Submitted:
11 February 2026
Posted:
11 February 2026
You are already at the latest version
Abstract
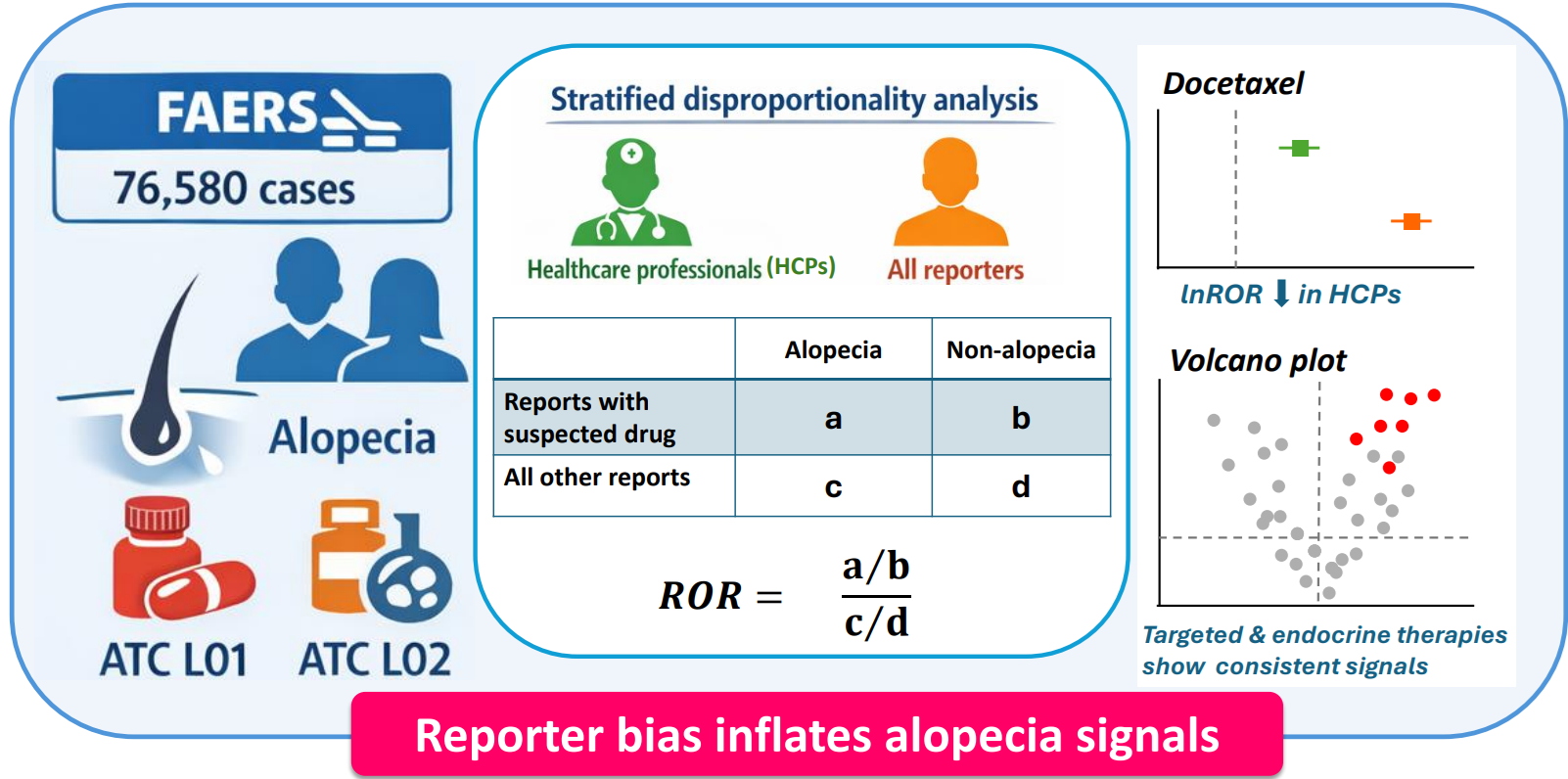
Keywords:
1. Introduction
2. Materials and Methods
2.1. Data Source and Study Period
2.2. Terminology for Target Drugs and Adverse Events
2.3. Selection Criteria for Drugs and Adverse Events
2.4. Outcomes
2.5. Data Extraction and Integration
2.6. Assessment of Reporting Frequency and Reporter Characteristics
2.7. Disproportionality Analysis
2.8. Stratified Analysis Restricted to HCPs
2.8.1. Definition of Stratification Criteria
2.8.2. Rational and Analytical Purpose
2.9. Statistical Analysis
3. Results
3.1. Baseline Characteristics of the Analytical Dataset
| a. All Reporter Types | b. Healthcare Professionals Only | ||||||
| (n = 76,580) | (n = 27,838) | ||||||
| Characteristics | No. | (%) | No. | (%) | |||
| Gender | |||||||
| Data available | 62,565 | Data available | 24,560 | ||||
| Female | 56,378 | 90.11% | Female | 21,488 | 87.49% | ||
| Male | 6,097 | 9.75% | Male | 3,015 | 12.28% | ||
| Unknown | 90 | 0.14% | Unknown | 57 | 0.23% | ||
| Age (years old) | |||||||
| Data available | 45,821 | Data available | 17,802 | ||||
| less than 30 | 1,190 | 2.60% | less than 30 | 710 | 3.99% | ||
| 30-39 | 2,474 | 5.40% | 30-39 | 818 | 4.60% | ||
| 40-49 | 10,267 | 22.41% | 40-49 | 4,457 | 25.04% | ||
| 50-59 | 12,355 | 26.96% | 50-59 | 3,954 | 22.21% | ||
| 60-69 | 11,624 | 25.37% | 60-69 | 4,190 | 23.54% | ||
| 70-79 | 6,190 | 13.51% | 70-79 | 2,861 | 16.07% | ||
| 80 or more | 1,721 | 3.76% | 80 or more | 812 | 4.56% | ||
| Median (IQR) | 57(47-66) | Median (IQR) | 58(45-67) | ||||
| Body weight (kg) | |||||||
| Data available | 22,371 | Data available | 6,434 | ||||
| less than 40 | 169 | 0.76% | less than 40 | 112 | 1.74% | ||
| 40-49 | 802 | 3.59% | 40-49 | 337 | 5.24% | ||
| 50-59 | 2,855 | 12.76% | 50-59 | 890 | 13.83% | ||
| 60-69 | 4,829 | 21.59% | 60-69 | 1,620 | 25.18% | ||
| 70-79 | 4,294 | 19.19% | 70-79 | 1,024 | 15.92% | ||
| 80-89 | 3,181 | 14.22% | 80-89 | 635 | 9.87% | ||
| 90-99 | 3,321 | 14.85% | 90-99 | 1,445 | 22.46% | ||
| 100 or more | 2,920 | 13.05% | 100 or more | 371 | 5.77% | ||
| Median(IQR) | 75(64-91) | Median(IQR) | 72(62-93) | ||||
| Reported countries (Top6) | |||||||
| Data available | 76,308 | Data available | 27,711 | ||||
| United States | 52,928 | 69.36% | United States | 10,429 | 37.64% | ||
| Canada | 11,800 | 15.46% | Canada | 9,741 | 35.15% | ||
| United Kingdom | 1,683 | 2.21% | Germany | 1,079 | 3.89% | ||
| Country Not Specified | 1,335 | 1.75% | Japan | 1,004 | 3.62% | ||
| Germany | 1,331 | 1.74% | United Kingdom | 944 | 3.41% | ||
| Japan | 1,113 | 1.46% | Italy | 800 | 2.89% | ||
| Indication (pt_term, Top15) | |||||||
| Data available | 71,767 | 28,190 | |||||
| Product used for an unknown indication | 14,038 | 19.56% | Rheumatoid Arthritis | 7,740 | 27.46% | ||
| Breast Cancer Female | 13,615 | 18.97% | Product used for an unknown indication | 5,687 | 20.17% | ||
| Rheumatoid Arthritis | 9,270 | 12.92% | Breast Cancer | 1,728 | 6.13% | ||
| Breast Cancer | 7,635 | 10.64% | Breast Cancer Metastatic | 1,251 | 4.44% | ||
| Breast Cancer Metastatic | 3,025 | 4.22% | Breast Cancer Female | 1,160 | 4.12% | ||
| Chemotherapy | 1,355 | 1.89% | Chronic Myeloid Leukaemia | 456 | 1.62% | ||
| Invasive ductal breast carcinoma | 1,020 | 1.42% | Basal Cell Carcinoma | 407 | 1.44% | ||
| Chronic Myeloid Leukaemia | 985 | 1.37% | Non-Small Cell Lung Cancer | 357 | 1.27% | ||
| Basal Cell Carcinoma | 976 | 1.36% | Ovarian Cancer | 277 | 0.98% | ||
| Lung Neoplasm Malignant | 742 | 1.03% | Psoriatic Arthropathy | 222 | 0.79% | ||
| Ovarian Cancer | 734 | 1.02% | Renal Cell Carcinoma | 197 | 0.70% | ||
| Triple-negative breast cancer | 699 | 0.97% | Colorectal Cancer Metastatic | 194 | 0.69% | ||
| Non-Small Cell Lung Cancer | 651 | 0.91% | Arthritis | 193 | 0.69% | ||
| Prostate Cancer | 587 | 0.82% | Neoplasm Malignant | 189 | 0.67% | ||
| Gastrointestinal Stromal Tumour | 529 | 0.74% | Lung Neoplasm Malignant | 184 | 0.65% | ||
3.2. Alopecia-Related PTs Included in the Analysis
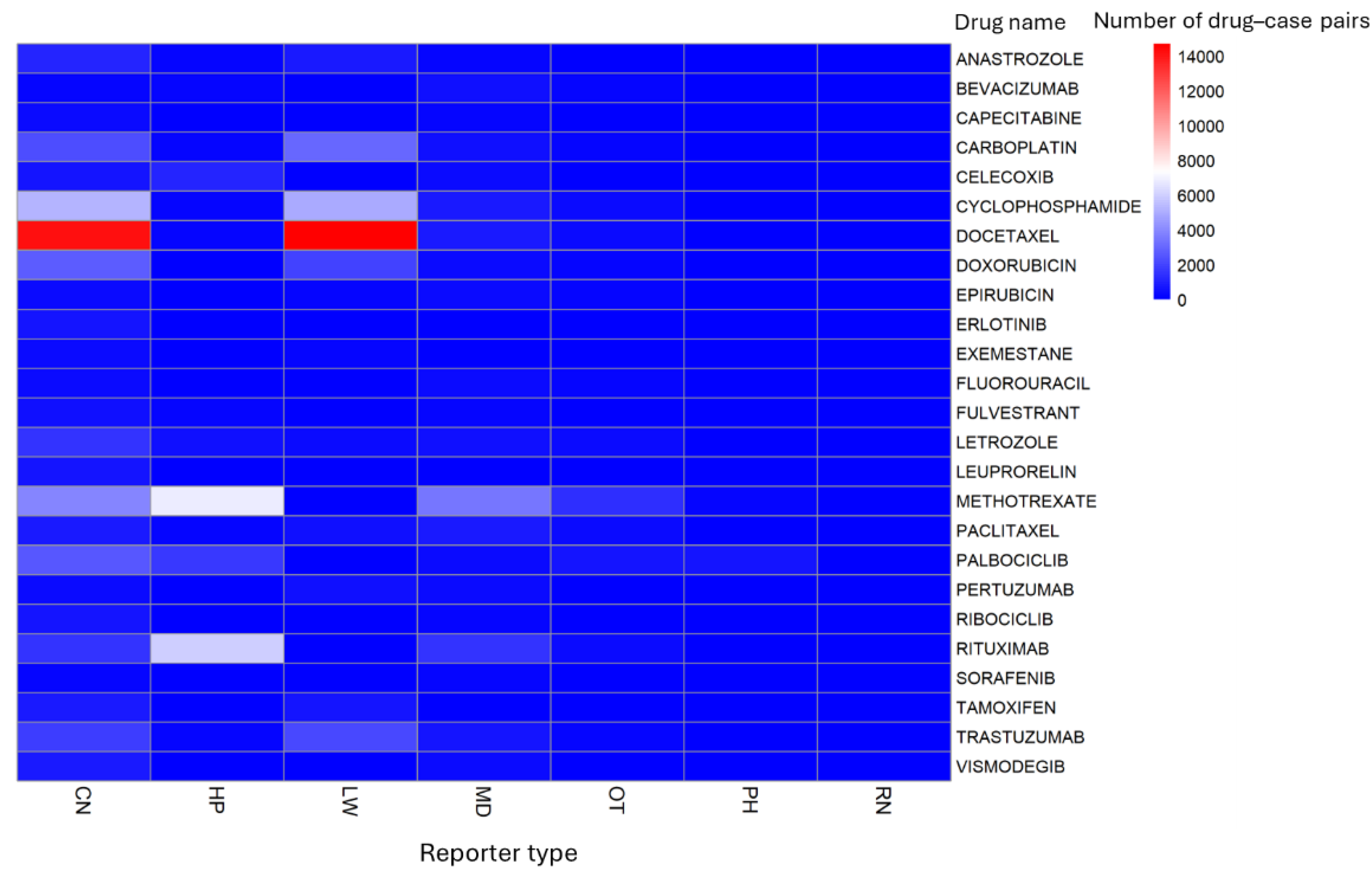
3.3. Drug-Specific Reporting Frequencies
3.4. Distribution of Reporter Characteristics
3.5. Disproportionality Analysis in the All-Reporter Dataset
3.6. Results of the Stratified Analysis Restricted to HCPs
3.6.1. Patient Characteristics in the HCP-Restricted Dataset
3.6.2. Alopecia-Related PTs Reported by HCPs
3.6.3. Drug-Specific Reporting Frequencies in HCP Reports
3.6.4. Disproportionality Analysis in the HCP-Restricted Dataset
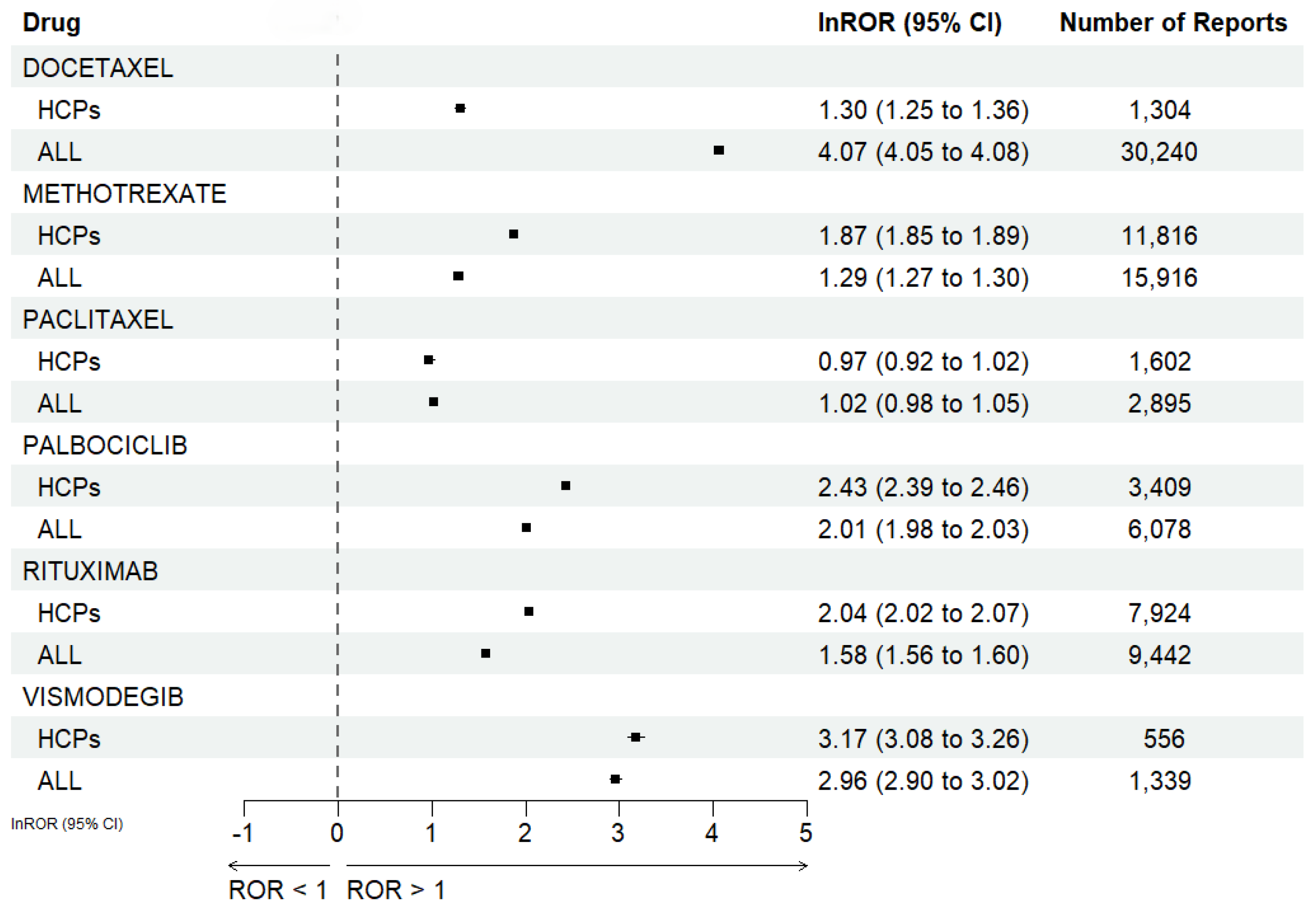
3.6.5. Differences in RORs According to Reporter Type
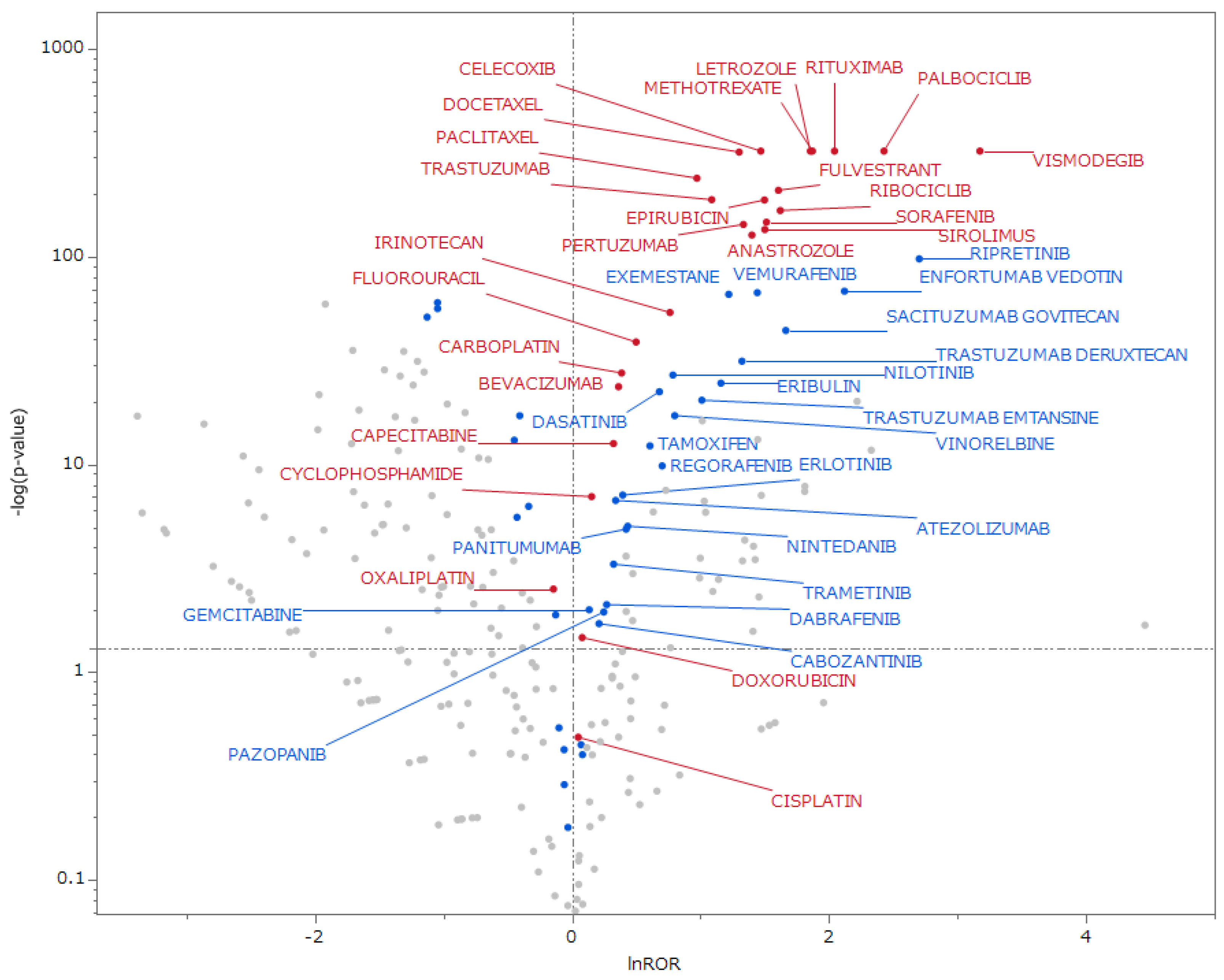
3.6.6. Volcano Plot
4. Discussion
4.1. Characteristics of Alopecia Reporting and Pharmacological Background
4.2. Reporter Type and Bias in Reporting Patterns
4.3. HCP-Stratified Analysis and Visualization Using Volcano Plots
4.4. Psychological Impact of Alopecia and QoL
4.5. Study Limitations and Future Directions
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| FAERS | FDA Adverse Event Reporting System |
| SRS | Spontaneous reporting system |
| AE | Adverse event |
| MedDRA | Medical Dictionary for Regulatory Activities |
| HLT | High Level Term |
| PT | Preferred Term |
| LLT | Lowest Level Term |
| ATC | Anatomical Therapeutic Chemical Classification System |
| HCPs | Healthcare professionals |
| ROR | Reporting odds ratio |
| lnROR | Natural logarithm of the reporting odds ratio |
| CI | Confidence interval |
| IQR | Interquartile range |
| CTIA | Cancer therapy–induced alopecia |
| CIA | Chemotherapy-induced alopecia |
| EIA | Endocrine therapy–induced alopecia |
| pCIA | Permanent chemotherapy–induced alopecia |
| QoL | quality of life |
| HRQoL | Health-related quality of life |
References
- McGarvey, E.L.; Baum, L.D.; Pinkerton, R.C.; Rogers, L.M. Psychological sequelae and alopecia among women with cancer. Cancer Pract. 2001, 9, 283–289. [Google Scholar] [CrossRef] [PubMed]
- Hunt, N.; McHale, S. The psychological impact of alopecia. BMJ 2005, 331, 951–953. [Google Scholar] [CrossRef] [PubMed]
- Lemieux, J.; Maunsell, E.; Provencher, L. Chemotherapy-induced alopecia and effects on quality of life among women with breast cancer: A literature review. Psychooncology 2008, 17, 317–328. [Google Scholar] [CrossRef]
- Paus, R.; Haslam, I.S.; Sharov, A.A.; Botchkarev, V.A. Pathobiology of chemotherapy-induced hair loss. Lancet Oncol. 2013, 14, e50–e59. [Google Scholar] [CrossRef]
- Freites-Martinez, A.; Shapiro, J.; Chan, D.; Fornier, M.; Modi, S.; Gajria, D.; Dusza, S.; Goldfarb, S.; Lacouture, M.E. Endocrine therapy-induced alopecia in patients with breast cancer. JAMA Dermatol. 2018, 154, 670–675. [Google Scholar] [CrossRef]
- Belum, V.R.; Marulanda, K.; Ensslin, C.; Gorcey, L.; Parikh, T.; Wu, S.; Busam, K.J.; Gerber, P.A.; Lacouture, M.E. Alopecia in patients treated with molecularly targeted anticancer therapies. Ann. Oncol. 2015, 26, 2496–2502. [Google Scholar] [CrossRef] [PubMed]
- Cutroneo, P.M.; Sartori, D.; Tuccori, M.; Crisafulli, S.; Battini, V.; Carnovale, C.; Rafaniello, C.; Capuano, A.; Poluzzi, E.; Moretti, U.; Raschi, E. Conducting and interpreting disproportionality analyses derived from spontaneous reporting systems. Front. Drug Saf. Regul. 2024, 3, 1323057. [Google Scholar] [CrossRef]
- Petracek, J.; Fialova, M. Spontaneous reporting systems. In Principles and Practice of Pharmacovigilance and Drug Safety;Chapter 10; Springer: Cham, Switzerland, 2023. [Google Scholar] [CrossRef]
- Palleria, C.; Leporini, C.; Chimirri, S.; Marrazzo, G.; Sacchetta, S.; Bruno, L.; Lista, R.M.; Staltari, O.; Scuteri, A.; Scicchitano, F.; Russo, E. Limitations and obstacles of the spontaneous adverse drug reactions reporting: Two “challenging” case reports. J. Pharmacol. Pharmacother. 2013, 4, S66–S72. [Google Scholar] [CrossRef]
- Dueck, A.C.; Mendoza, T.R.; Mitchell, S.A.; Reeve, B.B.; Castro, K.M.; Rogak, L.J.; Atkinson, T.M.; Bennett, A.V.; Denicoff, A.M.; O’Mara, A.M.; Li, Y.; Clauser, S.B.; Bryant, D.M.; Bearden, J.D., III; Gillis, T.A.; Harness, J.K.; Siegel, R.D.; Paul, D.B.; Cleeland, C.S.; Schrag, D.; Sloan, J.A.; Abernethy, A.P.; Bruner, D.W.; Minasian, L.M.; Basch, E. National Cancer Institute PRO-CTCAE Study Group. Validity and reliability of the U.S. National Cancer Institute’s patient-reported outcomes version of the Common Terminology Criteria for Adverse Events (PRO-CTCAE). JAMA Oncol. 2015, 1, 1051–1059. [Google Scholar] [CrossRef]
- Minasian, L.M.; O’Mara, A.; Mitchell, S.A. Clinician and patient reporting of symptomatic adverse events in cancer clinical trials: Using CTCAE and PRO-CTCAE® to provide two distinct and complementary perspectives. Patient Relat. Outcome Meas. 2022, 13, 249–258. [Google Scholar] [CrossRef]
- Veitch, Z.W.; Shepshelovich, D.; Gallagher, C.; Wang, L.; Abdul Razak, A.R.; Spreafico, A.; Bedard, P.L.; Siu, L.L.; Minasian, L.; Hansen, A.R. Underreporting of symptomatic adverse events in phase I clinical trials. J. Natl. Cancer Inst. 2021, 113, 980–988. [Google Scholar] [CrossRef]
- U.S. Food and Drug Administration. FDA Adverse Event Reporting System (FAERS). Available online: https://www.fda.gov/drugs/drug-approvals-and-databases/fda-adverse-event-reporting-system-faers-database (accessed on 5 December 2025).
- WHO Collaborating Centre for Drug Statistics Methodology. ATC/DDD Index 2024; World Health Organization: Oslo, Norway, 2024; Available online: https://www.whocc.no.
- Lawson, R. Small sample confidence intervals for the odds ratio. Commun. Stat. Simul. Comput. 2004, 33, 1095–1113. [Google Scholar] [CrossRef]
- Jones, S.E.; Erban, J.; Overmoyer, B.; Budd, G.T.; Hutchins, L.; Lower, E.; Laufman, L.; Sundaram, S.; Urba, W.J.; Pritchard, K.I.; Mennel, R.; Richards, D.; Olsen, S.; Meyers, M.L.; Ravdin, P.M. Randomized phase III study of docetaxel compared with paclitaxel in metastatic breast cancer. J. Clin. Oncol. 2005, 23, 5542–5551. [Google Scholar] [CrossRef]
- Slaught, C.; Roman, M.; Yashar, S.; Holland, V.; Goh, C. Permanent alopecia in breast cancer patients: Role of taxanes and endocrine therapies. Cutis 2021, 107, E17–E22. [Google Scholar] [CrossRef] [PubMed]
- Freites-Martinez, A.; Chan, D.; Sibaud, V.; et al. Assessment of quality of life and treatment outcomes of patients with persistent postchemotherapy alopecia. JAMA Dermatol. 2019, 155, 724–728. [Google Scholar] [CrossRef]
- Dubin, C.; Lamb, A. Hair regrowth in endocrine therapy alopecia with dutasteride treatment in a woman with estrogen-positive breast cancer. JAAD Case Rep. 2023, 35, 5–7. [Google Scholar] [CrossRef]
- Moscetti, L.; Fabbri, M.A.; Sperduti, I.; et al. Adjuvant aromatase inhibitor therapy in early breast cancer: What factors lead patients to discontinue treatment? Tumori 2015, 101, 469–473. [Google Scholar] [CrossRef] [PubMed]
- Gallicchio, L.; Calhoun, C.; Helzlsouer, K.J. Aromatase inhibitor therapy and hair loss among breast cancer survivors. Breast Cancer Res. Treat. 2013, 142, 435–443. [Google Scholar] [CrossRef]
- Saggar, V.; Wu, S.; Dickler, M.N.; Lacouture, M.E. Alopecia with endocrine therapies in patients with cancer. Oncologist 2013, 18, 1126–1134. [Google Scholar] [CrossRef]
- Wysocki, P.J. Combination of chemotherapy and endocrine treatment in breast cancer—Is it still a taboo? Oncol. Clin. Pract. 2024, 20, 302–307. [Google Scholar] [CrossRef]
- Blanpain, C. CDK4/6 inhibition mitigates stem cell damage in a novel model for taxane-induced alopecia. EMBO Mol. Med. 2019, 11, e201911031. [Google Scholar] [CrossRef]
- Zhao, Q.; Nian, Z.; He, Y.; Lai, L.; Liu, W.; Huang, S.; Yang, L. Toxicity spectrum of taxanes: A safety analysis from pre-marketing to post-marketing. Expert Opin. Drug Saf. 2025. [Google Scholar] [CrossRef]
- Martin, M.; de la Torre-Montero, J.C.; Lopez-Tarruella, S.; Pinilla, K.; Casado, A.; Fernandez, S.; Jerez, Y.; Puente, J.; Palomero, I.; Gonzalez Del Val, R.; et al. Persistent major alopecia following adjuvant docetaxel for breast cancer: Incidence, characteristics, and prevention with scalp cooling. Breast Cancer Res. Treat. 2018, 171, 627–634. [Google Scholar] [CrossRef] [PubMed]
- Chan, J.; Adderley, H.; Alameddine, M.; Armstrong, A.; Arundell, D.; Fox, R.; Harries, M.; Lim, J.; Salih, Z.; Tetlow, C.; Wong, H.; Thorp, N. Permanent hair loss associated with taxane chemotherapy use in breast cancer: A retrospective survey at two tertiary UK cancer centres. Eur. J. Cancer Care (Engl.) 2021, 30, e13395. [Google Scholar] [CrossRef] [PubMed]
- Perez, A.M.; Haberland, N.I.; Miteva, M.; Wikramanayake, T.C. Chemotherapy-induced alopecia by docetaxel: Prevalence, treatment and prevention. Curr. Oncol. 2024, 31, 5709–5721. [Google Scholar] [CrossRef]
- Núñez-Torres, R.; Martín, M.; García-Sáenz, J.Á.; Rodrigo-Faus, M.; Del Monte-Millán, M.; Tejera-Pérez, H.; Pita, G.; de la Torre-Montero, J.C.; Pinilla, K.; Herraez, B.; Peiró-Chova, L.; Bermejo, B.; Lluch, A.; González-Neira, A. Association between ABCB1 genetic variants and persistent chemotherapy-induced alopecia in women with breast cancer. JAMA Dermatol. 2020, 156, 987–991. [Google Scholar] [CrossRef] [PubMed]
- Blümel, J.E.; Lavín, P.; Vallejo, M.S.; Sarrá, S. Menopause or climacteric, just a semantic discussion or has it clinical implications? Climacteric 2014, 17, 235–241. [Google Scholar] [CrossRef]
- Nguyen, M.; Kraft, S. Approaches to management of endocrine therapy-induced alopecia in breast cancer patients. Support. Care Cancer 2025, 33, 199. [Google Scholar] [CrossRef]
- Lacouture, M.E.; Dréno, B.; Ascierto, P.A.; Dummer, R.; Basset-Seguin, N.; Fife, K.; et al. Characterization and management of Hedgehog pathway inhibitor-related adverse events in patients with advanced basal cell carcinoma. Oncologist 2016, 21, 1218–1229. [Google Scholar] [CrossRef]
- Wang, L.C.; Liu, Z.Y.; Gambardella, L.; Delacour, A.; Shapiro, R.; Yang, J.; Sizing, I.; Rayhorn, P.; Garber, E.A.; Benjamin, C.D.; Williams, K.P.; Taylor, F.R.; Barrandon, Y.; Ling, L.; Burkly, L.C. Conditional disruption of hedgehog signaling pathway defines its critical role in hair development and regeneration. J. Invest. Dermatol. 2000, 114, 901–908. [Google Scholar] [CrossRef]
- Migden, M.R.; Guminski, A.; Gutzmer, R.; Dirix, L.; Lewis, K.D.; Combemale, P.; Herd, R.M.; Kudchadkar, R.; Trefzer, U.; Gogov, S.; Pallaud, C.; Yi, T.; Mone, M.; Kaatz, M.; Loquai, C.; Stratigos, A.J.; Schulze, H.J.; Plummer, R.; Chang, A.L.; Cornélis, F.; Lear, J.T.; Sellami, D.; Dummer, R. Treatment with two different doses of sonidegib in patients with locally advanced or metastatic basal cell carcinoma (BOLT): A multicentre, randomised, double-blind phase 2 trial. Lancet Oncol. 2015, 16, 716–728. [Google Scholar] [CrossRef]
- Ferguson, J.S.; Hannam, S.; Toholka, R.; Chong, A.H.; Magee, J.; Foley, P. Hair loss and Hedgehog inhibitors: A class effect? Br. J. Dermatol. 2015, 173, 262–264. [Google Scholar] [CrossRef]
- Sibaud, V.; Sollena, P. Dermatologic toxicities to inhibitors of cyclin-dependent kinases CDK 4 and 6: An updated review for clinical practice. Ann. Dermatol. Venereol. 2023, 150, 208–212. [Google Scholar] [CrossRef]
- Tripathy, D.; Im, S.A.; Colleoni, M.; Franke, F.; Bardia, A.; Harbeck, N.; et al. Ribociclib plus endocrine therapy for premenopausal women with hormone-receptor-positive, advanced breast cancer (MONALEESA-7): A randomised phase 3 trial. Lancet Oncol. 2018, 19, 904–915. [Google Scholar] [CrossRef] [PubMed]
- Im, S.A.; Mukai, H.; Park, I.H.; Masuda, N.; Shimizu, C.; Kim, S.B.; et al. Palbociclib plus letrozole as first-line therapy in postmenopausal Asian women with metastatic breast cancer: Results from the phase III, randomized PALOMA-2 study. J. Glob. Oncol. 2019, 5, JGO.18.00173. [Google Scholar] [CrossRef] [PubMed]
- Purba, T.S.; Ng’andu, K.; Brunken, L.; Smart, E.; Mitchell, E.; Hassan, N.; et al. CDK4/6 inhibition mitigates stem cell damage in a novel model for taxane-induced alopecia. EMBO Mol. Med. 2020, 12, e11031. [Google Scholar] [CrossRef]
- Smolen, J.S.; Landewé, R.B.M.; Bergstra, S.A.; Kerschbaumer, A.; Sepriano, A.; Aletaha, D. EULAR recommendations for the management of rheumatoid arthritis with synthetic and biological disease-modifying antirheumatic drugs: 2022 update https://doi.org/10.1136/ard-2022-223356 (doi.org in Bing) Free Law Project; CourtListener. Taxotere (Docetaxel) Products Liability Litigation, MDL No. 2740—Docket. Ann. Rheum. Dis. 2023, 82, 3–18. Available online: https://www.courtlistener.com/docket/17279738/in-re-taxotere-docetaxel-products-liability-litigation/ (accessed on 7 December 2025).
- Fraenkel, L.; Bathon, J.M.; England, B.R.; StClair, E.W.; Arayssi, T.; Carandang, K.; et al. 2021 American College of Rheumatology guideline for the treatment of rheumatoid arthritis. Arthritis Care Res. (Hoboken) 2021, 73, 924–939. [Google Scholar] [CrossRef] [PubMed]
- Klareskog, L.; van der Heijde, D.; de Jager, J.P.; Gough, A.; Kalden, J.; Malaise, M.; et al. Therapeutic effect of the combination of etanercept and methotrexate compared with each drug alone in patients with rheumatoid arthritis: Double-blind randomized controlled trial. N. Engl. J. Med. 2000, 343, 1586–1593. [Google Scholar] [CrossRef]
- Lalani, R.; Lyu, H.; Vanni, K.; Solomon, D.H. Low-dose methotrexate and mucocutaneous adverse events: Results of a systematic literature review and meta-analysis of randomized controlled trials. Arthritis Care Res. (Hoboken) 2020, 72, 1140–1146. [Google Scholar] [CrossRef]
- van Ede, A.E.; Laan, R.F.; Rood, M.J.; Huizinga, T.W.; van de Laar, M.A.; van Denderen, C.J.; Westgeest, T.A.; Romme, T.C.; de Rooij, D.J.; Jacobs, M.J.; de Boo, T.M.; van der Wilt, G.J.; Severens, J.L.; Hartman, M.; Krabbe, P.F.; Dijkmans, B.A.; Breedveld, F.C.; van de Putte, L.B. Effect of folic or folinic acid supplementation on the toxicity and efficacy of methotrexate in rheumatoid arthritis: A forty-eight week, multicenter, randomized, double-blind, placebo-controlled study. Arthritis Rheum. 2001, 44, 1515–1524. [Google Scholar] [CrossRef]
- Judicial Panel on Multidistrict Litigation (JPML). IN RE: Taxotere (Docetaxel) Products Liability Litigation. MDL No. 2740. Transfer Order; JPML: Washington, DC, USA, 2016; Available online: https://www.jpml.uscourts.gov/sites/jpml/files/MDL-2740-Initial_Transfer-09-16.pdf (accessed on 7 December 2025).
- Judicial Panel on Multidistrict Litigation. MDL Statistics Report—Distribution of Pending MDL Dockets by Actions Pending—July 1, 2025 . Judicial Panel on Multidistrict Litigation: Washington, DC, USA, 2025. Available online: https://www.jpml.uscourts.gov/sites/jpml/files/Pending_MDL_Dockets_By_Actions_Pending-July-1-2025_0.pdf (accessed on 7 December 2025).
- Judicial Panel on Multidistrict Litigation. MDL Statistics Report—Distribution of Pending MDL Dockets by District—October 1, 2025 . Judicial Panel on Multidistrict Litigation: Washington, DC, USA, 2025. Available online: https://www.jpml.uscourts.gov/sites/jpml/files/Pending_MDL_Dockets_By_District-October-1-2025.pdf (accessed on 7 December 2025).
- United States District Court; Eastern District of Louisiana. MDL-2740: IN RE: Taxotere (Docetaxel) Products Liability Litigation—MDL Docket Page . Available online: https://www.laed.uscourts.gov/case-information/mdl-mass-class-action/taxotere (accessed on 7 December 2025).
- United States District Court; Eastern District of Louisiana. Order and Reasons, IN RE: Taxotere (Docetaxel) MDL No. 16-2740 . Rec. Doc. 16778. 21 May 2024. Available online: https://www.govinfo.gov/content/pkg/USCOURTS-laed-2_16-md-02740/pdf/USCOURTS-laed-2_16-md-02740-86.pdf (accessed on 7 December 2025).
- Project, Free Law; CourtListener. Taxotere (Docetaxel) Products Liability Litigation, MDL No. 2740—Docket . Available online: https://www.courtlistener.com/docket/17279738/in-re-taxotere-docetaxel-products-liability-litigation/ (accessed on 7 December 2025).
- European Medicines Agency (EMA). Spontaneous Adverse Drug Reactions—Subgroup Report . EMA/HMA: London, UK, 2018; Available online: https://www.ema.europa.eu/en/documents/report/spontaneous-adverse-drug-reactions-subgroup-report_en.pdf (accessed on 7 December 2025).
- Rolfes, L.; van Hunsel, F.; van der Linden, L.; Taxis, K.; van Puijenbroek, E. The quality of clinical information in adverse drug reaction reports by patients and healthcare professionals: A retrospective comparative analysis. Drug Saf. 2017, 40, 607–614. [Google Scholar] [CrossRef]
- Inch, J.; Watson, M.C.; Anakwe-Umeh, S. Patient versus healthcare professional spontaneous adverse drug reaction reporting: A systematic review. Drug Saf. 2012, 35, 807–818. [Google Scholar] [CrossRef]
- Uesawa, Y. Adverse effect predictions based on computational toxicology techniques and large-scale databases. Yakugaku Zasshi 2018, 138, 185–190. (In Japanese) [Google Scholar] [CrossRef] [PubMed]
- Tan, A.R.; Im, S.A.; Mattar, A.; Colomer, R.; Stroyakovskii, D.; Nowecki, Z.; De Laurentiis, M.; Pierga, J.Y.; Jung, K.H.; Schem, C.; Hogea, A.; Badovinac Crnjevic, T.; Heeson, S.; Shivhare, M.; Kirschbrown, W.P.; Restuccia, E.; Jackisch, C.; FeDeriCa Study Group. Fixed-dose combination of pertuzumab and trastuzumab for subcutaneous injection plus chemotherapy in HER2-positive early breast cancer (FeDeriCa): A randomised, open-label, multicentre, non-inferiority, phase 3 study. Lancet Oncol. 2021, 22, 85–97. [Google Scholar] [CrossRef] [PubMed]
- Ventura, I.; Salcedo, N.P.; Pérez-Bermejo, M.; Pérez-Murillo, J.; Tejeda-Adell, M.; Tomás-Aguirre, F.; Legidos-García, M.E.; Murillo-Llorente, M.T. Pertuzumab in combination with trastuzumab and docetaxel as adjuvant doublet therapy for HER2-positive breast cancer: A systematic review. Int. J. Mol. Sci. 2025, 26, 1908. [Google Scholar] [CrossRef]
- Yajima, A.; Uesawa, Y. A comprehensive analysis of adverse events associated with HER2 inhibitors approved for breast cancer using the FDA Adverse Event Reporting System (FAERS). Pharmaceuticals 2025, 18, 1510. [Google Scholar] [CrossRef] [PubMed]
- Genentech, Inc. Rituxan (rituximab) Injection, for Intravenous Use; U.S. Prescribing Information; Food and Drug Administration: Silver Spring, MD, USA, 2021; Available online: https://www.accessdata.fda.gov/drugsatfda_docs/label/2021/103705s5464lbl.pdf (accessed on 7 December 2025).
- Puiu, T.; Reimer, D.; Sokumbi, O. Rituximab-induced alopecia universalis in a patient with bullous pemphigoid. J. Drugs Dermatol. 2022, 21, 894–895. [Google Scholar] [CrossRef]
- Oke, A.R.; Young-Min, S. Successful treatment of alopecia universalis with rituximab therapy. Rheumatology (Oxford) 2020, 59, keaa109.005. [Google Scholar] [CrossRef]
- Saris, L.M.H.; Vlooswijk, C.; Kaal, S.E.J.; Nuver, J.; Bijlsma, R.M.; van der Hulle, T.; Kouwenhoven, M.C.M.; Tromp, J.M.; Lalisang, R.I.; Bos, M.E.M.M.; van der Graaf, W.T.A.; Husson, O. A negative body image among adolescent and young adult (AYA) cancer survivors: Results from the population-based SURVAYA study. Cancers 2022, 14, 5243. [Google Scholar] [CrossRef]
- Tallon, B.; Blanchard, E.; Goldberg, L.J. Permanent chemotherapy-induced alopecia: Case report and review of the literature. J. Am. Acad. Dermatol. 2010, 63, 333–336. [Google Scholar] [CrossRef]
- Lefevre, T.; Kruszynski, J.; Hamill, M.; et al. Permanent hair loss associated with taxane chemotherapy use in breast cancer: A retrospective survey at two tertiary UK cancer centres. Breast 2020, 54, 74–81. [Google Scholar] [CrossRef]
- Kluger, N.; Jacot, W.; Frouin, E.; Rigau, V.; Poujol, S.; Dereure, O.; Guillot, B.; Romieu, G.; Bessis, D. Permanent scalp alopecia related to breast cancer chemotherapy by sequential fluorouracil/epirubicin/cyclophosphamide (FEC) and docetaxel: A prospective study of 20 patients. Ann. Oncol. 2012, 23, 2879–2884. [Google Scholar] [CrossRef] [PubMed]
- Kang, D.; Kim, I.R.; Choi, E.K.; Im, Y.H.; Park, Y.H.; Ahn, J.S.; Lee, J.E.; Nam, S.J.; Lee, H.K.; Park, J.H.; et al. Permanent chemotherapy-induced alopecia in patients with breast cancer: A 3-year prospective cohort study. Oncologist 2019, 24, 414–420. [Google Scholar] [CrossRef]
- Nozawa, K.; Toma, S.; Shimizu, C. Distress and impacts on daily life from appearance changes due to cancer treatment: A survey of 1,034 patients in Japan. Glob. Health Med. 2023, 5, 54–61. [Google Scholar] [CrossRef] [PubMed]
- Browall, M.; Gaston-Johansson, F.; Danielson, E. Postmenopausal women with breast cancer: Their experiences of the chemotherapy treatment period. Cancer Nurs. 2006, 29, 34–42. [Google Scholar] [CrossRef]
- European Organisation for Research and Treatment of Cancer (EORTC). EORTC QLQ-BR42 Module (English, Final Version); EORTC: Brussels, Belgium, 2024; Available online: https://www.eortc.org/app/uploads/sites/2/2024/04/BR42-Module-English-FINAL.doc (accessed on 7 December 2025).
- Bjelic-Radisic, V.; Cardoso, F.; Cameron, D.; Brain, E.; Kuljanic, K.; da Costa, R.A.; Conroy, T.; Inwald, E.C.; Serpentini, S.; Pinto, M.; Weis, J.; Morag, O.; Lindviksmoen Astrup, G.; Tomaszweksi, K.A.; Pogoda, K.; Sinai, P.; Sprangers, M.; Aaronson, N.; Velikova, G.; Greimel, E.; Arraras, J.; Bottomley, A. EORTC Quality of Life Group and Breast Cancer Group. An international update of the EORTC questionnaire for assessing quality of life in breast cancer patients: EORTC QLQ-BR45. Ann. Oncol. 2020, 31, 283–288. [Google Scholar] [CrossRef]
- Williams, J.; Wood, C.; Cunningham-Warburton, P. A narrative study of chemotherapy-induced alopecia. Oncol. Nurs. Forum 1999, 26, 1463–1468. [Google Scholar]
- Boehmke, M.M.; Dickerson, S.S. Symptom, symptom experiences, and symptom distress encountered by women with breast cancer undergoing current treatment modalities. Cancer Nurs. 2005, 28, 382–389. [Google Scholar] [CrossRef]
- Shen, X.F.; et al. Efficacy of scalp cooling for prevention of chemotherapy-induced alopecia: A systematic review and meta-analysis. Eur. Rev. Med. Pharmacol. Sci. 2021, 25, 5090–5103. [Google Scholar] [PubMed]
- Trujillo-Martín, M.M.; de Armas-Castellano, A.; González-Hernández, Y.; González-Pacheco, H.; Infante-Ventura, D.; Del Pino-Sedeño, T.; Ramallo-Fariña, Y.; Abt-Sack, A.; Rueda Domínguez, A.; Serrano-Aguilar, P. Scalp cooling for the prevention of chemotherapy-induced alopecia: Systematic review and meta-analysis. Rev. Esp. Salud Publica 2023, 97, e202303024. (In Spanish) [Google Scholar]
- Duvic, M.; Lemak, N.A.; Valero, V.; Hymes, S.R.; Farmer, K.L.; Hortobagyi, G.N.; Trancik, R.J.; Bandstra, B.A.; Compton, L.D. A randomized trial of minoxidil in chemotherapy-induced alopecia. J. Am. Acad. Dermatol. 1996, 35, 74–78. [Google Scholar] [CrossRef]
- Godse, K.; De, A.; Vedamurthy, M.; Shankar, D.S.K.; Shah, B.; Girdhar, M.; Bhat, R.; Ganjoo, A.; Tahiliani, S.; Patil, A. Low-dose oral minoxidil in the treatment of alopecia: Evidence- and experience-based consensus statement of Indian experts. Int. J. Trichology 2023, 15, 91–97. [Google Scholar] [CrossRef] [PubMed]
- Kuo, A.M.; Reingold, R.E.; Ketosugbo, K.F.; Pan, A.; Kraehenbuehl, L.; Dusza, S.; Gajria, D.; Lake, D.E.; Bromberg, J.F.; Traina, T.A.; Fornier, M.N.; Gucalp, A.; D’Alessandro, B.M.; Rotemberg, V.; Dauscher, M.; Shapiro, J.; Goldfarb, S.B.; Markova, A.; Lacouture, M.E. Oral minoxidil for late alopecia in cancer survivors. Breast Cancer Res. Treat. 2024, 208, 491–499. [Google Scholar] [CrossRef] [PubMed]
- Taggart, L.R.; Ozolins, L.; Hardie, H.; Nyhof-Young, J. Look good feel better workshops: A “big lift” for women with cancer. J. Cancer Educ. 2009, 24, 94–99. [Google Scholar] [CrossRef] [PubMed]
- Ikeda, M.; Tamai, N.; Kanai, H.; Osaka, M.; Kondo, K.; Yamazaki, T.; Sanada, H.; Kamibeppu, K. Effects of the appearance care program for breast cancer patients receiving chemotherapy: A mixed method study. Cancer Rep. (Hoboken) 2020, 3, e1242. [Google Scholar] [CrossRef]
- Vagnini, D.; Grassi, M.M.; Valenti, F.; Bombardieri, E.; Saita, E. Beauty therapy to support psychosocial recovery from oncological care: A qualitative research on the lived experience of women with breast cancer treated with chemotherapy. Curr. Oncol. 2024, 31, 2527–2541. [Google Scholar] [CrossRef]
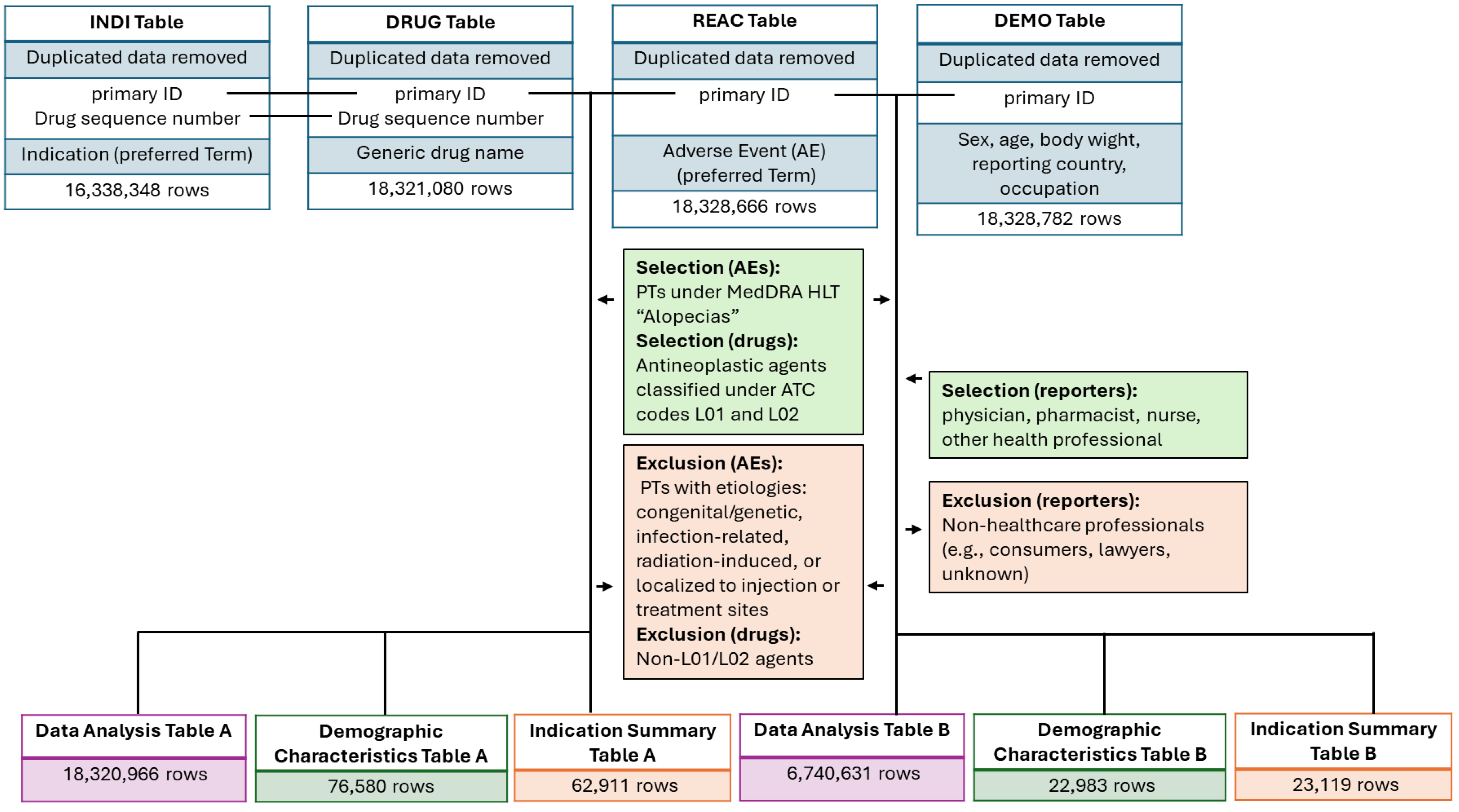
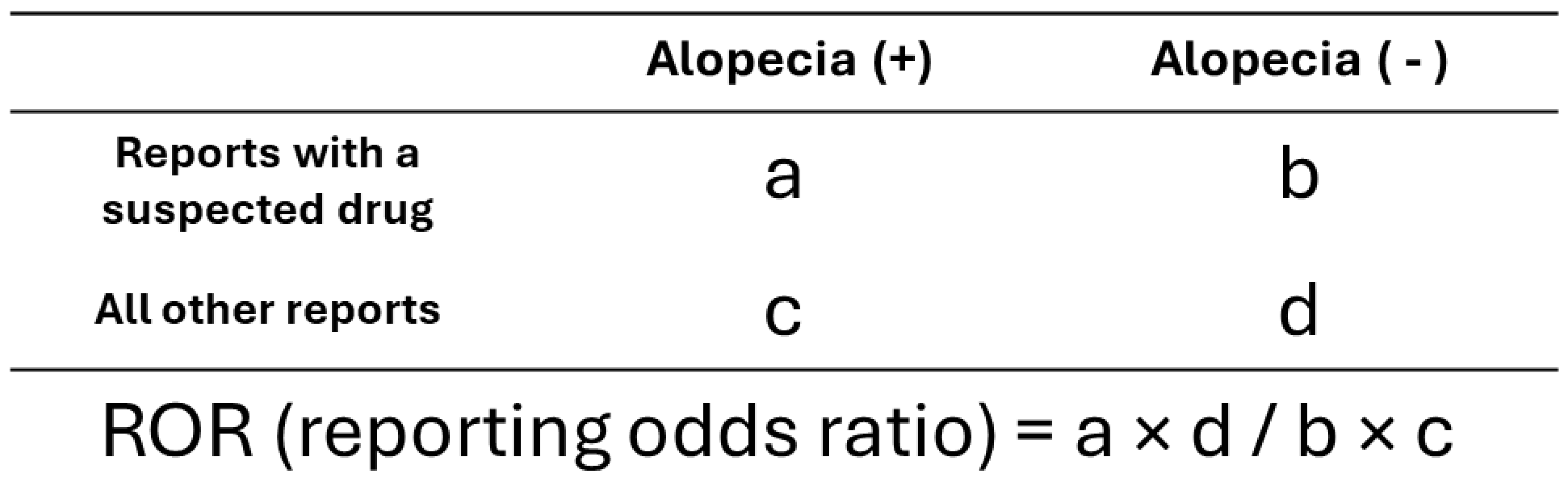
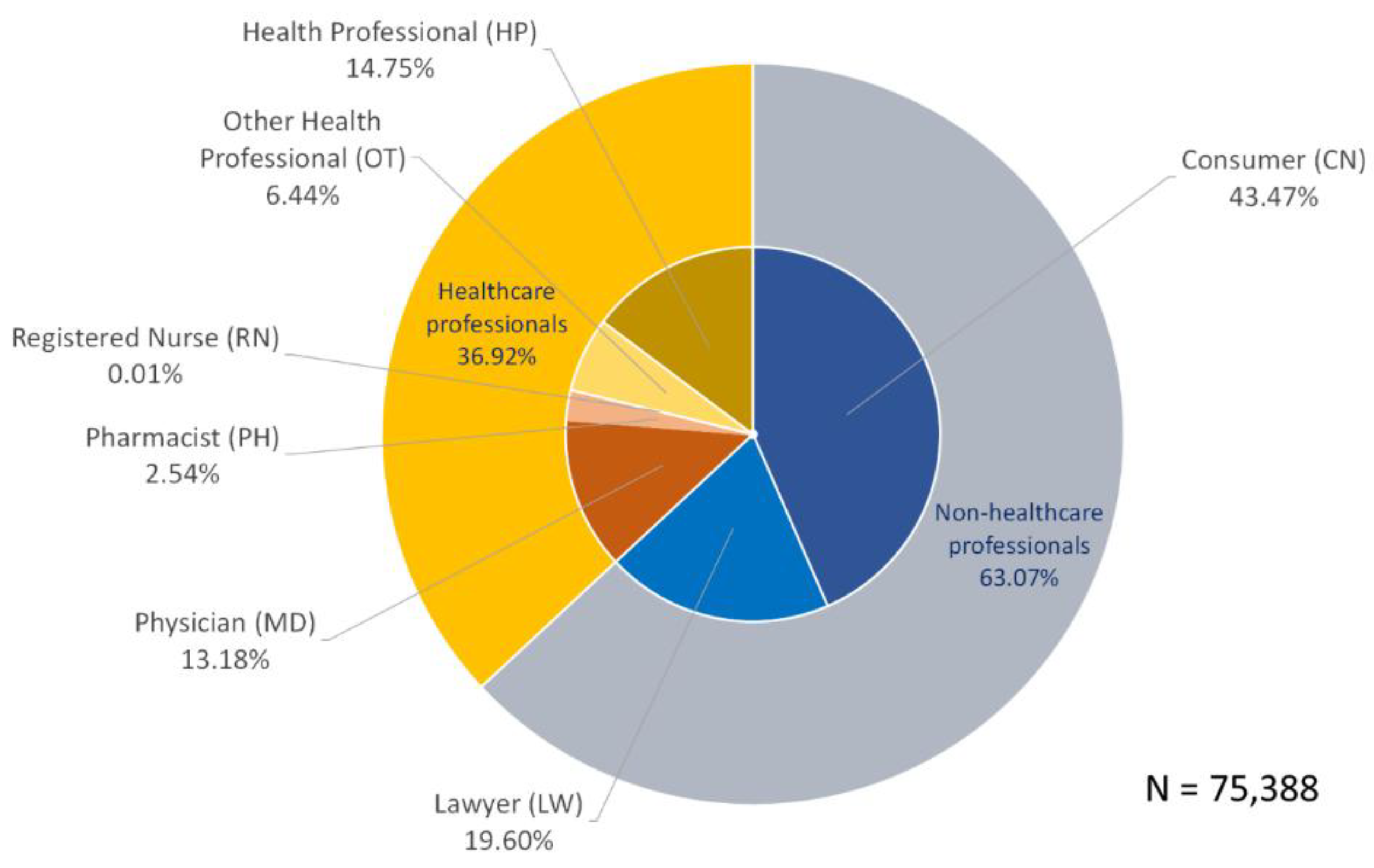
| a. All Reporter Types | b. Healthcare Professionals Only | |||
|---|---|---|---|---|
| Adverse Event | Number of Reports | Adverse Event | Number of Reports | |
| ALOPECIA | 135,323 | ALOPECIA | 49,986 | |
| MADAROSIS | 17,871 | MADAROSIS | 754 | |
| ALOPECIA AREATA | 1,203 | ALOPECIA AREATA | 469 | |
| ALOPECIA TOTALIS | 294 | DIFFUSE ALOPECIA | 176 | |
| DIFFUSE ALOPECIA | 278 | ALOPECIA TOTALIS | 130 | |
| HYPOTRICHOSIS | 168 | ALOPECIA SCARRING | 74 | |
| ALOPECIA SCARRING | 105 | ANDROGENETIC ALOPECIA | 52 | |
| ANDROGENETIC ALOPECIA | 79 | HYPOTRICHOSIS | 40 | |
| ALOPECIA UNIVERSALIS | 61 | ALOPECIA UNIVERSALIS | 32 | |
| LICHEN PLANOPILARIS | 18 | LICHEN PLANOPILARIS | 14 | |
| FOLLICULAR MUCINOSIS | 15 | FOLLICULAR MUCINOSIS | 13 | |
| NON-SCARRING ALOPECIA | 4 | NON-SCARRING ALOPECIA | 4 | |
| a. All Reporter Types | b. Healthcare Professionals Only | ||||
| (n = 155,419) | (n = 51,744) | ||||
| Rank | Drug Name | Number of Reports | Drug Name | Number of Reports | |
| 1 | DOCETAXEL | 37,305 | METHOTREXATE | 11,863 | |
| 2 | METHOTREXATE | 16,038 | RITUXIMAB | 7,929 | |
| 3 | CYCLOPHOSPHAMIDE | 14,557 | PALBOCICLIB | 3,470 | |
| 4 | RITUXIMAB | 9,454 | CELECOXIB | 1,728 | |
| 5 | CARBOPLATIN | 8,258 | PACLITAXEL | 1,623 | |
| 6 | DOXORUBICIN | 6,698 | LETROZOLE | 1,507 | |
| 7 | TRASTUZUMAB | 6,539 | DOCETAXEL | 1,408 | |
| 8 | PALBOCICLIB | 6,182 | CYCLOPHOSPHAMIDE | 1,374 | |
| 9 | LETROZOLE | 3,850 | TRASTUZUMAB | 1,091 | |
| 10 | PACLITAXEL | 3,233 | CARBOPLATIN | 979 | |
| 11 | ANASTROZOLE | 3,050 | BEVACIZUMAB | 909 | |
| 12 | CELECOXIB | 2,681 | FLUOROURACIL | 838 | |
| 13 | TAMOXIFEN | 2,104 | DOXORUBICIN | 779 | |
| 14 | PERTUZUMAB | 1,960 | EPIRUBICIN | 614 | |
| 15 | FLUOROURACIL | 1,487 | FULVESTRANT | 614 | |
| 16 | VISMODEGIB | 1,382 | CAPECITABINE | 588 | |
| 17 | FULVESTRANT | 1,290 | PERTUZUMAB | 585 | |
| 18 | EPIRUBICIN | 1,272 | VISMODEGIB | 571 | |
| 19 | BEVACIZUMAB | 1,210 | IRINOTECAN | 539 | |
| 20 | RIBOCICLIB | 1,192 | RIBOCICLIB | 481 | |
| 21 | CAPECITABINE | 994 | ANASTROZOLE | 469 | |
| 22 | EXEMESTANE | 961 | SORAFENIB | 469 | |
| 23 | LEUPRORELIN | 926 | CISPLATIN | 440 | |
| 24 | ERLOTINIB | 923 | SIROLIMUS | 434 | |
| 25 | SORAFENIB | 826 | OXALIPLATIN | 410 | |
| a. All Reporter Types | |||||
|---|---|---|---|---|---|
| drug | ROR | 95%CI [lower, upper] | lnROR | 95%CI [lower, upper] | p-value |
| DOCETAXEL | 58.31 | [57.46, 59.17] | 4.07 | [4.05, 4.08] | p < 0.001 |
| VISMODEGIB | 19.35 | [18.24, 20.52] | 2.96 | [2.90, 3.02] | p < 0.001 |
| TRASTUZUMAB | 8.23 | [8.00, 8.47] | 2.11 | [2.08, 2.14] | p < 0.001 |
| ANASTROZOLE | 8.02 | [7.70, 8.35] | 2.08 | [2.04, 2.12] | p < 0.001 |
| TAMOXIFEN | 7.60 | [7.23, 7.99] | 2.03 | [1.98, 2.08] | p < 0.001 |
| PALBOCICLIB | 7.44 | [7.25, 7.64] | 2.01 | [1.98, 2.03] | p < 0.001 |
| LETROZOLE | 6.60 | [6.38, 6.84] | 1.89 | [1.85, 1.92] | p < 0.001 |
| CYCLOPHOSPHAMIDE | 6.59 | [6.46, 6.72] | 1.89 | [1.87, 1.90] | p < 0.001 |
| PERTUZUMAB | 6.19 | [5.88, 6.51] | 1.82 | [1.77, 1.87] | p < 0.001 |
| CARBOPLATIN | 5.94 | [5.79, 6.09] | 1.78 | [1.76, 1.81] | p < 0.001 |
| EPIRUBICIN | 5.13 | [4.83, 5.44] | 1.63 | [1.58, 1.69] | p < 0.001 |
| DOXORUBICIN | 4.97 | [4.83, 5.10] | 1.60 | [1.58, 1.63] | p < 0.001 |
| RIBOCICLIB | 4.91 | [4.63, 5.21] | 1.59 | [1.53, 1.65] | p < 0.001 |
| RITUXIMAB | 4.86 | [4.75, 4.96] | 1.58 | [1.56, 1.60] | p < 0.001 |
| FULVESTRANT | 4.57 | [4.32, 4.84] | 1.52 | [1.46, 1.58] | p < 0.001 |
| EXEMESTANE | 4.22 | [3.94, 4.52] | 1.44 | [1.37, 1.51] | p < 0.001 |
| SORAFENIB | 3.95 | [3.68, 4.24] | 1.37 | [1.30, 1.44] | p < 0.001 |
| METHOTREXATE | 3.62 | [3.56, 3.68] | 1.29 | [1.27, 1.30] | p < 0.001 |
| PACLITAXEL | 2.76 | [2.66, 2.87] | 1.02 | [0.98, 1.05] | p < 0.001 |
| CELECOXIB | 2.10 | [2.02, 2.18] | 0.74 | [0.70, 0.78] | p < 0.001 |
| ERLOTINIB | 2.00 | [1.87, 2.14] | 0.69 | [0.63, 0.76] | p < 0.001 |
| FLUOROURACIL | 1.59 | [1.51, 1.68] | 0.46 | [0.41, 0.52] | p < 0.001 |
| BEVACIZUMAB | 1.06 | [1.00, 1.12] | 0.06 | [0.00, 0.12] | p = 0.042 |
| CAPECITABINE | 1.05 | [0.99, 1.12] | 0.05 | [-0.01, 0.12] | p = 0.114 |
| LEUPRORELIN | 0.99 | [0.93, 1.06] | -0.01 | [-0.08, 0.06] | p = 0.764 |
| b. Healthcare Professionals Only | |||||
| drug | ROR | 95%CI [lower, upper] | lnROR | 95%CI [lower, upper] | p-value |
| VISMODEGIB | 23.92 | [21.86, 26.17] | 3.17 | [3.08, 3.26] | p < 0.001 |
| PALBOCICLIB | 11.34 | [10.94, 11.75] | 2.43 | [2.39, 2.46] | p < 0.001 |
| RITUXIMAB | 7.72 | [7.53, 7.91] | 2.04 | [2.02, 2.07] | p < 0.001 |
| METHOTREXATE | 6.50 | [6.37, 6.63] | 1.87 | [1.85, 1.89] | p < 0.001 |
| LETROZOLE | 6.39 | [6.06, 6.74] | 1.86 | [1.80, 1.91] | p < 0.001 |
| RIBOCICLIB | 5.06 | [4.62, 5.55] | 1.62 | [1.53, 1.71] | p < 0.001 |
| FULVESTRANT | 4.99 | [4.60, 5.41] | 1.61 | [1.53, 1.69] | p < 0.001 |
| SORAFENIB | 4.54 | [4.14, 4.99] | 1.51 | [1.42, 1.61] | p < 0.001 |
| SIROLIMUS | 4.49 | [4.08, 4.94] | 1.50 | [1.41, 1.60] | p < 0.001 |
| EPIRUBICIN | 4.47 | [4.12, 4.85] | 1.50 | [1.42, 1.58] | p < 0.001 |
| CELECOXIB | 4.35 | [4.14, 4.56] | 1.47 | [1.42, 1.52] | p < 0.001 |
| ANASTROZOLE | 4.06 | [3.70, 4.46] | 1.40 | [1.31, 1.49] | p < 0.001 |
| PERTUZUMAB | 3.80 | [3.49, 4.13] | 1.33 | [1.25, 1.42] | p < 0.001 |
| DOCETAXEL | 3.68 | [3.48, 3.89] | 1.30 | [1.25, 1.36] | p < 0.001 |
| TRASTUZUMAB | 2.97 | [2.79, 3.16] | 1.09 | [1.03, 1.15] | p < 0.001 |
| PACLITAXEL | 2.64 | [2.51, 2.78] | 0.97 | [0.92, 1.02] | p < 0.001 |
| IRINOTECAN | 2.14 | [1.97, 2.34] | 0.76 | [0.68, 0.85] | p < 0.001 |
| FLUOROURACIL | 1.65 | [1.54, 1.76] | 0.50 | [0.43, 0.57] | p < 0.001 |
| CARBOPLATIN | 1.47 | [1.38, 1.57] | 0.39 | [0.32, 0.45] | p < 0.001 |
| BEVACIZUMAB | 1.44 | [1.35, 1.54] | 0.36 | [0.30, 0.43] | p < 0.001 |
| CAPECITABINE | 1.38 | [1.27, 1.50] | 0.32 | [0.24, 0.41] | p < 0.001 |
| CYCLOPHOSPHAMIDE | 1.17 | [1.10, 1.23] | 0.15 | [0.10, 0.21] | p < 0.001 |
| DOXORUBICIN | 1.08 | [1.01, 1.16] | 0.08 | [0.01, 0.15] | p = 0.034 |
| CISPLATIN | 1.05 | [0.96, 1.15] | 0.05 | [-0.05, 0.14] | p = 0.326 |
| OXALIPLATIN | 0.87 | [0.79, 0.95] | -0.14 | [-0.24, -0.05] | p = 0.003 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




