Submitted:
18 March 2026
Posted:
19 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Data Collection
2.2.1. Questionnaire Survey
2.2.2. Body Composition Testing
2.2.3. Resting Metabolic Rate Testing
2.2.4. Quality Control
2.3. Statistical Analysis
2.4. Ethical Approval
3. Results
3.1. General Characteristics of Participants
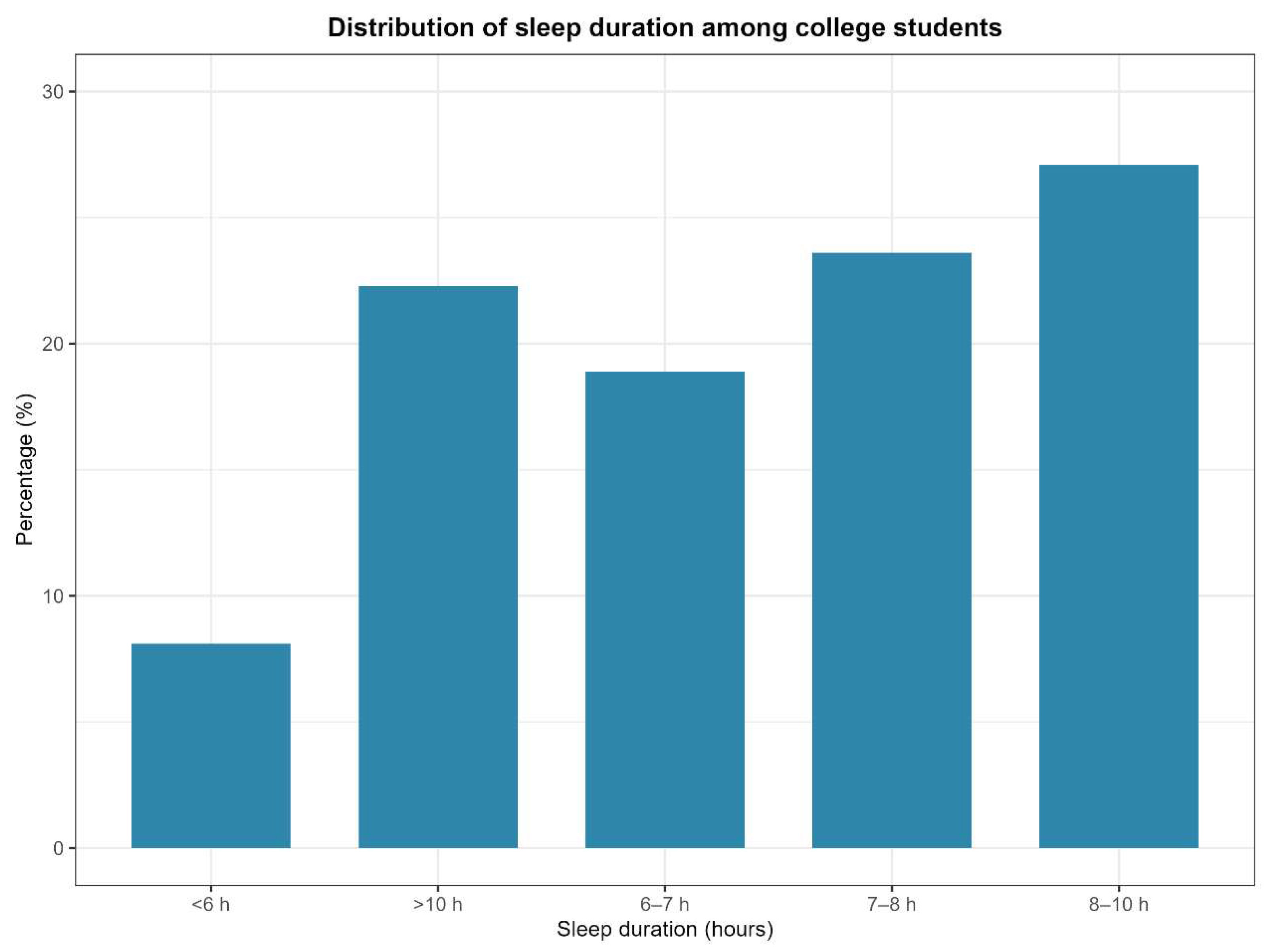
3.2. Sleep Timing Characteristics Among College Students
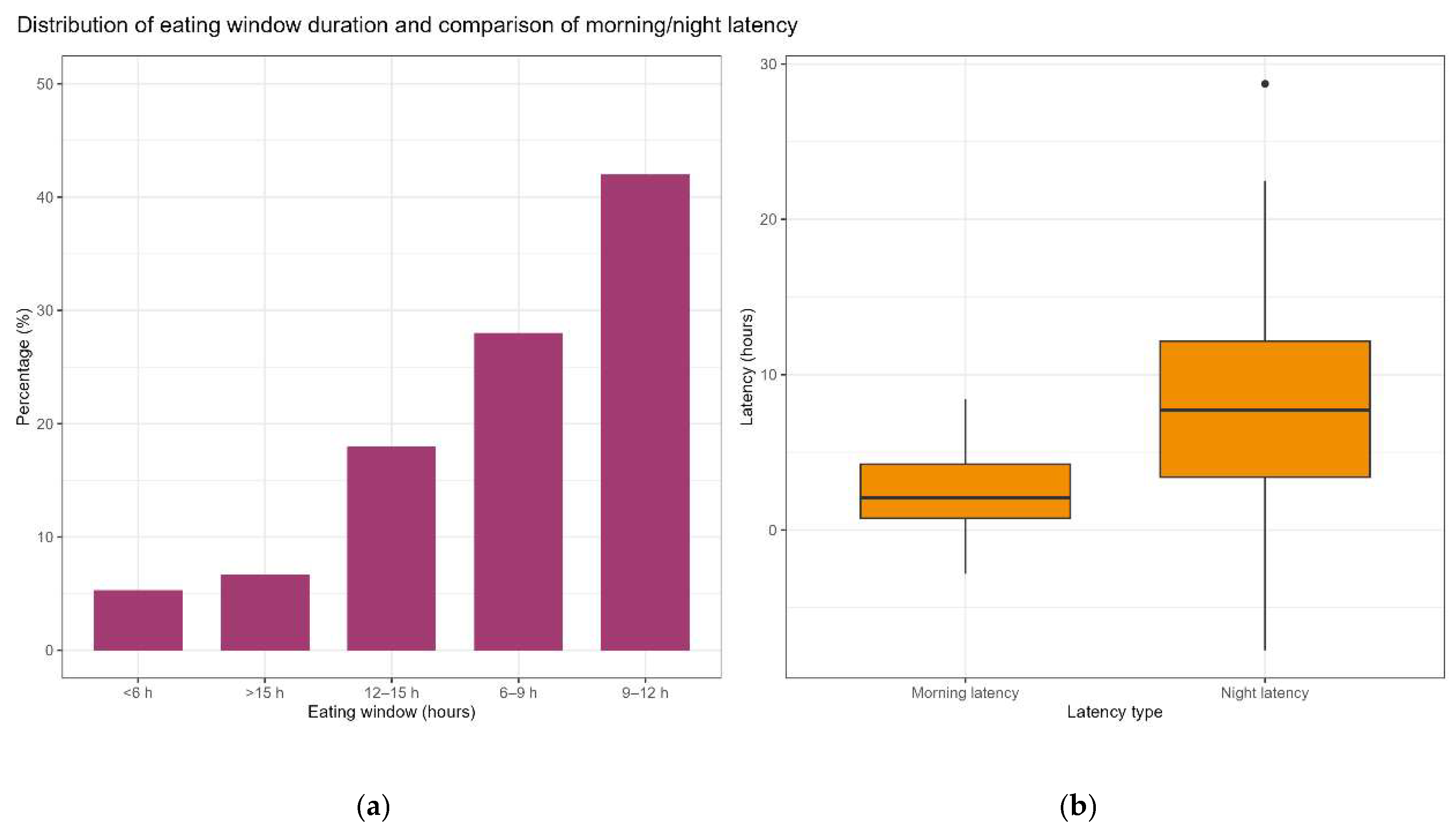
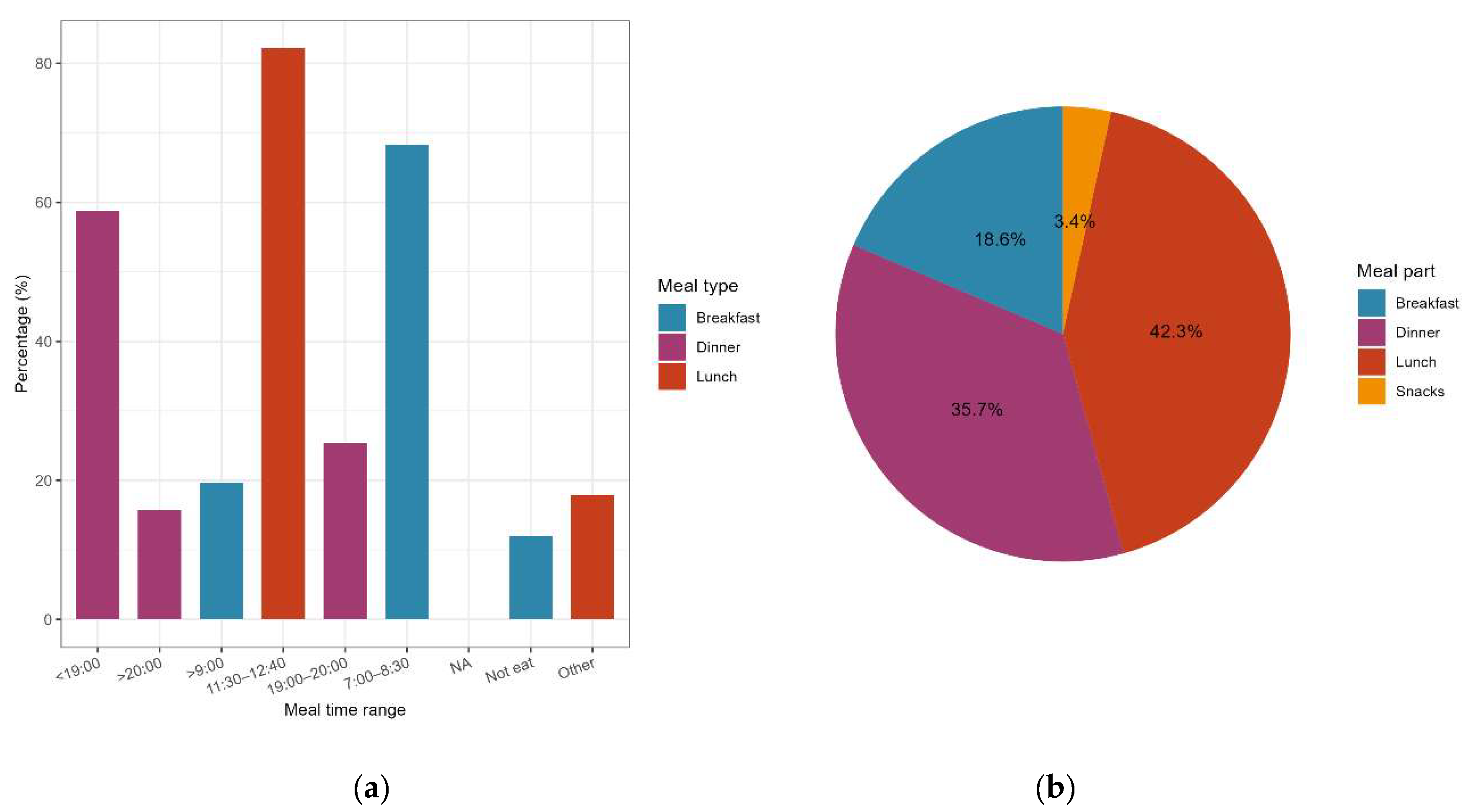
3.3. Distribution Characteristics of Eating Chronotypes Among College Students
3.4. Frequency-Related Chrononutrition Behaviors Among College Students
3.4.1. Breakfast Consumption Behavior
3.4.2. Distribution of the Most Abundant Meal
3.4.3. Post-Meal Snacks and Night Eating Behaviors
| Dietary Behavior Type |
Sample Size (n) |
Mean Frequency | Distribution Details | |
| Breakfast consumption behavior |
169 | 3.9 days/week | Never eat: 10.1%; Occasional (1–3 days): 36.7%; Frequent (4–6 days): 38.5%; Daily (7 days): 14.8% | |
| Distribution of the most abundant meal |
174 | — | Lunch: 71.0%; Dinner: 26.0%; Breakfast: 2.4%; Others: 0.6% |
|
| Post-meal snacks | 169 | 2.6 days/week | Never eat: 14.8%; Occasional (1–3 days): 57.4%; Frequent (4–7 days): 27.8% | |
| Night eating behavior | 169 | — | No night eating: 90.5%; 1 day/week: 4.7%; 2 days/week: 3.6%; ≥3 days/week: 1.2% |
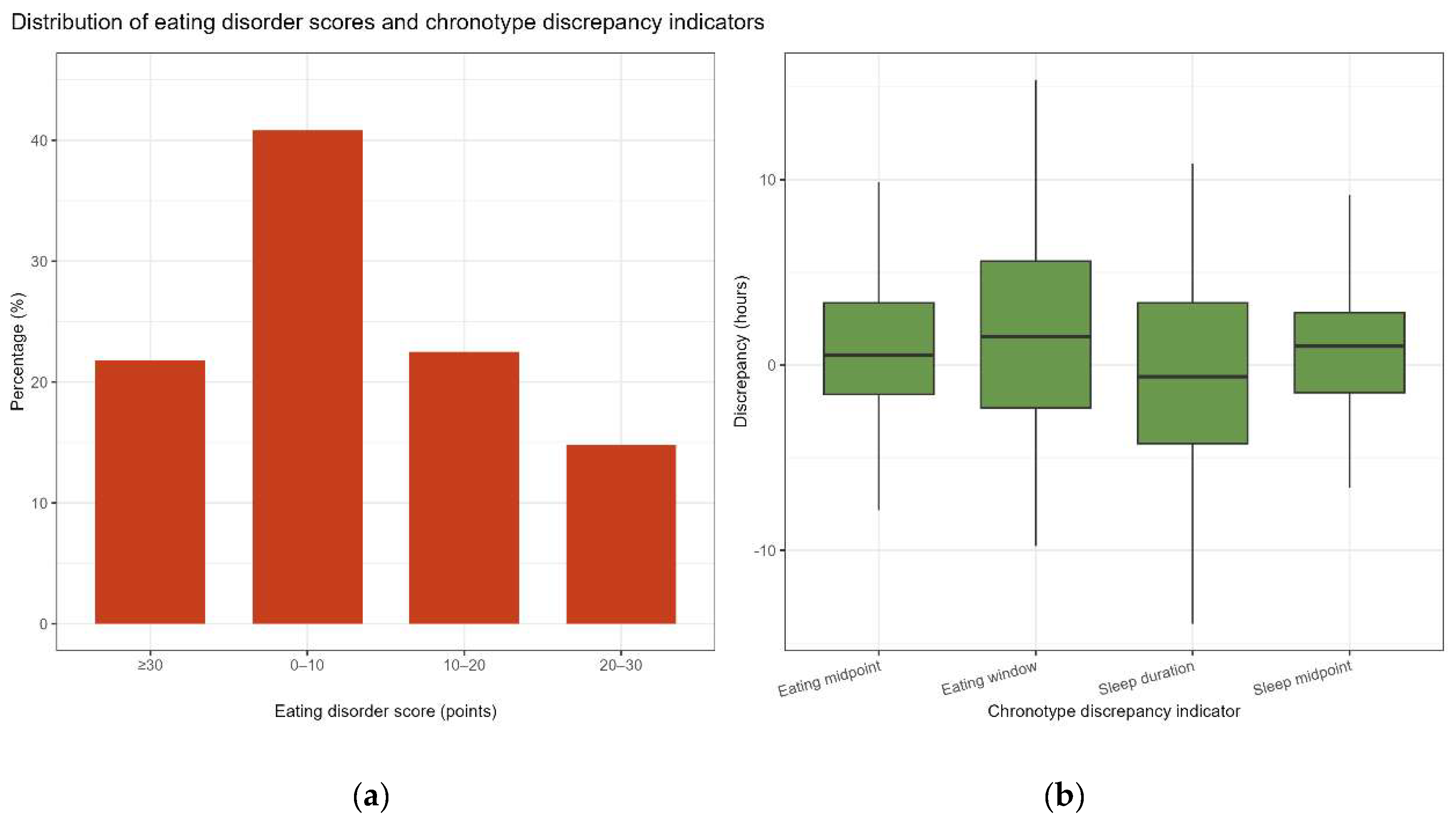
3.5. Chrononutrition Disturbance Score and Discrepancy Indicators Among College Students
3.6. Distribution Characteristics of Chrononutrition Patterns Among Chinese College Students
3.7. Chrononutrition Patterns on Weekdays vs. Weekends
3.8. Body Composition, Resting Metabolic Rate (RMR) and Body-Weight-Standardized RMR
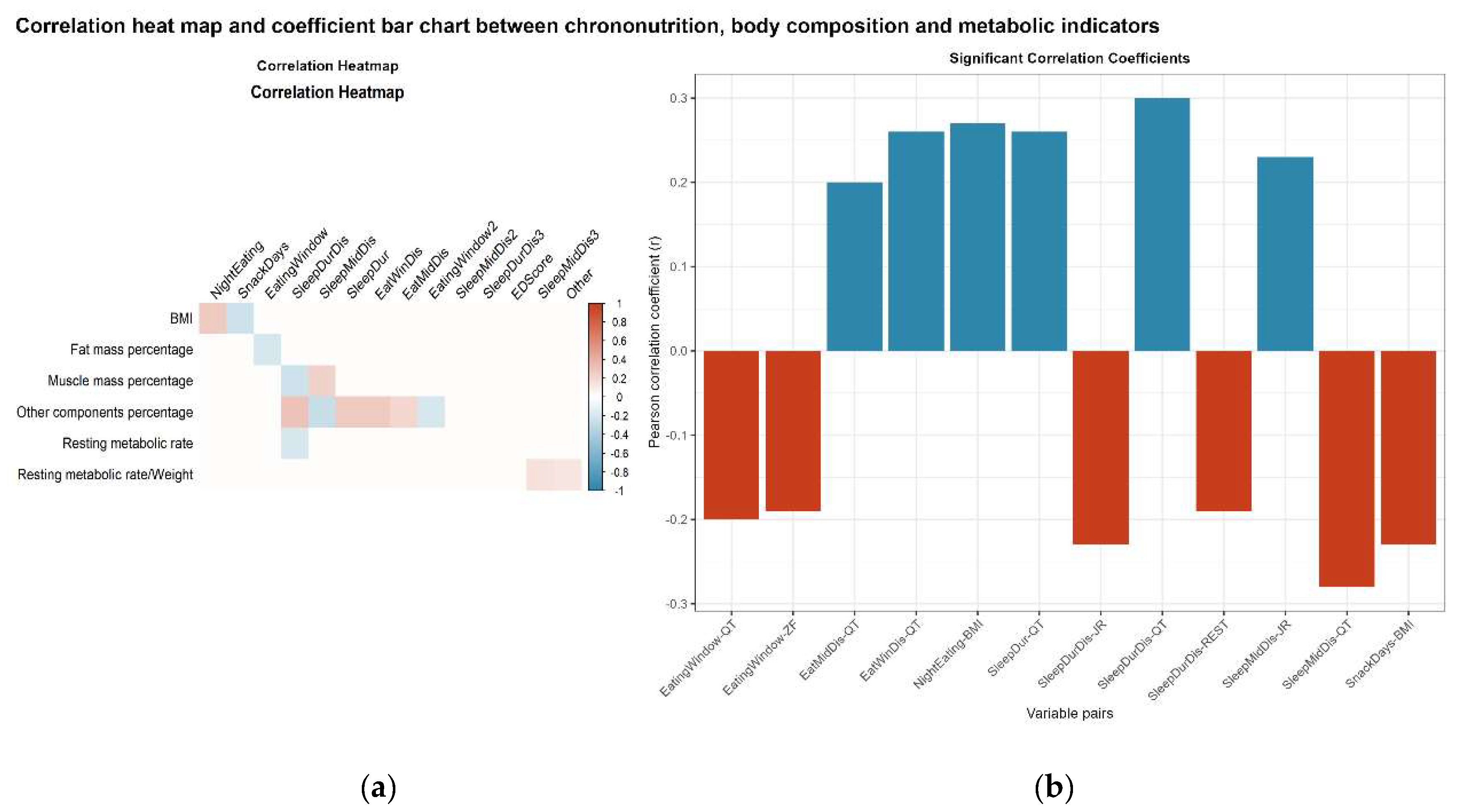
3.9. Correlation Analysis of Chrononutrition with Body Composition and Metabolic Indicators
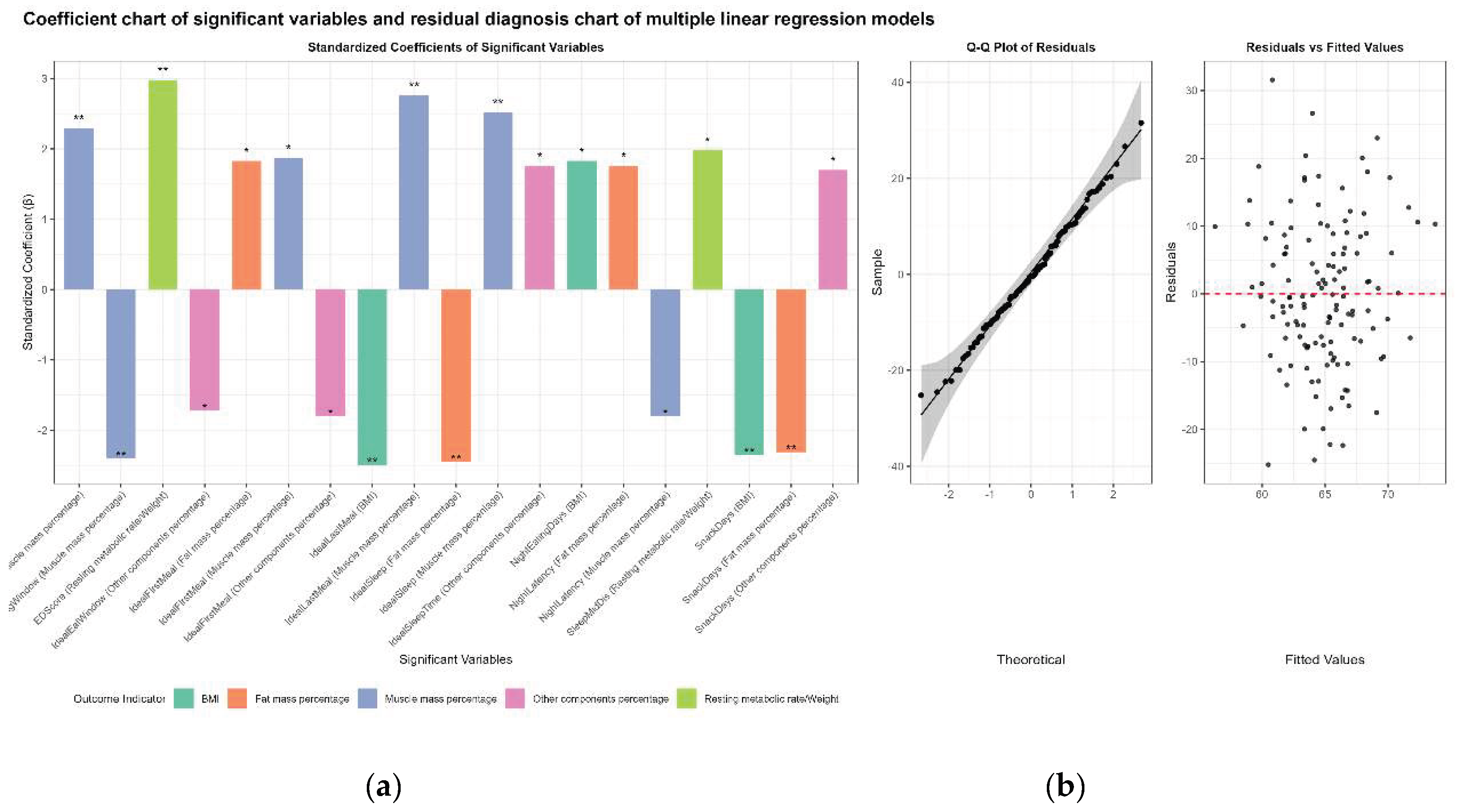
3.10. Multiple Linear Regression Analysis of the Associations of Chrononutrition with Body Composition and Metabolic Indicators
3.10.1. Common Influencing Factors
3.10.2. Independent Predictive Effect of Chrononutrition Behaviors in Each Model
3.10.3. Sex Interaction Effects
| Adjusted R² | Significant Chrononutrition Variables | β | sr² | P | Significance | Direction | |
| RMR | 0.46 | None | — | — | — | — | — |
| Standardized RMR | 0.20 | Chrononutrition disturbance score | 2.98 | 0.06 | 0.008 | ** | Positive |
| Sleep midpoint discrepancy | 1.98 | 0.04 | 0.042 | * | Positive | ||
| Muscle mass % | 0.41 | Ideal last meal time | 2.76 | 0.05 | <0.01 | ** | Positive |
| Ideal sleep time | 2.52 | 0.05 | <0.01 | ** | Positive | ||
| Weekday eating window | −2.40 | −0.05 | <0.01 | ** | Negative | ||
| Breakfast days/week | 2.29 | 0.05 | <0.01 | ** | Positive | ||
| Ideal first meal time | 1.87 | 0.03 | 0.045 | * | Positive | ||
| Night latency | −1.80 | −0.03 | 0.048 | * | Negative | ||
| Fat mass % | 0.29 | Ideal sleep time | −2.45 | −0.05 | <0.01 | ** | Negative |
| Snack days/week | −2.31 | −0.05 | <0.01 | ** | Negative | ||
| Ideal first meal time | 1.83 | 0.03 | 0.046 | * | Positive | ||
| Night latency | 1.76 | 0.03 | 0.049 | * | Positive | ||
| BMI | 0.20 | Ideal last meal time | −2.49 | −0.05 | <0.01 | ** | Negative |
| Snack days/week | −2.35 | −0.05 | <0.01 | ** | Negative | ||
| Night eating days/week | 1.83 | 0.03 | 0.046 | * | Positive |
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| RMR | Resting Metabolic Rate |
| DXA | Dual-Energy X-ray Absorptiometry |
| BMI | Body Mass Index |
| ICC | Intraclass Correlation Coefficient |
| FDR | False Discovery Rate |
| VIF | Variance Inflation Factor |
| CV | Coefficient of Variation |
| VO₂ | Oxygen Consumption |
| VCO₂ | Carbon Dioxide Production |
| APC | Article Processing Charge |
| SD | Standard Deviation |
| IQR | Interquartile Range |
| h | Hours |
| min | Minutes |
| kg | Kilograms |
| cm | Centimeters |
| kcal | Kilocalories |
References
- Almoosawi, S.; Vingeliene, S.; Gachon, F.; Voortman, T.; Palla, L.; Johnston, J.D.; Van Dam, R.M.; Darimont, C.; Karagounis, L.G. Chronotype: Implications for Epidemiologic Studies on Chrono-Nutrition and Cardiometabolic Health. Advances in Nutrition 2019, 10, 30–42. [Google Scholar] [CrossRef] [PubMed]
- Crispim, C.A.; Mota, M.C. New perspectives on chrononutrition. Biological Rhythm Research 2019, 50, 63–77. [Google Scholar] [CrossRef]
- Dashti, H.S.; Jansen, E.C.; Zuraikat, F.M.; Dixit, S.; Brown, M.; Laposky, A.; Broussard, J.L.; Butler, M.P.; Creasy, S.A.; Crispim, C.A.; et al. Advancing Chrononutrition for Cardiometabolic Health: A 2023 National Heart, Lung, and Blood Institute Workshop Report. J Am Heart Assoc 2025, 14, e039373. [Google Scholar] [CrossRef]
- Raji, O.E.; Kyeremah, E.B.; Sears, D.D.; St-Onge, M.P.; Makarem, N. Chrononutrition and Cardiometabolic Health: An Overview of Epidemiological Evidence and Key Future Research Directions. Nutrients 2024, 16. [Google Scholar] [CrossRef]
- Liu, H.Y.; Eso, A.A.; Cook, N.; O'Neill, H.M.; Albarqouni, L. Meal Timing and Anthropometric and Metabolic Outcomes: A Systematic Review and Meta-Analysis. JAMA Netw Open 2024, 7, e2442163. [Google Scholar] [CrossRef]
- Dote-Montero, M.; Acosta, F.M.; Sanchez-Delgado, G.; Merchan-Ramirez, E.; Amaro-Gahete, F.J.; Labayen, I.; Ruiz, J.R. Association of meal timing with body composition and cardiometabolic risk factors in young adults. Eur J Nutr 2023, 62, 2303–2315. [Google Scholar] [CrossRef] [PubMed]
- Wang, Z.R. Chronobiology; People’s Medical Publishing House: Beijing, China, 2008; p. 226. [Google Scholar]
- Tevy, M.F.; Giebultowicz, J.; Pincus, Z.; Mazzoccoli, G.; Vinciguerra, M. Aging signaling pathways and circadian clock-dependent metabolic derangements. Trends in Endocrinology & Metabolism 2013, 24, 229–237. [Google Scholar] [CrossRef]
- Makarem, N.; Paul, J.; Giardina, E.-G.V.; Liao, M.; Aggarwal, B. Evening chronotype is associated with poor cardiovascular health and adverse health behaviors in a diverse population of women. Chronobiology International 2020, 37, 673–685. [Google Scholar] [CrossRef]
- Saidi, O.; Rochette, E.; Dambel, L.; St-Onge, M.P.; Duché, P. Chrono-nutrition and sleep: lessons from the temporal feature of eating patterns in human studies - A systematic scoping review. Sleep Med Rev 2024, 76, 101953. [Google Scholar] [CrossRef]
- Chen, H.J.; Tsai, Y.C.; Hsu, Y.T.; Chu, J. Effect of recommendations of breakfast and late-evening snack habits on body composition and blood pressure: A pilot randomized trial. Chronobiol Int 2024, 41, 1021–1033. [Google Scholar] [CrossRef]
- Almoosawi, S.; Vingeliene, S.; Karagounis, L.G.; Pot, G.K. Chrono-nutrition: a review of current evidence from observational studies on global trends in time-of-day of energy intake and its association with obesity. Proc Nutr Soc 2016, 75, 487–500. [Google Scholar] [CrossRef] [PubMed]
- Johnston, J.D.; Ordovás, J.M.; Scheer, F.A.; Turek, F.W. Circadian Rhythms, Metabolism, and Chrononutrition in Rodents and Humans. Adv Nutr 2016, 7, 399–406. [Google Scholar] [CrossRef] [PubMed]
- Potter, G.D.; Cade, J.E.; Grant, P.J.; Hardie, L.J. Nutrition and the circadian system. Br J Nutr 2016, 116, 434–442. [Google Scholar] [CrossRef]
- Seike, K.; Oshita, K.; Ishihara, Y.; Myotsuzono, R.; Nagamine, K. Relationship Between Breakfast Skipping and Body Composition, Nutritional Status or Chronotype in Female University Students With Normal Body Weight. Physiol Res 2025, 74, 989–998. [Google Scholar] [CrossRef]
- Westerterp, K.R. Physical activity as determinant of daily energy expenditure. Physiol Behav 2008, 93, 1039–1043. [Google Scholar] [CrossRef]
- Challet, E. The circadian regulation of food intake. Nat Rev Endocrinol 2019, 15, 393–405. [Google Scholar] [CrossRef]
- Theodorakis, N.; Nikolaou, M. The Human Energy Balance: Uncovering the Hidden Variables of Obesity. Diseases 2025, 13. [Google Scholar] [CrossRef]
- Nishimura, K.; Tamari, Y.; Nose, Y.; Yamaguchi, H.; Onodera, S.; Nagasaki, K. Effects of Irregular Mealtimes on Social and Eating Jet Lags among Japanese College Students. Nutrients 2023, 15. [Google Scholar] [CrossRef]
- Gong, Y.; Zhang, J.X.; Li, S.N.; Li, L.L.; Dong, X.J.; Liu, L.J.; Fan, Z.H.; Li, Y.; Yang, Y.D. The relationship between chrononutrition profile, social jet lag and obesity: A cross-sectional study of Chinese college students. Chronobiol Int 2025, 42, 328–339. [Google Scholar] [CrossRef] [PubMed]
- Gong, Y.; Chen, M.X.; Fan, Z.H.; Huang, Z.H.; Xiao, T.L.; Fan, X.L.; Zheng, C.J.; Yang, Y.D. Reliability and validity of the Chinese version of the Chrononutrition Profile Questionnaire. Modern Preventive Medicine 2024, 51, 2182–2187. [Google Scholar] [CrossRef]
- Jigeer, G.; Huang, Z.; Wang, P.; Chen, S.; Sun, L.; Li, Y.; Wu, S.; Gao, X. Longitudinal associations of skipping breakfast and night eating with 4-year changes in weight and waist circumference among Chinese adults. Am J Clin Nutr 2024, 120, 442–448. [Google Scholar] [CrossRef]
- Ekiz Erim, S.; Sert, H. The relationship between chronotype and obesity: A systematic review. Chronobiol Int 2023, 40, 529–541. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.; Nie, Q.; Wang, Y.; Liu, Y.; Liu, W.; Wang, T.; Zhang, Y.; Cao, S.; Li, Z.; Zheng, J.; et al. Associations between temporal eating patterns and body composition in young adults: a cross-sectional study. Eur J Nutr 2024, 63, 2071–2080. [Google Scholar] [CrossRef] [PubMed]
- Mao, Z.; Cawthon, P.M.; Kritchevsky, S.B.; Toledo, F.G.S.; Esser, K.A.; Erickson, M.L.; Newman, A.B.; Farsijani, S. The association between chrononutrition behaviors and muscle health among older adults: The study of muscle, mobility and aging. Aging Cell 2023, e14059. [Google Scholar] [CrossRef] [PubMed]
- He, M.; Li, B.; Li, M.; Gao, S. Does early time-restricted eating reduce body weight and preserve fat-free mass in adults? A systematic review and meta-analysis of randomized controlled trials. Diabetes Metab Syndr 2024, 18, 102952. [Google Scholar] [CrossRef]
| Variables | Total (n=174) Mean ± SD/Median (IQR) | Male (n=64) Mean ± SD | Female (n=110) Mean ± SD | Sports-majoring (n=131) Mean ± SD | Non-sports-majoring (n=43) Mean ± SD | P-value (sex) | P-value (major) |
| Age (years) | 20.5 ± 1.8 | 20.7 ± 1.7 | 20.3 ± 1.9 | 20.6 ± 1.7 | 20.4 ± 1.9 | 0.210 | 0.374 |
| BMI (kg/m²) | 23.3 ± 4.5 | 24.8 ± 4.2 | 22.4 ± 4.4 | 23.5 ± 4.4 | 22.8 ± 4.6 | <0.001 | 0.450 |
| Physical exercise frequency (times/week) | 5.2 ± 2.1 | 5.8 ± 2.0 | 4.8 ± 2.0 | 5.6 ± 1.9 | 3.2 ± 1.5 | <0.001 | <0.001 |
| Sleep duration (h/day) | 9.0 (7.2, 11.5) |
8.8 (7.0, 11.2) |
9.1 (7.3, 11.8) |
8.9 (7.1, 11.3) |
9.2 (7.5, 12.0) |
0.286 | 0.312 |
| Discrepancy Indicator | Sample Size (n) | Mean ± SD (hours) | Interpretation |
| Sleep duration discrepancy | 142 | -0.5 ± 5.5 | Actual sleep duration was slightly shorter than ideal |
| Sleep midpoint discrepancy | 142 | 0.3 ± 3.2 | Small difference between ideal and actual sleep midpoint |
| Eating midpoint discrepancy | 142 | 0.7 ± 3.4 | Small difference between ideal and actual eating midpoint |
| Weekday eating window discrepancy | 142 | 1.6 ± 5.8 | Actual weekday eating window was longer than ideal |
| Chrononutrition Indicator | Male (n=64) Mean ± SD | Female (n=110) Mean ± SD | P-value |
| Average breakfast time | 7:58 ± 0:42 | 7:46 ± 0:46 | <0.05* |
| Average dinner time | 18:55 ± 0:50 | 18:41 ± 0:53 | <0.05* |
| Weekday eating window (hours) | 11.5 ± 1.7 | 10.9 ± 1.8 | <0.05* |
| Regular meal days per week (days) | 3.9 ± 1.6 | 4.5 ± 1.4 | <0.05* |
| Breakfast energy proportion (%) | 17.8 ± 5.5 | 19.4 ± 5.0 | <0.05* |
| Dinner energy proportion (%) | 37.9 ± 6.9 | 33.2 ± 6.8 | <0.05* |
| Variables | Total (n=133) | Male (n=50) | Female (n=83) | P-value (Sex) | Sports (n=93) | Non-sports (n=40) | P-value (Major) |
| Muscle mass percentage (%) | 64.6 ± 12.7 | 73.1 ± 9.4 | 59.5 ± 11.8 | <0.001* | 66.8 ± 11.9 | 58.2 ± 12.5 | <0.001 |
| Fat mass percentage (%) | 23.6 ± 9.3 | 17.2 ± 6.9 | 27.6 ± 8.3 | <0.001* | 21.5 ± 8.9 | 28.7 ± 8.5 | <0.001 |
| Limb muscle mass (kg) | 26.8 ± 11.5 | 36.5 ± 8.2 | 20.7 ± 6.3 | <0.001* | 28.9 ± 10.8 | 20.5 ± 7.1 | <0.001 |
| Visceral fat area (cm²) | 85.2 ± 41.3 | 112.5 ± 38.6 | 68.3 ± 32.5 | <0.001* | 76.5 ± 35.2 | 102.8 ± 42.6 | <0.001 |
| Other components percentage (%) | 11.8 ± 7.8 | 9.7 ± 4.3 | 13.0 ± 9.1 | *<0.05 | 11.7 ± 7.5 | 12.1 ± 8.2 | 0.422 |
| RMR (kcal/d) | 1982.0 ± 593.4 | 2522.3 ± 440.4 | 1646.4 ± 401.3 | <0.001* | 2085.6 ± 568.2 | 1652.3 ± 489.5 | <0.001 |
| Standardized RMR (kcal·kg⁻¹·d⁻¹) | 29.9 ± 7.1 | 32.7 ± 6.5 | 28.2 ± 6.9 | <0.01* | 31.2 ± 6.8 | 27.5 ± 6.9 | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




