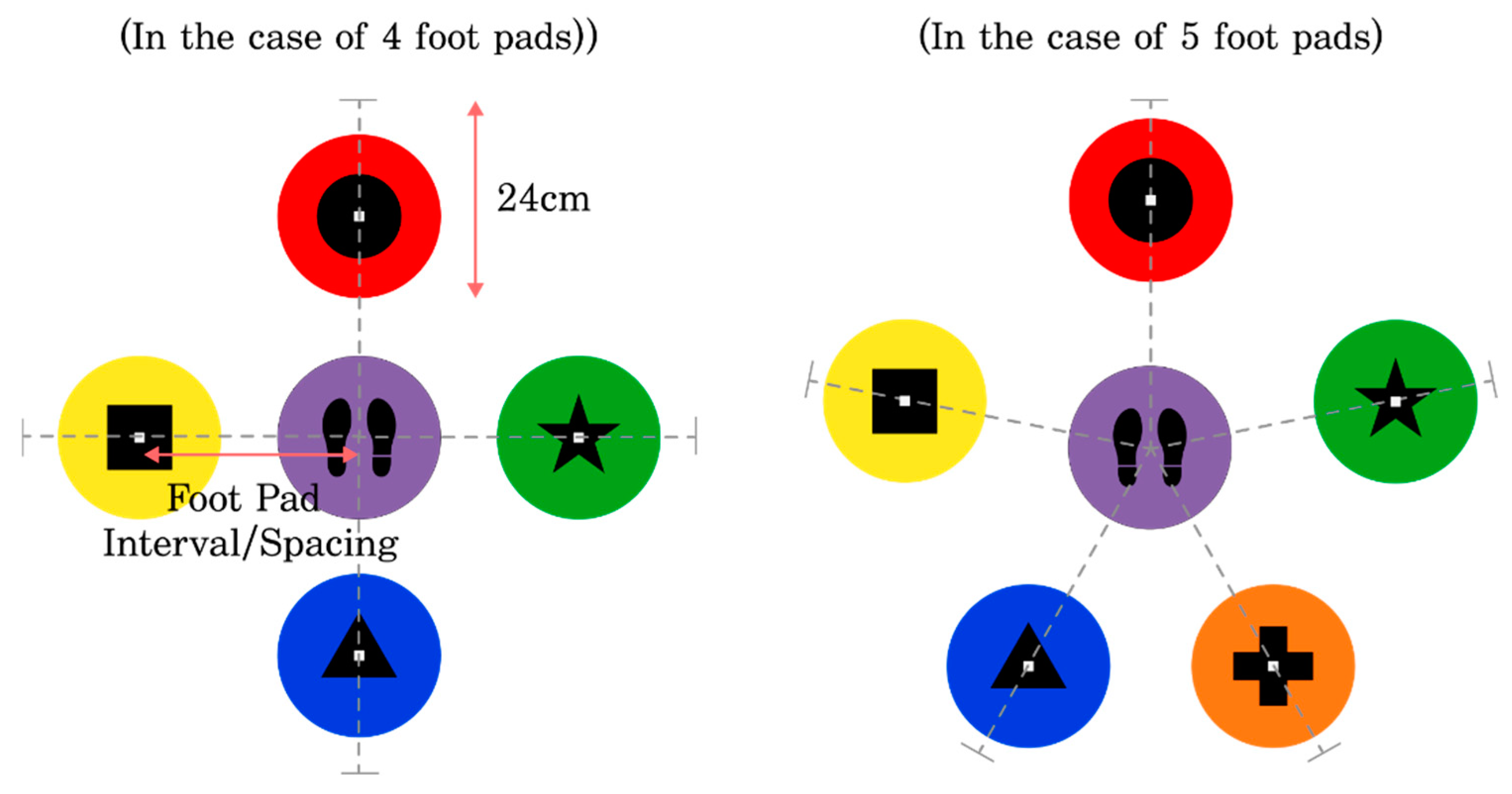
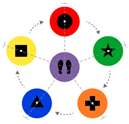
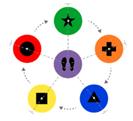
Figure 1.
Stepping-pad configuration for the Stroop Stepping Game.
Figure 1.
Stepping-pad configuration for the Stroop Stepping Game.
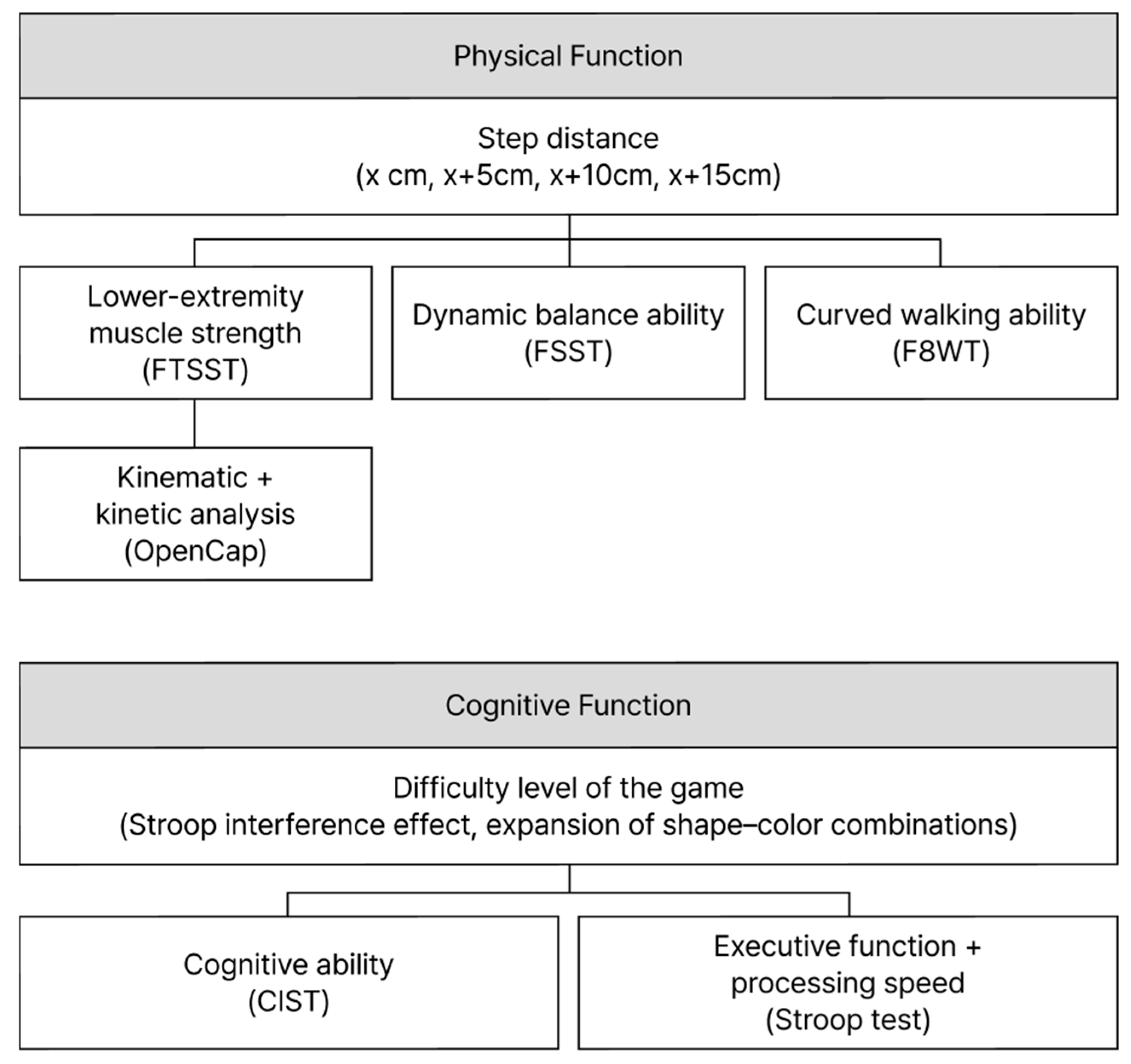
Figure 2.
Physical and Cognitive Research Model.
Figure 2.
Physical and Cognitive Research Model.
Figure 3.
“Match It!” Color-Step game (individual mode) (a), “Match It!” Color-Step game (team-based mode) (b).
Figure 3.
“Match It!” Color-Step game (individual mode) (a), “Match It!” Color-Step game (team-based mode) (b).
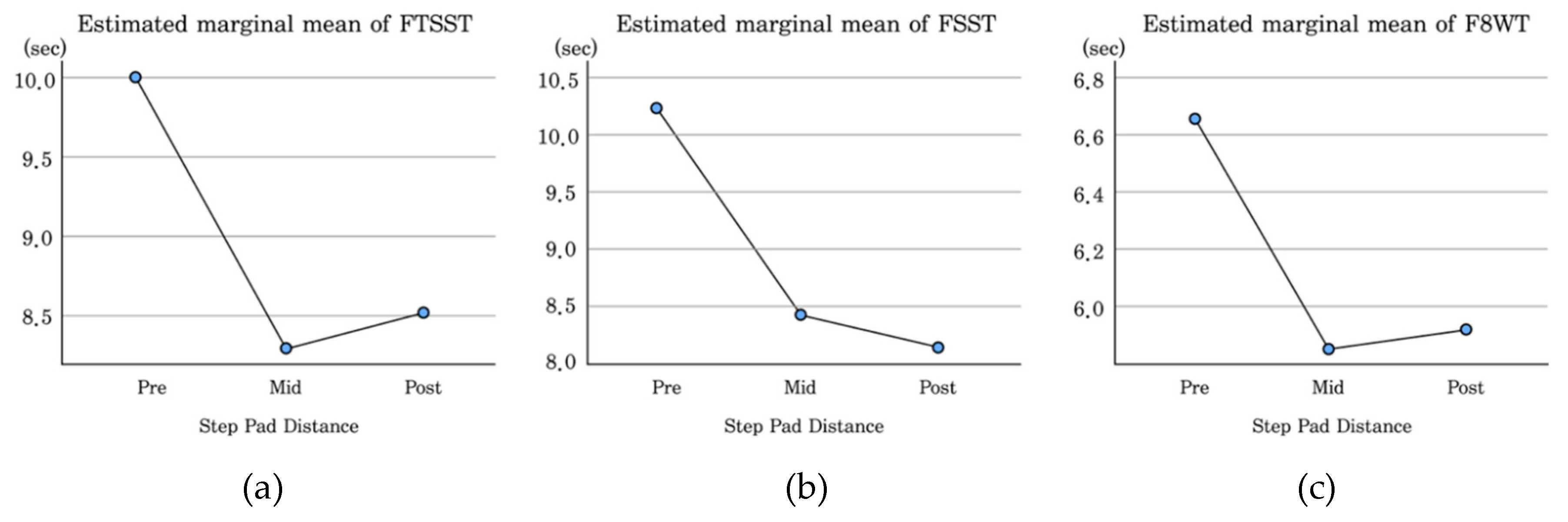
Figure 4.
Estimated marginal averages of FTSST (a), FSST (b), F8WT (c).
Figure 4.
Estimated marginal averages of FTSST (a), FSST (b), F8WT (c).
Figure 5.
Pre–post knee joint angles (a), knee joint angles at 25% (b), 50% (c), and 75% (d) of the movement phase.
Figure 5.
Pre–post knee joint angles (a), knee joint angles at 25% (b), 50% (c), and 75% (d) of the movement phase.
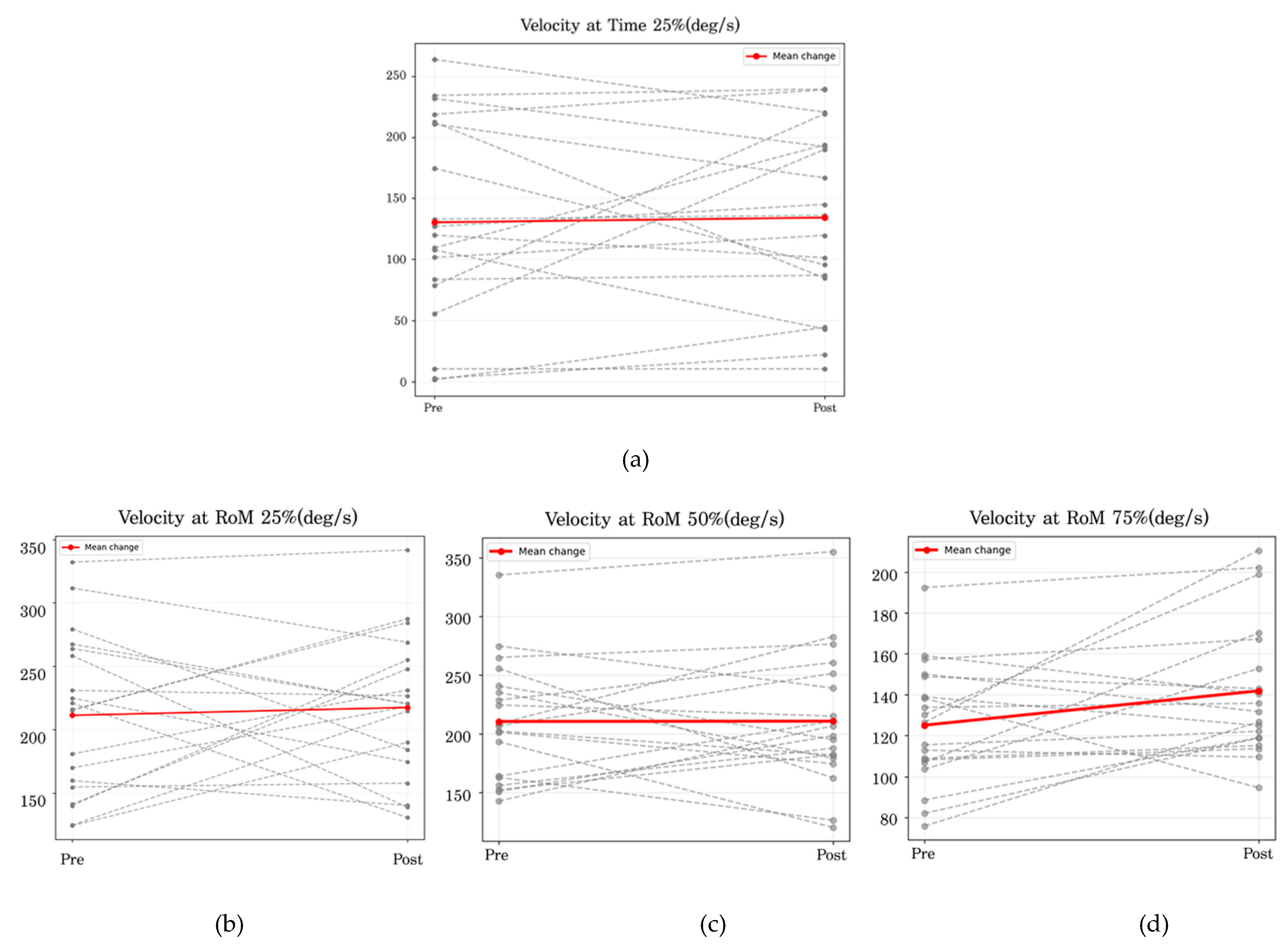
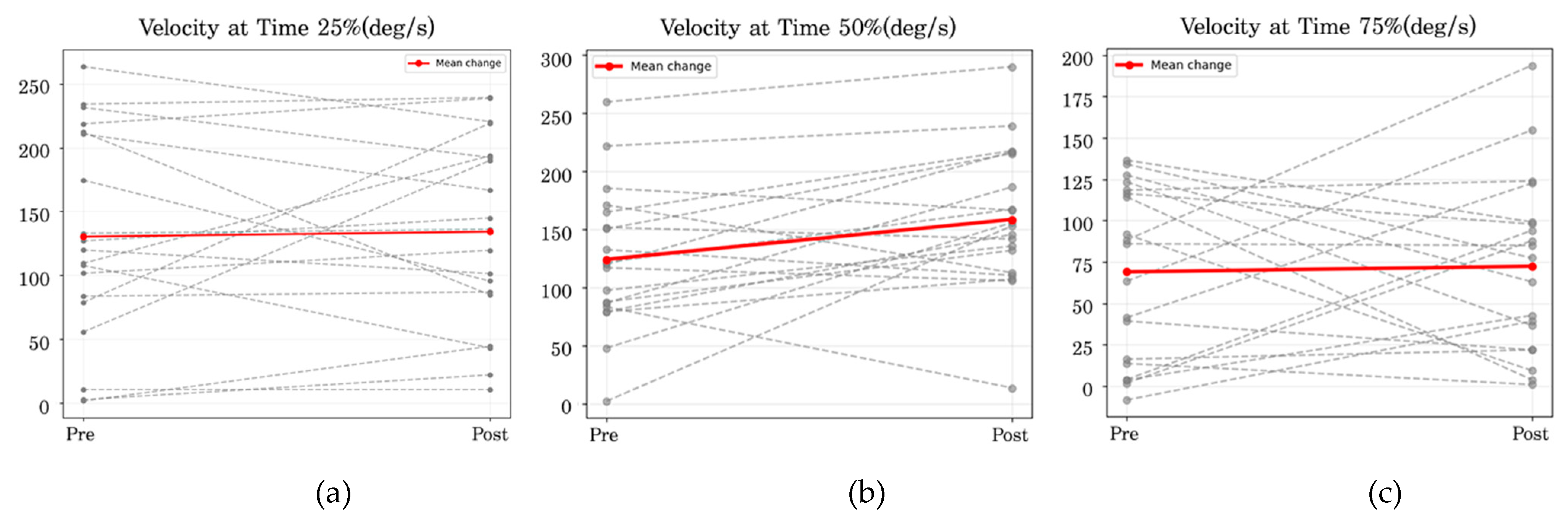
Figure 6.
Pre–post intervention angular velocity at the 25% (a), 50% (b), and 75% (c) phases.
Figure 6.
Pre–post intervention angular velocity at the 25% (a), 50% (b), and 75% (c) phases.
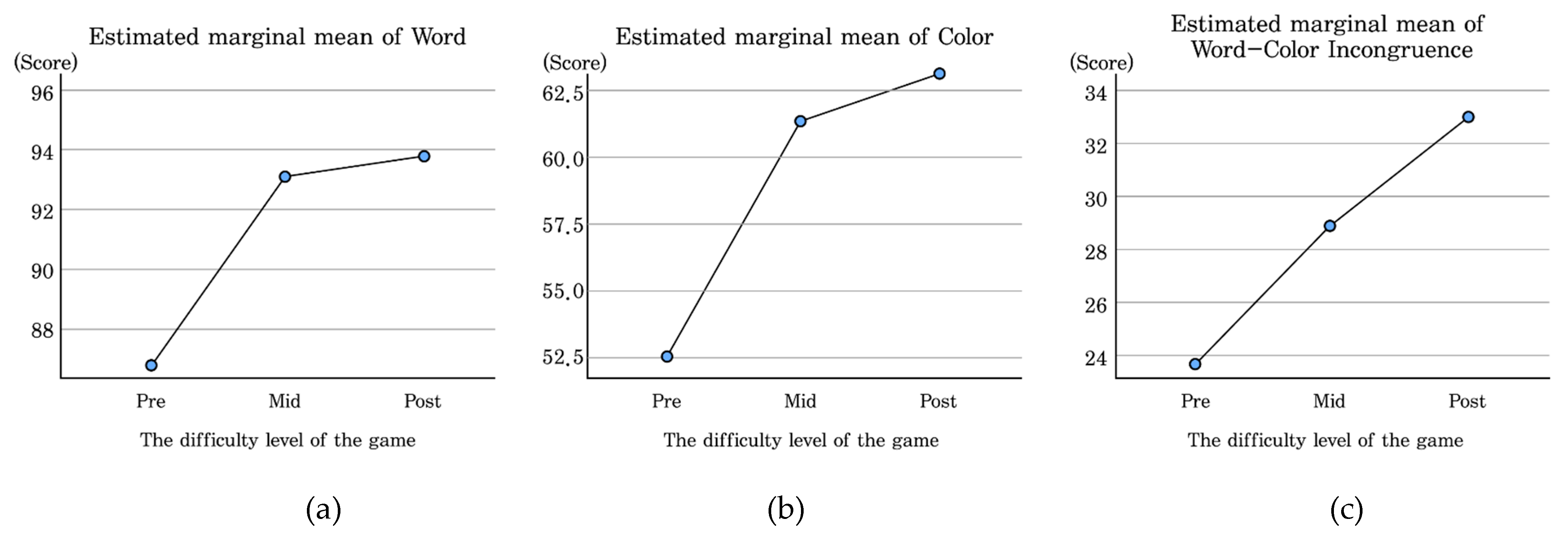
Figure 7.
Estimated marginal averages of Word (a), Color (b), and Word–Color Incongruence (c).
Figure 7.
Estimated marginal averages of Word (a), Color (b), and Word–Color Incongruence (c).
Table 1.
Expert Interviews on Program Design.
Table 1.
Expert Interviews on Program Design.
| Design Domain |
Interview Content |
Revisions and Refinements |
| Participation Motivation |
Meaningful goals and emotional interaction are critical for sustaining participation. |
Incorporation of gamification elements, immediate feedback, and interactive components within the program. |
| Assessment Tools |
Time-based functional assessments are more sensitive to detecting change than score-based tests. (2) Fall prevention requires evaluation tools that capture balance ability rather than lower-extremity strength alone. |
Adoption of functional assessments such as FSST (dynamic balance) and F8WT (curved walking). |
| Cognitive Assessment |
In addition to the general cognitive level, tools that assess cognitive processing speed and cognitive flexibility are necessary. |
Additional application of the Stroop Test. |
| Game Difficulty |
Progressive escalation of game difficulty is essential to maintain safety and sustained program engagement. |
Gradual increase in stepping-pad distance and task complexity. |
| Program Safety |
The risk of falls is highest during program execution; therefore, continuous and attentive monitoring is required. |
Continuous observation and health monitoring during program implementation. |
Table 2.
Expert Interviews on the Use of OpenCap.
Table 2.
Expert Interviews on the Use of OpenCap.
| Design Domain |
Interview Content |
Revisions and Refinements |
| Measurement Environment |
Maintaining a consistent recording environment and accurate calibration and having subjects wear tight-fitting clothing are critical for data reliability. |
Use of a consistent space and camera setup, prior calibration, and careful control of clothing conditions. |
| Recording Conditions |
Proper vertical placement of the checkerboard, sufficient recording space, and minimization of camera distortion through appropriate angle settings are essential. |
Pre-checking the measurement environment and conducting pilot tests before data collection. |
| Analytical Limitations |
Pre-checking the measurement environment and conducting pilot tests prior to data collection. |
Restricting analysis to FTSST tasks, which involve minimal leg overlap and high measurement stability. |
| Applicability |
Restricting analysis to FTSST tasks, which involve minimal leg overlap and high measurement stability. |
Conducting pre–post analyses of joint range of motion and angular velocity. |
| Applicability |
Conducting pre–post analyses of joint range of motion and angular velocity. |
Applying repetition segmentation and time normalization, followed by phase-specific analysis. |
Table 3.
Characteristics of Participants (N = 19).
Table 3.
Characteristics of Participants (N = 19).
| Measure |
Characteristics |
Number of Participants (n) |
| Gender |
Male |
4 |
| Female |
15 |
| Education Level |
Elementary school |
3 |
| Middle school |
5 |
| High school |
7 |
| University degree |
4 |
| Age |
60s |
5 |
| 70s |
13 |
| 80s |
1 |
| Cognitive Status (CIST) |
Normal |
16 |
| Suspected cognitive decline |
3 |
Table 4.
Physical Characteristics of Participants (N = 19).
Table 4.
Physical Characteristics of Participants (N = 19).
| Measure |
Mean ± SD
|
| Age (years) |
73.68 ± 2.76 |
| Height (cm) |
157.21 ± 5.09 |
| Weight (kg) |
58.09 ± 8.4 |
| BMI (kg/m²) |
23.46 ± 2.79 |
| Skeletal Muscle Mass (kg) |
21.36 ± 3.22 |
| Body Fat Mass (kg) |
18.07 ± 4.48 |
| Body Fat Percentage (%) |
30.89 ± 4.85 |
Table 5.
Assessment Tools and Measurement Timeline for Physical and Cognitive Outcomes.
Table 5.
Assessment Tools and Measurement Timeline for Physical and Cognitive Outcomes.
| Measure |
Assessment Tool |
Pre |
Mid |
Post |
| Physical |
FTSST |
O |
O |
O |
| FSST |
O |
O |
O |
| F8WT |
O |
O |
O |
| OpenCap |
O |
O |
O |
| Cognitive |
CIST |
O |
- |
O |
| Stroop Test |
O |
O |
O |
| Program Satisfaction |
|
- |
- |
O |
Table 6.
Program Overview.
Table 6.
Program Overview.
| Category |
Description |
| Program Title |
Match It! Color Step |
| Participants |
19 Participants |
| Period |
August 25, 2025–November 7, 2025 (11 weeks) |
| Sessions |
Twice per week, total of 20 sessions
(1 program orientation and practice game, 16 main program sessions, and 3 assessment sessions) |
| Session Duration |
About 50–55min |
Table 7.
Program Components and Materials.
Table 7.
Program Components and Materials.
| Title |
Game Procedure |
Game Equipment |
| Match It! Color Step |
 |
 |
Circular Marker Set Made of SEBS Material, 24cm Diameter
Styrofoam Rings |
Table 8.
Program Structure of the “Match It! Color Step” Program.
Table 8.
Program Structure of the “Match It! Color Step” Program.
| Category |
Detailed Description |
Time (min) |
| Start-Up Preparation |
Greeting (daily health check) and
attendance confirmation, warm-up exercises,
and game setup |
5 |
Individual
Exercise |
“Match It!” Color-Step game |
25 |
| Break |
Break and preparation for the next session |
5 |
Group
Exercise |
“Match It!” Color-Step game (team-based mode) |
15 |
| Closing |
Closing remarks and preview of the next session |
5 |
| Total |
- |
About
50–55 |
Table 9.
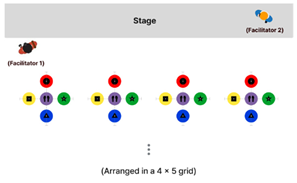
Layout of Individual and Team-Based Game Operations.
Table 9.
Layout of Individual and Team-Based Game Operations.
| Game Layout Diagram |
|---|
| Individual Mode |
Team-Based Mode |
 |
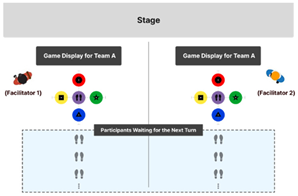 |
Table 10.
Session-Based Progression of Step-Pad Configuration and Stroop Task Difficulty.
Table 11.
Gamification Strategies Applied in the Program.
Table 11.
Gamification Strategies Applied in the Program.
| Gamification Strategies |
|---|
| Competition |
Competition with other teams, individual leaderboards |
| Achievement |
Attendance scoreboard, progression of game difficulty, sharing of task performance |
| Rewards |
Three rounds of physical and cognitive assessments, program completion certificate, gift rewards |
| Social Interaction |
Community building and interaction among program participants |
Table 12.
Changes in the Physical Performance of Participants (N = 19).
Table 12.
Changes in the Physical Performance of Participants (N = 19).
| Variable |
Pre |
Mid |
Post |
| Body weight (kg) |
58.09 ± 8.4 |
58.16 ± 8.24 |
57.72 ± 8.51 |
| BMI (kg/m ²) |
23.46 ± 2.79 |
23.37 ± 2.71 |
23.3 ± 2.88 |
| Skeletal muscle mass (kg) |
21.36 ± 3.22 |
21.57 ± 3.15 |
21.22 ± 2.91 |
| Body fat mass (kg) |
18.07 ± 4.48 |
17.7 ± 4.56 |
17.94 ± 5.1 |
| Body fat percentage (%) |
30.89 ± 4.85 |
30.25 ± 5.09 |
30.67 ± 5.52 |
Table 13.
Means and Standard Deviations of FTSST, FSST, and F8WT Scores (N = 19).
Table 13.
Means and Standard Deviations of FTSST, FSST, and F8WT Scores (N = 19).
| Variable |
Measure |
Pre |
Mid |
Post |
| Lower-extremity muscle strength |
FTSST |
9.99 ± 2.38 |
8.24 ± 1.69 |
8.48 ± 1.76 |
| Dynamic balance ability |
FSST |
10.19 ± 2.19 |
8.37 ± 1.23 |
8.13 ± 1.38 |
| Curved walking ability |
F8WT |
6.63 ± 1.12 |
5.86 ± 1.08 |
5.93 ±1.3 |
Table 14.
Repeated-Measures ANOVA Results for FTSST, FSST, and F8WT Scores (N = 19).
Table 14.
Repeated-Measures ANOVA Results for FTSST, FSST, and F8WT Scores (N = 19).
| Variable |
Type III SS |
df |
MS |
F |
p |
| FTSST |
34.245 |
2 |
17.122 |
11.754 |
< .001*** |
| FSST |
48.311 |
2 |
24.155 |
16.429 |
< .001*** |
| F8WT |
6.867 |
2 |
3.434 |
10.938 |
< .001*** |
Table 15.
Shapiro–Wilk Tests of Normality for Joint Angles and Angular Velocities (N = 19).
Table 15.
Shapiro–Wilk Tests of Normality for Joint Angles and Angular Velocities (N = 19).
| Variable |
Pre |
Post |
| RoM |
0.004** |
0.778 |
| Vel RoM 25% |
0.404 |
0.775 |
| Vel time 25% |
0.280 |
0.290 |
| Vel RoM 50% |
0.305 |
0.384 |
| Vel time 50% |
0.920 |
0.632 |
| Vel RoM 75% |
0.902 |
0.047* |
| Vel time 75% |
0.026* |
0.406 |
Table 16.
Paired-Samples t-Tests for Joint Angles and Angular Velocities at 25% and 50% Phases (N = 19).
Table 16.
Paired-Samples t-Tests for Joint Angles and Angular Velocities at 25% and 50% Phases (N = 19).
| Variable |
Pre |
Post |
t |
df |
p |
| Vel RoM 25% |
211.35 ± 63.05 |
217.53 ± 56.19 |
−0.378 |
18 |
0.710 |
| Vel time: 25% |
130.26 ± 82.23 |
134.14 ± 74.48 |
−0.253 |
18 |
0.803 |
| Vel RoM 50% |
210.33 ± 50.74 |
210.59 ± 56.76 |
−0.023 |
18 |
0.982 |
| Vel time: 50% |
124.07 ± 60.9 |
158.36 ± 61.05 |
−2.605 |
18 |
0.018* |
Table 17.
Wilcoxon Signed-Rank Tests for Overall Joint Angles and for Joint Angles and Angular Velocities at the 75% Phase (N = 19).
Table 17.
Wilcoxon Signed-Rank Tests for Overall Joint Angles and for Joint Angles and Angular Velocities at the 75% Phase (N = 19).
| Variable |
Pre |
Post |
Z |
p |
| RoM |
81.86 ± 12.82 |
83.29 ± 8.65 |
−0.483 |
0.629 |
| Vel_RoM_75% |
125.12± 29.39 |
141.93 ± 33.33 |
−1.811 |
0.07 |
| Vel_time_75% |
68.94 ± 52.55 |
72.33 ± 53.35 |
−0.161 |
0.872 |
Table 18.
Paired-Samples t-Test Results for Pre–Post Cognitive Function (N = 19).
Table 18.
Paired-Samples t-Test Results for Pre–Post Cognitive Function (N = 19).
| Variable |
Measure |
Pre |
Post |
t |
p |
| Cognitive Function |
CIST |
25.47 ± 4.2 |
28 ± 1.91 |
−2.808 |
.012* |
Table 19.
Paired-Samples t-Test Results for Subdomains of Cognitive Function (N = 19).
Table 19.
Paired-Samples t-Test Results for Subdomains of Cognitive Function (N = 19).
| Variable |
Pre |
Post |
t |
p |
| Immediate Memory |
4.89 ± 0.45 |
5.0 ± 0 |
−1.00 |
0.331 |
| Attention |
2.52 ± 0.61 |
2.57 ± 0.5 |
−0.325 |
0.749 |
| Visuospatial Ability |
1.84 ± 0.5 |
1.68 ± 0.67 |
0.900 |
0.380 |
| Executive Function |
4.31 ± 1.0 |
5.36 ± 0.89 |
−5.410 |
< 0.001*** |
| Memory Recall |
8.21 ± 2.65 |
9.68 ± 0.89 |
−2.384 |
0.028* |
| Language Ability |
3.63 ± 0.59 |
3.68 ± 0.47 |
−0.567 |
0.578 |
Table 20.
Means and Standard Deviations of the Stroop Test (N = 19).
Table 20.
Means and Standard Deviations of the Stroop Test (N = 19).
| Variable |
Pre |
Mid |
Post |
| Word |
86.89 ± 11.37 |
93.95 ± 8.93 |
94.74 ± 9.42 |
| Color |
52.42 ± 13.07 |
61.32 ± 12 |
62.11 ± 12.8 |
| Word–Color Incongruent |
23.68 ± 7.59 |
28.84± 9.33 |
32.95 ± 11.28 |
Table 21.
Repeated-Measures ANOVA Results for the Stroop Test (N = 19).
Table 21.
Repeated-Measures ANOVA Results for the Stroop Test (N = 19).
| Variable |
Type III SS |
df |
MS |
F |
p |
| Word |
708.456 |
2 |
354.228 |
10.96 |
< 0.001*** |
| Color |
1244.316 |
2 |
622.158 |
15.028 |
< 0.001*** |
| Word–Color Incongruent |
818.667 |
2 |
409.333 |
12.39 |
< 0.001*** |
Table 22.
Structure of the Program Survey Items.
Table 22.
Structure of the Program Survey Items.
| Survey Items |
Item Description |
Number of Questionnaire Items |
| Usability |
Items assessing program pace, comprehensibility, level of game difficulty,
and the facilitator’s program delivery competence |
10 |
| Usefulness |
Items comparing perceived improvements in physical and
cognitive functions before and after the program |
3 |
| Safety |
Items evaluating overall program safety |
1 |
| Sustainability |
Items assessing willingness to participate in other programs and intention to recommend the program to others |
2 |
| Open-ended Questions |
Open-ended items exploring motivation for program participation and factors influencing continued engagement |
2 |
Table 23.
Results of the Program Satisfaction Evaluation (N = 19).
Table 23.
Results of the Program Satisfaction Evaluation (N = 19).
| Survey Items |
Post |
| Usability |
4.64 ± 0.63 |
| Usefulness |
4.7 ± 0.56 |
| Safety |
4.73 ± 0.45 |
| Sustainability |
4.64 ± 0.62 |
| Total |
4.66 |