Introduction
Active ageing is commonly regarded as a desirable phenomenon in our global society, given that it is expected to have a positive impact on health and subsequently a negative one on the care burden which societies face worldwide. A valuable social activity for an active life is helping out, which is, in the existing literature, primarily discussed in the context of voluntarism. This social activity of helping out is primarily expected to trigger beneficial effects on well-being and health. An overarching study of this association is provided by de Wit, Qu and Bekkers [
1] through their ‘mega-analysis’ across 33 years and 22 European countries of six longitudinal panel surveys, SHARE included. They estimate that, through volunteering, a health advantage of, on average, more than 13 per cent is acquired. The health advantage tends to increase with age, and to be a priori larger for those with a worse state of health. On top of their fixed-effects regressions, first-difference estimators confirm the significant positive influence of continuing volunteering compared to stopping with it. This effect also results from the analysis of Kleiner et al. [
2], who document the impact of volunteering on health through quality of life scores extracted from questionnaires and focus groups covering the older Swiss community. The scores are regressed with logistic estimators on variables covering age, gender, education, subsidy recipient, and impairment for both the states of stopped and continued volunteering. They find the odds of a decrease in quality of life to be higher in the stopped state, more precisely 75 per cent and 66 per cent higher for, respectively, self-esteem and autonomy. The study of Weziak-Bialowolska, Skiba, and Bialowolski [
3] also supports the health advantage resulting from helping out. Based on SHARE-data from 15 European countries and with generalised estimating models, they document reciprocal longitudinal associations, of which the significant and positive associations of optimism and vitality with doing voluntary activity at least once a week are the most explicit. Other positive psychological well-being effects resulting from volunteering are illustrated by Huo, Miller, Kim, and Liu [
4] through an autoregressive cross-lagged panel model based on the Health and Retirement Study Wave 2010 and 2014. Individuals aged 65 or older confirm significantly increased positive self-perceptions of ageing, and decreased negative perceptions when volunteering more than 100 hours. The effect appears not to significantly impact depressive symptoms, just as volunteering less than 100 hours overall. Volunteering at least 200 hours during the past year might even reduce the risk of deterioration or dying for adults with cardiovascular disease. Heisler et al. [
5] conclude the latter based on the Health and Retirement Study in the United States with, among others, ordered logistic regressions. The importance of the frequency of volunteering is also illustrated by Lawton, Gramatki, Watt, and Fujiwara [
6], who find that more volunteering results in higher well-being in the United Kingdom across a period of 20 years. With fixed-effects estimators they notice that self-rated health on a one-to-five scale increases with the volunteering frequency, i.e. from rarely (baseline) over several times a year (coefficient 0.098, p<.01) to at least once a week (coefficient 0.126, p<.01). Pavlova and Lühr [
7] document an additional psychological impact of volunteering on social well-being with data from the 2012 European Social Survey covering 29 European countries. For their three dependent variables representing well-being, i.e. generalised trust, perceived social support, and loneliness, the positive impact of volunteering is significant at a 0.1 level. Significant independent variables at the same level are, among others, education, employment, income, gender, and self-reported general health. Additionally, the impact of offering help tends to vary geographically. Lakomy [
8] distinguishes this variation between welfare regimes with panel fixed-effects regressions based on SHARE data from Waves 4 to 6. He finds that caregiving outside the household has no significant influence under any regime, but that providing care within the household significantly influences quality of life under all regimes except the social-democratic one, as found in Denmark or Sweden. In turn, under the latter regime, volunteering has a significant influence on the quality of life as well as in the Mediterranean countries, for example, Italy or Spain. Yet, in conservative countries like Austria, Belgium, France, or Germany, and post-communist countries, like Czech Republic, Estonia and Slovenia, the benefits of voluntarism for quality of life are expected to be limited. Additionally, Morawski, Okulicz-Kozaryn, and Strzelecka [
9] find, also with SHARE data, that voluntary work positively correlates to quality of life. Their Kendall tau-b correlation coefficients reveal that intrinsic aspects like self-realisation relate to higher volunteering rates, not extrinsic ones like control. Meneghini and Colledani [
10] notice the same dominant contribution of intrinsic motivation to satisfaction with life and well-being in their smaller sample of 133 Italians. They find a 40 per cent increase in life satisfaction allocatable to the commitment to volunteering. Besides improving life quality, those who help out others are also expected to live longer, an expectation which is mediated by prospective health [
11]. Lastly, the impact of a health shock on self-perceived health is worth mentioning, given the more recent occurrence of COVID-19. The latter appears to undo the positive effect of volunteering, and might even trigger a negative effect of volunteering on well-being [
12]. To conclude, the act of helping out is, besides factors like life satisfaction, health shocks or income, proven to influence well-being, self-perceived health included. Overall, past research indicates that helping behaviour facilitates healthy ageing.
On top of well-being, helping out relates to status. Three kinds of status are documented, i.e. job, financial, and social status. First, job status is known to influence volunteering as well as health. Hämäläinen et al. [
13] find that retirement initiates more volunteering, in particular, for those who perceive having better health. Their results rely on fixed-effects panel regressions based on SHARE data from 2011 to 2018 of 19 European countries. Kalbarczyk and Łopaciuk-Gonczaryk [
14] use the same dataset, limited to 2011 and 2015, for 14 European countries to conclude, based on a Generalised Structural Equation Model, that “active people remain active and inactive people remain so after retirement”. Besides acknowledging the relevance of retirement, the relationship between volunteering and employment is discussed. Strauss [
15] scrutinises five waves of SHARE data from 2004 up to 2015 for 13 nationalities in the EU in the age category 50 years and older. He relies on multi-level random-effects as well as conditional fixed-effects logistic regressions to explore the impact of caregiving on volunteering. His research illustrates how caregivers tend to volunteer more than non-caregivers, as well as that cash-for-care expenditures stimulate both groups to volunteer, likely resulting from receiving compensation for the loss of income from paid work. Almeida-Meza, Di Gessa, Lacey, McMunn, and Xue [
16] similarly find carers and former carers to volunteer more than non-carers across five waves of SHARE covering 16 European countries. Moreover, they note that the frequency of care positively relates to the frequency of volunteering. Second, on top of job status, the relationship between financial status and frequency of helping is documented. Hämäläinen et al. [
17] explore Waves 4 to 8 of SHARE with a fixed-effects ordered logit model to find a positive relationship between the frequency of volunteering and deteriorating health as well as worsening financial condition. They find that a change to a worse financial condition increases the probability of not volunteering, while the inverse effect, i.e. a change to a better financial condition, appears to have no significant effect. Besides job status, financial status, as measured by income, influences the effect of frequency of participation in formal social activities on loneliness, being an aspect of mental health. Nissanholtz-Gannot and Peretz-Dayan [
18] scrutinise this effect through hierarchical multiple regression models for 18 European countries based on Wave 6 of SHARE. Formal social activity is defined as participating in, e.g., charity or social organisations, and can be considered as a conditioned form of helping, as it mostly comes with private financial expenses. Nissanholtz-Gannot et al. find frequent formal social activity relevant for the lower income quintiles, as it significantly reduces the self-perceived loneliness scores. In a similar social context, Näsman et al. [
19] discuss formal volunteering jointly with three other factors of civic engagement, e.g., political participation. Relying on data from the European Quality of Life Survey covering 32 European countries, their logistic regressions reveal significant relationships between formal volunteering and individual resources, i.e. education level, income, and health. They conclude that civic engagement, volunteering included, benefits from additional investment in the individual resources on top of the country-level social expenditures. As such, the individual as well as the national financial context is relevant for cultivating a culture of helping out. Lastly, the societal recognition or position a volunteer enjoys is of interest. Sánchez-García et al. [
20] conclude, based on 29 countries covered in the European Social Survey (ESS), that people aged 70 years and older “who volunteer are 1.7 times more likely to report better health and life satisfaction”. Additionally, their multilevel regression models with fixed and random effects reveal a significant moderation effect of older people’s social status on volunteering. To conclude, the act of helping others is expected to occur in a context conditioned by the financial, work, and social status.
Data
The longitudinal analysis in this study relies on data from SHARE. The latter is a recurring health survey that inquires European citizens about the effects of health, social, economic and environmental policies. The data used for this study covers Waves 4 to 9, and 12 countries in Europe, being Austria, Germany, Sweden, the Netherlands, Spain, Italy, France, Denmark, Switzerland, Belgium, Czech Republic, and Slovenia. [
21,
22,
23,
24,
25,
26]. The dataset based on the six SHARE waves is unbalanced on the panel level, i.e. on the level of an individual respondent, due to the fact that the same respondents from Wave 4 are taken forward up to Wave 9 without replacement. The latter is accounted for by integrating calibrated longitudinal weights in the estimators. Additionally, the panel time level comes with gaps resulting from the frequency of surveying; nevertheless, this is no cause for concern. Nonetheless, the dataset is well balanced based on gender, as on average 43.9 per cent of the respondents are female and 56.1 per cent are male. Worth mentioning is that it primarily regards retired respondents, given that 75.9 per cent report being retired in Wave 4 (2011), up to 87.9 per cent in Wave 9 (2022).
Besides the structure, the content of the dataset is highlighted. As
Table 1 illustrates, the dataset consists of 16 variables, of which four are considered continuous. It consists of 109,546 observations for 29,995 respondents, each reporting maximally six times across the panel time horizon.
Table 1 reveals the one-to-five scale of the dependent variable self-perceived health, which is the health status from Excellent to Poor. The independent variables are primarily individual characteristics, except for the occurrence of COVID-19, the respondent’s unique number and year of survey. As such, the pandemic is specified with a binary variable, which is set to one when the year of survey is 2022. The responses of Wave 8, i.e. from 2020, are not marked as 70 per cent of the interviews for that wave were already conducted at the time of the lockdown [
27]. The total time horizon covers Wave 4 for 2011, Wave 5 for 2013, Wave 6 for 2015, Wave 7 for 2017, Wave 8 for 2019/2020, and Wave 9 for 2021/2022. The respondent’s individual characteristics are reflected through 13 independent variables, of which two are of prior interest. First, the former are summarised. Age has a range from 59 to 100 and a mean of approx.74 years, while the respondents’ years of education range from zero to 30, with a mean of 10 years. Total household income is stated, if required through conversion, in Euro and has a minimum of zero and a maximum of approx.94,000 euro. On average, a household reports a total household income of 27,489 euro, which can consist of earnings from any kind of employment, pensions, benefits, rent, financial products, as well as those from other household members. Total household income is preferred as it reflects the financial power of the respondent’s household, which is assumed to be available for supporting the living conditions of the household as a whole, including the respondent. Given its relatively wide scale, the income variable has been standardised by subtracting the mean from each income and subsequently dividing it by the standard deviation. Besides household income, the household type is included in three non-overlapping categories, namely “Single”, “Couple, both responding”, and “Multiple, at least 1 responding”. This variable results from regrouping the original variable with nine categories, of which the categories “Single”, with 37,717 observations, and “Couple, both responding”, with 62,737 observations, are preserved. The newly created category “Multiple, at least 1 responding” comprises the remaining 9,092 observations. Additionally, the variable Job situation indicates if the respondent is retired, employed or self-employed, unemployed, permanently sick or disabled, homemaker, or in another situation (e.g., studying or volunteering). The Job situation variable includes, as three other variables, a category “Not in universe”, which is not included in the output yet bundles the feedback of respondents refusing to answer, not knowing an answer, and the like. For Job situation, this category accounts for 1.6 per cent of the total number of observations. The Being limited binary indicator, also known as the Global Activity Limitation Indicator, reflects a respondent’s limitation in activities because of a health problem, and denotes “Not limited” or “Limited”. The Number of activities last year originally reflects whether the respondent did sports, reading, charity, and the like. It is regrouped to “None”, i.e. participated in no activities, and “At least 1”. It also includes the category “Not in universe”, which accounts for 1.6 per cent of the total number of observations. The variable Country holds the original SHARE country numbers for the 12 European countries in the dataset, being Austria, Germany, Sweden, the Netherlands, Spain, Italy, France, Denmark, Switzerland, Belgium, Czech Republic, and Slovenia. Lastly, the value of a helping hand is reflected in the covariates of interest Receiving help from, and Giving help to others. Both cover help from or to people inside or outside the household provided during the last 12 months, and originally specify an exact number of persons. Both have been converted to a variable with categories “None” and “At least 1”. The “Not in universe” category occurs in both the Receiving and Giving help variables, with, respectively, 7.6 per cent and 21.7 per cent of the total number of observations. In conclusion, the dataset variables are constructed to facilitate the regression analysis as well as to safeguard the integration of a maximum of known relevant determinants.
To visualise the time dimension of the dataset, two figures are included.
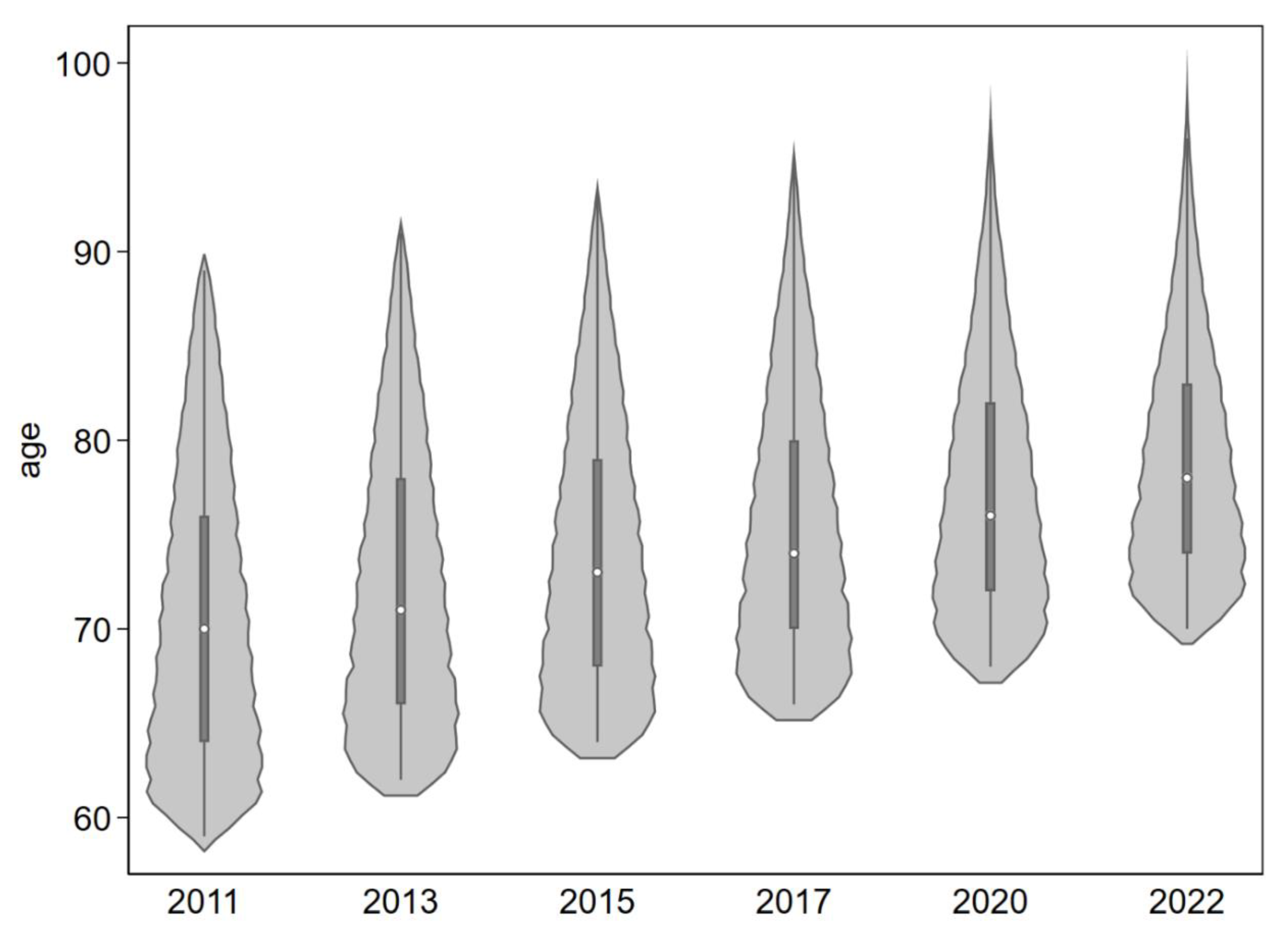
Figure 1 shows the age distribution of the respondents over time, while
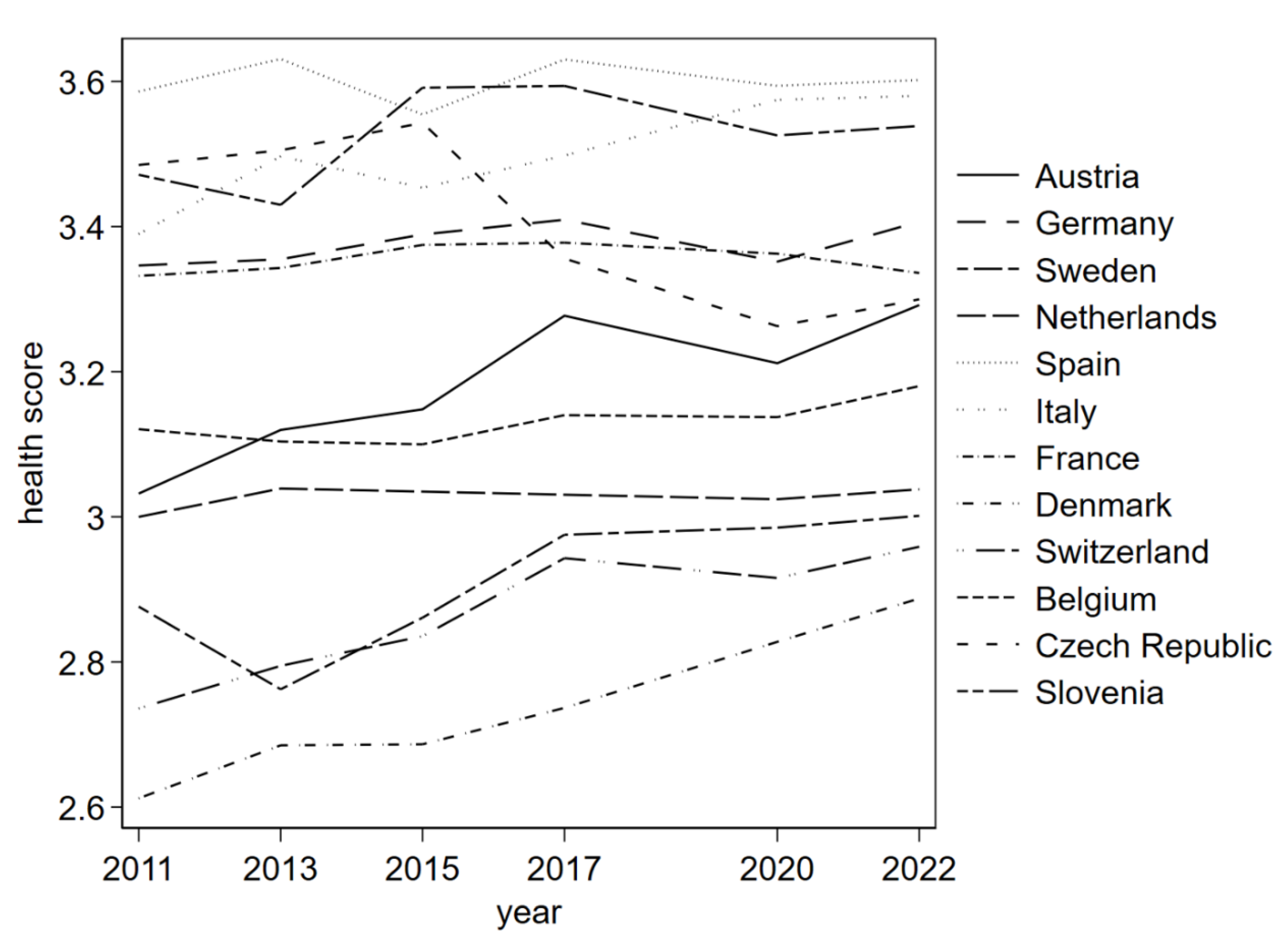
Figure 2 plots the average self-perceived health score per country over time.
Figure 1 Age distributions per wave across countries from 2011 to 2022. Based on SHARE-data Wave 4 to 9.
Figure 2 Average self-perceived health status per country per year
Besides the time dimension, the correlation structure of the variables is verified to ensure that the variables are compatible in regression analysis. Both the Pearson and Spearman Rank Order correlations are referred to.
Table 2 illustrates the Pearson correlations, which are merely interpretable as an approximation, given that Skewness and Kurtosis tests don’t accept the null hypothesis of normality (n = 109,546) of the continuous variables. Nevertheless, thanks to the sufficiently large sample size, the Pearson correlations remain informative.
Table 2 reveals that the Pearson coefficients are well below a 0.60 threshold. Additionally, the Spearman Rank correlations are calculated between all variables (see
Table A1 in
Appendix A). Being limited appears strongly yet soundly related to self-perceived health, given the 0.533 correlation coefficient. Life satisfaction modestly correlates with the dependent variable by noting a -0.353 coefficient. On top, Total household income appears correlated with the Household type as well as with Receiving help, given their coefficients of, respectively, 0.352 and -0.358. Overall, the correlation tests do not suggest the exclusion of any of the selected variables for the regression analysis.
Two final characteristics of the dataset are worth mentioning. First, as commonly experienced with surveys, SHARE has issues of non-response and subsequently missing values. The SHARE data uses two approaches to handle these issues, i.e. the Hot-deck Imputations and Fully Conditional Specification approach. The former is used for negligible fractions of missing data, primarily of socio-demographic characteristics, and replaces the missing values with those of a similar recipient or donor. The latter handles the sizeable fractions of missing values, primarily in monetary variables. The imputation procedure is repeated five times, which results in five imputed datasets differing only in values, not structure. Completing a robustness test by repeating the regression analysis across the five imputed datasets is motivated by the fact that 12 of the 14 regressed variables, including the dependent variable, are referred to as being imputed with one of the two imputation procedures [
27]. Second, the analysis of SHARE data across the targeted time horizon preferably integrates calibrated longitudinal weights, which are calculated based on the reweighing procedure advised by Pacifico [
28]. This procedure reweighs the data according to the mortality per year, country, age and gender as provided by Eurostat. It aims to “compensate for both problems of unit nonresponse in the baseline and refreshment samples of each wave, and problems of attrition in the longitudinal samples of different waves” [
29]. Both imputations and weights are expected to improve the longitudinal analysis.
Descriptive Analysis
To exploit the informativeness of the data, a descriptive analysis is documented of the dependent variable, i.e. self-perceived health, as well as of the two covariates of interest, i.e. Receiving and Giving help.
Table 3 shows the distribution of older people’s reported health status across its five categories per year.
Table 3 illustrates that a category’s rank within years holds across the years. As such, the categories fluctuate around the following percentages across the time horizon: “Good” (approx. 40 per cent), “Fair” (approx. 29 per cent), “Very good” (approx. 15 per cent), “Poor” (approx. 11 per cent) and “Excellent” (approx. 5 per cent). On top, the health status moves gradually towards the middle category, as reflected by the combined decrease in 2022 of the categories “Poor” and “Excellent” of approximately three percentage points in favour of the category “Good”. Another interesting movement is how the respondents transition between categories over the years.
Table 4 documents the transitions for the entire time horizon.
The transition probabilities in
Table 4 on the main left diagonal indicate that the respondent most likely rates the same health score. Moreover, no large shifts to the extreme categories can be noted, as illustrated by the low percentages in the top right and bottom left corners. A respondent appears to move primarily to neighbouring categories. As such, with a 33.4 per cent likelihood, the respondent shifts from “Excellent” to the nearest lower category “Very good”, while, likewise, with a 38.7 per cent likelihood from “Very good” to “Good”. The transition from “Good” is also primarily downwards, given that a respondent moves 23.8 per cent of the time to the category “Fair”. The lowest but one category turns the trend as a 28.7 per cent likelihood applies to the shift from “Fair” to “Good”. The lowest category, “Poor”, notes a 34.3 per cent likelihood that a respondent shifts to the category “Fair”. Lastly, the total reveals that approximately 40 per cent of the time a respondent marks a good health status.
After the dependent variable, the two variables of interest are described and subsequently analysed.
Table 5 describes the Receiving help variable according to the categories of self-perceived health.
Table 5 shows that, over time, a minimum of 50.1 per cent and a maximum of 88.9 per cent of the respondents report receiving no help, while a minimum of 11.1 per cent and a maximum of 49.9 per cent apply to those who report receiving help. These boundaries indicate that respondents dominantly receive no help across the time horizon. Another finding is that receiving help negatively relates to health status. Of those who report a poor health status, 43.7 per cent of all respondents across years report receiving help, while of those who report an excellent health status, merely 14.7 per cent receive help. This is no surprise as poor health suggests a need for additional help, and vice versa. Across categories and years, the majority of the older people consistently report not receiving help; however, across years, the cohort that receives help grows from 20.4 per cent in 2011 to 31.4 per cent in 2022. Overall, an increasing trend in receiving help arises from the data. To reveal the trend in the variable, it is described in
Table 6.
For Giving help, an inverse trend can be concluded as giving help positively relates to self-perceived health status. In total, 37.3 per cent of the older people across years who report excellent health actually give help to at least one other, while merely 10.8 per cent of those who report poor health provide a helping hand. Overall, a larger part of the population appears not to give help. Over time, a minimum of 55.7 per cent and a maximum of 91.7 per cent of the respondents report not giving help, while a minimum of 8.3 per cent and a maximum of 44.3 per cent applies to the givers of help. Moreover, a declining trend over the years suggests that fewer people give help. To conclude, the descriptive analysis documents a diminishing trend of giving help and an increasing one of receiving help. In the subsequent section, the regression analysis will explore the relations between self-perceived health and receiving as well as giving help in depth while accounting for the influence of other health determinants.
Results
The value of a helping hand is estimated through five estimators, of which two are considered supportive for the choice of estimator, while three are regarded as valuable for interpretation. The coefficients with standard errors and the estimators’ specifications of all five estimators are listed in
Table 7.
Table 7 shows, in the second and third columns, the output of the FE and RE, which show differences in sign and significance, yet are primarily reported to support the Breusch and Pagan Lagrange test, the Hausman specification test, and the Mundlak specification test. Based on the FE and RE, the three tests suggest the RE being the most efficient, given that a Mundlak correction is implemented. The latter, i.e. CRE, is reported in column four and relies on a Generalised Least Squares estimation method which provides robust standard errors. It integrates longitudinal weights on top of the Mundlak means, which appear most relevant as supported by the zero p-value of the Mundlak specification test. The primary disadvantage of the CRE is that it is unable to take the order of the dependent variable, i.e. self-perceived health, into account. Nevertheless, it explains a considerable amount of variation (R-Squared 0.447). Moreover, it reports a non-zero panel-level deviation (0.439), which supports the use of a panel instead of a pooled estimator, as well as a non-zero variance due to random individual differences, i.e. the random effects (0.319, not documented in a table). Moreover, the CRE confirms the theory of Yair Mundlak as its time-variant coefficients are the same as those of the FE, yet estimated with the more efficient random effects method. For convenience, the effects are interpreted per variable as specified in
Table 7. The odds ratio of the REO is referred to between brackets unless specified otherwise.
First, the results for the time-invariant variables Gender and Country, inestimable for the FEO, are highlighted. As such, older women appear to report a better health status (coefficient -0.018, SE 0.007, p<.05) on average across years, yet the REO marks this effect as insignificant (1.005, SE 0.040, p>.05), implying that there is no notifiable difference, on average across years, in the health reporting of men and women. For the variable Country, merely the ORs of the more accurate REO are interpreted as they express the same as the coefficients of the CRE. As such, Danish older people consistently mark a better health status (0.734, SE 0.056, p<.001) than the Swedish, while the odds to report a less healthy status than the Swedish are two to three times higher for older Spanish (3.249, SE 0.258, p<.001), Italian (2.262, 0.171, p<.001), and Slovenian citizens (2.198, 0.194, p<.001). The remaining countries report a more average health status, ranging incrementally from Austria (1.179, SE 0.077, p<.05), over Switzerland, Czech Republic and France, to Germany (1.863, SE 0.137, p<.001). In contrast to the findings from
Figure 2, the Low Countries, i.e. Belgium and the Netherlands, report non-significant coefficients, implying that they do not differ from Sweden.
Second, the time-variant variables are interpreted. For four continuous variables, nonlinearity is tested through their squares. For age and its square, the CRE and FEO contrast in significance, while the REO marks the main effect insignificant (0.955, SE 0.044, p>.05) and the nonlinear negative effect on health as significant (1.001, SE 0.000, p<.01). None of the latter three estimators finds nor the years of education nor its squares significantly impacting the health status. However, they dominantly mark the total household income (0.897, SE 0.032, p<.01) and its square (1.034, SE 0.017, p<.05), as well as the life satisfaction level (0.807, SE 0.04, p<.001) as positive influencers of health. For the remaining seven categorical variables, two appear to be mainly not significant, i.e. the impact of COVID-19, and four out of five categories of the variable Job situation. For the latter, only being permanently sick or disabled increases the odds of reporting a lower health status (1.851, SE 0.306, p<.001) compared to the baseline, i.e. the older people who are employed. Additionally, four categorical variables are consistently significant. Households with a couple of which both are responding (1.205, 0.087, p<.01), as well as with multiple members of which at least one is responding (1.221, 0.120, p<.05), considerably increase the odds of reporting a less favourable health status compared to older people who live alone. Being limited in activities due to health problems drastically increases the expectation of reporting worse health (3.904, 0.131, p<.001), while participating in at least one activity decreases this expectation compared to the baseline of no participation (0.812, SE 0.037, p<.001). Regarding the two variables of interest, all three estimators consider that receiving help significantly impacts the health status. In particular, the REO reveals that receiving help from at least one other person implies a 24.8 per cent increase in the odds of reporting worse health (1.248, SE 0.056, p<.001). For the act of giving help, the interpretation of significance levels of the CRE, FEO and REO is twofold. Or, the main effects are considered significant as suggested by the CRE (coefficient -0.025, SE 0.008, p<.01) and FEO (0.903, SE 0.043, p<.05), and the interactions with Receiving help are considered not significant. Or, the interaction effect of giving help and receiving help (0.863, SE 0.064, p<.05), and not the main effect of giving help, is regarded as relevant for health status. For two reasons, the latter is assumed to be most rational. First, the CRE neglects the order of the dependent variable; second, the FEO is expected to be less efficient than the REO. As such, the value of a helping hand is confirmed by the fact that, on average across years, older people who receive help from at least one other person are 24.8 per cent more likely to report worse health. Yet, when they, on top, also give help, the odds are lower, i.e. merely 7.7 per cent higher, to report worse health. As such, this decrease of 17.1 percentage points reflects the positive value of a helping hand and suggests an improvement in health status thanks to the act of giving help.
To support the results of the regression analysis, a robustness check is documented (see Materials and Code availability). As such, to account for the SHARE imputation procedure, the CRE, FEO, and REO referred to in
Table 7 are also estimated with the remaining four imputed datasets. The CRE reports for the 13 significant coefficients, the same significance level and sign for all five imputed datasets. On top, three estimated coefficients are numerically the same for these five regressions, while the remaining coefficients deviate on average by 0.004 and maximally by 0.011. For the FEO, the same significant eight estimated odds ratios appear with the same sign, yet with three times another significance level for two estimated odds ratios. The difference between the estimated FEO odds ratios is minimally 0.004 and maximally 0.091. For the REO, 18 estimated odds ratios maintain the same sign; however, six differ in significance level, of which three even altered into non-significant odds ratios across the five imputed datasets, namely “Total household income” as well as its square, and “Household: Multiple, at least 1 responding”. Besides the latter, the squared age is consistently identical, while the largest variation in the REO odds ratios is 0.106 and detected in the job situation category “Permanently sick or disabled”. Overall, these findings illustrate that the robustness of the regression output is primarily related to the complexity of the estimator, not the imputation procedure. To conclude, the findings documented in
Table 7 based on the first imputed dataset are regarded as robust, except for the household type and total household income as well as its squares.
Besides the interpretation of the coefficients, the estimators CRE, FEO, and REO are used to predict margins and marginal effects. However, all three underperform in estimating predictions due to the Giving help variable. For the latter, its limited number of observations in certain time segments is expected to cause the underperformance. As such, solely the best performing, i.e. the CRE, is used to generate plots of and predictions for the average older European citizen. First, three plots with margins are documented for the effect of Receiving as well as Giving help on, respectively, age, income, and life satisfaction.
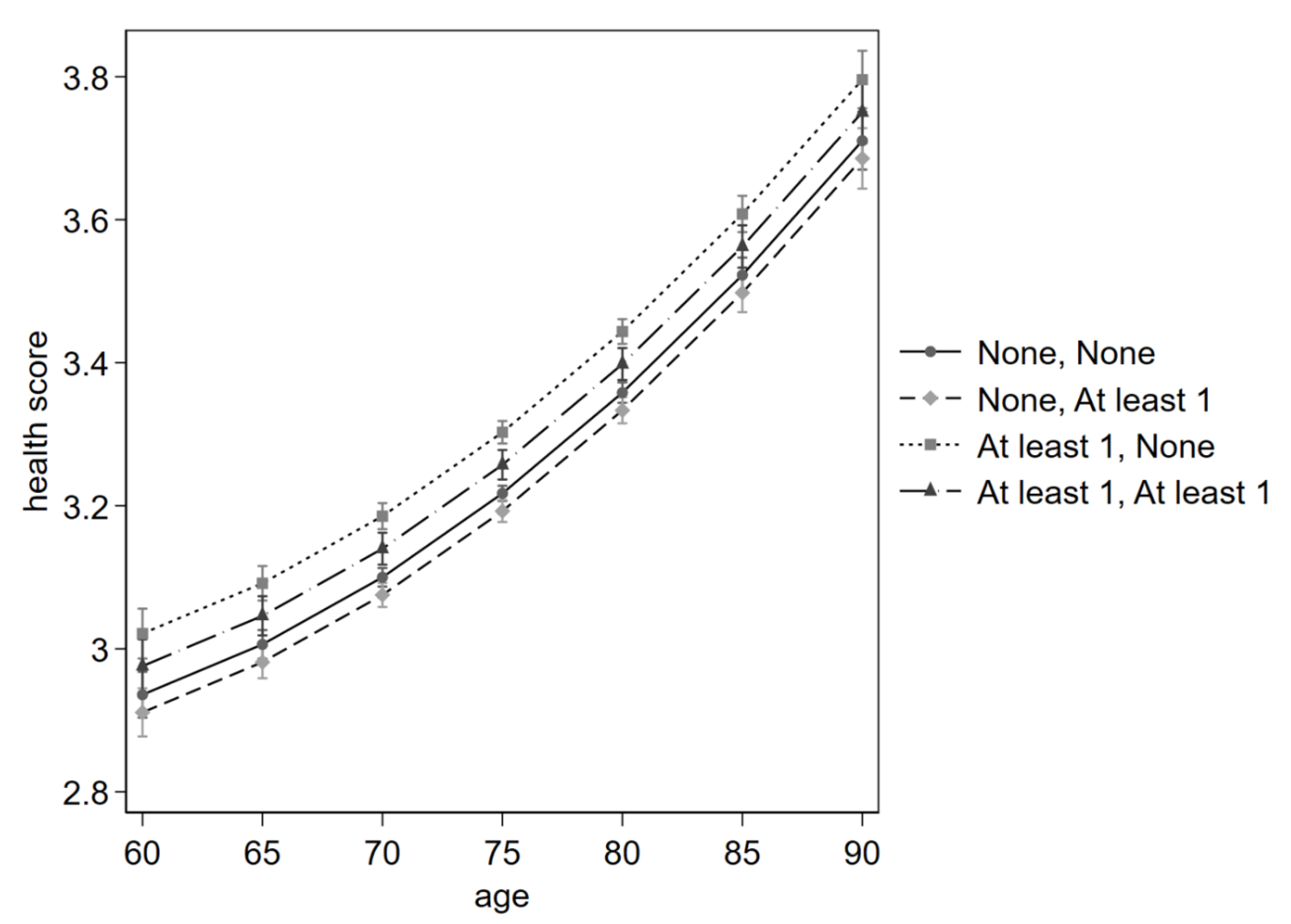
Figure 3 reports the predictions for the self-perceived health status of older people according to four combinations of receiving and giving help.
Figure 3 CRE Margins of responses of the self-perceived health score according to age, visualised in steps of five years from 60 to 90 years. Four combinations of receiving and giving help are plotted, each from or to no other, and from or to at least one other. The legend specifies Receiving help and subsequently Giving help.
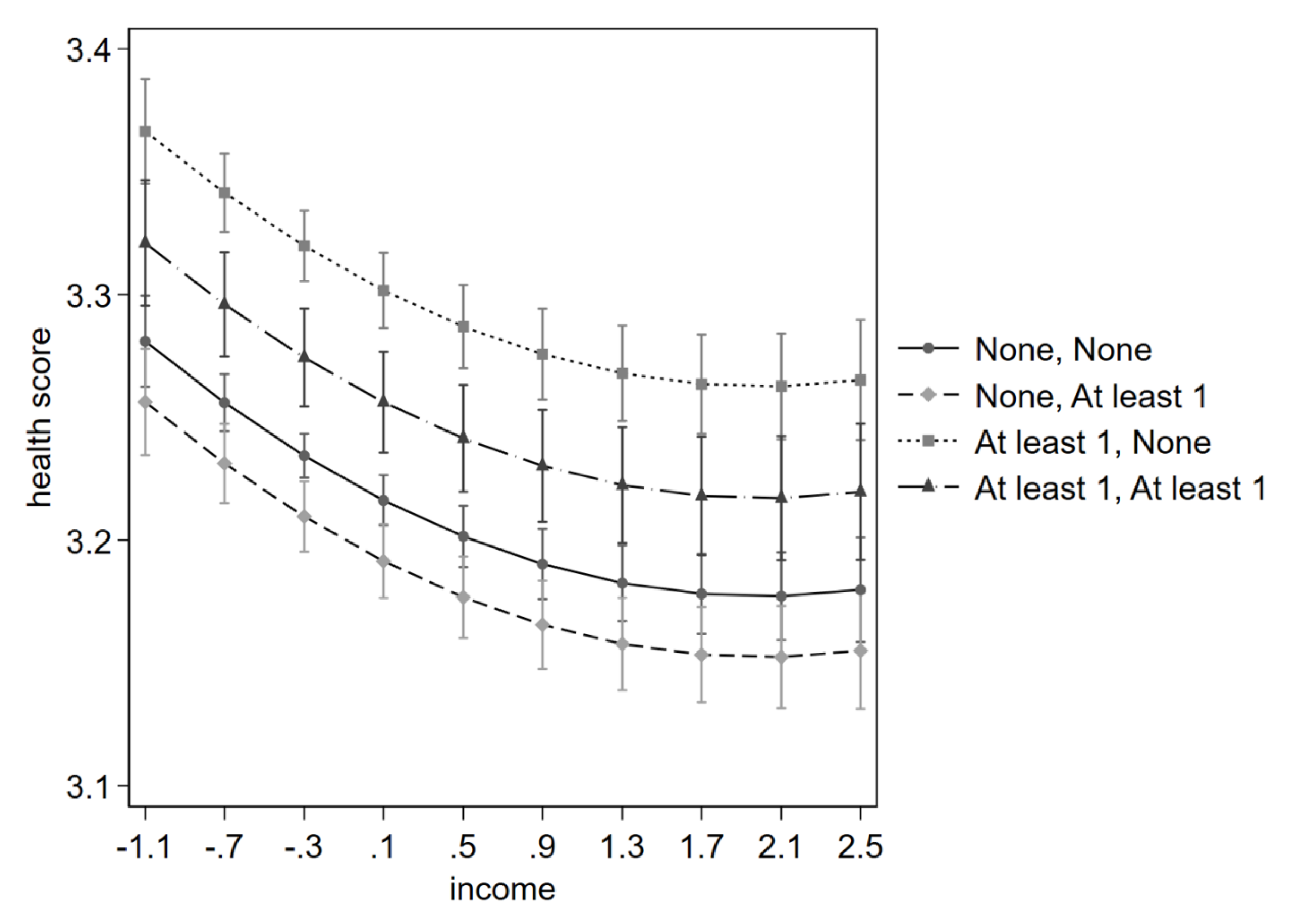
Figure 4 CRE Margins of responses of the self-perceived health score according to income (standardised), visualised in steps of 9,737.517 euro (0.4) from zero (-1.1) to 87,637.651 euro (2.5). Four combinations of receiving and giving help are plotted, each from or to no other, and from or to at least one other. The legend specifies Receiving help and subsequently Giving help.
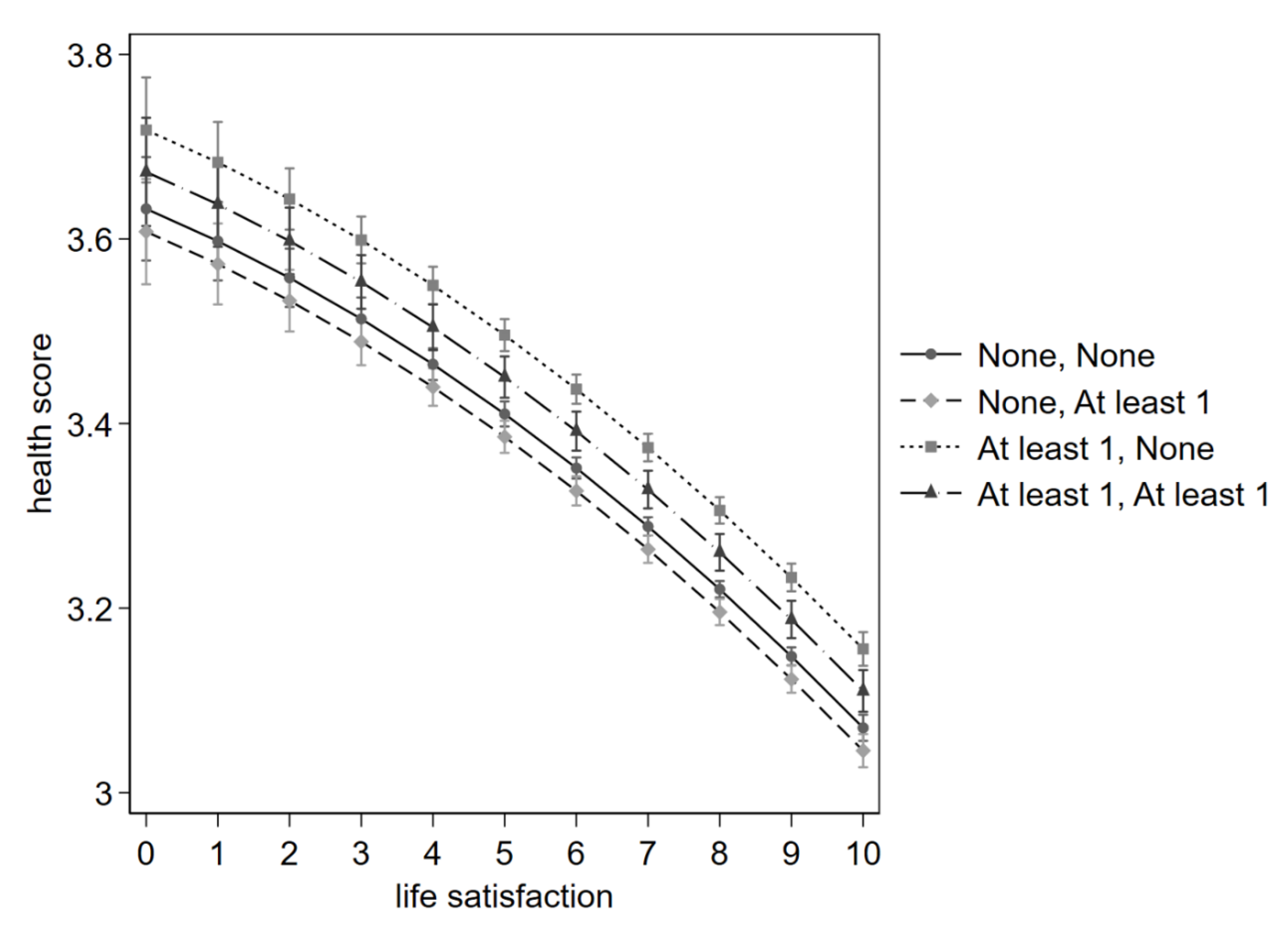
Figure 5 CRE Margins of responses of the self-perceived health score according to the level of life satisfaction, visualised in steps of one from zero to ten. Four combinations of receiving and giving help are plotted, each from or to no other, and from or to at least one other. The legend specifies Receiving help and subsequently Giving help.
Table 8 illustrates that the predictive margins are consistently lower, i.e. reflecting better health status, for those who give help. The predictions are the same across imputed datasets, except for a varying third digit after the decimal point of two coefficients. As expected, receiving help is predicted to relate to a worse health status, i.e. a higher score.
Conclusion
Active ageing reflects a lifestyle which is beneficial for the health of older people. An important aspect of this lifestyle is the act of helping and its contribution to health. This study documents the value of giving help, which appears more beneficial for European older people who also receive help. As such, the act of giving help decreases the odds of reporting a less favourable health status by 17.1 percentage points. This finding suggests seizing the opportunity of stimulating older people who receive help, to also give help. This stimulus can be provided by caretakers, policymakers, family, and the like, as it is expected to improve the self-perceived health status overall.
Statement of funding: The SHARE data collection has been funded by the European Commission, DG RTD through FP5 (QLK6-CT-2001-00360), FP6 (SHARE-I3: RII-CT-2006-062193, COMPARE: CIT5-CT-2005-028857, SHARELIFE: CIT4-CT-2006-028812), FP7 (SHARE-PREP: GA N°211909, SHARE-LEAP: GA N°227822, SHARE M4: GA N°261982, DASISH: GA N°283646) and Horizon 2020 (SHARE-DEV3: GA N°676536, SHARE-COHESION: GA N°870628, SERISS: GA N°654221, SSHOC: GA N°823782, SHARE-COVID-19: GA N°101015924) and by DG Employment, Social Affairs & Inclusion through VS 2015/0195, VS 2016/0135, VS 2018/0285, VS 2019/0332, VS 2020/0313, SHARE-EUCOV: GA N°101052589 and EUCOVII: GA N°101102412. Additional funding from the German Federal Ministry of Research, Technology and Space (01UW1301, 01UW1801, 01UW2202), the Max Planck Society for the Advancement of Science, the U.S. National Institute on Aging (U01_AG09740-13S2, P01_AG005842, P01_AG08291, P30_AG12815, R21_AG025169, Y1-AG-4553-01, IAG_BSR06-11, OGHA_04-064, BSR12-04, R01_AG052527-02, R01_AG056329-02, R01_AG063944, HHSN271201300071C, RAG052527A) and from various national funding sources is gratefully acknowledged (see
www.share-eric.eu).
Materials and Code availability: To provide insight into the longitudinal analysis completed in this article, do- and log-files of Stata are available via
https://github.com/hansgevers/thevalueofahelpinghand.git. Additionally, the illustrations included in this paper, as well as the graphs of the calibrated longitudinal weights versus the design weights per country for imputed dataset one, are available via the hyperlink.
Statement of competing interests: There are no conflicts of interest. The content of this article solely relies on the view of the author.