Submitted:
28 February 2026
Posted:
02 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. Epidemiology
3.2. Clinical Presentation
3.3. Assessment and Initial Management
3.4. Diagnostic Imaging
3.5. Operative Management
3.6. Infection Prophylaxis and Antibiotic Management
3.7. Rabies and Tetanus Management
3.8. Complications
4. Discussion
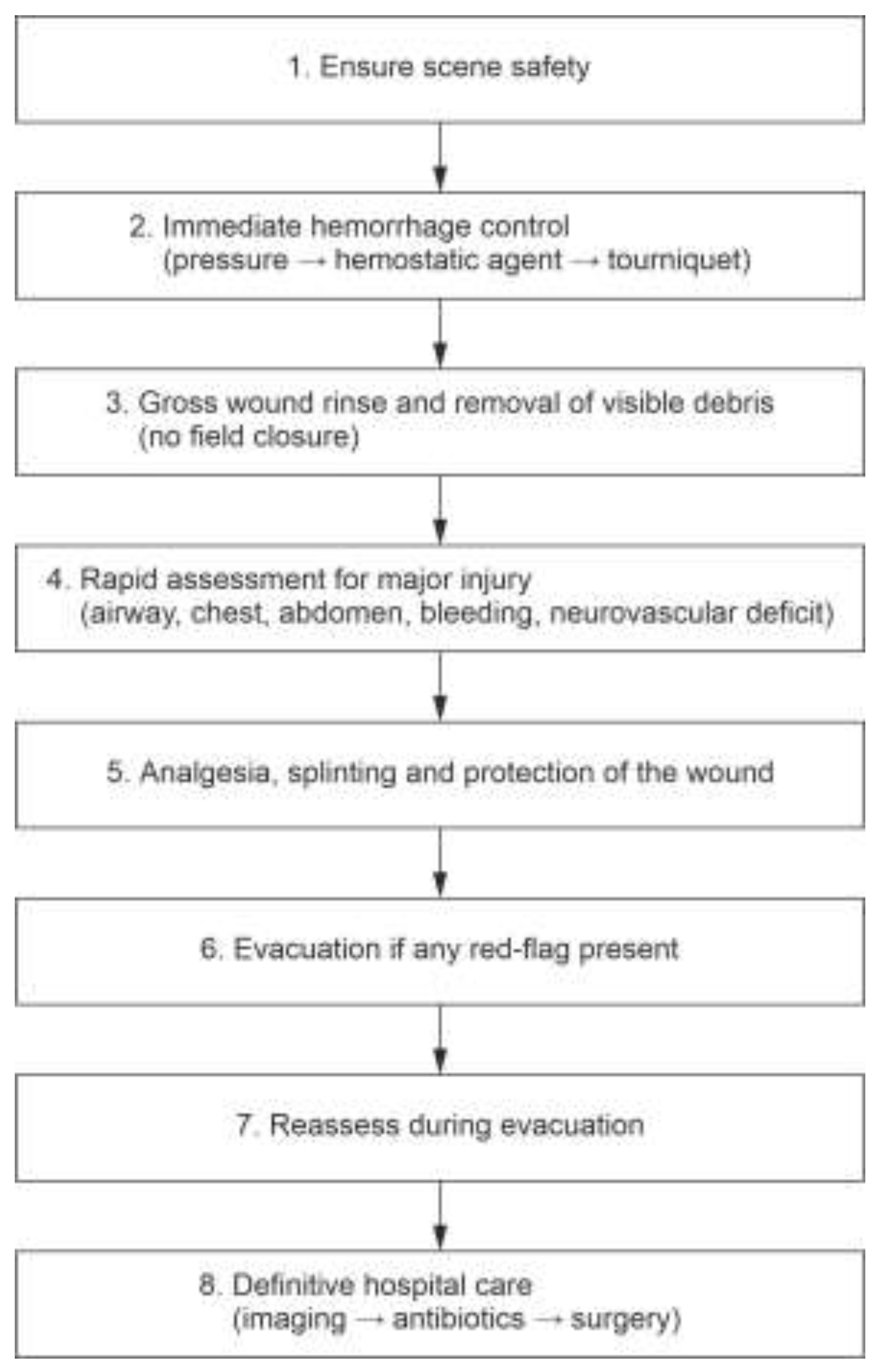
5. Recommendations / Management Guideline
6. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Massei, G.; Kindberg, J.; Licoppe, A.; Gačić, D.; Šprem, N.; Kamler, J.; Baubet, E.; Hohmann, U.; Monaco, A.; Ozoliņš, J.; Cellina, S.; Podgórski, T.; Fonseca, C.; Markov, N.; Pokorny, B.; Rosell, C.; Náhlik, A. Wild boar populations up, numbers of hunters down? A review of trends and implications for Europe. Pest Manag. Sci. 2015, 71(4), 492–500. [CrossRef]
- Kamieniarz, R.; Jankowiak, Ł.; Fratczak, M.; Panek, M.; Wojtczak, J.; Tryjanowski, P. The relationship between hunting methods and the sex, age and body mass of wild boar Sus scrofa. Animals 2020, 10(12), 2345. [CrossRef]
- Vajas, P.; Von Essen, E.; Tickle, L.; Gamelon, M. Meeting the challenges of wild boar hunting in a modern society: The case of France. Ambio 2023, 52(8), 1359–1372. [CrossRef]
- Pujol, O.; Nuño, M.; Minguell, J.; Selga, J.; Tomás, J.; Rodríguez, D.; Martínez, X.; Mentaberre, G.; López-Olvera, J.R. Characterization and treatment protocol of injuries inflicted to humans by synurbic European wild boars (Sus scrofa). Eur. J. Trauma Emerg. Surg. 2024, 50(5), 2595–2604. [CrossRef]
- Mayer, J.J. Wild pig attacks on humans. In Proceedings of the 15th Wildlife Damage Management Conference; Armstrong, J.B., Gallagher, G.R., Eds.; 2013; pp. 17–35.
- Mayer, J.J.; Garabedian, J.E.; Kilgo, J.C. Human fatalities resulting from wild pig attacks worldwide: 2000–2019. Hum. Wildl. Interact. 2023, 17(1), 3–20. [CrossRef]
- Gudmannsson, P.; Berge, J. The forensic pathology of fatal attacks by the large mammals inhabiting the nordic wilderness-a literature review. J. Forensic Sci. 2019, 64(4), 976–981. [CrossRef]
- Bury, D.; Langlois, N.; Byard, R.W. Animal-related fatalities--part I: characteristic autopsy findings and variable causes of death associated with blunt and sharp trauma. J. Forensic Sci. 2012, 57(2), 370–374. [CrossRef]
- Freer, L. North American wild mammalian injuries. Emerg. Med. Clin. N. Am. 2004, 22(2), 445–473. [CrossRef]
- Bury, D.; Langlois, N.; Byard, R.W. Animal-related fatalities--part II: characteristic autopsy findings and variable causes of death associated with envenomation, poisoning, anaphylaxis, asphyxiation, and sepsis. J. Forensic Sci. 2012, 57(2), 375–380. [CrossRef]
- Hauer, T.; Grobert, S.; Wenniges, H.; Huschitt, N.; Willy, C. Explosionstrauma Teil 1: Physikalische Grundlagen und Pathophysiologie [Explosion trauma part 1 : Physical principles and pathophysiology]. Unfallchirurg. 2022, 125(2), 145-159. German. [CrossRef]
- Hauer, T.; Grobert, S.; Gaab, J.; Huschitt, N.; Willy, C. Explosionstrauma Teil 2: Medizinische Behandlungsprinzipien [Blast injuries part 2 : Principles of medical treatment]. Unfallchirurg. 2022, 125(3), 227-242. German. [CrossRef]
- Davis, C.A.; Schmidt, A.C.; Sempsrott, J.R.; Hawkins, S.C.; Arastu, A.S.; Giesbrecht, G.G.; Cushing, T.A. Wilderness Medical Society clinical practice guidelines for the treatment and prevention of drowning: 2024 update. Wilderness Environ Med. 2024, 35(1_suppl), 94S-111S. [CrossRef]
- Davis, C.A.; Lowry, C.; Billin, A.; Laskowski-Jones, L.; Sheets, A.; Fifer, D.; Hawkins, S.C. Wilderness Medical Society clinical practice guidelines for medical direction of search and rescue teams. Wilderness Environ Med. 2024, 35(3), 314-327. [CrossRef]
- Maier, M.; Maier, L.P.N., Hackl., S.; Eckermann, N.J.; Maffulli, N.; Barapatre, N.; Schmitz, C. At times, hunters should beware. Trauma from wild boar encounters during hunting: a nationwide survey in Germany with a systematic literature review. Preprint. [CrossRef]
- Page, M.J.; McKenzie, J.E.; Bossuyt, P.M.; Boutron, I.; Hoffmann, T.C.; Mulrow, C.D.; Shamseer, L.; Tetzlaff, J.M.; Akl, E.A.; Brennan, S.E.; Chou, R.; Glanville, J.; Grimshaw, J.M.; Hróbjartsson, A.; Lalu, M.M.; Li, T.; Loder, E.W.; Mayo-Wilson, E.; McDonald, S.; McGuinness, L.A.; Stewart, L.A.; Thomas, J.; Tricco, A.C.; Welch, V.A.; Whiting, P.; Moher, D. The PRISMA 2020 statement: an updated guideline for reporting systematic reviews. BMJ 2021, 372, n71. [CrossRef]
- Ammann, L.M.; Barnum, M.; Cardin, S. Traumatic knee arthrotomy induced by wild boar tusk in a 15-year-old male: a case report. Wilderness Environ. Med. 2026, 37(1), 102–105. [CrossRef]
- Okamoto, N.; Nagasawa, H.; Miura, K.; Tanaka, N.; Maekawa, C.; Yanagawa, Y. Open digital fractures by boar bite. J. Emerg. Trauma Shock 2025, 18(3), 145–146. [CrossRef]
- Adhikari, J.N.; Bhattarai, B.P.; Thapa, T.B. Correlates and impacts of human-mammal conflict in the central part of Chitwan Annapurna Landscape, Nepal. Heliyon 2024, 10(4), e26386. [CrossRef]
- Iacoponi, N.; Bugelli, V.; Fico, R.; Giaconi, C.; Lorenzini, R.; Minervini, P.; Di Paolo, M. Boar hunt or Manhunt? fatality during a wild boar hunting expedition. Need for a multidisciplinary forensic approach. Leg. Med. 2024, 69, 102459. [CrossRef]
- Köroğlu, M.; Özdeş, H.U.; Acet, Ö.; Sarıbas, T.; Ergen, E.; Karakaplan, M.; Aslantürk, O. Common peroneal nerve injury caused by a wild boar attack. Wilderness Environ. Med. 2024, 35(1), 88–93. [CrossRef]
- Na, K.; Oh, B.H.; Lee, J.; Cho, M.J.; Lee, M.; Kim, H.R. Penetrating head injury resulting from wild boar attack in republic of korea: a case report. Korean J. Neurotrauma 2023, 19(4), 496–501. [CrossRef]
- Shimizu, Y.; Kubo, H. Foreign body in chest wall with traumatic pneumothorax caused by fang of wild boar. Kyobu Geka 2023, 76, 455–458. (In Japanese).
- Thalgaspitya, S.; Wijerathne, B.; Madusanka, M. The wild boar Sus scrofa cristatus attacks in Sri Lanka: a case series and review of literature. Anuradhapura Med. J. 2023, 17(3), 27–34. [CrossRef]
- Zaimoglu, M.; Mete, E.B.; Bayatli, E.; Guner, Y.E.; Ozdemir, A.; Buyuktepe, M.; Eroglu, U. A rare cause of foot drop: wild boar bites. J. Ankara Univ. Fac. Med. 2023, 76, 166–168.
- Ketenci, H.Ç.; Boz, H.; Kırcı, G.S.; Özer, E.; Beyhun, N.E.; Büyük, Y. An evaluation of traumatic deaths associated with animal attacks: A 10-year autopsy study. Ulus. Travma Acil Cerrahi Derg. 2022, 28(3), 254–261. [CrossRef]
- Özsoy, S.; Ketenci, H.C.; Askay, M. Fatal land hunting-related injuries in the Eastern Black Sea region-Turkey. Ulus. Travma Acil Cerrahi Derg. 2022, 28(10), 1494–1499. [CrossRef]
- Kiran, M.; Shetty, M.; Shetty, S. Exsanguinated to death: A case of death due to wild boar attack. J. Indian Acad. Forensic Med. 2021, 43(2), 191–193. [CrossRef]
- Quraishi, A.H.; Damdoo, A.; Srinivasan, S.; Umare, G.; Tongse, P. Mechanisms and patterns of animal-related injuries in patients admitted to a major trauma center in central India. J. Emerg. Trauma Shock 2021, 14(3), 190–191. [CrossRef]
- Singh, P.K.; Ali, S.M.; Radhakrishnan, R.V.; Mohanty, C.R.; Sahu, M.R.; Patro, B.P.; Ms, I.; Panda, S.K. Pattern of injuries due to wild animal attack among patients presenting to the emergency department: A retrospective observational study. Chin. J. Traumatol. 2021, 24(6), 383–388. [CrossRef]
- Ruda, A.; Kolejka, J.; Silwal, A.T. Spatial concentrations of wildlife attacks on humans in chitwan national park, nepal. Animals 2020, 10(1), 153. [CrossRef]
- Dokter, M.; Philipp, K.P.; Bockholdt, B. Der vermeidbare (?) Jagdunfall – tödliche Oberschenkelverletzung durch ein Wildschwein. Rechtsmedizin 2018, 28, 442–445. [CrossRef]
- Nagasawa, H.; Omori, K.; Takeuchi, I.; Fujiwara, K.; Uehara, H.; Jitsuiki, K.; Kondo, A.; Ohsaka, H.; Ishikawa, K.; Yanagawa, Y. A case of near-fatal drowning caused by an attack from a wild boar. Wilderness Environ. Med. 2018, 29(4), 549–551. [CrossRef]
- Okano, I.; Midorikawa, Y.; Kushima, N.; Watanabe, Y.; Sugiyama, T.; Mitachi, K.; Shinohara, K.; Sawada, T.; Inagaki, K. Penetrating anorectal injury caused by a wild boar attack: a case report. Wilderness Environ. Med. 2018, 29(3), 375–379. [CrossRef]
- Oliveira, S.V. de; Vargas, A.; Rocha, S.M.; Pereira, L.R.M.; Oliveira, C.G. de; Silva, V.S. The nature of attacks by wild boar (Sus scrofa) and wild boar/domestic pig hybrids (“Javaporcos”) and the conduct of anti-rabies care in Brazil. InterAm. J. Med. Health 2018, 1, e-201801001. [CrossRef]
- Singaravelu, K.P.; Pandit, V.; Saya, R.P.; Nagasubramanyam, V. Unusual cause of chest trauma: Case report of wild boar attack. J. Dr. NTR Univ. Health Sci. 2018, 7(4), 285. [CrossRef]
- Nagasawa, H.; Omori, K.; Maeda, H.; Takeuchi, I.; Kato, S.; Iso, T.; Jitsuiki, K.; Yoshizawa, T.; Ishikawa, K.; Ohsaka, H.; Yanagawa, Y. Bite wounds caused by a wild boar: a case report. Wilderness Environ. Med. 2017, 28(4), 313–317. [CrossRef]
- Silwal, T.; Kolejka, J.; Bhatta, B.P.; Rayamajhi, S.; Sharma, R.P.; Poudel, B.S. When, where and whom: assessing wildlife attacks on people in Chitwan National Park, Nepal. Oryx 2017, 51, 370–377. [CrossRef]
- Tumram, N.K.; Ambade, V.N.; Dixit, P.G. Human fatalities caused by animal attacks: A six-year autopsy study. Med. Leg. J. 2017, 85(4), 194–199. [CrossRef]
- Bhingare, P.D.; Shelke, U.R.; Bang, Y.A. A case of recto-vesico-cutaneous fistula following perineal injury by wild boar. J. Clin. Diagn. Res. 2016, 10(5), PD03–PD04. [CrossRef]
- Akhade, S.P.; Rohi, K.R.; Phad, L.G.; Dixit, P.G. Fatal penetrating lacerated wound by tusk of indian wild boar. J. Indian Acad. Forensic Med. 2015, 37(1), 100–102. [CrossRef]
- Tumram, N.K.; Dhawne, S.G.; Ambade, V.N.; Dixit, P.G. Fatal tusk injuries from a wild boar attack. Med. Leg. J. 2015, 83(1), 54–56. [CrossRef]
- Sprem, N.; Skavić, P.; Dezdek, D.; Keros, T. The wild boar attack--a case report of a wild boar inflicted injury and treatment. Coll. Antropol. 2014, 38(4), 1211–1212.
- Sprem, N.; Skavić, P.; Krupec, I.; Budor, I. Patterns of game animal attacks on hunters in Croatia over a 13-year period. Wilderness Environ. Med. 2013, 24(3), 267–272. [CrossRef]
- Attarde, H.; Badjate, S.; Shenoi, S.R. Wild boar inflicted human injury. J. Maxillofac. Oral Surg. 2011, 10(1), 77–79. [CrossRef]
- Kose, O.; Guler, F.; Baz, A.B.; Akalin, S.; Turan, A. Management of a wild boar wound: a case report. Wilderness Environ. Med. 2011, 22(3), 242–245. [CrossRef]
- Rajendra, K.R.; Chandru, K. Death—Who Caused It? Wild Boar or Doctor—Case Report. Anil Aggrawal’s Internet Journal of Forensic Medicine and Toxicology 2011, 11, No. 2. Available online: https://anil.aggrawal.org/ij/vol_012_no_002/papers/paper001.html (accessed on 16 February 2026).
- Shetty, M.; Menezes, R.G.; Kanchan, T.; Shetty, B.S.; Chauhan, A. Fatal craniocerebral injury from wild boar attack. Wilderness Environ. Med. 2008, 19(3), 222–223. [CrossRef]
- Gunduz, A.; Turedi, S.; Nuhoglu, I.; Kalkan, A.; Turkmen, S. Wild boar attacks. Wilderness Environ. Med. 2007, 18(2), 117–119. [CrossRef]
- Manipady, S.; Menezes, R.G.; Bastia, B.K. Death by attack from a wild boar. J. Clin. Forensic Med. 2006, 13(2), 89–91. [CrossRef]
- Escande, F.; Bailly, A.; Bone, S.; Lemozy, J. Actinobacillus suis infection after a pig bite. Lancet 1996, 348, 888. [CrossRef]
- Gubler, J.G.H. Septic arthritis of the knee induced by Pasteurella multocida and Bacteroides fragilis following an attack by a wild boar. J. Wilderness Med. 1992, 3(3), 288–291. [CrossRef]
- Van Demark, R.E., Sr.; Van Demark, R.E., Jr. Swine bites of the hand. J. Hand Surg. Am. 1991, 16(1), 136–138. [CrossRef]
- Goldstein, E.J.; Citron, D.M.; Merkin, T.E.; Pickett, M.J. Recovery of an unusual Flavobacterium group IIb-like isolate from a hand infection following pig bite. J. Clin. Microbiol. 1990, 28, 1079–1081. [CrossRef]
- Barnham, M. Pig bite injuries and infection: report of seven human cases. Epidemiol. Infect. 1988, 101(3), 641–645. [CrossRef]
- Barss, P.; Ennis, S. Injuries caused by pigs in Papua New Guinea. Med. J. Aust. 1988, 149, 649–656. [CrossRef]
| Study | Y | C/R | Study type | N | Animal type | Main content / relevance |
| [17] | 2025 | USA (central Florida) | Case report | 1 | WB | Pediatric knee arthrotomy from WB tusk during hunting; intra-articular air on imaging; required urgent irrigation/debridement. Cultures grew Stenotrophomonas maltophilia and Aspergillus spp.; recovered fully after targeted therapy. |
| [18] | 2025 | Japan | Case report | 1 | WB | Penetrating thoracic injury with pneumothorax; CT-based diagnosis and chest tube placement; good recovery. |
| [19] | 2024 | Nepal | Case report | 1 | WB | Penetrating lower-extremity WB injury in a rural setting; deep soft-tissue laceration with significant contamination; treated with debridement, irrigation, and antibiotics; uneventful recovery. |
| [20] | 2024 | Japan | Case report | 1 | WB | Penetrating upper-body WB injury in suburban environment; deep soft-tissue trauma requiring surgical debridement; full recovery. |
| [21] | 2024 | Turkey | Case report | 1 | WB | Lower-extremity WB laceration with extensive contamination; operative irrigation/debridement and antibiotics; uncomplicated outcome. |
| [4] | 2024 | Spain | Case series / institutional protocol revision | Several | WB | Trauma service experience with WB extremity injuries; emphasizes standardized debridement protocol and broad-spectrum antibiotics. |
| [22] | 2023 | South Korea | Case report | 1 | WB | Lower-limb WB bite/laceration; surgically treated with irrigation/debridement and antibiotics; favorable recovery. |
| [23] | 2023 | Japan | Case report | 1 | WB | Chest/upper-body trauma from WB; emphasizes need for imaging and monitoring even in apparently stable patients. |
| [24] | 2023 | Sri Lanka | Case series | Several | WB | Series of WB attacks in agricultural workers; includes severe perineal, thigh, abdominal injuries with evisceration; describes surgery, tetanus and rabies prophylaxis. |
| [25] | 2023 | Turkey | Case report | 1 | WB | Peroneal nerve injury from deep calf laceration; required neurolysis; persistent foot drop; highlights neurovascular risk. |
| [26] | 2022 | Turkey | Case report | 1 | WB | Lower-extremity boar wound; illustrates management and need for surgical debridement and antibiotics. |
| [27] | 2022 | Turkey | Case report | 1 | WB | Knee joint–penetrating boar injury with joint involvement; orthopedic washout and infection prevention. |
| [28] | 2021 | India | Small series / retrospective | Several | WB/DP (mixed context) | Describes patterns of pig-related wounds (mostly lower-limb), mechanisms, and outcomes; provides additional Indian data on severity and contamination. |
| [29] | 2021 | Oman | Retrospective review of animal-related injuries | Subset | WB among other species | Describes patterns of wildlife trauma; WB cases characterized by lower-limb soft-tissue injuries requiring operative care. |
| [30] | 2021 | India | Animal-attack review | Subset | WB among others | Provides broader context of wildlife injuries in India; WB attacks form a small but severe portion. |
| [31] | 2020 | Europe | Spatial / epidemiologic study | N/A | Wildlife including WB | Spatial analysis of wildlife-related injuries and conflicts; relevant for prevention and risk mapping in regions with WB. |
| [32] | 2018 | Global | Review of wildlife trauma | Mixed | Various wild animals | Broad review of animal-related trauma; WB injuries are one component; used mainly for general trauma context, not specific case data. |
| [33] | 2018 | Japan | Case report | 1 | WB | Penetrating chest / rib fracture / pneumothorax; demonstrates thoracic risk even with small skin wounds. |
| [34] | 2018 | Japan | Case report (WEM) | 1 | WB | Complex attack: femoral artery and sciatic nerve injury, anorectal injury, pelvic fractures, open pneumothorax; prolonged, staged surgical management and complications. |
| [35] | 2018 | Brazil (national) | Retrospective analysis of human rabies treatment forms | 309 WB / WB–DP attacks | WB and WB/DP (“javaporcos”) | Nationwide Brazilian dataset: 309 attacks (271 WB, 38 hybrids); mainly deep single bites to lower limbs; anti-rabies serum+vaccine most commonly indicated; shows expanding WB invasion and health-system response. |
| [36] | 2018 | India | Case report | 1 | WB | Penetrating chest injury from WB with pneumothorax and subcutaneous emphysema; diagnosed via ultrasound and CT; treated with tube thoracostomy. |
| [37] | 2017 | Japan | Case report | 1 | WB | WB bite wounds to lower extremity; significant contamination; wound infection requiring re-debridement. |
| [38] | 2017 | Nepal (Chitwan NP) | 10-year wildlife conflict registry | 38 WB attacks | WB | Wildlife attacks on people in buffer zone; 38 WB-related events with pattern of lower-limb injuries and risk factors (time of day, activity). |
| [39] | 2017 | India | 6-year autopsy series of animal-attack deaths | Subset | Mixed including WB | Describes human fatalities caused by animal attacks; WB attacks are a subset, emphasizing that WB can be a cause of fatal trauma. |
| [40] | 2016 | India | Case report | 1 | WB | Perineal penetrating injury with recto-vesico-cutaneous fistula after WB attack; complex pelvic reconstruction and fistula repair. |
| [41] | 2015 | India | Forensic case report | 1 | WB | Fatal penetrating thigh wound from WB tusk with femoral vessel injury; illustrates exsanguinating potential of lower-limb tusk injuries. |
| [42] | 2015 | India | Forensic case report | 1 | WB | Fatal tusk injuries to thigh with transection of femoral vessels and nerve; provides detailed autopsy description of hemorrhagic death. |
| [43] | 2014 | Croatia | Case report | 1 | WB | Single WB-inflicted lower-extremity bite wounds in hunter; irrigation, debridement, primary closure; antibiotics; no complications. |
| [44] | 2013 | Croatia | Retrospective series of hunter injuries | Several | Mixed game including WB | Patterns of game-animal attacks on hunters; WB a prominent species; lower-limb soft-tissue injuries dominate; most require surgical management. |
| [45] | 2011 | India | Case report | 1 | WB | Facial/maxillofacial injury caused by WB; deep soft-tissue laceration; emphasizes need for surgical debridement and layered closure. |
| [46] | 2011 | Turkey | Case report | 1 | WB | Severe thigh laceration from WB attack; surgically treated; underscores contamination risk and need for broad-spectrum antibiotics. |
| [47] | 2010 | India | Case report | 1 | WB | Severe scrotal/testicular laceration by WB; highlights groin vulnerability and reconstructive issues. |
| [48] | 2008 | India | Case report | 1 | WB | Major thigh injury with significant hemorrhage during WB encounter; demonstrates risk of shock and need for emergency surgery. |
| [49] | 2007 | Turkey | Case series | 3 | WB | “Wild Boar Attacks” – 3 rural cases; significant soft-tissue trauma, mostly lower extremities; one case with upper abdomen/chest involvement. |
| [50] | 2006 | India | Forensic case report | 1 | WB | Fatal WB attack with deep groin and thigh penetration and major vascular injury; classic example of exsanguination mechanism. |
| [51] | 1996 | France | Single infected-bite case | 1 | DP | Actinobacillus suis infection after DP bite to knee; highlights unusual pathogens and confirms amoxicillin-clavulanate as good empiric choice. |
| [52] | 1992 | Switzerland (WEM) | Case report | 1 | WB | Septic arthritis of knee after WB attack; mixed Pasteurella multocida and Bacteroides fragilis infection; classic example of deep joint contamination. |
| [53] | 1991 | USA | Case report | 1 | Domestic boar | Severe hand wound with deep-space infection after domestic boar bite; emphasizes need for aggressive debridement and antibiotic therapy. |
| [54] | 1990 | USA | Case report (microbiology) | 1 | Pig (DP) | Hand infection following pig bite; recovery of unusual Flavobacterium group IIb-like organism; part of pathogen spectrum relevant to pig / WB wounds. |
| [55] | 1988 | United Kingdom (North Yorkshire) | Case series | 7 | Swine (DP / boar) | “Pig bite injuries and infection”; deep posterior-thigh lacerations and other wounds; mixed infections (streptococci, Pasteurella, Bacteroides etc.); argues for broad-spectrum antibiotics in severe pig bites. |
| [56] | 1988 | Papua New Guinea | 6-year hospital-based review | 15 pig-injury admissions | Mainly DP, some feral pigs | Med J Aust paper: injuries caused by pigs; mixture of abdominal, chest, limb, and scrotal wounds; includes “sucking” chest wound, bilateral pneumothoraces, open fractures, nerve and tendon injuries; demonstrates severity of pig gorings. |
| [6] | 2023 | Global | Extended/updated review | >400 attacks / fatalities | Wild pigs | Expanded analysis of world-wide wild-pig attacks and fatalities; confirms pattern of severe soft-tissue and blunt trauma, with majority of deaths due to hemorrhage. |
| [3] | 2023 | France / Europe | Socio-ecologic analysis | N/A | WB | Addresses synurbic WB and human–boar conflicts in peri-urban settings; directly relevant for prevention and public-health messaging. |
| [2] | 2020 | Poland / Europe | Ecologic / management paper | N/A | WB | Explores WB population management, hunting pressure, and landscape changes; informs risk reduction discussion. |
| [7] | 2019 | Nordic countries / literature-based | Forensic literature review of fatal attacks by large mammals in the Nordic wilderness | 3 fatal WB cases extracted from literature | WB (plus bear, moose, wolf) | Reviews species-specific injury patterns in fatal attacks by brown bear, moose, wild boar, and wolf; WB section synthesizes three Indian fatal boar cases (lower-body tusk penetration, exsanguination or craniocerebral injury) to help forensic differentiation. |
| [1] | 2015 | Europe (general) | Ecologic / population review | N/A | WB | Describes expanding WB populations and implications for human–boar interactions and conflicts; crucial for prevention context. |
| [5] | 2013 | Global | Narrative review | 412 attacks compiled | Wild pigs (WB + feral) | Comprehensive global review of wild-pig attacks; describes circumstances (hunting, non-hunting), injury patterns (single lacerations, puncture wounds, fractures), and causes of death (mostly exsanguination). |
| [9] | 2004 | North America (Yellowstone / US context) | Narrative review of wild mammalian injuries | Not specified (review) | Various wild mammals (not pig-specific) | “North American wild mammalian injuries” (Emerg Med Clin N Am 2004); covers general patterns of wild animal trauma, field care, wound management, antibiotic choices, rabies & tetanus guidance; used for general wilderness/animal-attack management principles, not WB case data. |
| Anatomic region | Primary evidence [15A] | Additional findings [15B] | Clinical implications |
|---|---|---|---|
| Lower extremities | Most common injury site; deep penetrating wounds; heavy contamination. | Consistently reported internationally with long wound tracts. | High hemorrhage risk; mandatory imaging and exploration. |
| Groin / pelvis | Injuries near femoral vessels; soft-tissue avulsion. | Additional reports of vascular penetration and genital trauma. | Rapid hemorrhage control; vascular assessment essential. |
| Abdomen | Occasional upward penetration. | Multiple reports of peritoneal violation and visceral injury. | Exploratory laparotomy often required. |
| Thorax | Rare in cohort. | Reports of pneumothorax, hemothorax, rib fractures. | Requires immediate imaging. |
| Upper extremities | Mainly defensive wounds. | Deep-space infections and tendon injuries. | High infection risk. |
| Head / neck | Rare. | Severe and fatal cases reported. | Airway priority; rapid transfer. |
| Neurovascular structures | Occasional involvement. | Cases of nerve palsy and arterial injury. | Full neurovascular examination essential. |
| Presentation | Differential diagnoses | Imaging |
|---|---|---|
| Lower-extremity wound | Vascular injury, occult fracture | Doppler US, X-ray, CT angiography |
| Groin injury | Femoral vessel penetration | CT angiography |
| Abdominal penetration | Bowel perforation, organ injury | CT with contrast |
| Chest symptoms | Pneumothorax, hemothorax | X-ray, eFAST, CT |
| Neurologic deficit | Nerve injury, compartment syndrome | MRI |
| Joint penetration | Septic arthritis | X-ray, CT, operative assessment |
| Domain | Recommendation |
|---|---|
| Early assessment | High suspicion for deep injury |
| Hemorrhage control | Direct pressure, hemostatic agents, tourniquet |
| Imaging | X-ray, ultrasound, CT |
| Surgical care | Thorough exploration, delayed closure |
| Antibiotics | Early broad-spectrum therapy |
| Tetanus/rabies | Universal tetanus; rabies per region |
| Disposition | Early evacuation for major injury |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




