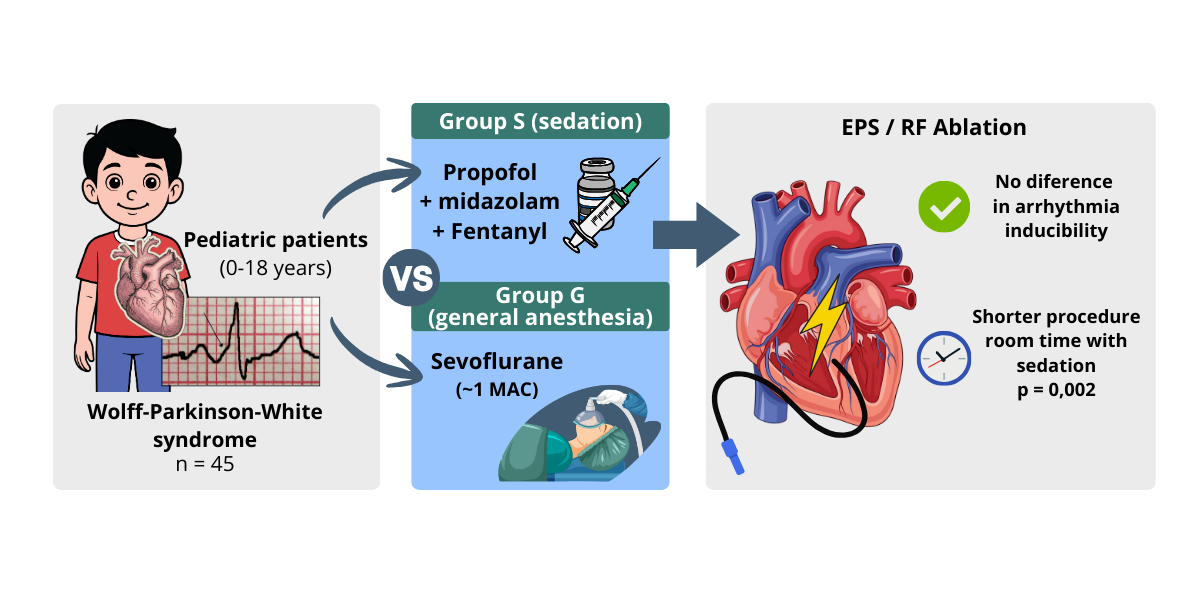
Introduction: Propofol is one of the most commonly used intravenous anesthetics worldwide and is considered safe for all age groups. However, there have been reports that propofol can induce severe atrioventricular block in humans, and several studies have shown that propofol hinders or prevents the inducibility of arrhythmias during electrophysiological studies (EPS) and radiofrequency (RF) ablation. Objectives: Verify whether propofol prevents or hinders the inducibility of arrhythmias during EPS and RF ablation procedures in children with Wolff-Parkinson-White Syndrome. Methods:We conducted a retrospective observational cohort study including 45 pediatric patients aged 0–18 years. Patients were identified through a review and analysis of a database of individuals with Wolff–Parkinson–White syndrome who were referred for electrophysiological study and/or radiofrequency ablation at the Electrophysiology Laboratory of the Institute of Cardiology (IC/FUC) in Porto Alegre over the past five years (2019-2024). Patients with prior ablation, structural heart disease, or ongoing antiarrhythmic therapy were excluded. The patients were divided into two groups and designated as group S (who received sedation) or group G (who received general anesthesia). Sedation (group S) was performed with midazolam (0.08–0.2 mg/kg), fentanyl (0.1–0.2 μcg/kg), and propofol 50–60 µg/kg/min in continuous infusion. General anesthesia (group G), in turn, was performed with sevoflurane at an average dose of 2% (1 MAC according to age). Results: From 4,874 invasive electrophysiology procedures performed during the study period, 45 involved pediatric patients with WPW. The sedation group (n=29) had significantly older patients (14.6±2.5 vs 10.3±2.8 years, p<0.001) with higher weight (65.9±16.3 vs 41.2±7.8 kg, p<0.001) compared to the general anesthesia group (n=16). Arrhythmia was successfully induced in 15/29 (51.7%) patients in the sedation group compared to 13/16 (81.2%) in the general anesthesia group (p=0.062, Fisher's exact test). Although this difference did not reach statistical significance, it represents a clinically relevant 29.5% lower induction rate in the sedation group. Post-hoc power analysis revealed the study was underpowered (49.8%), suggesting a possible Type II error. Analysis of the "procedure room time" revealed a longer duration in the general anesthesia group (97.8±36.7 vs 67.8±24.4 minutes), and this difference was statistically significant (p = 0.002). Conclusions: This study compared propofol-based sedation with sevoflurane-based general anesthesia in pediatric WPW patients. While sedation with propofol did not show a statistically significant reduction in arrhythmia inducibility, there was a concerning trend toward lower induction rates (29.5% difference) that may be clinically relevant. The study's limited statistical power (49.8%) suggests these findings should be interpreted cautiously, and larger prospective studies are needed to definitively establish whether propofol affects arrhythmia inducibility in this population. Propofol remains a viable option for these procedures, but clinicians should be aware of the potential for reduced inducibility, particularly in cases where arrhythmia induction is critical for diagnosis and treatment.