Submitted:
11 March 2026
Posted:
12 March 2026
You are already at the latest version
Abstract
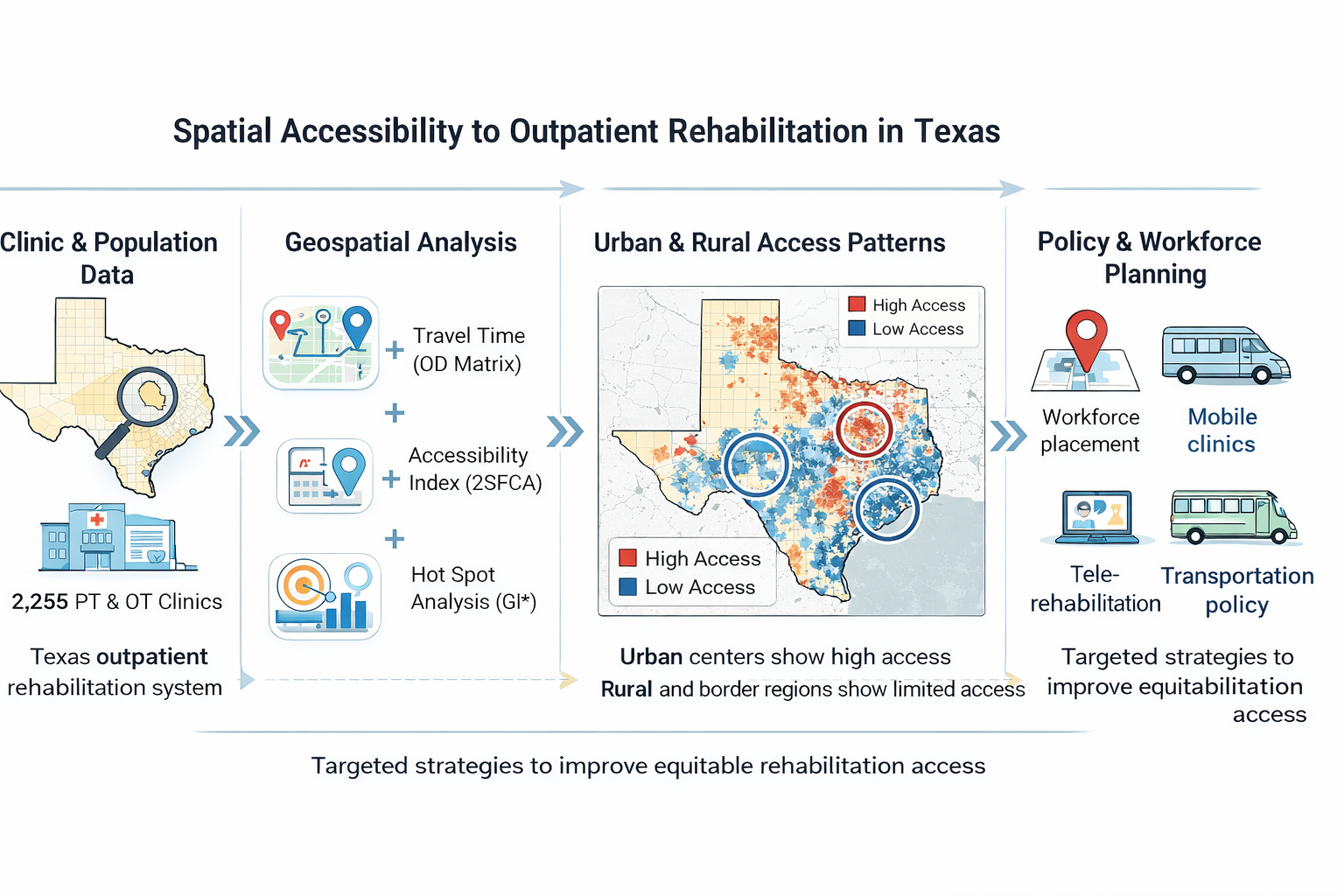
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Data Sources and Study Population
2.3. Data Preparation
2.4. Geospatial Analysis
2.4.1. Origin-Destination Cost Matrix:
2.4.2. Accessibility Index Calculation Using a Two-Step Floating Catchment Area (2SFCA):
2.4.3. Hot Spot Analysis
2.5. Statistical Analysis
3. Results
3.1. Geospatial Results
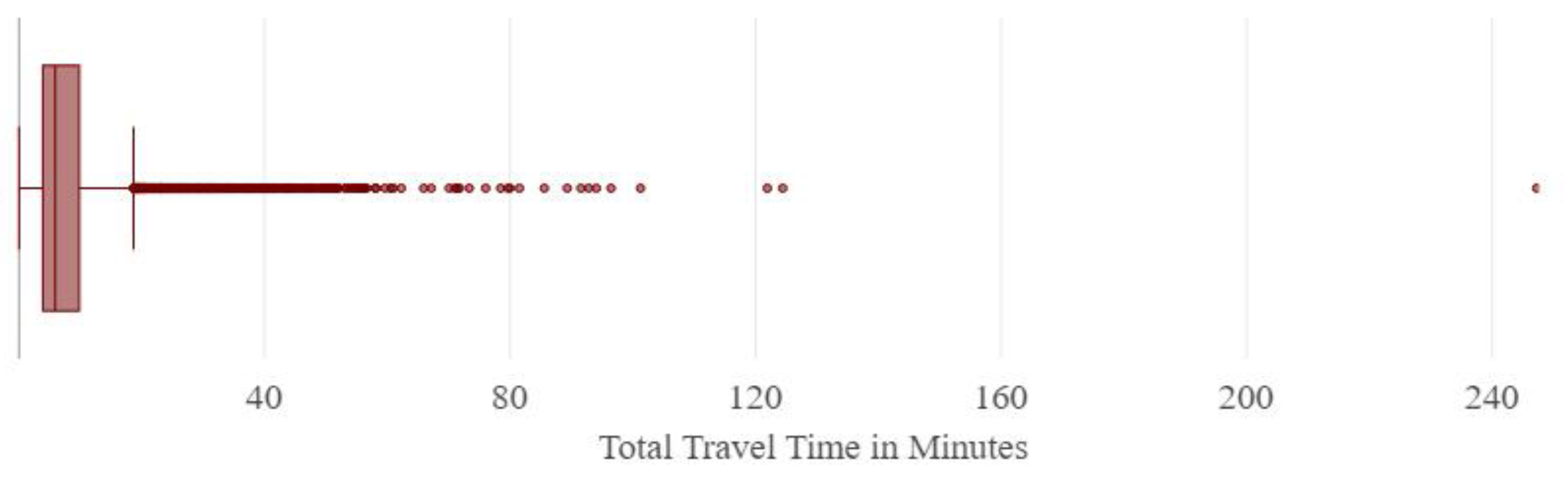
3.1.1. Origin Destination Cost Matrix Results
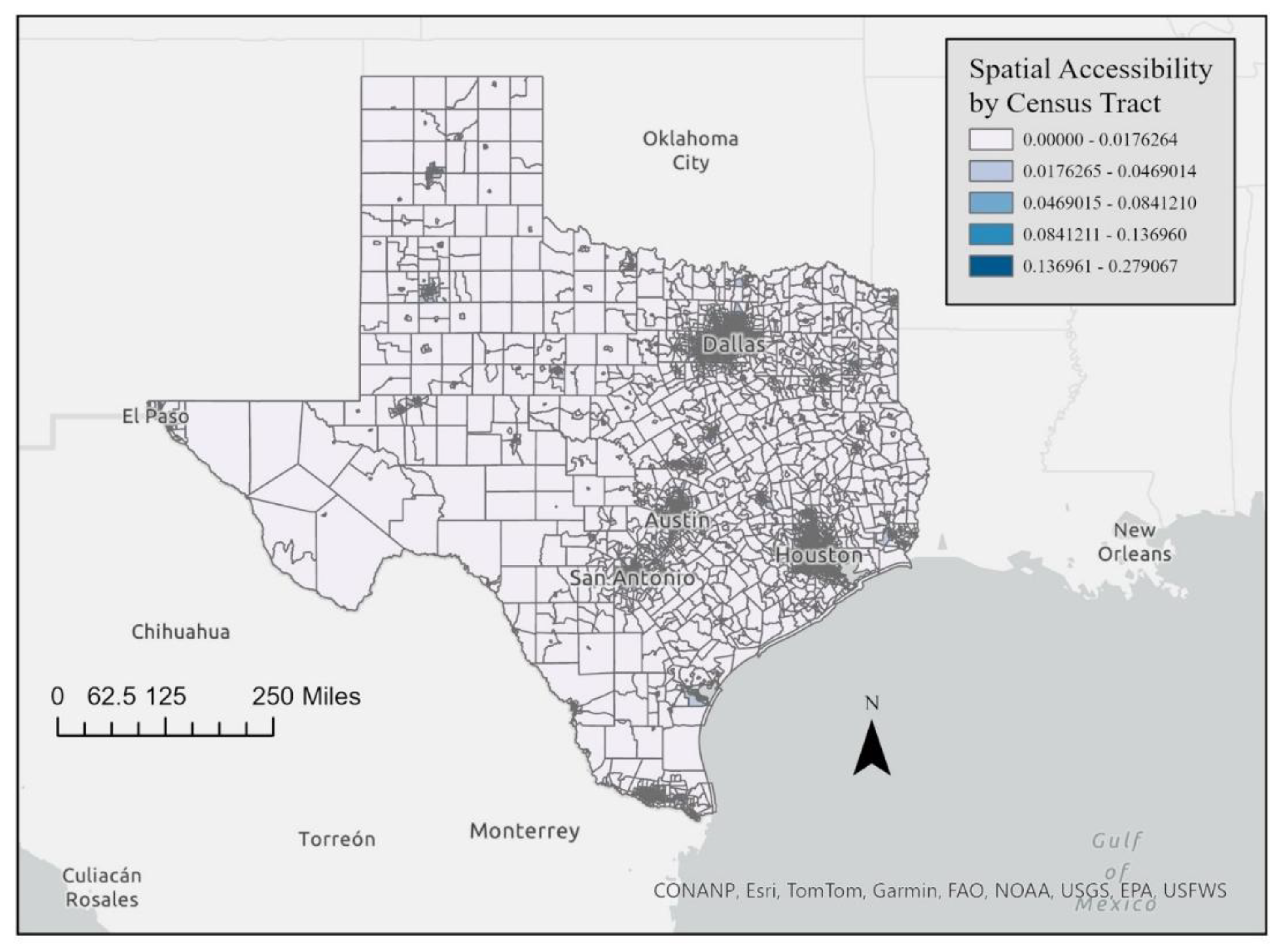
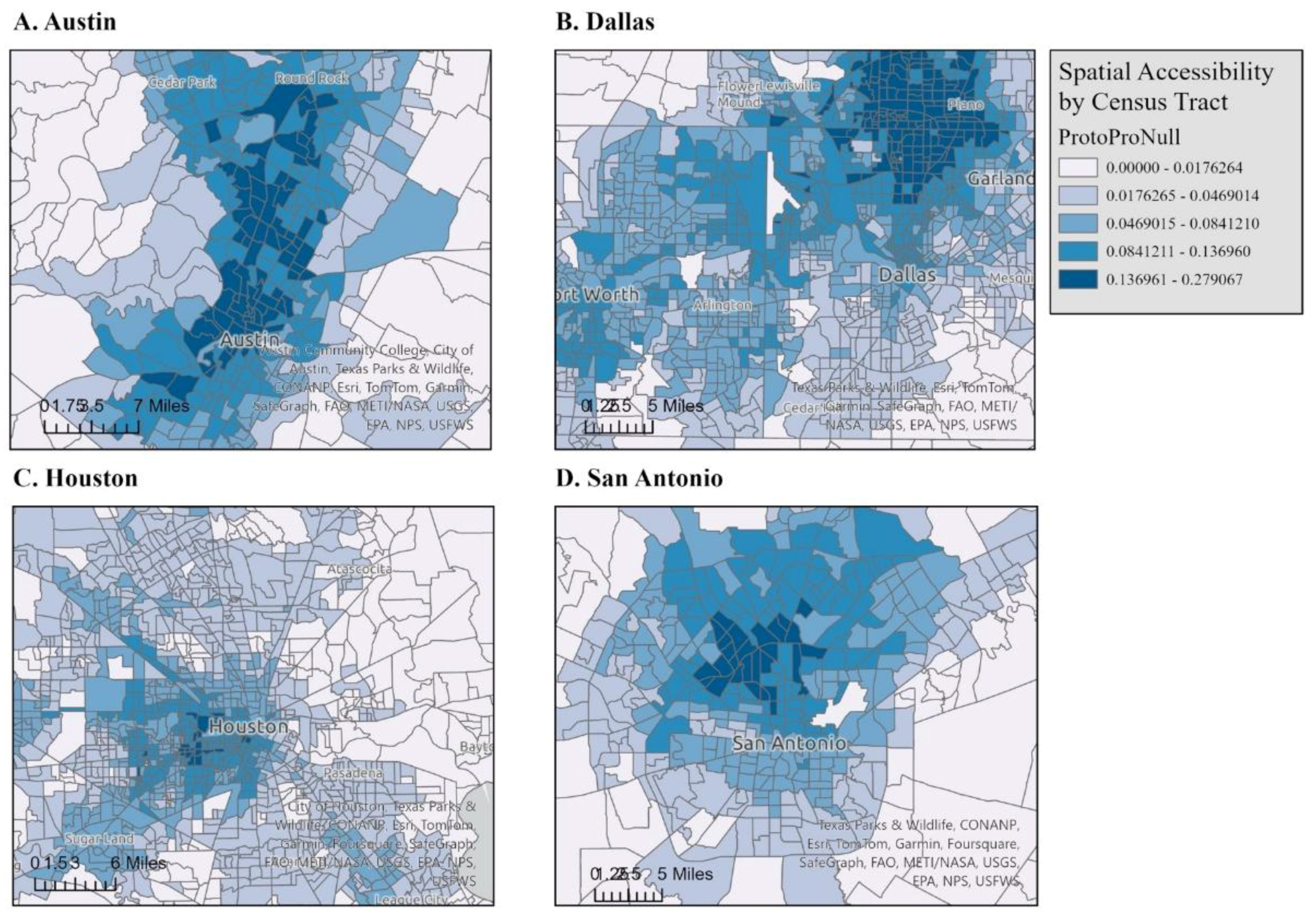
3.1.2. Accessibility Index Results
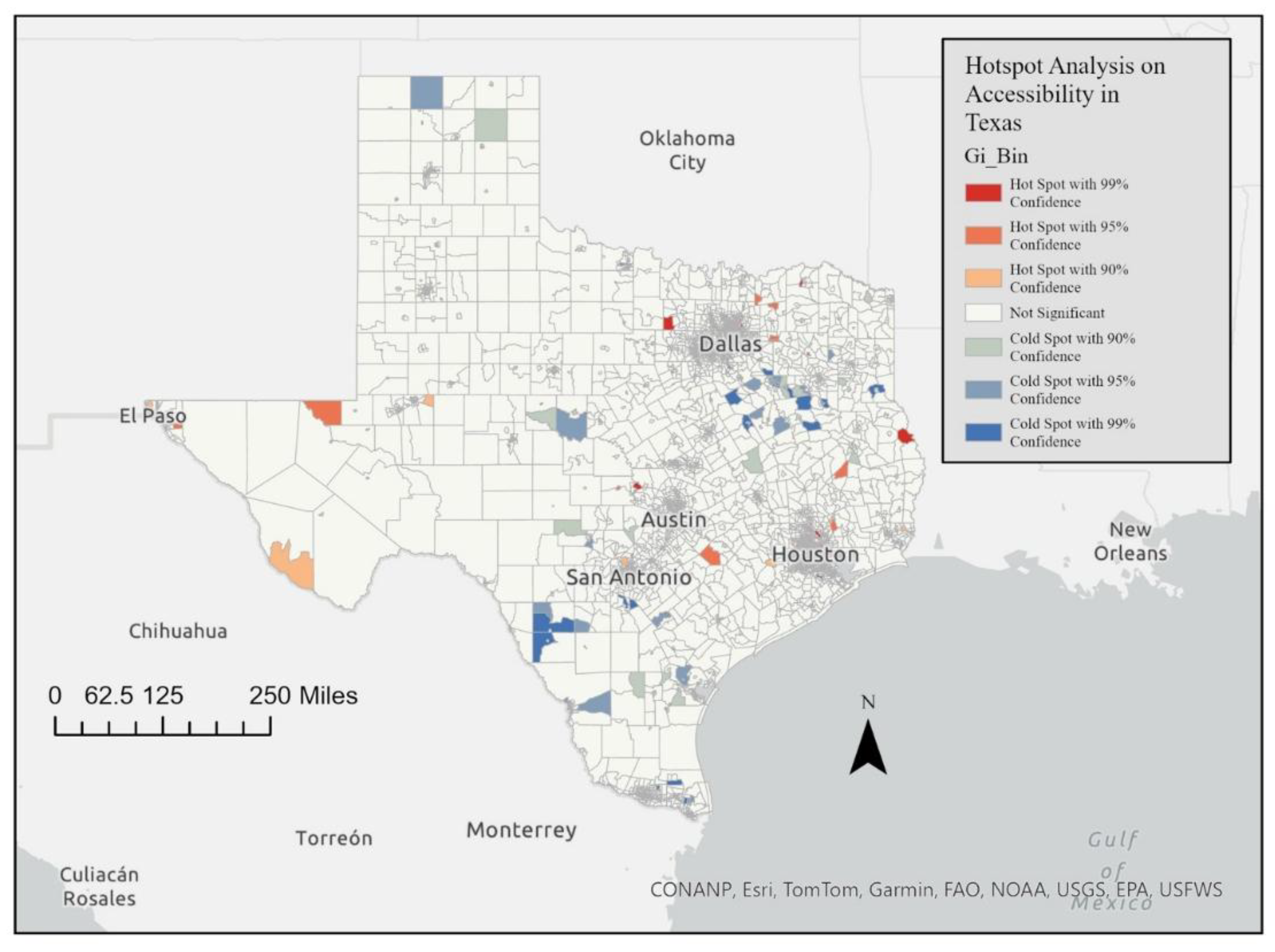
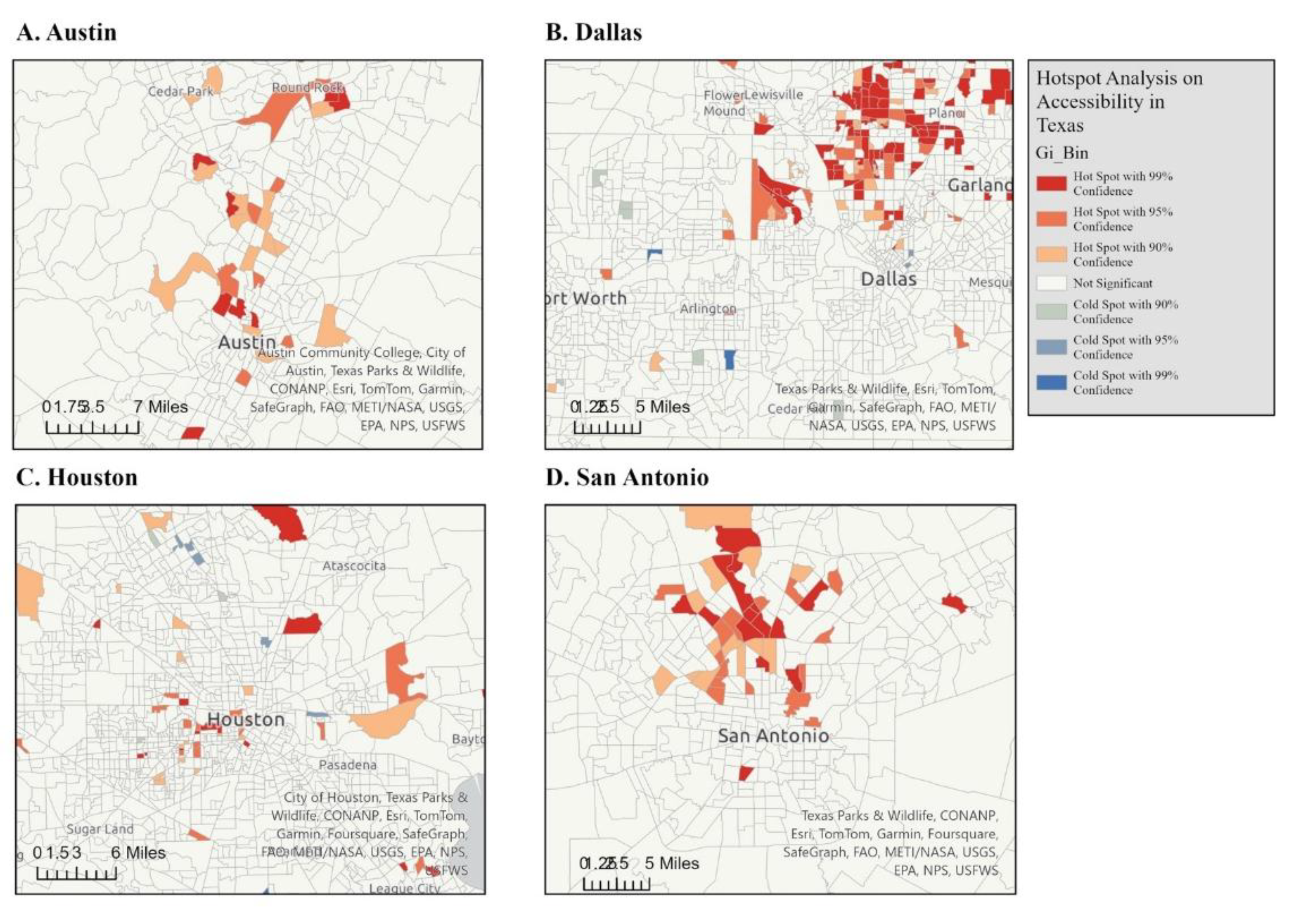
3.1.3. Getis-Ord Gi* Results
3.1.3. Statistical Results
| Variable | Unstandardized β | SE | z value | P Value | Odds Ratio | CI (lower) | CI (upper) |
| Intercept | -9.34 | 3.98 | -2.35 | 0.019 | 8.79×10−5 | 2.59x10-8 | 0.193 |
| Hispanic | 0.136 | 0.041 | 3.29 | <0.001 | 1.146 | 1.058 | 1.246 |
| White | 0.107 | 0.041 | 2.62 | 0.009 | 1.113 | 1.029 | 1.211 |
| Black | 0.099 | 0.041 | 2.43 | 0.015 | 1.104 | 1.020 | 1.200 |
| American Indian | 0.371 | 0.257 | 1.44 | 0.149 | 1.449 | 0.901 | 2.483 |
| Asian | 0.111 | 0.042 | 2.65 | 0.008 | 1.117 | 1.030 | 1.216 |
| No Vehicle Households | -0.075 | 0.026 | -2.88 | 0.004 | 0.928 | 0.880 | 0.975 |
| Households No Partner Present | -0.045 | 0.011 | -4.12 | <0.001 | 0.956 | 0.934 | 0.975 |
| Households Single Parent | 0.124 | 0.027 | 4.5 | <0.001 | 1.132 | 1.07 | 1.196 |
| No Internet Households | 0.037 | 0.019 | 1.94 | 0.052 | 1.038 | 1.001 | 1.078 |
| With Disability | 0.17 | 0.031 | 5.51 | <0.001 | 1.185 | 1.118 | 1.262 |
| No HS Diploma | -0.073 | 0.019 | -3.75 | <0.001 | 0.930 | 0.894 | 0.964 |
|
1Abbreviations: SE, standard error; β, log-odds unstandardized coefficient. 2All predictors refer to the percentage of the population in the census tract. |
|||||||
4. Discussion
4.1. The Origin-Destination Cost matrix
4.2. Accessibility Index
4.3. Implications for Access Interventions
4.4. Transportation Networks and Access
4.5. Getis-Ord Gi* Statistic
4.6. Population Characteristics
4.7. Strengths
4.8. Limitations
4.9. Future Directions
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| 2SFCA | Two-step floating catchment area |
| AI | Accessibility Index |
| ACS | American Community Survey |
| OD | Origin-destination |
| Gi* | Getis-Ord statistic |
| PT | Physical therapy |
| OT | Occupational therapy |
| FDR | False discovery rate |
References
- County Health Rankings & Roadmaps. Access to Care. Available online: https://www.countyhealthrankings.org/explore-health-rankings/measures-data-sources/county-health-rankings-model/health-factors/clinical-care/access-to-care (accessed on 17 October 2022).
- Center, Graham. Access Denied. Available online: https://www.graham-center.org/content/dam/rgc/documents/publications-reports/monographs-books/Access%20Denied.pdf.
- Kaiser Family Foundation. The Uninsured: A Primer. Available online: https://files.kff.org/attachment/primer-the-uninsured-a-primer-key-facts-about-health-insurance-and-the-uninsured-in-the-era-of-health-reform.
- Penchansky, R.; Thomas, J.W. The concept of access: Definition and relationship to consumer satisfaction. Med. Care 1981, 19, 127–140. [Google Scholar] [CrossRef] [PubMed]
- Saurman, E. Improving access: Modifying Penchansky and Thomas’s theory of access. J. Health Serv. Res. Policy 2016, 21, 36–39. [Google Scholar] [CrossRef] [PubMed]
- American Physical Therapy Association. Direct Access Advocacy. Available online: https://www.apta.org/advocacy/issues/direct-access-advocacy (accessed on 30 August 2024).
- Clark, B.; Clark, L.; Showalter, C.; Stoner, T. A call to action: Direct access to physical therapy is highly successful in the US military. When will professional bodies, legislatures, and payors provide the same advantages to all US civilian physical therapists? J. Man. Manip. Ther. 2022, 30, 199–206. [Google Scholar] [CrossRef] [PubMed]
- Zahnd, W.E.; Del Vecchio, N.; Askelson, N.; et al. Definition and categorization of rural and assessment of realized access to care. Health Serv. Res. 2022, 57, 693–702. [Google Scholar] [CrossRef]
- Khan, A.A.; Bhardwaj, S.M. Access to health care: A conceptual framework and its relevance to health care planning. Eval. Health Prof. 1994, 17, 60–76. [Google Scholar] [CrossRef]
- Sullivan, J.; Orris, A.; Lukens, G. Entering Their Second Decade, Affordable Care Act Coverage Expansions Have Helped Millions, Provide the Basis for Further Progress. Available online: https://www.cbpp.org/research/health/entering-their-second-decade-affordable-care-act-coverage-expansions-have-helped (accessed on 30 August 2024).
- U.S. Government Accountability Office. Why Health Care Is Harder to Access in Rural America. Available online: https://www.gao.gov/blog/why-health-care-harder-access-rural-america (accessed on 30 August 2024).
- Bodenheimer, T.; Grumbach, K. Understanding Health Policy: A Clinical Approach, 8th ed.; McGraw Hill Medical: New York, NY, USA, 2020. [Google Scholar]
- Wong, A.; Hoang, T.M.H.; Ferrara, V.; Nguyen, T.H. How systemic barriers can impact health inequities when facing climate change stressors: A scoping review of global differences. GeoHealth 2025, 9, e2024GH001272. [Google Scholar] [CrossRef]
- Arrington, J.C. One Big Beautiful Bill Act. Available online: https://www.congress.gov/bill/119th-congress/house-bill/1 (accessed on 25 September 2025).
- Johns Hopkins Bloomberg School of Public Health. The Changes Coming to the ACA, Medicaid, and Medicare. Available online: https://publichealth.jhu.edu/2025/the-changes-coming-to-the-aca-medicaid-and-medicare (accessed on 25 September 2025).
- American Physical Therapy Association Health Policy; Administration. PTJ-PAL. No. 3. Vol. 19. Available online: https://cdn.ymaws.com/www.aptahpa.org/resource/resmgr/ptj-pal/ptj-palvol19no3.pdf.
- Gao, F.; Foster, M.; Liu, Y. Disability concentration and access to rehabilitation services: A pilot spatial assessment applying geographic information system analysis. Disabil. Rehabil. 2019, 41, 2468–2476. [Google Scholar] [CrossRef]
- Lakhani, A.; Parekh, S.; Gudes, O.; et al. Disability support services in Queensland, Australia: Identifying service gaps through spatial analysis. Appl. Geogr. 2019, 110, 102045. [Google Scholar] [CrossRef]
- Kinder Institute for Urban Research. After Census redefines urban and rural, Texas remains steadfastly both. Available online: https://kinder.rice.edu/urbanedge/census-redefines-urban-rural (accessed on 3 November 2023).
- Mora, D.S.; Noble, G.; Alamos, C.L.; McKinley Sandoval Harding, B.M.; Moore, T.P.H. Three rural definitions. Available online: https://www.ers.usda.gov/webdocs/DataFiles/53180/25598_TX.pdf (accessed on 13 February 2023).
- Rural Health Information Hub. Transportation to Support Rural Healthcare. Available online: https://www.ruralhealthinfo.org/topics/transportation (accessed on 10 March 2026).
- Wolfe, M.K.; McDonald, N.C.; Holmes, G.M. Transportation barriers to health care in the United States: Findings from the National Health Interview Survey, 1997–2017. Am. J. Public Health 2020, 110, 815–822. [Google Scholar] [CrossRef]
- Jiao, J. Identifying transit deserts in major Texas cities where the supplies missed the demands. J. Transp. Land Use 2017, 10, 529–540. [Google Scholar] [CrossRef]
- Texas Department of Transportation. 2023 Texas Transit Statistics. Available online: https://www.txdot.gov/content/dam/docs/government/texas-transit-statistics-report-2023..pdf (accessed on 2024).
- Autoinsurance.com. Commuting in the U.S. Facts and Statistics. Available online: https://www.autoinsurance.com/research/us-commuting-statistics/ (accessed on 30 August 2024).
- Centers for Disease Control and Prevention. Disability & Health U.S. State Profile Data: Texas. Available online: https://www.cdc.gov/ncbddd/disabilityandhealth/impacts/texas.html (accessed on 30 August 2024).
- Ratoza, M.R.; Patel, R.M.; Brewer, W.; Mitchell, K.; Chevan, J. Geographic disparities in rehabilitation provider availability and community demographics in Texas: A cross-sectional geographic information systems study accepted. Phys. Ther. 2025. [Google Scholar] [CrossRef]
- Texas Department of State Health Services. Available online: https://www.dshs.texas.gov/ (accessed on 28 August 2025).
- U.S. Census Bureau. American Community Survey (ACS). Available online: https://www.census.gov/programs-surveys/acs (accessed on 24 November 2024).
- Texas Executive Council of Physical Therapy and Occupational Therapy Examiners. Open Records Request. Available online: https://ptot.texas.gov/open-records-request/ (accessed on 23 January 2023).
- U.S. Census Bureau. Census.gov. Available online: https://www.census.gov/ (accessed on 23 January 2023).
- Ratoza, M.; Patel, R.M.; Chevan, J.; Brewer, W.; Mitchell, K. Mapping the availability of rehabilitation providers using public licensure and population data for a geographic information system-based approach to workforce planning: Cross-sectional feasibility study. JMIR Form. Res. 2025, 9, e85025. [Google Scholar] [CrossRef]
- Esri. ArcGIS. Available online: https://www.esri.com/en-us/arcgis/geospatial-platform/overview (accessed on 12 September 2024).
- Esri. ArcGIS World Geocoding. Available online: https://www.arcgis.com/sharing/rest/content/items/305f2e55e67f4389bef269669fc2e284 (accessed on 25 September 2025).
- Esri. On-Premises and Offline Routing, Geocoding & Mapping. Available online: https://www.esri.com/en-us/arcgis/products/arcgis-streetmap-premium/overview (accessed on 25 September 2025).
- Radke, J.; Mu, L. Spatial decompositions, modeling and mapping service regions to predict access to social programs. Ann. GIS 2000, 6, 105–112. [Google Scholar] [CrossRef]
- Dong, Y.; Fu, L.; Tan, R.; Ding, L. The dilemma of medical reimbursement policy in rural China: Spatial variability between reimbursement region and medical catchment area. Int. J. Environ. Res. Public Health 2019, 16, 2867. [Google Scholar] [CrossRef] [PubMed]
- Naylor, K.B.; Tootoo, J.; Yakusheva, O.; Shipman, S.A.; Bynum, J.P.W.; Davis, M.A. Geographic variation in spatial accessibility of U.S. healthcare providers. PLoS ONE 2019, 14, e0215016. [Google Scholar] [CrossRef] [PubMed]
- Pervorse, A. Spatial Accessibility in Health Care. Available online: https://storymaps.arcgis.com/stories/afec06281a264b3e9bdcb02b1ece8778 (accessed on 11 November 2024).
- Gautam, S.; Li, Y.; Johnson, T.G. Do alternative spatial healthcare access measures tell the same story? GeoJournal 2014, 79, 223–235. [Google Scholar] [CrossRef]
- Kanuganti, S.; Sarkar, A.K.; Singh, A.P. Quantifying accessibility to health care using two-step floating catchment area method (2SFCA): A case study in Rajasthan. Transp. Res. Procedia 2016, 17, 391–399. [Google Scholar] [CrossRef]
- Cypress Health Partners. Why Distance Is So Important for Patient Access, and What We’re Doing About It. Available online: https://cypresshealthpartners.com/why-distance-is-so-important-for-patient-access-and-what-were-doing-about-it/ (accessed on 12 December 2024).
- Esri. How Hot Spot Analysis (Getis-Ord Gi*) Works. Available online: https://pro.arcgis.com/en/pro-app/latest/tool-reference/spatial-statistics/h-how-hot-spot-analysis-getis-ord-gi-spatial-stati.htm (accessed on 21 July 2024).
- Grekousis, G. Spatial Analysis Methods and Practice: Describe – Explore – Explain through GIS; Cambridge University Press: Cambridge, UK, 2020. [Google Scholar]
- Chen, X.; Orom, H.; Hay, J.L.; et al. Differences in rural and urban health information access and use. J. Rural Health 2019, 35, 405–417. [Google Scholar] [CrossRef]
- McManus, B.M.; Lindrooth, R.; Richardson, Z.; Rapport, M.J. Urban/rural differences in therapy service use among Medicaid children aged 0–3 with developmental conditions in Colorado. Acad. Pediatr. 2016, 16, 358–365. [Google Scholar] [CrossRef]
- Quigley, D.D.; Chastain, A.M.; Kang, J.A.; et al. Systematic review of rural and urban differences in care provided by home health agencies in the United States. J. Am. Med. Dir. Assoc. 2022, 23, 1653.e1–1653.e13. [Google Scholar] [CrossRef]
- Young, S. Dallas County Remains Segregated by Race, Income and Education Level, New Study Says. Available online: https://www.dallasobserver.com/news/dallas-county-has-widespread-ethnic-disparities-according-to-new-study-10566546 (accessed on 15 December 2024).
- University of Richmond. Mapping Inequality. Available online: https://dsl.richmond.edu/panorama/redlining/ (accessed on 15 December 2024).
- Munson, L. What Is Economic Segregation, and Why Does It Matter? Available online: https://hebfdn.org/echoes/economic-segregation-matter/ (accessed on 15 December 2024).
- Florida, R.; Mellander, C. Segregated City: The Geography of Economic Segregation in America’s Metros. Available online: https://hj.diva-portal.org/smash/get/diva2:868382/FULLTEXT01 (accessed on 15 December 2024).
- Yu, S.W.Y.; Hill, C.; Ricks, M.L.; Bennet, J.; Oriol, N.E. The scope and impact of mobile health clinics in the United States: A literature review. Int. J. Equity Health 2017, 16, 178. [Google Scholar] [CrossRef]
- Malone, N.C.; Williams, M.M.; Smith Fawzi, M.C.; et al. Mobile health clinics in the United States. Int. J. Equity Health 2020, 19, 40. [Google Scholar] [CrossRef]
- Tulane University School of Public Health. How Do Mobile Health Clinics Improve Access to Health Care? Available online: https://publichealth.tulane.edu/blog/mobile-health-clinics/ (accessed on 16 December 2024).
- Bärnighausen, T.; Bloom, D.E. Financial incentives for return of service in underserved areas: A systematic review. BMC Health Serv. Res. 2009, 9, 86. [Google Scholar] [CrossRef]
- University of Washington Center for Health Workforce Studies. State Incentive Programs that Encourage Allied Health Professionals to Provide Care for Underserved Populations. Available online: https://familymedicine.uw.edu/chws/studies/state-incentive-programs-that-encourage-allied-health-professionals-to-provide-care-for-underserved-populations/ (accessed on 16 December 2024).
- Health Affairs. Public Transportation in the US: A Driver of Health and Equity. Available online: https://www.healthaffairs.org/do/10.1377/hpb20210630.810356/full/ (accessed on 16 December 2024).
- Centers for Disease Control and Prevention. Public Transportation System: Introduction or Expansion. Available online: https://archive.cdc.gov/www_cdc_gov/policy/hi5/publictransportation/index.html (accessed on 16 December 2024).
- Smith, L.B.; Yang, Z. Public Transportation Facilitates Access to Health Care, Particularly for People Covered by Medicaid. Available online: https://www.urban.org/urban-wire/public-transportation-facilitates-access-health-care-particularly-people-covered-medicaid (accessed on 16 December 2024).
- Kopczewska, K.; Kubara, M.; Kopyt, M. Population density as the attractor of business to the place. Sci. Rep. 2024, 14, 22234. [Google Scholar] [CrossRef]
- Combes, P.P.; Gobillon, L. The empirics of agglomeration economies. In Handbook of Regional and Urban Economics; Elsevier: Amsterdam, The Netherlands, 2015; Vol. 5, pp. 247–348. [Google Scholar]
- Cochran, A.L.; McDonald, N.C.; Prunkl, L.; et al. Transportation barriers to care among frequent health care users during the COVID pandemic. BMC Public Health 2022, 22, 1783. [Google Scholar] [CrossRef]
- Syed, S.T.; Gerber, B.S.; Sharp, L.K. Traveling towards disease: Transportation barriers to health care access. J. Community Health 2013, 38, 976–993. [Google Scholar] [CrossRef]
- The Annie E. Casey Foundation. Child Well-Being in Single-Parent Families. Available online: https://www.aecf.org/blog/child-well-being-in-single-parent-families (accessed on 6 January 2025).
- Esri. Where Are Children in Single-Parent Families? Available online: https://www.arcgis.com/home/item.html?id=2a15d985d0ad466ab8532885a07ae61d (accessed on 6 January 2025).
- Robinson, M. Map Reveals States with Most Single-Parent Households. Available online: https://www.newsweek.com/us-census-data-map-reveals-states-most-single-parent-households-1908428 (accessed on 6 January 2025).
- Kent, D. U.S. Has World’s Highest Rate of Children Living in Single-Parent Households. Available online: https://www.pewresearch.org/short-reads/2019/12/12/u-s-children-more-likely-than-children-in-other-countries-to-live-with-just-one-parent/ (accessed on 6 January 2025).
- Raghupathi, V.; Raghupathi, W. The influence of education on health: An empirical assessment of OECD countries for the period 1995–2015. Arch. Public Health 2020, 78, 20. [Google Scholar] [CrossRef] [PubMed]
- Sullivan, K. Lack of education breeds disparities despite equal access to care. Available online: https://www.fiercehealthcare.com/healthcare/lack-education-breeds-disparities-despite-equal-access-to-care (accessed on 16 December 2024).
- Esri. Temporal Analysis. Available online: https://doc.arcgis.com/en/insights/latest/analyze/temporal-analysis.htm (accessed on 15 December 2024).
- Janatabadi, F.; Ermagun, A. Access weight matrix: A place and mobility infused spatial weight matrix. Geogr. Anal. 2024, 56, 746–767. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




