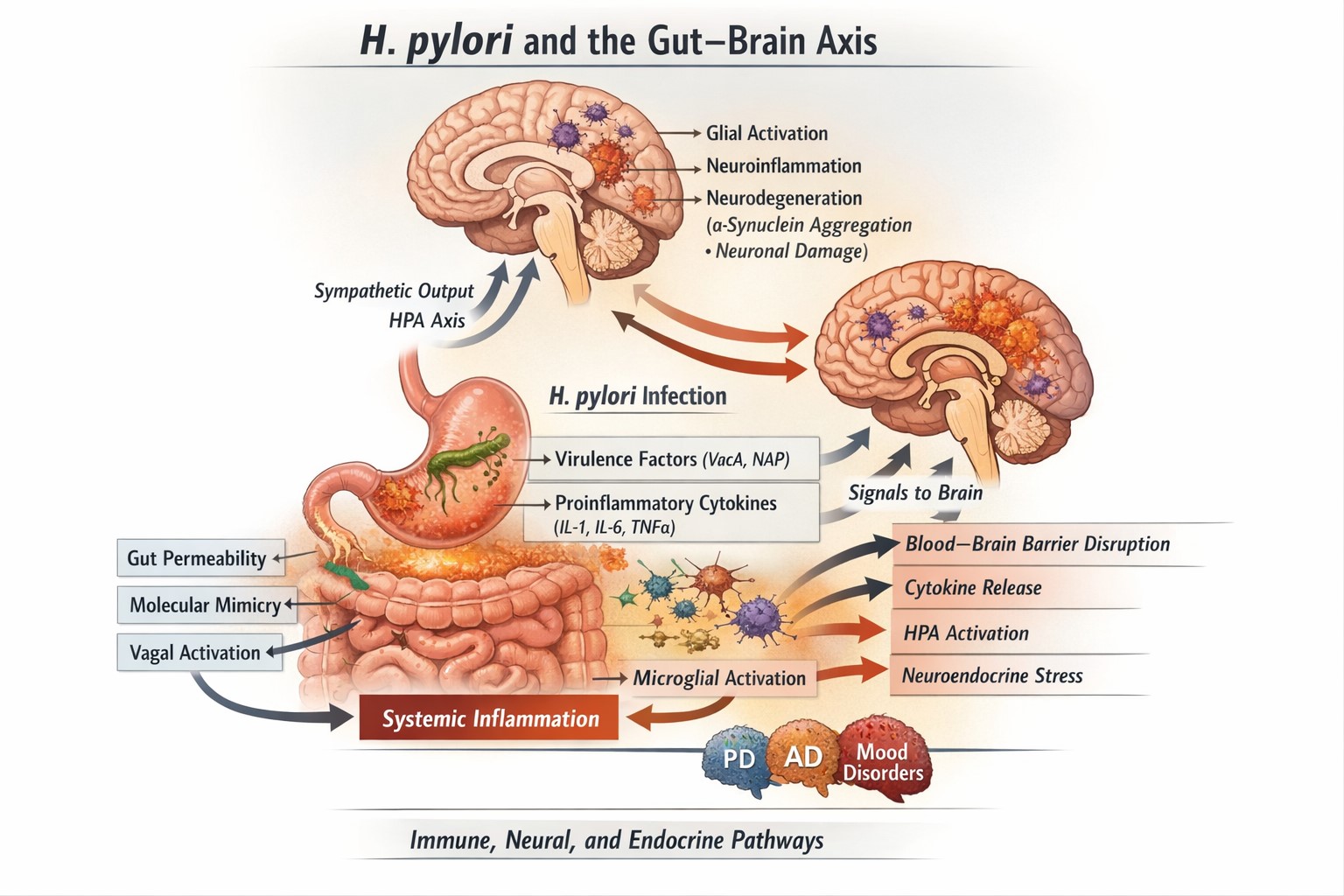
Objective: Helicobacter pylori infects nearly half of the global population and has traditionally been viewed as a pathogen restricted to the gastric mucosa. Growing evidence, however, suggests that chronic infection may exert systemic effects extending to the central nervous system. This review critically examines the potential neurological implications of H. pylori infection within the emerging framework of the gut–brain axis. Methods: We performed a narrative, hypothesis-generating review of human observational and interventional studies complemented by mechanistic experimental research. The literature was evaluated with particular attention to study design, heterogeneity, and potential confounding in reported associations between H. pylori infection and neurological disorders. Results: Across multiple studies, H. pylori infection has been linked to a modestly increased prevalence of Parkinson’s disease and dementia, although findings remain heterogeneous. In Parkinson’s disease, infection may exacerbate motor fluctuations and reduce levodopa bioavailability, with partial clinical improvement reported following eradication in selected patients. Experimental studies further demonstrate that bacterial outer membrane vesicles can access the brain and promote neuroinflammatory and amyloidogenic processes, supporting biological plausibility. By contrast, several epidemiological studies report an inverse association with multiple sclerosis, suggesting potential immunomodulatory effects. Evidence relating H. pylori to migraine and mood disorders remains inconsistent. Conclusions: Current data do not support H. pylori as a primary cause of neurological disease. Instead, the infection may act as a context-dependent modifier within the complex inflammatory and immunometabolic networks of the gut–brain axis. Clarifying this relationship will require prospective studies integrating microbial strain profiling, biomarker-defined neurological phenotypes, and adequately powered interventional trials.