Submitted:
07 March 2026
Posted:
10 March 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Materials and Methods
Study Design and Data Source
Variables and Data Integration
Outcome Measures
Pandemic-Period Sensitivity Analysis
Statistical Analyses and Tools
Results
Study Population and Demographic Characteristics
Temporal Distribution of Gynecologic Cancer Diagnoses
Normalized Annual Gynecologic Cancer Admission Rates
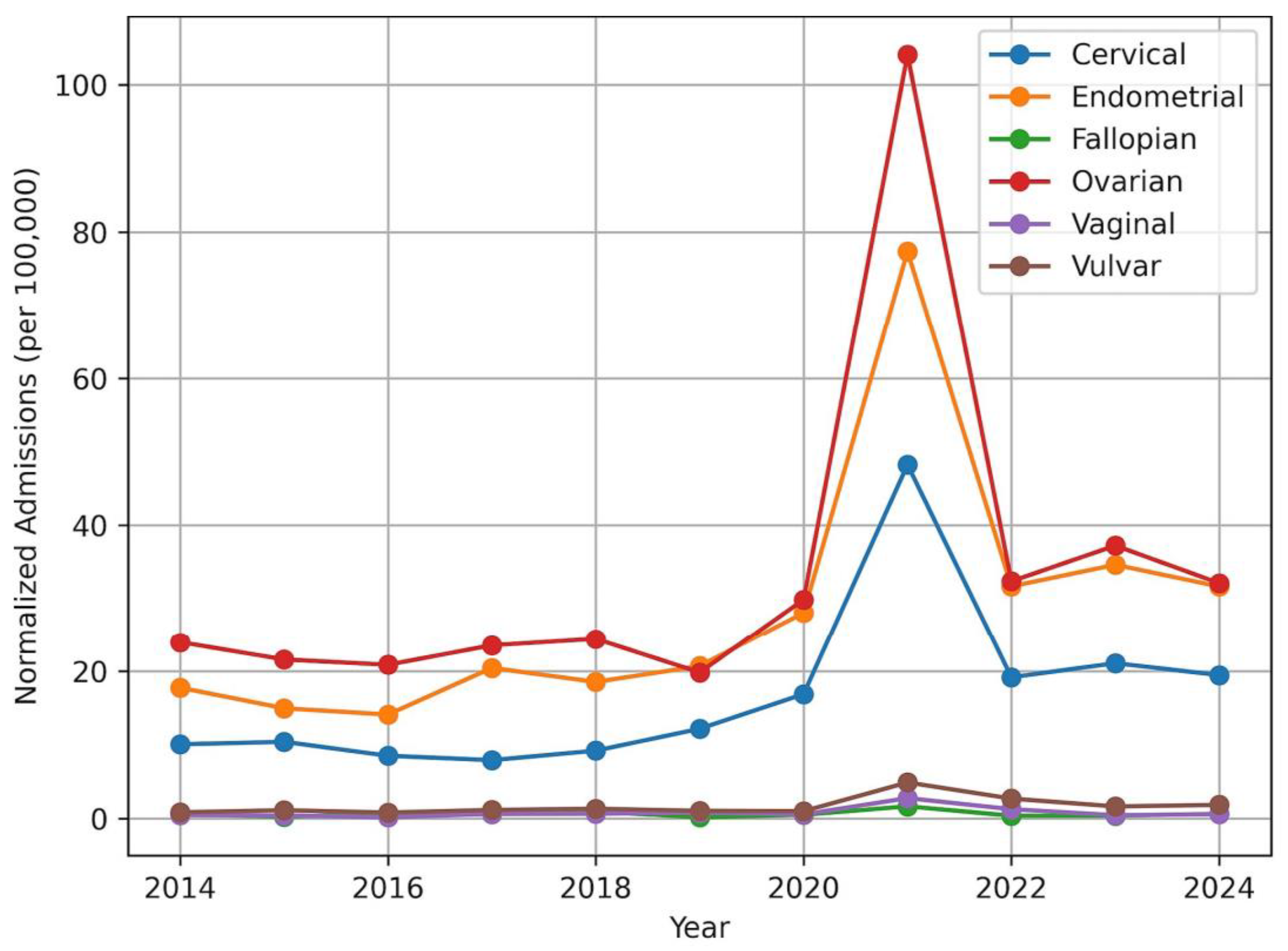
Cancer-Type–Specific Normalized Trends
Discussion
Conclusions
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Liu, L; Zhou, Y; Lin, J; Xie, N; Yu, H; Deng, S; et al. Trends in incidence and mortality for gynaecological cancers in Southeastern China during 2011-2020: a retrospective analysis of registry data. BMJ Open 2024, 14, e083336. [Google Scholar] [CrossRef] [PubMed]
- Sekar, S; Budithi, S; Fernando, S. Trends in the incidence and mortality of cervical, ovarian, and corpus uteri cancers in Wales, UK: A joinpoint regression analysis from 2002 to 2021. Cancer Epidemiol 2024, 93, 102660. [Google Scholar] [CrossRef] [PubMed]
- Lian, Y; Luo, P. Mortality of Three Major Gynecological Cancers in the European Region: An Age-Period-Cohort Analysis from 1992 to 2021 and Predictions in a 25-Year Period. Ann Glob Health 2025, 91, 30. [Google Scholar] [CrossRef] [PubMed]
- Nakai, H; Higashi, T; Kakuwa, T; Matsumura, N. Trends in gynecologic cancer in Japan: incidence from 1980 to 2019 and mortality from 1981 to 2021. Int J Clin Oncol 2024, 29, 363–71. [Google Scholar] [CrossRef] [PubMed]
- Gultekin, M; Kucukyildiz, I; Karaca, MZ; Dundar, S; Boztas, G; Turan, SH; et al. Trends of Gynecological Cancers in Turkey: Toward Europe or Asia? Int J Gynecol Cancer Off J Int Gynecol Cancer Soc 2017, 27, 1525–33. [Google Scholar] [CrossRef] [PubMed]
- Zhou, XH; Yang, DN; Zou, YX; Tang, DD; Chen, J; Li, ZY; et al. Long-Term Survival Trend of Gynecological Cancer: A Systematic Review of Population-Based Cancer Registration Data. Biomed Environ Sci BES 2024, 37, 897–921. [Google Scholar] [CrossRef] [PubMed]
- Lian, Y; Luo, P. Mortality of Three Major Gynecological Cancers in the European Region: An Age-Period-Cohort Analysis from 1992 to 2021 and Predictions in a 25-Year Period. Ann Glob Health 2025, 91, 30. [Google Scholar] [CrossRef] [PubMed]
- Olawaiye, AB; Cuello, MA; Rogers, LJ. Cancer of the vulva: 2021 update. Int J Gynaecol Obstet Off Organ Int Fed Gynaecol Obstet 2021, 155 Suppl 1, 7–18. [Google Scholar] [CrossRef] [PubMed]
- Dittmer, C; Katalinic, A; Mundhenke, C; Thill, M; Fischer, D. Epidemiology of vulvar and vaginal cancer in Germany. Arch Gynecol Obstet 2011, 284, 169–74. [Google Scholar] [CrossRef] [PubMed]
- Hemminki, K; Kanerva, A; Försti, A; Hemminki, A. Cervical, vaginal and vulvar cancer incidence and survival trends in Denmark, Finland, Norway and Sweden with implications to treatment. BMC Cancer 2022, 22, 456. [Google Scholar] [CrossRef] [PubMed]
- Zhu, B; Gu, H; Mao, Z; Beeraka, NM; Zhao, X; Anand, MP; et al. Global burden of gynaecological cancers in 2022 and projections to 2050. J Glob Health 2024, 14, 04155. [Google Scholar] [CrossRef] [PubMed]
- Emons, J; Gocke, J; Schulmeyer, C; Stübs, FA; Krückel, A; Amann, N; et al. Update Gynecologic Malignancies 2025 - Expert Opinion on Systemic Therapy for Early and Advanced Gynecological Cancers. Geburtshilfe Frauenheilkd 2025, 85, 736–45. [Google Scholar] [CrossRef] [PubMed]
- Duan, R; Zhang, H; Yu, J; Deng, S; Yang, H; Zheng, Y-T; et al. Temporal trends and projections of gynecological cancers in China, 2007-2030. BMC Womens Health 2023, 23, 346. [Google Scholar] [CrossRef] [PubMed]
- Wijayabahu, AT; Shiels, MS; Arend, RC; Clarke, MA. Uterine cancer incidence trends and 5-year relative survival by race/ethnicity and histology among women under 50 years. Am J Obstet Gynecol 2024, 231, 526.e1–526.e22. [Google Scholar] [CrossRef] [PubMed]
- Rodriguez, VE; Tanjasiri, SP; Ro, A; Hoyt, MA; Bristow, RE; LeBrón, AMW. Trends in endometrial cancer incidence in the United States by race/ethnicity and age of onset from 2000 to 2019. Am J Epidemiol 2025, 194, 103–13. [Google Scholar] [CrossRef] [PubMed]
- Zhao, X; Kong, W; Jiang, Y; Sui, F. Current and future burden of gynecological cancers attributable to high body-mass index: A comprehensive global analysis and projection study. PloS One 2025, 20, e0333281. [Google Scholar] [CrossRef] [PubMed]
- Son, Y; Hong, S; Jang, W; Kim, S; Lee, H; Lee, S; et al. Global, regional, and national burden of cervical cancer in 2022 and projections to 2050: a population-based analysis of GLOBOCAN. Int J Gynecol Cancer Off J Int Gynecol Cancer Soc 2026, 36, 102751. [Google Scholar] [CrossRef] [PubMed]
| Variables | Cases Mean ± SD, N (%) |
|---|---|
| Age | 62.75 ± 13.95 n= 22468 |
| Age Group | |
| 18 - 40 | 1211 (5.4%) |
| 40 - 60 | 7573 (33.7%) |
| > 60 | 13684 (60.9%) |
| CancerType | |
| cervical cancer | 4646 (20.7%) |
| endometrial cancer | 7789 (34.7%) |
| fallopian tube cancer | 164 (0.7%) |
| ovarian cancer | 9173 (40.8%) |
| vaginal cancer | 225 (1.0%) |
| vulvar cancer | 471 (2.1%) |
| Year of Diagnosis | |
| 2014 | 693 (3.1%) |
| 2015 | 773 (3.4%) |
| 2016 | 769 (3.4%) |
| 2017 | 1021 (4.5%) |
| 2018 | 1154 (5.1%) |
| 2019 | 1196 (5.3%) |
| 2020 | 1744 (7.8%) |
| 2021 | 6873 (30.6%) |
| 2022 | 2677 (11.9%) |
| 2023 | 2884 (12.8%) |
| 2024 | 2684 (11.9%) |
| Exitus Status | |
| No | 21844 (97.2%) |
| Yes | 624 (2.8%) |
| Overall Survival For Exitus Patients (months) | 13.13 ± 17.79 n= 563 |
| Year | Gynecologic Cancer Cases (n) | Annual Unique Patient Admissions (n) | Normalized Cancer Admission Rate (per 100,000) |
|---|---|---|---|
| 2014 | 693 | 1,289,817 | 53.7 |
| 2015 | 773 | 1,583,468 | 48.8 |
| 2016 | 769 | 1,700,543 | 45.2 |
| 2017 | 1,021 | 1,878,278 | 54.4 |
| 2018 | 1,154 | 2,093,384 | 55.1 |
| 2019 | 1,196 | 2,182,777 | 54.8 |
| 2020 | 1,744 | 2,267,602 | 76.9 |
| 2021 | 6,873 | 2,874,999 | 239.1 |
| 2022 | 2,677 | 3,055,568 | 87.6 |
| 2023 | 2,884 | 3,021,390 | 95.5 |
| 2024 | 2,684 | 3,108,271 | 86.4 |
| Variables | cervical cancer Mean ± SD, N (%) |
endometrial cancer Mean ± SD, N (%) |
fallopian tube cancer Mean ± SD, N (%) |
ovarian cancer Mean ± SD, N (%) |
vaginal cancer Mean ± SD, N (%) |
vulvar cancer Mean ± SD, N (%) |
p |
|---|---|---|---|---|---|---|---|
| Age | 58.78 ± 13.86 n= 4646 |
65.63 ± 12.34 n= 7789 |
59.54 ± 13.51 n= 164 |
62.10 ± 14.51 n= 9173 |
65.52 ± 14.26 n= 225 |
66.82 ± 17.08 n= 471 |
<0.001 |
| Age Group | |||||||
| 18 - 40 | 369 (7.9%) | 187 (2.4%) | 20 (12.2%) | 587 (6.4%) | 8 (3.6%) | 40 (8.5%) | |
| 40 - 60 | 2093 (45.0%) | 2042 (26.2%) | 56 (34.1%) | 3230 (35.2%) | 62 (27.6%) | 90 (19.1%) | |
| > 60 | 2184 (47.0%) | 5560 (71.4%) | 88 (53.7%) | 5356 (58.4%) | 155 (68.9%) | 341 (72.4%) | |
| Year of Diagnosis | |||||||
| 2014 | 130 (2.8%) | 229 (2.9%) | 8 (4.9%) | 309 (3.4%) | 6 (2.7%) | 11 (2.3%) | |
| 2015 | 165 (3.6%) | 237 (3.0%) | 4 (2.4%) | 342 (3.7%) | 7 (3.1%) | 18 (3.8%) | |
| 2016 | 145 (3.1%) | 240 (3.1%) | 12 (7.3%) | 355 (3.9%) | 3 (1.3%) | 14 (3.0%) | |
| 2017 | 149 (3.2%) | 384 (4.9%) | 12 (7.3%) | 442 (4.8%) | 12 (5.3%) | 22 (4.7%) | |
| 2018 | 193 (4.2%) | 388 (5.0%) | 20 (12.2%) | 511 (5.6%) | 14 (6.2%) | 28 (5.9%) | |
| 2019 | 266 (5.7%) | 452 (5.8%) | 4 (2.4%) | 433 (4.7%) | 18 (8.0%) | 23 (4.9%) | |
| 2020 | 383 (8.2%) | 636 (8.2%) | 12 (7.3%) | 677 (7.4%) | 13 (5.8%) | 23 (4.9%) | |
| 2021 | 1387 (29.9%) | 2225 (28.6%) | 48 (29.3%) | 2992 (32.6%) | 80 (35.6%) | 141 (29.9%) | |
| 2022 | 586 (12.6%) | 968 (12.4%) | 12 (7.3%) | 989 (10.8%) | 39 (17.3%) | 83 (17.6%) | |
| 2023 | 637 (13.7%) | 1046 (13.4%) | 12 (7.3%) | 1125 (12.3%) | 14 (6.2%) | 50 (10.6%) | |
| 2024 | 605 (13.0%) | 984 (12.6%) | 20 (12.2%) | 998 (10.9%) | 19 (8.4%) | 58 (12.3%) | |
| Exitus | <0.001 | ||||||
| No | 4546 (97.8%) | 7596 (97.5%) | 164 (100.0%) | 8859 (96.6%) | 220 (97.8%) | 459 (97.5%) | |
| Yes | 100 (2.2%) | 193 (2.5%) | 0 (0.0%) | 314 (3.4%) | 5 (2.2%) | 12 (2.5%) | |
| Overall Survival For Exitus Patients (months) | 13.07 ± 16.22 n= 89 |
12.35 ± 18.28 n= 175 |
n= 0 |
13.74 ± 18.27 n= 285 |
23.70 ± 13.15 n= 2 |
8.67 ± 9.66 n= 12 |
0.369 |
| Year | Cervical | Endometrial | Fallopian Tube | Ovarian | Vaginal | Vulvar |
|---|---|---|---|---|---|---|
| 2014 | 10.1 | 17.8 | 0.62 | 24.0 | 0.47 | 0.85 |
| 2015 | 10.4 | 15.0 | 0.25 | 21.6 | 0.44 | 1.14 |
| 2016 | 8.5 | 14.1 | 0.71 | 20.9 | 0.18 | 0.82 |
| 2017 | 7.9 | 20.4 | 0.64 | 23.5 | 0.64 | 1.17 |
| 2018 | 9.2 | 18.5 | 0.96 | 24.4 | 0.67 | 1.34 |
| 2019 | 12.2 | 20.7 | 0.18 | 19.8 | 0.82 | 1.05 |
| 2020 | 16.9 | 28.0 | 0.53 | 29.9 | 0.57 | 1.01 |
| 2021 | 48.2 | 77.4 | 1.67 | 104.1 | 2.78 | 4.90 |
| 2022 | 19.2 | 31.7 | 0.39 | 32.4 | 1.28 | 2.72 |
| 2023 | 21.1 | 34.6 | 0.40 | 37.2 | 0.46 | 1.65 |
| 2024 | 19.5 | 31.7 | 0.64 | 32.1 | 0.61 | 1.87 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




