Submitted:
25 January 2026
Posted:
26 January 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
Methods and Literature Search Strategy
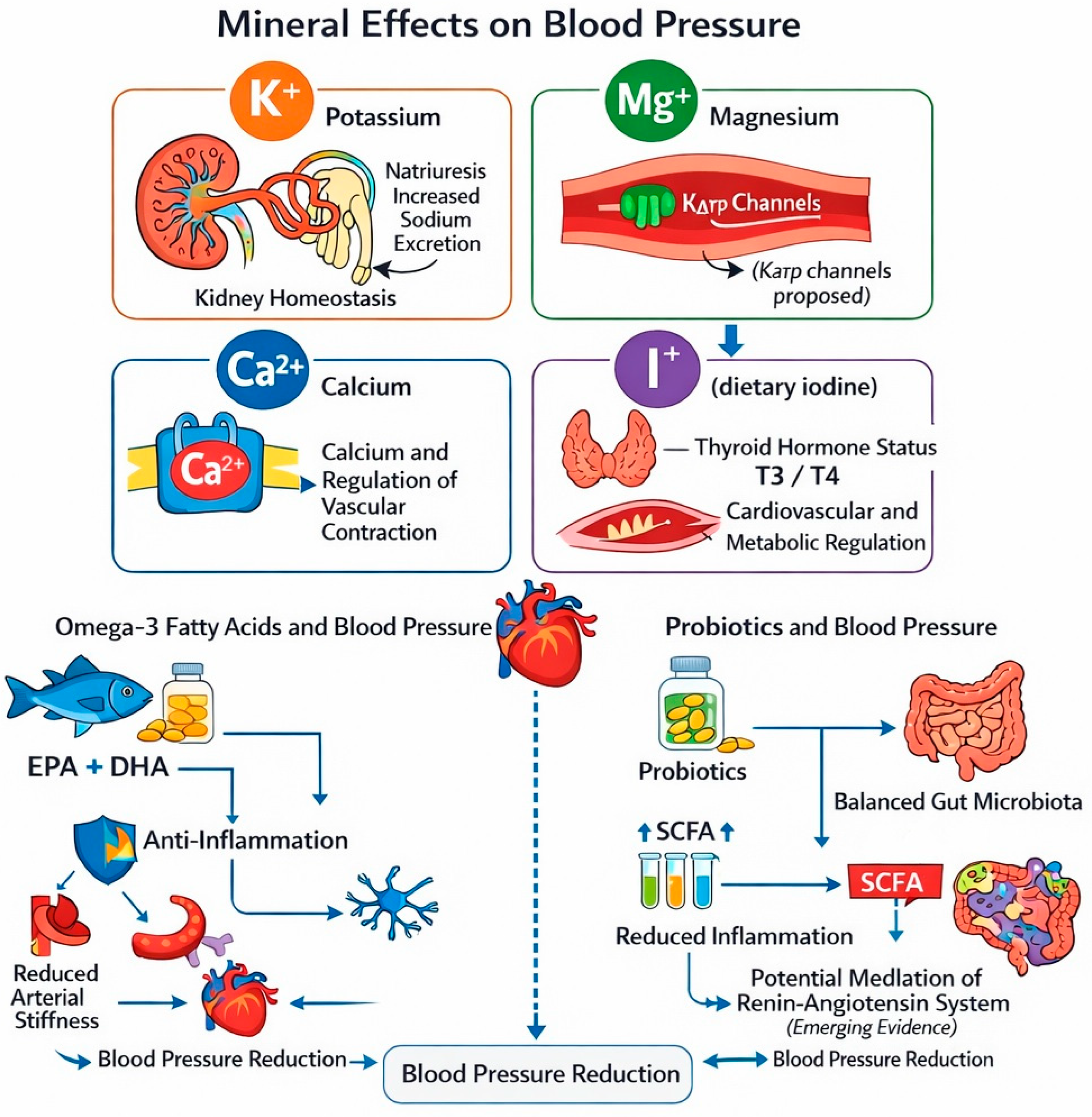
2. Essential Minerals and Blood Pressure Regulation
2.1. Potassium: A Central Dietary Determinant of Blood Pressure
2.2. Magnesium: A Physiological Calcium Antagonist
2.3. Calcium: The Dietary Calcium Paradox
2.4. Iodine: Thyroid-Mediated Blood Pressure Regulation
3. Polyphenols and Blood Pressure Regulation
3.1. General Mechanisms of Polyphenol Action in Blood Pressure Regulation
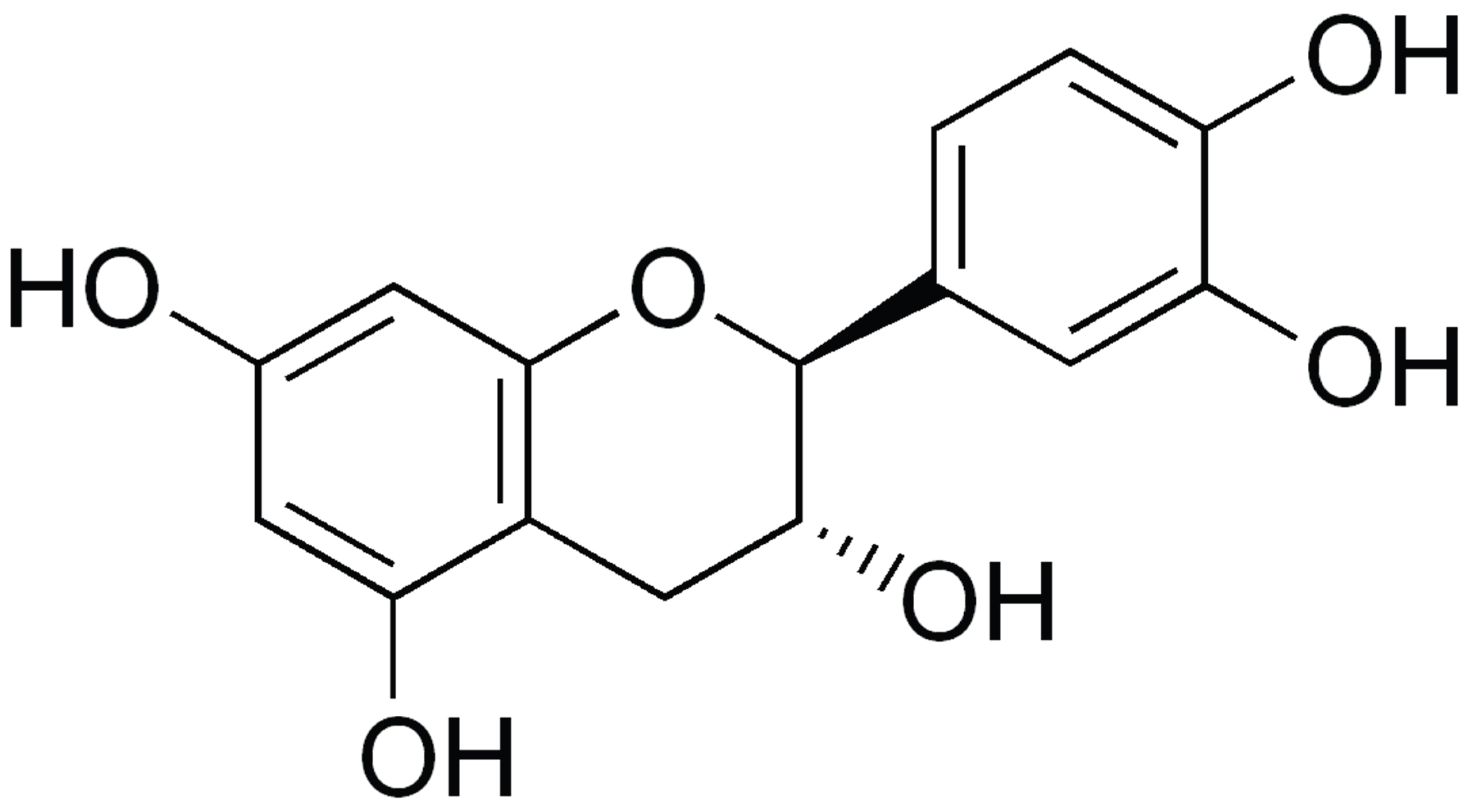
3.2. Cocoa and Flavanols
3.3. Tea Polyphenols: Green and Black Tea
3.4. Berries and Anthocyanins
4. Omega-3 Fatty Acids
4.1. Mechanisms Underlying the Antihypertensive Effects of Omega-3 Fatty Acids
4.2. Clinical Evidence for Blood Pressure Reduction
4.3. Safety, Dosage, and Clinical Considerations
5. Probiotics and the Gut–Vascular Axis
5.1. Gut Microbiota Dysbiosis and Hypertension
5.2. Mechanisms Linking Probiotics to Blood Pressure Regulation
5.3. Clinical Evidence for Probiotic Interventions
5.4. Limitations and Future Perspectives
6. Coenzyme Q10 and L-Arginine
6.1. Coenzyme Q10
6.2. L-Arginine
6.3. Summary
7. Nutrients Influencing Endothelial Function and the Renin–Angiotensin System (RAS)
7.1. Endothelial Function as a Target for Nutraceutical Intervention
7.2. Nutritional Modulation of the Renin–Angiotensin System
7.3. Integrated Effects on Vascular Remodeling and Blood Pressure
7.4. Clinical and Translational Implications
7.5. Summary
8. Conclusions
List of Abbreviations
| ACE | Angiotensin-converting enzyme |
| BP | Blood pressure |
| CoQ10 | Coenzyme Q10 |
| DASH | Dietary Approaches to Stop Hypertension |
| DHA | Docosahexaenoic acid |
| eNOS | Endothelial nitric oxide synthase |
| EPA | Eicosapentaenoic acid |
| NO | Nitric oxide |
| PUFA | Polyunsaturated fatty acid |
| RAAS | Renin–angiotensin–aldosterone system |
| RAS | Renin–angiotensin system |
| RCT | Randomized controlled trial |
| ROS | Reactive oxygen species |
| SCFA | Short-chain fatty acid |
| WHO | World Health Organization |
References
- World Health Organization. Global Report on Hypertension: The Race Against a Silent Killer; World Health Organization: Geneva, 2023; Available online: https://www.who.int/publications/i/item/9789240081062 (accessed on 14 December 2025).
- Burnier, M.; Egan, B.M. Adherence in hypertension. Circ. Res. 2019, 124, 1124–1140. [Google Scholar] [CrossRef]
- Williams, B.; Mancia, G.; Spiering, W.; et al. 2018 ESC/ESH Guidelines for the management of arterial hypertension. Eur. Heart J. 2018, 39, 3021–3104. [Google Scholar] [CrossRef] [PubMed]
- Whelton, P.K.; Carey, R.M.; Aronow, W.S.; et al. 2017 ACC/AHA Guideline for the Prevention, Detection, Evaluation, and Management of High Blood Pressure in Adults. Hypertension 2018, 71, e13–e115. [Google Scholar] [CrossRef]
- Kalra, E.K. Nutraceutical—Definition and introduction. AAPS PharmSci 2003, 5, 27–28. [Google Scholar] [CrossRef]
- Huang, L.; Trieu, K.; Yoshimura, S.; et al. Effect of nutraceuticals on blood pressure: A systematic review and meta-analysis. J. Clin. Hypertens. 2020, 22, 327–336. [Google Scholar] [CrossRef]
- He, F.J.; MacGregor, G.A. Dietary minerals and blood pressure. Curr. Opin. Nephrol. Hypertens. 2008, 17, 224–229. [Google Scholar]
- Aburto, N.J.; Hanson, S.; Gutierrez, H.; Hooper, L.; Elliott, P.; Cappuccio, F.P. Effect of increased potassium intake on cardiovascular risk factors and disease: Systematic review and meta-analyses. BMJ 2013, 346, f1378. [Google Scholar] [CrossRef]
- Houston, M.C. The role of magnesium in hypertension and cardiovascular disease. Journal of Clinical Hypertension 2011, 13(11), 843–847. [Google Scholar] [CrossRef]
- Weaver, C.M.; Heaney, R.P. Calcium in Human Health; Humana Press: Totowa, NJ, USA, 2006. [Google Scholar]
- Appel, L.J.; Moore, T.J.; Obarzanek, E.; et al. A clinical trial of the effects of dietary patterns on blood pressure (DASH). N. Engl. J. Med. 1997, 336, 1117–1124. [Google Scholar] [CrossRef]
- Mente, A.; O’Donnell, M.J.; Rangarajan, S.; et al. Association of urinary sodium and potassium excretion with blood pressure. N. Engl. J. Med. 2014, 371, 601–611. [Google Scholar] [CrossRef] [PubMed]
- Hall, J.E. The kidney, hypertension, and obesity. Hypertension 2003, 41, 625–633. [Google Scholar] [CrossRef]
- Haddy, F.J.; Vanhoutte, P.M.; Feletou, M. Role of potassium in regulating blood flow and blood pressure. Am. J. Physiol. Regul. Integr. Comp. Physiol. 2006, 290, R546–R552. [Google Scholar] [CrossRef] [PubMed]
- Filippini, T.; Violi, F.; D’Amico, R.; Vinceti, M. The effect of potassium supplementation on blood pressure in hypertensive and normotensive subjects: A systematic review and meta-analysis. Int. J. Cardiol. 2017, 230, 127–135. [Google Scholar] [CrossRef]
- Aaron, K.J.; Sanders, P.W. Role of dietary salt and potassium intake in cardiovascular health and disease: A review of the evidence. Mayo Clin. Proc. 2013, 88, 987–995. [Google Scholar] [CrossRef]
- Palmer, B.F.; Clegg, D.J. Physiology and pathophysiology of potassium homeostasis. Adv. Physiol. Educ. 2016, 40, 480–490. [Google Scholar] [CrossRef] [PubMed]
- de Baaij, J.H.F.; Hoenderop, J.G.J.; Bindels, R.J.M. Magnesium in man: Implications for health and disease. Physiol. Rev. 2015, 95, 1–46. [Google Scholar] [CrossRef]
- Rosanoff, A.; Weaver, C.M.; Rude, R.K. Suboptimal magnesium status in the United States: Are the health consequences underestimated? Nutr. Rev. 2012, 70, 153–164. [Google Scholar] [CrossRef]
- Del Gobbo, L.C.; Imamura, F.; Wu, J.H.Y.; et al. Circulating and dietary magnesium and risk of cardiovascular disease: A systematic review and meta-analysis. Am. J. Clin. Nutr. 2013, 98, 160–173. [Google Scholar] [CrossRef]
- Touyz, R.M. Role of magnesium in the pathogenesis of hypertension. Mol. Aspects Med. 2003, 24, 107–136. [Google Scholar] [CrossRef] [PubMed]
- Sontia, B.; Touyz, R.M. Role of magnesium in hypertension. Arch. Biochem. Biophys. 2007, 458, 33–39. [Google Scholar] [CrossRef]
- Altura, B.M.; Altura, B.T. Role of magnesium in patho-physiological processes and the clinical utility of magnesium ion selective electrodes. Scand. J. Clin. Lab. Invest. 1996, 56, 211–234. [Google Scholar] [CrossRef]
- Maier, J.A.M. Low magnesium and atherosclerosis: An evidence-based link. Mol. Aspects Med. 2003, 24, 137–146. [Google Scholar] [CrossRef]
- Dibaba, D.T.; Xun, P.; He, K. Dietary magnesium intake is inversely associated with serum C-reactive protein levels: Meta-analysis and systematic review. Eur. J. Clin. Nutr. 2014, 68, 510–516. [Google Scholar] [CrossRef]
- Zhang, X.; Li, Y.; Del Gobbo, L.C.; et al. Effects of magnesium supplementation on blood pressure: A meta-analysis of randomized controlled trials. Hypertension 2016, 68, 324–333. [Google Scholar] [CrossRef]
- Kass, L.; Weekes, J.; Carpenter, L. Effect of magnesium supplementation on blood pressure: A meta-analysis. Eur. J. Clin. Nutr. 2012, 66, 411–418. [Google Scholar] [CrossRef]
- Ranade, V.V.; Somberg, J.C. Bioavailability and pharmacokinetics of magnesium after administration of magnesium salts to humans. Am. J. Ther. 2001, 8, 345–357. [Google Scholar] [CrossRef] [PubMed]
- McCarron, D.A.; Morris, C.D.; Cole, C. Dietary calcium in human hypertension. Science 1982, 217, 267–269. [Google Scholar] [CrossRef] [PubMed]
- Blaustein, M.P.; Lederer, W.J. Sodium/calcium exchange: Its physiological implications. Physiol. Rev. 1999, 79, 763–854. [Google Scholar] [CrossRef]
- Resnick, L.M. Calcium metabolism in hypertension and allied metabolic disorders. Diabetes Care 1991, 14, 505–520. [Google Scholar] [CrossRef] [PubMed]
- Buchanan, J.R.; McCarron, D.A. Calcium metabolism and blood pressure. Journal of Clinical Endocrinology & Metabolism 1984, 59, 1129–1134. [Google Scholar] [CrossRef]
- van Mierlo, L.A.J.; Arends, L.R.; Streppel, M.T.; Zeegers, M.P.A.; Kok, F.J.; Grobbee, D.E. Blood pressure response to calcium supplementation: A meta-analysis of randomized controlled trials. J. Hum. Hypertens. 2006, 20, 571–580. [Google Scholar] [CrossRef]
- Bolland, M.J.; Grey, A.; Avenell, A.; Gamble, G.D.; Reid, I.R. Calcium supplements with or without vitamin D and risk of cardiovascular events. BMJ 2011, 342, d2040. [Google Scholar] [CrossRef]
- Dickinson, H.O.; Nicolson, D.J.; Cook, J.V.; et al. Calcium supplementation for the management of primary hypertension in adults. Cochrane Database Syst. Rev. 2006, CD004639. [Google Scholar] [CrossRef]
- Laurberg, P.; Cerqueira, C.; Ovesen, L.; et al. Iodine intake as a determinant of thyroid disorders in populations. Best Pract. Res. Clin. Endocrinol. Metab. 2010, 24, 13–27. [Google Scholar] [CrossRef]
- Danzi, S.; Klein, I. Thyroid hormone and the cardiovascular system. Med. Clin. N. Am. 2012, 96, 203–218. [Google Scholar] [CrossRef] [PubMed]
- Biondi, B.; Cooper, D.S. The clinical significance of subclinical thyroid dysfunction. Endocr. Rev. 2008, 29, 76–131. [Google Scholar] [CrossRef]
- Napoli, R.; Guardasole, V.; Angelini, V.; et al. Acute effects of triiodothyronine on endothelial function in human subjects. J. Clin. Endocrinol. Metab. 2007, 92, 250–254. [Google Scholar] [CrossRef] [PubMed]
- Taylor, P.N.; Albrecht, D.; Scholz, A.; et al. Global epidemiology of hyperthyroidism and hypothyroidism. Nat. Rev. Endocrinol. 2018, 14, 301–316. [Google Scholar] [CrossRef]
- Leung, A.M.; Braverman, L.E. Consequences of excess iodine. Nat. Rev. Endocrinol. 2014, 10, 136–142. [Google Scholar] [CrossRef] [PubMed]
- Zimmermann, M.B.; Boelaert, K. Iodine deficiency and thyroid disorders. Lancet Diabetes Endocrinol. 2015, 3, 286–295. [Google Scholar] [CrossRef]
- Manach, C.; Scalbert, A.; Morand, C.; Rémésy, C.; Jiménez, L. Polyphenols: Food sources and bioavailability. Am. J. Clin. Nutr. 2004, 79, 727–747. [Google Scholar] [CrossRef]
- Del Rio, D.; Rodriguez-Mateos, A.; Spencer, J.P.E.; Tognolini, M.; Borges, G.; Crozier, A. Dietary polyphenolics in human health: Structures, bioavailability, and evidence of protective effects. Antioxid. Redox Signal. 2013, 18, 1818–1892. [Google Scholar] [CrossRef]
- Schroeter, H.; Heiss, C.; Balzer, J.; et al. (–)-Epicatechin mediates beneficial effects of flavanol-rich cocoa on vascular function. Proc. Natl. Acad. Sci. USA 2006, 103, 1024–1029. [Google Scholar] [CrossRef] [PubMed]
- Heiss, C.; Kleinbongard, P.; Dejam, A.; et al. Acute consumption of flavanol-rich cocoa improves endothelial function. J. Am. Coll. Cardiol. 2005, 46, 1277–1283. [Google Scholar] [CrossRef] [PubMed]
- Halliwell, B. Dietary polyphenols: Good, bad, or indifferent for your health? Cardiovasc. Res. 2007, 73, 341–347. [Google Scholar] [CrossRef]
- Förstermann, U.; Xia, N.; Li, H. Roles of vascular oxidative stress and nitric oxide in the pathogenesis of atherosclerosis. Circ. Res. 2017, 120, 713–735. [Google Scholar] [CrossRef]
- González-Gallego, J.; García-Mediavilla, M.V.; Sánchez-Campos, S.; Tuñón, M.J. Fruit polyphenols, immunity and inflammation. Br. J. Nutr. 2010, 104, S15–S27. [Google Scholar] [CrossRef] [PubMed]
- Actis-Goretta, L.; Ottaviani, J.I.; Fraga, C.G. Inhibition of angiotensin-converting enzyme activity by flavanol-rich foods. J. Agric. Food Chem. 2006, 54, 229–234. [Google Scholar] [CrossRef]
- Williamson, G.; Clifford, M.N. Role of the small intestine, colon and microbiota in determining the metabolic fate of polyphenols. Biochem. Pharmacol. 2017, 139, 24–39. [Google Scholar] [CrossRef]
- Katz, D.L.; Doughty, K.; Ali, A. Cocoa and chocolate in human health and disease. Antioxid. Redox Signal. 2011, 15, 2779–2811. [Google Scholar] [CrossRef]
- Fraga, C.G.; Oteiza, P.I. Dietary flavonoids: Role of (–)-epicatechin and related procyanidins in cardiovascular health. Free Radic. Biol. Med. 2011, 51, 813–823. [Google Scholar] [CrossRef]
- Heiss, C.; Dejam, A.; Kleinbongard, P.; et al. Vascular effects of cocoa rich in flavan-3-ols. JAMA 2003, 290, 1030–1031. [Google Scholar] [CrossRef]
- Grassi, D.; Desideri, G.; Necozione, S.; et al. Blood pressure is reduced and insulin sensitivity increased by dark chocolate. Hypertension 2005, 46, 398–405. [Google Scholar] [CrossRef]
- Vlachopoulos, C.; Aznaouridis, K.; Alexopoulos, N.; et al. Effect of dark chocolate on arterial stiffness. Am. J. Hypertens. 2005, 18, 785–791. [Google Scholar] [CrossRef] [PubMed]
- Ried, K.; Fakler, P.; Stocks, N.P. Effect of cocoa on blood pressure. BMC Med. 2009, 7, 22. [Google Scholar] [CrossRef]
- Hooper, L.; Kay, C.; Abdelhamid, A.; et al. Effects of chocolate, cocoa, and flavan-3-ols on cardiovascular health. Am. J. Clin. Nutr. 2012, 95, 740–751. [Google Scholar] [CrossRef] [PubMed]
- Ried, K.; Sullivan, T.; Fakler, P.; Frank, O.R.; Stocks, N.P. Does chocolate reduce blood pressure? BMC Med. 2010, 8, 39. [Google Scholar] [CrossRef] [PubMed]
- Cooper, K.A.; Donovan, J.L.; Waterhouse, A.L.; Williamson, G. Cocoa and health: A decade of research. Br. J. Nutr. 2008, 99, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Cabrera, C.; Artacho, R.; Giménez, R. Beneficial effects of green tea: A review. J. Am. Coll. Nutr. 2006, 25, 79–99. [Google Scholar] [CrossRef]
- Deka, A.; Vita, J.A. Tea and cardiovascular disease. Pharmacol. Res. 2011, 64, 136–145. [Google Scholar] [CrossRef]
- Lorenz, M.; Urban, J.; Engelhardt, U.; Baumann, G.; Stangl, K.; Stangl, V. Green tea polyphenols and cardiovascular protection. Eur. Heart J. 2009, 30, 2024–2032. [Google Scholar] [CrossRef]
- Kim, W.; Jeong, M.H.; Cho, S.H.; et al. Effect of green tea catechins on endothelial function. Circ. J. 2006, 70, 153–159. [Google Scholar] [CrossRef]
- Hodgson, J.M.; Croft, K.D. Tea flavonoids and cardiovascular health. Mol. Aspects Med. 2010, 31, 495–502. [Google Scholar] [CrossRef] [PubMed]
- Yang, Y.; Lu, F.; Wu, J.S.; Wu, C.H.; Chang, C.J. The protective effect of habitual tea consumption on hypertension. Arch. Intern. Med. 2004, 164, 1534–1540. [Google Scholar] [CrossRef]
- Liu, G.; Mi, X.; Zheng, X.; et al. Effects of tea intake on blood pressure: A meta-analysis. Br. J. Nutr. 2014, 112, 1043–1054. [Google Scholar] [CrossRef]
- He, J.; Giusti, M.M. Anthocyanins: Natural colorants with health-promoting properties. Annu. Rev. Food Sci. Technol. 2010, 1, 163–187. [Google Scholar] [CrossRef] [PubMed]
- Wallace, T.C. Anthocyanins in cardiovascular disease. Adv. Nutr. 2011, 2, 1–7. [Google Scholar] [CrossRef]
- Khan, F.; Ray, S.; Craigie, A.M.; et al. Lowering of blood pressure by berry-derived polyphenols. Am. J. Clin. Nutr. 2014, 100, 1385–1393. [Google Scholar] [CrossRef]
- Rodriguez-Mateos, A.; Del Pino-García, R.; George, T.W.; et al. Impact of anthocyanins on vascular function. Am. J. Clin. Nutr. 2014, 99, 1280–1290. [Google Scholar] [CrossRef]
- Curtis, P.J.; van der Velpen, V.; Berends, L.; et al. Blueberry anthocyanins improve vascular function. Am. J. Clin. Nutr. 2019, 109, 1535–1545. [Google Scholar] [CrossRef]
- Huang, H.; Chen, G.; Liao, D.; Zhu, Y.; Xue, X. Effects of anthocyanin supplementation on blood pressure: A meta-analysis. Nutrients 2016, 8, 198. [Google Scholar] [CrossRef]
- Calder, P.C. Omega-3 fatty acids and cardiovascular disease: Evidence explained and mechanisms explored. Clin. Sci. 2004, 107, 1–11. [Google Scholar] [CrossRef]
- Mozaffarian, D.; Wu, J.H.Y. Omega-3 fatty acids and cardiovascular disease: Effects on risk factors, molecular pathways, and clinical events. J. Am. Coll. Cardiol. 2011, 58, 2047–2067. [Google Scholar] [CrossRef]
- Harris, W.S.; Miller, M.; Tighe, A.P.; Davidson, M.H.; Schaefer, E.J. Omega-3 fatty acids and coronary heart disease risk. J. Cardiovasc. Risk 2008, 15, 4–11. [Google Scholar] [CrossRef]
- Dangardt, F.; Chen, Y.; Gronowitz, E.; Dahlgren, J.; Friberg, P.; Strandvik, B. High physiological omega-3 fatty acid supplementation affects endothelial function. 78. Circulation 2010, 121, 252–258. [Google Scholar] [CrossRef]
- Harris, W.S.; Miller, M. Omega-3 fatty acids and cardiovascular disease: New developments and applications. Postgraduate Medicine 2012, 124, 100–113. [Google Scholar] [CrossRef]
- Serhan, C.N.; Chiang, N.; Van Dyke, T.E. Resolving inflammation: Dual anti-inflammatory and pro-resolution lipid mediators. Nat. Rev. Immunol. 2008, 8, 349–361. [Google Scholar] [CrossRef]
- Calder, P.C. Omega-3 fatty acids and inflammatory processes. Nutrients 2010, 2, 355–374. [Google Scholar] [CrossRef] [PubMed]
- Yates, C.M.; Calder, P.C.; Ed Rainger, G. Pharmacology and therapeutics of omega-3 polyunsaturated fatty acids in chronic inflammatory disease. Pharmacol. Ther. 2014, 141, 272–282. [Google Scholar] [CrossRef]
- Nestel, P.J.; Shige, H.; Pomeroy, S.; et al. The n−3 fatty acids eicosapentaenoic acid and docosahexaenoic acid increase arterial compliance. Am. J. Clin. Nutr. 2002, 76, 326–330. [Google Scholar] [CrossRef]
- Mori, T.A.; Bao, D.Q.; Burke, V.; et al. Differential effects of omega-3 fatty acids on blood pressure. Hypertension 1999, 34, 253–260. [Google Scholar] [CrossRef] [PubMed]
- Geleijnse, J.M.; Giltay, E.J.; Grobbee, D.E.; Donders, A.R.T.; Kok, F.J. Blood pressure response to fish oil supplementation. J. Hypertens. 2002, 20, 1493–1499. [Google Scholar] [CrossRef]
- Knapp, H.R.; FitzGerald, G.A. The antihypertensive effects of fish oil. N. Engl. J. Med. 1989, 320, 1037–1043. [Google Scholar] [CrossRef]
- Miller, P.E.; Van Elswyk, M.; Alexander, D.D. Long-chain omega-3 fatty acids eicosapentaenoic acid and docosahexaenoic acid and blood pressure. Am. J. Hypertens. 2014, 27, 885–896. [Google Scholar] [CrossRef]
- Zhang, X.; Ritonja, J.A.; Zhou, N.; et al. Omega-3 fatty acids and blood pressure: A meta-analysis of randomized controlled trials. J. Am. Heart Assoc. 2022, 11, e025070. [Google Scholar] [CrossRef]
- Mori, T.A.; Woodman, R.J. The independent effects of EPA and DHA on cardiovascular risk factors. J. Nutr. 2006, 136, 300S–304S. [Google Scholar] [CrossRef]
- Mozaffarian, D.; Lemaitre, R.N.; Kuller, L.H.; et al. Cardiac benefits of fish consumption. Circulation 2003, 107, 1372–1377. [Google Scholar] [CrossRef]
- Burdge, G.C.; Calder, P.C. Conversion of α-linolenic acid to longer-chain polyunsaturated fatty acids in humans. Reprod. Nutr. Dev. 2005, 45, 581–597. [Google Scholar] [CrossRef]
- Kris-Etherton, P.M.; Harris, W.S.; Appel, L.J. Fish consumption, fish oil, omega-3 fatty acids, and cardiovascular disease. Circulation 2002, 106, 2747–2757. [Google Scholar] [CrossRef]
- Skulas-Ray, A.C.; Wilson, P.W.F.; Harris, W.S.; et al. Omega-3 fatty acids for the management of hypertension. Circulation 2019, 140, e673–e691. [Google Scholar] [CrossRef] [PubMed]
- Gomes, A.C.; Hoffmann, C.; Mota, J.F. The human gut microbiota: Metabolism and perspective in obesity. Gut Microbes 2018, 9, 308–325. [Google Scholar] [CrossRef]
- Tilg, H.; Zmora, N.; Adolph, T.E.; Elinav, E. The intestinal microbiota fuelling metabolic inflammation. Nat. Rev. Immunol. 2020, 20, 40–54. [Google Scholar] [CrossRef] [PubMed]
- Ahtesh, F.B.; Stojanovska, L.; Apostolopoulos, V. Anti-hypertensive peptides derived from milk proteins. Nutrients 2018, 10, 1779. [Google Scholar] [CrossRef]
- Joyce, S.A.; Gahan, C.G.M. Bile acid modifications at the microbe–host interface. Gut Microbes 2016, 7, 381–392. [Google Scholar] [CrossRef]
- Khalesi, S.; Sun, J.; Buys, N.; Jayasinghe, R. Effect of probiotics on blood pressure: A systematic review and meta-analysis. Hypertension 2014, 64, 897–903. [Google Scholar] [CrossRef]
- Qi, D.; Nie, X.; Sun, J.; et al. Probiotics supplementation improves blood pressure: A meta-analysis. Lipids Health Dis. 2020, 19, 146. [Google Scholar] [CrossRef]
- Khalesi, S.; Bellissimo, N.; Vandelanotte, C.; Williams, S.; Stanley, D.; Irwin, C. A review of probiotic supplementation in blood pressure regulation. Nutrients 2019, 11, 2539. [Google Scholar] [CrossRef]
- O’Toole, P.W.; Marchesi, J.R.; Hill, C. Next-generation probiotics: From probiotics to live biotherapeutics. Nat. Microbiol. 2017, 2, 17057. [Google Scholar] [CrossRef]
- Didari, T.; Solki, S.; Mozaffari, S.; Nikfar, S.; Abdollahi, M. A systematic review of the safety of probiotics. Expert Opin. Drug Saf. 2014, 13, 227–239. [Google Scholar] [CrossRef]
- Zmora, N.; Suez, J.; Elinav, E. Diet, health, and the gut microbiota. Nat. Rev. Gastroenterol. Hepatol. 2019, 16, 35–56. [Google Scholar] [CrossRef]
- Tiano, L.; Belardinelli, R.; Carnevali, P.; et al. Effect of coenzyme Q10 administration on endothelial function and inflammatory markers. Mol. Aspects Med. 2007, 28, 168–176. [Google Scholar] [CrossRef]
- Böger, R.H. The pharmacodynamics of L-arginine. J. Nutr. 2007, 137, 1650S–1655S. [Google Scholar] [CrossRef] [PubMed]
- Crane, F.L. Biochemical functions of coenzyme Q10. J. Am. Coll. Nutr. 2001, 20, 591–598. [Google Scholar] [CrossRef]
- Langsjoen, P.H.; Langsjoen, A.M. The clinical use of HMG-CoA reductase inhibitors and the associated depletion of coenzyme Q10. J. Am. Coll. Cardiol. 2003, 41, 122–124. [Google Scholar] [CrossRef]
- Ernster, L.; Dallner, G. Biochemical, physiological and medical aspects of ubiquinone function. Biochim. Biophys. Acta 1995, 1271, 195–204. [Google Scholar] [CrossRef]
- Littarru, G.P.; Tiano, L. Bioenergetic and antioxidant properties of coenzyme Q10. Mol. Aspects Med. 2007, 28, 137–148. [Google Scholar] [CrossRef]
- Zhao, D.; et al. Dose-response effect of Coenzyme Q10 supplementation on blood pressure in patients with cardiometabolic diseases: A meta-analysis. Nutrition, Metabolism & Cardiovascular Diseases. This study reported modest but significant reductions in systolic BP with higher circulating CoQ10 following supplementation 2022.
- Hodgson, J.M.; et al. Coenzyme Q10 improves blood pressure and endothelial function. Am. J. Hypertens. 2002, 15, 686–690. [Google Scholar] [CrossRef]
- Singh, R.B.; et al. Effect of coenzyme Q10 on risk of atherosclerosis in patients with hypertension. Mol. Cell. Biochem. 1999, 196, 179–187. [Google Scholar] [CrossRef]
- Rosenfeldt, F.L.; et al. Coenzyme Q10 in the treatment of hypertension: A meta-analysis. J. Hum. Hypertens. 2007, 21, 297–306. [Google Scholar] [CrossRef] [PubMed]
- Ho, M.J.; Bellusci, M.; Wright, J.M. Blood pressure lowering efficacy of coenzyme Q10. Cochrane Database Syst. Rev. 2009, CD007435. [Google Scholar] [CrossRef]
- Hidaka, T.; et al. Safety assessment of coenzyme Q10. Biofactors 2008, 32, 199–208. [Google Scholar] [CrossRef]
- Bhagavan, H.N.; Chopra, R.K. Coenzyme Q10 pharmacokinetics. Free Radic. Res. 2006, 40, 445–453. [Google Scholar] [CrossRef] [PubMed]
- Garrido-Maraver, J.; et al. Coenzyme Q10 therapy. Mol. Syndromol. 2014, 5, 187–197. [Google Scholar] [CrossRef]
- Karimi, M.; Rahmani, J.; Varkaneh, H.K.; Clark, C.C.T.; Salehi-Sahlabadi, A.; Day, A.S.; Mirmiran, P.; Hekmatdoost, A. Effects of coenzyme Q10 supplementation on blood pressure: A systematic review and meta-analysis of randomized controlled trials. Int. J. Cardiol. Cardiovasc. Risk Prev. 2025, 24, 100301. [Google Scholar] [CrossRef]
- Gambardella, J.; et al. Arginine and endothelial function. Biomedicines 2020, 8, 277. [Google Scholar] [CrossRef]
- McRae, M.P. Therapeutic benefits of L-arginine: Umbrella review. J. Chiropr. Med. 2016, 15, 184–189. [Google Scholar] [CrossRef]
- Dong, J.Y.; et al. Effect of oral L-arginine on blood pressure. Am. Heart J. 2011, 162, 959–965. [Google Scholar] [CrossRef]
- Shiraseb, F.; et al. Dose–response meta-analysis of L-arginine and blood pressure. Adv. Nutr. 2022, 13, 1226–1242. [Google Scholar] [CrossRef] [PubMed]
- Grimble, G.K. Adverse gastrointestinal effects of arginine. J. Nutr. 2007, 137, 1693S–1701S. [Google Scholar] [CrossRef]
- Allerton, T.D.; et al. L-citrulline supplementation and cardiometabolic health. Nutrients 2018, 10, 921. [Google Scholar] [CrossRef]
- Vanhoutte, P.M.; Shimokawa, H.; Tang, E.H.C.; Feletou, M. Endothelial dysfunction and vascular disease. Acta Physiol. 2009, 196, 193–222. [Google Scholar] [CrossRef]
- Atlas, S.A. The renin–angiotensin aldosterone system: Pathophysiological role and pharmacologic inhibition. J. Manag. Care Pharm. 2007, 13, S9–S20. [Google Scholar] [CrossRef] [PubMed]
- Lüscher, T.F.; Barton, M. Biology of the endothelium. Clin. Cardiol. 1997, 20, II-3–II-10. [Google Scholar] [CrossRef]
- Förstermann, U.; Sessa, W.C. Nitric oxide synthases: Regulation and function. Eur. Heart J. 2012, 33, 829–837. [Google Scholar] [CrossRef]
- Higashi, Y.; Noma, K.; Yoshizumi, M.; Kihara, Y. Endothelial function and oxidative stress in cardiovascular diseases. Circ. J. 2009, 73, 411–418. [Google Scholar] [CrossRef] [PubMed]
- Heiss, C.; Keen, C.L.; Kelm, M. Flavanols and cardiovascular health. J. Cardiovasc. Pharmacol. 2010, 56, 2–6. [Google Scholar] [CrossRef]
- Mori, T.A. Dietary omega-3 fatty acids, endothelial function, and cardiovascular risk. Lipids 2014, 49, 301–309. [Google Scholar] [CrossRef]
- Vanhoutte, P.M.; Shimokawa, H.; Feletou, M.; Tang, E.H.C. Endothelial dysfunction and vascular disease. Acta Physiol. 2017, 219, 22–35. [Google Scholar] [CrossRef]
- Tousoulis, D.; Kampoli, A.M.; Tentolouris, C.; Papageorgiou, N.; Stefanadis, C. The role of nitric oxide on endothelial function. Curr. Vasc. Pharmacol. 2012, 10, 4–18. [Google Scholar] [CrossRef]
- Zuchi, C. Nutraceuticals and endothelial function: clinical evidence and cardiovascular implications. Clin. Cardiol. 2010, 33, 375–384. [Google Scholar] [CrossRef]
- Gimbrone, M.A.; García-Cardeña, G. Endothelial cell dysfunction and the pathobiology of atherosclerosis. Circ. Res. 2016, 118, 620–636. [Google Scholar] [CrossRef]
- Carey, R.M.; Padia, S.H. Role of the renin–angiotensin–aldosterone system in hypertension. Circ. Res. 2008, 102, 127–137. [Google Scholar] [CrossRef]
- He, F.J.; MacGregor, G.A. Beneficial effects of potassium on human health. Physiol. Plant. 2008, 133, 725–735. [Google Scholar] [CrossRef]
- Touyz, R.M.; Campbell, N.; Logan, A.; Gledhill, N.; Petrella, R. The role of magnesium in hypertension. J. Clin. Hypertens. 2018, 20, 150–159. [Google Scholar] [CrossRef]
- Burnier, M.; Egan, B.M. Adherence in hypertension. Circ. Res. 2019, 124, 1124–1140. [Google Scholar] [CrossRef]
- Kris-Etherton, P.M.; Petersen, K.S.; Hibbeln, J.R.; et al. Nutrition and behavioral health disorders: Depression and anxiety. Nutrients 2021, 13, 213. [Google Scholar] [CrossRef] [PubMed]
- Whelton, P.K.; Carey, R.M.; Aronow, W.S.; et al. 2017 ACC/AHA guideline for the prevention, detection, evaluation, and management of high blood pressure in adults. Hypertension 2018, 71, e13–e115. [Google Scholar] [CrossRef] [PubMed]
- Schiffrin, E.L. Vascular remodeling in hypertension: Mechanisms and treatment. Hypertension 2012, 59, 367–374. [Google Scholar] [CrossRef] [PubMed]
- Montezano, A.C.; Touyz, R.M. Reactive oxygen species, vascular Noxs, and hypertension: Focus on translational and clinical research. Antioxid. Redox Signal. 2014, 20, 164–182. [Google Scholar] [CrossRef]
- Appel, L.J.; Moore, T.J.; Obarzanek, E.; et al. A clinical trial of the effects of dietary patterns on blood pressure. N. Engl. J. Med. 1997, 336, 1117–1124. [Google Scholar] [CrossRef] [PubMed]
- Estruch, R.; Ros, E.; Salas-Salvadó, J.; et al. Primary prevention of cardiovascular disease with a Mediterranean diet. N. Engl. J. Med. 2018, 378, e34. [Google Scholar] [CrossRef] [PubMed]
- Gimbrone, M.A.; García-Cardeña, G. Endothelial cell dysfunction and the pathobiology of atherosclerosis. Circ. Res. 2016, 118, 620–636. [Google Scholar] [CrossRef]
- Ordovás, J.M.; Ferguson, L.R.; Tai, E.S.; Mathers, J.C. Personalized nutrition and health. BMJ 2018, 361, k2173. [Google Scholar] [CrossRef]
- Zeevi, D.; Korem, T.; Zmora, N.; et al. Personalized nutrition by prediction of glycemic responses. Cell 2015, 163, 1079–1094. [Google Scholar] [CrossRef] [PubMed]
| Nutraceutical category | Key compounds / examples | Main mechanisms relevant to blood pressure | Evidence from human studies | Typical effect on blood pressure | Key clinical considerations |
| Essential minerals | Potassium | Increased natriuresis, reduced sodium retention, vascular smooth muscle hyperpolarization, partial RAAS suppression | Strong evidence (RCTs, meta-analyses) | ↓ SBP ~3–5 mmHg; ↓ DBP ~2–3 mmHg | Avoid supplementation in advanced CKD or with potassium-sparing diuretics |
| Magnesium | Calcium antagonism, improved endothelial function, reduced oxidative stress and inflammation | Moderate–strong evidence | ↓ SBP ~2–4 mmHg | Organic salts show better bioavailability; high doses may cause GI effects | |
| Calcium | Modulation of parathyroid hormone and RAAS activity | Moderate evidence (dietary intake strongest) | ↓ SBP ~2–3 mmHg | Prefer dietary sources; caution with high-dose supplements | |
| Iodine | Indirect effects via thyroid hormone regulation | Epidemiological evidence | Indirect / variable | Both deficiency and excess may adversely affect BP | |
| Polyphenols | Cocoa flavanols (epicatechin) | Increased eNOS activity, improved nitric oxide bioavailability, reduced arterial stiffness | Strong evidence | ↓ SBP ~3–5 mmHg | Effects depend on flavanol content; sugar-rich products not recommended |
| Tea polyphenols (catechins, theaflavins) | Improved endothelial function, reduced oxidative stress | Moderate evidence | ↓ SBP ~2–3 mmHg | Benefits accumulate with habitual intake | |
| Berry anthocyanins | Improved endothelial function, reduced inflammation and arterial stiffness | Moderate evidence | ↓ SBP ~2–4 mmHg | Whole berries preferred over isolated supplements | |
| Omega-3 fatty acids | EPA, DHA | Improved endothelial function, anti-inflammatory effects, reduced arterial stiffness, lower sympathetic activity | Strong evidence | ↓ SBP ~4–5 mmHg; ↓ DBP ~2–3 mmHg | DHA may be more potent; caution at high doses in bleeding risk |
| Probiotics | Lactobacillus, Bifidobacterium spp. | SCFA production, reduced inflammation, ACE inhibition, improved gut barrier integrity | Emerging–moderate evidence | ↓ SBP ~2–4 mmHg | Effects depend on strain, dose, and duration |
| Bioactive compounds | Coenzyme Q10 | Reduced oxidative stress, improved mitochondrial and endothelial function | Moderate evidence | ↓ SBP ~5–17 mmHg | Generally well tolerated; formulation affects bioavailability |
| L-Arginine | Substrate for nitric oxide synthesis, improved endothelium-dependent vasodilation | Moderate evidence | ↓ SBP ~4–5 mmHg | Limited long-term data; caution in severe cardiovascular disease |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




