Submitted:
02 March 2026
Posted:
03 March 2026
You are already at the latest version
Abstract
Keywords:
Background
Methods
Study Design and Setting
Study Population, Participants, and Sampling
Data Collection
Statistical Analysis
Ethical Considerations
Results
Characteristics of Study Participants
Forms of Discrimination Experienced by Participants Since Start of COVID-19 Pandemic
- a)
- Race-based discrimination
- b) Gender-based discrimination
- c) Sexual orientation-based discrimination
- d) Substance use-based discrimination
- e) Economic status-based discrimination
- f) Disability-based discrimination
- g) Age-based discrimination
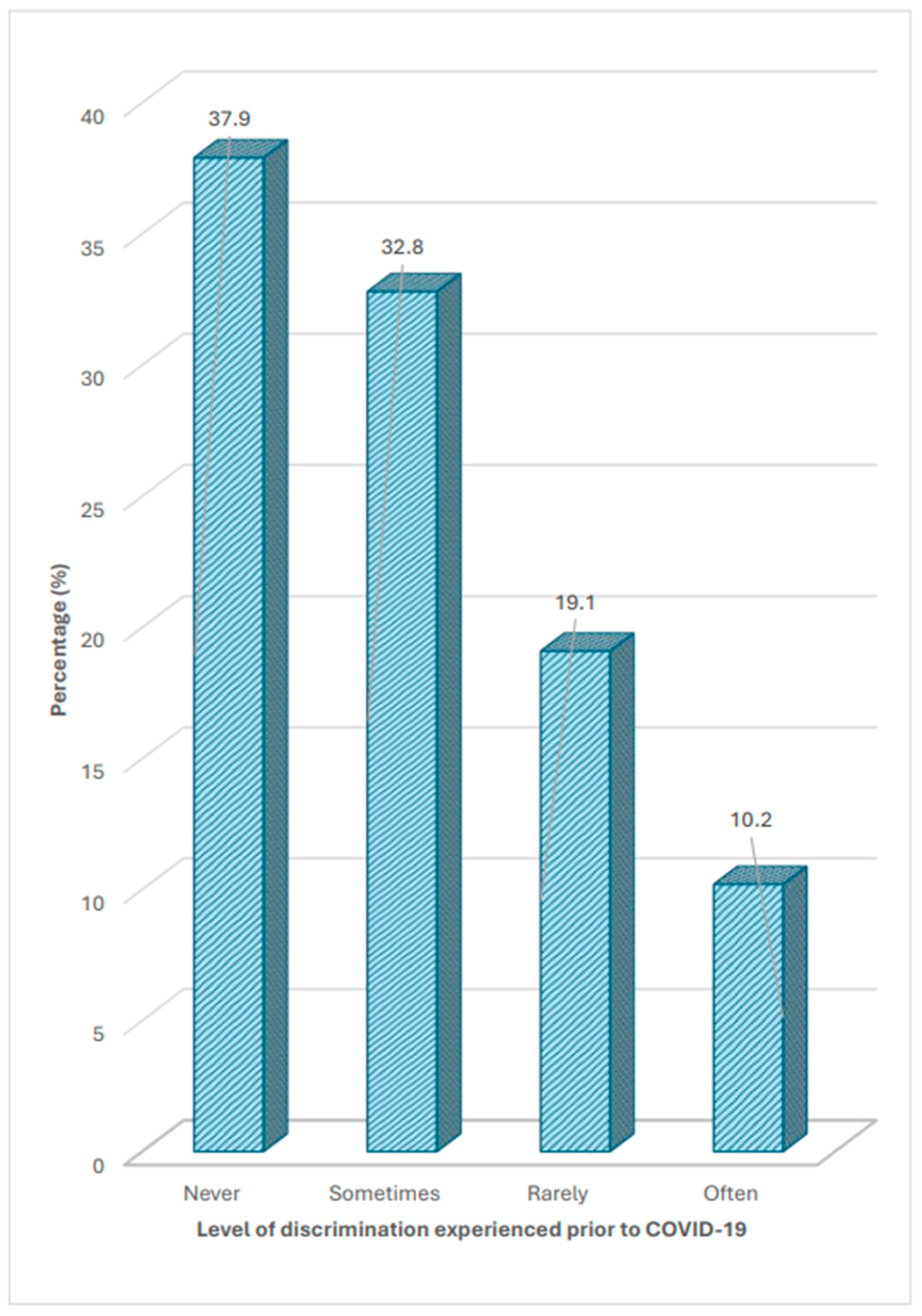
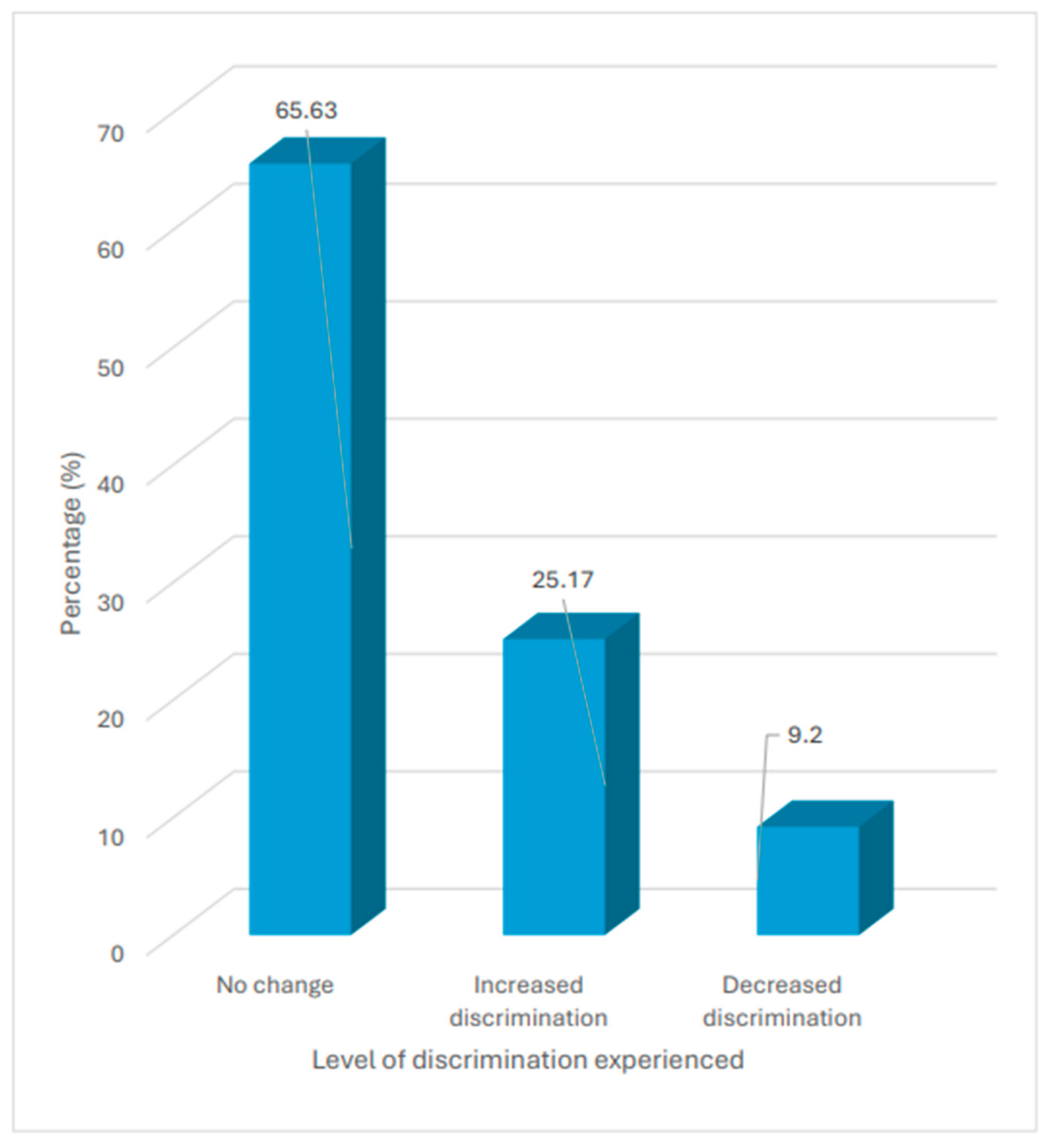
Participants’ Discrimination Prior and During COVID-19 Pandemic
Factors Associated with Increased Experiences of Discrimination During COVID-19
Discussion
Limitations and Strengths of This Study
Conclusion
Availability of data and materials
Competing interests
Funding Statement
Author Contributions
Acknowledgments
Abbreviations
| AB | Alberta |
| ACB | African, Caribbean and Black |
| aOR | Adjusted odds ratio |
| BC | British Columbia |
| CHC | Community Health Centre |
| COVID-19 | Coronavirus disease 2019 |
| CI | Confidence interval |
| HIV | Human immunodeficiency virus |
| MB | Manitoba |
| N | Frequency |
| NB | New Brunswick |
| NL | Newfoundland and Labrador |
| NS | Nova Scotia |
| NU | Nunavut |
| NWT | Northwest Territories |
| ON | Ontario |
| OR | Odds ratio |
| PEI | Prince Edward Island |
| PHAC | Public Health Agency of Canada |
| QC | Québec |
| REB | Research Ethics Board |
| Ref | Reference variable |
| SK | Saskatchewan |
| STBBI | Sexually transmitted and blood-borne infections |
| USA | United States of America |
| YT | Yukon Territories |
References
- WHO. The COVID-19 pandemic and continuing challenges to global health [Internet]. 2025. Available online: https://www.who.int/about/funding/invest-in-who/investment-case-2.0/challenges.
- Filip, R; Gheorghita Puscaselu, R; Anchidin-Norocel, L; Dimian, M; Savage, WK. Global Challenges to Public Health Care Systems during the COVID-19 Pandemic: A Review of Pandemic Measures and Problems. J Pers Med. 2022, 12(8), 1295. [Google Scholar] [CrossRef]
- Olanlesi-Aliu, A; Kemei, J; Alaazi, D; Tunde-Byass, M; Renzaho, A; Sekyi-Out, A; Mullings, DV; Osei-Tutu, K; Salami, B. Evidence synthesis - COVID-19 among Black people in Canada: a scoping review. Health Promot Chronic Dis Prev Can Res Policy Pract. 2024, 44(3), 112–25. [Google Scholar]
- Vanden Bossche, D; Zhao, QJ; Ares-Blanco, S; Peña, MPA; Decat, P; Kondo, N; Kroneman, M; Nishioka, D; Petrazzuoli, F; Rortveit, G; Schaubroeck, E; Stark, S; Pinto, AD; Willems, S. Addressing health inequity during the COVID-19 pandemic through primary health care and public health collaboration: a multiple case study analysis in eight high-income countries. Int J Equity Health 2023, 22(1), 171. [Google Scholar] [CrossRef]
- Komeiha, M; Artyukh, I; Ogundele, OJ; Zhao, QJ; Massaquoi, N; Straus, S; Razak, F; Hosseini, B; Persaud, N; Mishra, S; Eissa, A; Isabel, M; Pinto, AD. Unveiling the Impact: A Scoping Review of the COVID-19 Pandemic’s Effects on Racialized Populations in Canada. Int J Environ Res Public Health 2025, 22(7), 1054. [Google Scholar] [CrossRef] [PubMed]
- Willems, SJ; Castells, MC; Baptist, AP. The Magnification of Health Disparities During the COVID-19 Pandemic. J Allergy Clin Immunol Pract. 2022, 10(4), 903–8. [Google Scholar] [CrossRef] [PubMed]
- Malcom. 1 in 5 Have Been Discriminated Against in the Healthcare Setting [Internet]. 2020. Available online: https://www.michiganmedicine.org/health-lab/1-5-have-been-discriminated-against-healthcare-setting.
- Nong, P; Raj, M; Creary, M; Kardia, SLR; Platt, JE. Patient-Reported Experiences of Discrimination in the US Health Care System. JAMA Netw Open 2020, 3(12), e2029650. [Google Scholar] [CrossRef]
- Rosemberg, MAS; Tsai, JHC. Connecting Gender, Race, Class, and Immigration Status to Disease Management at the Workplace. J Health Disparities Res Pract. 2014, 7(5), 13–31. [Google Scholar]
- Loi, S; Li, P; Myrskylä, M. Unequal weathering: How immigrants’ health advantage vanishes over the life-course. J Migr Health 2025, 11, 100303. [Google Scholar] [CrossRef]
- Macias-Konstantopoulos, WL; Collins, KA; Diaz, R; Duber, HC; Edwards, CD; Hsu, AP; Ranney, ML; Riviello, RJ; Wettstein, ZS; Sachs, CJ. Race, Healthcare, and Health Disparities: A Critical Review and Recommendations for Advancing Health Equity. West J Emerg Med 2023, 24(5), 906–18. [Google Scholar] [CrossRef]
- DiA, AL. Minorities have longer wait times at hospital than whites [Internet]. Al Día News. 2025. Available online: https://aldianews.com/en/leadership/advocacy/minorities-have-longer-wait.
- Hennein, R; Gorman, H; Chung, V; Lowe, SR. Gender discrimination among women healthcare workers during the COVID-19 pandemic: Findings from a mixed methods study. PloS One 2023, 18(2), e0281367. [Google Scholar] [CrossRef]
- Statistics Canada. The Daily — Half of racialized people have experienced discrimination or unfair treatment in the past five years [Internet]. 2024. Available online: https://www150.statcan.gc.ca/n1/daily-quotidien/240516/dq240516b-eng.htm.
- Burrowes, SAB; Casey, SM; Pierre-Joseph, N; Talbot, SG; Hall, T; Christian-Brathwaite, N; Del-Carmen, M; Garofalo, C; Lundberg, B; Mehta, PK; Mottl-Santiago, J; Schechter-Perkins, EM; Weber, A; Yarrington, CD; Perkins, RB. COVID-19 pandemic impacts on mental health, burnout, and longevity in the workplace among healthcare workers: A mixed methods study. J Interprofessional Educ Pract. 2023, 32, 100661. [Google Scholar] [CrossRef]
- Maunder, RG; Heeney, ND; Strudwick, G; Shin, HD; O’Neill, B; Young, N; Jeffs, LP; Barrett, K; Bodmer, NS; Born, KB; Hopkins, J; Jüni, P; Perkhun, A; Price, DJ; Razak, F; Mushquash, CJ; Mah, L. Burnout in Hospital-Based Healthcare Workers during COVID-19 [Internet]. Ontario COVID-19 Science Advisory Table. Oct 2021. Available online: https://covid19-sciencetable.ca/sciencebrief/burnout-in-hospital-based-healthcare-workers-during-covid-19.
- Cénat, JM. Racial discrimination in healthcare services among Black individuals in Canada as a major threat for public health: its association with COVID-19 vaccine mistrust and uptake, conspiracy beliefs, depression, anxiety, stress, and community resilience. Public Health 2024, 230, 207–15. [Google Scholar] [CrossRef] [PubMed]
- Elam-Evans, LD; Jones, CP; Vashist, K; Yankey, D; Smith, CS; Kriss, JL; Lu, PJ; St. Louis, ME; Brewer, NT; Singleton. The Association of Reported Experiences of Racial and Ethnic Discrimination in Health Care with COVID-19 Vaccination Status and Intent — United States, April 22, 2021–November 26, 2022. In MMWR Morb Mortal Wkly Rep [Internet]; 2023; p. 72. Available online: https://www.cdc.gov/mmwr/volumes/72/wr/mm7216a5.htm.
- Statistics Canada. Quality of life indicator: Discrimination and unfair treatment [Internet]. 2022. Available online: https://www.statcan.gc.ca/hub-carrefour/quality-life-qualite-vie/good-governance-saine-gouvernance/discrimination-eng.htm.
- Fernandez, JR; Richmond, J; Strassle, PD; Cunningham-Erves, J; Forde, AT. Motivators and Barriers to COVID-19 Vaccination Intentions Across U.S. County-Level Barriers in the COVID-19 Vaccine Coverage Index. J Racial Ethn Health Disparities [Internet]. Available from. 2 Aug 2024. [CrossRef]
- Kriss, JL; Hung, MC; Srivastav, A; Black, CL; Lindley, MC; Lee, JT; Koppaka, R; Tsai, Y; Lu, PJ; Yankey, D; Elam-Evans, LD; Singleton, JA. COVID-19 Vaccination Coverage, by Race and Ethnicity - National Immunization Survey Adult COVID Module, United States, December 2020-November 2021. MMWR Morb Mortal Wkly Rep. 2022, 71(23), 757–63. [Google Scholar] [CrossRef] [PubMed]
- Strassle, PD; Stewart, AL; Quintero, SM; Bonilla, J; Alhomsi, A; Santana-Ufret, V; Maldonado, AI; Forde, AT; Nápoles, AM. COVID-19-Related Discrimination Among Racial/Ethnic Minorities and Other Marginalized Communities in the United States. Am J Public Health 2022, 112(3), 453–66. [Google Scholar] [CrossRef] [PubMed]
- Suran, M. White Individuals Experience Less COVID-19–Related Discrimination. JAMA 2022, 327(16), 1538. [Google Scholar] [CrossRef]
- NIH. People from racial, ethnic, and other groups report frequent COVID-19–related discrimination | National Institutes of Health (NIH) [Internet]. 2025. Available online: https://www.nih.gov/news-events/news-releases/people-racial-ethnic-other-groups-report-frequent-covid-19-related-discrimination.
- Statistics Canada. Experiences of discrimination among the Black and Indigenous populations in Canada, 2019 [Internet]. 2022. Available online: https://www150.statcan.gc.ca/n1/pub/85-002-x/2022001/article/00002-eng.htm.
- Council of Europe. Intersectionality and Multiple Discrimination - Gender Matters - www.coe.int [Internet]. Gender Matters. 2025. Available online: https://www.coe.int/en/web/gender-matters/intersectionality-and-multiple-discrimination.
- Cormack, D; Stanley, J; Harris, R. Multiple forms of discrimination and relationships with health and wellbeing: findings from national cross-sectional surveys in Aotearoa/New Zealand. Int J Equity Health 2018, 17(1), 26. [Google Scholar] [CrossRef]
- Ontario Human Rights Commission. An intersectional approach to discrimination: Addressing multiple grounds in human rights claims [Internet]. 2025. Available online: https://www.ohrc.on.ca/en/book/export/html/2467.
- Grollman, TS. The Importance of Intersectionality: Multiple Forms of Discrimination and Health - Sociological Images [Internet]. 2025. Available online: https://thesocietypages.org/socimages/2012/07/05/the-importance-of-intersectionality-multiple-forms-of-discrimination-and-health/.
- PHAC. COVID-19 and the impact on services for sexually transmitted and blood-borne infections: Overview [Internet]. 2023. Available online: https://www.canada.ca/en/public-health/services/publications/diseases-conditions/covid-19-impact-services-sexually-transmitted-blood-borne-infections.html.
- PHAC. Survey on the impact of COVID-19 on access to STBBI-related services, including harm reduction services, for African, Caribbean and Black people in Canada [Internet]. 2022. Available online: https://www.canada.ca/en/public-health/services/publications/diseases-conditions/survey-impact-covid-19-access-stbbi-harm-reduction-services-african-caribbean-black-people.html.
- Bursac, Z; Gauss, CH; Williams, DK; Hosmer, DW. Purposeful selection of variables in logistic regression. Source Code Biol Med. 2008, 3, 17. [Google Scholar] [CrossRef]
- Ryu, S; Hirschtick, JL; Allgood, KL; Orellana, R; Fleischer, NL. Racial discrimination in healthcare settings and mental health among a population-based sample of racial and ethnic minoritized adults with COVID-19 in Michigan. Prev Med Rep. 2023, 36, 102529. [Google Scholar] [CrossRef]
- Zhang, X; Yu, P; Yan, J; Ton, A M; Spil, I. Using diffusion of innovation theory to understand the factors impacting patient acceptance and use of consumer e-health innovations: a case study in a primary care clinic. BMC Health Serv Res 2015, 15, 71. [Google Scholar] [CrossRef]
- Miconi, D; Li, ZY; Frounfelker, RL; Venkatesh, V; Rousseau, C. Socio-cultural correlates of self-reported experiences of discrimination related to COVID-19 in a culturally diverse sample of Canadian adults. Int J Intercult Relat. 2021, 81, 176–92. [Google Scholar] [CrossRef]
- Yu, H; Bauermeister, JA; Oyiborhoro, U; Villarruel, AM; Bonett, S. The relationship between racial discrimination in healthcare, loneliness, and mental health among Black Philadelphia residents. Int J Equity Health 2025, 24(1), 109. [Google Scholar] [CrossRef]
- McMurtry, CL; Findling, MG; Casey, LS; Blendon, RJ; Benson, JM; Sayde, JM; Miller, C. Discrimination in the United States: Experiences of Asian Americans. Health Serv Res. 2019, 54 (Suppl 2), 1419–30. [Google Scholar] [CrossRef] [PubMed]
- Ojukwu, E; Hirani, S; Sotindjo, T; McKay, E; Okedo-Alex, I; Magagula, P; Pashaei, A; Agudosi, GM. The Impact of Intersectional Discrimination and Stigma on HIV Care for African, Caribbean, and Black Women Living With HIV During the COVID-19 Pandemic in British Columbia: A Descriptive Study. J Assoc Nurses AIDS Care 2024, 35(3), 175–88. [Google Scholar] [CrossRef] [PubMed]
- Logie, C; Ll, James; Tharao, W; Loutfy, M. Associations Between HIV-Related Stigma, Racial Discrimination, Gender Discrimination, and Depression Among HIV-Positive African, Caribbean, and Black Women in Ontario, Canada. AIDS Patient Care STDs 2013, 27(2), 114–22. [Google Scholar] [CrossRef] [PubMed]
- Agterberg, S; Weinberger, AH; Stanton, CA; Shuter, J. Perceived racial/ethnic discrimination and cigarette smoking behaviors among a sample of people with HIV. J Behav Med. 2023, 46(5), 801–11. [Google Scholar] [CrossRef]
- Alexander, AC; Hébert, ET; Businelle, MS; Kendzor, DE. Everyday discrimination indirectly influences smoking cessation through post-quit self-efficacy. Drug Alcohol Depend. 2019, 198, 63–9. [Google Scholar] [CrossRef]
- Janoušková, M; Pekara, J; Kučera, M; Kearns, PB; Šeblová, J; Wolfová, K; Kuklová, M; Šeblová, D. Experiences of stigma, discrimination and violence and their impact on the mental health of health care workers during the COVID-19 pandemic. Sci Rep. 2024, 14(1), 10534. [Google Scholar] [CrossRef]
- Williams, DR; Lawrence, JA; Davis, BA; Vu, C. Understanding how discrimination can affect health. Health Serv Res. 2019, 54 (Suppl 2), 1374–88. [Google Scholar] [CrossRef]
- Hamed, S; Bradby, H; Ahlberg, BM; Thapar-Björkert, S. Racism in healthcare: a scoping review. BMC Public Health 2022, 22(1), 988. [Google Scholar] [CrossRef]
- Ramsoondar, N; Anawati, A; Cameron, E. Racism as a determinant of health and health care. Can Fam Physician 2023, 69(9), 594–8. [Google Scholar] [CrossRef]
- Baciu, A; Negussie, Y; Geller, A; Weinstein, JN; National Academies of Sciences E; Division H and M; Practice B on PH and PH; States C on CBS to PHE in the U. The Root Causes of Health Inequity. In Communities in Action: Pathways to Health Equity [Internet]; National Academies Press (US), 2017; Available online: https://www.ncbi.nlm.nih.gov/books/NBK425845/.
| Characteristic | N | % |
|---|---|---|
| Province or territory of residence | ||
| British Columbia | 169 | 10.9 |
| Alberta | 170 | 10.9 |
| Saskatchewan | 30 | 1.9 |
| Manitoba | 19 | 1.2 |
| Ontario | 664 | 42.7 |
| Quebec | 197 | 12.7 |
| New Brunswick | 62 | 4.0 |
| Nova Scotia | 54 | 3.5 |
| Prince Edward Island | 67 | 4.3 |
| Newfoundland and Labrador | 81 | 5.2 |
| Territories | 39 | 2.5 |
| None of the above | 2 | 0.1 |
| Age (years) | ||
| 18-24 | 178 | 11.4 |
| 25-39 | 616 | 39.6 |
| 40-54 | 519 | 33.4 |
| 55-64 | 173 | 11.1 |
| 65+ | 70 | 4.5 |
| Race or racial background | ||
| Black African | 983 | 63.2 |
| Black Caribbean | 441 | 28.3 |
| Black Indigenous or Black Canadian | 113 | 7.3 |
| Black American | 27 | 1.7 |
| Black Latin American | 17 | 1.1 |
| Multiracial (one Black parent) | 103 | 6.6 |
| Another Black race | 25 | 1.6 |
| Gender identity | ||
| Cisgender woman | 990 | 66.2 |
| Cisgender man | 462 | 30.9 |
| Transfeminine | 11 | 0.7 |
| Transmasculine | 33 | 2.2 |
| Sexual orientation | ||
| Heterosexual or straight | 1271 | 81.8 |
| Gay or lesbian | 73 | 4.7 |
| Bisexual | 102 | 6.6 |
| Two-spirit | 10 | 0.6 |
| Other | 55 | 3.5 |
| Don’t know | 42 | 2.7 |
| Citizenship status | ||
| Canadian born citizen | 358 | 23.2 |
| Canadian naturalized citizen | 630 | 40.8 |
| Permanent resident | 291 | 18.8 |
| Refugee or protected person | 59 | 3.8 |
| Refugee claimant or person needing protection | 35 | 2.3 |
| Asylum seeker | 5 | 0.3 |
| Temporary resident | 155 | 10.0 |
| Undocumented or no immigration status | 7 | 0.5 |
| Other | 6 | 0.4 |
| Number of years lived in Canada (years) | ||
| <5 | 282 | 29.0 |
| 5-9 | 229 | 23.5 |
| 10-14 | 167 | 17.2 |
| 15-19 | 81 | 8.3 |
| 20-24 | 63 | 6.5 |
| 25+ | 152 | 15.6 |
| Education | ||
| Less than high school | 67 | 4.6 |
| High school | 105 | 7.2 |
| Some college/vocational training | 94 | 6.4 |
| Completed college/vocational training | 159 | 10.9 |
| Some university | 111 | 7.6 |
| Completed university certificate or diploma | 131 | 9.0 |
| University undergraduate degree | 356 | 24.4 |
| University graduate or professional degree | 429 | 29.3 |
| Other | 10 | 0.7 |
| Employment | ||
| Unemployed | 336 | 22.6 |
| Student | 141 | 9.5 |
| Work part time | 263 | 17.7 |
| Work full time | 749 | 50.3 |
| Housing status | ||
| Stable housing | 1456 | 93.6 |
| Precarious housing | 99 | 6.4 |
| Health insurance coverage | ||
| Yes | 1031 | 66.3 |
| No | 373 | 24.0 |
| Don’t know | 150 | 9.7 |
| Indicator | N | % |
|---|---|---|
| Experienced race-based discrimination since start of COVID-19 pandemic | ||
| None | 328 | 33.6 |
| Any | 647 | 66.4 |
| Change in experienced race-based discrimination since start of COVID-19 | ||
| Increase | 202 | 31.2 |
| No change | 426 | 65.8 |
| Decrease | 19 | 2.9 |
| Experienced gender-based discrimination | ||
| None | 405 | 42.2 |
| Any | 555 | 57.8 |
| Change in experienced gender-based discrimination | ||
| Increase | 85 | 15.3 |
| No change | 453 | 81.6 |
| Decrease | 17 | 3.1 |
| Experienced sexual orientation-based discrimination | ||
| None | 505 | 53.2 |
| Any | 445 | 46.8 |
| Change in experiend sexual orientation-based discrimination | ||
| Increase | 48 | 10.8 |
| No change | 384 | 86.3 |
| Decrease | 13 | 2.9 |
| Experienced substance use-based discrimination | ||
| None | 604 | 64.5 |
| Any | 333 | 35.5 |
| Change in experienced substance use-based discrimination | ||
| Increase | 53 | 15.9 |
| No change | 270 | 81.1 |
| Decrease | 10 | 3.0 |
| Experienced economic status-based discrimination | ||
| None | 414 | 42.7 |
| Any | 555 | 57.3 |
| Change in experienced economic status-based discrimination | ||
| Increase | 104 | 18.7 |
| No change | 376 | 67.8 |
| Decrease | 75 | 13.5 |
| Experienced disability-based discrimination | ||
| None | 565 | 59.7 |
| Any | 382 | 40.3 |
| Change in experienced disability-based discrimination | ||
| Increase | 65 | 17.0 |
| No change | 294 | 77.0 |
| Decrease | 23 | 6.0 |
| Experienced age-based discrimination | ||
| None | 484 | 51.1 |
| Any | 463 | 48.9 |
| Change in experienced age-based discrimination | ||
| Increased | 84 | 18.1 |
| No change | 372 | 80.4 |
| Decreased | 7 | 1.5 |
| Characteristic | N | % | Increased experience of discrimination | P-values | |
|---|---|---|---|---|---|
| OR | 95% CI | ||||
| Province or territory of residence | |||||
| Western (BC) | 36 | 27.69 | Ref | ||
| Central (ON, QC) | 27 | 25.47 | 0.89 | 0.50-1.60 | 0.70 |
| Prairies (AB, SK, MB) | 112 | 24.14 | 0.83 | 0.54-1.29 | 0.41 |
| Atlantic (NB, NS, PEI, NL) | 47 | 27.33 | 0.98 | 0.59-1.63 | 0.94 |
| Northern (YT, NWT, NU) | 5 | 16.67 | 0.52 | 0.19-1.47 | 0.22 |
| Age (years) | |||||
| 31-40 | 79 | 30.74 | Ref | ||
| ≤20 | 4 | 14.81 | 0.39 | 0.13-1.17 | 0.09 |
| 21-30 | 54 | 25.23 | 0.76 | 0.51-1.14 | 0.19 |
| 41-50 | 58 | 28.43 | 0.90 | 0.60-1.34 | 0.59 |
| >50 | 32 | 16.00 | 0.43 | 0.27-0.68 | <0.01 |
| Gender identity | |||||
| Cisgender female or transfeminine | 153 | 25.21 | Ref | ||
| Cisgender male or transmasculine | 66 | 24.00 | 0.94 | 0.67-1.31 | 0.70 |
| Sex orientation | |||||
| Not heterosexual or straight | 45 | 29.03 | Ref | ||
| Heterosexual or straight | 182 | 24.43 | 0.79 | 0.54-1.16 | 0.23 |
| Canadian citizen | |||||
| No | 85 | 27.96 | Ref | ||
| Yes | 81 | 21.95 | 0.72 | 0.51-1.03 | 0.07 |
| Number of years lived in Canada (years) | |||||
| <5 | 48 | 31.17 | Ref | ||
| 5-10 | 42 | 22.46 | 0.64 | 0.39-1.04 | 0.07 |
| >10 | 64 | 24.71 | 0.72 | 0.47-1.13 | 0.15 |
| Education | |||||
| High school | 61 | 28.77 | Ref | ||
| Less than high school | 22 | 24.18 | 0.79 | 0.45-1.39 | 0.41 |
| Some college/vocational training | 71 | 23.20 | 0.75 | 0.50-1.11 | 0.15 |
| Completed university certificate or diploma | 72 | 25.71 | 0.86 | 0.57-1.28 | 0.45 |
| Housing status | |||||
| Living with friend/roommate | 38 | 29.23 | Ref | ||
| Living with family | 140 | 23.73 | 0.75 | 0.49-1.15 | 0.19 |
| Living alone/shelter/homeless | 48 | 28.57 | 0.97 | 0.58-1.60 | 0.90 |
| Employment | |||||
| Unemployed | 42 | 26.75 | Ref | ||
| Student | 18 | 24.66 | 0.90 | 0.47-1.70 | 0.74 |
| Work part time | 43 | 26.38 | 0.98 | 0.60-1.61 | 0.94 |
| Work full time | 120 | 24.19 | 0.87 | 0.58-1.32 | 0.52 |
| Characteristic | N | % | Increased experience of discrimination | P-values | |
|---|---|---|---|---|---|
| OR | 95% CI | ||||
| Province or territory of residence | |||||
| Western (BC) | 36 | 27.69 | Ref | ||
| Central (ON, QC) | 27 | 25.47 | 0.89 | 0.43-1.85 | 0.75 |
| Prairies (AB, SK, MB) | 112 | 24.14 | 0.83 | 0.48-1.44 | 0.52 |
| Atlantic (NB, NS, PEI, NL) | 47 | 27.33 | 0.74 | 0.37-1.47 | 0.39 |
| Northern (YT, NWT, NU) | 5 | 16.67 | 0.41 | 0.11-1.57 | 0.19 |
| Age (years) | |||||
| 31-40 | 79 | 30.74 | Ref | ||
| ≤20 | 4 | 14.81 | 0.77 | 0.21-2.81 | o.69 |
| 21-30 | 54 | 25.23 | 0.65 | 0.37-1.13 | 0.13 |
| 41-50 | 58 | 28.43 | 0.74 | 0.37-1.47 | 0.39 |
| >50 | 32 | 16.00 | 0.38 | 0.21-0.69 | <0.01 |
| Sex orientation | |||||
| Not heterosexual or straight | 45 | 29.03 | Ref | ||
| Heterosexual or straight | 182 | 24.43 | 0.78 | 0.45-1.33 | 0.36 |
| Canadian citizen | |||||
| No | 85 | 27.96 | Ref | ||
| Yes | 81 | 21.95 | 0.75 | 0.41-1.35 | 0.34 |
| Number of years lived in Canada (years) | |||||
| <5 | 48 | 31.17 | Ref | ||
| 5-10 | 42 | 22.46 | 0.75 | 0.41-1.31 | 0.31 |
| >10 | 64 | 24.71 | 1.11 | 0.56-2.22 | 0.77 |
| Education | |||||
| High school | 61 | 28.77 | Ref | ||
| Less than high school | 22 | 24.18 | 0.82 | 0.37-1.83 | 0.63 |
| Some college/vocational training | 71 | 23.20 | 0.72 | 0.42-1.23 | 0.23 |
| Completed university certificate or diploma | 72 | 25.71 | 0.90 | 0.52-1.56 | 0.71 |
| Housing status | |||||
| Living with friend/roommate | 38 | 29.23 | Ref | ||
| Living with family | 140 | 23.73 | 0.83 | 0.47-1.45 | 0.51 |
| Living alone/shelter/homeless | 48 | 28.57 | 1.35 | 0.69-2.66 | 0.39 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).





