Submitted:
10 February 2026
Posted:
11 February 2026
You are already at the latest version
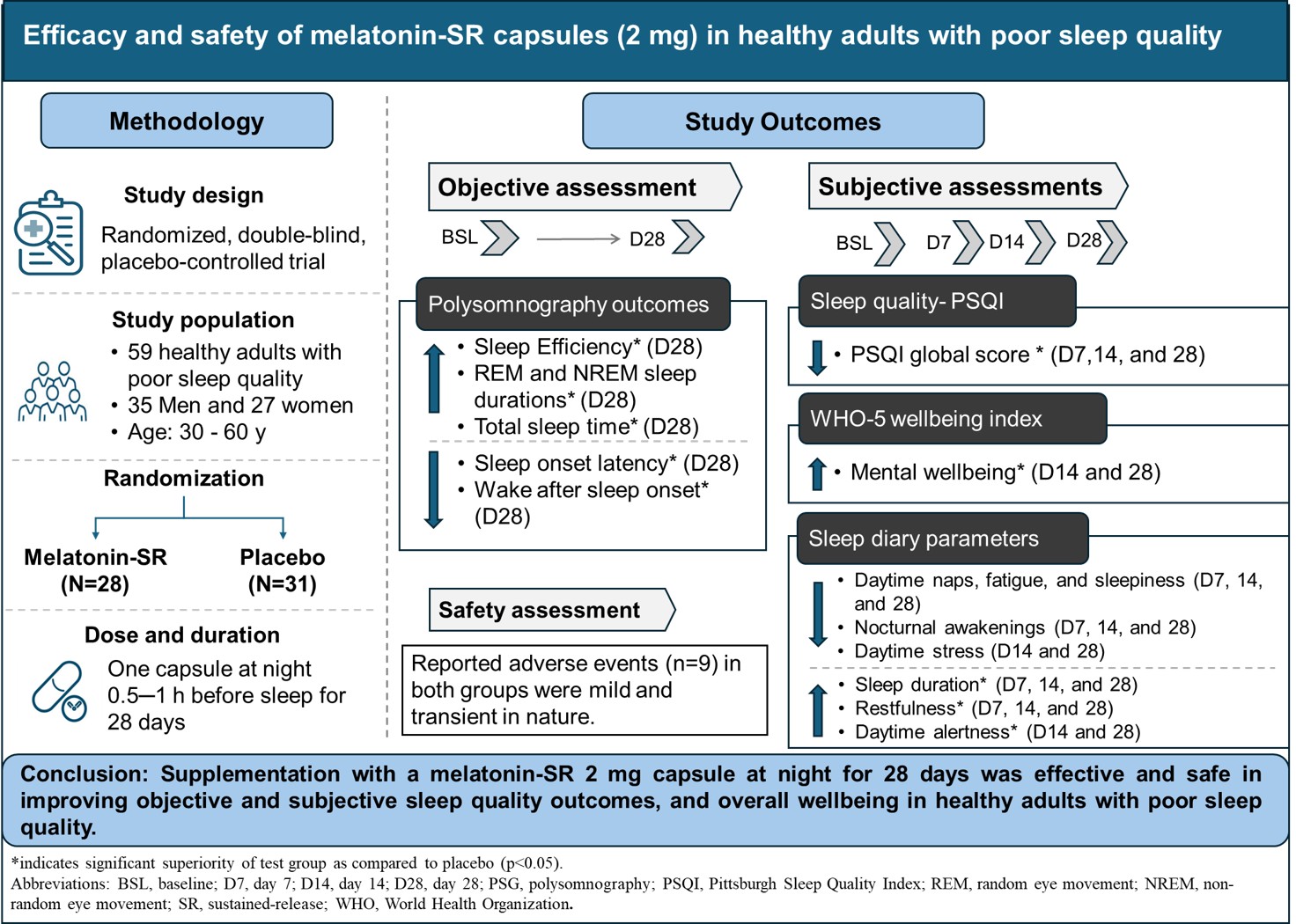
Abstract
Keywords:
1. Introduction
2. Results
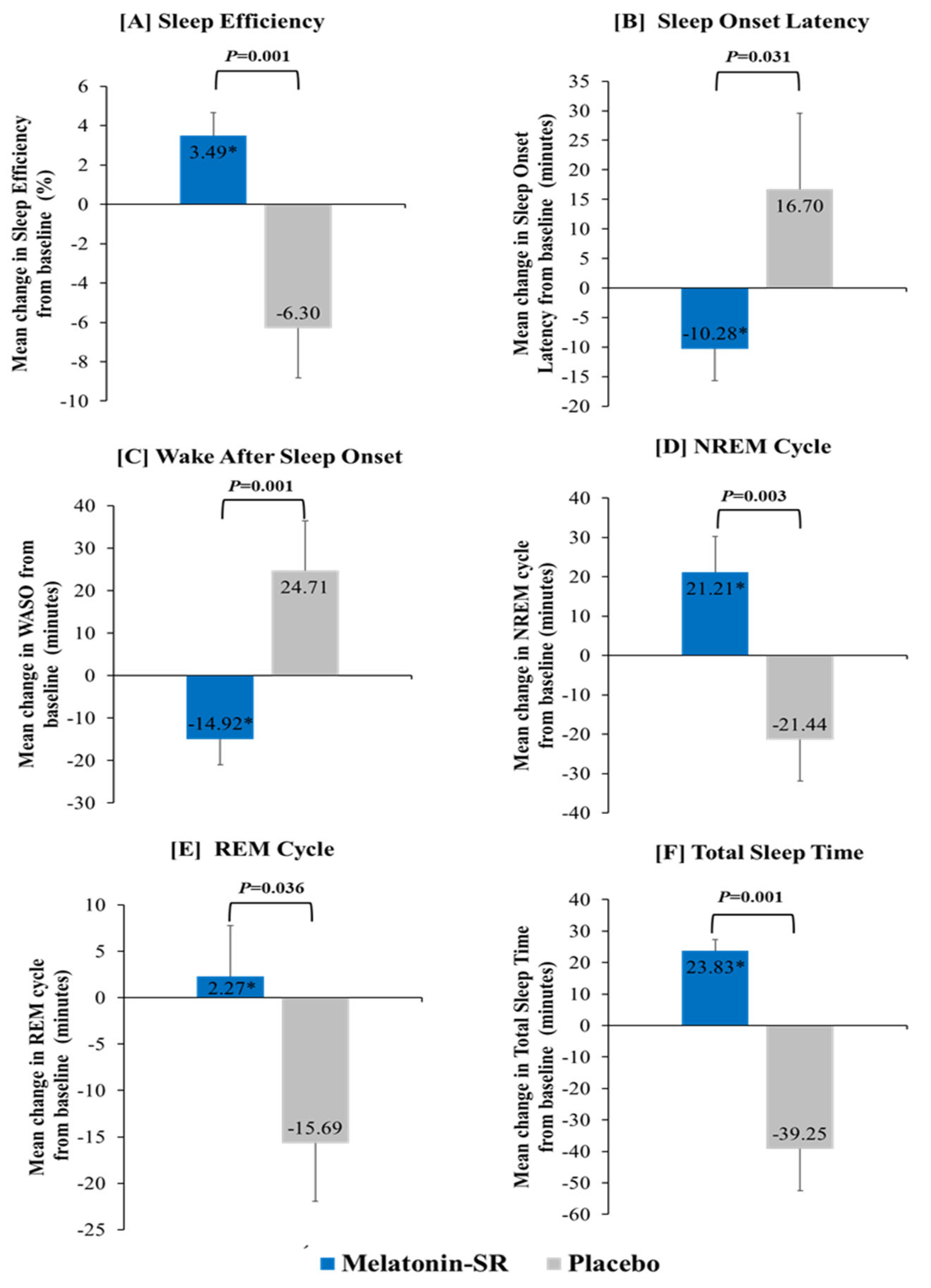
2.1. Change in Sleep Study Parameters Assessed Using PSG
2.1.1. Sleep Efficiency Assessment
2.1.2. Sleep Onset Latency (SOL) Assessment
2.1.3. Wake After Sleep Onset (WASO) Assessment
2.1.4. Non-Rapid Eye Movement (NREM) and Rapid Eye Movement (REM) Cycle Assessment
2.1.5. Total Sleep Time (TST) Assessment
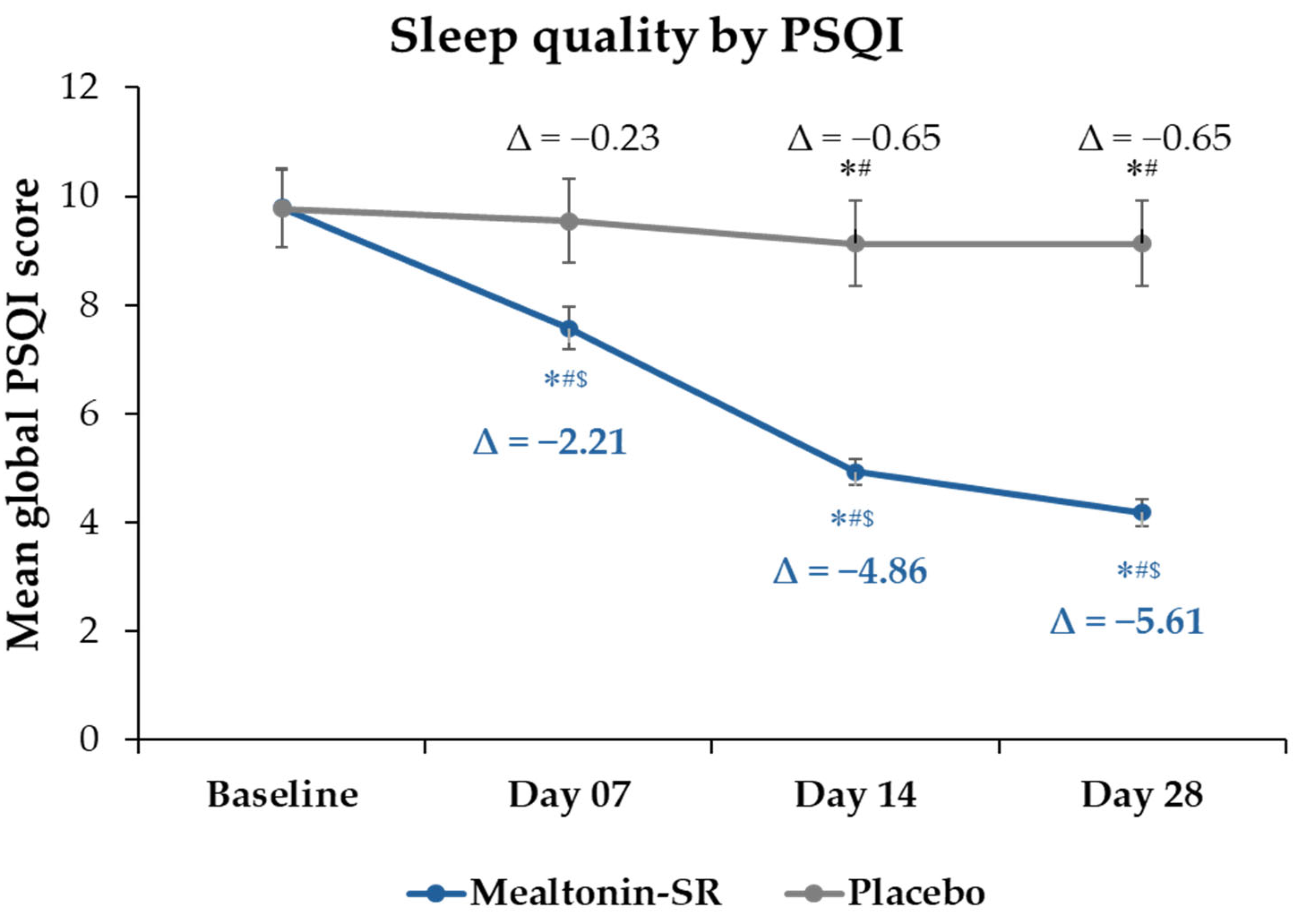
2.2. Change in Sleep Quality Evaluated Using Pittsburgh Sleep Quality Index (PSQI)
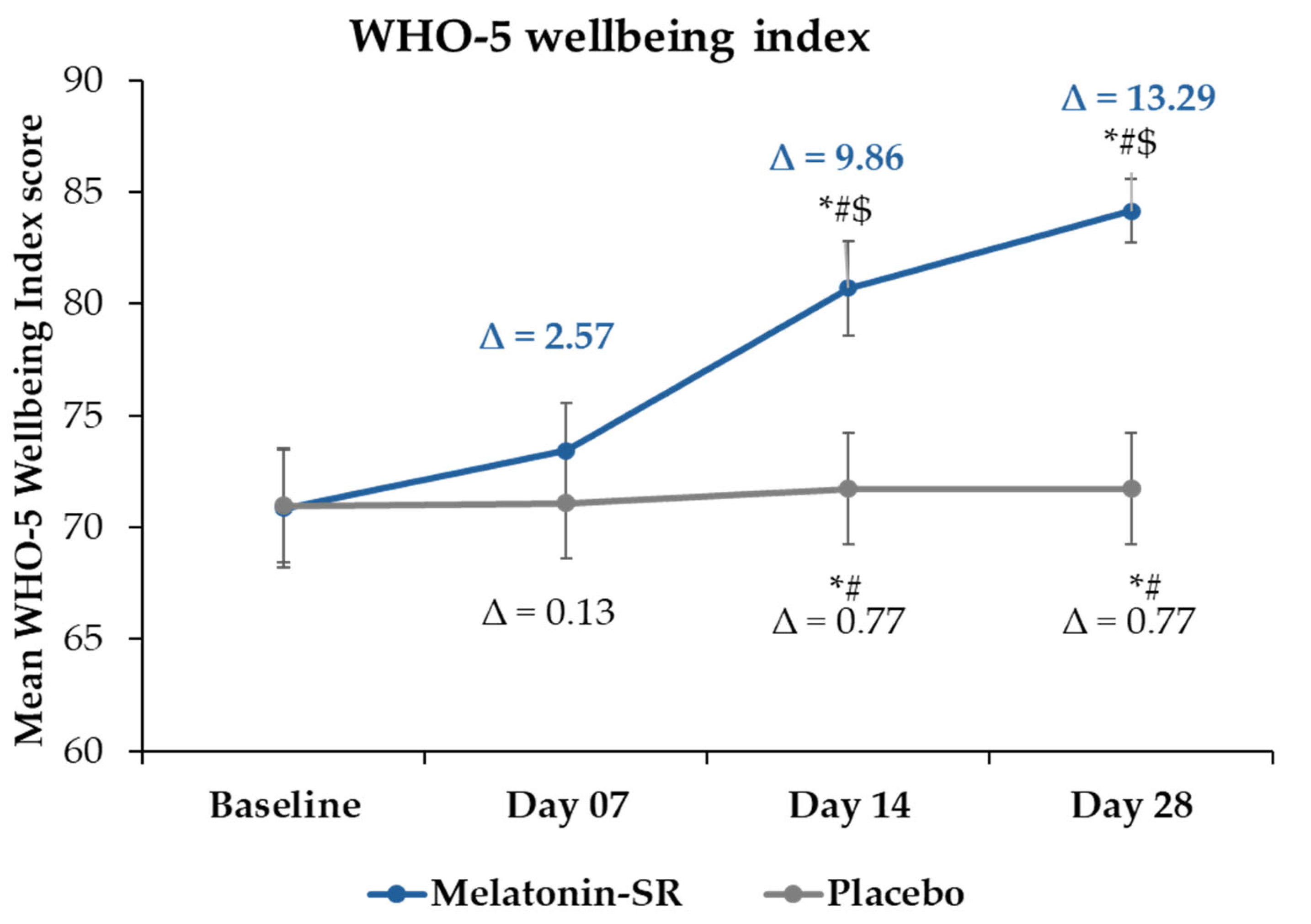
2.3. Change in QoL Assessed Using World Health Organization Five-Item (WHO-5) Well-Being Index
2.4. Change in Sleep-Related Parameters Assessed Using Participants’ Sleep Diary
2.5. Safety Assessment
3. Discussion
4. Materials and Methods
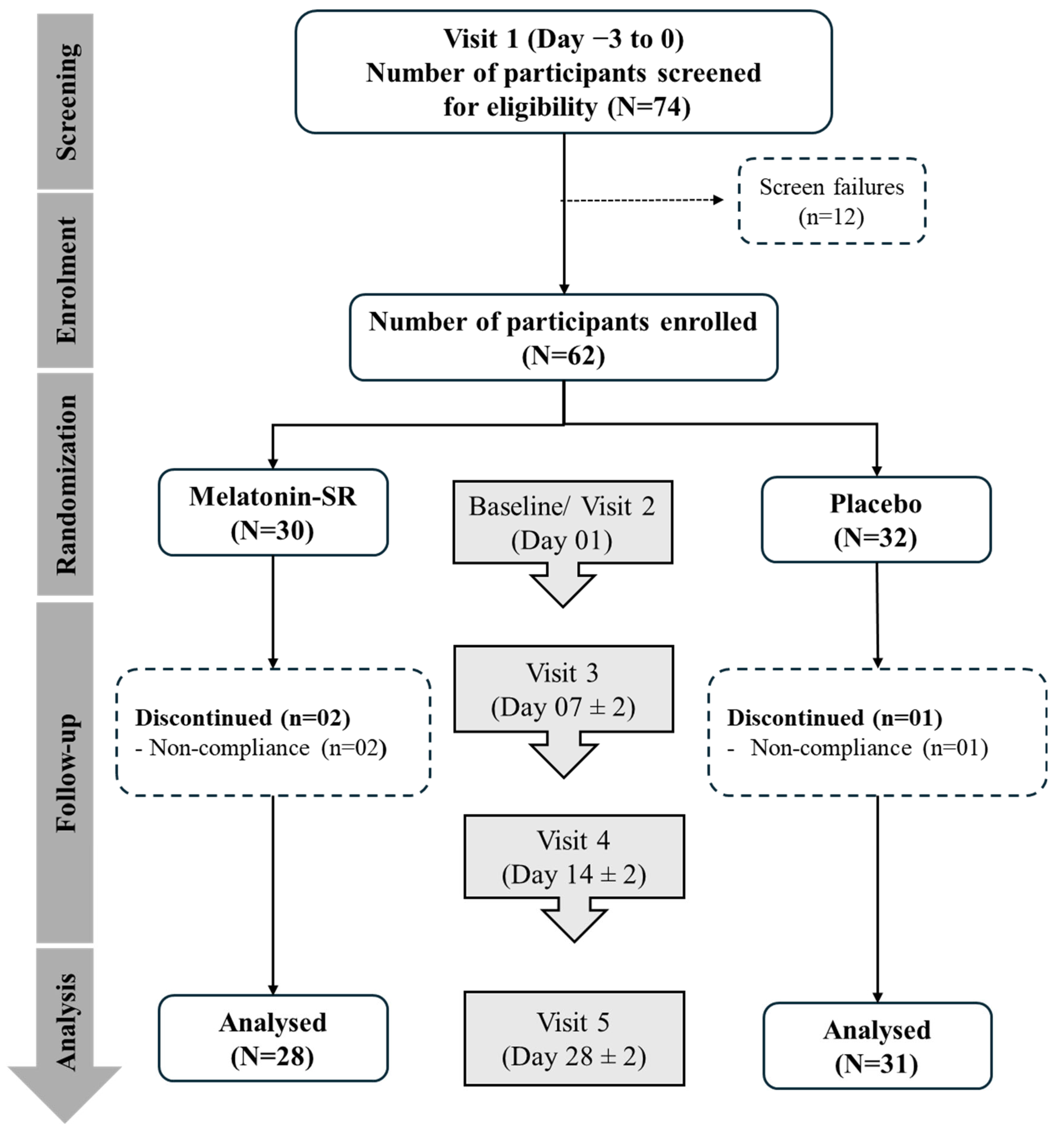
4.1. Study Design and Ethical Considerations
4.2. Study Population
4.3. Study Products
4.4. Randomization and Blinding
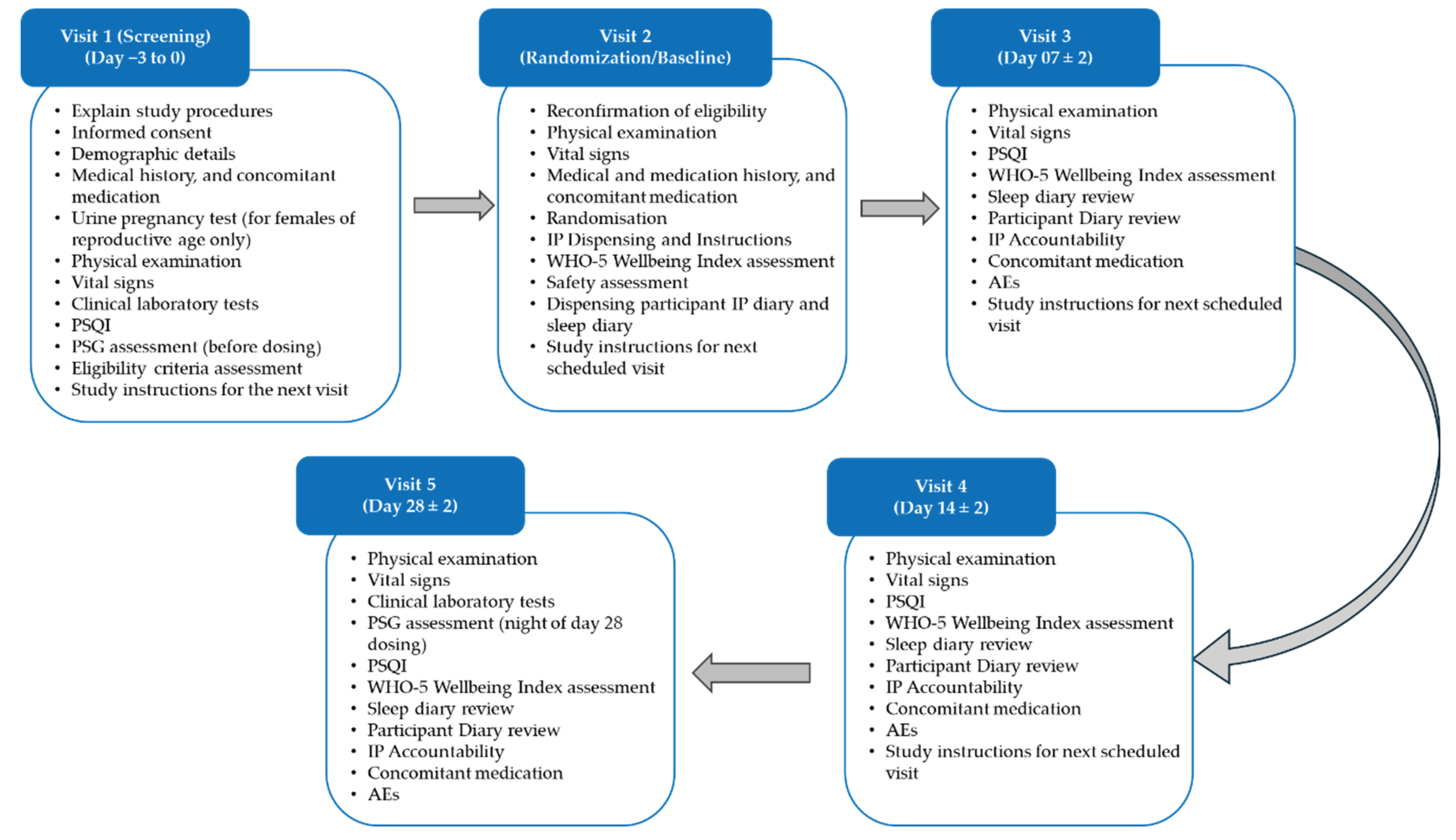
4.5. Study Procedure
4.6. Endpoints
4.7. Study Assessment Tools
4.7.1. Polysomnography
4.7.2. Pittsburgh Sleep Quality Index
4.7.3. WHO-5 Wellbeing Index
4.7.4. Sleep Diary Assessment
4.8. Statistical Analysis
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| AEs | Adverse event |
| AASM | American Academy of Sleep Medicine |
| BMI | Body mass index |
| CDC | Centers for Disease Control and Prevention |
| CTRI | Clinical Trials Registry-India |
| IP | Investigational product |
| ICMR | Indian Council of Medical Research |
| ICH-GCP | International Conference on Harmonization-Good Clinical Practices |
| Melatonin-SR | Sustained-release melatonin formulation |
| NREM | Non-rapid eye movement |
| NHIS | National Health Interview Survey |
| PI | Principal investigator |
| PSG | Polysomnography |
| PSQI | Pittsburgh Sleep Quality Index |
| QoL | Quality of life |
| REM | Rapid eye movement |
| SR | Sustained release |
| SD | Standard deviation |
| SE | Standard error |
| SOL | Sleep onset latency |
| SpO2 | Blood oxygen saturation |
| TEAEs | Treatment-emergent adverse events |
| TST | Total sleep time |
| WASO | wake after sleep onset |
| WHO | World Health Organization |
References
- Buysse, D.J. Sleep health: can we define it? Does it matter? Sleep 2014, 37(1), 9–17. [Google Scholar] [CrossRef] [PubMed]
- Ramar, K.; Malhotra, R.K.; Carden, K.A.; Martin, J.L.; Abbasi-Feinberg, F.; Aurora, R.N.; Kapur, V.K.; Olson, E.J.; Rosen, C.L.; Rowley, J.A.; Shelgikar, A.V.; Trotti, L.M. Sleep is essential to health: an American Academy of Sleep Medicine position statement. J Clin Sleep Med. 2021, 17(10), 2115–2119. [Google Scholar] [CrossRef]
- Liu, Y.; Wheaton, A.G.; Chapman, D.P.; Cunningham, T.J.; Lu, H.; Croft, J.B. Prevalence of healthy sleep duration among adults — United States, 2014. MMWR Morb Mortal Wkly Rep. 2016, 65, 137–141. [Google Scholar] [CrossRef] [PubMed]
- Adjaye-Gbewonyo, D.; Ng, A.E.; Black, L.I. Sleep difficulties in adults: United States, 2020. In NCHS Data Brief; National Center for Health Statistics: Hyattsville, MD, 2022; Volume no 436. [Google Scholar] [CrossRef]
- Chattu, V.K.; Manzar, M.D.; Kumary, S.; Burman, D.; Spence, D.W.; Pandi-Perumal, S.R. The global problem of insufficient sleep and its serious public health implications. Healthcare (Basel). 2018, 7(1), 1. [Google Scholar] [CrossRef]
- Esmaeilzadeh, S.; Habibolahi, F.; Moher, D.; Basirat, Z.; Gholinia, H.; Golsorkhtabaramiri; Mirabi, M.P. Melatonin and sleep parameters in infertile women with endometriosis: first results from the triple-blind randomized controlled trial of administration of melatonin in chronic pelvic pain and sleep disturbance. PLoS ONE. 2025, 20(4), e0321635. [Google Scholar] [CrossRef] [PubMed]
- Hafner, M.; Stepanek, M.; Taylor, J.; Troxel, W.M.; van Stolk, C. Why Sleep Matters-The Economic Costs of Insufficient Sleep: A Cross-Country Comparative Analysis. Rand Health Q. 2017, 6(4), 11. [Google Scholar]
- Fatemeh, G.; Sajjad, M.; Niloufar, R.; Neda, S.; Leila, S.; Khadijeh, M. Effect of melatonin supplementation on sleep quality: a systematic review and meta-analysis of randomized controlled trials. J Neurol. 2022, 269(1), 205–216. [Google Scholar] [CrossRef]
- Ramar, K.; Olson, E.J. Management of common sleep disorders. Am Fam Physician. 2013, 88(4), 231–238. [Google Scholar]
- Cardinali, D.P.; Pévet, P. Basic aspects of melatonin action. Sleep Med. Rev. 1998, 2, 175–190. [Google Scholar] [CrossRef]
- Poza, J.J.; Pujol, M.; Ortega-Albás, J.J.; Romero, O. Melatonin in sleep disorders. Neurología (English Edition) 2022, 37(7), 575–585. [Google Scholar] [CrossRef]
- Baser, K.H.C.; Haskologlu, I.C.; Erdag, E. Molecular links between circadian rhythm disruption, melatonin, and neurodegenerative diseases: An updated review. Molecules. 2025, 30, 1888. [Google Scholar] [CrossRef]
- Verma, A.K.; Singh, S.; Rizvi, S.I. Aging, circadian disruption and neurodegeneration: Interesting interplay. Exp Gerontol. 2023, 172, 112076. [Google Scholar] [CrossRef]
- Givler, D.; Givler, A.; Luther, P.M.; Wenger, D.M.; Ahmadzadeh, S.; Shekoohi, S.; Edinoff, A.N.; Dorius, B.K.; Jean Baptiste, C.; Cornett, E.M.; Kaye, A.M.; Kaye, A.D. Chronic Administration of Melatonin: Physiological and Clinical Considerations. Neurol Int. 2023, 15(1), 518–533. [Google Scholar] [CrossRef]
- Mun, J.G.; Wang, D.; Doerflein Fulk, D.L.; Fakhary, M.; Gualco, S.J.; Grant, R.W.; Mitmesser, S.H. A Randomized, Double-Blind, Crossover Study to Investigate the Pharmacokinetics of Extended-Release Melatonin Compared to Immediate-Release Melatonin in Healthy Adults. J Diet Suppl. 2024, 21(2), 182–194. [Google Scholar] [CrossRef]
- Thanawala, S.; Abiraamasundari, R.; Shah, R. Comparative Pharmacokinetics of Sustained-Release versus Immediate-Release Melatonin Capsules in Fasting Healthy Adults: A Randomized, Open-Label, Cross-Over Study. Pharmaceutics 2024, 16(10), 1248. [Google Scholar] [CrossRef] [PubMed]
- Rundo, J.V.; Downey, R., 3rd. Polysomnography. Handb Clin Neurol. 2019, 160, 381–392. [Google Scholar] [CrossRef] [PubMed]
- Luthringer, R.; Muzet, M.; Zisapel, N.; Staner, L. The effect of prolonged-release melatonin on sleep measures and psychomotor performance in elderly patients with insomnia. Int Clin Psychopharmacol. 2009, 24(5), 239–249. [Google Scholar] [CrossRef] [PubMed]
- Duffy, J.F.; Wang, W.; Ronda, J.M.; Czeisler, C.A. High dose melatonin increases sleep duration during nighttime and daytime sleep episodes in older adults. J Pineal Res. 2022, 73(1), e12801. [Google Scholar] [CrossRef]
- Jafari, B.; Mohsenin, V. Polysomnography. Clin Chest Med. 2010, 31, 287–297. [Google Scholar] [CrossRef]
- Hirshkowitz, M.; Whiton, K.; Albert, S.M.; Alessi, C.; Bruni, O.; DonCarlos, L.; Hazen, N.; Herman, J.; Katz, E.S.; Kheirandish-Gozal, L.; Neubauer, D.N.; O'Donnell, A.E.; Ohayon, M.; Peever, J.; Rawding, R.; Sachdeva, R.C.; Setters, B.; Vitiello, M.V.; Ware, J.C.; Adams Hillard, P.J. National Sleep Foundation’s sleep time duration recommendations: methodology and results summary. Sleep Health 2015, 1(1), 40–43. [Google Scholar] [CrossRef]
- Ohayon, M.; Wickwire, E.M.; Hirshkowitz, M.; Albert, S.M.; Avidan, A.; Daly, F.J.; Dauvilliers, Y.; Ferri, R.; Fung, C.; Gozal, D.; Hazen, N.; Krystal, A.; Lichstein, K.; Mallampalli, M.; Plazzi, G.; Rawding, R.; Scheer, F.A.; Somers, V.; Vitiello, M.V. National Sleep Foundation’s sleep quality recommendations: first report. Sleep Health. 2017, 3(1), 6–19. [Google Scholar] [CrossRef] [PubMed]
- Almeida Montes, L.G.; Ontiveros Uribe, M.P.; Cortés Sotres, J.; Heinze Martin, G. Treatment of primary insomnia with melatonin: a double-blind, placebo-controlled, crossover study. J Psychiatry Neurosci. 2003, 28(3), 191–196. [Google Scholar] [CrossRef]
- Wade, A.G.; Ford, I.; Crawford, G.; McConnachie, A.; Nir, T.; Laudon, M.; Zisapel, N. Nightly treatment of primary insomnia with prolonged release melatonin for 6 months: a randomized placebo controlled trial on age and endogenous melatonin as predictors of efficacy and safety. BMC medicine 2010, 8, 51. [Google Scholar] [CrossRef]
- Kamkar, M.Z.; Mahyar, M.; Maddah, S.A.; Khoddam, H.; Modanloo, M. The effect of melatonin on quality of sleep in patients with sleep disturbance admitted to post coronary care units: A randomized controlled trial. Biomedicine (Taipei). 2021, 11(1), 34–40. [Google Scholar] [CrossRef]
- Lee, S.; Kim, J.H.; Chung, J.H. The association between sleep quality and quality of life: a population-based study. Sleep Med. 2021, 84, 121–126. [Google Scholar] [CrossRef]
- Wade, A.G.; Ford, I.; Crawford, G.; McMahon, A.D.; Nir, T.; Laudon, M.; Zisapel, N. Efficacy of prolonged release melatonin in insomnia patients aged 55-80 years: quality of sleep and next-day alertness outcomes. Curr Med Res Opin. 2007, 23(10), 2597–2605. [Google Scholar] [CrossRef]
- Lemoine, P.; Nir, T.; Laudon, M.; Zisapel, N. Prolonged-release melatonin improves sleep quality and morning alertness in insomnia patients aged 55 years and older and has no withdrawal effects. J Sleep Res. 2007, 16(4), 372–380. [Google Scholar] [CrossRef]
- de Seabra, M.L.V.; Bignotto, M.; Pinto, L.R., Jr.; Tufik, S. Randomized, Double-blind Clinical Trial, Controlled with Placebo, of the Toxicology of Chronic Melatonin Treatment. J Pineal Res. 2000, 29, 193–200. [Google Scholar] [CrossRef]
- Buscemi, N.; Vandermeer, B.; Hooton, N.; Pandya, R.; Tjosvold, L.; Hartling, L.; Baker, G.; Klassen, T.P.; Vohra, S. The efficacy and safety of exogenous melatonin for primary sleep disorders: A meta-analysis. J Gen Intern Med. 2005, 20, 1151–1158. [Google Scholar] [CrossRef] [PubMed]
- BaHammam, A.S.; Gacuan, D.E.; George, S.; Acosta, K.L.; Pandi-Perumal, S.R.; Gupta, R. Polysomnography I: procedure and technology. In Synopsis of sleep medicine; Pandi-Perumal, SR, Ed.; Apple Academic Press: Canada, 2016; p. 443456. [Google Scholar]
- Bruyneel, M.; Sanida, C.; Art, G.; Libert, W.; Cuvelier, L.; Paesmans, M.; Sergysels, R.; Ninane, V. Sleep efficiency during sleep studies: results of a prospective study comparing home-based and in-hospital polysomnography. J Sleep Res. 2011, 20 1 Pt 2, 201–206. [Google Scholar] [CrossRef] [PubMed]
- Bruyneel, M.; Libert, W.; Ameye, L.; Ninane, V. Comparison between home and hospital set-up for unattended home-based polysomnography: a prospective randomized study. Sleep Med. 2015, 16(11), 1434–1438. [Google Scholar] [CrossRef] [PubMed]
- Lehrer, H.M.; Yao, Z.; Krafty, R.T.; vans, M.A.; Buysse, D.J.; Kravitz, H.M.; Matthews, K.A.; Gold, E.B.; Harlow, S.D.; S–amuelsson, L.B.; Hall, M.H. Comparing polysomnography, actigraphy, and sleep diary in the home environment: The Study of Women's Health Across the Nation (SWAN) Sleep Study. Sleep Adv. 2022, 3(1), zpac001. [Google Scholar] [CrossRef]
- Buysse, D.; Reynolds, C.; Monk, T. Pittsburgh Sleep Quality Index: a new instrument for psychiatric practice and research. Psychiatry Res. 1989, 28(2), 193–213. [Google Scholar] [CrossRef] [PubMed]
- WHO. The World Health Organization-Five Well-Being Index (WHO-5) [Internet]. 2024. Available online: https://www.who.int/publications/m/item/WHO-UCN-MSD-MHE-2024.01.
- Topp, C.W.; Østergaard, S.D.; Søndergaard, S.; Bech, P. The WHO-5 Well-Being Index: A Systematic Review of the Literature. Psychother Psychosom. 2015, 84(3), 167–176. [Google Scholar] [CrossRef] [PubMed]
| Parameters | Melatonin-SR (N=30) | Placebo (N=32) |
Total (N=62) |
P-value |
|---|---|---|---|---|
| Age (years) | 40.63 (8.05) | 39.25 (5.62) | 39.92 (6.88) | 0.439 |
| Sex (n, %) Men Women |
15 (50.00) 15 (50.00) |
20 (62.50) 12 (37.50) |
35 (56.50) 27 (43.50) |
0.321 |
| Body weight (kg) | 66.02 (11.31) | 66.09 (9.04) | 66.05 (10.12) | 0.979 |
| Height (cm) | 164.60 (10.21) | 164.81 (6.93) | 164.71 (8.60) | 0.925 |
| BMI (kg/m2) | 24.11 (2.35) | 24.30 (2.73) | 24.20 (2.53) | 0.769 |
| Sleep diary questionnaire | Melatonin-SR | Placebo | ||||||||||||
|---|---|---|---|---|---|---|---|---|---|---|---|---|---|---|
| Baseline | Day 07 | Day 14 | Day 28 | Baseline | Day 07 | Day 14 | Day 28 | |||||||
| Mean number of daytime naps | 1.62 (0.57) | 1.63 (0.60) | 1.33*# (0.49) | 1.00*# (0.00) |
1.96 (0.66) | 2.00 (0.69) |
1.92 (0.74) | 2.00 (0.76) |
||||||
| Mean change from baseline | - | -0.05 | -0.33 | -1.17*$ | - | 0.04 | -0.04 | 0.04 | ||||||
| Mean duration of daytime naps (minutes) | 38.08 (13.86) | 37.89*# (18.43) | 33.33*# (14.14) | 10.00*# (0.00) | 38.08 (18.77) | 38.08 (18.77) | 37.12 (18.88) | 39.80 (20.02) | ||||||
| Mean change from baseline | - | -3.68*$ | -8.89*$ | -21.67*$ | - | 0.00 | -0.96 | 1.80 | ||||||
| Mean daytime Fatigue Level | 2.29 (1.08) | 1.96*# (1.43) | 1.36*# (1.13) | 0.25*# (0.44) | 2.23 (0.92) | 2.32 (1.01) |
2.52 (1.34) | 2.65 *# (1.38) | ||||||
| Mean change from baseline | - | -0.32*$ | -0.93*$ | -2.04*$ | - | 0.10 | 0.29 | 0.42 | ||||||
| Mean daytime Stress Level | 2.29 (1.21) | 2.04*# (1.48) | 1.39*# (1.10) | 0.25*# (0.44) | 2.23 (0.80) | 2.26 (0.86) |
2.19 (1.01) | 2.42 (1.36) | ||||||
| Mean change from baseline | - | -0.25 | -0.89*$ | -2.04*$ | - | 0.03 | -0.03 | 0.19 | ||||||
| Mean Lights out time (hours) | 22.98 (0.61) | 22.84*# (0.41) | 22.45*# (0.44) | 21.89*# (0.34) | 22.44 (0.70) | 22.52 (0.69) | 22.45 (0.73) | 22.53 (0.46) | ||||||
| Mean change from baseline | - | -0.14*$ | -0.54*$ | -1.09*$ | - | 0.08 | 0.01 | 0.09 | ||||||
| Mean Time taken to fall asleep after lights out (minutes) | 42.50 (13.78) | 33.75*# (7.77) | 23.57*# (4.88) | 14.46*# (3.14) | 38.06 (11.38) | 43.06*# (13.21) | 39.03 (11.06) | 41.94*# (14.47) | ||||||
| Mean change from baseline | - | -8.75*$ | -18.93*$ | -28.04*$ | - | 5.00 | 0.97 | 3.87 | ||||||
| Mean Number of times participants woke up during night | 1.82 (0.77) | 1.14*# (0.93) | 0.50*# (0.51) | 0.00*# (0.00) | 1.61 (0.99) | 1.81 (0.79) |
1.87*# (0.99) | 1.94*# (1.00) | ||||||
| Mean change from baseline | - | -0.68*$ | -1.32*$ | -1.82*$ | - | 0.19 | 0.26 | 0.32 | ||||||
| Mean duration of staying awake during the night (minutes) | 11.07 (5.83) | 5.29*# (5.03) | 2.75*# (3.15) | 0.00*# (0.00) | 10.65 (6.55) | 12.90*# (5.59) | 14.84*# (8.71) | 15.65*# (8.92) | ||||||
| Mean change from baseline | - | -5.79*$ | -8.32*$ | -11.07*$ | - | 2.26 | 4.19 | 5.00 | ||||||
| Mean number of hours of sleep at night | 7.13 (0.43) | 7.44*# (0.56) | 8.48*# (0.62) | 9.45*# (0.50) | 8.13 (1.16) | 8.10 (1.13) | 8.18 (1.10) | 8.00*# (1.05) | ||||||
| Mean change from baseline | - | 0.31*$ | 1.36*$ | 2.32*$ | - | -0.03 | 0.05 | -0.13 | ||||||
| Mean Time of waking up in morning (Hours) | 6.11 (0.42) | 6.28*# (0.65) | 6.96*# (0.71) | 7.34*# (0.51) | 6.86 (0.86) | 6.91 (0.88) | 6.92*# (0.94) | 6.81 (0.87) | ||||||
| Mean change from baseline | - | 0.17*$ | 0.86*$ | 1.23*$ | - | 0.05 | 0.05 | -0.05 | ||||||
| Mean Rest Score | 2.79 (0.42) | 3.75*# (0.44) | 4.39*# (0.50) | 5.00*# (0.00) | 3.45 (0.51) | 3.29*# (0.74) | 3.29*# (0.74) | 2.55*# (0.62) | ||||||
| Mean change from baseline | - | 0.96*$ | 1.61*$ | 2.21*$ | - | -0.16 | -0.16 | -0.90 | ||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




