Submitted:
17 February 2026
Posted:
26 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. The Core Argument: The Integrated Environmental-Health Accountability Framework (IEHAF)
2.1. Genesis and Positioning of IEHAF
2.2. IEHAF as a Normative Decision Framework
2.3. Moving Beyond Remediation: A Call for Structural Reform
3. The Environmental-to-Health Pathway in Extractive Regions
- i.
- Oil Extraction & Infrastructure Failure: The first stage in the environmental-to-health pathway is the extraction process itself, which includes significant infrastructure failures. Pipeline corrosion, wellhead leakage, and gas flaring are common occurrences that release hazardous substances into the environment. In addition, waste pit overflow often leads to uncontrolled discharges of toxic substances into both land and water systems. These operational failures expose the surrounding environment to chemicals that can persist for long periods, thereby ensuring that communities remain exposed to harmful toxins [27,28,29,30,31,32,33,34,35,36,37]. These pollutants initiate a chain reaction of environmental degradation that ultimately reaches the human population.
- ii.
- Ecological Degradation: Following the initial contamination, ecological degradation occurs through the contamination of groundwater, surface water hydrocarbon loading, and soil toxicity. Biodiversity collapse is another consequence of these pollutants, as aquatic and terrestrial ecosystems are severely affected by the introduction of hydrocarbons, heavy metals, and other toxic chemicals [1,2,3,4,5,6,7,8,9,10,11,12,13,14,15]. These ecological changes are particularly significant in the Niger Delta, where many local communities rely on fishing, agriculture, and water resources for their livelihoods. As Eli et al. [34] highlight, water contamination in particular serves as the central transmission mechanism, linking oil extraction activities to health risks that affect the most vulnerable populations. This environmental degradation sets the stage for a multi-faceted public health crisis, as ecosystems and human health become increasingly interconnected.
- iii.
- Human Exposure Pathways: The next stage in the pathway involves human exposure to contaminants through several key pathways. The most direct and immediate form of exposure is through contaminated drinking water, which is often the primary source of water for many communities in the Niger Delta. Additionally, polluted fisheries and food chains contribute to chronic exposure, as aquatic organisms accumulate contaminants such as petroleum hydrocarbons and heavy metals. Inhalation of flaring emissions from gas flaring and dermal contact during occupational activities in contaminated environments also exacerbate exposure risks. As Saliu et al. [28] point out, these exposure pathways are not merely environmental parameters; they are the core mechanisms through which extractive activities translate into chronic disease burdens, particularly for vulnerable populations who have limited capacity to mitigate exposure.
- iv.
- Health Outcomes: The health consequences of these multiple exposure pathways are far-reaching and multifaceted. Immediate health outcomes include gastrointestinal disorders, caused by the ingestion of contaminated water, and respiratory diseases linked to inhaling the fumes from gas flaring. Over time, exposure to heavy metals such as lead and cadmium can lead to neurological damage, kidney failure, and developmental issues. In addition to these physical health outcomes, there are growing concerns about reproductive and developmental effects in communities living in proximity to extractive operations. As mental health distress rises due to both physical illness and the economic hardships caused by environmental degradation, these health outcomes further compound the vulnerabilities of affected populations [79,80,81,82,83,84,85,86,87,88,89,90,91,92,93,94,95]. Figure 1 provides a visual representation of these interlinked health risks, illustrating how exposure pathways lead to a range of health issues that further strain already fragile healthcare systems.
- v.
- Socioeconomic Feedback: The final stage in the extractive exposure cascade is the socioeconomic feedback loop, where health deterioration is tied directly to economic decline. As livelihoods collapse due to environmental damage and the loss of agricultural and fishing income, affected communities experience escalating food insecurity. This economic decline, coupled with distress migration, which is often a result of the collapse of local economies, leads to broader socioeconomic instability. Reduced productivity, both at the individual and community level, contributes to intergenerational poverty [36,37], as future generations inherit the compounded effects of environmental pollution and health decline. This feedback loop highlights the urgency of addressing environmental degradation as a public health issue, emphasizing that prevention and remediation must be part of a larger strategy for socioeconomic recovery in the Niger Delta [1,2,3,4,5,6,7,8].
4. Multi-Pollutant Exposure and Water Contamination as the Central Health Determinant
5. The Three Core Domains of IEHAF
5.1. Domain I: Environmental Toxicity and Ecological Collapse
5.1.1. Niger Delta-Specific Manifestations
- Persistent groundwater hydrocarbon contamination is one of the most visible signs of extractive industry-related pollution. Oil spills and pipeline leaks result in hydrocarbons seeping into groundwater, rendering it undrinkable and dangerous for both humans and wildlife.
- Heavy metal accumulation in soil and water has also been documented, particularly lead, cadmium, and zinc, which are released into the environment through the flaring of natural gas, improper disposal of toxic waste, and ongoing oil spills. These metals accumulate over time, leading to soil and water toxicity that affects food production, water sources, and overall ecosystem health.
- The loss of mangrove ecosystems is another major consequence, as the mangroves act as vital buffers against storm surges, provide habitats for biodiversity, and contribute to water purification. However, they are being destroyed by oil spills, land reclamation projects, and deforestation.
- Fisheries decline is particularly devastating for communities that rely on fish as their primary food source. Contaminated waterways have caused fish populations to decrease, reducing the availability of both protein and livelihoods for many local people.
5.1.2. Guiding Accountability Questions
- Are water monitoring systems longitudinal and transparent? Ensuring that water quality is consistently monitored over time and that data is made available to the public is crucial for understanding the long-term impacts of contamination.
- Do remediation standards account for cumulative toxicity? Remediation efforts must not only address immediate pollution but also take into account the cumulative effects of long-term exposure to multiple contaminants.
- Is ecosystem restoration linked to health surveillance metrics? Restoration projects should be designed to not only rehabilitate ecosystems but also track their progress in improving health outcomes, such as reductions in waterborne diseases or improvements in food security.
5.2. Domain II: Human Exposure, Vulnerability, and Behavioural Adaptation
5.2.1. Critical Pathways
- Drinking untreated borehole or surface water is one of the most immediate pathways of exposure. Many communities in the Niger Delta rely on groundwater and surface water sources that have been contaminated by oil spills, gas flaring, and other extractive activities.
- Consuming contaminated fish is another direct exposure pathway. The contamination of aquatic ecosystems by petroleum hydrocarbons and heavy metals leads to the bioaccumulation of toxins in fish, which are then ingested by the local population.
- Inhalation of gas flaring emissions exposes nearby communities to toxic gases and particulate matter, leading to chronic respiratory problems.
- Occupational exposure during artisanal activities, such as fishing, farming, and working in contaminated oil fields, increases the likelihood of direct exposure to harmful pollutants.
5.2.2. Amplifiers of Risk
- Weak primary healthcare systems make it difficult for local populations to receive timely diagnosis and treatment for diseases caused by environmental contamination. Without proper healthcare infrastructure, the population is more susceptible to chronic conditions and infections.
- The absence of toxicological screening means that many health issues related to pollution go undiagnosed, and individuals who are exposed to harmful toxins may not receive appropriate treatment or preventative care.
- Socioeconomic constraints limit the ability of local communities to avoid exposure. For example, in many cases, people cannot afford bottled water or water filtration systems, forcing them to rely on contaminated sources.
5.2.3. Guiding Questions
- Are vulnerable groups (pregnant women, children, fisherfolk) systematically screened? Vulnerable groups must be identified and prioritized for health screening to detect early signs of illness due to environmental exposure.
- Is safe water access treated as a health intervention? Access to clean water should be considered a public health intervention, requiring investment in infrastructure and regular water quality assessments.
- How do livelihood losses alter dietary and exposure patterns? Understanding how the collapse of local industries (e.g., fishing) affects dietary habits and exposure to pollutants is essential for developing targeted health interventions.
5.3. Domain III: Institutional Accountability and Policy Inertia
5.3.1. Structural Failures
- Fragmented regulatory oversight exists because multiple agencies are often responsible for regulating environmental health, leading to inconsistencies and inefficiencies in enforcement.
- Weak enforcement mechanisms mean that even when environmental regulations are in place, they are often not adequately enforced, allowing polluting companies to continue harmful practices without consequence.
- Delayed remediation responses have led to a slow recovery from oil spills and other environmental disasters. Despite the evidence of contamination, the process of cleaning up polluted areas is often delayed or inefficient, prolonging exposure for local communities.
- Limited community participation in monitoring results in a lack of local accountability and representation in decision-making processes. Communities should have the right to participate in environmental monitoring and hold both the government and corporations accountable for their actions.
5.3.2. Guiding Questions
- Who bears legal and financial responsibility for long-term health monitoring? Identifying the parties responsible for funding and conducting long-term health surveillance is essential for ensuring that the impacts of contamination are consistently monitored.
- Are health-cost externalities internalized into extractive licensing? Extractive industries must be held accountable for the health costs they impose on local populations, which should be incorporated into the licensing and regulatory framework.
- Is environmental data publicly accessible and independently verified? Transparent access to data is essential for holding companies and regulators accountable. Publicly available, verified environmental data would allow communities to better understand the risks they face and advocate for action.
| Contaminant Category | Primary Extractive Source | Environmental Medium | Exposure Pathway | Biological Mechanism / Toxicodynamics | Documented / Associated Health Effects | Population Groups Most Affected | Long-Term Public Health Implication |
|---|---|---|---|---|---|---|---|
| Petroleum Hydrocarbons (e.g., BTEX, PAHs, TPH) | Oil spills, pipeline leaks, artisanal refining | Surface water, groundwater, sediments | Drinking water, dermal absorption, ingestion of contaminated fish | Lipophilic bioaccumulation; hepatic enzyme disruption; oxidative stress | Gastrointestinal disorders (nausea, vomiting), liver toxicity (hepatocellular damage, cirrhosis), skin rashes, carcinogenic risk (from PAHs) | Fishing communities, children, pregnant women | Long-term liver disease burden, skin cancer incidence, systemic environmental contamination effects |
| Heavy Metals (Pb, Cd, Zn, Hg) | Produced water discharge, oil drilling effluents, soil leaching | Groundwater, surface water, aquatic biota | Drinking water, food chain bioaccumulation (fish, crops) | Lead (Pb) neurotoxicity (blood-brain barrier); Cadmium (Cd) renal tubular damage, zinc bioaccumulation | Neurodevelopmental delay (Pb), renal impairment (Cd), hypertension, reproductive toxicity, gastrointestinal disturbances | Children (neurodevelopment), women of reproductive age (pregnancy, fetal exposure) | Chronic kidney disease prevalence, developmental disabilities, elevated blood pressure rates |
| Combustion By-products (SO2, NOx, PM2.5, Black Carbon) | Gas flaring, petroleum refining | Air, water deposition, soil | Inhalation, ingestion of contaminated rainwater | Pulmonary inflammation; oxidative stress; placental vascular impairment | Respiratory disease (asthma, bronchitis, emphysema), adverse pregnancy outcomes (low birth weight, preterm birth), cardiovascular disease | Infants, elderly, pregnant women, individuals with pre-existing respiratory conditions | Increased maternal-child morbidity and mortality, chronic respiratory disease rates, cardiovascular risks |
| Polycyclic Aromatic Hydrocarbons (PAHs) | Incomplete combustion (oil burning, flaring) | Surface water, food chain, sediment | Ingestion of contaminated fish and shellfish, dermal exposure | DNA adduct formation; mutagenic properties; carcinogenic risk | Carcinogenic risk (skin, lung, bladder cancer), immunotoxicity, oxidative damage | Fishing communities, workers in oil industries | Increased lifetime cancer risk, immune suppression, birth defects linked to PAH exposure |
| Salinity & Total Dissolved Solids (TDS) | Produced water discharge, seawater intrusion, brine from drilling | Groundwater, surface water | Drinking water, irrigation, consumption of contaminated fish | Osmotic imbalance; renal stress; hypertension | Hypertension, dehydration, kidney strain | Rural households, farmers reliant on shallow wells for water | |
| Endocrine Disrupting Chemicals (EDCs) | Petrochemical effluents, industrial additives | Surface water, groundwater | Drinking water, food chain | Hormonal receptor interference, thyroid disruption, gonadal impairment | Fertility issues, menstrual irregularities, developmental abnormalities | Adolescents, women of reproductive age | Long-term reproductive health decline, increase in endocrine-related cancers |
| Microbial Contamination (due to infrastructure damage) | Flooded oil-impacted sites, damaged boreholes | Groundwater, surface water | Oral ingestion | Gastrointestinal infection pathways | Cholera, diarrheal disease, typhoid fever, gastroenteritis | Children under five, immunocompromised individuals | Persistent waterborne diseases, hospital burden, stunted growth and cognitive development in children |
| Cyanides & Chemical Additives | Illegal refining, petrochemical discharges | Surface water, soil | Dermal exposure, oral ingestion | Inhibition of cellular respiration; hypoxia | Acute poisoning symptoms, neurological impairment (headaches, dizziness), dizziness | Local communities near artisanal refineries | Acute toxicity episodes, high emergency care burden |
6. From Exposure to Economic Entrenchment: The Extractive Poverty Loop

- 1.
- Pollution reduces fish catch and crop yield: In regions where local populations rely heavily on fishing and agriculture, contamination of water and soil leads to declining yields. Pollutants such as hydrocarbons, heavy metals, and toxic by-products from gas flaring disrupt aquatic ecosystems, making fishing increasingly unproductive. Similarly, polluted soils, laden with toxic metals, impair crop growth, leading to food insecurity and loss of livelihood [163,164,165,166,167,168,169,170,171,172,173,174,175].
- 2.
- Households incur out-of-pocket medical costs: Health issues resulting from exposure to pollutants, such as gastrointestinal diseases, respiratory illnesses, and neurological impairments, impose heavy financial burdens on households. In many cases, local healthcare systems are weak or nonexistent, forcing families to pay out-of-pocket for medical treatment. This expenditure on healthcare diverts scarce financial resources, further limiting families’ ability to invest in productive activities or escape poverty [85,86,87,88,89,90].
- 3.
- Reduced work capacity lowers income: As health deteriorates from prolonged exposure to environmental contaminants, work capacity diminishes. Workers, particularly those in informal or subsistence sectors like fishing and farming, find themselves unable to maintain full productivity. Illness, particularly chronic conditions resulting from toxic exposure, leads to absenteeism or early retirement, reducing household income and perpetuating the poverty cycle [74,76].
- 4.
- Children withdrawn from school: One of the most devastating effects of poverty exacerbated by pollution is the withdrawal of children from school. Families facing food insecurity, health crises, and economic hardship often prioritize immediate survival over long-term educational goals. As a result, children are taken out of school to help support the household or care for sick relatives, diminishing future prospects and trapping families in a cycle of poverty and low educational attainment. This dynamic has intergenerational consequences, as children who miss education are less likely to break out of the poverty cycle in adulthood [36,37].
- 5.
- Poverty limits exposure avoidance: Finally, poverty itself limits the ability of communities to mitigate exposure to pollutants. In the Niger Delta, many households cannot afford the costs of water filtration, safe housing, or healthcare services that would allow them to avoid exposure to contaminated water or air. Moreover, impoverished households are often forced to rely on contaminated water sources because they lack access to cleaner alternatives. As pollution levels rise and resources become more constrained, the vulnerability to future exposure only increases, perpetuating the cycle.
- 6.
- Cycle repeats: This extractive poverty loop is not only self-reinforcing but also intergenerational. As children grow up in households affected by pollution, poor health, and economic hardship, they inherit the same structural vulnerabilities. The cycle of poverty, poor health, and environmental exposure is thus passed down, making it difficult for affected communities to break free from their current conditions. These dynamic highlights the urgent need for systemic reform to address both environmental and socio-economic inequities.
- 7.
- The Extractive System: Environmental Externalities and Economic Inequity
- 8.
- Logical Pathway: From IEHAF to Action
7. Environmental Surveillance
8. Environmental Impact Assessments (EIAs)
9. Extractive Licensing and Health Liabilities
9.1. IEHAF as an Architectural Blueprint
9.2. The Need for Systemic Reform
10. Discussion
10.1. Navigating Governance Tensions, Power Asymmetries, and Framework Limitations
10.1.1. Navigating Tensions: Environmental vss. Economic Interests
10.1.2. Power Asymmetries and Policy Implementation
10.1.3. Limitations of IEHAF
11. Conclusion & Call to Action
11.1. Reaffirmation of IEHAF’s Urgency
11.2. Audience-Specific Calls to Action
- For policymakers, the time has come to integrate IEHAF principles into environmental regulation. The environmental-health nexus must no longer be an afterthought. We urge policymakers to adopt IEHAF as a foundational framework for extractive industry regulation, ensuring that health outcomes are integrated into licensing agreements and operational standards for oil and gas companies. By doing so, extractive industries would be held accountable not only for environmental damage but also for its direct consequences on public health, encouraging the adoption of sustainable practices that protect both the environment and the people who depend on it. This would also involve mandating environmental and health monitoring as part of any ongoing extractive project to ensure compliance and long-term remediation.
- For health practitioners, we call for the systematic screening of populations for waterborne diseases and other illnesses related to multi-pollutant exposure. These screenings should focus not only on acute conditions but also on the long-term health impacts of chronic exposure to pollutants like hydrocarbons and heavy metals. Furthermore, longitudinal health registries should be developed to track the cumulative health impacts of pollution over time, enabling policymakers to make data-driven decisions that better address public health needs. Health professionals must also advocate for community-based health education programs to raise awareness about pollution-related risks and encourage preventive health measures.
- For researchers, the immediate priority must be the long-term evaluation of IEHAF’s application in real-world contexts. This includes pilot studies in affected communities to assess the framework’s effectiveness in improving health outcomes, environmental quality, and community resilience. Researchers should also engage in cross-disciplinary collaboration to refine IEHAF, ensuring that it can be adapted to other extractive regions worldwide. Collaboration between public health experts, environmental scientists, and social scientists is crucial to fully understanding the interconnections between environmental degradation, public health, and socioeconomic factors. Additionally, researchers should contribute to building local capacity for data collection and analysis, enabling communities to better track their own health and environmental conditions.
- For civil society and community leaders, we call for grassroots environmental monitoring and advocacy efforts to demand greater transparency from both government bodies and extractive corporations regarding their environmental and health liabilities. Local communities must be empowered to take an active role in environmental monitoring, using tools such as community-led water quality assessments, environmental reporting platforms, and litigation to hold companies accountable. Communities must also advocate for better access to healthcare and alternative livelihoods in regions severely impacted by pollution. Transparency and community involvement are essential for creating a more just and equitable system of environmental governance in extractive regions.
12. Recommendations
- i.
- Integration of Environmental Surveillance with Health Monitoring Systems: Policymakers and environmental agencies must establish longitudinal environmental surveillance programs that are directly linked with health data systems. This integration will allow for the real-time monitoring of environmental pollution levels and their corresponding health outcomes. By systematically tracking pollutants such as hydrocarbons and heavy metals in drinking water and food sources, authorities can better understand how long-term exposure impacts public health. This integration should be a priority in the design of public health infrastructures in extractive regions.
- ii.
- Incorporation of Health Metrics into Environmental Impact Assessments (EIAs): It is essential that Environmental Impact Assessments (EIAs) now include projected disease burden metrics, particularly focusing on the public health consequences of pollution exposure. Governments should mandate that extractive companies include health projections as part of their licensing process, ensuring that they account for long-term health risks posed to local populations. This would ensure that potential environmental harms are fully understood and mitigated before projects are approved.
- iii.
- Health Liabilities in Extractive Licensing Agreements: Future extractive industry licensing agreements should incorporate long-term health liabilities for corporations. Companies should be required to establish health compensation funds that provide financial support for communities affected by pollution. This includes coverage for medical expenses related to pollution-induced diseases, as well as health monitoring programs to track the cumulative impacts of contamination over time. Extractive industries should be held accountable for the long-term consequences of their activities on public health, ensuring that they bear the cost of healthcare and environmental restoration.
- iv.
- Strengthening Governance and Accountability Mechanisms: Governments must strengthen regulatory oversight and enforcement mechanisms to hold extractive industries accountable for their environmental and health impacts. This includes regular audits, community-led monitoring systems, and transparency measures that ensure companies follow through on their environmental and health commitments. Community participation in decision-making processes should be prioritized to ensure that affected populations have a voice in the policies that govern their health and environment.
- v.
- Community-Led Environmental Monitoring and Advocacy: Local communities must be empowered through capacity building to take part in environmental monitoring and advocacy. Governments should support grassroots environmental initiatives that focus on water quality monitoring and health assessments, giving local populations the tools to demand accountability from corporations and policymakers. Civil society organizations should also be engaged to amplify community concerns and push for stronger environmental regulations that prioritize public health and sustainability.
13. Health Significance
Author Contributions
Funding
Acknowledgments
Conflicts of Interest
References
- Akayinaboderi, AE; Tano, DA; Okoro, E; Adedoyin, OO; Diagha, ON; Meshach, OO; Ilemi, JS; Tamuno, TT; Igoniama, EG; Charles, O; Perekibina, AB; Douye, PM; Morufu, OR. World Environment Day 2024 Initiatives in Bayelsa State: Promoting Environmental Stewardship and Sustainable Practices—A Collaboration Between Federal University Otuoke, Niger Delta University, and the Nigerian Environmental Society. Advance 2024. [Google Scholar] [CrossRef]
- Ayibatonyo, MN; Ilemi, JS; Igoniama, EG; Akayinaboderi, AE; Morufu, OR. Fecundity Estimation of Atlantic mudskipper Periophthalmus barbarus in Ogbo-Okolo mangrove Forest of Santa Barbara River, Bayelsa State Niger Delta, Nigeria. bioRxiv 2024. [Google Scholar] [CrossRef]
- Ayibatonyo, MN; Bob-Manuel Faye-Ofori, G; Morufu, OR. Food and Feeding of Atlantic Mudskipper Periophthalmus Barbarus in Ogbo-Okolo Mangrove Forest of Santa Barbara River, Bayelsa State Niger Delta, Nigeria; Qeios, 2024. [Google Scholar] [CrossRef]
- Nathaniel, AM; Soberekon, IJ; Gamage, IE; Eli, AA; Raimi, MO. Fecundity insights: the breeding habits of Atlantic mudskippers in Ogbo-Okolo mangrove forest of santa Barbara River, Bayelsa State Niger Delta, Nigeria. Int J Hydro 2025, 9, 27‒33. [Google Scholar] [CrossRef]
- Okoyen, E; Raimi, MO; Omidiji, AO; Ebuete, AW. Governing the Environmental Impact of Dredging: Consequences for Marine Biodiversity in the Niger Delta Region of Nigeria. Insights Mining Science and technology 2020, 2, 555586. Available online: https://juniperpublishers.com/imst/pdf/IMST.MS.ID.555586.pdf. [CrossRef]
- Akayinaboderi, AE; Tano, DA; Okoro, E; Adedoyin, OO; Digha, ON; Meshach, OO; Ilemi, JS; Tamuno, TT; Igoniama, EG; Charles, O; Perekibina, AB; Douye, PM; Morufu, OR. World Environment Day 2024 Initiatives in Bayelsa State: Promoting Environmental Stewardship and Sustainable Practices—A Collaboration Between Federal University Otuoke, Niger Delta University, and the Nigerian Environmental Society. Sustainability in Environment 2025, 10. Available online: www.scholink.org/ojs/index.php/se. [CrossRef]
- Fubara, GE; Dokuboba, A; Ilemi, JS; Esther, OA; Digha, ON; Akayinaboderi, AE; Enyinnaya, O; Igoniama, EG; Ayibatonyo, MN; Morufu, OR. The Niger Delta is Under a Pollution Warning: Hydrocarbon profiles in crude oil polluted soil remediated with Pleurotus ostreatus and Eisenia fitida. bioRxiv 2024. [Google Scholar] [CrossRef]
- Fubara, G.; Amachree, D.; Soberekon, I.; Akhigbe, E.; Nicholas, D.; Eli, A.; Okoro, E.; Gamage, I.; Nathaniel, A.; Raimi, M. From Crisis to Recovery: Addressing Hydrocarbon Pollution in Niger Delta Soils Treated with Pleurotus ostreatus and Eisenia fitida. Open Journal of Yangtze Oil and Gas 2025, 10, 1–29. [Google Scholar] [CrossRef]
- Glory, R; Sylvester, CI; Morufu, OR; AustinAsomeji, I. Public and environmental health implications of artisanal petroleum refining and risk reduction strategies in the Niger Delta region of Nigeria. Journal of Biological Research & Biotechnology 2023, 21, 1836–1851. [Google Scholar] [CrossRef]
- Morufu, OR; Olawale, HS; Clinton, IE. Quality water not everywhere: Exploratory Analysis of Water Quality Across Ebocha-Obrikom Oil and Gas Flaring Area in the Core Niger Delta Region of Nigeria. Preprint 2021. [Google Scholar] [CrossRef]
- Deinkuro, NS; Charles, WK; Raimi, MO; Nimlang, HN. Oil Spills in the Niger Delta Region, Nigeria: Environmental Fate of Toxic Volatile Organics PREPRINT (Version 1) available at Research Square; 2021. [Google Scholar] [CrossRef]
- Olalekan, MR; Olawale, HS; Clinton, IE; Opasola, AO. Quality Water, Not Everywhere: Assessing the Hydrogeochemistry of Water Quality across Ebocha-Obrikom Oil and Gas Flaring Area in the Core Niger Delta Region of Nigeria. Pollution 2022, 8(3), 751–778. [Google Scholar]
- Raimi, M.; Sawyerr, H. Preliminary Study of Groundwater Quality Using Hierarchical Classification Approaches for Contaminated Sites in Indigenous Communities Associated with Crude Oil Exploration Facilities in Rivers State, Nigeria. Open Journal of Yangtze Oil and Gas 2022, 7, 124–148. [Google Scholar] [CrossRef]
- Raimi, MO; Sabinus, CE. Influence of Organic Amendment on Microbial Activities and Growth of Pepper Cultured on Crude Oil Contaminated Niger Delta Soil. International Journal of Economy, Energy and Environment. 2017, Vol. 2(No. 4), 56–76. [Google Scholar] [CrossRef]
- Olalekan, R. M; Dodeye, E. O; Efegbere, H. A; Odipe, O. E.; Deinkuro, N. S; Babatunde, A; Ochayi, E. O. Leaving No One Behind? Drinking-Water Challenge on the Rise in Niger Delta Region of Nigeria: A Review. Merit Research Journal of Environmental Science and Toxicology (ISSN: 2350-2266) 2020, Vol. 6(1), 031–049. [Google Scholar] [CrossRef]
- Suleiman, RM; Raimi, MO; Sawyerr, HO. A Deep Dive into the Review of National Environmental Standards and Regulations Enforcement Agency (NESREA) Act. International Research Journal of Applied Sciences 2019. Available online: https://scirange.com/abstract/irjas.2019.108.125.
- Olalekan, RM; Adedoyin, OO; Ayibatonbira, A; et al. “Digging deeper” evidence on water crisis and its solution in Nigeria for Bayelsa state: a study of current scenario. International Journal of Hydrology 2019, 3(4), 244‒257. [Google Scholar] [CrossRef]
- Morufu, OR; Aziba-anyam, GR; Teddy, CA. ‘Silent Pandemic’: Evidence-Based Environmental and Public Health Practices to Respond to the Covid-19 Crisis. IntechOpen. 2021. Available online: https://www.intechopen.com/online-first/silent-pandemic-evidence-based-environmental-and-public-health-practices-to-respond-to-the-covid-19-. [CrossRef]
- Morufu OR, Aziba-anyam GR, Teddy CA (2021). Evidence-based Environmental and Public Health Practices to Respond to the COVID-19 Crisis, 07 May 2021, PREPRINT (Version 1) available at Research Square [https://doi.org/10.21203/rs.3.rs-504983/v1] https://europepmc.org/article/PPRID/PPR335534; EMSID:EMS123969.
- Elemuwa, C., Ariyo, A., Ogunyemi, B. and Raimi, M. (2025) Invisible Threats, Shared Fates: Strengthening One Health Defenses against Environmental Toxins. Open Journal of Preventive Medicine, 15, 241-272. https://doi.org/10.4236/ojpm.2025.1511014.
- Raimi, M.O., Ezekwe, I.C., Agusomu, T.D., Enyinnaya, O., Amakama, N.J. and German, I.C. (2025) Enhancing Methane Emissions Management in Nigeria’s Oil and Gas Sectors: A Comprehensive Policy and Strategic Framework. Open Journal of Yangtze Oil and Gas, 10, 31-62. https://doi.org/10.4236/ojogas.2025.102002.
- Abiye T, Raimi MO (2025). Assessing groundwater contamination near dumpsites in port Harcourt using water quality index (WQI): insights from seasonal and distance-based variations. Int J Hydro. 2025;9(1):35‒44. https://doi.org/10.15406/ijh.2025.09.00401.
- Enang, OT., Azeez, BO., Ogunyemi, BT., Sulayman, AA., Araromi. DO. and Raimi, MO. (2025) Revolutionizing Hemodialysis Water Quality: Development and Evaluation of TiO2 Nanoparticle-Enhanced Microporous Filters. Advances in Nanoparticles, 14, 12-36. https://doi.org/10.4236/anp.2025.141002. https://www.scirp.org/journal/anp ISSN Online: 2169-0529 ISSN Print: 2169-0510.
- Raimi, MO., Mcfubara, KG., Abisoye, OS., Ifeanyichukwu EC., Henry SO., & Raimi, GA (2021) Responding to the call through Translating Science into Impact: Building an Evidence-Based Approaches to Effectively Curb Public Health Emergencies [COVID-19 Crisis]. Global Journal of Epidemiology and Infectious Disease, 1(1). https://doi.org/10.31586/gjeid.2021.010102. Retrieved from https://www.scipublications.com/journal/index.php/gjeid/article/view/72.
- Raimi MO & Raimi AG (2020). The Toughest Triage in Decision Impacts: Rethinking Scientific Evidence for Environmental and Human Health Action in the Times of Concomitant Global Crises. CPQ Medicine, 11(1), 01-05.
- Raimi MO, Moses T, Okoyen E, Sawyerr HO, Joseph BO, Oyinlola BO (2020) “A Beacon for Dark Times: Rethinking Scientific Evidence for Environmental and Public Health Action in the Coronavirus Diseases 2019 Era” Medical and Research Microbiology, Vol. 1, Issues 3.
- Akhigbe EO, Izah SC, Ogidi OI, Iyingiala A-A, and Raimi MO (2025) The Role of Edible Mushrooms in Immune Support. In: S.C. Izah et al. (eds.), Bioactive Compounds in Edible Mushrooms, Reference Series in Phytochemistry. https://doi.org/10.1007/978-3-031-52642-8_21-1.
- Saliu, A.O., Komolafe, O.O., Bamidele, C.O., Raimi, M.O. (2023). The Value of Biodiversity to Sustainable Development in Africa. In: Izah, S.C., Ogwu, M.C. (eds) Sustainable Utilization and Conservation of Africa’s Biological Resources and Environment. Sustainable Development and Biodiversity, vol 888. Springer, Singapore. https://doi.org/10.1007/978-981-19-6974-4_10.
- Raimi MO, Abiola OS, Atoyebi B, Okon GO, Popoola AT, Amuda-KA, Olakunle L, Austin-AI & Mercy T. (2022). The Challenges and Conservation Strategies of Biodiversity: The Role of Government and Non-Governmental Organization for Action and Results on the Ground. In: Chibueze Izah, S. (eds) Biodiversity in Africa: Potentials, Threats, and Conservation. Sustainable Development and Biodiversity, vol 29. Springer, Singapore. https://doi.org/10.1007/978-981-19-3326-4_18.
- Raimi MO, Austin-AI, Olawale HS, Abiola OS, Abinotami WE, Ruth EE, Nimisingha DS & Walter BO (2022). Leaving No One Behind: Impact of Soil Pollution on Biodiversity in the Global South: A Global Call for Action. In: Chibueze Izah, S. (eds) Biodiversity in Africa: Potentials, Threats and Conservation. Sustainable Development and Biodiversity, vol 29. Springer, Singapore. https://doi.org/10.1007/978-981-19-3326-4_8.
- Christopher OE, Adenike BA, Babatunde TO, Morufu OR (2025). The Silent Poison: National Strategies to Protect Health and Ecosystems from Toxic Threats. Authorea. August 19. https://doi.org/10.22541/au.175562297.78702237/v1.
- Opaminola Nicholas D, Raimi MO (2025) Groundwater Contamination in Bayelsa’s Oil-Producing Communities: Physico-Chemical Quality, WHO Standards, and Health Implications. JMIR Preprints. 24/08/2025:82921. https://doi.org/10.2196/preprints.82921. URL: https://preprints.jmir.org/preprint/82921.
- Tomquin A, Ayotamuno A, Ezekwe IC, Imiete G, Raimi MO (2025) Ten Dumpsites, One Crisis: Geoelectrical Evidence of Widespread Subsurface Contamination and Groundwater Vulnerability in Port Harcourt. JMIR Preprints. https://doi.org/10.2196/preprints.79884. URL: https://preprints.jmir.org/preprint/79884.
- Eli AA, Raimi MO, Amachree D (2025) Evaluating the Role of Marine Protected Areas (MPAs) in Enhancing Biodiversity and Supporting Sustainable Economic Growth in the Blue Economy. JMIR Preprints. 26/03/2025:74970. https://doi.org/10.2196/preprints.74970. URL: https://preprints.jmir.org/preprint/74970.
- Raheem WB, Fadina OO, Idowu OO, Raimi MO, Austin-Asomeji I (2023) The Application of Biomaterials in Ecological Remediation of Land Pollution: Bioremediation of Heavy Metals in Cement Contaminated Soil Using White-Rot Fungus Pleurotus sajor-caju, 11 January 2023, PREPRINT (Version 1) available at Research Square [https://doi.org/10.21203/rs.3.rs-2459820/v1].
- Oweibia M, Elemuwa UG, Akpan E et al. (2024). Analyzing Nigeria’s Journey Towards Sustainable Development Goals: A Comprehensive Review From Inception To Present [version 1; peer review: awaiting peer review]. F1000Research 2024, 13:984 (https://doi.org/10.12688/f1000researtch.148020.1).
- Mordecai O, Uchenna GE, Emma A, Elemuwa TD; Gabriel JO; Egberipou T; Etim EO; Christopher OE; Morufu OR; Anuoluwapo B (2024). Analyzing Nigeria’s Journey Towards Sustainable Development Goals: A Comprehensive Review From Inception to Present. Qeios. https://doi.org/10.32388/8O5QEG.
- Olaniyi Afolabi Opasola; Morufu Olalekan Raimi (2025) From Crisis to Catalyst: Leveraging Public Health Emergencies to Redesign Urban Health Policy in Nigerian Megacities. Oral Presentation Presented at the 3rd Ku8+International Conference, Kwara State University, Malete with the theme “Innovation and Sustainability of Higher Education in a Changing World.”, which held on Wednesday, 6th – Friday 8th August, 2025.
- Henry Olawale Sawyerr; Morufu Olalekan Raimi (2025) Surveillance in the Shadows: Reinventing Community-Based Disease Monitoring Systems in Rural Nigeria. Oral Presentation Presented at the 3rd Ku8+International Conference, Kwara State University, Malete with the theme “Innovation and Sustainability of Higher Education in a Changing World.”, which held on Wednesday, 6th – Friday 8th August, 2025.
- Morufu Olalekan Raimi, Christopher Ononiwu Elemuwa, Teddy Charles Adias, Uchenna Geraldine Elemuwa (2025) Environmental Toxins and Public Health in Sub-Saharan Africa: Unraveling the Invisible Pandemic. Oral Presentation Presented at the 10th International Conference on Health, Medicine and Life Sciences (MEDLIFE2025). (ISBN: 979-8-88599-124-7).
- Yusuf Babatunde Adiama; Morufu Olalekan Raimi; Agbebaku Henry Usiobaifo (2025) Echoes of Outbreaks Past: Rethinking Public Health Preparedness in Sub-Saharan Africa in the Age of Emerging Pandemics. Oral Presentation Presented at the 3rd Ku8+International Conference, Kwara State University, Malete with the theme “Innovation and Sustainability of Higher Education in a Changing World.”, which held on Wednesday, 6th – Friday 8th August, 2025.
- Elemuwa CO, Raimi MO, Ainu M, Adias TC, Ufuoma RS, Elemuwa UG, Oginifolunnia OC, Rath BA, Obermeier PE (2024) Conquering Mpox: A Comprehensive Public Health Strategy for Addressing Mpox and Poxvirus Infections in Nigeria – Understanding Global Trends, Transmission Dynamics, and Effective Prevention and Control Measures in Nigeria. JMIR Preprints. 14/10/2024:67534. https://doi.org/10.2196/preprints.67534. URL: https://preprints.jmir.org/preprint/67534.
- Nimisingha JA, Morufu OR, Lawan MI, Alina P, Anuoluwapo AB, Sarah SJ, Funmilayo AA (2024) Advancements in Disaster Response through Telemedicine and Emergency Medical Operating System (TELEMED-EMOS) Integration: A Narrative Review. Advance. August 20, 2024. https://doi.org/10.31124/advance.172416246.69722926/v1.
- Okechukwu CO, Ainu M, Adias TC, Elemuwa CO, Rotifa SU, Ogbointuwei C, Raimi MO, Oweibia M, Alabo AF, Okoyen E, Appah WW (2024) Evaluating the Impact of Rotavirus Vaccination on Childhood Diarrhea Incidence in Bayelsa State, Nigeria: Achievements, Challenges, and Future Directions. JMIR Preprints. 27/07/2024:64822. https://doi.org/10.2196/preprints.64822. URL: https://preprints.jmir.org/preprint/64822.
- Christopher OE, Muyi A, Teddy CA, Rotifa SU, Oyeyemi AS, Uchenna GE, Ansa H, Oyindiepreye LA, Akinloye BO, Morufu OR (2024) Transforming Primary Healthcare in Nigeria: Enhancing Universal Health Coverage through Strong and Sustainable Primary Healthcare Laboratories. Qeios. https://doi.org/10.32388/74E67L.
- Elemuwa CO, Ainu M, Adias TC, Sunday OA, Ufuoma RS, Elemuwa UG, Christopher O, Raimi MO, Oginifolunnia OC, Oweibia M, Ozoemena OV, Daniel ET (2024) Boosting community engagement: Leveraging the ward health system approach for enhanced HPV vaccination acceptance in Nigeria. [version 1; peer review: awaiting peer review]. F1000Research 2024, 13:1392. (https://doi.org/10.12688/f1000research.153919.1).
- Kwen K-I, Eli AA, Morufu OR. (2024). Making the Invisible Visible: The Effects of Gas Flaring on Artisanal Fisheries in the Down-Stream Area of Taylor Creek, Bayelsa State, Nigeria. Qeios. https://doi.org/10.32388/UIM59Z.
- Keme-Iderikumo K, Augustus EA, Raimi MO (2025). Unveiling the impact: gas flaring on artisanal fisheries in Taylor creek, Bayelsa state, Nigeria. Int J Hydro. 2024;8(6):235‒248. https://doi.org/10.15406/ijh.2024.08.00395.
- Evans FG, Nkalo UH, Amachree D, Raimi MO (2024). From Killer to Solution: Evaluating Bioremediation Strategies on Microbial Diversity in Crude Oil-Contaminated Soil over Three to Six Months in Port Harcourt, Nigeria. Adv Environ Eng Res 5(4): 023;. https://doi.org/10.21926/aeer.2404023.
- Olalekan AS, Adewoye SO, Henry SO, Olaniyi OA, Raimi MO (2023). Comprehensive understanding of hydrogeochemical evaluation of seasonal variability in groundwater quality dynamics in the gold mining areas of Osun state, Nigeria. Int J Hydro. 2023;7(5):206‒220. https://doi.org/10.15406/ijh.2023.07.00359.
- Jacob OA, Anuoluwa OE and Raimi MO (2023) The notorious daredevils: potential toxic levels of cyanide and heavy metals in cassava flour sold in selected markets—taken Oke Ogun Community, Oyo State as an example. Front. Sustain. Food Syst. 7:1165501. https://doi.org/10.3389/fsufs.2023.1165501. http://journal.frontiersin.org/article/10.3389/fsufs.2023.1165501/full?&utm_source=Email_to_authors_&utm_medium=Email&utm_content=T1_11.5e1_author&utm_campaign=Email_publica.
- Raimi, MO., Oyeyemi, AS., Mcfubara, KG., Richard, GT., Austin-Asomeji, I., Omidiji, AO. (2023). Geochemical Background and Correlation Study of Ground Water Quality in Ebocha-Obrikom of Rivers State, Nigeria. Trends Appl. Sci. Res, 18(1), 149-168. https://doi.org/10.17311/tasr.2023.149.168.
- Olalekan RM, Bukola RW, Omowunmi FO, Omowumi IO, Iyingiala A-A (2023). The application of biomaterials in ecological remediation of land pollution: bioremediation of heavy metals in cement contaminated soil using white-rot fungus Pleurotus. sajor-caju. J Environ Chem Toxicol;7(1):1-6.
- Stephen OA, Olayinka AS, Olawale HS, Olalekan RM (2023). Comparative Assessment of Seasonal Variations in the Quality of Surface Water and Its Associated Health Hazards in Gold Mining Areas of Osun State, South-West Nigeria. Adv Environ Eng Res; 4(1): 011;. https://doi.org/10.21926/aeer.2301011.
- Oshatunberu, MA., Oladimeji, A., Sawyerr, OH., & Raimi, MO. (2023). Searching for What You Can’t See—Evaluation of Pesticide Residues in Grain Sold at Selected Markets of Southwest Nigeria. Current Research in Public Health, 3(1), 10–36. Retrieved from https://www.scipublications.com/ journal/index.php/crph/article/vie w/566.
- Ifeanyichukwu CE, Christian LO, Morufu OR, Iyingiala AA (2022) Hydrocarbon-Based Contaminants in Drinking Water Sources and Shellfish in the Soku Oil and Gas Fields of South-South Nigeria. Open Journal of Yangtze Gas and Oil, 7, ISSN Online: 2473-1900 ISSN Print: 2473-1889. https://doi.org/10.4236/ojogas.2022.74012. https://www.scirp.org/journal/ojogas.
- Asiegbu OV, Ezekwe IC, Raimi MO (2022). Assessing pesticides residue in water and fish and its health implications in the Ivo river basin of South-eastern Nigeria. MOJ Public Health. 2022;11(4):136‒142. https://doi.org/10.15406/mojph.2022.11.00390.
- Clinton-Ezekwe IC, Osu IC, Ezekwe IC, Raimi MO (2022). Slow death from pollution: potential health hazards from air quality in the mgbede oil fields of south-south Nigeria. Open Access J Sci. 2022;5(1):61‒69. https://doi.org/10.15406/oajs.2022.05.00177.
- Olalekan MR, Albert O, Iyingiala AA, Sanchez DN, Telu M (2022) An environmental/scientific report into the crude oil spillage incidence in Tein community, Biseni, Bayelsa state Nigeria. J Environ Chem Toxicol. 2022;6(4):01-06.. https://doi.org/10.37532/pulject.2022.6(4);01-06.
- Raimi, O., Ezekwe, C., Bowale, A. and Samson, T. (2022) Hydrogeochemical and Multivariate Statistical Techniques to Trace the Sources of Ground Water Contaminants and Affecting Factors of Groundwater Pollution in an Oil and Gas Producing Wetland in Rivers State, Nigeria. Open Journal of Yangtze Oil and Gas, 7, 166-202. https://doi.org/10.4236/ojogas.2022.73010.
- Raimi OM, Sawyerr OH, Ezekwe CI, Gabriel S (2022) Many oil wells, one evil: comprehensive assessment of toxic metals concentration, seasonal variation and human health risk in drinking water quality in areas surrounding crude oil exploration facilities in rivers state, Nigeria. International Journal of Hydrology. 2022;6(1):23‒42. https://doi.org/10.15406/ijh.2022.06.00299.
- Hussain MI, Morufu OR, Henry OS (2021). Probabilistic Assessment of Self-Reported Symptoms on Farmers Health: A Case Study in Kano State for Kura Local Government Area of Nigeria. Environmental Analysis & Ecology Studies 9(1). EAES. 000701. 2021. https://doi.org/10.31031/EAES.2021.09.000701. Pp. 975- 985. ISSN: 2578-0336.
- Afolabi AS, Raimi MO (2021) When Water Turns Deadly: Investigating Source Identification and Quality of Drinking Water in Piwoyi Community of Federal Capital Territory, Abuja Nigeria. Online Journal of Chemistry, 2021, 1, 38-58;. https://doi.org/10.31586/ojc.2021.010105. www.scipublications.org/journal/index.php/ojc.
- Olalekan MR, Abiola I, Ogah A, Dodeye EO (2021) Exploring How Human Activities Disturb the Balance of Biogeochemical Cycles: Evidence from the Carbon, Nitrogen and Hydrologic Cycles. Research on World Agricultural Economy. Volume 02, Issue 03. https://doi.org/10.36956/rwae.v2i3.426. http://ojs.nassg.org/index.php/rwae.
- Raimi, OM., Samson, TK., Sunday, AB., Olalekan, AZ., Emmanuel, OO., & Jide, OT. (2021). Air of Uncertainty from Pollution Profiteers: Status of Ambient Air Quality of Sawmill Industry in Ilorin Metropolis, Kwara State, Nigeria. Research Journal of Ecology and Environmental Sciences, 1(1), 17–38. https://doi.org/10.31586/rjees.2021.010102. Retrieved from https://www.scipublications.com/journal/index.php/rjees/article/view/60.
- Hussain MI, Morufu OR, Henry OS (2021) Patterns of Chemical Pesticide Use and Determinants of Self-Reported Symptoms on Farmers Health: A Case Study in Kano State for Kura Local Government Area of Nigeria. Research on World Agricultural Economy. Vol 2, No. 1. https://doi.org/10.36956/rwae.v2i1.342.http://ojs.nassg.org/index.php/rwae/issue/view/31.
- Hussain MI, Morufu OR, Henry OS (2021) Probabilistic Assessment of Self-Reported Symptoms on Farmers Health: A Case Study in Kano State for Kura Local Government Area of Nigeria. Research on World Agricultural Economy. Vol 2, No. 1. https://doi.org/10.36956/rwae.v2i1.336. http://ojs.nassg.org/index.php/rwae-cn/article/view/336/pdf.
- Morufu OR, Tonye VO, Ogah A, Henry AE, Abinotami WE (2021) Articulating the effect of Pesticides Use and Sustainable Development Goals (SDGs): The Science of Improving Lives through Decision Impacts. Research on World Agricultural Economy. Vol 2, No. 1. https://doi.org/10.36956/rwae.v2i1.347. http://ojs.nassg.org/index.php/rwae/issue/view/31.
- Isah, HM., Sawyerr, HO., Raimi, MO., Bashir, BG., Haladu, S. & Odipe, OE. (2020). Assessment of Commonly Used Pesticides and Frequency of Self-Reported Symptoms on Farmers Health in Kura, Kano State, Nigeria. Journal of Education and Learning Management (JELM), HolyKnight, vol. 1, 31-54. doi.org/10.46410/jelm.2020.1.1.05. https://holyknight.co.uk/journals/jelm-articles/.
- Olalekan RM, Muhammad IH, Okoronkwo UL, Akopjubaro EH (2020). Assessment of safety practices and farmer’s behaviors adopteisad when handling pesticides in rural Kano state, Nigeria. Arts & Humanities Open Access Journal. 2020;4(5):191‒201. https://doi.org/10.15406/ahoaj.2020.04.00170.
- Isah HM, Raimi MO, Sawyerr HO, Odipe OE, Bashir BG, Suleiman H (2020) Qualitative Adverse Health Experience Associated with Pesticides Usage among Farmers from Kura, Kano State, Nigeria. Merit Research Journal of Medicine and Medical Sciences (ISSN: 2354-323X) Vol. 8(8) pp. 432-447, August, 2020. https://doi.org/10.5281/zenodo.4008682.https://meritresearchjournals.org/mms/content/2020/August/Isah%20et%20al.htm.
- Raimi MO, Adio ZO, Odipe OE, Timothy KS, Ajayi BS & Ogunleye Temitope J (2020) Impact of Sawmill Industry on Ambient Air Quality: A Case Study of Ilorin Metropolis, Kwara State, Nigeria. Energy and Earth Science Vol. 3, No. 1, 2020. URL:. https://doi.org/10.22158/ees.v3n1p1. www.scholink.org/ojs/index.php/ees ISSN 2578-1359 (Print) ISSN 2578-1367 (Online).
- Raimi MO, Adeolu AT, Enabulele CE, Awogbami SO (2018) Assessment of Air Quality Indices and its Health Impacts in Ilorin Metropolis, Kwara State, Nigeria. Science Park Journals of Scientific Research and Impact Vol. 4(4), pp. 060-074, September 2018 ISSN 2315-5396. https://doi.org/10.14412/SRI2018.074.http://www.scienceparkjournals.org/sri/pdf/2018/September/Olalekan_et_al.pdf.http://www.scienceparkjournals.org/sri/Content/2018/September/2018.htm.
- Perekibina AB, Charles O, Morufu OR (2025). Beyond Compliance: Evaluating Environmental Standards for oil Spills and their implications for Environmental Protection in the Niger Delta, Nigeria. Authorea. October 13, 2025.DOI: 10.22541/au.176038620.00516100/v1.
- Agusomu TD, Ohwo O, Raimi MO (2025). Living with the waters: perception, adaptation, and policy implications of flooding in Yenagoa metropolis, Nigeria. Open Access J Sci. 2025;8(1):117‒131. https://doi.org/10.15406/oajs.2025.08.00254.
- Anthony BP, Charles O, Raimi MO (2025) Black Gold, Empty Plates: How Oil and Gas Are Destroying Food Security in the Niger Delta. JMIR Preprints. 13/05/2025:77458. https://doi.org/10.2196/preprints.77458. URL: https://preprints.jmir.org/preprint/77458.
- Morufu OR, Christopher O, Emeka CL, Ebikapaye O, Alabo AF (2022) Beyond Palliatives: Responding to the Current Flooding and Preventing the Next One from Kogi to Bayelsa State. Bayelsa State Judiciary Magazine. 4th Edition.
- Morufu OR, Ebikapaye O, Tuebi M, Aziba-anyam GR, Adedoyin OO, Aishat FA, Mariam OR, Beatrice OJ (2021) Do Weak Institutions Prolong Crises? [#ENDSARs] in the Light of the Challenges and opportunities beyond COVID-19 Pandemic and the Next Normal in Nigeria. Communication, Society and Media. ISSN 2576-5388 (Print) ISSN 2576-5396 (Online) Vol. 4, No. 2. https://doi.org/10.22158/csm.v4n2p1. http://www.scholink.org/ojs/index.php/csm/article/view/3790.
- Tinimoye, M.; Raimi, M. O.; Daberechi, A (2026). Urban-Rural Disparities in Primary Healthcare Service Delivery and Implications for Sustainable Development Goal 3 in Southern Nigeria. Preprints 2026, 2026010828. https://doi.org/10.20944/preprints202601.0828.v1.
- Oyibo C, Authority B, Eze C, Morufu OR (2025). Physicochemical and Microbiological Assessment of Sachet Water Stored Under Different Conditions in Yenagoa Metropolis, Nigeria. Authorea. January 07, 2026. https://doi.org/10.22541/au.176781783.37074336/v1.
- Ayodele Jacob Omotoso, Tope Isaac Akinwumi, Elizabeth Anuoluwa Omotoso, Morufu Olalekan Raimi, Stephen Olalekan Awogbami (2025). Analytical Evaluation of Antibiotic Residues in Fish Tissues, Pond Water, and Sediment in Selected Fish Pond Ecosystems in Osun State, Nigeria. Authorea. December 15, 2025. https://doi.org/10.22541/au.176582224.41821315/v1.
- Iyoha OW, Omotoso AJ, Usiobaifo BE, Raimi MO, Ofor TN (2025) Beyond the Tap: Water Insecurity, Environmental Contamination, and Health Inequities in Uselu, Benin City. JMIR Preprints. 01/11/2025:86938. https://doi.org/10.2196/preprints.86938. URL: https://preprints.jmir.org/preprint/86938.
- Omotoso AJ, Ojile MO, Morufu OR (2025). Uncovering the Hidden Burden: Water, Sanitation, and Hygiene (WaSH) Gaps and Their Impact on Health and Learning Outcomes in Secondary Schools, Ede South LGA, Nigeria. Authorea. October 13, 2025. https://doi.org/10.22541/au.176038377.77904469/v1.
- Adindu IB, Ubouh EA, Obasi KO, Raimi MO (2025). Automobile Spray Paint Dust and Human Health: A Multi-Site Environmental Health Risk Assessment of Carcinogenic and Non-Carcinogenic Effects in South-Eastern Nigeria. Authorea. October 13, 2025. https://doi.org/10.22541/au.176038621.14623228/v1.
- Oginifolunnia OC, Elemuwa CO, Adias TC, Raimi MO, Angalabiri C (2025) Bridging the Gaps: Unveiling Weaknesses in Disease Surveillance During Mass Immunization Campaigns in Nigeria JMIR Preprints. 04/07/2025:80148. https://doi.org/10.2196/preprints.80148. URL: https://preprints.jmir.org/preprint/80148.
- Abdulraheem AF, Ononokpono DN, Raimi MO (2025a) Breaking Barriers: How Socio-Demographic, Cultural, and Geographic Factors Shape Skilled Birth Attendance in Nigeria – A Call for Equity and Empowerment. JMIR Preprints. 25/05/2025:78050. URL: https://preprints.jmir.org/preprint/78050.
- Abdulraheem AF, Raimi MO, Ononokpono DN (2025b) Who Delivers Safely? The Hidden Role of Transport and Education in Nigeria’s Maternal Health Crisis. JMIR Preprints. 21/06/2025:79460. https://doi.org/10.2196/preprints.79460. URL: https://preprints.jmir.org/preprint/79460.
- Adias LT, Raimi AaG, Raimi MO (2025) Breaking the Silence on Workplace Stress: Scalable HRM Solutions for Mental Health in Nigeria’s Evolving Workforce. JMIR Preprints. 19/05/2025:77758. https://doi.org/10.2196/preprints.77758. URL: https://preprints.jmir.org/preprint/77758.
- Promise VI, Alabere I, Abdulraheem I, Raimi MO (2025) The Effect of Mobile Phone and Home Visit on Childhood Vaccination Uptake in Rural Communities of Bayelsa State Nigeria. A Pragmatic Cluster Randomized Control Trial. JMIR Preprints. 01/04/2025:75332. https://doi.org/10.2196/preprints.75332. URL: https://preprints.jmir.org/preprint/75332.
- Ibrahim ML, Sawyerr HO, Opasola OA, Adiama YB, Raimi MO (2025) Bridging Knowledge and Practice Gaps in Lassa Fever Prevention: Awareness, Attitudes, and Infection Control Measures Among Healthcare Workers and Residents in Edo, Ondo, and Kwara States. JMIR Preprints. 30/03/2025:75233. https://doi.org/10.2196/preprints.75233. URL: https://preprints.jmir.org/preprint/75233.
- Abiye T, Raimi MO (2025) Unlocking the Secrets Beneath: Utilizing the Water Quality Index (WQI) to Assess Groundwater Contamination Near Dumpsites – A Case Study of Port Harcourt. JMIR Preprints. https://doi.org/10.2196/preprints.73643. URL: https://preprints.jmir.org/preprint/73643.
- Enang OT, Azeez BO, Ogunyemi BT, Sulayman AA, Araromi DO, Raimi MO (2025) Innovative Water Purification for Hemodialysis: TiO2 Nanoparticle-Based Microporous Filter Development and Analysis. JMIR Preprints. 27/01/2025:71835. https://doi.org/10.2196/preprints.71835. URL: https://preprints.jmir.org/preprint/71835.
- Raimi MO, Ezekwe IC, Agusomu TD, Enyinnaya O, Amakama NJ, German IC (2024) Institutional Framework for Methane Emissions Reduction in Nigeria: Policy Insights and Implementation Strategies. JMIR Preprints. 28/10/2024:68103. https://doi.org/10.2196/preprints.68103. URL: https://preprints.jmir.org/preprint/68103.
- Awogbami SO, Ogunyemi O, Adebayo PA, Raimi MO (2024) Protecting the Health of Black Communities: Assessing the Impact of Environmental Hazards from Gold Mining Activities on Health Outcomes among Residents of Osun State, Nigeria. JMIR Preprints. 15/09/2024:66508. https://doi.org/10.2196/preprints.66508. URL: https://preprints.jmir.org/preprint/66508.
- Tano DA, Odafivwotu O, Morufu OR (2024). Residents’ Perception and Adjustment to Floods in Yenagoa Metropolis, Nigeria. Advance. September 12. https://doi.org/10.31124/advance.172611915.58295101/v1.
- Abaya ST, Ogoina D, Stow J, Abaye BB, Emeka C, Raimi MO (2024) Beyond the Epidemic: Effective Public Health Strategies in Response to Nigeria’s First Lassa Fever Outbreak in a Non-Endemic Region. JMIR Preprints. 19/08/2024:65539. https://doi.org/10.2196/preprints.65539 URL: https://preprints.jmir.org/preprint/65539.
- Omoyajowo, K.; Ogunyebi, A.; Ogunkanmi, A.; Njoku, K.; Omoyajowo, K.; Oludoye, O.; Gupta, J.; Raimi, M (2024). Empirical Study of Ecological Innovation and Occupational Health Hazard among Nigerian Paddy Rice Farmers: Response to Potential Field Contamination and Climate Risks. Preprints, 2024080683. https://doi.org/10.20944/preprints202408.0683.v1.
- Clinton-Ezekwe I, Raimi MO, Ezekwe IC, Osu CI, Ordinioha B (2024) Ensuring Safety: Groundwater Quality and Its Potential Health Effects in the Mgbede Oil Fields Environment of South-South Nigeria. JMIR Preprints. 14/07/2024:64294. https://doi.org/10.2196/preprints.64294. URL: https://preprints.jmir.org/preprint/64294.
- Omoyajowo, K., Omoyajowo, K., Akinola, A., Ogunyebi, A., Alao, R., Makinde, O., Orekoya, O., Makengo, B. M., Akinola, O., Jatau, S. S., Kakwi, J. D., Ukoh, S. N. B., & Raimi, M. O. (2024). Genetically Modified Foods: Victoria Islanders’ Perspectives on the Common Good. Preprints. https://doi.org/10.20944/preprints202407.0454.v1.
- Fubara GE, Ukoima HN, Dokuboba A, Morufu OR (2024). Evaluating Bioremediation Strategies on Microbial Diversity in Crude Oil-Contaminated Soil Over Three to Six Months in Port Harcourt, Nigeria., 14 May 2024, PREPRINT (Version 1) available at Research Square. https://doi.org/10.21203/rs.3.rs-4409893/v1.
- Raimi MO, Bilewu OO, Adio ZO, Abdulrahman H (2019) Women Contributions to Sustainable Environments in Nigeria. Journal of Scientific Research in Allied Sciences. 5(4), 35-51. ISSN NO. 2455-5800. DOI No. 10.26838/JUSRES.2019.5.4.104.
- Raimi MO, Suleiman RM, Odipe OE, Salami JT, Oshatunberu M, et al. (2019). Women Role in Environmental Conservation and Development in Nigeria. Ecology & Conservation Science; 1(2):. https://doi.org/10.19080/ECOA.2019.01.555558. Volume 1 Issue 2 - July 2019. https://juniperpublishers.com/ecoa/pdf/ECOA.MS.ID.555558.pdf.
- Raimi MO, Odubo TR, Ogah A (2022) Women, Water and Development in the Global South. Oral Presentation Presented at the Multidisciplinary International Conference on Water in Africa (ICWA 2022) on the theme: Towards Successful Delivery of SDGs 3 & 6, which held February 09–11, 2022.
- Raimi MO, Odubo TR, Odubo TV, Omidiji AO (2022) Gender and Sustainability in the Niger Delta. Oral Presentation Presented at the Multidisciplinary International Conference on Water in Africa (ICWA 2022) on the theme: Towards Successful Delivery of SDGs 3 & 6, which held February 09–11, 2022.
- Raimi, MO, Pigha, Tarilayun K and Ochayi, E. O (2017). Water-Related Problems and Health Conditions in the Oil-Producing Communities in Central Senatorial District of Bayelsa State. Imperial Journal of Interdisciplinary Research (IJIR) Vol-3, Issue-6, ISSN: 2454-1362.
- Raimi MO and Sabinus CE (2017) An Assessment of Trace Elements in Surface and Ground Water Quality in the Ebocha-Obrikom Oil and Gas Producing Area of Rivers State, Nigeria. International Journal for Scientific and Engineering Research (Ijser): Volume 8, Issue 6, July Edition. ISSN: 2229-5518.
- Olalekan, RM., Omidiji, AO., Nimisngha, D., Odipe, OE. and Olalekan, AS. (2018). Health Risk Assessment on Heavy Metals Ingestion through Groundwater Drinking Pathway for Residents in an Oil and Gas Producing Area of Rivers State, Nigeria. Open Journal of Yangtze Gas and Oil, 3, 191-206. https://doi.org/10.4236/ojogas.2018.33017.
- Premoboere EA and Raimi MO (2018). Corporate Civil Liability and Compensation Regime for Environmental Pollution in the Niger Delta. International Journal of Recent Advances in Multidisciplinary Research Vol. 05, Issue 06, pp. 3870-3893, June, 2018.
- Olalekan RM, Vivien O. T, Adedoyin O. O, et al. (2018). The sources of water supply, sanitation facilities and hygiene practices in oil producing communities in central senatorial district of Bayelsa state, Nigeria. MOJ Public Health. 2018;7(6):337‒345. https://doi.org/10.15406/mojph.2018.07.00265.
- Odipe OE, Raimi MO, Suleiman F (2018). Assessment of Heavy Metals in Effluent Water Discharges from Textile Industry and River Water at Close Proximity: A Comparison of Two Textile Industries from Funtua and Zaria, North Western Nigeria. Madridge Journal of Agriculture and Environmental Sciences. 2018; 1(1): 1-6. https://doi.org/10.18689/mjaes-1000101. https://madridge.org/journal-of-agriculture-and-environmental-sciences/mjaes-1000101.php.
- Henry OS, Odipe EO, Olawale SA, Raimi MO (2019) Bacteriological Assessment of Selected Hand Dug Wells in Students’ Residential Area: A Case Study of Osun State College of Health Technology, Ilesa, Nigeria. Global Scientific Journal, Volume 7, Issue 1, January 2019, Online: ISSN 2320-9186. www.globalscientificjournal.com.
- Raimi MO, Abdulraheem AF, Major I, Odipe OE, Isa HM, Onyeche C (2019). The Sources of Water Supply, Sanitation Facilities and Hygiene Practices in an Island Community: Amassoma, Bayelsa State, Nigeria. Public Health Open Access 2019, 3(1): 000134. ISSN: 2578-5001. https://doi.org/10.23880/phoa-16000134.
- Oluwaseun EO., Raimi MO, Nimisingha DS, Abdulraheem AF, Okolosi-PE, Habeeb Modupe Lateefat and Mary Fadeyibi (2019) Assessment of Environmental Sanitation, Food Safety Knowledge, Handling Practice among Food Handlers of Bukateria Complexes in Iju Town, Akure North of Ondo-State, Nigeria. Acta Scientific Nutritional Health 3.6 (2019): 186-200. https://doi.org/10.31080/ASNH.2019.03.0308.
- Raimi MO, Omidiji AO, Adeolu TA, Odipe OE and Babatunde A (2019) An Analysis of Bayelsa State Water Challenges on the Rise and Its Possible Solutions. Acta Scientific Agriculture 3.8 (2019): 110-125. https://doi.org/10.31080/ASAG.2019.03.0572.
- Gift RA, Olalekan RM (2020). Access to electricity and water in Nigeria: a panacea to slow the spread of Covid-19. Open Access J Sci. 2020;4(2):34. https://doi.org/10.15406/oajs.2020.04.00148. https://medcrave.com/index.php?/articles/det/21409/.
- Gift RA, Olalekan RM, Owobi OE, Oluwakemi RM, Anu B, Funmilayo AA (2020). Nigerians crying for availability of electricity and water: a key driver to life coping measures for deepening stay at home inclusion to slow covid-19 spread. Open Access Journal of Science. 2020;4(3):69‒80. https://doi.org/10.15406/oajs.2020.04.00155.
- Omoyajowo, KO; Raimi, MO; Omoyajowo, KA; Makengo, MB; Adegboyo, S; Innocent, DC; Oni, S; Oguntuyi, J; Oyediran, A; Ogunyebi, A; Kakwi, D (2024). Towards a Reduced Pollution Society: Systematic Review on the Role of Storytelling, Social Media, Humor and Celebrities’Influence for Research Communication. J. Appl. Sci. Environ. Manage. 28 (2) 603-623. https://doi.org/10.4314/jasem.v28i2.34. https://www.ajol.info/index.php/jasem/article/view/266677.
- Morufu Raimi and Clinton Ezekwe (2017), Assessment of Trace Elements in Surface and Ground Water Quality (2017) LAP Lambert Academic Publishing. Mauritius. ISBN: 978-3-659-38813-2. www.omniscriptum.com.
- Raimi, MO., Sawyerr, HO., Ezekwe, IC., & Gabriel, S. (2022). Toxicants in Water: Hydrochemical Appraisal of Toxic Metals Concentration and Seasonal Variation in Drinking Water Quality in Oil and Gas Field Area of Rivers State, Nigeria. In P. H. Saleh, & P. A. I. Hassan (Eds.), Heavy Metals - New Insights [Working Title]. IntechOpen. https://doi.org/10.5772/intechopen.102656. ISBN 978-1-80355-526-3.
- Elemuwa CO, Raimi MO, Elemuwa UG, Adias TC (2024) Decoding E. coli O157:H7: Insights from DNA Sequencing and Phylogenetic Analysis for Enhanced Public Health Strategies. JMIR Preprints. 26/12/2024:70605. https://doi.org/10.2196/preprints.70605. URL: https://preprints.jmir.org/preprint/70605.
- Rauf, YO., & Raimi, MO. (2023). Wastes, Wastes, Everywhere Not A Place to Breathe: Redressing and Undressing Ilorin and Yenagoa City. AfricArXiv. https://doi.org/10.21428/3b2160cd.52bfd7dd.
- Raufu, YO., Olayinka, AS., Raimi, MO., Olawale, SH., & Olabisi, OL. (2023). Assessment of occupational risks of waste scavenging in Ilorin metropolis. AfricArXiv. https://doi.org/10.21428/3b2160cd.ffbb315b.
- Kader, S.; Raimi, MO.; Spalevic, V.; Austin-Asomeji, I.; Raheem, WB. (2023) A Concise Study on Essential Parameters for the Sustainability of Lagoon Waters in Terms of Scientific Literature. Preprints, 2023030099. https://doi.org/10.20944/preprints202303.0099.v1.
- Modupe AO, Adebayo O, Sawyerr OH, Opasola AO, Morufu OR (2022) Moving from Total Concentrations to Measures of Harm in Grain Sold at Selected Markets of Southwest Nigeria. medRxiv 2022.12.18.22283634;. https://doi.org/10.1101/2022.12.18.22283634.
- Modupe AO, Adebayo O, Sawyerr OH, Morufu OR (2022) Searching for What You Can’t See - Evaluation of Pesticide Residues in Grain Sold at Selected Markets of Southwest Nigeria. medRxiv 2022.12.09.22283068;. https://doi.org/10.1101/2022.12.09.22283068.
- Stephen OA, Solomon OA, Henry OS, Afolabi OO, Morufu OR (2022) Comprehensive Understanding of Hydrogeochemical evaluation of seasonal variability in groundwater quality Dynamics in the Gold Mining Areas of Osun State, Nigeria. medRxiv 2022.11.06.22282015;. https://doi.org/10.1101/2022.11.06.22282015.
- Awogbami SO, Solomon OA, Sawyerr OH et al. (2022) Comparative Assessment of Seasonal Variations in the Quality of Surface water and its associated health hazards in Gold Mining Areas of Osun State, South-West Nigeria. Preprint (Version 1) available at Research Square [https://doi.org/10.21203/rs.3.rs-2245715/v1]. 07 November 2022.
- Yusuf OR, Adewoye SO, Sawyerr HO, Morufu OR (2022) Incidence of Hepatitis B and C Viruses among the Scavengers in Kwara State, Nigeria. medRxiv preprint. https://doi.org/10.1101/2022.01.26.22269849.
- Morufu OR, Clinton IE, Bowale A (2021) Statistical and Multivariate Techniques to Trace the Sources of Ground Water Contaminants and Affecting Factors of Groundwater Pollution in an Oil and Gas Producing Wetland in Rivers State, Nigeria. medRxiv 2021.12.26.21268415;. https://doi.org/10.1101/2021.12.26.21268415.
- Morufu OR, Henry OS, Clinton IE, Gabriel S (2021) Many Oil Wells, One Evil: Potentially toxic metals concentration, seasonal variation and Human Health Risk Assessment in Drinking Water Quality in Ebocha-Obrikom Oil and Gas Area of Rivers State, Nigeria. medRxiv 2021.11.06.21266005;. https://doi.org/10.1101/2021.11.06.21266005.
- Afolabi AS, Morufu OR (2021) Investigating Source Identification and Quality of Drinking Water in Piwoyi Community of Federal Capital Territory, Abuja Nigeria., 20 July 2021, PREPRINT (Version 1) available at Research Square [https://doi.org/10.21203/rs.3.rs-736140/v1].
- Omotoso AJ, Omotoso EA, Morufu OR (2021) Potential Toxic levels of Cyanide and Heavy Metals in Cassava Flour Sold in Selected Markets in Oke Ogun Community, Oyo State, Nigeria, 01 July 2021, PREPRINT (Version 1) available at Research Square [https://doi.org/10.21203/rs.3.rs-658748/v1].
- Morufu R, Timothy KS, Ajayi BS et al. (2021). Air of Uncertainty from pollution profiteers: Status of ambient air quality of sawmill industry in Ilorin Metropolis, Kwara State, Nigeria, 25 February 2021, PREPRINT (Version 1) available at Research Square [https://doi.forg/10.21203/rs.3.rs-270757/v1].
- Nicholas, D.O. and Raimi, M.O. (2025). Silent Contamination Beneath: Groundwater Quality, Health Risks, and Policy Implications in Bayelsa’s Oil-Producing Communities. Open Journal of Physical Chemistry, 15, 41-73. https://doi.org/10.4236/ojpc.2025.153004.
- Abiye T, Ayotamuno A, Ezekwe IC, Raimi MO (2025). Mapping leachate migration and groundwater risk in Port Harcourt: geoelectrical insights from ten open dumpsites. Open Access J Sci. 2025;8(1):187‒201. https://doi.org/10.15406/oajs.2025.08.00263.
- Christopher Ononiwu Elemuwa, Morufu Olalekan Raimi, Uchenna Geraldine Elemuwa, Teddy Charles Adias (2025). Genomic and Phylogenetic Analysis of E. coli O157:H7: Towards Improved Surveillance and Public Health Response. Nature and Trends in Science and Technology, 1(1). https://doi.org/10.69798/71081461.
- Yusuf OR, Opasola OA, Adewoye SO, Raimi OM and Balogun EM (2023) Assessment of Occupational Risks of Wastes Scavenging in Ilorin Metropolis. J of Agri Earth & Environ mental Sciences 2(3), 01-08.
- Modupe AO, Adebayo O, Sawyerr OH, Opasola Afolabi Olaniyan, Morufu Olalekan Raimi (2023) Concentrations of Pesticides Residues in Grain Sold at Selected Markets of Southwest Nigeria. Natural Resources for Human Health. 1-15 https://doi.org/10.53365/nrfhh/171368. eISSN: 2583-1194.
- Kader, S; Raimi, MO; Spalevic, V; Iyingiala, A-A; Bukola, RW; Jaufer, L; and Butt, TE. (2023) “A concise study on essential parameters for the sustainability of Lagoon waters in terms of scientific literature,” Turkish Journal of Agriculture and Forestry: Vol. 47: No. 3, Article 3. https://doi.org/10.55730/1300-011X.3087. Available at: https://journals.tubitak.gov.tr/agriculture/vol47/iss3/3.
- Adiama, YB., Sawyerr, OH., Olaniyi, OA., Fregene, AF., Alabede, M., & Raimi, MO. (2022). Assessment of Microbiological Quality of Ready to Eat Food Served in Ships Along Warri, Koko and Port Harcourt Water Ways, Nigeria. Online Journal of Microbiological Research, 1(1), 1–7. Retrieved from https://www.scipublications.com/journal/index.php/ojmr/article/view/230.
- Lateefat HM, Faith A, Yusuf AB and Raimi OM (2022) Food for the Stomach Nourishing our Future: Assessment of Potassium Bromate in Local and Packaged Bread Sold in Ilorin Metropolis. Public H Open Acc, 6(1):. https://doi.org/10.23880/phoa-16000197 Medwin Publishers ISSN: 2578-5001.
- Habeeb ML, Opasola AO, Garba M, Olalekan MR. (2022). A Wake-Up Call: Determination of Antibiotics Residue Level in Raw Meat in Abattoir and Selected Slaughterhouses in Five Local Government in Kano State, Nigeria. J Vet Heal Sci, 3(1), 54-61.
- Morufu OR, Tonye VO & Adedoyin OO (2021) Creating the Healthiest Nation: Climate Change and Environmental Health Impacts in Nigeria: A Narrative Review. Scholink Sustainability in Environment. ISSN 2470-637X (Print) ISSN 2470-6388 (Online) Vol. 6, No. 1, 2021 www.scholink.org/ojs/index.php/se. URL:. https://doi.org/10.22158/se.v6n1p61.http://www.scholink.org/ojs/index.php/se/article/view/3684.
- Raimi MO (2025e). Peer Review Report For: Development of a Health Impact Assessment Implementation Model: Enhancing Intersectoral Approaches in Tackling Health Inequalities- A Mixed Methods Study Protocol [version 3; peer review: 2 approved, 1 approved with reservations]. HRB Open Res 2025, 7:14 (https://doi.org/10.21956/hrbopenres.15466.r45418). https://hrbopenresearch.org/articles/7-14/v3#referee-response-45418.
- Raimi MO, Ihuoma BA, Esther OU, Abdulraheem AF, Opufou T, Deinkuro NS, Adebayo PA and Adeniji AO (2020) “Health Impact Assessment: Expanding Public Policy Tools for Promoting Sustainable Development Goals (SDGs) in Nigeria”. EC Emergency Medicine and Critical Care 4.9 (2020).
- Adedoyin OO, Olalekan RM, Olawale SH, et al. (2020). A review of environmental, social and health impact assessment (Eshia) practice in Nigeria: a panacea for sustainable development and decision making. MOJ Public Health. 2020;9(3):81‒87. https://doi.org/10.15406/mojph.2020.09.00328. https://medcraveonline.com/MOJPH/MOJPH-09-00328.pdf.
- Ajayi FA, Raimi MO, Steve-Awogbami OC, Adeniji AO, Adebayo PA (2020) Policy Responses to Addressing the Issues of Environmental Health Impacts of Charcoal Factory in Nigeria: Necessity Today; Essentiality Tomorrow. Communication, Society and Media. Vol 3, No 3. https://doi.org/10.22158/csm.v3n3p1. http://www.scholink.org/ojs/index.php/csm/article/view/2940.
- Olalekan RM, Oluwatoyin OA, Olawale SH, Emmanuel OO, Olalekan AZ (2020) A Critical Review of Health Impact Assessment: Towards Strengthening the Knowledge of Decision Makers Understand Sustainable Development Goals in the Twenty-First Century: Necessity Today; Essentiality Tomorrow. Research and Advances: Environmental Sciences. 2020(1): 72-84. https://doi.org/10.33513/RAES/2001-13. https://ospopac.com/journal/environmental-sciences/early-online.
- Olalekan RM, Oluwatoyin O and Olalekan A (2020) Health Impact Assessment: A tool to Advance the Knowledge of Policy Makers Understand Sustainable Development Goals: A Review. ES Journal of Public Health; 1(1); 1002. https://escientificlibrary.com/public-health/in-press.php.
- Raimi MO, Omidiji AO, Adio ZO (2019) Health Impact Assessment: A Tool to Advance the Knowledge of Policy Makers Understand Sustainable Development Goals. Conference paper presented at the: Association for Environmental Impact Assessment of Nigeria (AEIAN) On Impact Assessment: A Tool for Achieving the Sustainable Development Goals in Nigeria, 7th and 8th November, 2019 in University of Port Harcourt. https://doi.org/10.13140/RG.2.2.35999.51366 https://www.researchgate.net/publication/337146101.
- Omidiji AO and Raimi MO (2019) Practitioners Perspective of Environmental, Social and Health Impact Assessment (ESHIA) Practice in Nigeria: A Vital Instrument for Sustainable Development. Paper Presented at the Association for Environmental Impact Assessment of Nigeria (AEIAN) On Impact Assessment: A Tool for Achieving the Sustainable Development Goals in Nigeria, 7th and 8th November, 2019 In University of Port Harcourt. https://aeian.org/wp-content/uploads/2019/08/EIA-Presentations-Portharcourt.pdf.
- Ojile Meshach Owhotemu, Morufu Olalekan Raimi (2025) Harnessing Health Impact Assessment and Artificial Intelligence for Sustainable Policy Implementation in Nigeria: A Community-Engaged Case Study. Oral Presentation Presented at the ACS-FUO Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Harnessing Green Chemistry & Artificial Intelligence for Sustainable Development, which held Tuesday, 4th - Thursday 7th November, 2025. Pg. 96.
- Raimi MO & Odubo TR (2022) Dutch Diseases and Resources Curse: Key Regulatory Challenges and Opportunities Associated with Extractive Industries in Nigeria. 8th National Conference on Political Stability, Security and Economic Development. Merit House, Abuja-Nigeria. 21st - 22nd July 2022.
- Tomquin Abiye, Morufu Olalekan Raimi, Charles Oyibo (2025) A Predictive Analytics Framework for Water-Land Resource Conflict and Public Health Risk Mitigation in Nigeria. Oral Presentation Presented at the ACS-FUO Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Harnessing Green Chemistry & Artificial Intelligence for Sustainable Development, which held Tuesday, 4th - Thursday 7th November, 2025. Pg. 121.
- Adindu Ihuoma Blossom, Raimi Morufu Olalekan (2025) Occupational Exposure to Volatile Organic Compounds and Heavy Metals in Automobile Spray Painting: A Health Risk Assessment in Imo State, Nigeria. Oral Presentation Presented at the ACS-FUO Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Harnessing Green Chemistry & Artificial Intelligence for Sustainable Development, which held Tuesday, 4th - Thursday 7th November, 2025. Pg. 122.
- Raimi MO (2019) 21st Century Emerging Issues in Pollution Control. 6th Global Summit and Expo on Pollution Control May 06-07, 2019 Amsterdam, Netherlands.
- Raimi MO, Tonye VO, Omidiji AO, Oluwaseun EO (2018) Environmental Health and Climate Change in Nigeria. World Congress on Global Warming. Valencia, Spain. December 06-07, 2018.
- Raimi MO, Clinton IE, Olawale HS (2021) Problematic Groundwater Contaminants: Impact of Surface and Ground Water Quality on the Environment in Ebocha-Obrikom Oil and Gas Producing Area of Rivers State, Nigeria. Oral Presentation Presented at the United Research Forum. 2nd International E-Conference on Geological and Environmental Sustainability during July 29-30, 2021.
- Raimi MO, Sawyerr HO and Isah HM (2020) Health risk exposure to cypermethrin: A case study of kano state, Nigeria. Journal of Agriculture. 7th International Conference on Public Healthcare and Epidemiology. September 14-15, 2020 | Tokyo, Japan.
- Abdulsalam RR; Ayibatonyo MN; Emmanuel GE; Karibi EI; Morufu OR (2025) Enhancing Agricultural Sustainability Through Biotechnology and Biodiversity Conservation. Oral Presentation Presented at the 1st International Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Revolutionizing a Sustainable Tomorrow: Harnessing Science, Innovation and Community Power to Drive Circular Economy Solutions, Climate Resilience, and a Thriving Green Economy, which held Tuesday, 4th–Friday 7th March, 2025. Pp. 76.
- Christopher OE; Morufu OR; Teddy CA; Uchenna GE (2025) Biotechnology, Agriculture, and Biodiversity: A Tripartite Approach to Achieving Sustainable Development Goals in Nigeria. Oral Presentation Presented at the 1st International Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Revolutionizing a Sustainable Tomorrow: Harnessing Science, Innovation and Community Power to Drive Circular Economy Solutions, Climate Resilience, and a Thriving Green Economy, which held Tuesday, 4th–Friday 7th March, 2025. Pp. 23.
- Christopher OE; Morufu OR; Teddy CA; Uchenna GE (2025) Impact of Climate Change on Public Health in Rural Areas of the South-South Region of Nigeria and the Digital Citizen Science Observatories Laboratory Intervention. Oral Presentation Presented at the 1st International Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Revolutionizing a Sustainable Tomorrow: Harnessing Science, Innovation and Community Power to Drive Circular Economy Solutions, Climate Resilience, and a Thriving Green Economy, which held Tuesday, 4th–Friday 7th March, 2025. Pp. 62.
- Tamaraukepreye CO, Adams OI, Bukola OA, Ayotunde SK, Sylvester CI, Morufu OR, and Matthew CO (2024) Socioeconomic Values of Herbal Medicine. In: Izah, S.C., Ogwu, M.C., Akram, M. (eds), Herbal Medicine Phytochemistry, Reference Series in Phytochemistry, Springer, Cham. https://doi.org/10.1007/978-3-031-21973-3_1-1.
- Sylvester CI, Odangowei IO, Matthew CO, Saoban SS, Zaharadeen MY, Muhammad A, Morufu OR, and Austin-Asomeji I (2023) Historical Perspectives and Overview of the Value of Herbal Medicine. In: Izah, S.C., Ogwu, M.C., Akram, M. (eds), Herbal Medicine Phytochemistry, Reference Series in Phytochemistry, Springer, Cham. https://doi.org/10.1007/978-3-031-21973-3_1-1.
- Morufu OR (2021). “Self-reported Symptoms on Farmers Health and Commonly Used Pesticides Related to Exposure in Kura, Kano State, Nigeria”. Annals of Community Medicine & Public Health. 1(1): 1002. http://www.remedypublications.com/open-access/self-reported-symptoms-on-farmers-health-and-commonly-used-pesticides-related-6595.pdf. http:weak//www.remedypublications.com/annals-of-community-medicine-public-health-home.php.
- Raimi MO, Ochayi EO, Babatunde A, Okolosi-Patani IE, Oluwaseun EO, Adio ZO and Bilewu OO (2019) “Environmental Ethics Relevance to Public Health: Current Narratives and Implications for Policy”. EC Emergency Medicine and Critical Care 3.12:01-09.
- Ebuete AW, Raimi MO, Ebuete IY & Oshatunberu M (2019) Renewable Energy Sources for the Present and Future: An Alternative Power Supply for Nigeria. Energy and Earth Science. Vol. 2, No. 2, 2019. URL:. https://doi.org/10.22158/ees.v2n2p18. http://www.scholink.org/ojs/index.php/ees/article/view/2124.
- Odubo TR and Raimi MO (2019) Resettlement and Readjustment Patterns of Rural Dwellers During and After Flood Disasters in Bayelsa State Nigeria. British Journal of Environmental Sciences Vol .7, No .3, Pp. 45-52, July 2019. www.eajournals.org.
- Sawyerr OH, Odipe OE, Olalekan RM, et al. (2018) Assessment of cyanide and some heavy metals concentration in consumable cassava flour “lafun” across Osogbo metropolis, Nigeria. MOJ Eco Environ Sci. 2018;3(6):369‒372. https://doi.org/10.15406/mojes.2018.03.00115.
- Adeolu T, Odipe OE and Raimi MO (2018). Practices and Knowledge of Household Residents to Lead Exposure in Indoor Environment in Ibadan, Oyo State, Nigeria. Journal of Scientific Research & Reports 19(6): 1-10, 2018; Article NO. JSRR.43133 ISSN: 2320-0227.
- Raimi MO, Omidiji AO, Abdulraheem AF, Ochayi EO (2018) A Survey of Hand Washing Behaviour and Awareness among Health Care Workers in Health Care Facilities in Kubwa District of Bwari Area Council, F.C.T. Abuja, Nigeria. Annals of Ecology and Environmental Science Volume 2, Issue 2, 2018, PP 1-18.
- Agbebeku Henry Usiobaifo, Morufu Olalekan Raimi, Anthony Olusoji Ayeleso (2025) Integrative OMICS for Sustainability: Advancing Environmental Bioremediation and Public Health through Systems Biology. Oral Presentation Presented at the ACS-FUO Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Harnessing Green Chemistry & Artificial Intelligence for Sustainable Development, which held Tuesday, 4th - Thursday 7th November, 2025. Pg. 105.
- Tano Dumoyei Agusomu, Digha Opaminola Nicholas, Morufu Olalekan Raimi (2025) Urban Green Development and Public Health: Assessing the Health Implications of Green City Development Principles Implementation in Lagos Megacity, Nigeria. Oral Presentation Presented at the ACS-FUO Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Harnessing Green Chemistry & Artificial Intelligence for Sustainable Development, which held Tuesday, 4th - Thursday 7th November, 2025. Pg. 108.
- Raimi Aziba-anyam Gift, Raimi Morufu Olalekan (2025) AI-Driven Synthesis of Personalized ECG Signals for Privacy-Preserving Healthcare Innovation in Nigeria: Toward Sustainable and Ethical Medical Data Generation. Oral Presentation Presented at the ACS-FUO Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Harnessing Green Chemistry & Artificial Intelligence for Sustainable Development, which held Tuesday, 4th - Thursday 7th November, 2025. Pg. 139.
- Uchenna Geraldine Elemuwa, Christopher Ononiwu Elemuwa, Teddy Charles Adias, Morufu Olalekan Raimi (2025) The Role of Local Food Systems in Mitigating Dietary Toxin Exposure in Nigeria. Oral Presentation Presented at the 10th International Conference on Health, Medicine and Life Sciences (MEDLIFE2025). (ISBN: 979-8-88599-124-7).
- Abdulraheem AF, Ononokpono DN, Raimi MO (2025). Breaking barriers to safe motherhood: how social, cultural, and geographic inequalities shape skilled birth attendance in Nigeria. Sociol Int J.;9(5):188‒200. https://doi.org/10.15406/sij.2025.09.00437.
- Kakwi JD, Yakasai KM, Kakwi JD, Raimi MO (2025). Promotion over pixels: a mixed-methods analysis of vaccine communication strategies in Plateau State, Nigeria. BMJ Open 2025;0:e094029. https://doi.org/10.1136/ bmjopen-2024-094029.
- Adias, L. T., Raimi, A. G., & Raimi, M. O. (2025b). From Stress to Strategy: Scalable and Inclusive HRM Strategies for Mental Health Reform in Nigeria’s Evolving Workforce. International Journal of Research and Innovation in Social Science (IJRISS), IX(XIV), 1576–1601. https://doi.org/IJRISS.2025.914MG00120.
- Koleayo O, Kolawole O, Adeyemi A, Amos O, Rebecca A, Oladapo M, Oluseye O, Benjamin M, Olusegun A, Sarah J, Josephine K, Sandra B-U, Morufu R (2024). Are Genetically-Modified Foods Made for the Common Good? The Perspectives of the Victoria Islanders Global Journal of Enviromental Science & Sustainability, 1(1). https://doi.org/10.69798/53920008.
- Raimi OM, Lucky EC, Okoyen E, Clement A, Ogbointuwei C, et al. (2021) Making Better Informed, More Confident COVID-19 Decisions: Vaccine Hesitancy, Its Barriers and Impact Studies: Taking Bayelsa State as an Example. Int J Vaccine Immunizat 5(1): dx.doi. org/10.16966/2470-9948.126. https://sciforschenonline.org/journals/vaccines/IJVI126.php.
- Raimi MO, Ayinla LO, Ogah A (2021) First to Respond, Last to Leave: The Role of Para-Military Agencies in Disaster Management: Evidence from Nigeria. Sumerianz Journal of Medical and Healthcare, 2021, Vol. 4, No. 2, pp. 96-100 ISSN(e): 2663-421X, ISSN(p): 2706-8404 Website: https://www.sumerianz.com. https://doi.org/10.47752/sjmh.42.96.100. https://www.sumerianz.com/?ic=journal-home&journal=31&info=archive-detail&month=06-2021&issue=2&volume=4.
- Samson TK, Ogunlaran OM, Raimi OM (2020); A Predictive Model for Confirmed Cases of COVID-19 in Nigeria. European Journal of Applied Sciences, Volume 8, No 4, Aug 2020;pp:1-10. https://doi.org/10.14738/aivp.84.8705. DOI: https://doi.org/10.14738/aivp.84.8705.
- Olalekan RM (2020). “What we learn today is how we behave tomorrow”: a study on satisfaction level and implementation of environmental health ethics in Nigeria institutions. Open Access Journal of Science; 4(3):82‒92. https://doi.org/10.15406/oajs.2020.04.00156.
- Olalekan RM, Olawale SH, Christian A, Simeon AO (2020). Practitioners Perspective of Ethical Cases and Policy Responses by Professional Regulator: The Case of Environmental Health Officers Registration Council of Nigeria (EHORECON). American Journal of Epidemiology & Public Health. 2020;4(1): 016-023. https://www.scireslit.com/PublicHealth/AJEPH-ID23.pdf https://www.scireslit.com/PublicHealth/articles.php?volume=4&issue=1.
- Henry OS, Morufu OR, Adedotun TA & Oluwaseun EO (2019) Measures of Harm from Heavy Metal Pollution in Battery Technicians’ Workshop within Ilorin Metropolis, Kwara State, Nigeria. Scholink Communication, Society and Media ISSN 2576-5388 (Print) ISSN 2576-5396 (Online) Vol. 2, No. 2, 2019 www.scholink.org/ojs/index.php/csm. https://doi.org/10.22158/csm.v2n2p73.
- Raimi MO, Omidiji AO, Ebikapaye O, Moses T, Adeolu TA, Makanjuola Bosede C (2019), Situational Analysis of National Immunization Programme in Nigeria, Journal of Immunology and Inflammation Diseases Therapy. https://doi.org/10.31579/2637-8876.2019/008.
- Lateefat MH, Opasola AO, Misbahu G, Morufu OR (2022) A Wake-Up Call: Determination of Antibiotics Residue Level in Raw Meat in Abattoir and Selected Slaughterhouses in Five Local Government in Kano State, Nigeria. bioRxiv 2022.01.04.474991;. https://doi.org/10.1101/2022.01.04.474991. Link: https://en.x-mol.com/paper/article/1479559526563860480.
- Lateefat MH, Opasola AO, Adiama BY, Ibrahim A, Morufu OR (2022) Elixirs of Life, threats to Human and Environmental Well-being: Assessment of Antibiotic Residues in Raw Meat Sold Within Central Market Kaduna Metropolis, Kaduna State, Nigeria. bioRxiv 2022.01.04.474997;. https://doi.org/10.1101/2022.01.04.474997.
- Raimi MO, Emeka CL, Ebikapaye O, Angalabiri C, Christopher O, Atoyebi B (2021) COVID-19 Decision Impacts: Vaccine Hesitancy, its Barriers and Impact Studies: Taking Bayelsa State as an Example., 27 May 2021, PREPRINT (Version 1) available at Research Square [https://doi.org/10.21203/rs.3.rs-566532/v1].
- Promise, V.I., Alabere, I., Abdulraheem, I. and Raimi, M.O. (2026) Improving Childhood Immunization Completion in Rural Bayelsa State, Nigeria: A Pragmatic Cluster Randomized Trial of Mobile Phone Reminders and Home Visits. Open Journal of Preventive Medicine, 16, 1-20. https://doi.org/10.4236/ojpm.2026.161001.
- Kakwi JD, Yakasai KM, Kakwi JD, Raimi MO (2024) Campaigning Against Vaccine Hesitancy: Evaluating the Effectiveness of Health Communication on COVID-19 Vaccination Uptake in Plateau State, Nigeria. JMIR Preprints. 22/09/2024:66755. https://doi.org/10.2196/preprints.66755 URL: https://preprints.jmir.org/preprint/66755.
- Promise VI, Macauley T, Alabere I, Abdulraheem I, Raimi MO (2024) Closing the Gap: Assessment of Vaccination Coverage Among Under Two Children in Bayelsa State, Nigeria. JMIR Preprints. 29/12/2024:70671. https://doi.org/10.2196/preprints.70671. URL: https://preprints.jmir.org/preprint/70671.
- Kakwi JD, Yakasai KM, Raimi MO, Kakwi JD (2024) Understanding the Dynamics of COVID-19 Vaccine Uptake in Plateau State, Nigeria: Analyzing Socioeconomic, Cultural, and Communication Influences. JMIR Preprints. 30/12/2024:70702. https://doi.org/10.2196/preprints.70702. URL: https://preprints.jmir.org/ojs/index.php/preprints/preprint/70702.
- Efiok, J.N, Oluseye, O, Uduak, T and Olalekan, R (2015) Safety Culture, Policies and Practices in Nigeria Maritime Industry: The Exxon – Mobil Experience. Open Journal of Safety Science and Technology, 5, 69-76. https://doi.org/10.4236/ojsst.2015.53009.
- Aziba-anyam Gift Raimi, Morufu Olalekan Raimi (2025) Leveraging Digital Platforms for Community-Driven Public Health Surveillance in the Niger Delta: A Feasibility Study from Bayelsa State, Nigeria. Oral Presentation Presented at the ACS-FUO Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Harnessing Green Chemistry & Artificial Intelligence for Sustainable Development, which held Tuesday, 4th - Thursday 7th November, 2025. Pg. 124.
- Teddy CA; Christopher OE; Morufu OR (2025) Community Engagement and Social Innovation for Environmental Justice in Sub-Saharan Africa. Oral Presentation Presented at the 1st International Conference of the Faculty of Science, Federal University Otuoke, Bayelsa State on the theme: Revolutionizing a Sustainable Tomorrow: Harnessing Science, Innovation and Community Power to Drive Circular Economy Solutions, Climate Resilience, and a Thriving Green Economy, which held Tuesday, 4th–Friday 7th March, 2025. Pp. 75.

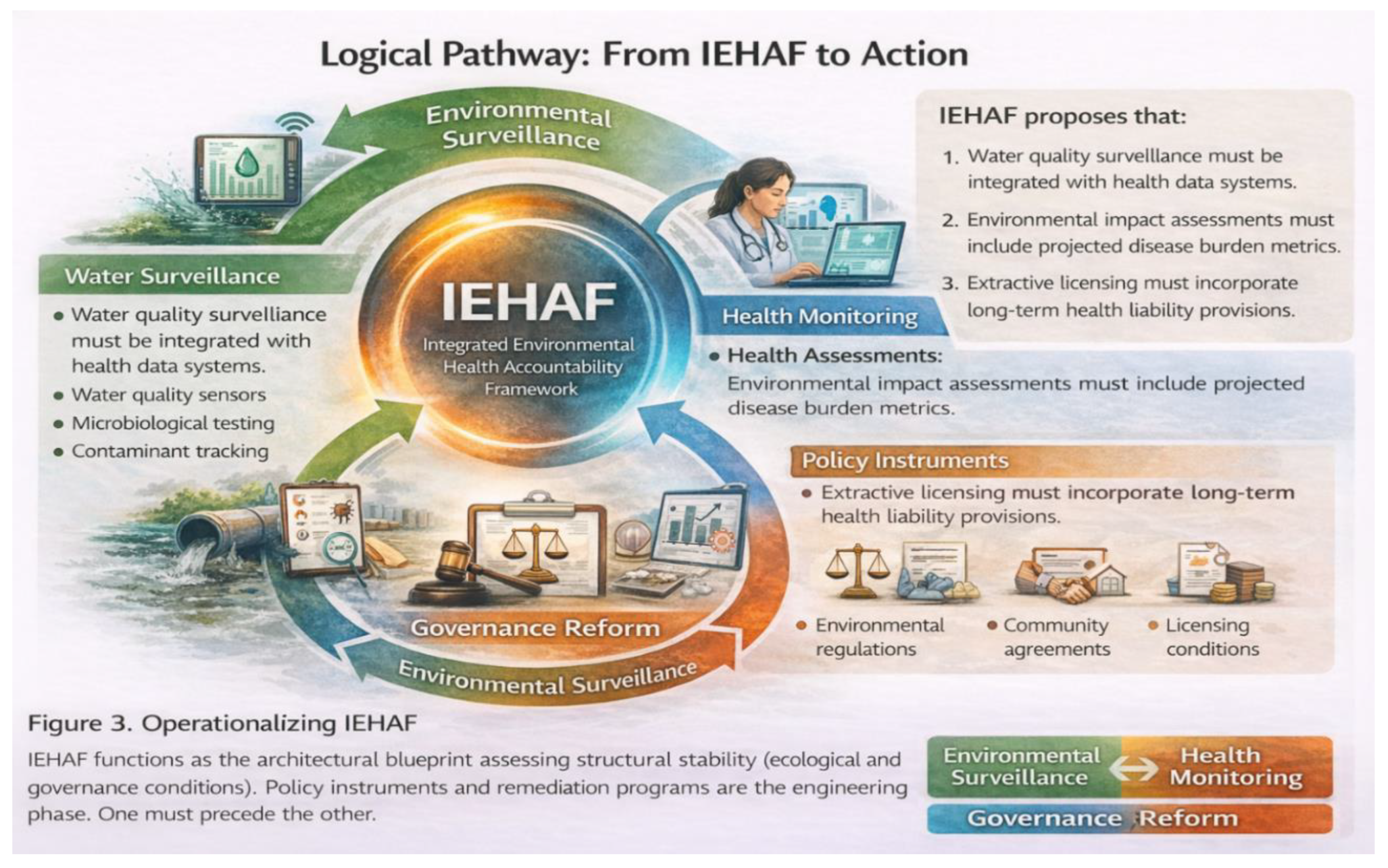
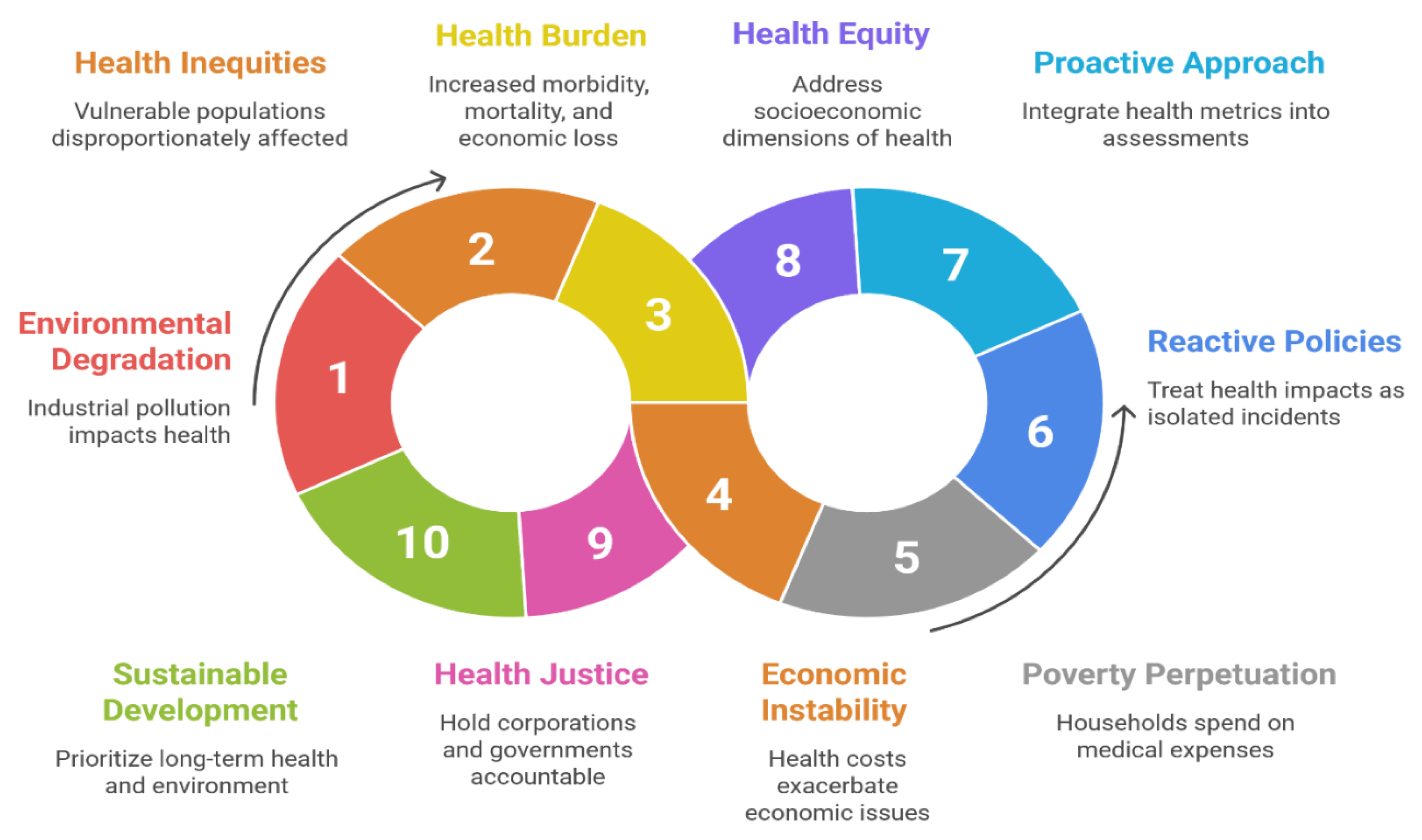
| Pathway | Environmental Trigger | Immediate Health / Economic Impact | Intermediate Household-Level Effect | Long-Term Structural Consequence | Intergenerational Implication |
|---|---|---|---|---|---|
| Contaminated Water Ingestion | Hydrocarbon spills, heavy metal contamination, microbial pollution | Acute gastrointestinal illness, dermatological conditions, toxic exposure | Recurrent medical visits; school absenteeism; temporary work loss | Chronic disease burden (renal disease, liver dysfunction, neurodevelopmental delay); rising healthcare costs | Reduced cognitive attainment in children; diminished lifetime earning potential |
| Fisheries Collapse | Oil spills, sediment contamination, mangrove destruction | Decline in fish catch; immediate income loss among artisanal fishers | Reduced household protein intake; coping strategies (borrowing, asset sales) | Food insecurity; malnutrition; collapse of local blue economy | Stunting, impaired child development, long-term poverty transmission |
| Agricultural Yield Decline | Soil salinization, polluted irrigation water, acid deposition | Reduced crop productivity; harvest losses | Increased food prices; dietary compromise; rural indebtedness | Entrenched rural poverty; migration to urban informal settlements | Loss of agrarian livelihood skills; youth unemployment cycle |
| Healthcare Expenditure | Pollution-induced morbidity (respiratory, renal, reproductive disorders) | Out-of-pocket medical spending; catastrophic health expenditure | Household financial strain; diversion of education funds; borrowing at high interest | Asset depletion; deepened poverty; inability to invest in livelihood recovery | Persistent socioeconomic disadvantage; limited upward mobility |
| Reduced Labor Productivity | Chronic illness; occupational exposure to polluted environments | Fatigue, absenteeism, reduced physical capacity | Lower household income; unstable employment | Reduced regional GDP contribution; suppressed economic growth | Structural underdevelopment of oil-producing communities |
| Maternal and Child Health Impacts | Exposure to heavy metals, PAHs, air pollutants | Low birth weight; preterm birth; childhood infections | Increased caregiving burden; higher healthcare utilization | Elevated maternal and infant mortality rates; weakened human capital base | Lifelong health vulnerabilities; diminished educational attainment |
| Psychosocial Stress & Displacement | Environmental loss, livelihood collapse, forced migration | Anxiety, depression, social conflict | Community fragmentation; erosion of social capital | Regional instability; weakened governance trust | Cycles of marginalization and social exclusion |
| Actor | Immediate Action (Short-Term Response) | Intermediate Institutional Shift | Structural Reform (Long-Term Transformation) | Intended Public Health Outcome |
|---|---|---|---|---|
| Policymakers (Federal & State Governments) | Mandate integrated water–health surveillance; enforce transparent reporting of spills and flaring | Harmonize environmental, petroleum, and public health regulations; allocate budget lines for environmental health | Embed long-term health liability and remediation trust funds in extractive contracts; adopt polluter-pays enforcement mechanisms | Reduced exposure burden; institutional accountability; prevention-oriented governance |
| Public Health Agencies | Establish toxicological screening programs in oil-producing communities; deploy mobile clinics | Integrate environmental exposure indicators into routine health information systems; strengthen disease surveillance | Develop regional environmental health registries and longitudinal cohort monitoring systems | Early detection of chronic disease; life-course exposure tracking; improved health equity |
| Environmental Regulatory Bodies | Conduct independent water and soil quality audits; enforce compliance thresholds | Digitalize environmental monitoring systems; require cumulative impact assessments | Institutionalize health-inclusive Environmental Impact Assessments (EIAs) with projected disease burden metrics | Evidence-based regulation; reduced cumulative toxic exposure |
| Researchers & Academic Institutions | Quantify multi-pollutant cumulative risk; conduct biomonitoring studies | Develop interdisciplinary exposure–disease models linking ecology and economics | Model intergenerational economic burden of pollution; establish predictive risk mapping frameworks | Stronger causal evidence; policy-relevant burden-of-disease estimates |
| Civil Society & Community Organizations | Community-based water monitoring; risk communication campaigns | Participatory environmental governance platforms; social accountability reporting | Strategic litigation, transparency advocacy, and extractive revenue tracking | Empowered communities; improved environmental justice outcomes |
| Oil & Extractive Corporations | Immediate spill response and remediation; disclose emission inventories | Adopt transparent ESG reporting tied to measurable health indicators | Internalize environmental health costs; establish independent remediation and compensation funds | Corporate accountability; reduced long-term liability |
| International Partners & Donors | Technical support for exposure assessment and surveillance | Fund integrated environmental–health data systems | Support structural reforms aligned with global environmental justice frameworks | Strengthened institutional capacity; sustainable development alignment |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




