Submitted:
27 February 2026
Posted:
02 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
- Development of V-ARC, a vasopressor adaptive resuscitation controller specifically designed for hemorrhagic shock trauma scenarios rather than surgical support applications
- Systematic comparison of traditional and custom control architectures for vasopressor management on a hardware-in-loop testbed
- Identification of best performing controller logic for managing fluid non-responsiveness in a hardware-in-loop simulation
2. Materials and Methods
2.1. Overview of Animal Study
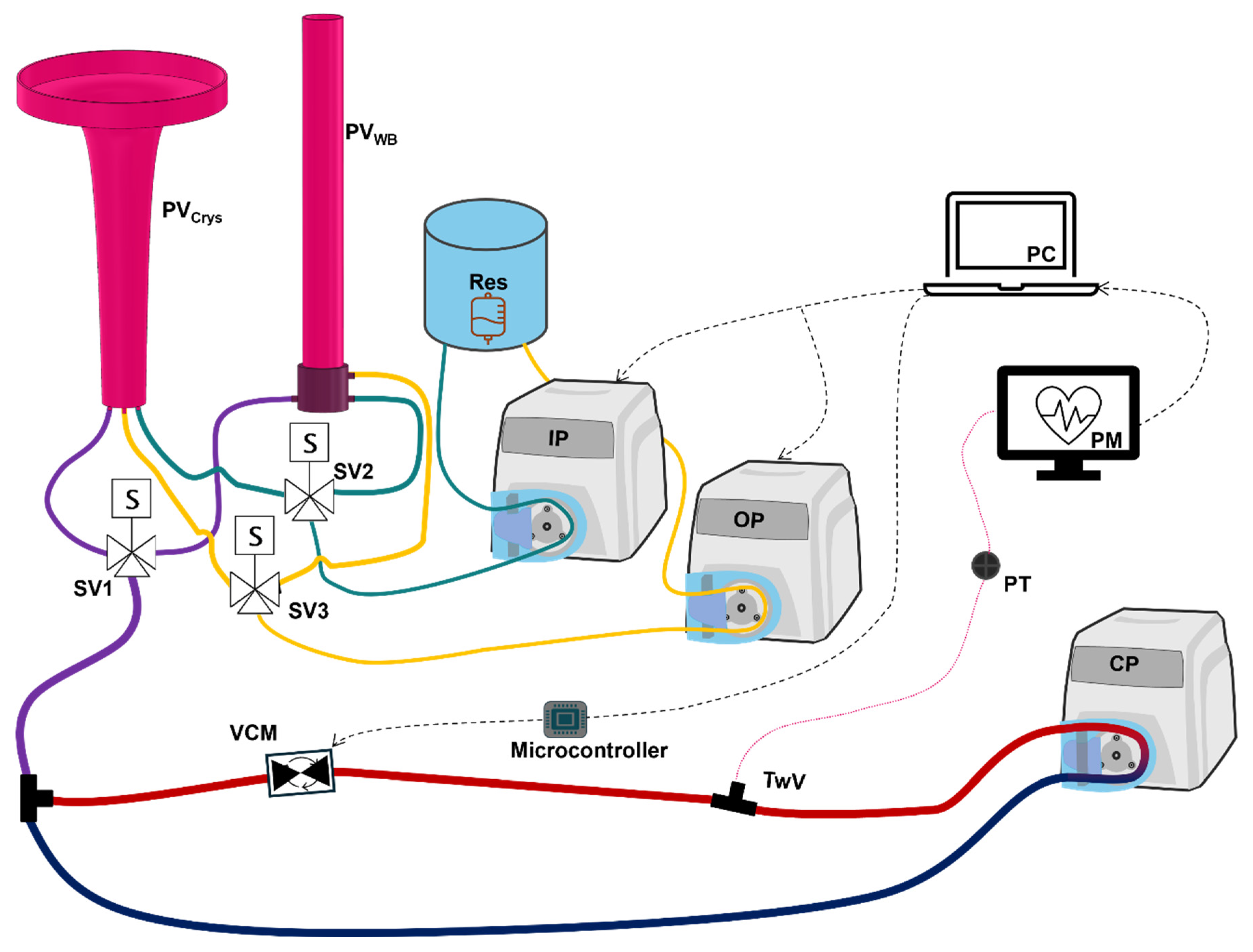
2.2. Overview of V-ARC Test Platform
2.3. Physiological Closed Loop Controller Development
2.3.1. Proportional-Integral-Derivative Controller
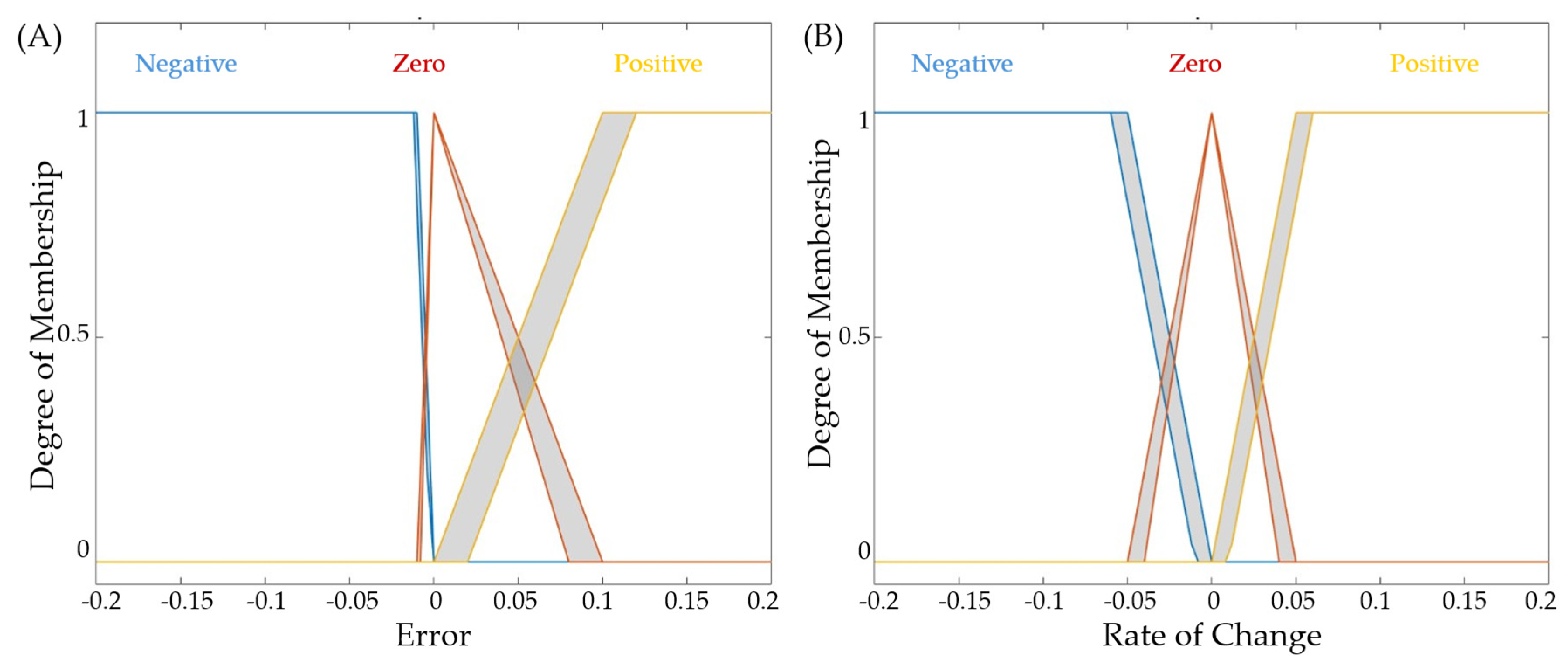
2.3.2. Step Fuzzy Inference System
- Negative – a linear Z-shaped function capturing negative deviations,
- Zero – a triangular function centered around the target condition
- Positive – a linear S-shaped function representing positive deviations.
2.3.3. Adaptive Neural Fuzzy Inference System
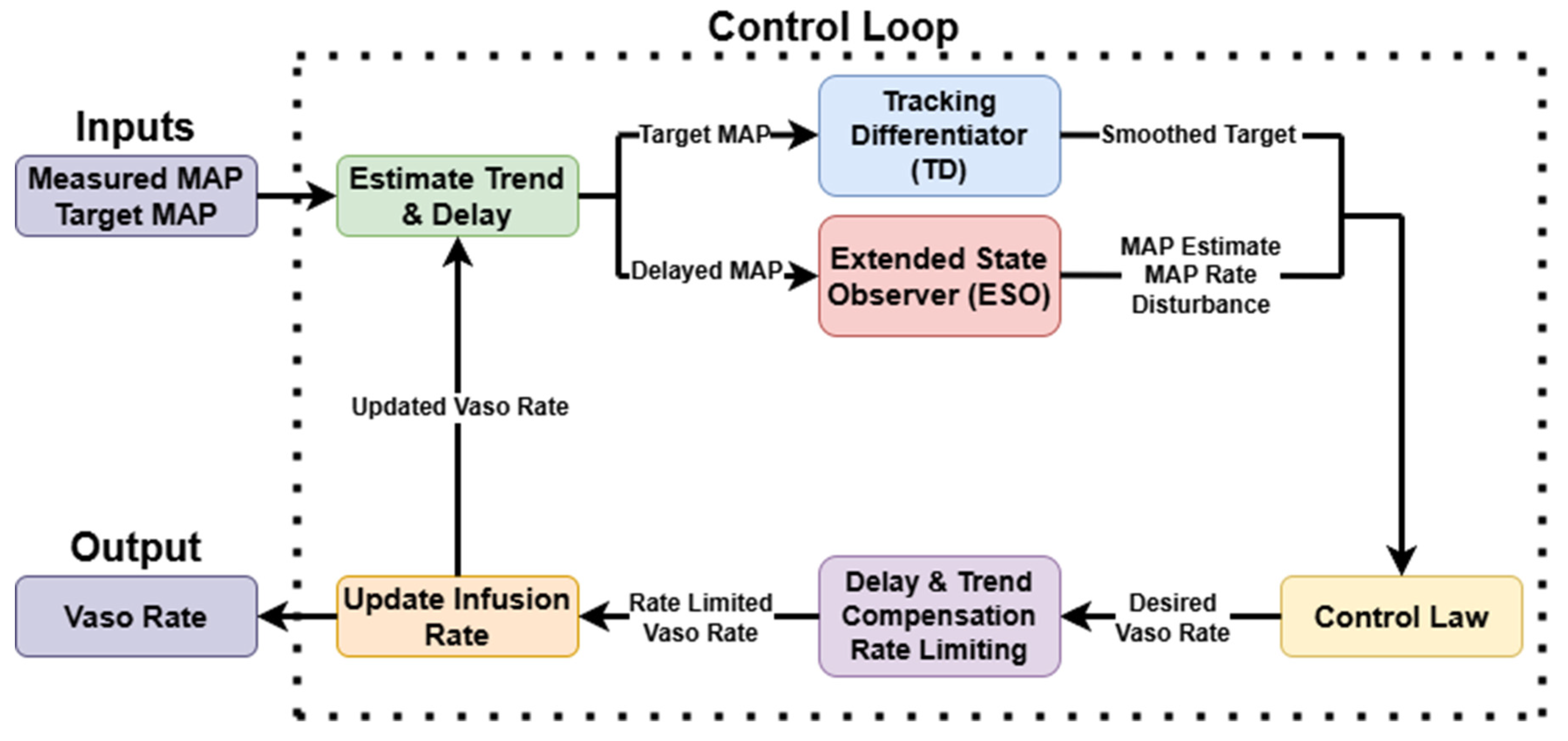
2.3.4. Active Disturbance Rejection Control
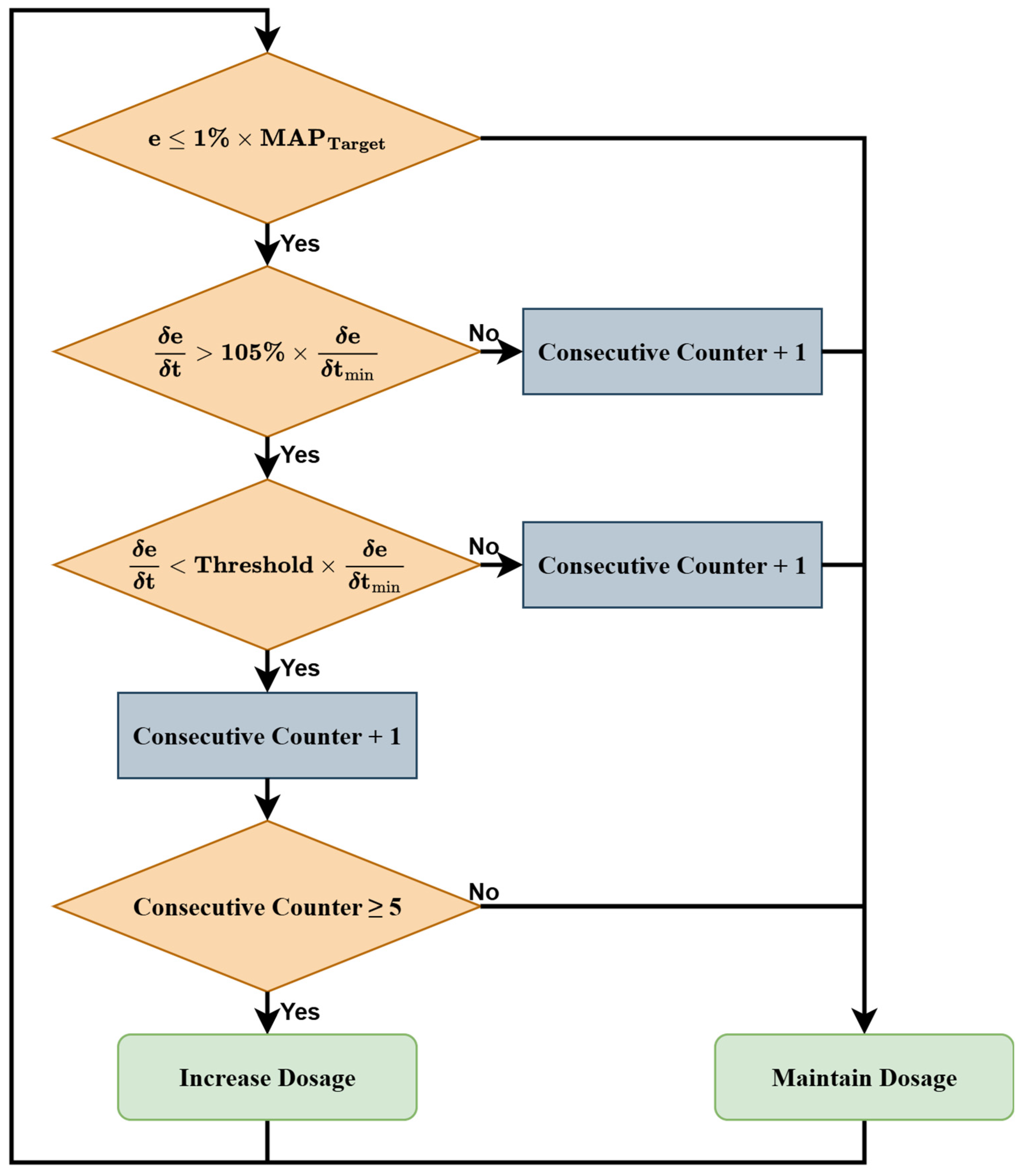
2.3.5. Patient-Following Controller
2.4. Controller Evaluation Using Hardware in Loop Test Platform
2.5. Controller Comparison Data Analyses
3. Results
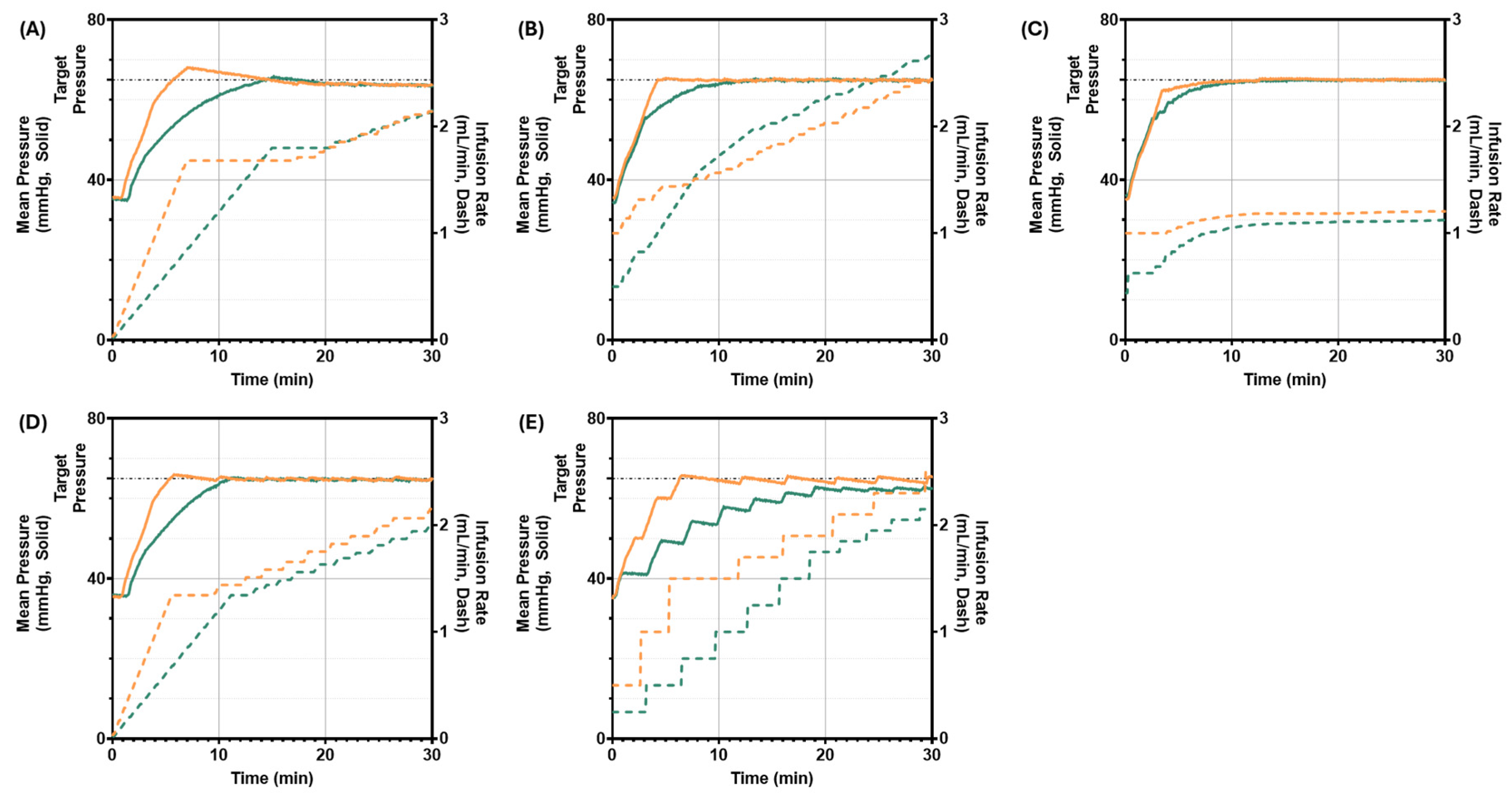
3.1. Scenario 1: Starting Pressure 35 mmHg
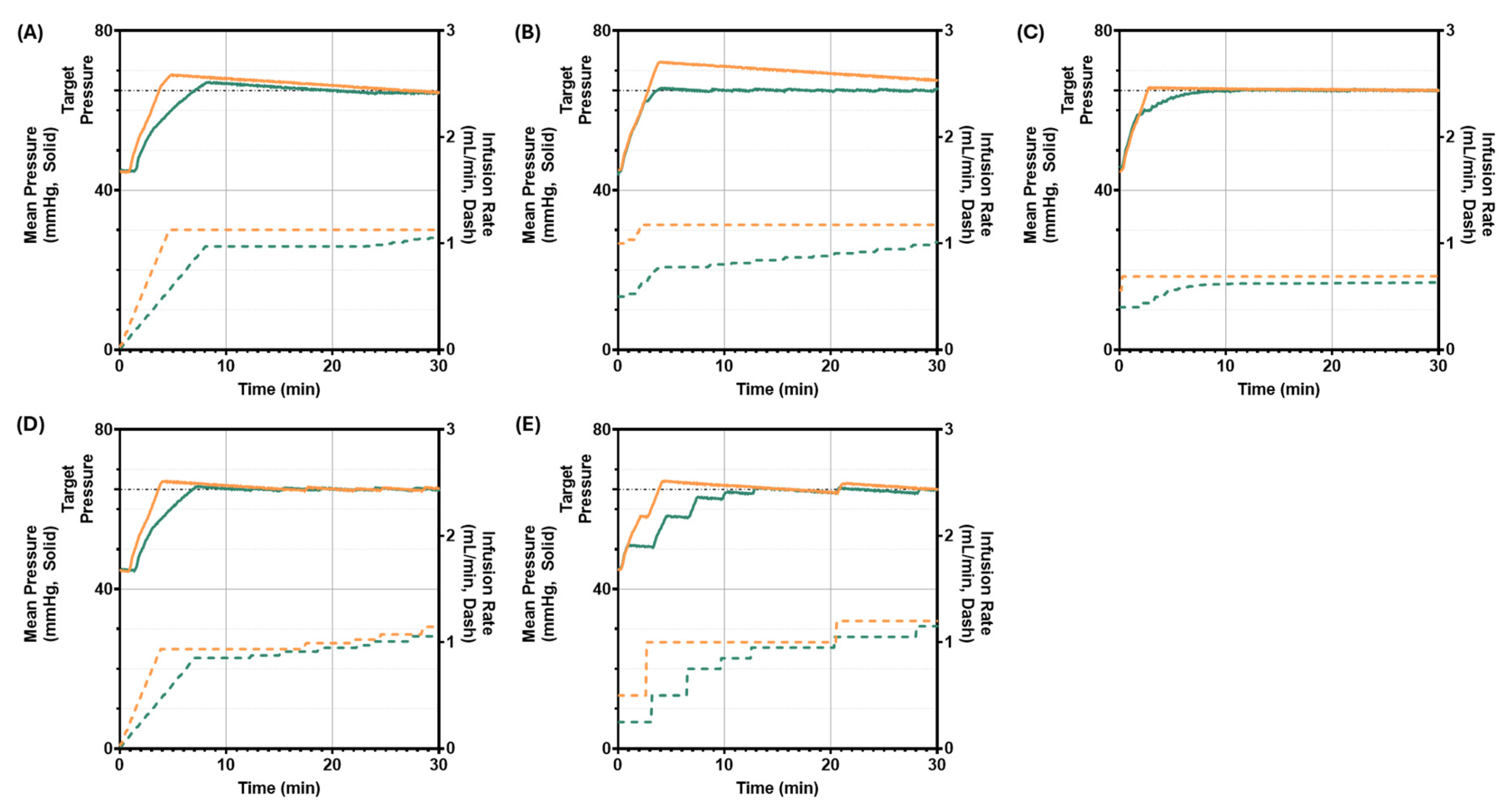
3.2. Scenario 2: Starting Pressure 45 mmHg
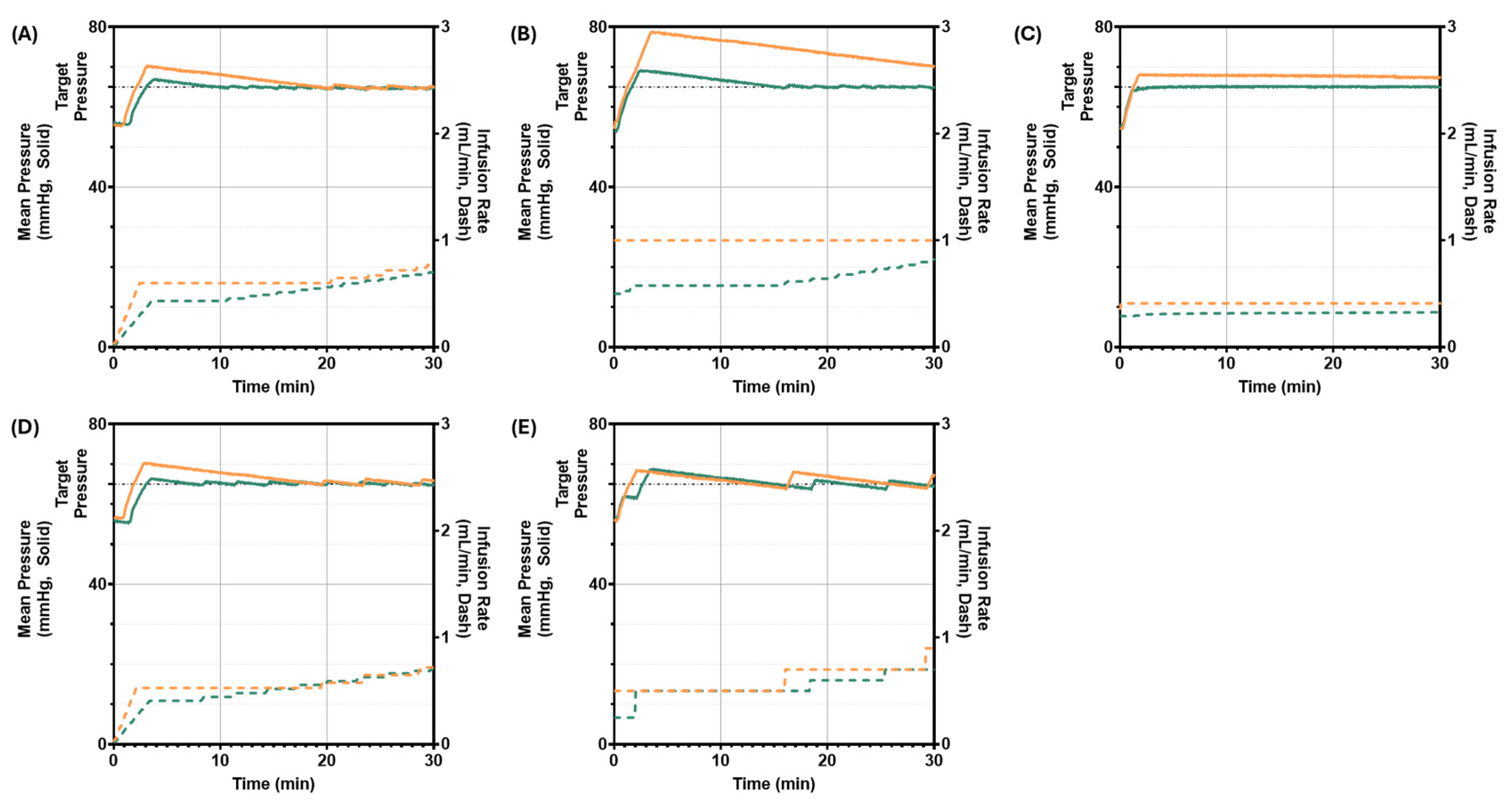
3.3. Scenario 3: Starting Pressure 55 mmHg
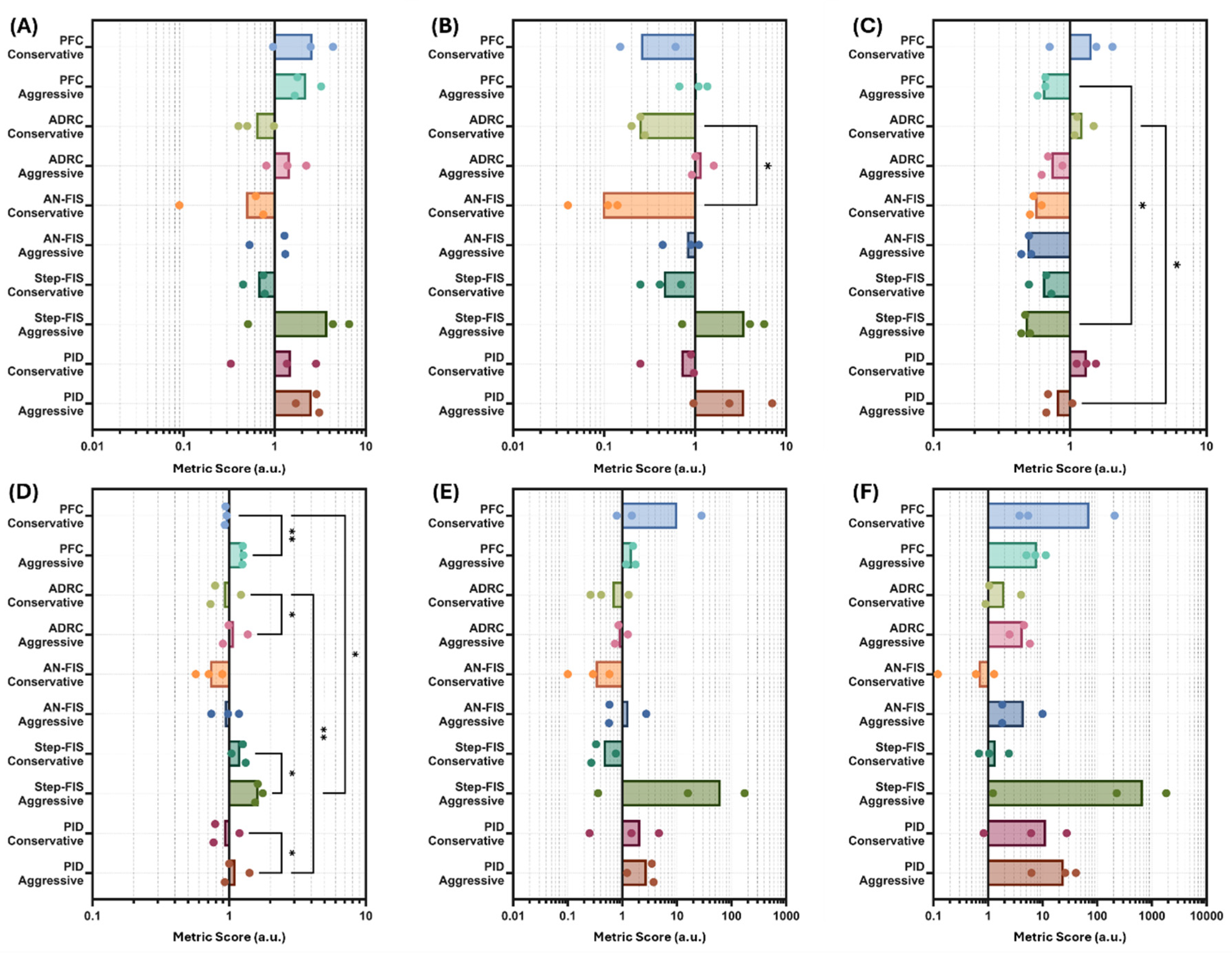
3.4. Overall Vasopressor PCLC Performance
4. Discussion
5. Conclusions
Author Contributions
Funding
Data Availability Statement
Regulatory Statement
Acknowledgments
DOD Disclaimer
Abbreviations
| AAALAC | Association for Assessment and Accreditation of Laboratory Animal Care International |
| AN-FIS | Adaptive Neural Inference System |
| ADRC | Active Disturbance Rejection Control |
| ANOVA | Analysis of Variance |
| ARC | Adaptive Resuscitation Controller |
| AreaAbove | Area Above Target Pressure |
| AreaBelow | Area Below Target Pressure |
| ESO | Extended State Observer |
| HATRC | Hardware-in-Loop Testbed for Resuscitation Controllers |
| IACUC | Institutional Animal Care and Use Committee |
| IMC | Internal Model Controller |
| LPV | Linear Parameter Varying |
| MAP | Mean Arterial Pressure |
| MaxRateChange | Maximum Infusion Rate Change |
| MDAPE | Median Absolute Performance Error |
| MDAPESS | Median Absolute Performance at Steady-State |
| MDPE | Median Performance Error |
| MeanInf | Mean Vasopressor Infusion Rate |
| MMEKF | Multiple-Model Extended Kalman Filter |
| NE | Norepinephrine |
| PCLC | Physiological Closed-Loop Controller |
| PFC | Patient-Following Controller |
References
- Baykuziyev, T.; Khan, M. J.; Karmakar, A.; Baloch, M. A. Closed-loop pharmacologic control of blood pressure: A review of existing systems. Cureus 2023, 15(9). [Google Scholar] [CrossRef]
- Brogi, E.; Cyr, S.; Kazan, R.; Giunta, F.; Hemmerling, T. M. Clinical performance and safety of closed-loop systems: A systematic review and meta-analysis of randomized controlled trials. Anesth. Analg. 2017, 124(2), 446–455. [Google Scholar] [CrossRef] [PubMed]
- Schaffer, C.; Goldart, E.; Ligsay, A.; Mazwi, M.; Gallant, S.; Ehrmann, D. Take a load off: Understanding, measuring, and reducing cognitive load for cardiologists in high-stakes care environments. Curr. Treat. Options Pediatr. 2023, 9(3), 122–135. [Google Scholar] [CrossRef]
- von Platen, P.; Pomprapa, A.; Lachmann, B.; Leonhardt, S. The dawn of physiological closed-loop ventilation—A review. Crit. Care 2020, 24, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Pasha, S.; Babar, E. T. R.; Schneider, J.; Heithaus, J.; Mujeeb-U-Rahman, M. “A Low-cost, Automated, Portable Mechanical Ventilator for Developing World,” in 2021 IEEE Global Humanitarian Technology Conference (GHTC); IEEE, 2021; pp. 112–118. [Google Scholar] [CrossRef]
- Snider, E. J.; et al. In Vivo Evaluation of an Adaptive Resuscitation Controller Using Whole Blood and Crystalloid Infusates for Hemorrhagic Shock. Front. Bioeng. Biotechnol. 2024, 12, 1420330. [Google Scholar] [CrossRef]
- Vega, S. J.; Berard, D.; Avital, G.; Ross, E.; Snider, E. J. Adaptive closed-loop resuscitation controllers for hemorrhagic shock resuscitation. Transfusion (Paris) 2023, 63(S3), S230–S240. [Google Scholar] [CrossRef]
- Russell, J. A. Vasopressor therapy in critically ill patients with shock. Intensive Care Med. 2019, 45, 1503–1517. [Google Scholar] [CrossRef]
- Bauer, S. R.; Gellatly, R. M.; Erstad, B. L. Precision fluid and vasoactive drug therapy for critically ill patients. Pharmacother. J. Hum. Pharmacol. Drug Ther. 2023, 43(11), 1182–1193. [Google Scholar] [CrossRef]
- De Backer, D.; et al. Comparison of dopamine and norepinephrine in the treatment of shock. N. Engl. J. Med. 2010, 362(9), 779–789. [Google Scholar] [CrossRef]
- Sviri, S.; Hashoul, J.; Stav, I.; Van Heerden, P. V. Does high-dose vasopressor therapy in medical intensive care patients indicate what we already suspect? J. Crit. Care 2014, 29(1), 157–160. [Google Scholar] [CrossRef]
- Padmanaban, A.; Venkataraman, R.; Rajagopal, S.; Devaprasad, D.; Ramakrishnan, N. Feasibility and safety of peripheral intravenous administration of vasopressor agents in resource-limited settings. J. Crit. Care Med. 2020, 6(4), 210. [Google Scholar] [CrossRef] [PubMed]
- Rinehart, J.; Ma, M.; Calderon, M.-D.; Cannesson, M. Feasibility of automated titration of vasopressor infusions using a novel closed-loop controller. J. Clin. Monit. Comput. 2018, 32, 5–11. [Google Scholar] [CrossRef] [PubMed]
- Khan, M. N.; Grigoriadis, K. M.; Kramer, G. C.; Franchek, M. A. AUTOMATIC CONTROL OF MEAN ARTERIAL PRESSURE DURING TRAUMA RESUSCITATION USING CLOSED-LOOP VASOPRESSOR THERAPY. System 30(20), 50.
- Luspay, T.; Grigoriadis, K. Robust linear parameter-varying control of blood pressure using vasoactive drugs. Int. J. Control 2015, 88(10), 2013–2029. [Google Scholar] [CrossRef]
- Merouani, M.; et al. Norepinephrine weaning in septic shock patients by closed loop control based on fuzzy logic. Crit. Care 2008, 12, 1–8. [Google Scholar] [CrossRef]
- D. Berard et al., “Vasopressor Control Module Development and Integration into the Hardware-in-Loop Automated Testbed for Resuscitation Controller Evaluation,” Oct. 29, 2025, Research Square. [CrossRef]
- Snider, E. J.; Berard, D.; Vega, S. J.; Hernandez Torres, S. I.; Avital, G.; Boice, E. N. An Automated Hardware-in-Loop Testbed for Evaluating Hemorrhagic Shock Resuscitation Controllers. Bioengineering 2022, 9(8), 373. [Google Scholar] [CrossRef]
- Rodgers, T. M.; et al. In Vivo Evaluation of Two Hemorrhagic Shock Resuscitation Controllers with Non-Invasive, Intermittent Sensors. Bioengineering 2024, 11(12), 1296. [Google Scholar] [CrossRef]
- Beloncle, F.; Meziani, F.; Lerolle, N.; Radermacher, P.; Asfar, P. Does vasopressor therapy have an indication in hemorrhagic shock? Ann. Intensive Care 2013, 3(1), 13. [Google Scholar] [CrossRef]
- Bray, A.; et al. Pulse Physiology Engine: An Open-Source Software Platform for Computational Modeling of Human Medical Simulation. SN Compr. Clin. Med. 2019, 1(5), 362–377. [Google Scholar] [CrossRef]
- Jang, J.-S. ANFIS: Adaptive-network-based fuzzy inference system. IEEE Trans. Syst. Man Cybern. 1993, 23(3), 665–685. [Google Scholar] [CrossRef]
- Basar, G.; Der, O.; Guvenc, M. A. AI-powered hybrid metaheuristic optimization for predicting surface roughness and kerf width in CO2 laser cutting of 3D-printed PLA-CF composites. J. Thermoplast. Compos. Mater. 2025, 38(7), 2688–2717. [Google Scholar] [CrossRef]
- Islam, M. A.; et al. Modeling and performance evaluation of ANFIS controller-based bidirectional power management scheme in plug-in electric vehicles integrated with electric grid. IEEE Access 2021, 9, 166762–166780. [Google Scholar] [CrossRef]
- Jumani, T. A.; et al. Computational Intelligence-Based Optimization Methods for Power Quality and Dynamic Response Enhancement of ac Microgrids. Energies 2020, 13(16). [Google Scholar] [CrossRef]
- Han, J. From PID to active disturbance rejection control. IEEE Trans. Ind. Electron. 2009, 56(3), 900–906. [Google Scholar] [CrossRef]
- Libert, N.; et al. Performance of closed-loop resuscitation of haemorrhagic shock with fluid alone or in combination with norepinephrine: An experimental study. Ann. Intensive Care 2018, 8(1), 89. [Google Scholar] [CrossRef]
- Libert, N.; et al. Performance of closed-loop resuscitation in a pig model of haemorrhagic shock with fluid alone or in combination with norepinephrine, a pilot study. J. Clin. Monit. Comput. 2021, 35(4), 835–847. [Google Scholar] [CrossRef]
- Varvel, J. R.; Donoho, D. L.; Shafer, S. L. Measuring the predictive performance of computer-controlled infusion pumps. J. Pharmacokinet. Biopharm. 1992, 20, 63–94. [Google Scholar] [CrossRef]
- Mirinejad, H.; et al. Evaluation of fluid resuscitation control algorithms via a hardware-in-the-loop test bed. IEEE Trans. Biomed. Eng. 2019, 67(2), 471–481. [Google Scholar] [CrossRef]
- Berard, D.; Vega, S. J.; Avital, G.; Snider, E. J. Dual input fuzzy logic controllers for closed loop hemorrhagic shock resuscitation. Processes 2022, 10(11), 2301. [Google Scholar] [CrossRef]
- Master, T.; Mark, T. Medical electrical equipment Part 1: General requirements for basic safety and essential performance. 2012. [Google Scholar]
- Marques, N. R. Automated closed-loop resuscitation of multiple hemorrhages: A comparison between fuzzy logic and decision table controllers in a sheep model. Disaster Mil. Med. 2017, 3, 1–10. [Google Scholar] [CrossRef]
- Snider, E. J.; Berard, D.; Vega, S. J.; Avital, G.; Boice, E. N. Evaluation of a proportional–integral–derivative controller for hemorrhage resuscitation using a hardware-in-loop test platform. J. Pers. Med. 2022, 12(6), 979. [Google Scholar] [CrossRef] [PubMed]
- SHAPIRO, S. S.; WILK, M. B. An analysis of variance test for normality (complete samples)†. Biometrika 1965, 52(3–4), 591–611. [Google Scholar] [CrossRef]
- Tukey, J. W. Comparing individual means in the analysis of variance. Biometrics 1949, 99–114. [Google Scholar] [CrossRef]
- Friedman, M. The use of ranks to avoid the assumption of normality implicit in the analysis of variance. J. Am. Stat. Assoc. 1937, 32(200), 675–701. [Google Scholar] [CrossRef]
- Dunn, O. J. Multiple comparisons using rank sums. Technometrics 1964, 6(3), 241–252. [Google Scholar] [CrossRef]
- Fage, N.; Asfar, P.; Radermacher, P.; Demiselle, J. Norepinephrine and Vasopressin in Hemorrhagic Shock: A Focus on Renal Hemodynamics. Int. J. Mol. Sci. 2023, 24(4), 4. [Google Scholar] [CrossRef]
- Smith, J. B.; Pittet, J.-F.; Pierce, A. Hypotensive Resuscitation. Curr. Anesthesiol. Rep. 2014, 4(3), 209–215. [Google Scholar] [CrossRef]
- T. Kowalenko, S. Stern, S. Dronen, and X. Wang, “Improved outcome with hypotensive resuscitation of uncontrolled hemorrhagic shock in a swine model,” J. Trauma, vol. 33, no. 3, pp. 349–353; discussion 361-362, Sep. 1992.
- Chalkias, A. Shear Stress and Endothelial Mechanotransduction in Trauma Patients with Hemorrhagic Shock: Hidden Coagulopathy Pathways and Novel Therapeutic Strategies. Int. J. Mol. Sci. 2023, 24(24), 17522. [Google Scholar] [CrossRef]
- Beloncle, F.; Meziani, F.; Lerolle, N.; Radermacher, P.; Asfar, P. Does vasopressor therapy have an indication in hemorrhagic shock? Ann. Intensive Care 2013, 3(1), 13. [Google Scholar] [CrossRef]
- Fage, N.; Asfar, P.; Radermacher, P.; Demiselle, J. Norepinephrine and Vasopressin in Hemorrhagic Shock: A Focus on Renal Hemodynamics. Int. J. Mol. Sci. 2023, 24(4), 4103. [Google Scholar] [CrossRef]
- Gutierrez, G.; Reines, H. D.; Wulf-Gutierrez, M. E. Clinical review: Hemorrhagic shock. Crit. Care Lond. Engl. 2004, 8(5), 373–381. [Google Scholar] [CrossRef]
| Step | Norepinephrine Dose (mcg/min) | Norepinephrine Rate (mL/min) |
|---|---|---|
| 1 | 0.5 | 0.13 |
| 2 | 1 | 0.25 |
| 3 | 2 | 0.5 |
| 4 | 4 | 1 |
| 5 | 8 | 2 |
| 6 | 12 | 3 |
| 7 | 16 | 4 |
| 8 | 20 | 5 |
| Performance Metrics | Description | Reference |
|---|---|---|
| Median Performance Error (MDPE, %) | Median value of the performance errors vs. target pressure |
[29,30] |
| Median Absolute Performance Error (MDAPE, %) | Median of the absolute value of performance errors vs. target pressure | [29] |
| MDAPE at Steady State (MDAPESS, %) | MDAPE values once the controller has reached steady-state | [31] |
| Target Overshoot (%) | Percent by how much the target was maximally overshot | [32] |
| Effectiveness (%) | Percentage of the time the controller was within +/- 5 mmHg of the target | [33] |
| Wobble (%) | Measurement of the dispersion of performance errors, relative to MDPE | [29,30] |
| Divergence (%/hr) | Measurement of the trend of MDAPE over the final 10% of the scenario | [30] |
| Rise-Time Efficiency (min) | Time for the controller to initially be within 90% of target MAP | [32] |
| Mean Infusion Rate (MeanInf, mL/min) | Average of the infusion rates used during the scenario | [18] |
| Area Above Target Pressure (AreaAbove, min) | Quantifies over-resuscitation using cumulative area of the time spent above target MAP during scenario | [18] |
| Area Below Target Pressure (AreaBelow, min) | Quantifies under-resuscitation using cumulative area of the time spent below target MAP (after reaching target for the first time) during scenario | [18] |
| Maximum Infusion Rate Change (MaxRateChange, mL/min/min) | Quantifies the maximum timeof change of the infusion rate across the test using a 3-minute moving average window | N/A |
| Variable Infusion Rate (VarInfRate, mL/min) | Standard deviation of a 2-minute window of infusion rates relative to mean infusion rate | [34] |
| PID | Step-FIS | AN-FIS | ADRC | PFC | |||||||
| Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | ||
| Performance Metrics | MDPE (%) | -1.53 | -2.07 | -0.12 | -0.38 | -0.13 | -0.31 | -0.29 | -0.61 | -0.85 | -8.36 |
| MDAPE (%) | 1.90 | 2.07 | 0.20 | 0.39 | 0.33 | 0.31 | 0.47 | 0.61 | 0.94 | 8.36 | |
| MDAPESS (%) | 1.77 | 1.73 | 0.17 | 0.25 | 0.27 | 0.21 | 0.35 | 0.46 | 0.70 | 4.31 | |
| Target Overshoot (%) | 4.74 | 1.26 | 0.65 | 0.44 | 0.60 | 0.21 | 1.53 | 0.39 | 1.23 | 0.00 | |
| Effectiveness (%) | 86.35 | 69.64 | 88.58 | 81.62 | 89.42 | 84.95 | 86.64 | 74.10 | 85.23 | 46.79 | |
| Wobble (%) | 0.87 | 0.43 | 0.17 | 0.25 | 0.27 | 0.20 | 0.32 | 0.21 | 0.66 | 0.48 | |
| Divergence (%/hr) | 3.86 | 5.69 | -1.12 | 1.87 | -0.04 | 1.36 | 9.76 | -2.27 | 11.79 | -1.60 | |
| Rise-Time Efficiency (min) | 3.75 | 8.10 | 3.25 | 4.51 | 3.00 | 3.92 | 3.76 | 7.10 | 3.92 | 13.10 | |
| MeanInf (ml/min) | 1.59 | 1.41 | 1.80 | 1.87 | 1.15 | 1.01 | 1.51 | 1.28 | 1.68 | 1.26 | |
| AreaAbove (min) | 0.22 | 0.01 | 0.02 | 0.01 | 0.03 | 0.00 | 0.04 | 0.00 | 0.03 | 0.00 | |
| AreaBelow (min) | -1.50 | -2.69 | -1.00 | -1.47 | -1.05 | -1.24 | -1.30 | -2.23 | -1.38 | -4.01 | |
| MaxRateChange (mL/min2) | 0.0041 | 0.0020 | 0.0182 | 0.0094 | 0.0167 | 0.01 | 0.0041 | 0.0020 | 0.0083 | 0.0042 | |
| VarInfRate (mL/min) | 0.0448 | 0.0432 | 0.0299 | 0.0427 | 0.0040 | 0.0200 | 0.0431 | 0.0422 | 0.0546 | 0.0542 | |
| PID | Step-FIS | AN-FIS | ADRC | PFC | |||||||
| Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | ||
| Performance Metrics | MDPE (%) | 2.25 | -0.53 | 7.02 | 0.07 | 0.42 | -0.03 | 0.28 | -0.04 | 0.79 | -1.08 |
| MDAPE (%) | 3.16 | 1.16 | 7.60 | 0.23 | 0.50 | 0.25 | 0.62 | 0.32 | 1.32 | 1.08 | |
| MDAPESS (%) | 2.63 | 0.94 | 7.42 | 0.20 | 0.46 | 0.21 | 0.47 | 0.24 | 1.13 | 0.63 | |
| Target Overshoot (%) | 6.15 | 3.21 | 11.05 | 0.97 | 1.19 | 0.51 | 3.14 | 1.19 | 3.24 | 0.75 | |
| Effectiveness (%) | 89.97 | 83.84 | 50.97 | 92.75 | 93.32 | 91.36 | 89.97 | 83.84 | 89.69 | 76.60 | |
| Wobble (%) | 1.72 | 1.11 | 1.78 | 0.20 | 0.23 | 0.20 | 0.50 | 0.24 | 0.86 | 0.58 | |
| Divergence (%/hr) | 13.30 | 2.58 | -17.15 | 2.62 | -1.01 | -0.17 | 7.09 | -5.12 | -13.47 | -31.31 | |
| Rise-Time Efficiency (min) | 2.75 | 4.34 | 2.00 | 2.00 | 1.84 | 1.67 | 2.75 | 4.26 | 2.92 | 6.76 | |
| MeanInf (ml/min) | 1.04 | 0.85 | 1.17 | 0.83 | 0.69 | 0.59 | 0.92 | 0.82 | 1.02 | 0.83 | |
| AreaAbove (min) | 0.71 | 0.20 | 2.00 | 0.05 | 0.13 | 0.03 | 0.21 | 0.05 | 0.30 | 0.01 | |
| AreaBelow (min) | -0.70 | -1.17 | -0.45 | -0.50 | -0.43 | -0.60 | -0.70 | -1.10 | -0.60 | -1.46 | |
| MaxRateChange (mL/min2) | 0.0041 | 0.0020 | 0.0171 | 0.0086 | 0.0108 | 0.01 | 0.0041 | 0.0020 | 0.0083 | 0.0042 | |
| VarInfRate (mL/min) | 0.0219 | 0.0208 | 0.0028 | 0.0115 | 0.0030 | 0.0044 | 0.0237 | 0.0222 | 0.0219 | 0.0238 | |
| PID | Step-FIS | AN-FIS | ADRC | PFC | |||||||
| Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | ||
| Performance Metrics | MDPE (%) | 1.04 | -0.18 | 14.13 | 0.33 | 4.33 | 0.09 | 1.59 | 0.21 | 1.58 | 0.55 |
| MDAPE (%) | 1.84 | 0.38 | 14.18 | 0.53 | 4.35 | 0.15 | 1.90 | 0.40 | 1.86 | 1.26 | |
| MDAPESS (%) | 1.38 | 0.33 | 11.00 | 0.40 | 4.34 | 0.15 | 1.71 | 0.37 | 1.78 | 1.16 | |
| Target Overshoot (%) | 8.04 | 3.00 | 21.23 | 6.34 | 4.80 | 0.36 | 8.14 | 2.08 | 5.23 | 5.76 | |
| Effectiveness (%) | 92.49 | 93.32 | 5.01 | 96.94 | 97.49 | 97.77 | 92.48 | 93.05 | 97.49 | 97.78 | |
| Wobble (%) | 1.77 | 0.29 | 1.48 | 0.56 | 0.23 | 0.13 | 1.54 | 0.35 | 1.63 | 1.33 | |
| Divergence (%/hr) | 0.76 | 3.46 | -28.51 | 0.89 | -2.73 | 0.06 | 35.47 | 2.18 | 34.16 | 1.92 | |
| Rise-Time Efficiency (min) | 1.17 | 1.75 | 0.50 | 0.75 | 0.58 | 0.58 | 1.09 | 1.75 | 0.50 | 0.50 | |
| MeanInf (ml/min) | 0.61 | 0.50 | 1.00 | 0.63 | 0.41 | 0.32 | 0.55 | 0.50 | 0.60 | 0.54 | |
| AreaAbove (min) | 0.71 | 0.10 | 4.09 | 0.47 | 1.22 | 0.03 | 0.77 | 0.11 | 0.54 | 0.39 | |
| AreaBelow (min) | -0.24 | -0.36 | -0.10 | -0.16 | -0.12 | -0.13 | -0.18 | -0.33 | -0.17 | -0.24 | |
| MaxRateChange (mL/min2) | 0.0041 | 0.0020 | 0.0167 | 0.0086 | 0.0065 | 0.00 | 0.0041 | 0.0020 | 0.0083 | 0.0048 | |
| VarInfRate (mL/min) | 0.0155 | 0.0154 | 0.0000 | 0.0070 | 0.0008 | 0.0008 | 0.0155 | 0.0160 | 0.0067 | 0.0057 | |
| PID | Step-FIS | AN-FIS | ADRC | PFC | |||||||
| Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | Agg. | Cons. | ||
| 35mmhg | Stable Term | 3.08 | 2.84 | 0.51 | 0.78 | 0.53 | 0.62 | 2.22 | 0.98 | 3.23 | 4.37 |
| Overshoot Term | 7.02 | 0.97 | 0.72 | 0.41 | 0.90 | 0.11 | 1.60 | 0.25 | 1.36 | 0.00 | |
| Undershoot Term | 0.67 | 1.32 | 0.51 | 0.73 | 0.50 | 0.62 | 0.62 | 1.13 | 0.66 | 2.05 | |
| Infusion Term | 0.93 | 0.77 | 1.62 | 1.26 | 1.18 | 0.89 | 0.90 | 0.73 | 1.25 | 0.93 | |
| Effectiveness Term | 3.47 | 4.68 | 0.36 | 0.76 | 0.58 | 0.58 | 0.85 | 1.30 | 1.75 | 28.21 | |
| Overall Score | 40.61 | 27.60 | 1.23 | 2.41 | 1.81 | 1.29 | 4.56 | 4.01 | 11.36 | 207.45 | |
| 45mmhg | Stable Term | 2.87 | 1.36 | 6.56 | 0.75 | 1.31 | 0.75 | 0.81 | 0.40 | 1.66 | 0.96 |
| Overshoot Term | 2.38 | 0.90 | 5.74 | 0.25 | 0.44 | 0.14 | 0.92 | 0.28 | 1.09 | 0.15 | |
| Undershoot Term | 0.69 | 1.12 | 0.47 | 0.50 | 0.44 | 0.51 | 0.69 | 1.08 | 0.66 | 1.56 | |
| Infusion Term | 1.00 | 0.79 | 1.55 | 1.04 | 0.98 | 0.71 | 0.99 | 0.79 | 1.26 | 0.96 | |
| Effectiveness Term | 3.73 | 1.47 | 15.85 | 0.27 | 0.57 | 0.29 | 0.73 | 0.41 | 1.57 | 1.49 | |
| Overall Score | 25.90 | 6.13 | 227.08 | 0.68 | 1.82 | 0.60 | 2.47 | 1.05 | 7.33 | 5.41 | |
| 55mmhg | Stable Term | 1.71 | 0.33 | 4.35 | 0.45 | 1.28 | 0.09 | 1.38 | 0.50 | 1.78 | 2.48 |
| Overshoot Term | 0.96 | 0.25 | 4.00 | 0.70 | 1.10 | 0.04 | 1.01 | 0.20 | 0.67 | 0.61 | |
| Undershoot Term | 1.04 | 1.55 | 0.44 | 0.67 | 0.52 | 0.54 | 0.88 | 1.49 | 0.58 | 0.71 | |
| Infusion Term | 1.41 | 1.19 | 1.76 | 1.32 | 0.74 | 0.57 | 1.37 | 1.22 | 1.27 | 0.94 | |
| Effectiveness Term | 1.22 | 0.25 | 173.65 | 0.33 | 2.74 | 0.10 | 1.26 | 0.26 | 1.17 | 0.79 | |
| Overall Score | 6.24 | 0.83 | 1833.27 | 1.05 | 9.96 | 0.12 | 5.84 | 0.90 | 5.04 | 3.75 | |
| Average | Stable Term | 2.55 | 1.51 | 3.81 | 0.66 | 1.04 | 0.49 | 1.47 | 0.63 | 2.22 | 2.60 |
| Overshoot Term | 3.45 | 0.71 | 3.49 | 0.45 | 0.81 | 0.10 | 1.17 | 0.24 | 1.04 | 0.25 | |
| Undershoot Term | 0.80 | 1.33 | 0.47 | 0.63 | 0.49 | 0.56 | 0.73 | 1.23 | 0.63 | 1.44 | |
| Infusion Term | 1.11 | 0.92 | 1.64 | 1.21 | 0.97 | 0.72 | 1.08 | 0.92 | 1.26 | 0.94 | |
| Effectiveness Term | 2.81 | 2.13 | 63.29 | 0.45 | 1.30 | 0.32 | 0.95 | 0.66 | 1.50 | 10.16 | |
| Overall Score | 24.25 | 11.52 | 687.19 | 1.38 | 4.53 | 0.67 | 4.29 | 1.99 | 7.91 | 72.21 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




