Submitted:
19 February 2026
Posted:
25 February 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Material and Methods
- age ≥ 18 years
- symptomatic hiatal hernia confirmed by upper gastrointestinal endoscopy and/or computed tomography
- elective laparoscopic hiatal hernia repair
- complete perioperative and follow-up data
- previous esophageal or gastric surgery
- emergency procedures
- concomitant bariatric surgery
- follow-up shorter than six months
- demographic data (age, sex)
- body mass index (BMI)
- comorbidities (obesity, diabetes mellitus, cardiovascular and pulmonary disease)
- duration and type of symptoms (heartburn, regurgitation, dysphagia, chest pain)
- type of hiatal hernia (sliding, mixed, paraesophageal)
- hiatal defect size measured intraoperatively (maximum transverse diameter)
- surgical technique employed
- operative time
- length of postoperative hospital stay
- postoperative complications
- early hernia recurrence
- hiatal defects ≥ 5 cm
- significant intrathoracic stomach migration
- esophageal shortening or increased tension at the hiatal repair
- persistence of postoperative dysphagia
- operative time
- length of hospital stays
- perioperative complications
Results
Patient Demographics
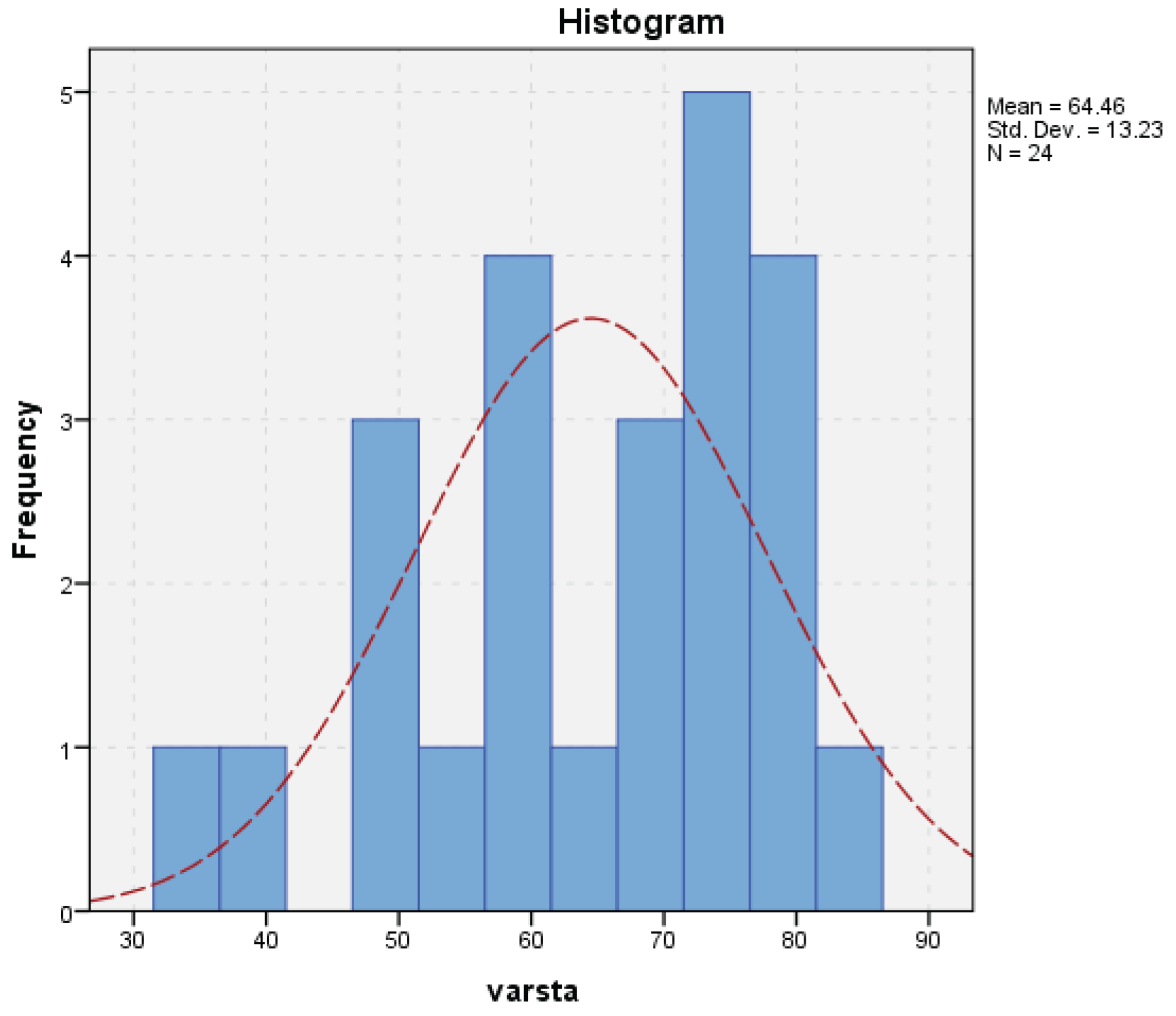
| Gender | Mean | N | Std. dev. | Median | Min | Max |
| F | 62.79 | 22 | 11.98 | 64 | 34 | 79 |
| M | 70.80 | 7 | 17.22 | 77 | 41 | 84 |
| Total | 64.46 | 29 | 13.23 | 68 | 34 | 84 |
| Gender | Mean (onset of simpt) |
N | Std. dev. | Median | Min | Max |
|---|---|---|---|---|---|---|
| F | 9.55 | 22 | 3.113 | 10 | 4 | 15 |
| M | 11.50 | 7 | 4.087 | 10 | 8 | 18 |
| Total | 9.96 | 29 | 3.361 | 10 | 4 | 18 |
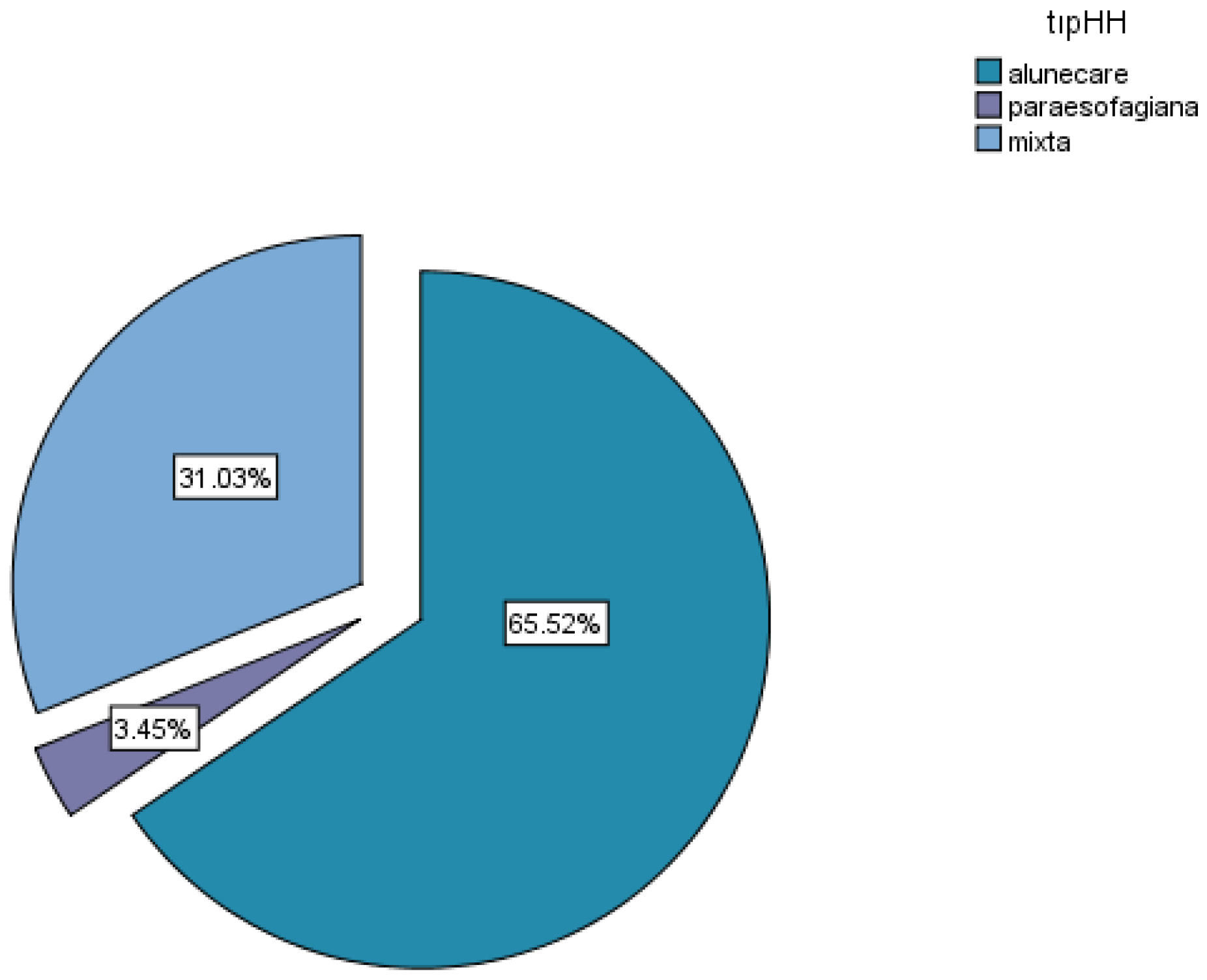
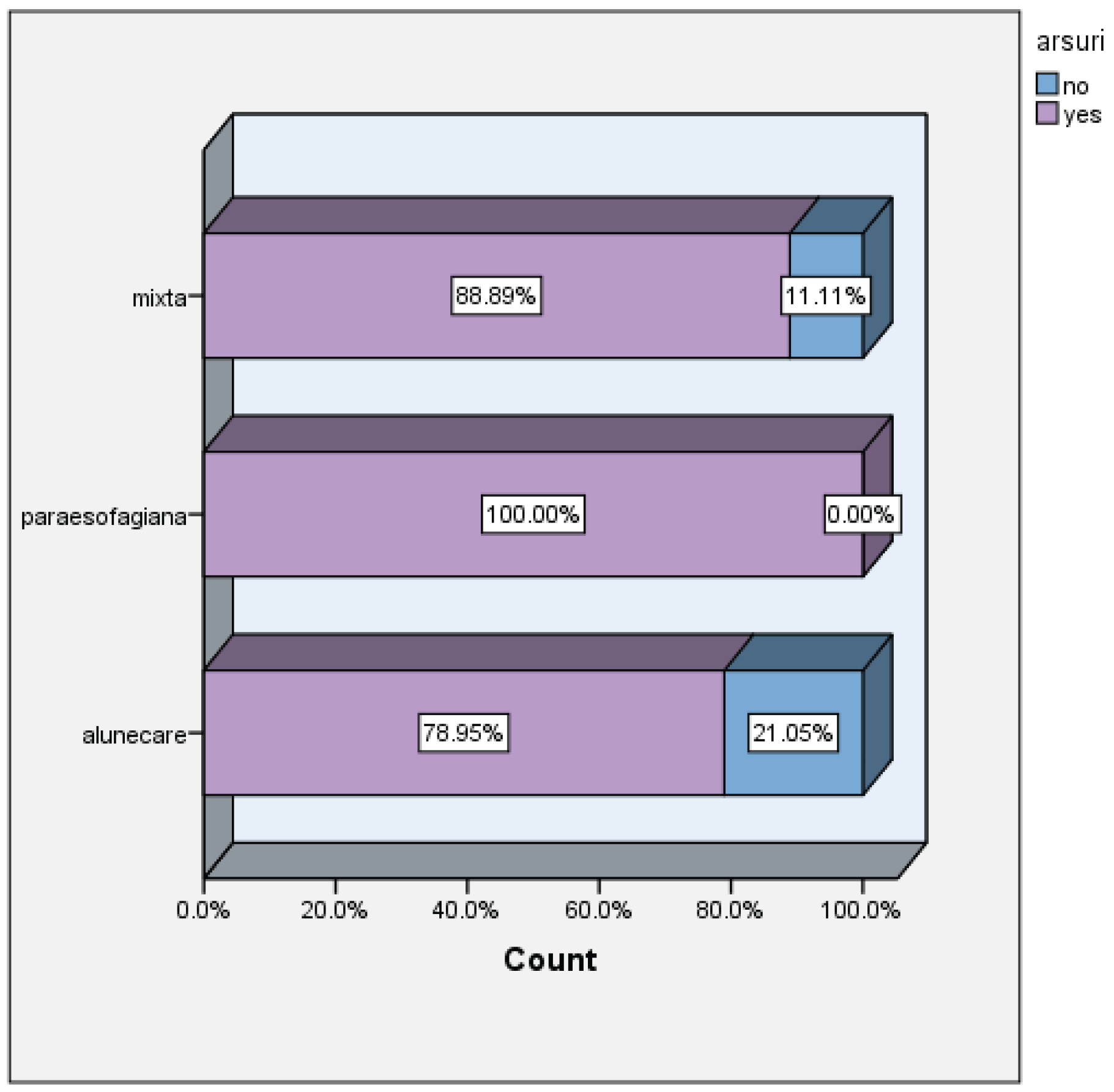
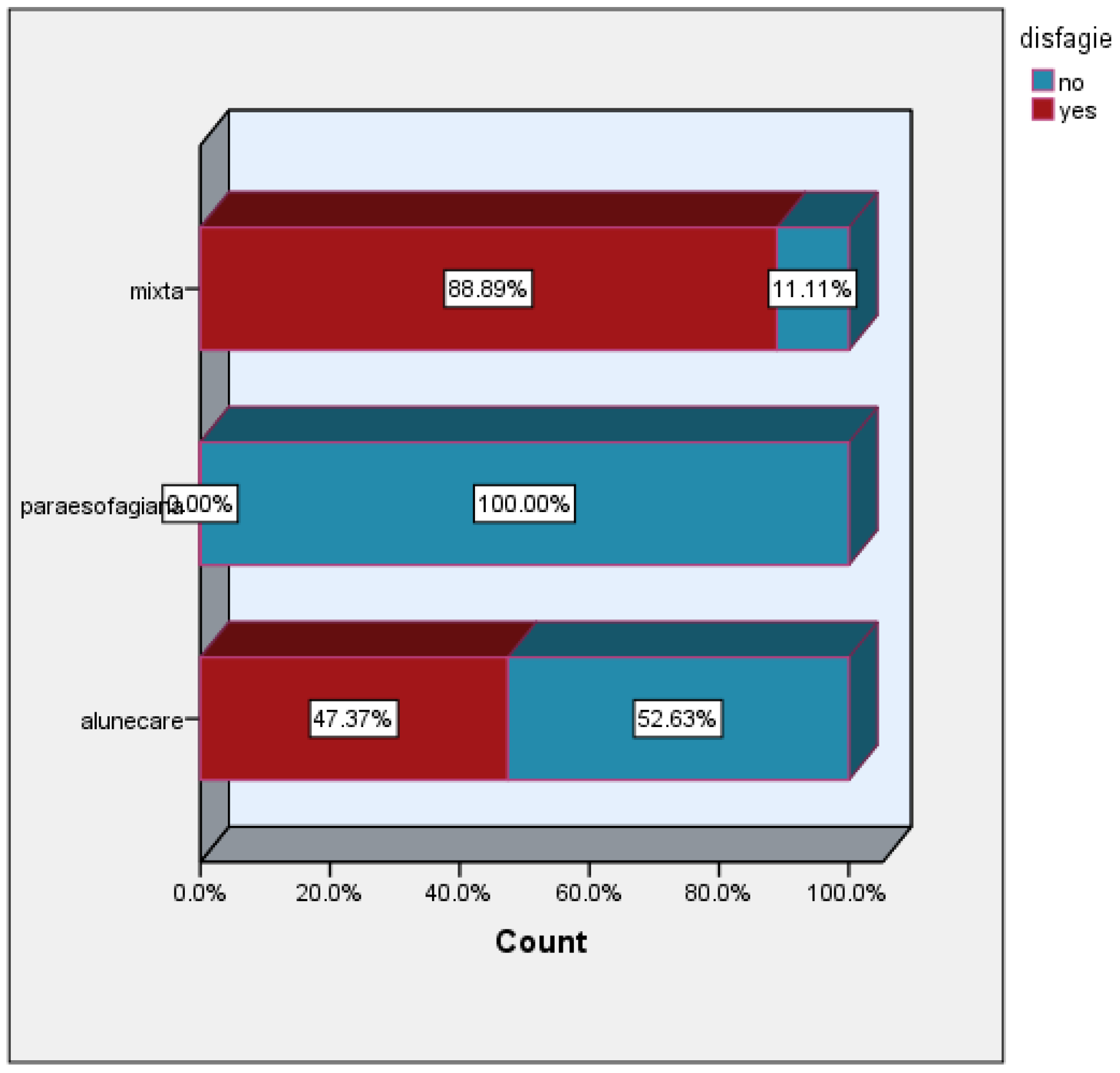
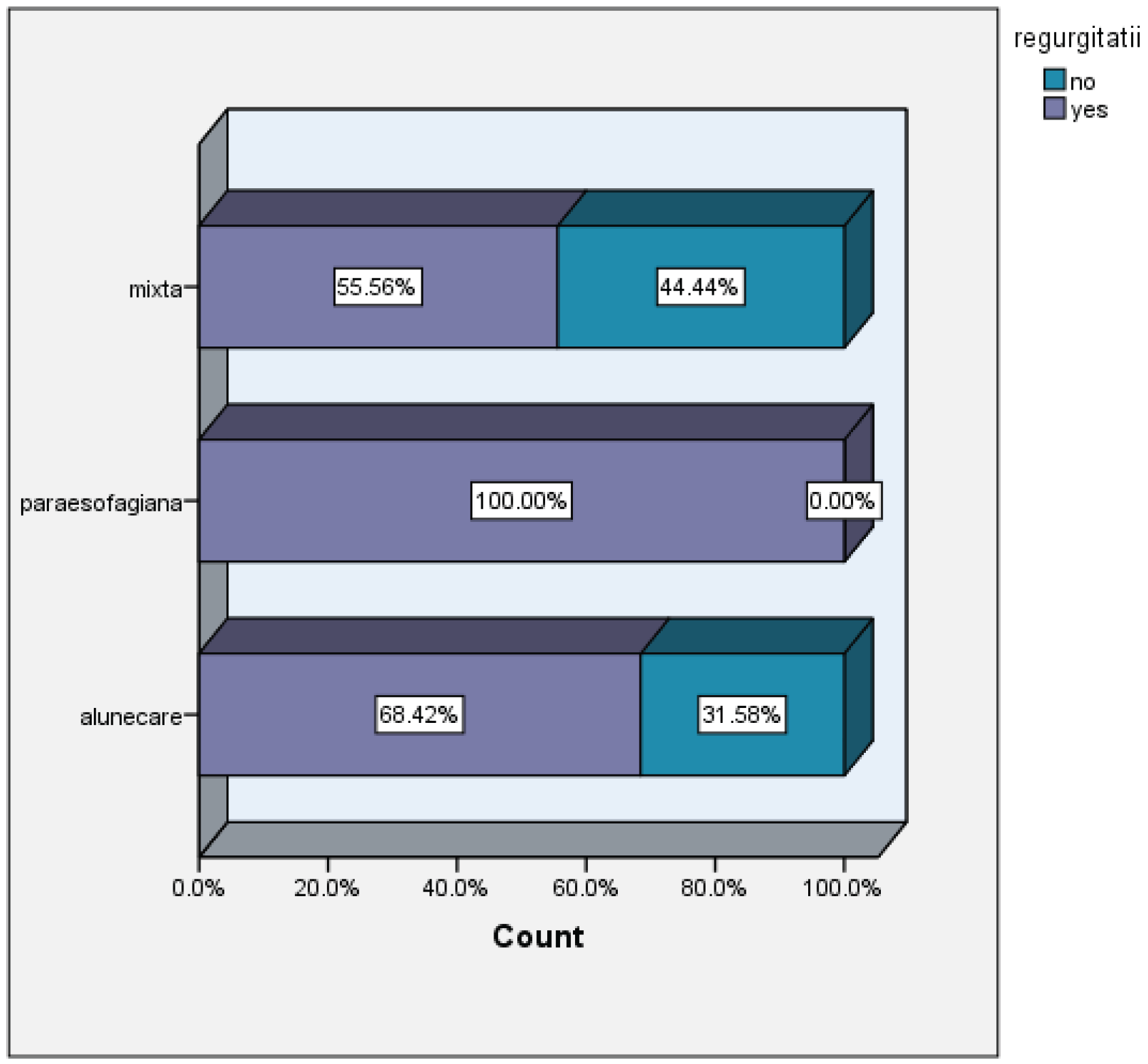
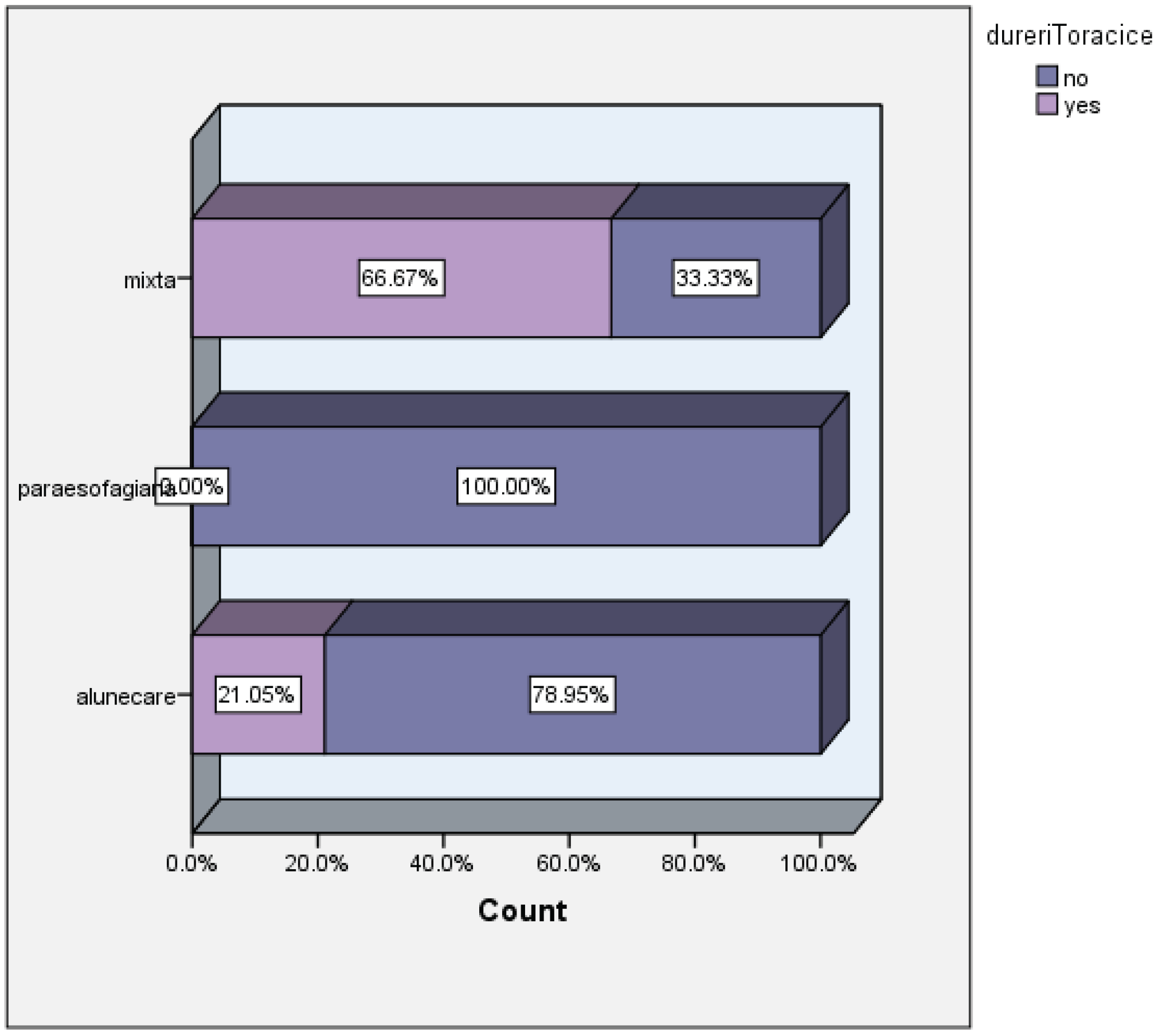
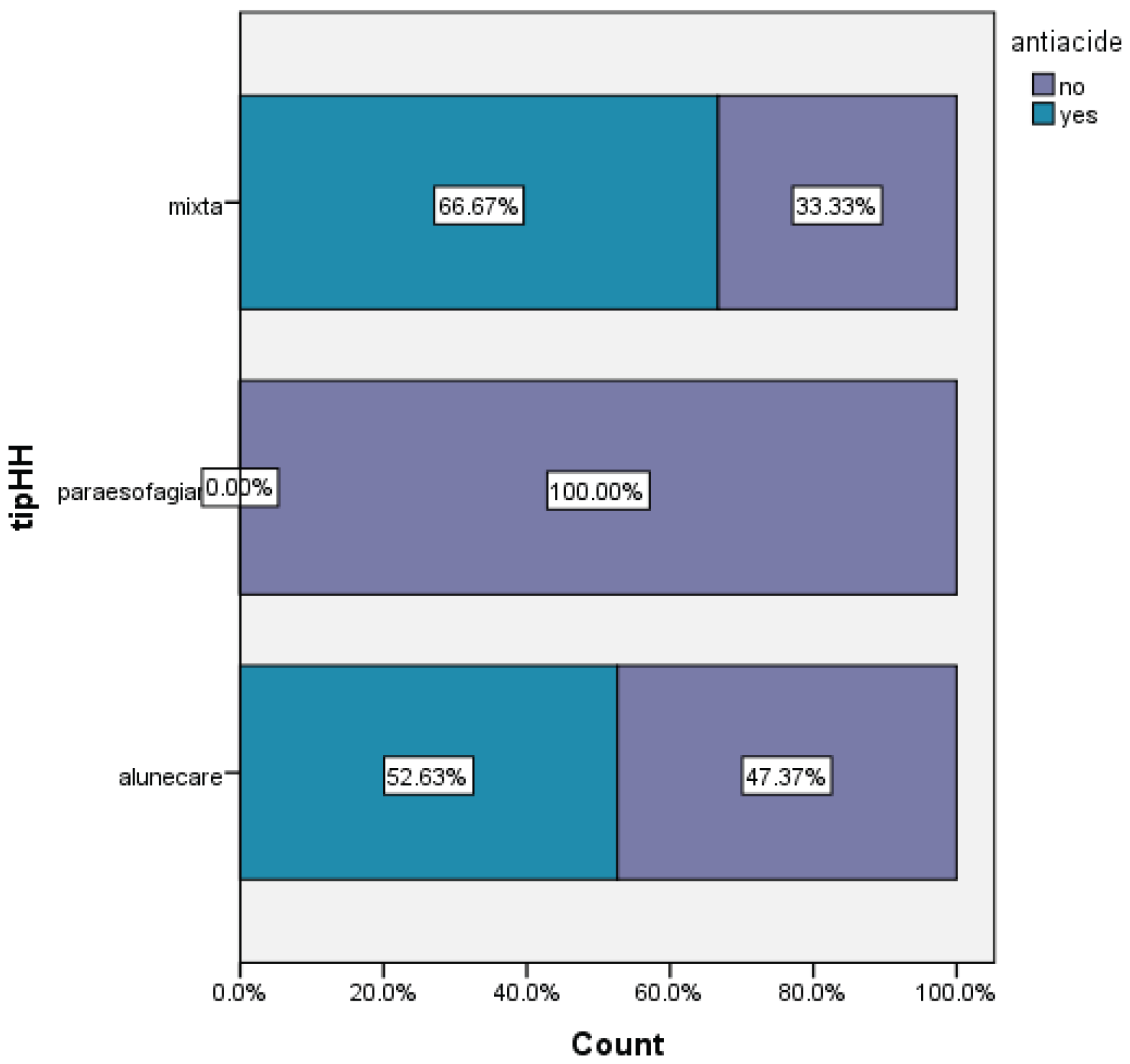
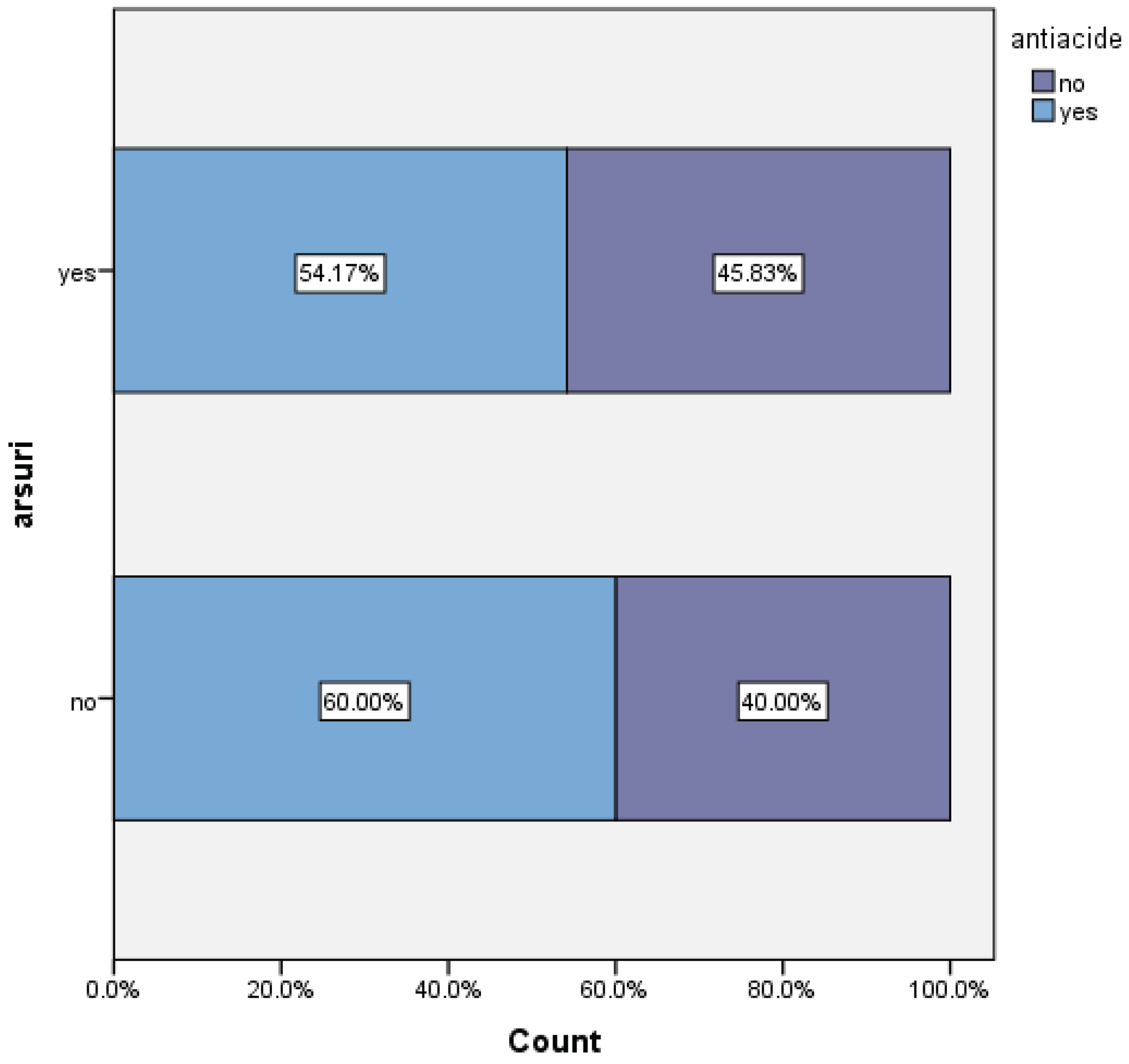
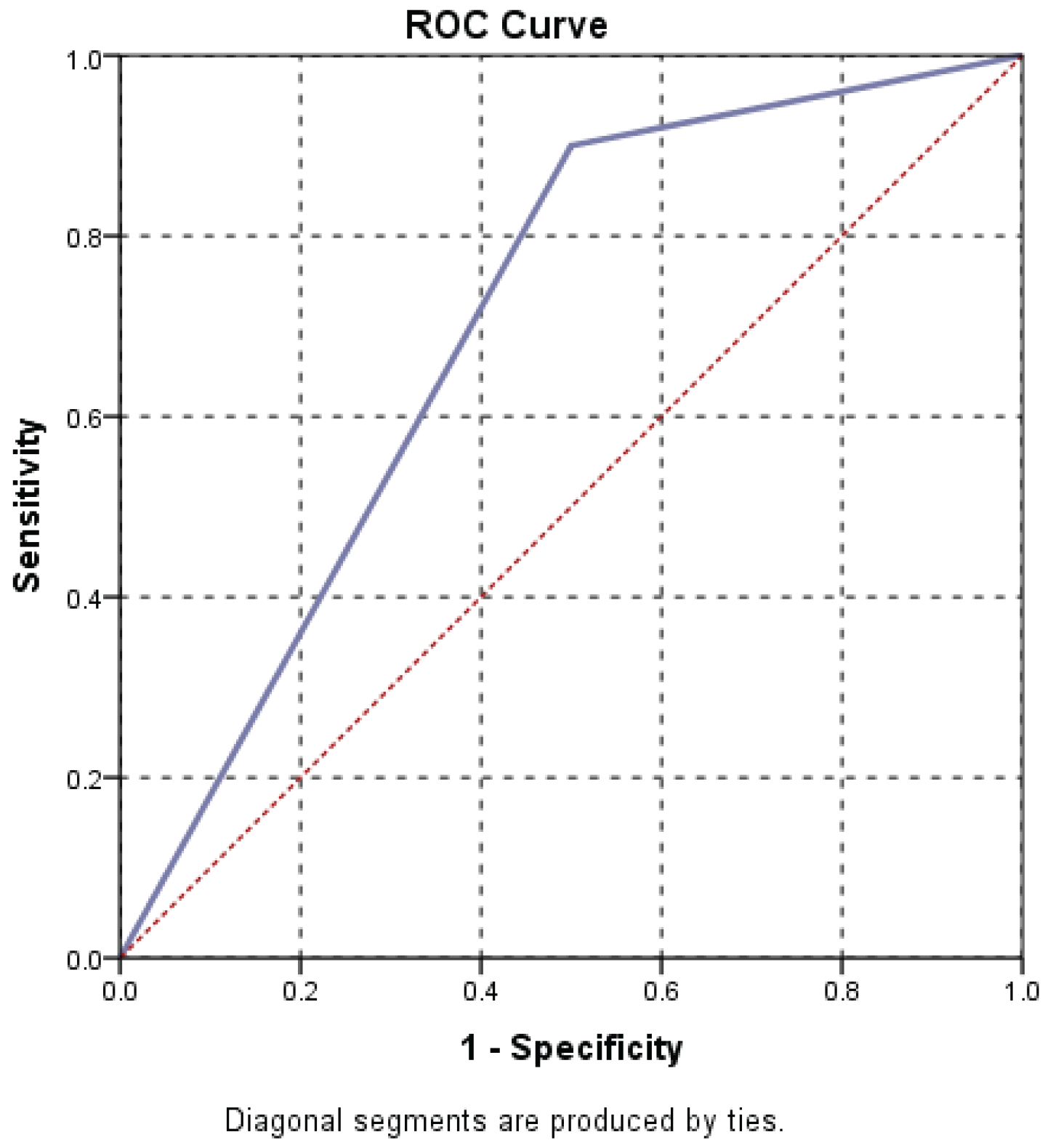
| Size of hiatal hernia versus dysphagia | |||||||
| Dysphagia | Mean | N | Std dev | Min | Max | Median | P value |
| No | 5.417 | 12 | .7930 | 5 | 7 | 5 | 0.004 |
| Yes | 6.853 | 17 | 1.4226 | 5 | 9 | 7 | |
| Total | 6.259 | 29 | 1.3863 | 5 | 9 | 6 | |
| F=9.970 | |||||||
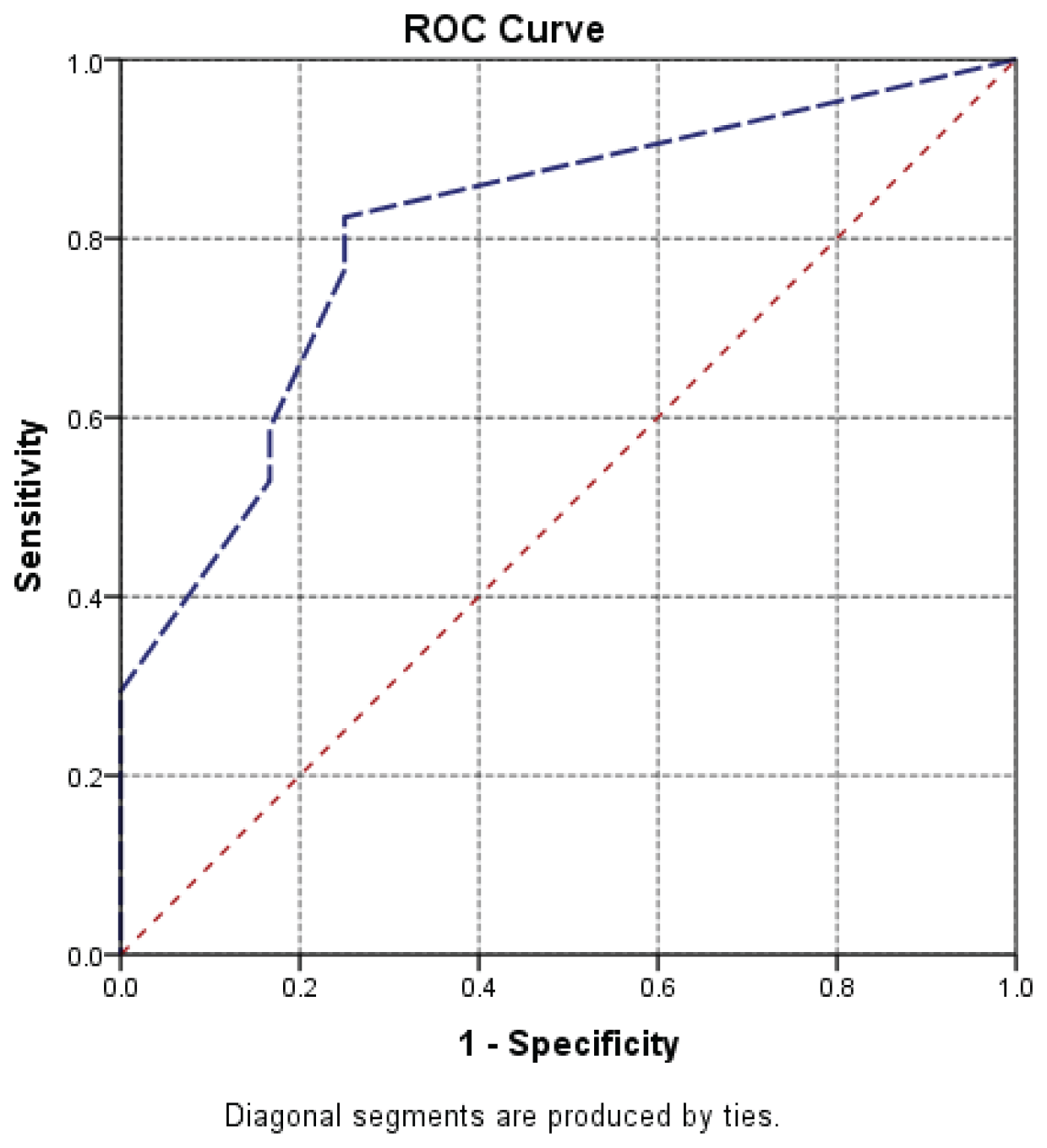
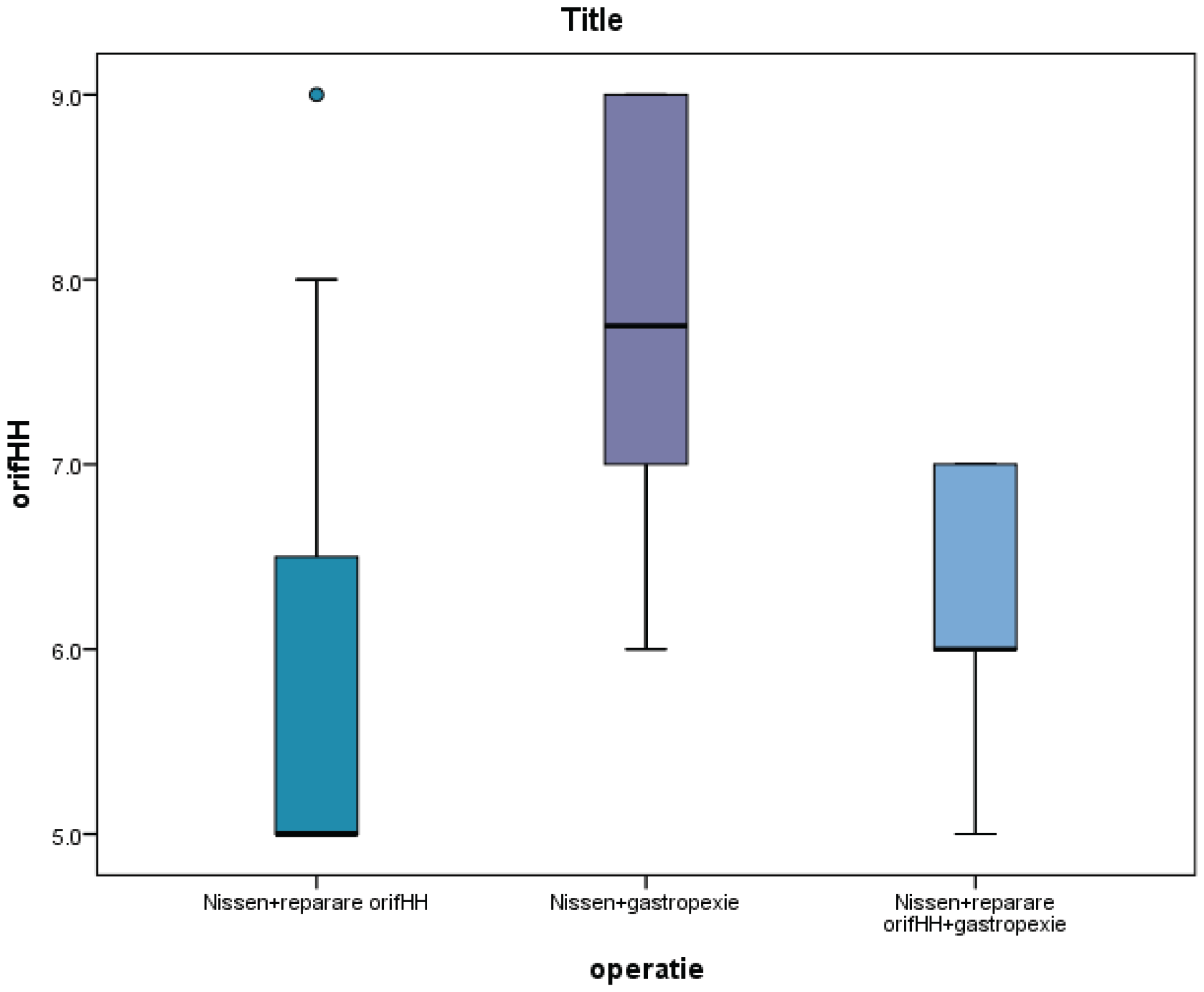
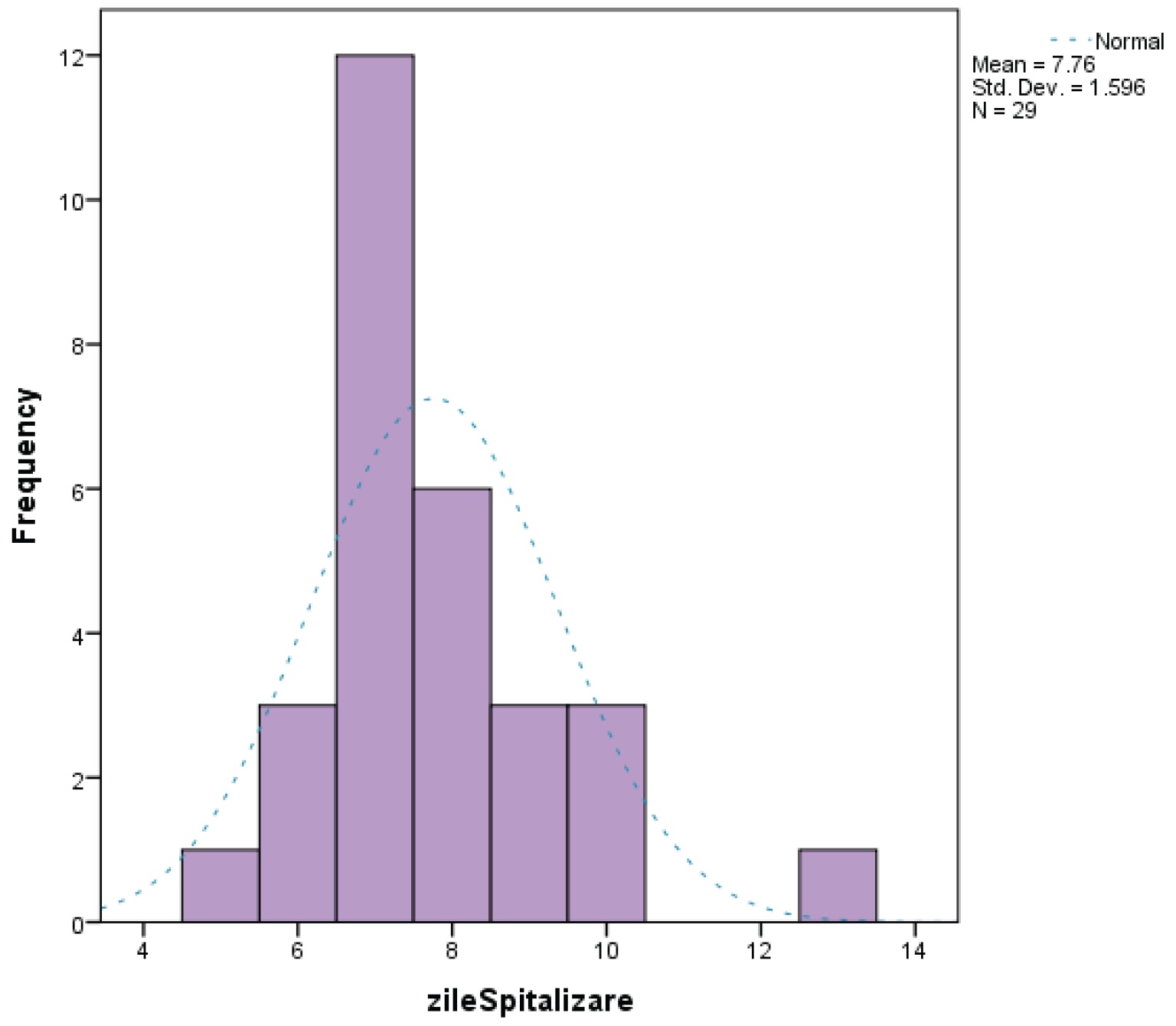
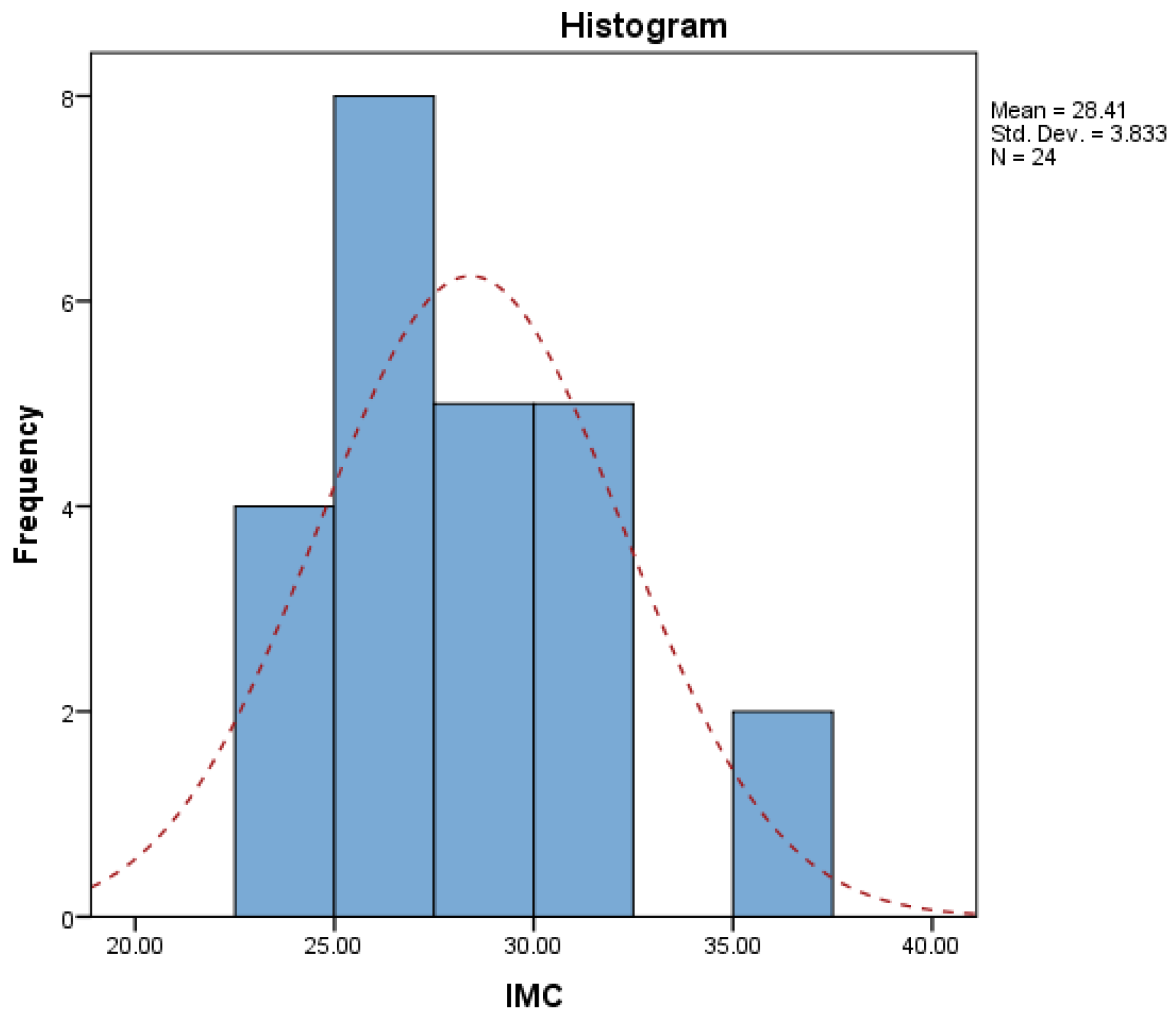
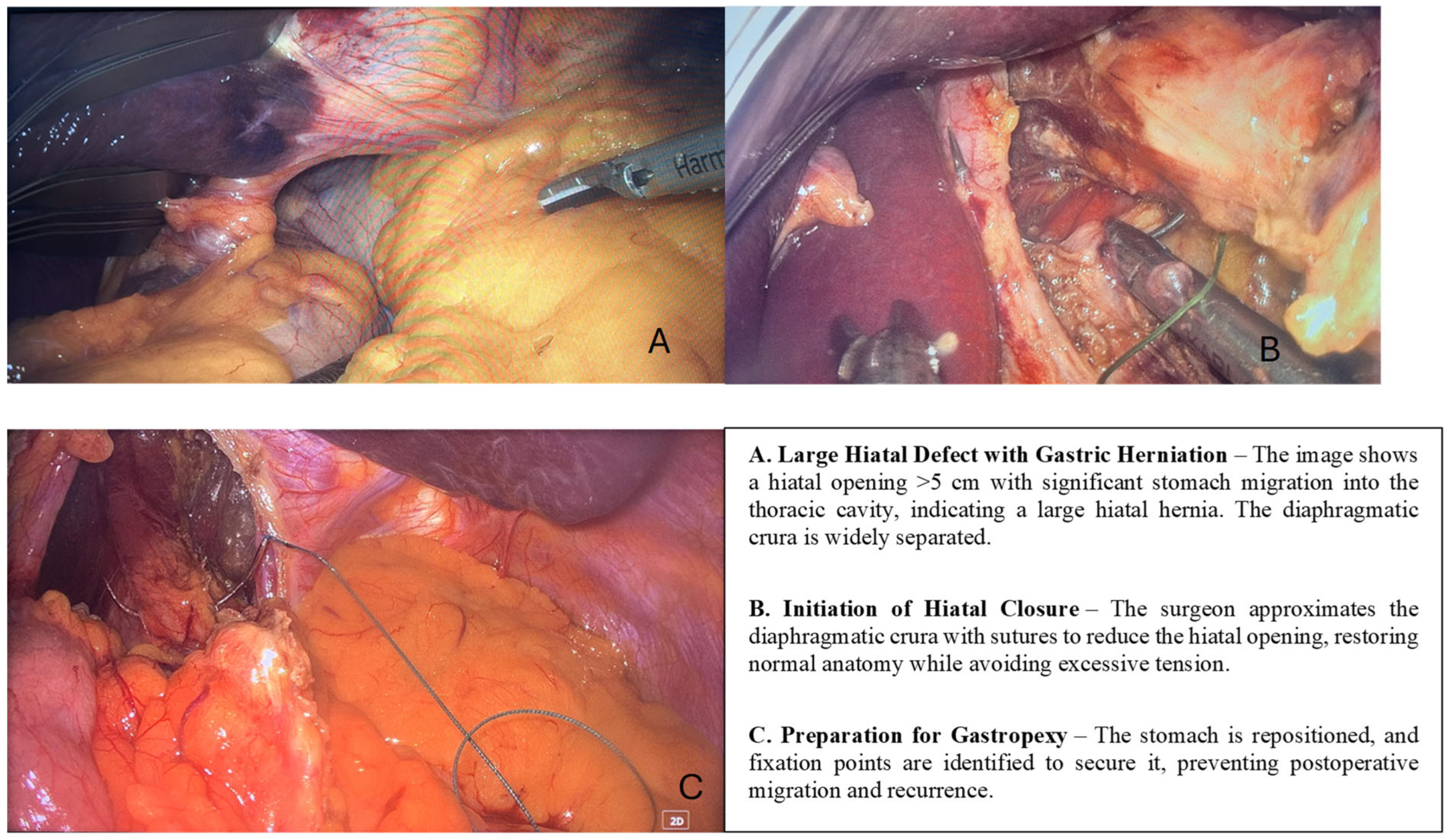
Discussions
The Role of Gastropexy in Recurrence Prevention
- 1.
- Comparative studies evaluating long-term recurrence rates with versus without gastropexy in cases involving large hiatal hernias. While existing retrospective data suggest potential benefits, randomized controlled trials would generate more definitive conclusions.
- 2.
- Investigation into alternative fixation techniques, such as mesh-reinforced repairs, alongside gastropexy to discover the most effective treatment strategy for large or recurrent hiatal hernias.
- 3.
- Exploration of the role of gastropexy in individuals exhibiting altered esophageal motility, including those diagnosed with achalasia or ineffective peristalsis, to determine if additional gastric fixation contributes to improved symptom management.
- 1.
- Surgeons should contemplate the use of gastropexy for patients with extensive hiatal defects (greater than 5 cm), particularly in cases involving mixed-type hernias or increased intra-abdominal pressure.
- 2.
- Gastropexy should be embraced as a preventive strategy to diminish the chances of recurrence, particularly when high tension at the hiatal level exists or stability following fundoplication is uncertain.
- 3.
- Timely surgical intervention in patients presenting with large hiatuses may help mitigate prolonged symptomology and reduce the risk of severe complications such as gastric volvulus.
- 4.
- A tailored approach should be adopted, with preoperative evaluations assessing the severity of GERD, esophageal motility, and anatomical risk factors guiding the decision to incorporate gastropexy.
Conclusions
Reference
Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




