanian | 1 | ≈3 |
| Area of residence | ||
| Urban | 22 | ≈73 |
| Semi-urban | 5 | ≈17 |
| Rural | 3 | 10 |
| Mode of delivery | ||
| Caesarean section | 18 | 60 |
| Vaginal birth | 12 | 40 |
| Breastfeeding status | ||
| Mixed feeding | 11 | ≈37 |
| Exclusive breastfeeding | 11 | ≈37 |
| Marital status | ||
| Married | 25 | ≈83 |
| Civil partnership | 3 | 10 |
| Divorced | 2 | ≈7 |
| Infant age (months) | ||
| Range | 1–12 | |
| 0–3 months | 8 | ≈27 |
| 4–6 months | 8 | ≈27 |
| 7–9 months | 7 | ≈23 |
| 10–12 months | 7 | ≈23 |
| Number of children | ||
| 1 | 13 | ≈43 |
| 2 | 11 | ≈37 |
| 3 | 4 | ≈13 |
| 4 | 2 | ≈7 |
| Familiarity with mobile apps | ||
| High | 22 | ≈73 |
| Moderate | 5 | ≈17 |
| Low | 3 | 10 |
| Prior experience with mental health apps | ||
| Yes | 9 | 30 |
| No | 21 | 70 |
| Device used | ||
| Android (incl. tablet) | 25 | ≈83 |
| iOS | 4 | ≈14 |
| Tablet only | 1 | ≈3 |
| EPDS Severity Category | n | % |
| 0–9 Low likelihood | 20 | ≈67 |
| 10–12 Possible (mild) | 7 | ≈23 |
| 13–14 Probable (moderate) | 1 | ≈3 |
| 15+ Severe | 2 | ≈7 |
| Total | 30 | 100 |
| GAD-7 Severity Category | n | % |
| 5–9 Mild | 5 | ≈17 |
| 10–14 Moderate | 19 | ≈63 |
| 15–21 Severe | 6 | 20 |
| Total | 30 | 100 |
|
Theme 1: Engagement and Functionality | |
| Subthemes: | Practical usability Personalisation features Connectivity and integration Self-regulation and coping support |
|
Theme 2: Aesthetics | |
| Subthemes: | Soothing visuals User-friendliness Professional design |
|
Theme 3: Information Quality | |
| Subthemes: | Clarity of information Relevance of content Perceived credibility |
| Theme 4: Privacy and Data Protection | |
| Subthemes: | Transparency and data governance User control and data autonomy Anonymity and identity protection |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




