Submitted:
05 March 2026
Posted:
06 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Setting
2.3. Participants
2.4. Ethics and Consent
2.5. Variables and Constructs
2.6. Instruments
2.7. Data Collection Procedures
2.8. Data Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Public Involvement Statement
Guidelines and Standards Statement
Use of Artificial Intelligence
Acknowledgments
Conflicts of Interest
Abbreviations
| IFI | Implementation Fidelity Index |
| PHC | Primary Health Care |
| NCDs | Non-communicable diseases |
| SD | Standard Deviation |
References
- Hasanbasri, M; Maula, AW; Wiratama, BS; Espressivo, A; Marthias, T. Analyzing Primary Healthcare Governance in Indonesia: Perspectives of Community Health Workers Data. Cureus 2024, 16(3). [Google Scholar] [CrossRef]
- Setiaasih, R; Sunjaya, DK; Sofiatin, Y; Afriandi, I; Hilfi, L. Readiness of health posts for primary health care integration in Indonesia: a mixed- methods study. BMC Public Health 2025, 25(1). [Google Scholar] [CrossRef]
- Widyaningsih, V; Augustania, C; Agustia, D; Febrinasari, RP; Fritz, M; Koot, J. Opportunities for improvement of community-based non-communicable disease screening practices in Indonesia: a participant satisfaction survey. BMC Health Serv Res. 2025, 25(1). [Google Scholar] [CrossRef]
- Solikha, DA; Butler, DC; Setiawan, E; Korda, RJ; Kelly, M. Primary health care performance measurement at the service delivery level in Indonesia: a scoping review. BMC Health Serv Res. 2025, 25(8). [Google Scholar] [CrossRef]
- Haemmerli, M; Jackson, TP; Goodman, C; Thabrany, H; Wiseman, V. Poor quality for the poor ? A study of inequalities in service readiness and provider knowledge in Indonesian primary health care facilities. Int J Equity Health 2021, 20(2), 1–12. [Google Scholar] [CrossRef]
- Beaudin, J; Chouinard, MC; Girard, A; Houle, J; Ellefsen, É; Hudon, C. Integrated self - management support provided by primary care nurses to persons with chronic diseases and common mental disorders: a scoping review. BMC Nurs. 2022, 21(2), 1–19. [Google Scholar] [CrossRef] [PubMed]
- Salma, Karami; Andrea Puspa Evindiyah Prita D; Umniyatun, Y. Evaluation of the Management Information System. J Community Health 2023, 9(3), 588–98. [Google Scholar]
- Sitthimongkol, Y; Srimoragot, M; Kasemsuk, W; Meekusol, S; Pongpattanapisit, P; Saenkla, P; et al. International Journal of Nursing Sciences Enhancing accessibility through nurse-led clinics in primary care: An integrative review of models of care. Int J Nurs Sci. 2025, 12(6), 593–600. [Google Scholar] [PubMed]
- Olson, MB; Mccreedy, EM; Baier, RR; Shield, RR; Zediker, EE; Uth, R; et al. Measuring implementation fidelity in a cluster-randomized pragmatic trial: development and use of a quantitative multi-component approach. BMC Prim Care 2022, 23(4), 1–12. [Google Scholar] [CrossRef]
- Azzellino, G; Vagnarelli, P; Passamonti, M; Mengoli, L; Ginaldi, L; De Martinis, M. Integrated Hospital – Territory Organizational Models and the Role of Family and Community Nurses in the Management of Chronic Conditions: A Scoping Review. Medicina (B Aires) 2025, 61(7), 1–23. [Google Scholar] [CrossRef]
- Damschroder, LJ; Reardon, CM; Widerquist, MAO; Lowery, J. The updated Consolidated Framework for Implementation Research based on user feedback. Implement Sci [Internet] 2022, 0, 1–16. [Google Scholar] [CrossRef] [PubMed]
- Powers, K; Clarke, S; Phillips, J; Holmes, JA; Cripps, R; Craven, K; et al. Developing an implementation fidelity checklist for a vocational rehabilitation intervention. Pilot Feasibility Stud. 2022, 1–12. [Google Scholar]
- Golden, CA; Estabrooks, PA; Heelan, KA; Bartee, RT; Porter, GC; Pereira, EL; et al. Developing an implementation fidelity measure for a family healthy weight program. Int J Behav Nutr Phys Act. 2025, 1–11. [Google Scholar]
- Fixsen, DL. Fidelity, not adaptation, is essential for implementation. Front Public Heal. 2025, 5(1), 1–8. [Google Scholar] [CrossRef] [PubMed]
- Sitthimongkol, Y; Srimoragot, M; Kasemsuk, W; Meekusol, S; Pongpattanapisit, P; Saenkla, P; et al. Enhancing accessibility through nurse-led clinics in primary care: An integrative review of models of care. Int J Nurs Sci [Internet] 2025, 12(6), 593–600. [Google Scholar] [CrossRef]
- Setiaasih, R; Sunjaya, DK; Sofiatin, Y; Afriandi, I; Hilfi, L; Herawati, DMD. Readiness of health posts for primary health care integration in Indonesia: a mixed-methods study. BMC Public Health [Internet] 2025, 25(1), 1429. [Google Scholar] [CrossRef]
- Haemmerli, M; Powell-Jackson, T; Goodman, C; Thabrany, H; Wiseman, V. Poor quality for the poor? A study of inequalities in service readiness and provider knowledge in Indonesian primary health care facilities. Int J Equity Health [Internet] 2021, 20(1), 239. [Google Scholar] [CrossRef]
- Widyaningsih, V; Augustania, C; Agustia, D; Febrinasari, RP; Fritz, M; Koot, J; et al. Opportunities for improvement of community-based non-communicable disease screening practices in Indonesia: a participant satisfaction survey. BMC Health Serv Res [Internet] 2025, 25(1), 1051. [Google Scholar] [CrossRef] [PubMed]
- Endalamaw, A; Khatri, RB; Erku, D; Zewdie, A; Wolka, E; Nigatu, F; et al. Barriers and strategies for primary health care workforce development: synthesis of evidence. BMC Prim Care [Internet] 2024, 25(1), 99. [Google Scholar] [CrossRef]
- Murad, MH; Vaa Stelling, BE; West, CP; Hasan, B; Simha, S; Saadi, S; et al. Measuring Documentation Burden in Healthcare. J Gen Intern Med [Internet] 2024, 39(14), 2837–48. [Google Scholar] [CrossRef]
- Cho, H; Nguyen, OT; Weaver, M; Pruitt, J; Marcelle, C; Salloum, RG; et al. Electronic health record system use and documentation burden of acute and critical care nurse clinicians: a mixed-methods study. J Am Med Informatics Assoc [Internet] 2024, 31(11), 2540–9. [Google Scholar] [CrossRef]
- Hesselink, G; Verhage, R; Hoiting, O; Verweij, E; Janssen, I; Westerhof, B; et al. Time spent on documenting quality indicator data and associations between the perceived burden of documenting these data and joy in work among professionals in intensive care units in the Netherlands: a multicentre cross-sectional survey. BMJ Open [Internet] 2023, 13(3), e062939–e062939. [Google Scholar] [CrossRef]
- Van Eeghen, C; Soucie, J; Clifton, J; Hitt, J; Mollis, B; Rose, GL; et al. Implementation outcomes from a randomized, controlled trial of a strategy to improve integration of behavioral health and primary care services. BMC Health Serv Res. 2024, 7(3). [Google Scholar]
- Dodds, E; Redsell, S; Timmons, S; Manning, JC. What validated instruments, that measure implementation outcomes, are suitable for use in the Paediatric Intensive Care Unit ( PICU ) setting ? A systematic review of systematic reviews. Implement Sci 2024. [Google Scholar] [CrossRef] [PubMed]
- Fontaine, G; Vinette, B; Weight, C; Maheu-Cadotte, MA; Lavallée, A; Deschênes, MF; et al. Effects of implementation strategies on nursing practice and patient outcomes: a comprehensive systematic review and meta-analysis. Implement Sci [Internet] 2024, 19(1), 68. [Google Scholar] [CrossRef] [PubMed]
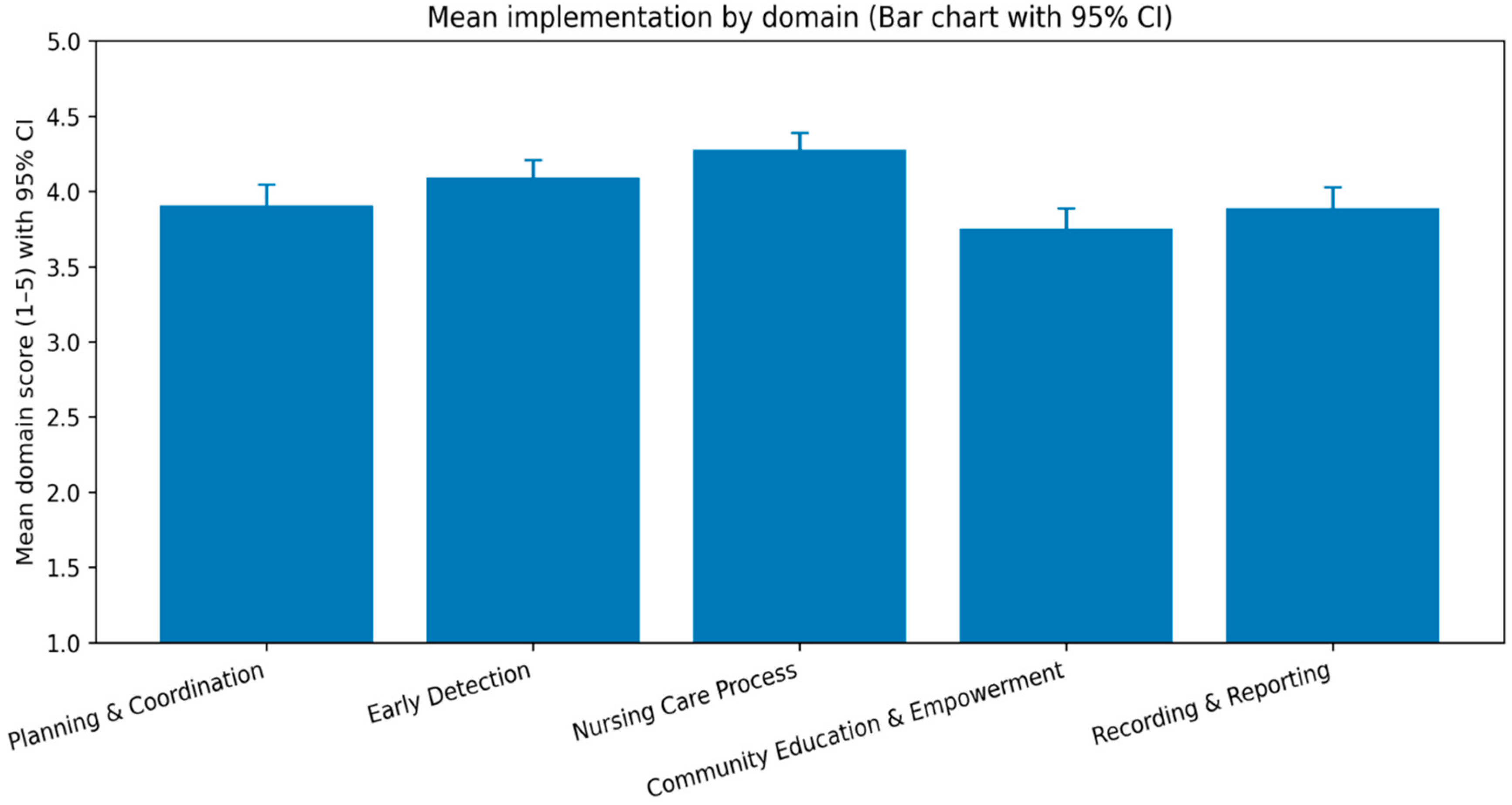
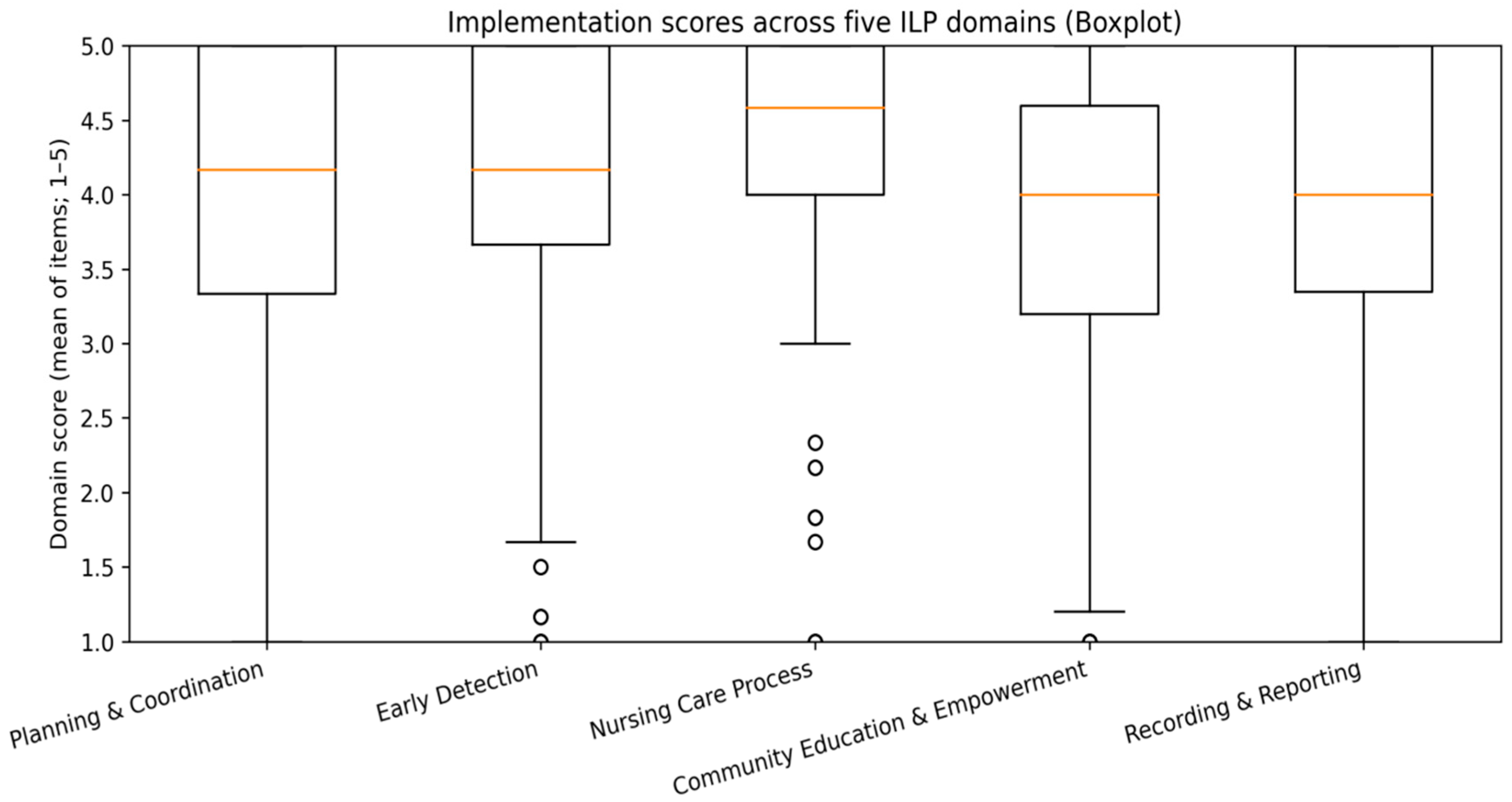
| Measure | Scoring approach | Possible range | Mean (SD) | Median (IQR) | Observed range |
|---|---|---|---|---|---|
| Overall IFI (mean score) | Mean of 28 items (each 1–5; equal weight) | 1.00–5.00 | 3.99 (0.92) | 4.14 (3.57–4.82) |
1.04–5.00 |
| Overall IFI (total score) | Sum of 28 items (each 1–5; equal weight) | 28–140 | 111.84 (25.90) | 116 (100–135) |
29–140 |
| Category | Cut-off (total score) | n | % |
|---|---|---|---|
| Low implementation | < 86 | 31 | 12.3 |
| Moderate implementation | 86–137 | 181 | 71.8 |
| High implementation | ≥ 138 | 40 | 15.9 |
| Total | 252 | 100.0 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




