Submitted:
01 March 2026
Posted:
03 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Study Population and Eligibility Criteria
2.3. Data Collection and Variables
2.4. Statistical Analysis
2.5. Ethical Considerations
2.6. Data Availability and Use of Generative Artificial Intelligence
3. Results
3.1. Patient Characteristics
| Characteristic | n (%) |
|---|---|
| Median age (IQR) | 6.5 years (0–32) |
| Sex | |
| Male | 142 (53.4) |
| Female | 124 (46.6) |
| Age group (years) | |
| <1 | 90 (33.8) |
| 1–14 | 65 (24.4) |
| 15–34 | 50 (18.8) |
| 35–55 | 36 (13.5) |
| ≥56 | 25 (9.4) |
| ICU type | |
| Adult | 110 (41.4) |
| Paediatric | 92 (34.6) |
| Neonatal | 64 (24.1) |
| Urinary catheter present | 132 (49.6) |
| Mortality | 72 (27.1) |
3.2. Prevalence and Spectrum of Healthcare-Associated Infections
| HAI Type | n (%) |
|---|---|
| Ventilator-associated pneumonia (VAP) | 37 (40.2) |
| Central line-associated bloodstream infection (CLABSI) | 26 (28.3) |
| Catheter-associated urinary tract infection (CAUTI) | 23 (25.0) |
| Surgical site infection (SSI) | 6 (6.5) |
3.3. Microbiological Profile and Antibiotic Utilisation
| Domain | Category | Variable | n | % |
|---|---|---|---|---|
| Microbiological Profile | Gram-negative isolates | Acinetobacter baumannii | 32 | 21.1 |
| Escherichia coli | 21 | 13.8 | ||
| Klebsiella pneumoniae | 17 | 11.2 | ||
| Pseudomonas aeruginosa | 16 | 10.5 | ||
| Fungal isolates | Candida species | 16 | 10.5 | |
| Gram-positive isolates | Coagulase-negative staphylococci | 17 | 11.2 | |
| Staphylococcus aureus | 12 | 7.9 | ||
| Enterococcus faecalis | 6 | 3.9 | ||
| Streptococcus group D | 5 | 3.3 | ||
| Antibiotic Utilisation | Adult ICU (most prescribed) | Ceftriaxone | 27 | 21.4* |
| Amoxicillin–clavulanate | 22 | 17.5* | ||
| Meropenem | 21 | 16.7* | ||
| Paediatric ICU (most prescribed) | Azithromycin | 32 | 22.5* | |
| Ampicillin | 27 | 19.0* | ||
| Meropenem | 21 | 14.8* | ||
| Neonatal ICU (most prescribed) | Ampicillin | 61 | 31.8* | |
| Gentamicin | 57 | 29.7* | ||
| Meropenem | 20 | 10.4* |
3.4. Risk Factors for Healthcare-Associated Infection
| Variable | AOR | 95% CI | p-value | Interpretation |
|---|---|---|---|---|
| Prolonged ICU stay (>8 days) | 4.51 | 2.39–8.50 | <0.001 | Independent risk factor |
| Age 1–14 years | 0.32 | Not reported | 0.006 | Protective vs infants |
| Age 15–34 years | 0.35 | Not reported | 0.021 | Protective vs infants |
| Sex | — | — | >0.05 | Not independently associated |
| Urinary catheterisation | — | — | >0.05 | Not independently associated |
| Invasive device presence | — | — | >0.05 | Not independently associated |
3.5. Healthcare-Associated Infection and Mortality
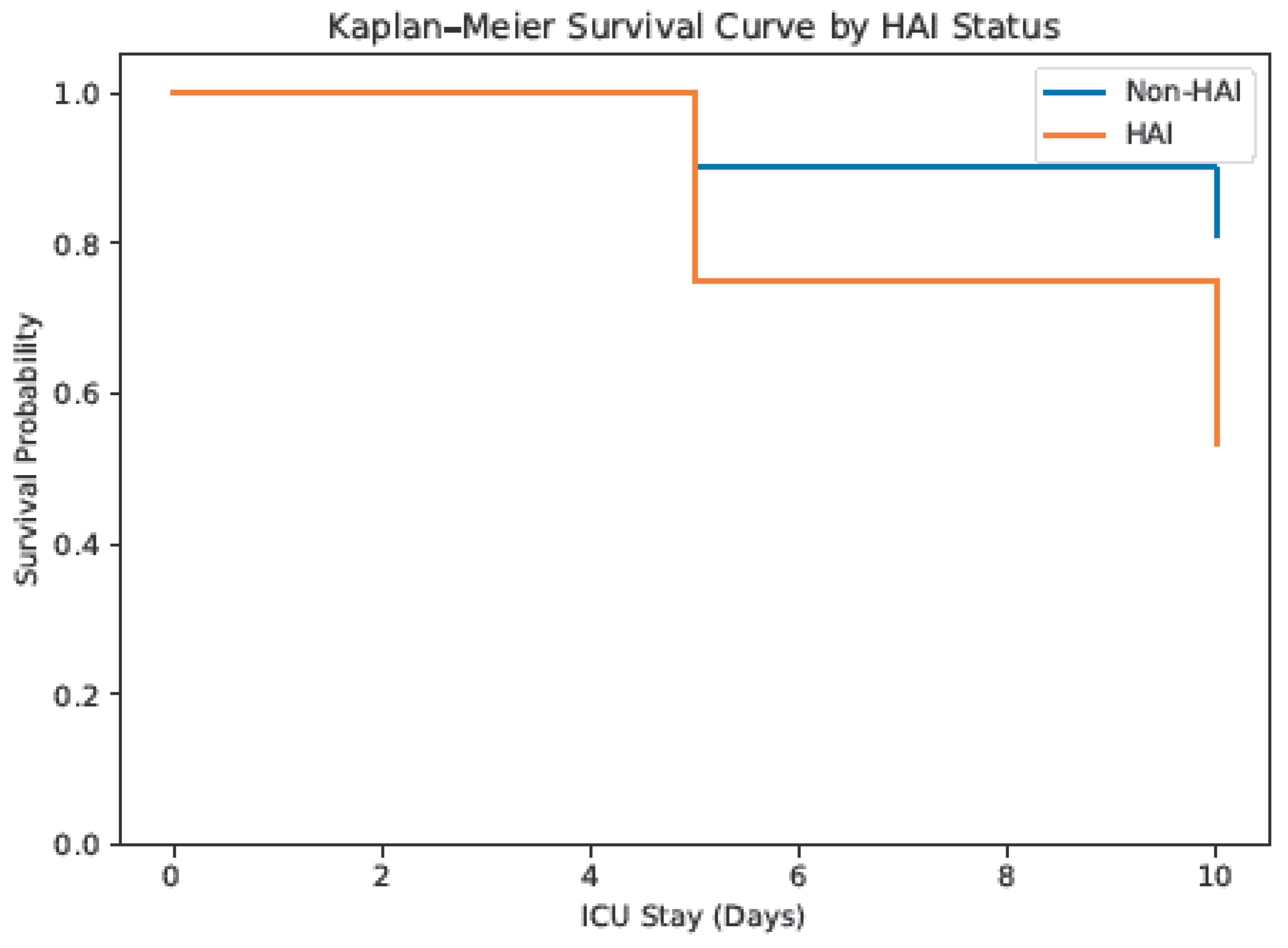
4. Discussion
4.1. Interpretation in the Context of Previous Evidence
4.2. Clinical Outcomes and Broader Implications
- Implementation of device-care bundles for VAP, CAUTI, and CLABSI, with daily device assessment and prompt removal when clinically feasible.
- Continuous surveillance and feedback mechanisms using standardised definitions.
- Structured IPC training programs, including paediatric- and neonatal-specific modules.
- Strengthened antimicrobial stewardship programs, integrated into routine ICU practice.
- Policy-level investment in IPC supplies, staffing, and laboratory capacity.
4.3. Limitations and Future Research
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| HAIs | Healthcare-associated infections |
| ICU | intensive care unit |
| LMIC | low- and middle-income countries |
| IPC | Infection prevention and control |
| WHO | World Health Organisation |
| VAP | ventilator-associated pneumonia |
| CLABSI | central line-associated bloodstream infection |
| CAUTI | catheter-associated urinary tract infection |
| AMR | antimicrobial resistance |
| CLSI | Clinical and Laboratory Standards Institute |
| SD | standard deviation |
| IQR | interquartile ranges |
| aOR | Adjusted odds ratios |
| SSI | Surgical site infections |
References
- World Health Organization. Global Report on the Burden of Endemic Health Care-Associated Infection Worldwide; WHO: Geneva, 2022. [Google Scholar]
- Centers for Disease Control and Prevention. National and State Healthcare-Associated Infections Progress Report; CDC: Atlanta, 2023. [Google Scholar]
- Adal, O; Tsehay, YT; Ayenew, B; et al. The burden and predictors of hospital-acquired infection in intensive care units across sub-Sahara Africa: systematic review and meta-analysis. BMC Infect Dis. 2025, 25, 634. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Global Antibiotic Resistance Surveillance Report 2025; WHO: Geneva, 2025. [Google Scholar]
- Dramowski, A; Whitelaw, A; et al. Healthcare-associated infections in South Africa: prevalence and implications. S Afr Med J. 2024; Published online ahead of print. [Google Scholar]
- Muhindo, R; et al. Healthcare-associated infections in Sub-Saharan African ICUs: a systematic review. BMC Infect Dis. 2025, 25, 38. [Google Scholar]
- Chigangaidze, R; et al. ICU-acquired infections among neonates and infants in resource-limited settings. BMC Infect Dis. 2025, 25, 110. [Google Scholar]
- European Centre for Disease Prevention and Control. Point prevalence survey of healthcare-associated infections in European acute care hospitals. 2023. [Google Scholar]
- Silva, E; et al. Device-associated infections in Brazilian ICUs: incidence and mortality. Crit Care 2025, 29, 203. [Google Scholar]
- Adegbite, BR; et al. Microbiological profile of ICU-acquired infections in African hospitals. One Health Bull. 2024, 12, 51–62. [Google Scholar]
- Dramowski, A; et al. Multidrug-resistant Gram-negative pathogens in African ICUs. BMC Infect Dis. 2022, 22, 387. [Google Scholar]
- Zingg, W; et al. Risk factors for ICU-acquired infections: a multicenter cohort study. Crit Care 2024, 28, 105. [Google Scholar]
- Rosenthal, VD; et al. Device-associated infection risk in pediatric and neonatal ICUs. BMC Infect Dis. 2022, 22, 122. [Google Scholar]
- Ghosh, R; et al. Effectiveness of infection prevention and control bundles in ICUs. RDS J. 2024, 5, 1783–1795. [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




