Submitted:
11 February 2026
Posted:
15 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Multi-Omics Dataset Integration
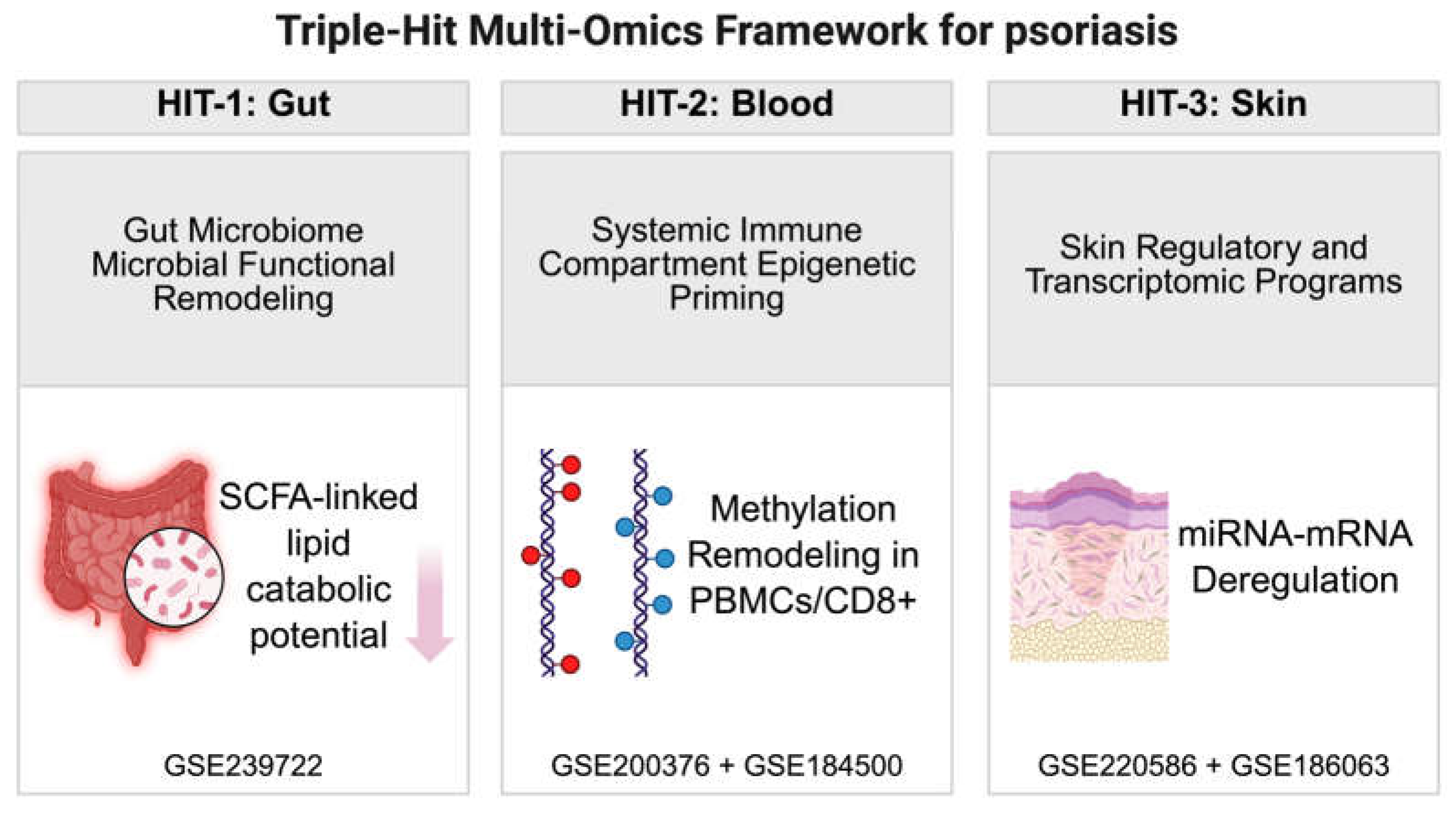
2.1.1. The “Triple-Hit” Framework Design
- Hit 1 (Putative Gut Trigger): Microbial functional remodeling and metabolic potential.
- Hit 2 (Putative Systemic Mediator): Epigenetic priming in circulating immune cells (PBMCs and CD8+ T cells).
- Hit 3 (Downstream Skin Effector): Post-transcriptional regulation and inflammatory transcriptomic programs in lesional skin.
2.1.2. Data Acquisition and Cohort Definitions
- Gut Microbiome (Metabolic Layer): Shotgun metagenomic sequencing data were obtained from GSE239722 [28]. To capture the baseline functional state without the confounding effects of systemic therapy, we selected samples from untreated psoriasis patients (PsO-UT, n = 8) and healthy controls (HC, n = 8).
- Systemic Epigenome (Epigenetic Layer): To profile systemic epigenetic alterations, we utilized two independent DNA methylation datasets generated on the Illumina Infinium MethylationEPIC BeadChip (850K) platform. For the aggregate immune state, we compared peripheral blood mononuclear cells (PBMCs) from psoriasis vulgaris patients (PsO-PB, n = 20) with healthy controls (HC, n = 19; GSE200376), while cell-type-specific epigenetic priming was investigated using purified CD8+ T cells from psoriasis patients (PsO-CD8, n = 10) and healthy controls (HC, n = 9; GSE184500) [29,30].
- Skin Transcriptome and Regulome (Effector Layer): To construct the regulatory bridge in psoriatic lesions, we integrated lesional miRNA profiles (GSE220586; PsO-L n = 4 vs HC n = 4) with lesional transcriptomic data (GSE186063; PsO-L n = 13). For the transcriptomic control group, we utilized healthy-appearing skin from patients with ankylosing spondylitis (AS-HC, n = 12), which serves as a robust non-lesional baseline to isolate the psoriasis-specific inflammatory program [31,32].
2.2. Gut Microbiome Shotgun Metagenomic Analysis (GSE239722)
2.2.1. Metagenomic Data Processing and Functional Profiling
- Assembly & Prediction: Reads were assembled into contigs using MEGAHIT and genes were predicted using MetaGeneMark.
- Gene Catalog Construction: A non-redundant gene catalog was constructed using MMseqs2 (95% identity, 90% overlap).
- Functional Annotation: Gene sequences were annotated against the KEGG database (E-value < 1e-5) to generate functional profiles.
- Normalization: The resulting gene abundance profiles were aggregated to KEGG Pathway Level 3 and normalized to relative abundance (proportions summing to 1 per sample) to correct for sequencing depth differences.
2.2.2. Statistical Analysis of Functional Remodeling
2.2.3. Lipid Degradation Functional Score
2.3. PBMC DNA Methylation Analysis (GSE200376)
2.3.1. Data Processing and Quality Control
- Detection P-value > 0.01 in any sample.
- Cross-reactive probes and probes overlapping known SNPs.
- Probes located on sex chromosomes (X, Y), to exclude sex-specific bias.
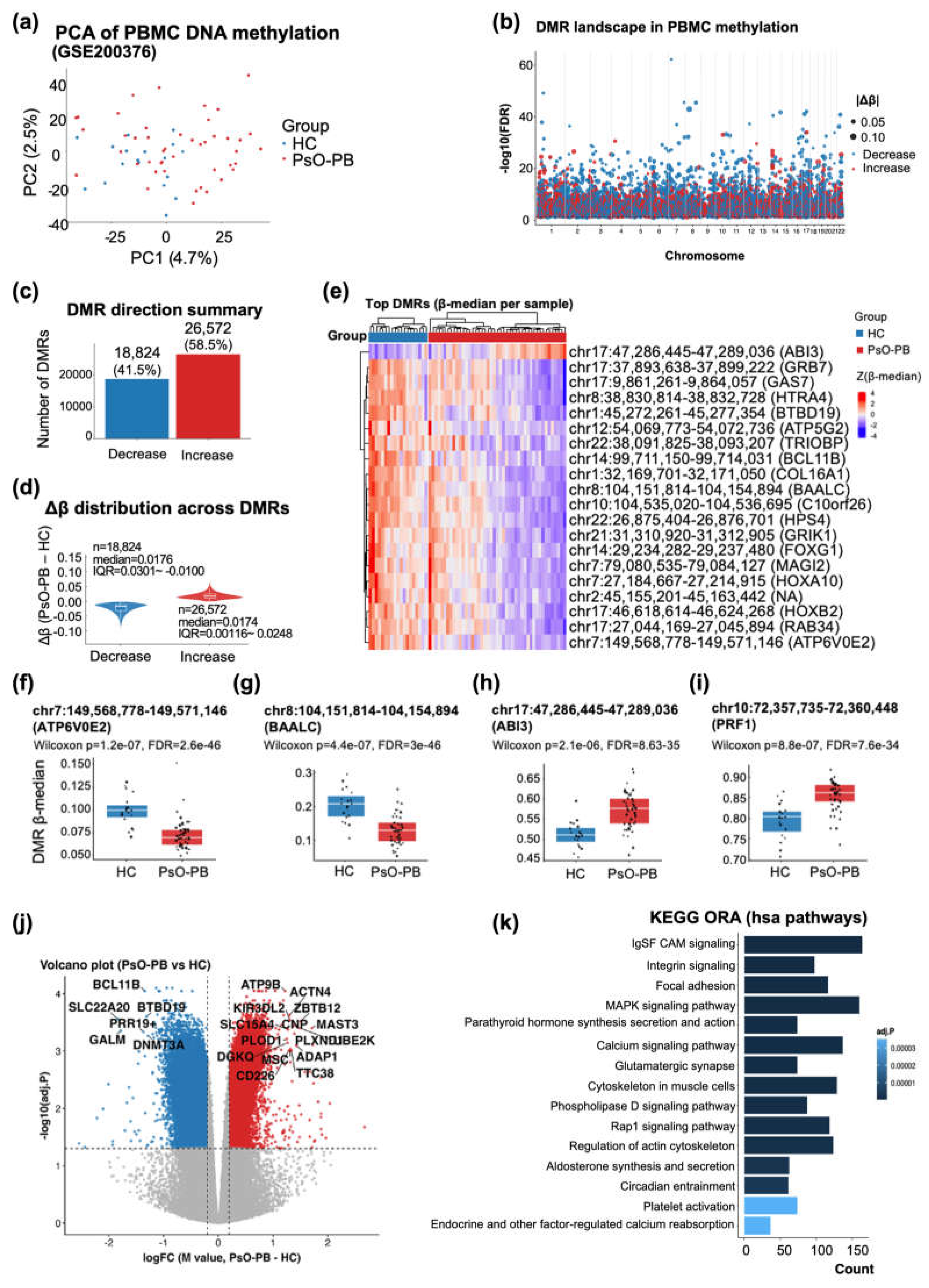
2.3.2. Identification of Systemic Epigenetic Alterations
- Cell Type Composition: Unlike tissue-specific analyses, we did not regress out cell type proportions. This decision was made to ensure that the epigenetic signature captures the aggregate systemic immune state, including the disease-associated shifts in circulating immune composition (e.g., monocytes and other myeloid populations) which is a hallmark of the “Trigger-Mediator” axis.
- Differentially Methylated Regions (DMRs): We utilized DMRcate with a Gaussian kernel smoothing (bandwidth lambda = 1000 bp, scaling factor C = 2) [39]. Significant DMRs were identified using an FDR < 0.05 threshold.
- Differentially Methylated Positions (DMPs): Single-CpG differences were assessed using limma on M-values [40]. To isolate the disease-specific effect from demographic confounders, Sex and Age were included as covariates in the linear model design matrix ( ~ Group + Sex + Age).
2.3.3. Functional Enrichment with Bias Correction
2.4. CD8+ T Cell DNA Methylation Analysis (GSE184500)
2.4.1. Data Processing and Quality Control
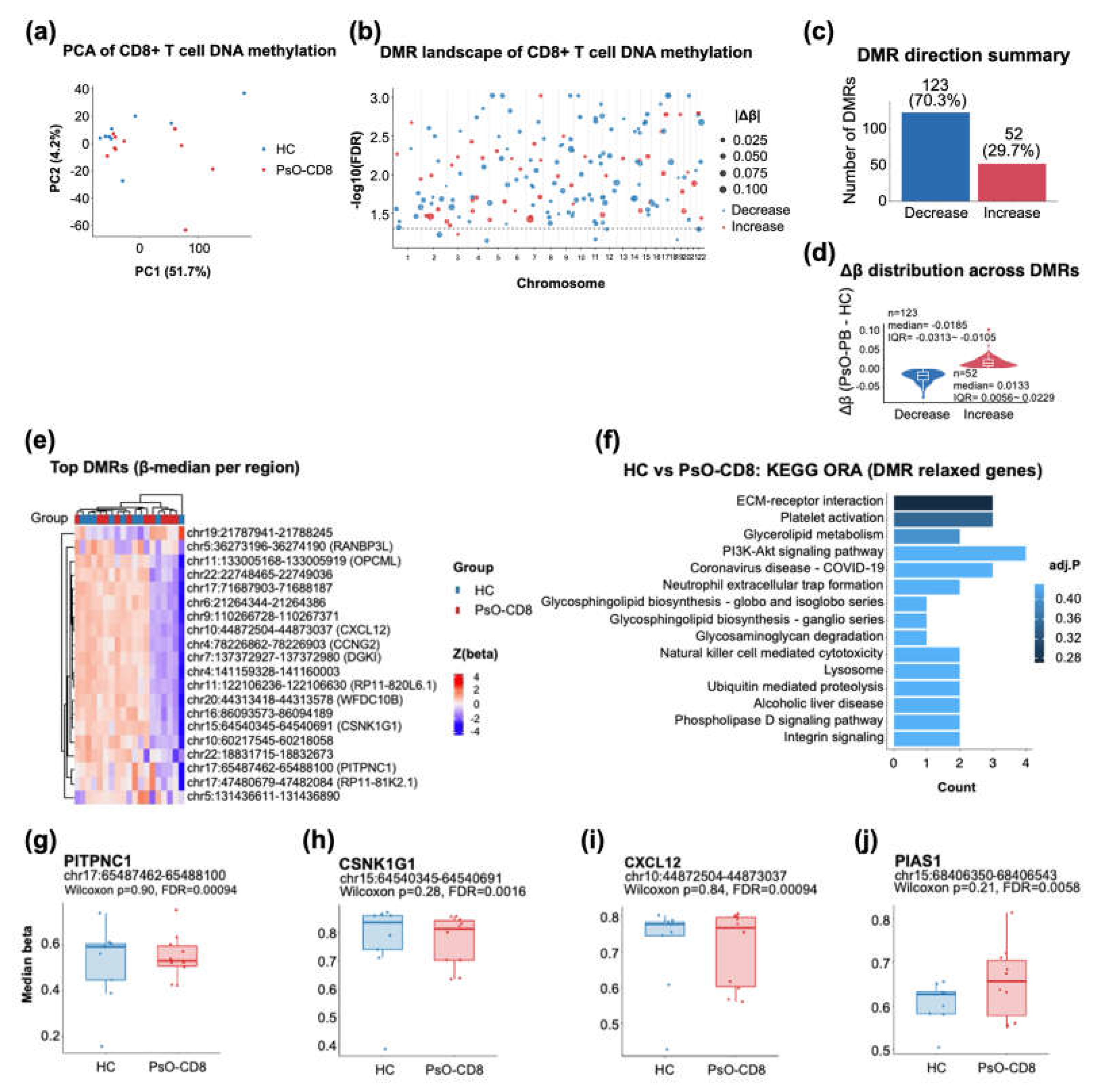
2.4.2. Identification of Differentially Methylated Regions (DMRs)
- Discovery Set: For functional enrichment and “Triple-Hit” system-level analysis, we applied a relaxed discovery threshold of FDR < 0.10 and a mean methylation difference |Δβ| ≥ 0.02.
- Visualization: For target loci visualization (Figure 4g-j), we calculated the region-median β value, representing the central methylation tendency of CpGs within each identified DMR.
2.4.3. Functional Enrichment Analysis (ORA)
2.5. Skin miRNA Expression Analysis (GSE220586)
2.5.1. Data Preprocessing and Quality Control
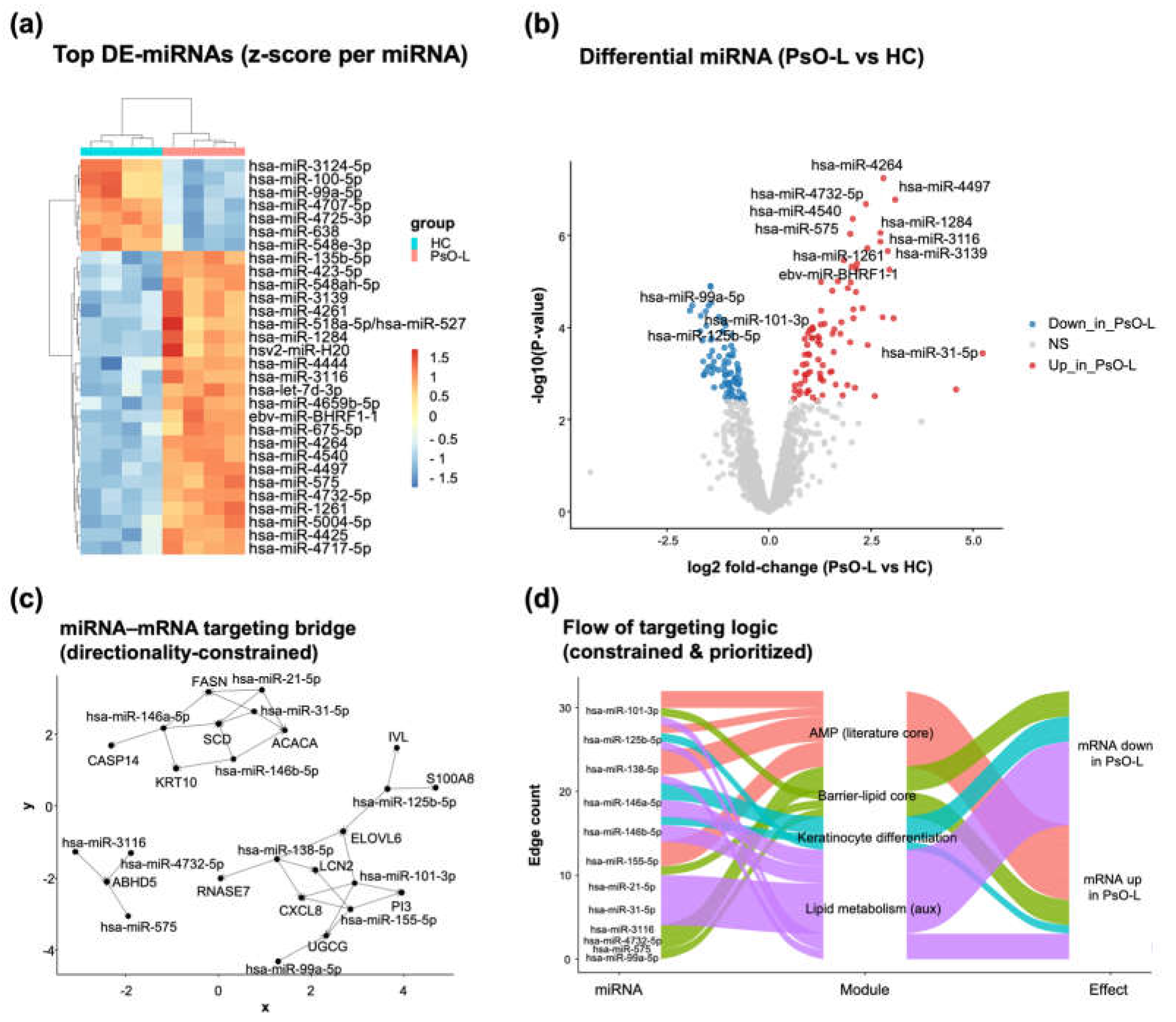
2.5.2. Differential miRNA Expression Analysis
0.05. However, to ensure that the downstream regulatory bridge focused only on biologically potent drivers, we utilized a subset of these DEMs satisfying an additional effect size threshold of
2.5.3. Multi-Tiered miRNA Target Prediction and Evidence Scoring
- Level 2 (High Confidence): Experimentally validated interactions (miRTarBase/TarBase) OR supported by ≥2 prediction databases.
- Level 1 (Moderate Confidence): Supported by multiple prediction databases but lacking experimental validation.
- Level 0 (Low Confidence): Single-database support (excluded from final analysis). Only interactions classified as Level 2 or higher were retained for the regulatory bridge analysis.
2.5.4. Directionality-constrained “Triple-Hit” Bridge Construction
- ID Mapping: Ensembl IDs from the mRNA dataset were mapped to HGNC symbols using org.Hs.eg.db.
- Directionality Constraint: We retained only pairs adhering to canonical repression logic: Upregulated miRNA (PsO-L) targeting downregulated mRNA, and downregulated miRNA (PsO-L) targeting upregulated mRNA.
- Pathological Module Filtering: The constrained pairs were mapped to predefined “Triple-Hit” effector modules: AMP Core (Literature/DEG-driven), Barrier-Lipid Core and Keratinocyte Differentiation. This filtering strategy prioritized mechanistically interpretable links over global correlation, specifically highlighting the epigenetic control of lipid metabolism and antimicrobial defense.
2.6. Skin Transcriptome Analysis (GSE186063)
2.6.1. Dataset and Preprocessing
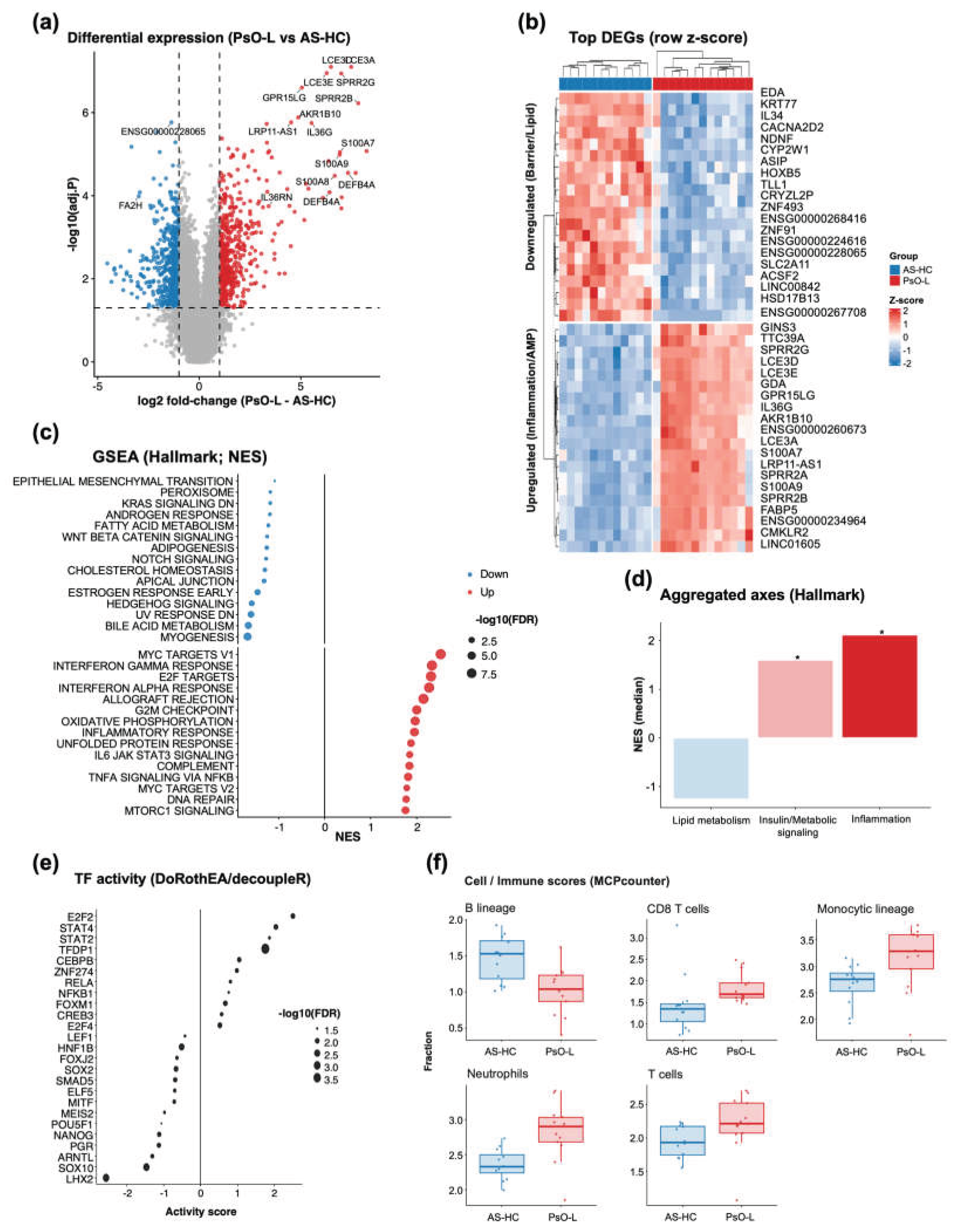
2.6.2. Differential Expression Analysis and Visualization
2.6.3. Hallmark Gene Set Enrichment Analysis and Axis-Level Aggregation
2.6.4. Transcription Factor Activity Inference
2.6.5. Immune and Stromal Cell Score Estimation (MCP-Counter)
2.7. Statistical Analysis and Visualization
3. Results
3.1. Triple-Hit Study Design and Dataset Overview for Psoriasis
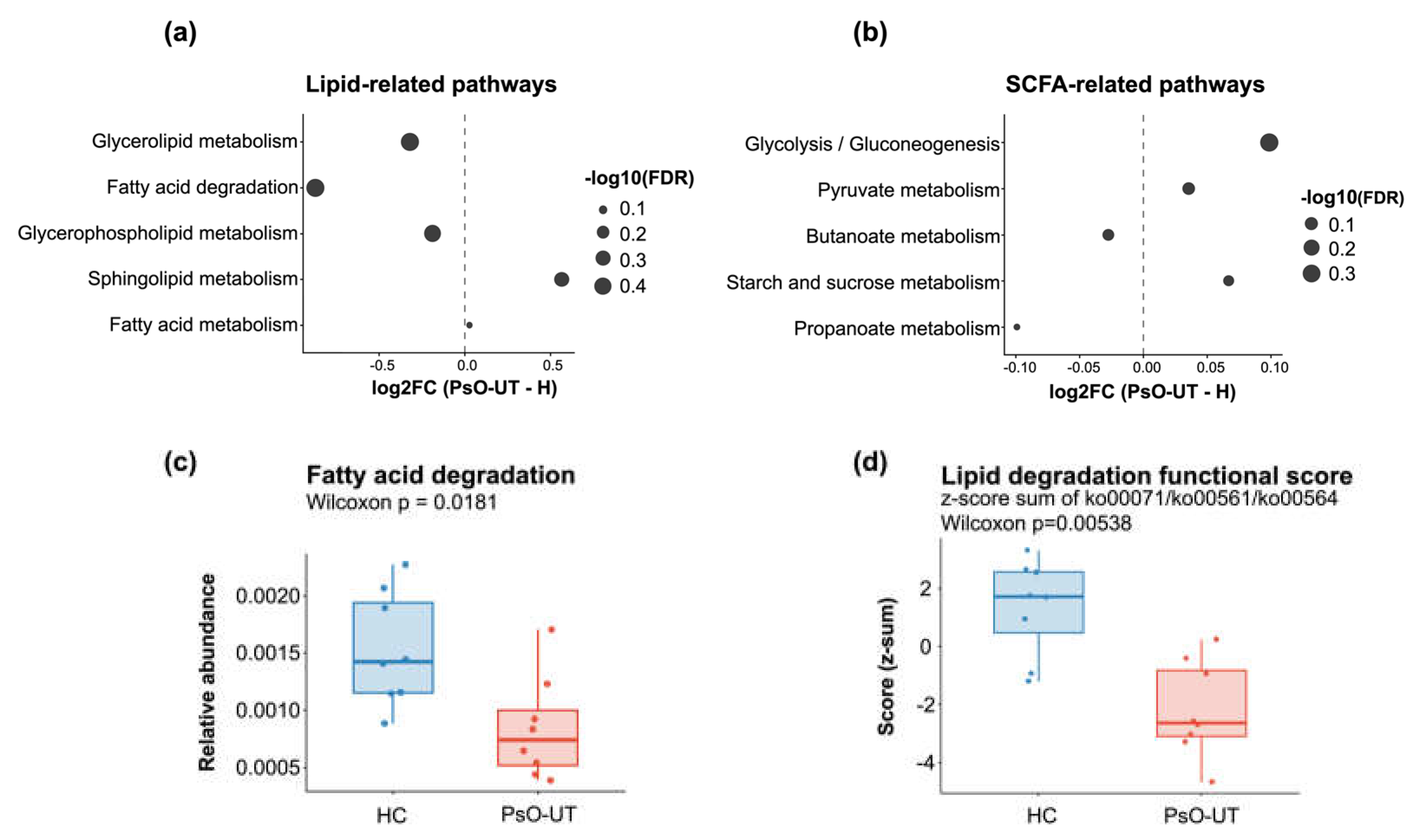
3.2. Gut Microbial Functional Remodeling in Psoriasis Reveals Reduced Lipid Catabolic Potential with Selective SCFA-Pathway Shifts
3.3. Systemic PBMC DNA Methylation Remodeling in Psoriasis (GSE200376) Highlights Widespread DMRs and Immune-State-Linked Epigenetic Priming
3.4. Directional DNA Methylation Remodeling of Circulating CD8+ T Cells in Psoriasis Reveals a Hypomethylation-Biased Regional Profile Enriched for Lipid- and Membrane-Associated Pathways (GSE184500)
3.5. Lesional miRNA Remodeling in Psoriasis and Directionality-Constrained miRNA–mRNA Bridging Aligns with AMP Activation and Barrier–Lipid/Keratinocyte Differentiation Modules (GSE220586)
3.6. Lesional Skin Transcriptomics in Psoriasis Reveals an Inflammatory-Proliferative State with Coordinated TF Activity Shifts and Immune-Cell Signature Remodeling
4. Discussion
5. Conclusions
6. Patents
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AMP | Antimicrobial peptide |
| AS-HC | Healthy-appearing skin from Ankylosing Spondylitis patients (Control) |
| BH | Benjamini-Hochberg |
| CPM | Counts Per Million |
| DEG | Differentially expressed gene |
| DE-miRNA | Differentially expressed microRNA |
| DMP | Differentially methylated position |
| DMR | Differentially methylated region |
| EPIC | Infinium MethylationEPIC BeadChip (850K) |
| FDR | False discovery rate |
| GEO | Gene Expression Omnibus |
| GO | Gene Ontology |
| GSEA | Gene set enrichment analysis |
| HC | Healthy control |
| KEGG | Kyoto Encyclopedia of Genes and Genomes |
| L2/L3 | KEGG Level 2/Level 3 functional hierarchy |
| logFC | Log2 Fold Change |
| NES | Normalized Enrichment Score |
| ORA | Over-representation analysis |
| PBMC | Peripheral blood mononuclear cell |
| PCoA | Principal coordinates analysis |
| PCA | Principal component analysis |
| PsO | Psoriasis |
| PsO-CD8 | CD8+ T cells from Psoriasis patients |
| PsO-L | Psoriatic lesional skin |
| PsO-PB | PBMCs from Psoriasis patients |
| PsO-UT | Untreated psoriasis |
| SCFA | Short-chain fatty acid |
| SRA | Sequence Read Archive |
| TF | Transcription factor |
| TMM | Trimmed Mean of M-values |
Appendix A. Definition of the Gut Lipid Degradation Functional Score (Figure 2d)
- Fatty acid degradation (ko00071)
- Glycerolipid metabolism (ko00561)
- Glycerophospholipid metabolism (ko00564)
Appendix B. Hallmark Gene Set Aggregation Logic (Figure 6d)
- Inflammation axis: grepl(“IL-17|TNF|INTERFERON|NF-KB|INFLAMM”, x, ignore.case = TRUE)
- Lipid metabolism axis: grepl(“LIPID|FATTY|SPHINGO|CHOLESTEROL”, x, ignore.case = TRUE)
- Insulin/Metabolic signaling axis: grepl(“INSULIN|PI3K|AKT|MTOR|GLYCOLYSIS”, x, ignore.case = TRUE) This rule captures anabolic and glycolysis-handling programs spanning PI3K/AKT/mTOR signaling and central carbon metabolism.
References
- Boehncke, W.-H.; Schön, M.P. Psoriasis. The Lancet 2015, 386, 983–994. [Google Scholar] [CrossRef] [PubMed]
- Nestle, F.O.; Kaplan, D.H.; Barker, J. Psoriasis. N Engl J Med 2009, 361, 496–509. [Google Scholar] [CrossRef] [PubMed]
- Codoñer, F.M.; Ramírez-Bosca, A.; Climent, E.; Carrión-Gutierrez, M.; Guerrero, M.; Pérez-Orquín, J.M.; Horga de la Parte, J.; Genovés, S.; Ramón, D.; Navarro-López, V.; et al. Gut Microbial Composition in Patients with Psoriasis. Sci Rep 2018, 8, 3812. [Google Scholar] [CrossRef]
- Branisteanu, D.E.; Pirvulescu, R.A.; Spinu, A.E.; Porumb, E.A.; Cojocaru, M.; Nicolescu, A.C.; Branisteanu, D.C.; Branisteanu, C.I.; Dimitriu, A.; Alexa, A.I.; et al. Metabolic Comorbidities of Psoriasis (Review). Experimental and Therapeutic Medicine 2022, 23, 1–7. [Google Scholar] [CrossRef] [PubMed]
- Davidovici, B.B.; Sattar, N.; Jörg, P.C.; Puig, L.; Emery, P.; Barker, J.N.; de Kerkhof, P. van; Ståhle, M.; Nestle, F.O.; Girolomoni, G.; et al. Psoriasis and Systemic Inflammatory Diseases: Potential Mechanistic Links between Skin Disease and Co-Morbid Conditions. J Invest Dermatol 2010, 130, 1785–1796. [Google Scholar] [CrossRef]
- Takeshita, J.; Grewal, S.; Langan, S.M.; Mehta, N.N.; Ogdie, A.; Voorhees, A.S.V.; Gelfand, J.M. Psoriasis and Comorbid Diseases: Epidemiology. Journal of the American Academy of Dermatology 2017, 76, 377–390. [Google Scholar] [CrossRef]
- Scher, J.U.; Ubeda, C.; Artacho, A.; Attur, M.; Isaac, S.; Reddy, S.M.; Marmon, S.; Neimann, A.; Brusca, S.; Patel, T.; et al. Decreased Bacterial Diversity Characterizes the Altered Gut Microbiota in Patients With Psoriatic Arthritis, Resembling Dysbiosis in Inflammatory Bowel Disease. Arthritis & Rheumatology 2015, 67, 128–139. [Google Scholar] [CrossRef]
- Hidalgo-Cantabrana, C.; Gómez, J.; Delgado, S.; Requena-López, S.; Queiro-Silva, R.; Margolles, A.; Coto, E.; Sánchez, B.; Coto-Segura, P. Gut Microbiota Dysbiosis in a Cohort of Patients with Psoriasis. Br J Dermatol 2019, 181, 1287–1295. [Google Scholar] [CrossRef]
- Zang, C.; Liu, J.; Mao, M.; Zhu, W.; Chen, W.; Wei, B. Causal Associations Between Gut Microbiota and Psoriasis: A Mendelian Randomization Study. Dermatol Ther (Heidelb) 2023, 13, 2331–2343. [Google Scholar] [CrossRef]
- Franzosa, E.A.; McIver, L.J.; Rahnavard, G.; Thompson, L.R.; Schirmer, M.; Weingart, G.; Lipson, K.S.; Knight, R.; Caporaso, J.G.; Segata, N.; et al. Species-Level Functional Profiling of Metagenomes and Metatranscriptomes. Nat Methods 2018, 15, 962–968. [Google Scholar] [CrossRef]
- Smith, P.M.; Howitt, M.R.; Panikov, N.; Michaud, M.; Gallini, C.A.; Bohlooly-Y, M.; Glickman, J.N.; Garrett, W.S. The Microbial Metabolites, Short Chain Fatty Acids, Regulate Colonic Treg Cell Homeostasis. Science 2013, 341, 10.1126/science.1241165. [Google Scholar] [CrossRef] [PubMed]
- Jian, T.; Craig, M.; Maria, P.; Alison N, T.; Charles R, M.; Laurence, M. The Role of Short-Chain Fatty Acids in Health and Disease. In Advances in Immunology; Academic Press, 2014; Vol. 121, pp. 91–119. [Google Scholar]
- Agus, A.; Planchais, J.; Sokol, H. Gut Microbiota Regulation of Tryptophan Metabolism in Health and Disease. Cell Host & Microbe 2018, 23, 716–724. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P.; Zhao, M.; Liang, G.; Yin, G.; Huang, D.; Su, F.; Zhai, H.; Wang, L.; Su, Y.; Lu, Q. Whole-Genome DNA Methylation in Skin Lesions from Patients with Psoriasis Vulgaris. Journal of Autoimmunity 2013, 41, 17–24. [Google Scholar] [CrossRef] [PubMed]
- Roberson, E.D.O.; Bowcock, A.M. Psoriasis Genetics: Breaking the Barrier. Trends Genet 2010, 26, 415–423. [Google Scholar] [CrossRef]
- Luo, Y.; Qu, K.; Kuai, L.; Ru, Y.; Huang, K.; Yan, X.; Xing, M. Epigenetics in Psoriasis: Perspective of DNA Methylation. Mol Genet Genomics 2021, 296, 1027–1040. [Google Scholar] [CrossRef]
- Zou, F.; Qiu, Y.; Huang, Y.; Zou, H.; Cheng, X.; Niu, Q.; Luo, A.; Sun, J. Effects of Short-Chain Fatty Acids in Inhibiting HDAC and Activating P38 MAPK Are Critical for Promoting B10 Cell Generation and Function. Cell Death Dis 2021, 12, 582. [Google Scholar] [CrossRef]
- Sanford, J.A.; Zhang, L.-J.; Williams, M.R.; Gangoiti, J.A.; Huang, C.-M.; Gallo, R.L. Inhibition of HDAC8 and HDAC9 by Microbial Short-Chain Fatty Acids Breaks Immune Tolerance of the Epidermis to TLR Ligands. Science Immunology 2016, 1, eaah4609. [Google Scholar] [CrossRef]
- Li, M.; van Esch, B.C.A.M.; Henricks, P.A.J.; Folkerts, G.; Garssen, J. The Anti-Inflammatory Effects of Short Chain Fatty Acids on Lipopolysaccharide- or Tumor Necrosis Factor α-Stimulated Endothelial Cells via Activation of GPR41/43 and Inhibition of HDACs. Front. Pharmacol. 2018, 9. [Google Scholar] [CrossRef]
- Lowes, M.A.; Suárez-Fariñas, M.; Krueger, J.G. Immunology of Psoriasis. Annu Rev Immunol 2014, 32, 227–255. [Google Scholar] [CrossRef]
- Greb, J.E.; Goldminz, A.M.; Elder, J.T.; Lebwohl, M.G.; Gladman, D.D.; Wu, J.J.; Mehta, N.N.; Finlay, A.Y.; Gottlieb, A.B. Psoriasis. Nat Rev Dis Primers 2016, 2, 16082. [Google Scholar] [CrossRef]
- Harder, J.; Schröder, J.-M. Antimicrobial Peptides in Human Skin. In Chemical Immunology and Allergy; Kabelitz, D., Schröder, J.-M., Eds.; KARGER: Basel, 2005; pp. 22–41. ISBN 978-3-8055-7862-2. [Google Scholar]
- Zenz, R.; Eferl, R.; Kenner, L.; Florin, L.; Hummerich, L.; Mehic, D.; Scheuch, H.; Angel, P.; Tschachler, E.; Wagner, E.F. Psoriasis-like Skin Disease and Arthritis Caused by Inducible Epidermal Deletion of Jun Proteins. Nature 2005, 437, 369–375. [Google Scholar] [CrossRef] [PubMed]
- Belizário, J.E. Role of Skin Antimicrobial Peptides in the Pathogenesis of Psoriasis, Atopic Dermatitis and Hidradenitis Suppurative: Highlights on Dermcidin. Clinical Immunology Communications 2025, 7, 18–26. [Google Scholar] [CrossRef]
- Christmann, C.; Zenker, S.; Martens, L.; Hübner, J.; Loser, K.; Vogl, T.; Roth, J. Interleukin 17 Promotes Expression of Alarmins S100A8 and S100A9 During the Inflammatory Response of Keratinocytes. Front. Immunol. 2021, 11. [Google Scholar] [CrossRef] [PubMed]
- Sonkoly, E.; Wei, T.; Janson, P.C.J.; Sääf, A.; Lundeberg, L.; Tengvall-Linder, M.; Norstedt, G.; Alenius, H.; Homey, B.; Scheynius, A.; et al. MicroRNAs: Novel Regulators Involved in the Pathogenesis of Psoriasis? PLOS ONE 2007, 2, e610. [Google Scholar] [CrossRef]
- O’Connell, R.M.; Rao, D.S.; Baltimore, D. microRNA Regulation of Inflammatory Responses. Annu. Rev. Immunol. 2012, 30, 295–312. [Google Scholar] [CrossRef]
- Du, X.; Yan, C.; Kong, S.; Che, D.; Peng, B.; Zhu, L.; Geng, S.; Guo, K. Successful Secukinumab Therapy in Plaque Psoriasis Is Associated with Altered Gut Microbiota and Related Functional Changes. Front. Microbiol. 2023, 14, 1227309. [Google Scholar] [CrossRef]
- Lu, Q.; Zhao, M.; Deng, M.; Su, Y. Whole Blood DNA Methylation Arrays of Individuals with Psoriatic Arthritis, Psoriasis Vulgaris, and Healthy Control Subjects (GSE200376). Gene Expression Omnibus (GEO), NCBI. Available online: https://www.ncbi.nlm.nih.gov/geo/query/acc.cgi?acc=GSE200376 (accessed on 10 February 2026).
- Charras, A.; Garau, J.; Hofmann, S.R.; Carlsson, E.; Cereda, C.; Russ, S.; Abraham, S.; Hedrich, C.M. DNA Methylation Patterns in CD8+ T Cells Discern Psoriasis From Psoriatic Arthritis and Correlate With Cutaneous Disease Activity. Front. Cell Dev. Biol. 2021, 9, 746145. [Google Scholar] [CrossRef]
- Quah, S.; Sundaram, G.M.; Subramanian, G.; Vaz, C.; Tan, J.S.L.; Kabir, R.F.; Ong, J.M.R.; Oon, H.H.; Theng, C.; Sampath, P. IL-17–Mediated Downregulation of miR-101 Facilitates the Expression of EZH2 to Promote Epidermal Hyperplasia in Psoriasis. J Invest Dermatol 2024, 144, 403–407.e7. [Google Scholar] [CrossRef]
- Deng, J.; Leijten, E.; Nordkamp, M.O.; Zheng, G.; Pouw, J.; Tao, W.; Hartgring, S.; Balak, D.; Rijken, R.; Huang, R.; et al. Multi-Omics Integration Reveals a Core Network Involved in Host Defence and Hyperkeratinization in Psoriasis. Clin Transl Med 2022, 12, e976. [Google Scholar] [CrossRef]
- Li, D.; Liu, C.-M.; Luo, R.; Sadakane, K.; Lam, T.-W. MEGAHIT: An Ultra-Fast Single-Node Solution for Large and Complex Metagenomics Assembly via Succinct de Bruijn Graph. Bioinformatics 2015, 31, 1674–1676. [Google Scholar] [CrossRef]
- Zhu, W.; Lomsadze, A.; Borodovsky, M. Ab Initio Gene Identification in Metagenomic Sequences. Nucleic Acids Res 2010, 38, e132. [Google Scholar] [CrossRef] [PubMed]
- Steinegger, M.; Söding, J. MMseqs2 Enables Sensitive Protein Sequence Searching for the Analysis of Massive Data Sets. Nat Biotechnol 2017, 35, 1026–1028. [Google Scholar] [CrossRef] [PubMed]
- Kanehisa, M.; Goto, S. KEGG: Kyoto Encyclopedia of Genes and Genomes. Nucleic Acids Res 2000, 28, 27–30. [Google Scholar] [CrossRef] [PubMed]
- Aryee, M.J.; Jaffe, A.E.; Corrada-Bravo, H.; Ladd-Acosta, C.; Feinberg, A.P.; Hansen, K.D.; Irizarry, R.A. Minfi: A Flexible and Comprehensive Bioconductor Package for the Analysis of Infinium DNA Methylation Microarrays. Bioinformatics 2014, 30, 1363–1369. [Google Scholar] [CrossRef]
- Triche, T.J., Jr.; Weisenberger, D.J.; Van Den Berg, D.; Laird, P.W.; Siegmund, K.D. Low-Level Processing of Illumina Infinium DNA Methylation BeadArrays. Nucleic Acids Res 2013, 41, e90. [Google Scholar] [CrossRef]
- Peters, T.J.; Buckley, M.J.; Statham, A.L.; Pidsley, R.; Samaras, K.; V Lord, R.; Clark, S.J.; Molloy, P.L. De Novo Identification of Differentially Methylated Regions in the Human Genome. Epigenetics & Chromatin 2015, 8, 6. [Google Scholar] [CrossRef]
- Ritchie, M.E.; Phipson, B.; Wu, D.; Hu, Y.; Law, C.W.; Shi, W.; Smyth, G.K. Limma Powers Differential Expression Analyses for RNA-Sequencing and Microarray Studies. Nucleic Acids Res 2015, 43, e47. [Google Scholar] [CrossRef]
- Wu, T.; Hu, E.; Xu, S.; Chen, M.; Guo, P.; Dai, Z.; Feng, T.; Zhou, L.; Tang, W.; Zhan, L.; et al. clusterProfiler 4.0: A Universal Enrichment Tool for Interpreting Omics Data. The Innovation 2021, 2, 100141. [Google Scholar] [CrossRef]
- Ru, Y.; Kechris, K.J.; Tabakoff, B.; Hoffman, P.; Radcliffe, R.A.; Bowler, R.; Mahaffey, S.; Rossi, S.; Calin, G.A.; Bemis, L.; et al. The multiMiR R Package and Database: Integration of microRNA–Target Interactions along with Their Disease and Drug Associations. Nucleic Acids Research 2014, 42, e133–e133. [Google Scholar] [CrossRef]
- Wong, N.; Wang, X. miRDB: An Online Resource for microRNA Target Prediction and Functional Annotations. Nucleic Acids Res 2015, 43, D146–152. [Google Scholar] [CrossRef]
- Agarwal, V.; Bell, G.W.; Nam, J.-W.; Bartel, D.P. Predicting Effective microRNA Target Sites in Mammalian mRNAs. eLife 2015, 4, e05005. [Google Scholar] [CrossRef] [PubMed]
- Cui, S.; Yu, S.; Huang, H.-Y.; Lin, Y.-C.-D.; Huang, Y.; Zhang, B.; Xiao, J.; Zuo, H.; Wang, J.; Li, Z.; et al. miRTarBase 2025: Updates to the Collection of Experimentally Validated microRNA–Target Interactions. Nucleic Acids Res 2025, 53, D147–D156. [Google Scholar] [CrossRef] [PubMed]
- Skoufos, G.; Kakoulidis, P.; Tastsoglou, S.; Zacharopoulou, E.; Kotsira, V.; Miliotis, M.; Mavromati, G.; Grigoriadis, D.; Zioga, M.; Velli, A.; et al. TarBase-v9.0 Extends Experimentally Supported miRNA–Gene Interactions to Cell-Types and Virally Encoded miRNAs. Nucleic Acids Res 2024, 52, D304–D310. [Google Scholar] [CrossRef] [PubMed]
- Karagkouni, D.; Paraskevopoulou, M.D.; Chatzopoulos, S.; Vlachos, I.S.; Tastsoglou, S.; Kanellos, I.; Papadimitriou, D.; Kavakiotis, I.; Maniou, S.; Skoufos, G.; et al. DIANA-TarBase v8: A Decade-Long Collection of Experimentally Supported miRNA–Gene Interactions. Nucleic Acids Res 2018, 46, D239–D245. [Google Scholar] [CrossRef]
- Robinson, M.D.; Oshlack, A. A Scaling Normalization Method for Differential Expression Analysis of RNA-Seq Data. Genome Biol 2010, 11, R25. [Google Scholar] [CrossRef]
- Huber, W.; Carey, V.J.; Gentleman, R.; Anders, S.; Carlson, M.; Carvalho, B.S.; Bravo, H.C.; Davis, S.; Gatto, L.; Girke, T.; et al. Orchestrating High-Throughput Genomic Analysis with Bioconductor. Nat Methods 2015, 12, 115–121. [Google Scholar] [CrossRef]
- Smyth, G.K. Linear Models and Empirical Bayes Methods for Assessing Differential Expression in Microarray Experiments. Stat Appl Genet Mol Biol 2004, 3, Article3. [Google Scholar] [CrossRef]
- Subramanian, A.; Tamayo, P.; Mootha, V.K.; Mukherjee, S.; Ebert, B.L.; Gillette, M.A.; Paulovich, A.; Pomeroy, S.L.; Golub, T.R.; Lander, E.S.; et al. Gene Set Enrichment Analysis: A Knowledge-Based Approach for Interpreting Genome-Wide Expression Profiles. Proceedings of the National Academy of Sciences 2005, 102, 15545–15550. [Google Scholar] [CrossRef]
- Mootha, V.K.; Lindgren, C.M.; Eriksson, K.-F.; Subramanian, A.; Sihag, S.; Lehar, J.; Puigserver, P.; Carlsson, E.; Ridderstråle, M.; Laurila, E.; et al. PGC-1alpha-Responsive Genes Involved in Oxidative Phosphorylation Are Coordinately Downregulated in Human Diabetes. Nat Genet 2003, 34, 267–273. [Google Scholar] [CrossRef]
- Liberzon, A.; Birger, C.; Thorvaldsdóttir, H.; Ghandi, M.; Mesirov, J.P.; Tamayo, P. The Molecular Signatures Database Hallmark Gene Set Collection. cels 2015, 1, 417–425. [Google Scholar] [CrossRef]
- Garcia-Alonso, L.; Iorio, F.; Matchan, A.; Fonseca, N.; Jaaks, P.; Peat, G.; Pignatelli, M.; Falcone, F.; Benes, C.H.; Dunham, I.; et al. Transcription Factor Activities Enhance Markers of Drug Sensitivity in Cancer. Cancer Res 2018, 78, 769–780. [Google Scholar] [CrossRef] [PubMed]
- Badia-i-Mompel, P.; Vélez Santiago, J.; Braunger, J.; Geiss, C.; Dimitrov, D.; Müller-Dott, S.; Taus, P.; Dugourd, A.; Holland, C.H.; Ramirez Flores, R.O.; et al. decoupleR: Ensemble of Computational Methods to Infer Biological Activities from Omics Data. Bioinformatics Advances 2022, 2, vbac016. [Google Scholar] [CrossRef] [PubMed]
- Becht, E.; Giraldo, N.A.; Lacroix, L.; Buttard, B.; Elarouci, N.; Petitprez, F.; Selves, J.; Laurent-Puig, P.; Sautès-Fridman, C.; Fridman, W.H.; et al. Estimating the Population Abundance of Tissue-Infiltrating Immune and Stromal Cell Populations Using Gene Expression. Genome Biol 2016, 17, 218. [Google Scholar] [CrossRef] [PubMed]
- Team, R. A Language and Environment for Statistical Computing. Computing 2006, 1. [Google Scholar] [CrossRef]
- Wickham, H. Ggplot2: Elegant Graphics for Data Analysis; Springer New York: New York, NY, 2009; ISBN 978-0-387-98140-6. [Google Scholar]
- Gu, Z.; Eils, R.; Schlesner, M. Complex Heatmaps Reveal Patterns and Correlations in Multidimensional Genomic Data. Bioinformatics 2016, 32, 2847–2849. [Google Scholar] [CrossRef]
- Kong, H.H.; Segre, J.A. Skin Microbiome: Looking Back to Move Forward. J Invest Dermatol 2012, 132, 933–939. [Google Scholar] [CrossRef]
- Furusawa, Y.; Obata, Y.; Fukuda, S.; Endo, T.A.; Nakato, G.; Takahashi, D.; Nakanishi, Y.; Uetake, C.; Kato, K.; Kato, T.; et al. Commensal Microbe-Derived Butyrate Induces the Differentiation of Colonic Regulatory T Cells. Nature 2013, 504, 446–450. [Google Scholar] [CrossRef]
- Arpaia, N.; Campbell, C.; Fan, X.; Dikiy, S.; van der Veeken, J.; deRoos, P.; Liu, H.; Cross, J.R.; Pfeffer, K.; Coffer, P.J.; et al. Metabolites Produced by Commensal Bacteria Promote Peripheral Regulatory T-Cell Generation. Nature 2013, 504, 451–455. [Google Scholar] [CrossRef]
- Frischknecht, L.; Vecellio, M.; Selmi, C. The Role of Epigenetics and Immunological Imbalance in the Etiopathogenesis of Psoriasis and Psoriatic Arthritis. Therapeutic Advances in Musculoskeletal 2019, 11, 1759720X19886505. [Google Scholar] [CrossRef]
- Nickoloff, B.J.; Qin, J.-Z.; Nestle, F.O. Immunopathogenesis of Psoriasis. Clin Rev Allergy Immunol 2007, 33, 45–56. [Google Scholar] [CrossRef]
- Cheuk, S.; Schlums, H.; Gallais Sérézal, I.; Martini, E.; Chiang, S.C.; Marquardt, N.; Gibbs, A.; Detlofsson, E.; Introini, A.; Forkel, M.; et al. CD49a Expression Defines Tissue-Resident CD8+ T Cells Poised for Cytotoxic Function in Human Skin. Immunity 2017, 46, 287–300. [Google Scholar] [CrossRef]
- Swindell, W.R.; Johnston, A.; Carbajal, S.; Han, G.; Wohn, C.; Lu, J.; Xing, X.; Nair, R.P.; Voorhees, J.J.; Elder, J.T.; et al. Genome-Wide Expression Profiling of Five Mouse Models Identifies Similarities and Differences with Human Psoriasis. PLOS ONE 2011, 6, e18266. [Google Scholar] [CrossRef]
- Li, B.; Tsoi, L.C.; Swindell, W.R.; Gudjonsson, J.E.; Tejasvi, T.; Johnston, A.; Ding, J.; Stuart, P.E.; Xing, X.; Kochkodan, J.J.; et al. Transcriptome Analysis of Psoriasis in a Large Case-Control Sample: RNA-Seq Provides Insights into Disease Mechanisms. J Invest Dermatol 2014, 134, 1828–1838. [Google Scholar] [CrossRef]
- Hawkes, J.E.; Nguyen, G.H.; Fujita, M.; Florell, S.R.; Callis Duffin, K.; Krueger, G.G.; O’Connell, R.M. microRNAs in Psoriasis. J Invest Dermatol 2016, 136, 365–371. [Google Scholar] [CrossRef]
- Armstrong, A.W.; Blauvelt, A.; Callis Duffin, K.; Huang, Y.-H.; Savage, L.J.; Guo, L.; Merola, J.F. Psoriasis. Nat Rev Dis Primers 2025, 11, 45. [Google Scholar] [CrossRef]
| Layer | Dataset | Omics/Platform | Groups used (n) | Key outputs |
| Gut microbiome | GSE239722 | Shotgun metagenomics |
HC (n=8), PsO-UT 1 (n=8) | Taxonomy; functional profiling (KEGG L2/L3, GO) |
| Systemic (PBMC) | GSE200376 | DNA methylation (EPIC 850K) | HC (n=19), PsO-PB 2 (n=20) | DMP/DMR; promoter focused enrichment |
| Systemic (CD8+ T) | GSE184500 | DNA methylation (EPIC 850K) | HC (n=9), PsO-CD8 3 (n=10) | Cell-type EWAS; DMP/DMR |
| Skin (miRNA) | GSE220586 | miRNA array | HC (n=4), PsO-L 4 (n=4) | DE-miRNA; target inference (TargetScan/miRDB) |
| Skin transcriptome | GSE186063 | Bulk RNA-seq | AS-HC 5 (n=12), PsO-L (n=13) | DEGs; AMP program; Immune/stromal deconvolution (MCP-counter) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




