Submitted:
30 January 2026
Posted:
02 February 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Materials and Methods
Study Design and Setting
Study Population and Data Sources
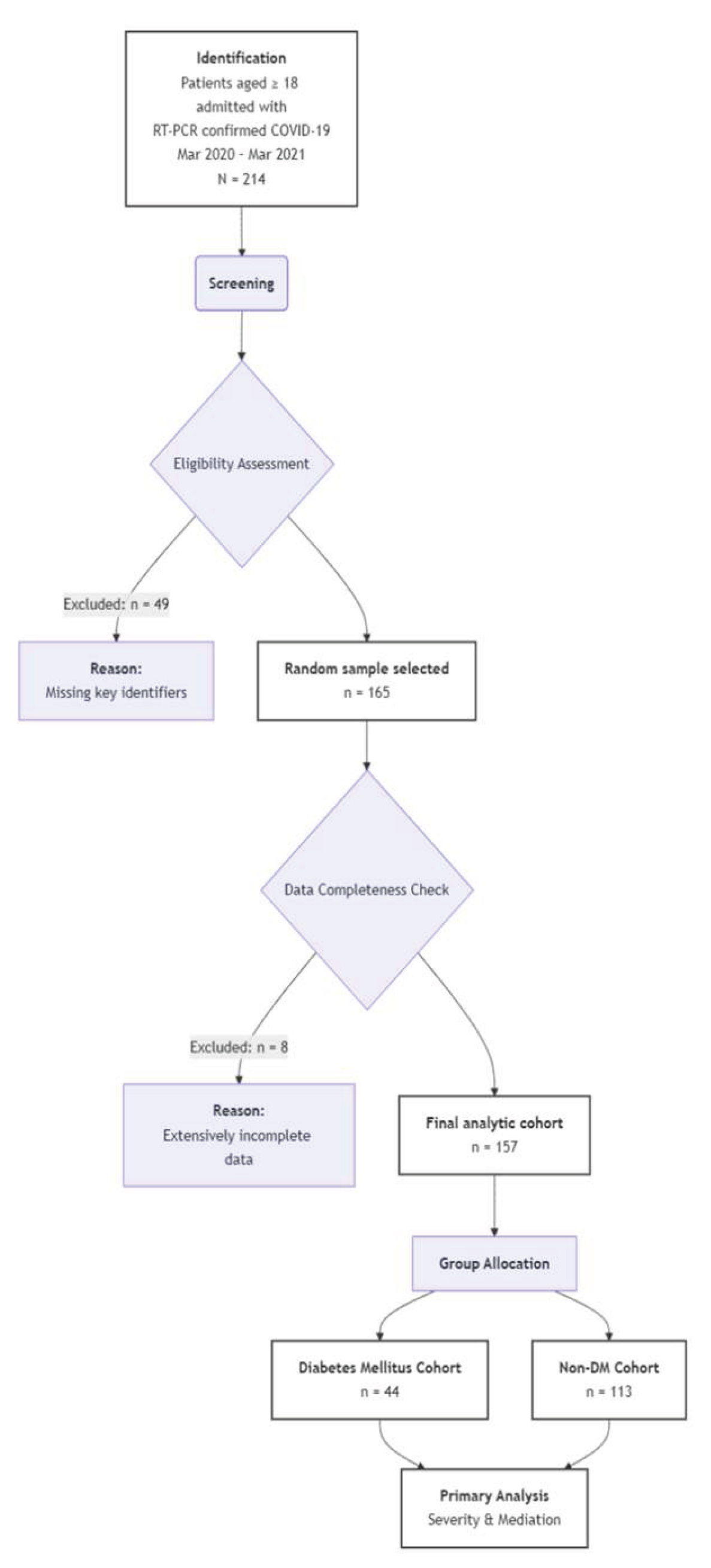
Sample Size and Participant Selection
Data Collection and Variables
Statistical Analysis
Ethical Considerations
Patient and Public Involvement
Results
Characteristics of the Study Cohort
Association Between DM and COVID-19 Severity and Outcomes
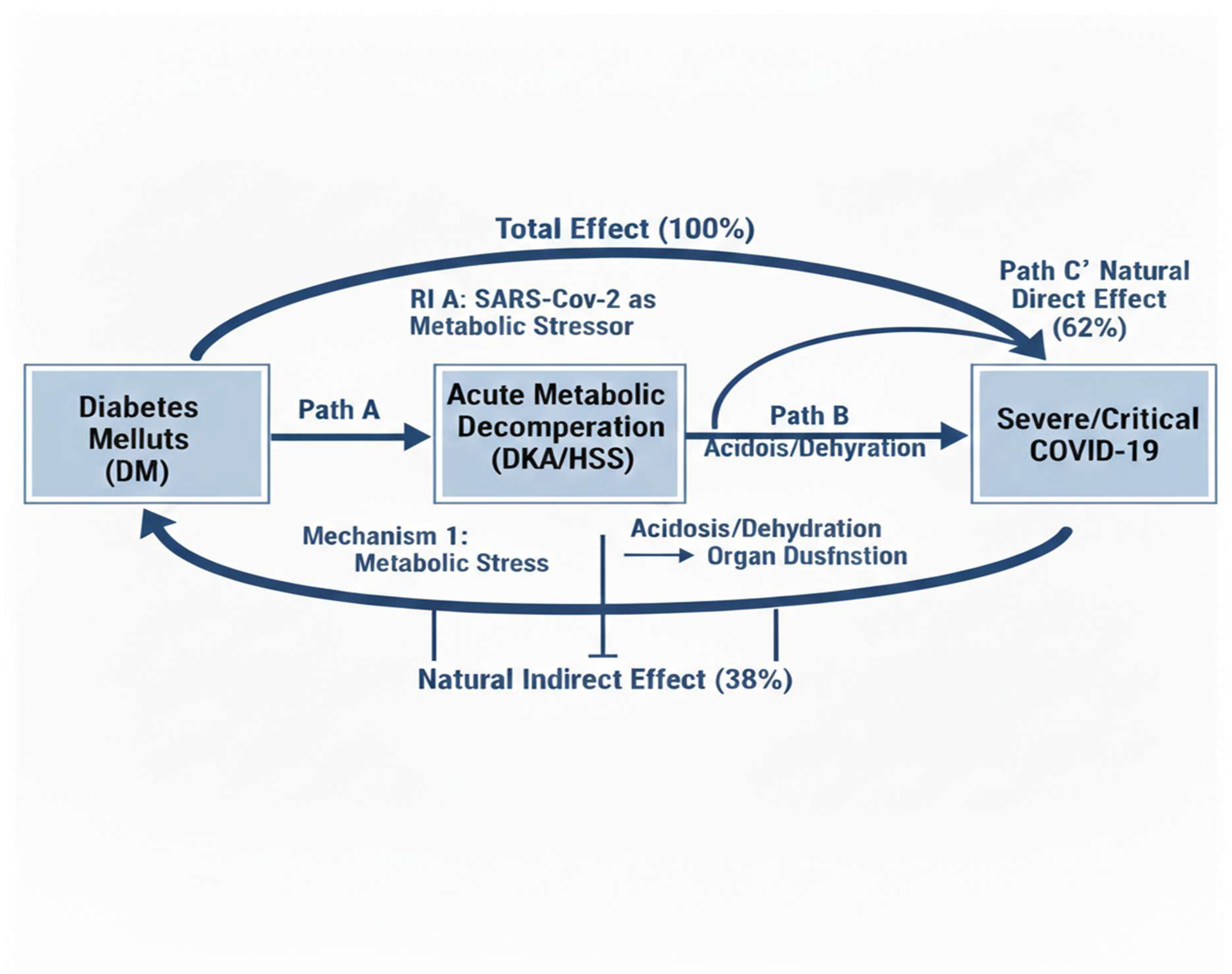
Incidence of Acute Diabetic Complications and Mediating Pathway
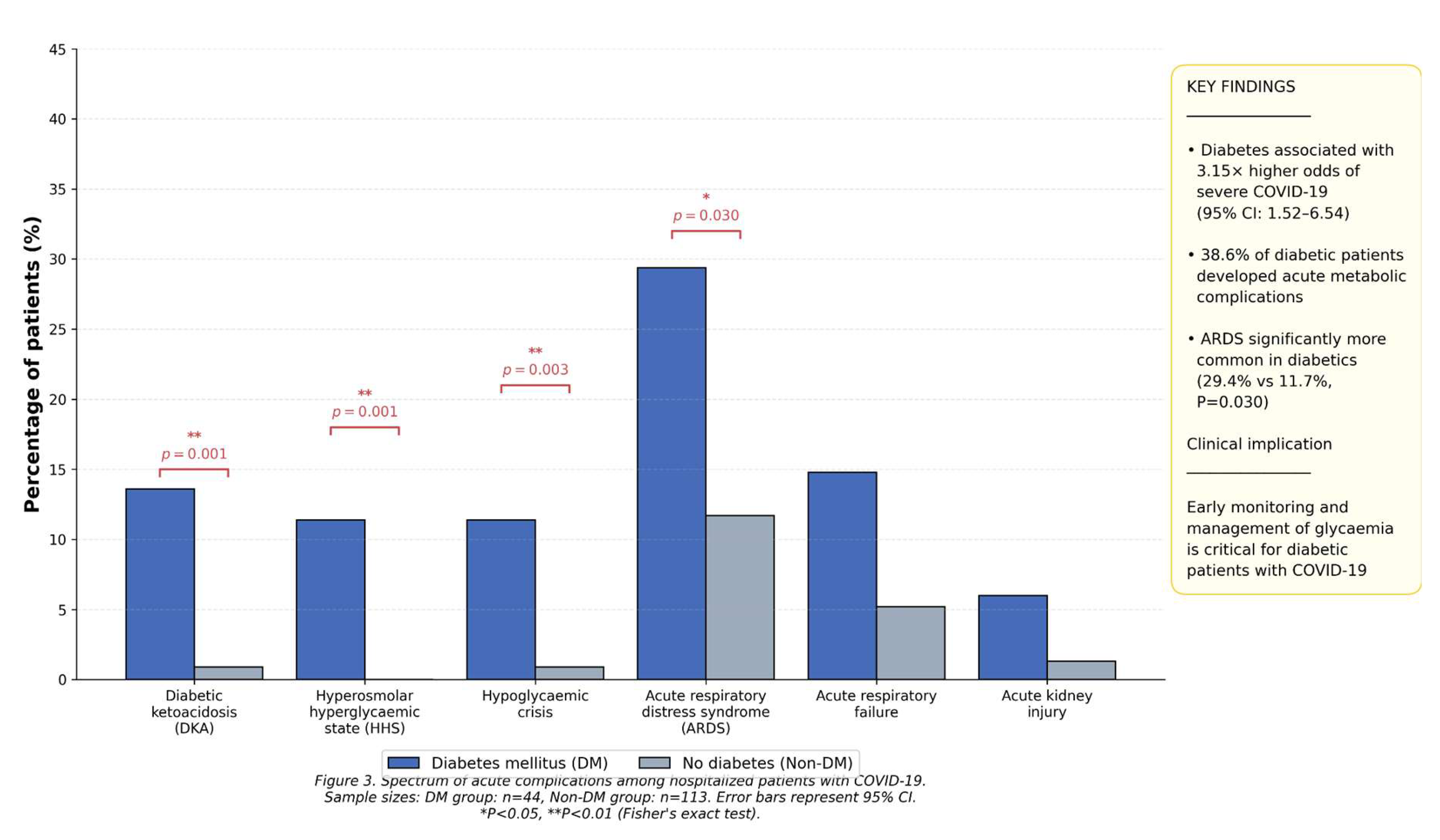
Specific COVID-19-Related Complications by Diabetes Status
Discussion
Conclusion
| Outcome | Total (N=157) | DM (n=44) | Non-DM (n=113) | p-value | Adjusted odds ratio (95% CI)† | p-value† |
|---|---|---|---|---|---|---|
| Disease severity, n (%) <0.001 | ||||||
| Mild/moderate disease | 109 (69.4) | 22 (50.0) | 87 (77.0) | 1.0 (Reference) | ||
| Severe/critical disease | 48 (30.6) | 22 (50.0) | 26 (23.0) | 3.15 (1.52-6.54) | 0.002 | |
| Any COVID-19 complication, n % | 111 (70.7) | 34 (77.3) | 77 (68.1) | 0.259 | 1.42 (0.63-3.21) | 0.402 |
| Acute diabetic complications n/N (%) | ||||||
| Diabetic ketoacidosis | 7/157 (4.5) | 6/44 (13.6) | 1/113 (0.9) | 0.001 | - | - |
| Hyperosmolar hyperglycemic state (HHS) | 5/157 (3.2) | 5/44 (11.4) | 0/113 (0.0) | <0.001 | - | - |
| Clinical outcomes, n (%) | ||||||
| Recovered | 129 (82.2) | 34 (77.3) | 95 (84.1) | 0.311 | 1.0 (Reference) | |
| Died | 28 (17.8) | 10 (22.7) | 18 (15.9) | 1.48 (0.62 - 3.55) | 0.380 | |
| Type of COVID-19 complication | Total (n=111) | DM (n=34) | Non-DM (n=77) | p-value* |
|---|---|---|---|---|
| Severe pneumonia, n (%) | 90 (81.1) | 27 (79.4) | 63 (81.8) | 0.757 |
| Acute respiratory distress syndrome (ARDS), n (%) | 19 (17.1) | 10 (29.4) | 9 (11.7) | 0.030 |
| Acute respiratory failure (%) | 9 (8.1) | 5 (14.7) | 4 (5.2) | 0.128 |
| Acute kidney injury, n (%) | 3 (2.7) | 2 (5.9) | 1(1.3) | 0.202 |
| Thromboembolic events (DVT & PE), n (%) | 8 (7.2) | 2 (5.9) | 6 (7.8) | 1.000 |
| Acute cardiac injury, n (%) | 7 (6.3) | 2 (5.9) | 5 (6.5) | 1.000 |
Author Contributions
References
- Fronteira, I; Sidat, M; Magalhães, JP; de Barros, FPC; Delgado, AP; Correia, T; Daniel-Ribeiro, CT; Ferrinho, P. The SARS-CoV-2 pandemic: A syndemic perspective. One Health 2021, 12, 100228. [Google Scholar] [CrossRef] [PubMed]
- Guo, W; Li, M; Dong, Y; et al. Diabetes is a risk factor for the progression and prognosis of COVID-19. Diabetes Metab Res Rev. 2020, 36(7), e3319. [Google Scholar] [CrossRef] [PubMed]
- Yu, H; Liu, J; He, X. From Glucotoxicity to Lung Injury: Emerging Perspectives on Diabetes-Associated Respiratory Complications. Lung 2025, 203, 80. [Google Scholar] [CrossRef] [PubMed]
- Zhou, F; Yu, T; Du, R; Fan, G; Liu, Y; Liu, Z; Xiang, J; Wang, Y; Song, B; Gu, X; Guan, L; Wei, Y; Li, H; Wu, X; Xu, J; Tu, S; Zhang, Y; Chen, H; Cao, B. Clinical course and risk factors for mortality of adult inpatients with COVID-19 in Wuhan, China: a retrospective cohort study. Lancet 2020, 395, 1054–1062. [Google Scholar] [CrossRef] [PubMed]
- Onder, G; Rezza, G; Brusaferro, S. Case-Fatality Rate and Characteristics of Patients Dying in Relation to COVID-19 in Italy. JAMA 2020, 323, 1775–1776. [Google Scholar] [CrossRef] [PubMed]
- Stokes, EK; Zambrano, LD; Anderson, KN; Marder, EP; Raz, KM; El Burai Felix, S; Tie, Y; Fullerton, KE. Coronavirus Disease 2019 Case Surveillance - United States, January 22-May 30, 2020. MMWR Morb Mortal Wkly Rep 2020, 69, 759–765. [Google Scholar] [CrossRef] [PubMed]
- Kumar, A; Arora, A; Sharma, P; Anikhindi, SA; Bansal, N; Singla, V; Khare, S; Srivastava, A. Is diabetes mellitus associated with mortality and severity of COVID-19? A meta-analysis. Diabetes Metab Syndr 2020, 14, 535–545. [Google Scholar] [CrossRef] [PubMed]
- Hussain, A; Bhowmik, B; do Vale Moreira, NC. COVID-19 and diabetes: Knowledge in progress. Diabetes Res Clin Pract 2020, 162, 108142. [Google Scholar] [CrossRef] [PubMed]
- Bornstein, SR; Dalan, R; Hopkins, D; Mingrone, G; Boehm, BO. Endocrine and metabolic link to coronavirus infection. Nat Rev Endocrinol 2020, 16, 297–298. [Google Scholar] [CrossRef] [PubMed]
- Yang, JK; Lin, SS; Ji, XJ; Guo, LM. Binding of SARS coronavirus to its receptor damages islets and causes acute diabetes. Acta Diabetol 2010, 47, 193–199. [Google Scholar] [CrossRef] [PubMed]
- Muniyappa, R; Gubbi, S. COVID-19 pandemic, coronaviruses, and diabetes mellitus. Am J Physiol Endocrinol Metab 2020, 318, E736–E741. [Google Scholar] [CrossRef] [PubMed]
- Pal, R; Bhadada, SK. Managing common endocrine disorders amid COVID-19 pandemic. Diabetes Metab Syndr. 2020, 14(5), 767–771. [Google Scholar] [CrossRef] [PubMed]
- Wu, Z; McGoogan, JM. Characteristics of and Important Lessons From the Coronavirus Disease 2019 (COVID-19) Outbreak in China: Summary of a Report of 72 314 Cases From the Chinese Center for Disease Control and Prevention. JAMA 2020, 323(13), 1239–1242. [Google Scholar] [CrossRef] [PubMed]
- Lone, SA; Ahmad, A. COVID-19 pandemic - an African perspective. Emerg Microbes Infect 2020, 9, 1300–1308. [Google Scholar] [CrossRef] [PubMed]
- Mohamed, SF; Mwangi, M; Mutua, MK; Kibachio, J; Hussein, A; Ndegwa, Z; Owondo, S; Asiki, G; Kyobutungi, C. Prevalence and factors associated with pre-diabetes and diabetes mellitus in Kenya: results from a national survey. BMC Public Health 2018, 18, 1215. [Google Scholar] [CrossRef] [PubMed]
- Nkengasong, JN; Ndembi, N; Tshangela, A; Raji, T. COVID-19 vaccines: how to ensure Africa has access. Nature 2020, 586, 197–199. [Google Scholar] [CrossRef] [PubMed]
- Haider, N; Osman, AY; Gadzekpo, A; Akipede, GO; Asogun, D; Ansumana, R; Lessells, RJ; Khan, P; Hamid, MMA; Yeboah-Manu, D; Mboera, L; Shayo, EH; Mmbaga, BT; Urassa, M; Musoke, D; Kapata, N; Ferrand, RA; Kapata, PC; Stigler, F; Czypionka, T; Zumla, A; Kock, R; McCoy, D. Lockdown measures in response to COVID-19 in nine sub-Saharan African countries. BMJ Glob Health 2020, 5, e003319. [Google Scholar] [CrossRef] [PubMed]
- Sardu, C; D’Onofrio, N; Balestrieri, ML; Barbieri, M; Rizzo, MR; Messina, V; Maggi, P; Coppola, N; Paolisso, G; Marfella, R. Outcomes in Patients With Hyperglycemia Affected by COVID-19: Can We Do More on Glycemic Control? Diabetes Care 2020, 43, 1408–1415. [Google Scholar] [CrossRef] [PubMed]
- Agyemang, C; Richters, A; Jolani, S; et al. Ethnic minority status as a determinant of COVID-19 vaccine hesitancy and a target for intervention strategies in the Netherlands: findings from the HELIUS study. Lancet Reg Health Eur. 2022, 17, 100372. [Google Scholar]
- Mbunge, E; Akinnuwesi, B; Fashoto, SG; et al. A critical review of emerging technologies for tackling COVID-19 pandemic. Hum Behav Emerg Technol. 2021, 3(1), 25–39. [Google Scholar] [CrossRef] [PubMed]
| Characteristic | Total (N=157) | DM (n=44) | Non-DM (n=113) | p-value |
|---|---|---|---|---|
| Demographics | ||||
| Age, years, Median | 57 (45, 68) | 61 (52, 70) | 55 (42,67) | 0.023 |
| Sex 0.264 | ||||
| Male, n (%) | 89 (56.7) | 28 (63.6) | 61(54.0) | |
| Female, n (%) | 68 (43.3) | 16 (36.4) | 52 (46.0) | |
| Preexisting condition, n (%) | ||||
| Hypertension | 88 (56.1) | 27 (61.4) | 61 (54.0) | 0.394 |
| Cardiovascular disease | 65 (41.4) | 25 (56.8) | 40 (35.4) | 0.013 |
| Chronic kidney disease | 28 (17.8) | 12 (27.3) | 16 (14.2) | 0.049 |
| Chronic lung disease | 15 (9.6) | 8 (18.2) | 7 (6.2) | 0.021 |
| Cancer | 10 (6.4) | 3 (6.8) | 7 (6.2) | 0.888 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




