Submitted:
26 February 2026
Posted:
27 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Participants
2.2. Data Collection
2.3. Assessment of Interleukins
2.4. Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Abbreviations
| ALT | Alanine aminotransferase (Alanina aminotransferasa) |
| APACHE II | Acute Physiology and Chronic Health Evaluation II |
| APTT / aPTT | Activated partial thromboplastin time |
| ARDS | Acute respiratory distress syndrome |
| AST | Aspartate aminotransferase |
| BR | Breathing rate |
| CI | Confidence Interval |
| CK | Creatine kinase |
| COVID-19 | Coronavirus Disease 2019 |
| CRP | C-reactive protein |
| DD | D-dimer (Dímero D) |
| ELISA | Enzyme-linked immunosorbent assay |
| FiO2 | Fraction of inspired oxygen |
| GCP | Good Clinical Practice |
| GGT | Gamma-glutamyl transferase |
| HR | Heart rate |
| ICH | International Conference on Harmonization |
| ICU | Intensive Care Unit |
| IFN-γ | Interferon-gamma |
| IL-1 ra | IL-1 receptor antagonist |
| IL-1β | Interleukin-1beta |
| IL-2 | Interleukin-2 |
| IL-4 | Interleukin-4 |
| IL-6 | Interleukin-6 |
| IL-6Rm | Membrane-bound IL-6 receptors |
| IL-6Rs | Soluble IL-6 receptors |
| IL-7 | Interleukin-7 |
| IL-8 | Interleukin-8 |
| IL-10 | Interleukin-10 |
| IL-11 | Interleukin-11 |
| IL-12 | Interleukin-12 |
| IL-13 | Interleukin-13 |
| IL-17 | Interleukin-17 |
| INR | International normalised ratio |
| LDH | Lactate dehydrogenase |
| MAP | Mean arterial pressure |
| MV / MVD | Mechanical ventilation / Mechanic ventilation days |
| PaFi | PaO2/FiO2 ratio |
| PaO2/FiO2 | Partial pressure of oxygen/Fraction of inspired oxygen |
| PCT | Procalcitonin |
| ROC | Receiver operating characteristic |
| RT-PCR | Real-time reverse transcriptase polymerase chain reaction |
| SARS-CoV-2 | Severe acute respiratory syndrome coronavirus 2 |
| SD | Standard deviation |
| SOFA | Sequential Organ Failure Assessment |
| TGF-ß | Transforming growth factor beta |
| TNF-α | Tumor necrosis factor-alpha |
References
- Wang, H.; Paulson, K.R.; Pease, S.A.; Watson, S.; Comfort, H.; Zheng, P.; Aravkin, A.Y.; Bisignano, C.; Barber, R.M.; Alam, T.; et al. Estimating Excess Mortality Due to the COVID-19 Pandemic: A Systematic Analysis of COVID-19-Related Mortality, 2020–21. Lancet 2022, 399, 1513–1536. [Google Scholar] [CrossRef]
- Barber, R.M.; Sorensen, R.J.D.; Pigott, D.M.; Bisignano, C.; Carter, A.; Amlag, J.O.; Collins, J.K.; Abbafati, C.; Adolph, C.; Allorant, A.; et al. Estimating Global, Regional, and National Daily and Cumulative Infections with SARS-CoV-2 through Nov 14, 2021: A Statistical Analysis. Lancet 2022, 399, 2351–2380. [Google Scholar] [CrossRef] [PubMed]
- Maamar, A.; Guillot, P.; Joussellin, V.; Delamaire, F.; Painvin, B.; Bichon, A.; Jartre, O.B.d.l.; Mauget, M.; Lesouhaitier, M.; Tadié, J.M.; et al. Moderate-to-Severe ARDS: COVID-19 Patients Compared to Influenza Patients for Ventilator Parameters and Mortality. ERJ Open Res. 2023, 9, 00554–2022. [Google Scholar] [CrossRef] [PubMed]
- Auld, S.C.; Harrington, K.R.V.; Adelman, M.W.; Robichaux, C.J.; Overton, E.C.; Caridi-Scheible, M.; Coopersmith, C.M.; Murphy, D.J.; Collaborative, E.C.-19. Trends in ICU Mortality From Coronavirus Disease 2019: A Tale of Three Surges. Crit. Care Med. 2022, 50, 245–254. [Google Scholar] [CrossRef] [PubMed]
- Meyer, N.J.; Gattinoni, L.; Calfee, C.S. Acute Respiratory Distress Syndrome. Lancet 2021, 398, 622–637. [Google Scholar] [CrossRef] [PubMed]
- Kim, J.S.; Lee, J.Y.; Yang, J.W.; Lee, K.H.; Effenberger, M.; Szpirt, W.; Kronbichler, A.; Shin, J.I. Immunopathogenesis and Treatment of Cytokine Storm in COVID-19. Theranostics 2021, 11, 316–329. [Google Scholar] [CrossRef]
- Mehta, P.; McAuley, D.F.; Brown, M.; Sanchez, E.; Tattersall, R.S.; Manson, J.J. COVID-19: Consider Cytokine Storm Syndromes and Immunosuppression. Lancet 2020, 395, 1033–1034. [Google Scholar] [CrossRef]
- Singh, A.K.; Singh, R. Hyperglycemia without Diabetes and New-Onset Diabetes Are Both Associated with Poorer Outcomes in COVID-19. Diabetes Res. Clin. Pract. 2020, 167, 108382. [Google Scholar] [CrossRef]
- Rastad, H.; Ejtahed, H.S.; Shafiee, G.; Safari, A.; Shahrestanaki, E.; Khodaparast, Z.; Hassani, N.S.; Rezaei, M.; Nazari, M.; Zakani, A.; et al. The Risk Factors Associated with COVID-19-Related Death among Patients with End-Stage Renal Disease. BMC Nephrol. 2021, 22, 33. [Google Scholar] [CrossRef]
- Loffi, M.; Piccolo, R.; Regazzoni, V.; Di Tano, G.; Moschini, L.; Robba, D.; Quinzani, F.; Esposito, G.; Franzone, A.; Danzi, G.B. Coronary Artery Disease in Patients Hospitalised with Coronavirus Disease 2019 (COVID-19) Infection. Open Heart 2020, 7, e001428. [Google Scholar] [CrossRef]
- Guan, W.J.; Liang, W.H.; Shi, Y.; Gan, L.X.; Wang, H.B.; He, J.X.; Zhong, N.S. Chronic Respiratory Diseases and the Outcomes of COVID-19: A Nationwide Retrospective Cohort Study of 39,420 Cases. J. Allergy Clin. Immunol. Pract. 2021, 9, 2645–2655. [Google Scholar] [CrossRef]
- Iavarone, M.; D’Ambrosio, R.; Soria, A.; Triolo, M.; Pugliese, N.; Del Poggio, P.; Perricone, G.; Massironi, S.; Spinetti, A.; Buscarini, E.; et al. High Rates of 30-Day Mortality in Patients with Cirrhosis and COVID-19. J. Hepatol. 2020, 73, 1063–1071. [Google Scholar] [CrossRef] [PubMed]
- Mosquera-Sulbaran, J.A.; Pedreañez, A.; Carrero, Y.; Callejas, D. C-Reactive Protein as an Effector Molecule in Covid-19 Pathogenesis. Rev. Med. Virol. 2021, 31*, e2221. [Google Scholar] [CrossRef] [PubMed]
- Zhan, H.; Chen, H.; Liu, C.; Cheng, L.; Yan, S.; Li, H.; Li, Y. Diagnostic Value of D-Dimer in COVID-19: A Meta-Analysis and Meta-Regression. Clin. Appl. Thromb. Hemost. 2021, 27, 10760296211010976. [Google Scholar] [CrossRef]
- Henry, B.M.; Aggarwal, G.; Wong, J.; Benoit, S.; Vikse, J.; Plebani, M.; Lippi, G. Lactate Dehydrogenase Levels Predict Coronavirus Disease 2019 (COVID-19) Severity and Mortality: A Pooled Analysis. Am. J. Emerg. Med. 2020, 38, 1722–1726. [Google Scholar] [CrossRef] [PubMed]
- Penttilä, P.A.; Van Gassen, S.; Panovska, D.; Vanderbeke, L.; Van Herck, Y.; Quintelier, K.; Emmaneel, A.; Filtjens, J.; Malengier-Devlies, B.; Ahmadzadeh, K.; et al. High Dimensional Profiling Identifies Specific Immune Types along the Recovery Trajectories of Critically Ill COVID19 Patients. Cell. Mol. Life Sci. 2021, 78, 3987–4002. [Google Scholar] [CrossRef]
- Groeneveld, P.H.; Kwappenberg, K.M.; Langermans, J.A.; Nibbering, P.H.; Curtis, L. Relation between Pro- and Anti-Inflammatory Cytokines and the Production of Nitric Oxide (NO) in Severe Sepsis. Cytokine 1997, 9, 138–142. [Google Scholar] [CrossRef]
- Chen, L.; Deng, H.; Cui, H.; Fang, J.; Zuo, Z.; Deng, J.; Li, Y.; Wang, X.; Zhao, L. Inflammatory Responses and Inflammation-Associated Diseases in Organs. Oncotarget 2017, 9, 7204–7218. [Google Scholar] [CrossRef]
- Blackwell, T.S.; Christman, J.W. Sepsis and Cytokines: Current Status. Br. J. Anaesth. 1996, 77, 110–117. [Google Scholar] [CrossRef]
- World Medical Association. World Medical Association Declaration of Helsinki: Ethical Principles for Medical Research Involving Human Subjects. JAMA 2013, 310, 2191–2194. [Google Scholar] [CrossRef]
- National Health Commission; National Administration of Traditional Chinese Medicine. Diagnosis and Treatment Protocol for Novel Coronavirus Pneumonia (Trial Version 7). Chin. Med. J. 2020, 133, 1087–1095. [Google Scholar] [CrossRef] [PubMed]
- Vincent, J.L.; Moreno, R.; Takala, J.; Willatts, S.; De Mendonça, A.; Bruining, H.; Reinhart, C.K.; Suter, P.M.; Thijs, L.G. The SOFA (Sepsis-Related Organ Failure Assessment) Score to Describe Organ Dysfunction/Failure. Intensive Care Med. 1996, 22, 707–710. [Google Scholar] [CrossRef] [PubMed]
- Knaus, W.A.; Draper, E.A.; Wagner, D.P.; Zimmerman, J.E. APACHE II: A Severity of Disease Classification System. Crit. Care Med. 1985, 13, 818–829. [Google Scholar] [CrossRef] [PubMed]
- de Alencar, J.C.G.; Moreira, C.L.; Müller, A.D.; Chaves, C.E.; Fukuhara, M.A.; da Silva, E.A.; Miyamoto, M.F.S.; Pinto, V.B.; Bueno, C.G.; Lazar Neto, F.; et al. Double-Blind, Randomized, Placebo-Controlled Trial With N-Acetylcysteine for Treatment of Severe Acute Respiratory Syndrome Caused by Coronavirus Disease 2019 (COVID-19). Clin. Infect. Dis. 2021, 72, e736–e741. [Google Scholar] [CrossRef]
- Taher, A.; Lashgari, M.; Sedighi, L.; Rahimi-Bashar, F.; Poorolajal, J.; Mehrpooya, M. A Pilot Study on Intravenous N-Acetylcysteine Treatment in Patients with Mild-to-Moderate COVID19-Associated Acute Respiratory Distress Syndrome. Pharmacol. Rep. 2021, 73, 1650–1659. [Google Scholar] [CrossRef]
- Siddiqi, H.K.; Mehra, M.R. COVID-19 Illness in Native and Immunosuppressed States: A Clinical-Therapeutic Staging Proposal. J. Heart Lung Transplant. 2020, 39, 405–407. [Google Scholar] [CrossRef]
- Wu, C.; Chen, X.; Cai, Y.; Xia, J.; Zhou, X.; Xu, S.; Huang, H.; Zhang, L.; Zhou, X.; Du, C.; et al. Risk Factors Associated With Acute Respiratory Distress Syndrome and Death in Patients With Coronavirus Disease 2019 Pneumonia in Wuhan, China. JAMA Intern. Med. 2020, 180, 934–943. [Google Scholar] [CrossRef]
- Kishimoto, T. IL-6: From Its Discovery to Clinical Applications. Int. Immunol. 2010, 22, 347–352. [Google Scholar] [CrossRef]
- Steinmetz, H.T.; Herbertz, A.; Bertram, M.; Diehl, V. Increase in Interleukin-6 Serum Level Preceding Fever in Granulocytopenia and Correlation with Death from Sepsis. J. Infect. Dis. 1995, 171, 225–228. [Google Scholar] [CrossRef]
- Hack, C.E.; De Groot, E.R.; Felt-Bersma, R.J.; Nuijens, J.H.; Strack Van Schijndel, R.J.; Eerenberg-Belmer, A.J.; Thijs, L.G.; Aarden, L.A. Increased Plasma Levels of Interleukin-6 in Sepsis. Blood 1989, 74, 1704–1710. [Google Scholar] [CrossRef]
- Hummel, M.; Czerlinski, S.; Friedel, N.; Liebenthal, C.; Hasper, D.; von Baehr, R.; Hetzer, R.; Volk, H.D. Interleukin-6 and Interleukin-8 Concentrations as Predictors of Outcome in Ventricular Assist Device Patients before Heart Transplantation. Crit. Care Med. 1994, 22, 448–454. [Google Scholar] [CrossRef] [PubMed]
- Buck, C.; Bundschu, J.; Gallati, H.; Bartmann, P.; Pohlandt, F. Interleukin-6: A Sensitive Parameter for the Early Diagnosis of Neonatal Bacterial Infection. Pediatrics 1994, 93, 54–58. [Google Scholar] [CrossRef] [PubMed]
- Garbers, C.; Hermanns, H.M.; Schaper, F.; Müller-Newen, G.; Grötzinger, J.; Rose-John, S.; Scheller, J. Plasticity and Cross-Talk of Interleukin 6-Type Cytokines. Cytokine Growth Factor Rev. 2012, 23, 85–97. [Google Scholar] [CrossRef] [PubMed]
- Li, H.; Liu, W.; Xie, J. Circulating Interleukin-6 Levels and Cardiovascular and All-Cause Mortality in the Elderly Population: A Meta-Analysis. Arch. Gerontol. Geriatr. 2017, 73, 257–262. [Google Scholar] [CrossRef]
- Chen, X.; Liu, X.; Dong, R.; Zhang, D.; Qin, S. A Retrospective Observational Study of the Association Between Plasma Levels of Interleukin 8 in 42 Patients with Sepsis-Induced Myocardial Dysfunction at a Single Center Between 2017 and 2020. Med. Sci. Monit. 2021, 27, e933065. [Google Scholar] [CrossRef]
- Zeng, G.; Chen, D.; Zhou, R.; Zhao, X.; Ye, C.; Tao, H.; Sheng, W.; Wu, Y. Combination of C-Reactive Protein, Procalcitonin, IL-6, IL-8, and IL-10 for Early Diagnosis of Hyperinflammatory State and Organ Dysfunction in Pediatric Sepsis. J. Clin. Lab. Anal. 2022, 36, e24505. [Google Scholar] [CrossRef]
- Zhang, X.; Wang, J.; Guo, S. Predictive Value of IL-8 for Mortality Risk in Elderly Sepsis Patients of Emergency Department. Cytokine 2024, 184*, 156774. [Google Scholar] [CrossRef]
- Vahabi, M.; Rostamian, A.; Mirsharif, E.S.; Latifi, K.; Iranparast, S.; Ghazanfari, T. Neutrophil Markers as Predictors of COVID-19 Severity at Hospital Admission: A Cross-Sectional Study. Iran. J. Allergy Asthma Immunol. 2025, 24, 21–30. [Google Scholar] [CrossRef]
- Del Valle, D.M.; Kim-Schulze, S.; Huang, H.H.; Beckmann, N.D.; Nirenberg, S.; Wang, B.; Lavin, Y.; Swartz, T.H.; Madduri, D.; Stock, A.; et al. An Inflammatory Cytokine Signature Predicts COVID-19 Severity and Survival. Nat. Med. 2020, 26, 1636–1643. [Google Scholar] [CrossRef]
- Zhang, W.; Wang, W.; Hou, W.; Jiang, C.; Hu, J.; Sun, L.; Hu, L.; Wu, J.; Shang, A. The Diagnostic Utility of IL-10, IL-17, and PCT in Patients with Sepsis Infection. Front. Public Health 2022, 10, 923457. [Google Scholar] [CrossRef]
- Mauad, T.; Duarte-Neto, A.N.; da Silva, L.F.F.; de Oliveira, E.P.; de Brito, J.M.; do Nascimento, E.C.T.; de Almeida Monteiro, R.A.; Ferreira, J.C.; de Carvalho, C.R.R.; do Nascimento Saldiva, P.H.; et al. Tracking the Time Course of Pathological Patterns of Lung Injury in Severe COVID-19. Respir. Res. 2021, 22, 32. [Google Scholar] [CrossRef]
- Savin, I.A.; Zenkova, M.A.; Sen’kova, A.V. Pulmonary Fibrosis as a Result of Acute Lung Inflammation: Molecular Mechanisms, Relevant In Vivo Models, Prognostic and Therapeutic Approaches. Int. J. Mol. Sci. 2022, 23, 14959. [Google Scholar] [CrossRef]
- Huang, C.; Wang, Y.; Li, X.; Ren, L.; Zhao, J.; Hu, Y.; Zhang, L.; Fan, G.; Xu, J.; Gu, X.; et al. Clinical Features of Patients Infected with 2019 Novel Coronavirus in Wuhan, China. Lancet 2020, 395, 497–506. [Google Scholar] [CrossRef]
- Wu, Z.; McGoogan, J.M. Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72,314 Cases From the Chinese Center for Disease Control and Prevention. JAMA 2020, 323, 1239–1242. [Google Scholar] [CrossRef]
- Zheng, K.I.; Gao, F.; Wang, X.B.; Sun, Q.F.; Pan, K.H.; Wang, T.Y.; Ma, H.L.; Chen, Y.P.; Liu, W.Y.; George, J.; et al. Letter to the Editor: Obesity as a Risk Factor for Greater Severity of COVID-19 in Patients with Metabolic Associated Fatty Liver Disease. Metabolism 2020, 108, 154244. [Google Scholar] [CrossRef]
- Lighter, J.; Phillips, M.; Hochman, S.; Sterling, S.; Johnson, D.; Francois, F.; Stachel, A. Obesity in Patients Younger Than 60 Years Is a Risk Factor for COVID-19 Hospital Admission. Clin. Infect. Dis. 2020, 71, 896–897. [Google Scholar] [CrossRef]
| n = 120 | 1st day median (p25th-p75th) |
3rd day median (p25th-p75th) |
p-value |
|---|---|---|---|
| Age (years) | 63.0 (56.0-72.0) | ||
| ICU stay (days) | 14.0 (9.0-28.0) | ||
| MV (days) | 9.0 (0.0-22.3) | ||
| SOFA (score) | 3.0 (3.0-4.0) | 5.0 (3.0-7.0) | 0.959 |
| APACHE II (score) | 13.0 (8.0-17.0) | ||
| MAP (mmHg) | 98.0 (81.8-110) | 84.0 (75.0-95.8) | 0.095 |
| HR (bpm) | 78.0 (65.0-89.0) | 62.5 (52.3-80.0) | 0.006* |
| BR (rpm) | 27.0 (22.0-30.0) | 22.0 (19.0-24.0) | 0.002* |
| FiO2 (%) | 0.85 (0.70-1.00) | 0.60 (0.50-0.70) | 0.001** |
| PaO2/FiO2 | 149 (100-224) | 200 (131-234) | 0.646 |
| n = 120 | 1st day median (p25th-p75th) |
3rd day median (p25th-p75th) |
P-value) |
|---|---|---|---|
| Biochemical variables | |||
| Sodium (mEq/L) | 139 (137-141) | 140 (137-144) | 0.059 |
| Potassium (mEq/L) | 4.10 (3.70-4.30) | 4.00 (3.70-4.40) | 0.763 |
| Creatinine (mg/dL) | 0.81 (0.72-1.12) | 0.74 (0.63-0.91) | 0.001** |
| ALT (U/L) | 34.5 (23.0-47.5) | 38.0 (25.0-62.8) | 0.001** |
| AST (U/L) | 34.0 (23.0-46.5) | 28.0 (20.0-42.5) | 0.014* |
| GGT (U/L) | 60.0 (40.5-105.3) | 95.5 (58.3-156.0) | 0.001** |
| LDH (U/L) | 495 (414-621) | 435 (352-510) | 0.001** |
| Creatine kinase (U/L) | 76.0 (35.5-141.8) | 39.0 (21.5-105.5) | 0.007* |
| Haematological variables | |||
| Haemoglobin g/dL | 13.5 (11.8-14.5) | 12.6 (11.1-13.7) | 0.001** |
| Haematocrit (%) | 38.8 (34.7-38.8) | 36.8 (33.0-40.2) | 0.001** |
| Leukocytes *103/µL | 9.67 (7.51-13.7) | 8.80 (6.86-11.84) | 0.013* |
| Lymphocytes (%) | 6.00 (3.68-9.03) | 9.15 (5.40-13.83) | 0.001** |
| Neutrophils (%) | 89.9 (86.1-92.8) | 84.4 (77.6-89.9) | 0.001** |
| Platelets *103/µL | 237 (197-295) | 264 (204-343) | 0.001** |
| INR | 1.08 (1.00-1.18) | 1.06 (0.97-1.14) | 0.088 |
| APTT (s) | 28.8 (26.9-32.2) | 28.8 (26.8-31.1) | 0.500 |
| Inflammatory markers | |||
| Fibrinogen (mg/dL) | 678 (541-792) | 573 (403-686) | 0.001** |
| DD (ng/mL) | 980 (553-1633) | 1400 (895-4550) | 0.001** |
| CRP (mg/L) | 131.1 (52.9-187.9) | 64.0 (23.5-122.6) | 0.001** |
| Ferritin (ng/mL) | 1447 (720-2107) | 1333 (740-2419) | 0.028* |
| IL-1β (pg/mL) | 0.51 (0.01-0.95) | 0.46(0.01-0.95) | 0.013* |
| IL-2 (pg/mL) | 0.93 (0.29-1.63) | 1.09 (0.30-1.57) | 0.865 |
| IL-6 (pg/mL) | 44.0 (16.0-105.0) | 47.0 (13.3-141.9) | 0.109 |
| IL-7 (pg/mL) | 2.39 (0.08-7.50) | 2.02 (0.04-7.05) | 0.141 |
| IL-8 (pg/mL) | 53.7 (31.1-102.0) | 69.3 (36.7-129.0) | 0.073 |
| IL-10 (pg/mL) | 43.2 (18.6-81.8) | 27.9 (12.2-49.8) | 0.001** |
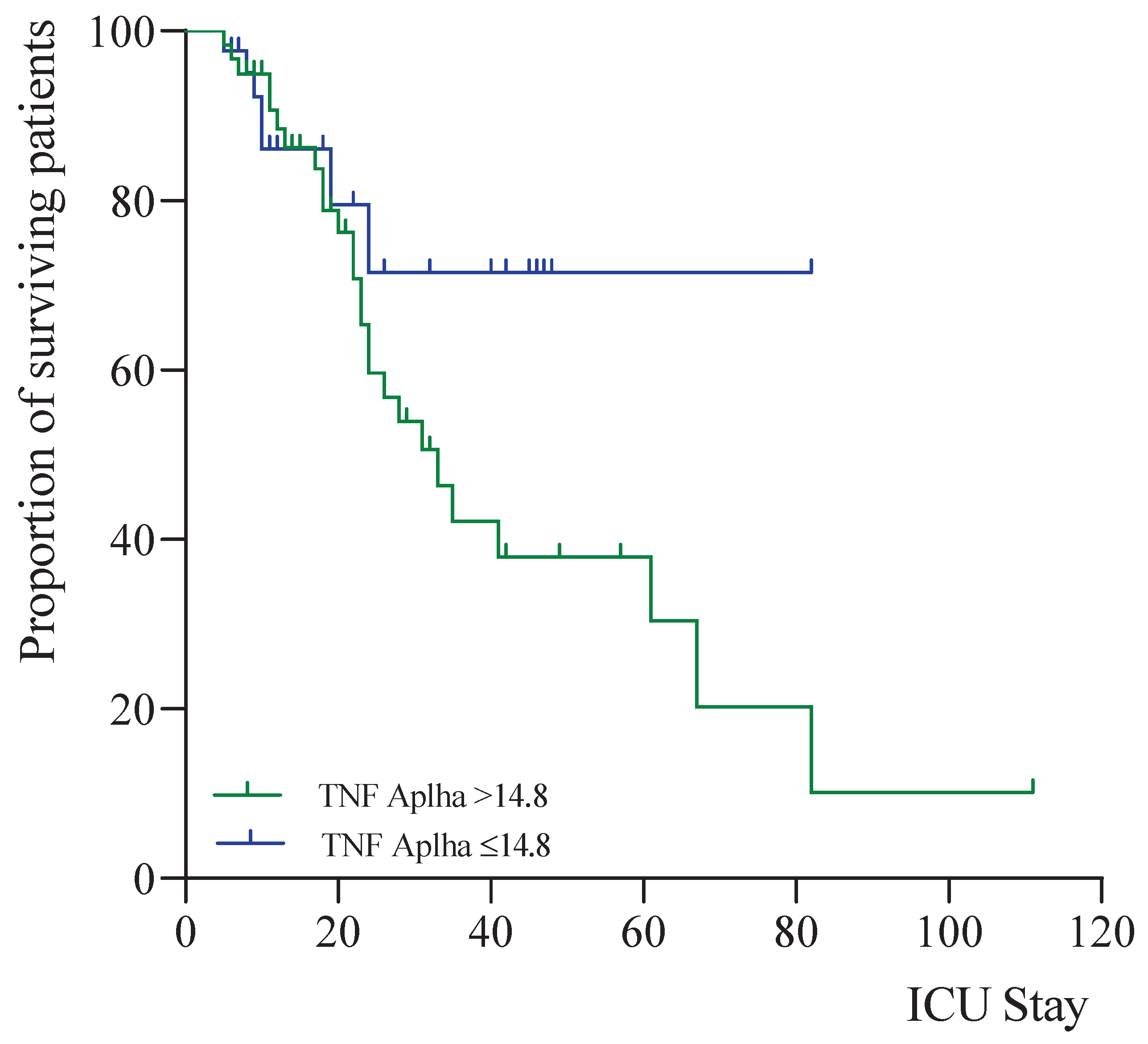
| TNFα (pg/mL) | 14.80 (8.98-23.30) | 19.29 (11.01-31.41) | 0.001** |
| n = 120 | 1st day | 3rd day | ||||
|---|---|---|---|---|---|---|
| Survivors Median (p25th-p75th) |
Deceased Median (p25th-p75th) |
P-value | Survivors Median (p25th-p75th) |
Deceased Median (p25th-p75th) |
P-value | |
| IL-1β (pg/mL) | 0.547 (0.010-1.261) | 0.547 (0.269-0.871) | 0.899 | 0.431 (0.010-0.976) | 0.547 (0.188-1.044) | 0.489 |
| IL-2 (pg/mL) | 1.151 (0.355-1.608) | 1.313 (0.250-1.66) | 0.947 | 1.20 (0.40-1.57) | 1.32 (0.20-1.64) | 0.912 |
| IL-6 (pg/mL) | 34.0 (15.7-87.6) | 69.1 (15.9-203.0) | 0.290 | 59.2 (15.8-172.7) | 24.5 (10.1-66.0) | 0.447 |
| IL-7 (pg/mL) | 2.40 (0.05-6.57) | 2.30 (0.040-10.128) | 0.861 | 1.29 (0.04-6.99) | 3.90 (0.05-7.64) | 0.185 |
| IL-8 (pg/mL) | 51.4 (31.6-86.6) | 63.4 (31.0-162.7) | 0.238 | 59.3 (26.8-107.7) | 103.1 (44.0-144.5) | 0.026* |
| IL-10 (pg/mL) | 34.1 (13.2-62.7) | 52.6 (35.7-124.5) | 0.004* | 19.7 (10.5-40.9) | 43.3 (22.6-97.7) | 0.001** |
| TNFα (pg/mL) | 13.2 (20.4) | 19.0 (12.9-35.6) | 0.003* | 16.1 (10.7-28.0) | 25.5 (16.8-60.5) | 0.004* |
| n = 120 | SOFA | APACHE | MVD | ICU stay | FiO2 | PaFi | |
|---|---|---|---|---|---|---|---|
| 1st day | IL-1β (pg/mL) | -.152 | .028 | -.164 | -.220* | -.052 | .057 |
| IL-2 (pg/mL) | .004 | -.079 | -.123 | -.185 | .088 | -.161 | |
| IL-6 (pg/mL) | .280 | .127 | -.164 | -.200 | .262 | .058 | |
| IL-7 (pg/mL) | -.333* | -.011 | -.082 | -.087 | .164 | -.133 | |
| IL-8 (pg/mL) | .100 | .085 | .085 | -.050 | .032 | -.415* | |
| IL-10 (pg/mL) | .198 | .201 | .198* | .072 | .028 | .070 | |
| TNFα (pg/mL) | .178 | .171 | .222* | .122 | -.172 | -.089 | |
| 3rd day | IL-1β (pg/mL) | -.013 | -.083 | -.136 | .017 | -.205 | |
| IL-2 (pg/mL) | .103 | .070 | -.132 | .002 | -.163 | ||
| IL-6 (pg/mL) | -.999 | -.233 | -.206 | .171 | .097 | ||
| IL-7 (pg/mL) | .626 | -.032 | -.009 | -.013 | -.032 | ||
| IL-8 (pg/mL) | .256 | .276* | .147 | .034 | -.336* | ||
| IL-10 (pg/mL) | .305 | .377** | .289* | -.219* | -.114 | ||
| TNFα (pg/mL) | .274 | .276* | .214* | -.062 | -.114 | ||
| n=120 | Fibrinogen | DD | CRP | Ferritin | |
|---|---|---|---|---|---|
| 1st day | IL-1β (pg/mL) | .005 | -.021 | -.040 | .007 |
| IL-2 (pg/mL) | .059 | -.045 | .072 | .082 | |
| IL-6 (pg/mL) | -.003 | .165 | .138 | .083 | |
| IL-7 (pg/mL) | -.030 | -006 | -.082 | -.186 | |
| IL-8 (pg/mL) | .044 | .202* | .137 | -.093 | |
| IL-10 (pg/mL) | .007 | .189* | .281* | .023 | |
| TNFα (pg/mL) | .139 | .130 | .104 | .053 | |
| 3rd day | IL-1β (pg/mL) | .162 | -.106 | .069 | .053 |
| IL-2 (pg/mL) | -.001 | -.065 | -.022 | .055 | |
| IL-6 (pg/mL) | -.029 | .593* | .261 | .084 | |
| IL-7 (pg/mL) | .024 | -.037 | .059 | -.106 | |
| IL-8 (pg/mL) | .191 | .010 | .334** | .007 | |
| IL-10 (pg/mL) | .148 | .101 | .355** | .059 | |
| TNFα (pg/mL) | .051 | .032 | .121 | .079 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




