Submitted:
11 February 2026
Posted:
12 February 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods
- -
- hormones: free Triiodothyronine (fT3), free Thyroxine (fT4), Thyroid-Stimulating Hormone (TSH), Growth Hormone (GH), Insuline-like Growth Factor 1 (IGF-1), Prolactine (PRL), Adrenocorticotropic Hormone (ACTH). Reference ranges: TSH 0.35–4.94 uU/ml; fT3 1.78–7.07pmol/l; fT4 9.01–19.05pmol/l, GH <8 ng/ml, IGF-1 89-290 ng/ml, PRL 108.8-557.1 mU/l, ACTH
- -
- Gonadotropic hormones were initially also assessed. However, due to the small size of the study cohort and the relatively high prevalence of confounding factors that could compromise the scientific validity of the collected data—including uncertain menopausal status, use of hormonal contraception, testosterone replacement therapy, and preparation for gender-affirming treatment—these data were excluded from the final analysis. Consequently, the scope of the study was restricted to hormones directly associated with symptoms that may mimic post-concussion syndrome, such as cognitive impairment, fatigue, and related mood fluctuations.
- -
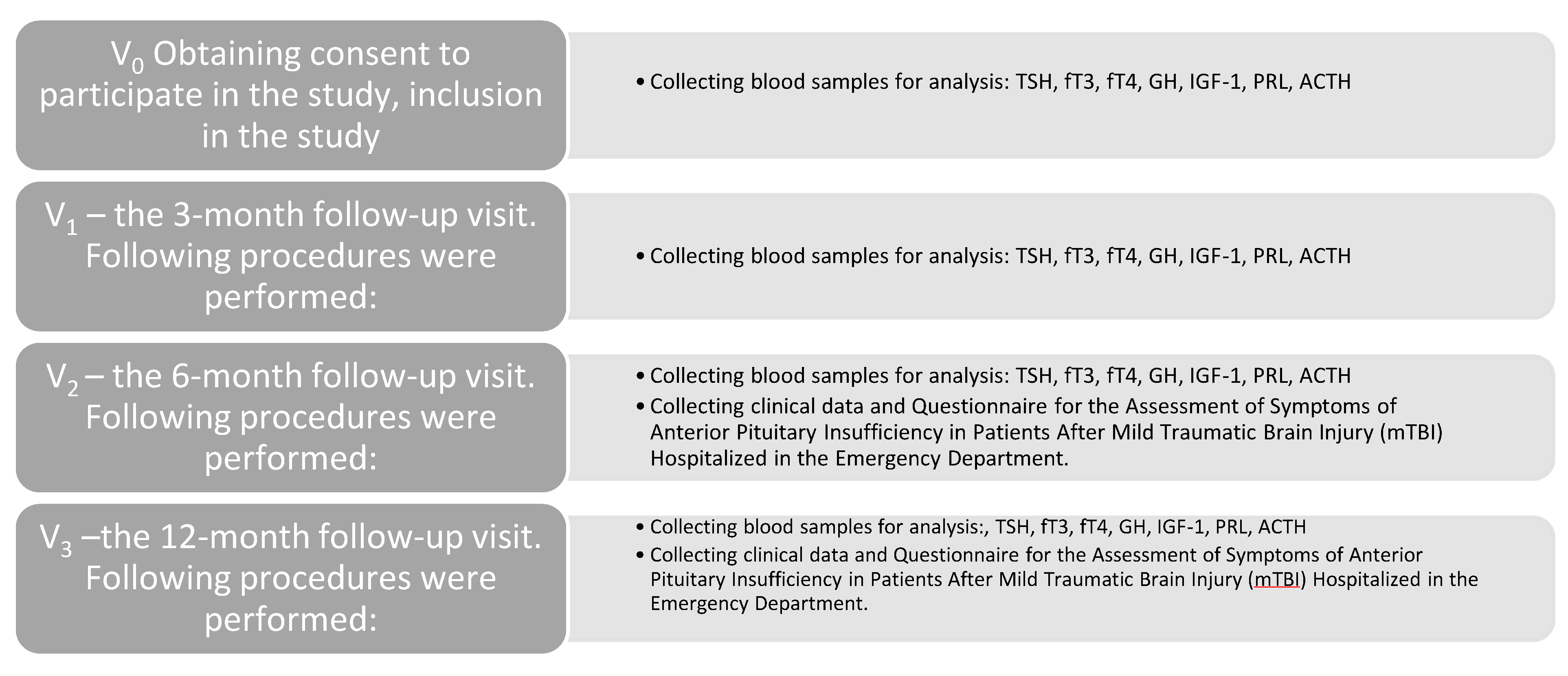
- Obtaining consent to participate in the study, inclusion in the study
- -
- Collecting blood samples for analysis: TSH, fT3, fT4, GH, IGF-1, PRL, ACTH
- -
- Collecting blood samples for analysis: TSH, fT3, fT4, GH, IGF-1, PRL, ACTH
- -
- Collecting blood samples for analysis: TSH, fT3, fT4, GH, IGF-1, PRL, ACTH
- -
- Collecting clinical data and Questionnaire for the Assessment of Symptoms of Anterior Pituitary Insufficiency in Patients After Mild Traumatic Brain Injury (mTBI) Hospitalized in the Emergency Department.
- -
- Collecting blood samples for analysis: TSH, fT3, fT4, GH, IGF-1, PRL, ACTH
- -
- Collecting clinical data and Questionnaire for the Assessment of Symptoms of Anterior Pituitary Insufficiency in Patients After Mild Traumatic Brain Injury (mTBI) Hospitalized in the Emergency Department.
Statistical Analysis
3. Results
4. Discussion
5. Conclusions
6. Limitations
Author Contributions
Informed Consent Statement
Data Availability Statement
Abbreviations
| ACTH | adrenocortycotropic hormone |
| CLIA | chemiluminescent immunoassay |
| CMIA | heterogenous immunochemiluminescence |
| ESS | euthyroid sick syndrome |
| fT3 | free triiodothyronine |
| GH | growth hormone |
| IGF-1 | insulin-like growth factor 1 |
| mTBI | mild traumatic brain injury |
| NTIS | non thyroidal illness syndrome |
| PRL | prolactin |
| PTHP | post traumatic hypopituitarism |
| T3 | triiodothyronine |
| TSH | thyroid-stimulating hormone |
| TH | thyroid hormones |
References
- Capizzi, A.; Woo, J.; Verduzco-Gutierrez, M. Traumatic Brain Injury: An Overview of Epidemiology, Pathophysiology, and Medical Management. Med Clin North Am 2020, 104, 213–238. [Google Scholar] [CrossRef]
- Kgosidialwa, O.; Agha, A. Hypopituitarism Post Traumatic Brain Injury (TBI): Review. Ir J Med Sci 2019, 188, 1201–1206. [Google Scholar] [CrossRef] [PubMed]
- Manley, G.T.; Dams-O’Connor, K.; Alosco, M.L.; Awwad, H.O.; Bazarian, J.J.; Bragge, P.; Corrigan, J.D.; Doperalski, A.; Ferguson, A.R.; Mac Donald, C.L.; et al. A New Characterisation of Acute Traumatic Brain Injury: The NIH-NINDS TBI Classification and Nomenclature Initiative. The Lancet Neurology 2025, 24, 512–523. [Google Scholar] [CrossRef]
- Brazinova, A.; Rehorcikova, V.; Taylor, M.S.; Buckova, V.; Majdan, M.; Psota, M.; Peeters, W.; Feigin, V.; Theadom, A.; Holkovic, L.; et al. Epidemiology of Traumatic Brain Injury in Europe: A Living Systematic Review. J Neurotrauma 2021, 38, 1411–1440. [Google Scholar] [CrossRef]
- Maas, A.I.R.; Menon, D.K.; Manley, G.T.; Abrams, M.; Åkerlund, C.; Andelic, N.; Aries, M.; Bashford, T.; Bell, M.J.; Bodien, Y.G.; et al. Traumatic Brain Injury: Progress and Challenges in Prevention, Clinical Care, and Research. Lancet Neurol 2022, 21, 1004–1060. [Google Scholar] [CrossRef]
- Wilson, L.; Stewart, W.; Dams-O’Connor, K.; Diaz-Arrastia, R.; Horton, L.; Menon, D.K.; Polinder, S. The Chronic and Evolving Neurological Consequences of Traumatic Brain Injury. Lancet Neurol 2017, 16, 813–825. [Google Scholar] [CrossRef]
- Pavlovic, D.; Pekic, S.; Stojanovic, M.; Popovic, V. Traumatic Brain Injury: Neuropathological, Neurocognitive and Neurobehavioral Sequelae. Pituitary 2019, 22, 270–282. [Google Scholar] [CrossRef]
- Dams-O’Connor, K.; Juengst, S.B.; Bogner, J.; Chiaravalloti, N.D.; Corrigan, J.D.; Giacino, J.T.; Harrison-Felix, C.L.; Hoffman, J.M.; Ketchum, J.M.; Lequerica, A.H.; et al. Traumatic Brain Injury as a Chronic Disease: Insights from the United States Traumatic Brain Injury Model Systems Research Program. Lancet Neurol 2023, 22, 517–528. [Google Scholar] [CrossRef]
- Gasco, V.; Cambria, V.; Bioletto, F.; Ghigo, E.; Grottoli, S. Traumatic Brain Injury as Frequent Cause of Hypopituitarism and Growth Hormone Deficiency: Epidemiology, Diagnosis, and Treatment. Frontiers in Endocrinology 2021, 12–2021. [Google Scholar] [CrossRef]
- Wexler, T.L. Neuroendocrine Disruptions Following Head Injury. Curr Neurol Neurosci Rep 2023, 23, 213–224. [Google Scholar] [CrossRef]
- Bensalah, M.; Donaldson, M.; Labassen, M.; Cherfi, L.; Nebbal, M.; Haffaf, E.M.; Abdennebi, B.; Guenane, K.; Kemali, Z.; Ould Kablia, S. Prevalence of Hypopituitarism and Quality of Life in Survivors of Post-Traumatic Brain Injury. Endocrinol Diabetes Metab 2020, 3, e00146. [Google Scholar] [CrossRef]
- Tan, C.L.; Hutchinson, P.J. A Neurosurgical Approach to Traumatic Brain Injury and Post-Traumatic Hypopituitarism. Pituitary 2019, 22, 332–337. [Google Scholar] [CrossRef]
- Kgosidialwa, O.; Hakami, O.; Muhammad Zia-Ul-Hussnain, H.; Agha, A. Growth Hormone Deficiency Following Traumatic Brain Injury. Int J Mol Sci 2019, 20. [Google Scholar] [CrossRef]
- Tanriverdi, F.; Schneider, H.J.; Aimaretti, G.; Masel, B.E.; Casanueva, F.F.; Kelestimur, F. Pituitary Dysfunction after Traumatic Brain Injury: A Clinical and Pathophysiological Approach. Endocr Rev 2015, 36, 305–342. [Google Scholar] [CrossRef]
- Karaboue, M.A.A.; Ministeri, F.; Sessa, F.; Nannola, C.; Chisari, M.G.; Cocimano, G.; Di Mauro, L.; Salerno, M.; Esposito, M. Traumatic Brain Injury as a Public Health Issue: Epidemiology, Prognostic Factors and Useful Data from Forensic Practice. Healthcare (Basel) 2024, 12. [Google Scholar] [CrossRef]
- De Bellis, A.; Bellastella, G.; Maiorino, M.I.; Costantino, A.; Cirillo, P.; Longo, M.; Pernice, V.; Bellastella, A.; Esposito, K. The Role of Autoimmunity in Pituitary Dysfunction Due to Traumatic Brain Injury. Pituitary 2019, 22, 236–248. [Google Scholar] [CrossRef]
- Mele, C.; Pingue, V.; Caputo, M.; Zavattaro, M.; Pagano, L.; Prodam, F.; Nardone, A.; Aimaretti, G.; Marzullo, P. Neuroinflammation and Hypothalamo-Pituitary Dysfunction: Focus of Traumatic Brain Injury. Int J Mol Sci 2021, 22. [Google Scholar] [CrossRef] [PubMed]
- The Autoimmune Basis of Hypopituitarism in Traumatic Brain Injury: Fiction or Reality? England, 2019; Vol. 33.
- Hacioglu, A.; Kelestimur, F.; Tanriverdi, F. Long-Term Neuroendocrine Consequences of Traumatic Brain Injury and Strategies for Management. Expert Rev Endocrinol Metab 2020, 15, 123–139. [Google Scholar] [CrossRef] [PubMed]
- Schneider, H.J.; Schneider, M.; Saller, B.; Petersenn, S.; Uhr, M.; Husemann, B.; von Rosen, F.; Stalla, G.K. Prevalence of Anterior Pituitary Insufficiency 3 and 12 Months after Traumatic Brain Injury. Eur J Endocrinol 2006, 154, 259–265. [Google Scholar] [CrossRef] [PubMed]
- Fleseriu, M.; Christ-Crain, M.; Langlois, F.; Gadelha, M.; Melmed, S. Hypopituitarism. Lancet 2024, 403, 2632–2648. [Google Scholar] [CrossRef]
- Klose, M.; Feldt-Rasmussen, U. Chronic Endocrine Consequences of Traumatic Brain Injury - What Is the Evidence? Nat Rev Endocrinol 2018, 14, 57–62. [Google Scholar] [CrossRef]
- Schneider, H.J.; Kreitschmann-Andermahr, I.; Ghigo, E.; Stalla, G.K.; Agha, A. Hypothalamopituitary Dysfunction Following Traumatic Brain Injury and Aneurysmal Subarachnoid Hemorrhage: A Systematic Review. JAMA 2007, 298, 1429–1438. [Google Scholar] [CrossRef]
- Silverberg, N.D.; Iverson, G.L.; Cogan, A.; Dams-O-Connor, K.; Delmonico, R.; Graf, M.J.P.; Iaccarino, M.A.; Kajankova, M.; Kamins, J.; McCulloch, K.L.; et al. The American Congress of Rehabilitation Medicine Diagnostic Criteria for Mild Traumatic Brain Injury. Arch Phys Med Rehabil 2023, 104, 1343–1355. [Google Scholar] [CrossRef] [PubMed]
- Woolf, P.D. Hormonal Responses to Trauma. Crit Care Med 1992, 20, 216–226. [Google Scholar] [CrossRef]
- Warner, M.H.; Beckett, G.J. Mechanisms behind the Non-Thyroidal Illness Syndrome: An Update. Journal of Endocrinology 2010, 205, 1–13. [Google Scholar] [CrossRef] [PubMed]
- Nourollahi, S.; Wille, J.; Weiß, V.; Wedekind, C.; Lippert-Grüner, M. Quality-of-Life in Patients with Post-Traumatic Hypopituitarism. Brain Inj 2014, 28, 1425–1429. [Google Scholar] [CrossRef] [PubMed]
- Talhada, D.; Santos, C.R.A.; Gonçalves, I.; Ruscher, K. Thyroid Hormones in the Brain and Their Impact in Recovery Mechanisms After Stroke. Front Neurol 2019, 10, 1103. [Google Scholar] [CrossRef]
- Liu, Y.-Y.; Brent, G.A. The Role of Thyroid Hormone in Neuronal Protection. Comprehensive Physiology 2021, 11, 2075–2095. [Google Scholar] [CrossRef]
- Mele, C.; De Marchi, L.; Pitino, R.; Costantini, L.; Cavigiolo, B.; Caputo, M.; Marzullo, P.; Aimaretti, G. The Interplay between Thyrotropic Axis, Neurological Complications, and Rehabilitation Outcomes in Patients with Traumatic Brain Injury. Best Pract Res Clin Endocrinol Metab 2025, 39, 102001. [Google Scholar] [CrossRef]
- Rovet, J.F. The Role of Thyroid Hormones for Brain Development and Cognitive Function. Endocr Dev 2014, 26, 26–43. [Google Scholar] [CrossRef]
- Fernández Rodriguez, E.; Villar Taibo, R.; Bernabeu, I. Hypopituitarism after Traumatic Brain Injury in Adults: Clinical Guidelines of the Neuroendocrinology Area of the Spanish Society of Endocrinology and Nutrition (SEEN). Endocrinol Diabetes Nutr (Engl Ed) 2023, 70, 584–591. [Google Scholar] [CrossRef]
- Malekpour, B.; Mehrafshan, A.; Saki, F.; Malekmohammadi, Z.; Saki, N. Effect of Posttraumatic Serum Thyroid Hormone Levels on Severity and Mortality of Patients with Severe Traumatic Brain Injury. Acta Med Iran 2012, 50, 113–116. [Google Scholar] [PubMed]
- Zhang, M.; Wei, J.-B.; Zhang, X.-B. Influence of Traumatic Brain Injury on Serum Levels of Pituitary, Thyroid, Adrenal and Gonadal Hormones. Medicine 2025, 104. [Google Scholar] [CrossRef]
- Mele, C.; Pagano, L.; Franciotta, D.; Caputo, M.; Nardone, A.; Aimaretti, G.; Marzullo, P.; Pingue, V. Thyroid Function in the Subacute Phase of Traumatic Brain Injury: A Potential Predictor of Post-Traumatic Neurological and Functional Outcomes. J Endocrinol Invest 2022, 45, 379–389. [Google Scholar] [CrossRef] [PubMed]
- Mele, C.; Bagnato, S.; De Tanti, A.; Lucca, L.F.; Saviola, D.; Marcuccio, L.; Moretta, P.; Scarponi, F.; Losavio, E.; Picciola, E.; et al. Free Thyroxine (fT4) as a Potential Biomarker of Neurological and Functional Outcome in Acquired Brain Injury: A Prospective Multicenter Cohort Study. J Clin Med 2023, 12. [Google Scholar] [CrossRef] [PubMed]
- Khandelwal, M.; Ying, Z.; Gomez-Pinilla, F. Thyroid Hormone T4 Alleviates Traumatic Brain Injury by Enhancing Blood–Brain Barrier Integrity. International Journal of Molecular Sciences 2025, 26. [Google Scholar] [CrossRef]
- Li, J.; Donangelo, I.; Abe, K.; Scremin, O.; Ke, S.; Li, F.; Milanesi, A.; Liu, Y.-Y.; Brent, G.A. Thyroid Hormone Treatment Activates Protective Pathways in Both in Vivo and in Vitro Models of Neuronal Injury. Molecular and cellular endocrinology 2017, 452, 120–130. [Google Scholar] [CrossRef]
- Crupi, R.; Paterniti, I.; Campolo, M.; Di Paola, R.; Cuzzocrea, S.; Esposito, E. Exogenous T3 Administration Provides Neuroprotection in a Murine Model of Traumatic Brain Injury. Pharmacological research 2013, 70, 80–89. [Google Scholar] [CrossRef]
- Lin, C.; Li, N.; Chang, H.; shen, Y.; Li, Z.; wei, W.; Chen, H.; Lu, H.; Ji, J.; Liu, N. Dual Effects of Thyroid Hormone on Neurons and Neurogenesis in Traumatic Brain Injury. Cell Death & Disease 2020, 11, 671. [Google Scholar] [CrossRef]
- Fliers, E.; Boelen, A. An Update on Non-Thyroidal Illness Syndrome. J Endocrinol Invest 2021, 44, 1597–1607. [Google Scholar] [CrossRef]
- Rolih, C.A.; Ober, K.P. The Endocrine Response to Critical Illness. Med Clin North Am 1995, 79, 211–224. [Google Scholar] [CrossRef]
- Eggertsdóttir Claessen, L.Ó.; Kristjánsdóttir, H.; Jónsdóttir, M.K.; Lund, S.H.; Unnsteinsdóttir Kristensen, I.; Sigurjónsdóttir, H.Á. Pituitary Dysfunction Following Mild Traumatic Brain Injury in Female Athletes. Endocr Connect 2024, 13, e230363. [Google Scholar] [CrossRef]
- Aljboor, G.S.; Tulemat, A.; Al-Saedi, A.R.; Radoi, M.P.; Toader, C.; Papacocea, T.M. Acute and Chronic Hypopituitarism Following Traumatic Brain Injury: A Systematic Review and Meta-Analysis. Neurosurg Rev 2024, 47, 841. [Google Scholar] [CrossRef]
- Jung, S.J.; Kang, J.H.; Roberts, A.L.; Nishimi, K.; Chen, Q.; Sumner, J.A.; Kubzansky, L.; Koenen, K.C. Posttraumatic Stress Disorder and Incidence of Thyroid Dysfunction in Women. Psychological Medicine 2019, 49, 2551–2560. [Google Scholar] [CrossRef] [PubMed]
- Stochholm, K.; Gravholt, C.H.; Laursen, T.; Jørgensen, J.O.; Laurberg, P.; Andersen, M.; Kristensen, L.Ø.; Feldt-Rasmussen, U.; Christiansen, J.S.; Frydenberg, M.; et al. Incidence of GH Deficiency - a Nationwide Study. Eur J Endocrinol 2006, 155, 61–71. [Google Scholar] [CrossRef] [PubMed]
- Magyar-Sumegi, Z.D.; Stankovics, L.; Lendvai-Emmert, D.; Czigler, A.; Hegedus, E.; Csendes, M.; Toth, L.; Ungvari, Z.; Buki, A.; Toth, P. Acute Neuroendocrine Changes after Traumatic Brain Injury. Brain and Spine 2024, 4, 102830. [Google Scholar] [CrossRef]
- Yousefvand, S.; Hadjzadeh, M.-A.-R.; Vafaee, F.; Dolatshad, H. The Protective Effects of Prolactin on Brain Injury. Life Sci 2020, 263, 118547. [Google Scholar] [CrossRef] [PubMed]
- Elgellaie, A.; Larkin, T.; Kaelle, J.; Mills, J.; Thomas, S. Plasma Prolactin Is Higher in Major Depressive Disorder and Females, and Associated with Anxiety, Hostility, Somatization, Psychotic Symptoms and Heart Rate. Compr Psychoneuroendocrinol 2021, 6, 100049. [Google Scholar] [CrossRef]
| Clinical data | Value |
|---|---|
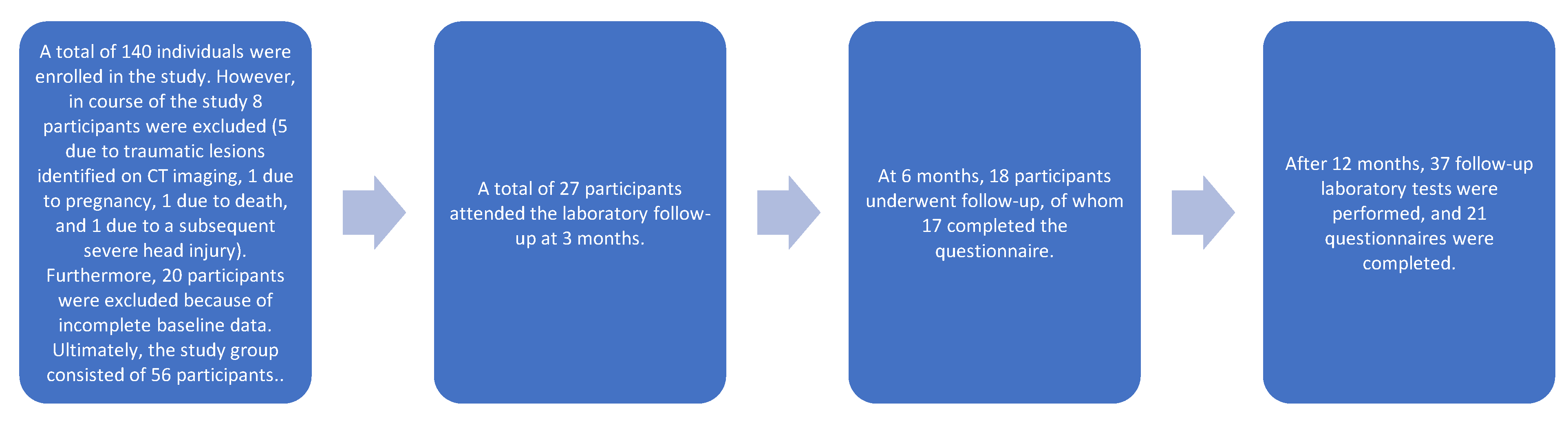
| Total number of patients (N) | 56 |
| Female sex, n (%) | 35 (62.5) |
| Male sex, n (%) | 21 (37.5) |
| Age, median (Q1–Q3), years | 45.0 (30.0–61.5) |
| Positive endocrinological history, n (%) | 15 (26.8) |
| Symptom | Frequency at 6 months (%) | Frequency at 12 months (%) |
|---|---|---|
| Increased fatigue | 25 | 52,6 |
| Pallor | 0 | 5,3 |
| Decreased appetite and weight loss | 0 | 10,5 |
| Cold intolerance | 18,8 | 26,3 |
| Tendency toward constipation | 0 | 21,1 |
| Hoarseness | 12,5 | 10,5 |
| Increased hair loss and dry skin | 6,3 | 26,3 |
| Impaired concentration | 62,5 | 42,1 |
| Decreased libido | 6,3 | 5,3 |
| Mood fluctuations and/or depressive symptoms | 37,5 | 21,1 |
| Loss of hair in the genital area | 0 | 0 |
| Men: loss of facial hair and/or chest hair | 0 | 0 |
| Premenopausal women: menstrual irregularities or hypomenorrhea | 0 | 5,3 |
| Premenopausal women: difficulty conceiving | 0 | 0 |
| Body weight fluctuations | 0 | 15,8 |
| Memory impairment | 31,3 | 36,8 |
| Reduced muscle strength | 0 | 21,1 |
| Abdominal (central) obesity | 0 | 26,3 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




