Submitted:
19 January 2026
Posted:
21 January 2026
You are already at the latest version
Abstract
Keywords:
1. Background
2. Aims of the Study
- To record any delays faced by newly diagnosed IBD patients at our centre
- If so, to understand the various points at which there are delays and identify bottlenecks
- To understand the factors leading to delays i.e., patient-related factors, community-related factors, or hospital-related factors
- To understand if the clinical outcomes were worse in patients who faced a delay compared to those who did not.
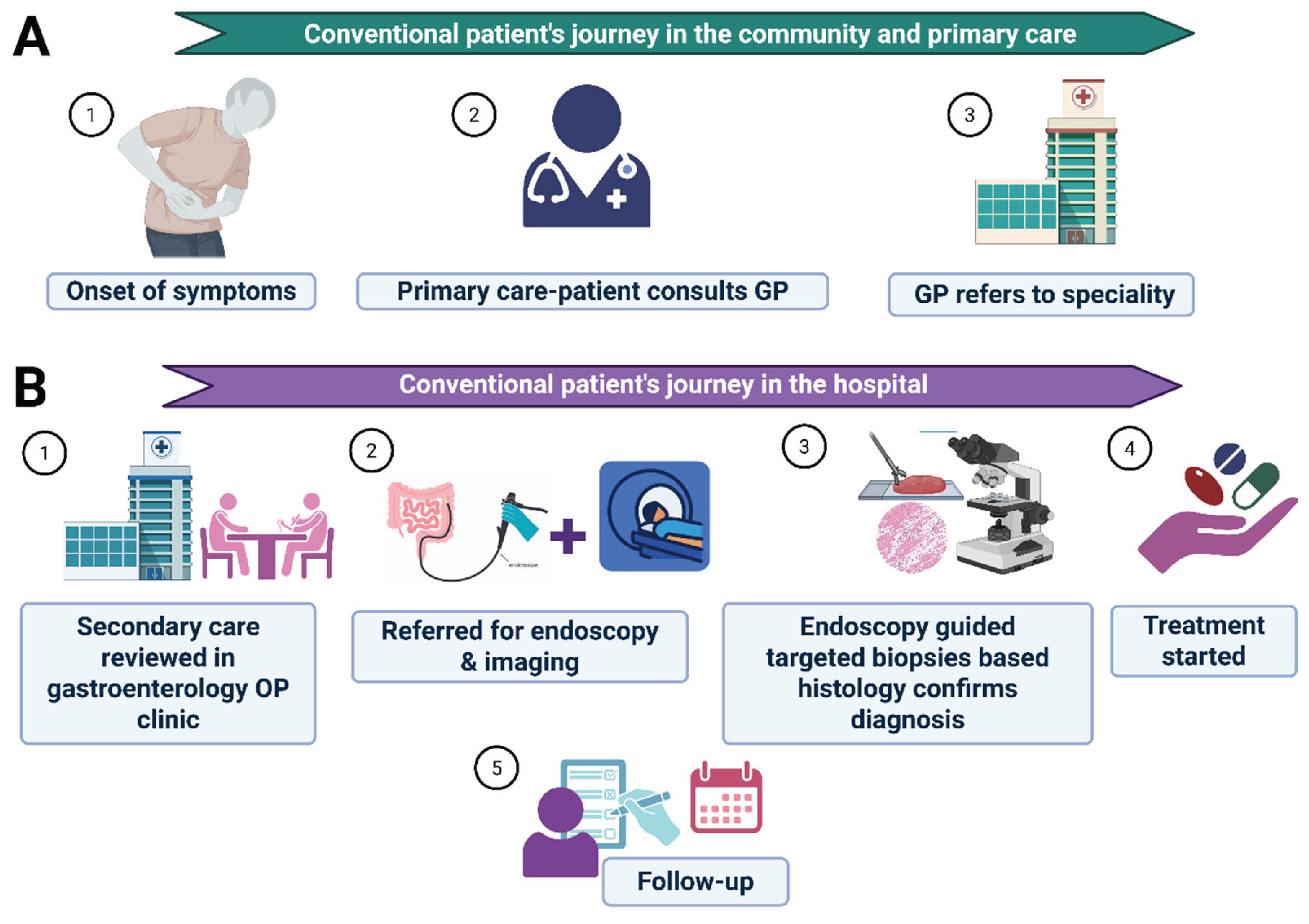
3. Patients and Methods
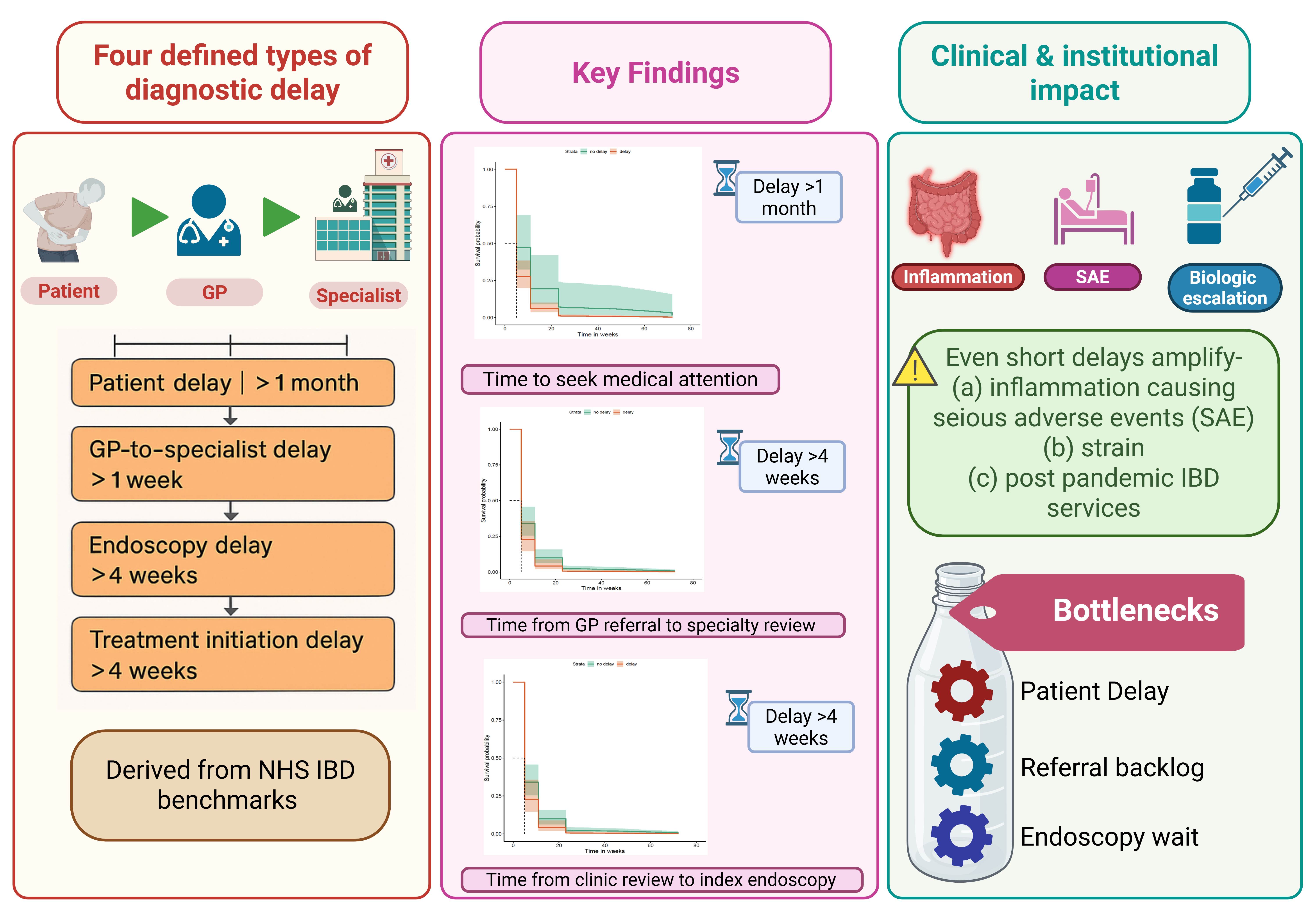
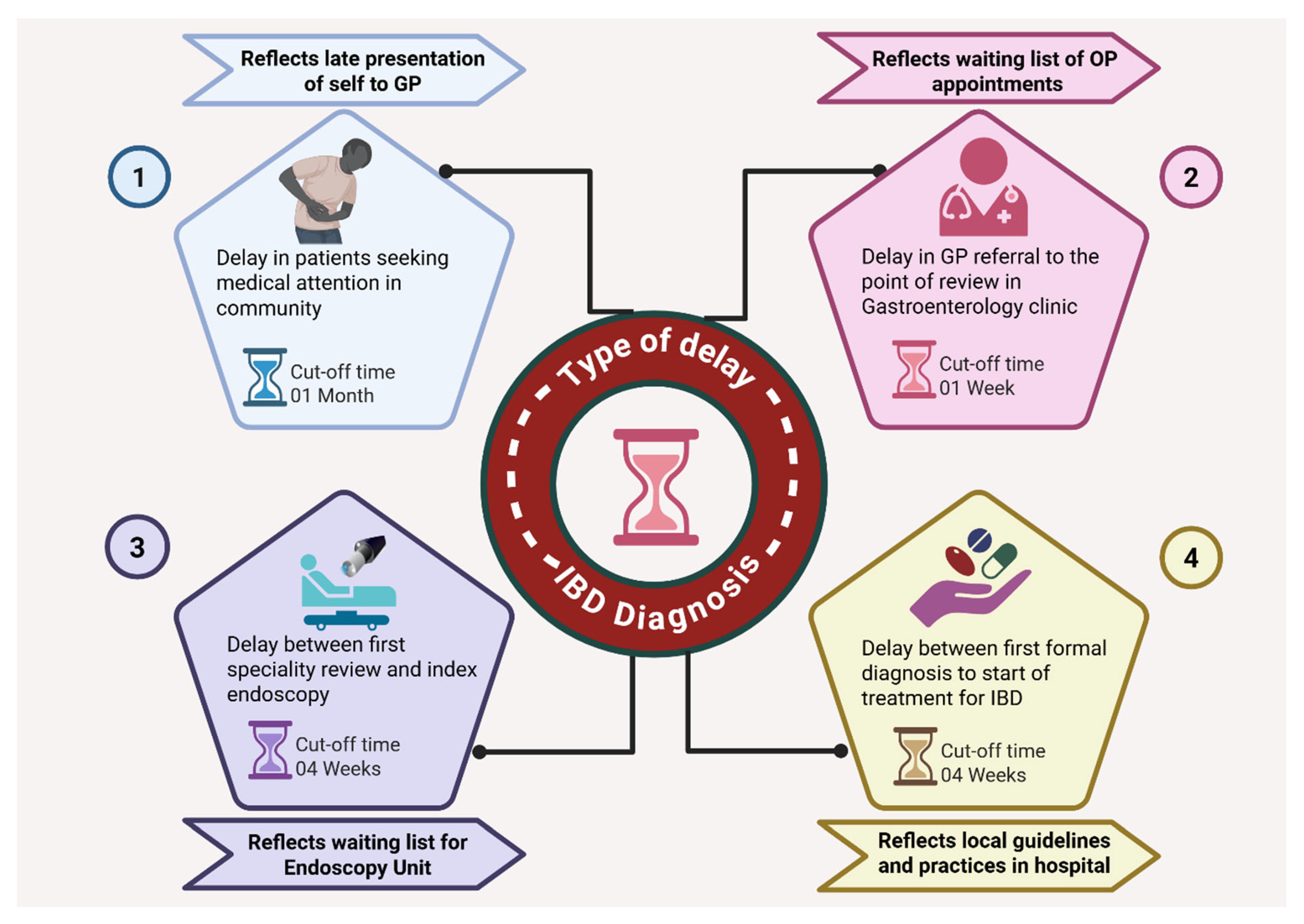
| Type of delay | Cut-off time |
|---|---|
|
Delay in patients seeking medical attention in community (Reflects late self-presentation to GP) |
1 month |
|
Delay in GP referral to the point of review in Gastroenterology clinic (Reflects waiting list for outpatient appointments in hospital) |
1 week |
|
Delay between first specialty review and index endoscopy (Reflects waiting list for endoscopy) |
4 weeks |
|
Delay between first formal diagnosis to start of treatment for IBD (Reflects local guidelines and practices in hospital) |
4 weeks |
3.1. Statistical Analysis
3.2. Ethical Considerations
4. Results
- -
- Delay in patients seeking medical attention (median= 4 months; range 1 to 84 months)
- -
- Delay between GP referral to Gastroenterology clinic appointment (median=5 weeks; range 1 to 30 weeks)
- -
- Delay between first specialty review and index endoscopy (median=3 weeks; 1 to 36 weeks)
- -
- Delay between first formal diagnosis to start of treatment for IBD (median=2 weeks; range 0 to 12 weeks)
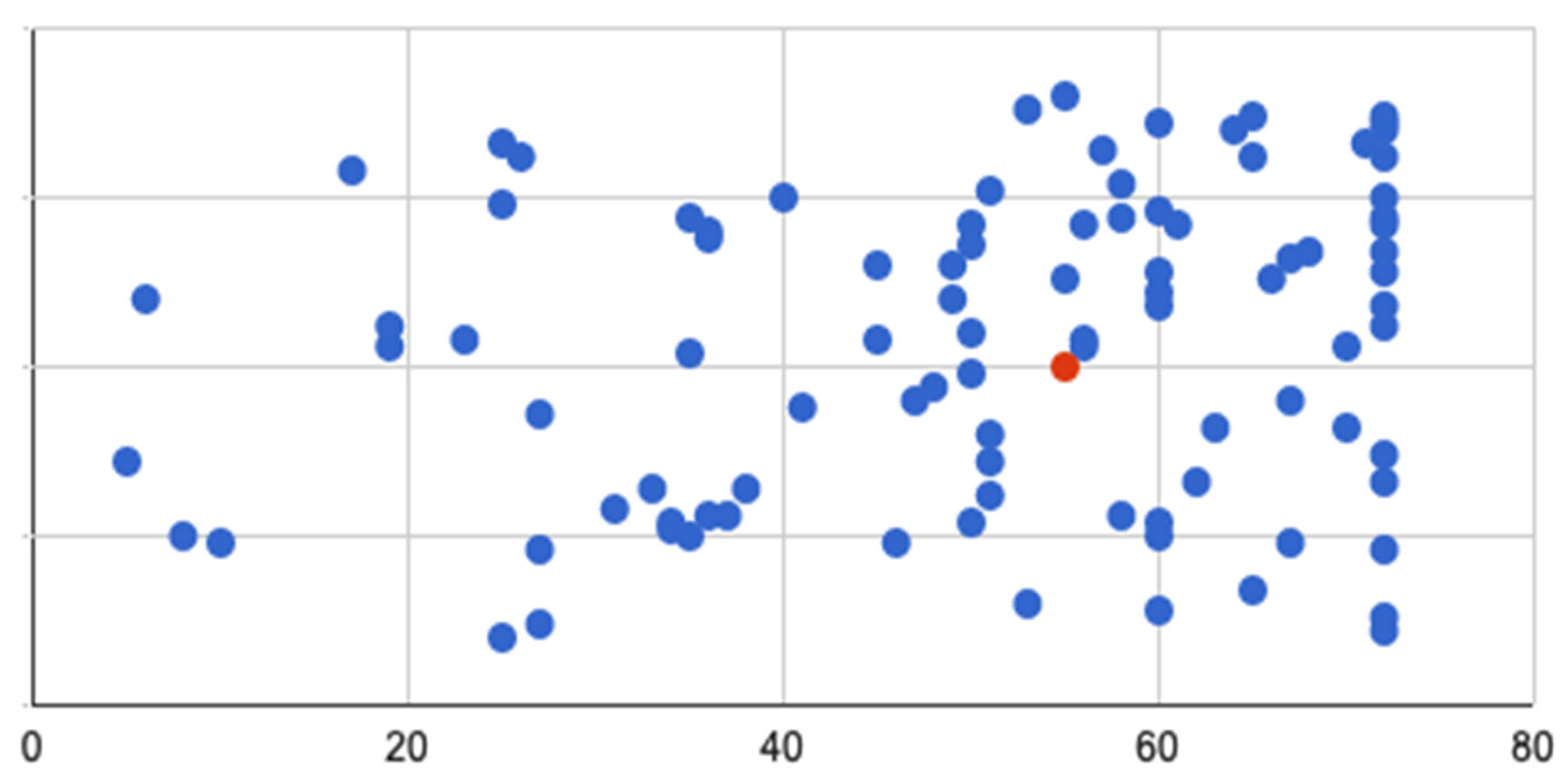
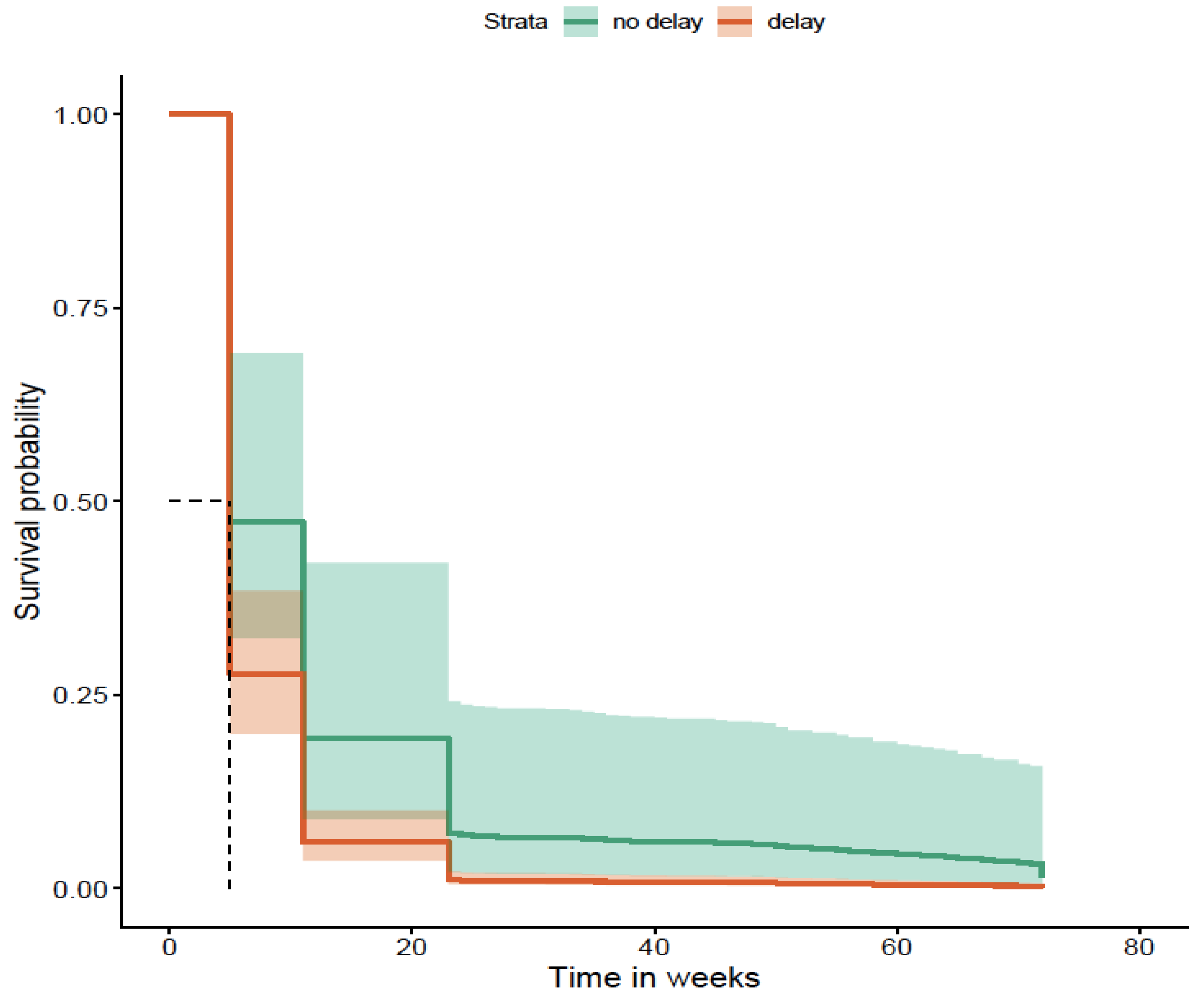
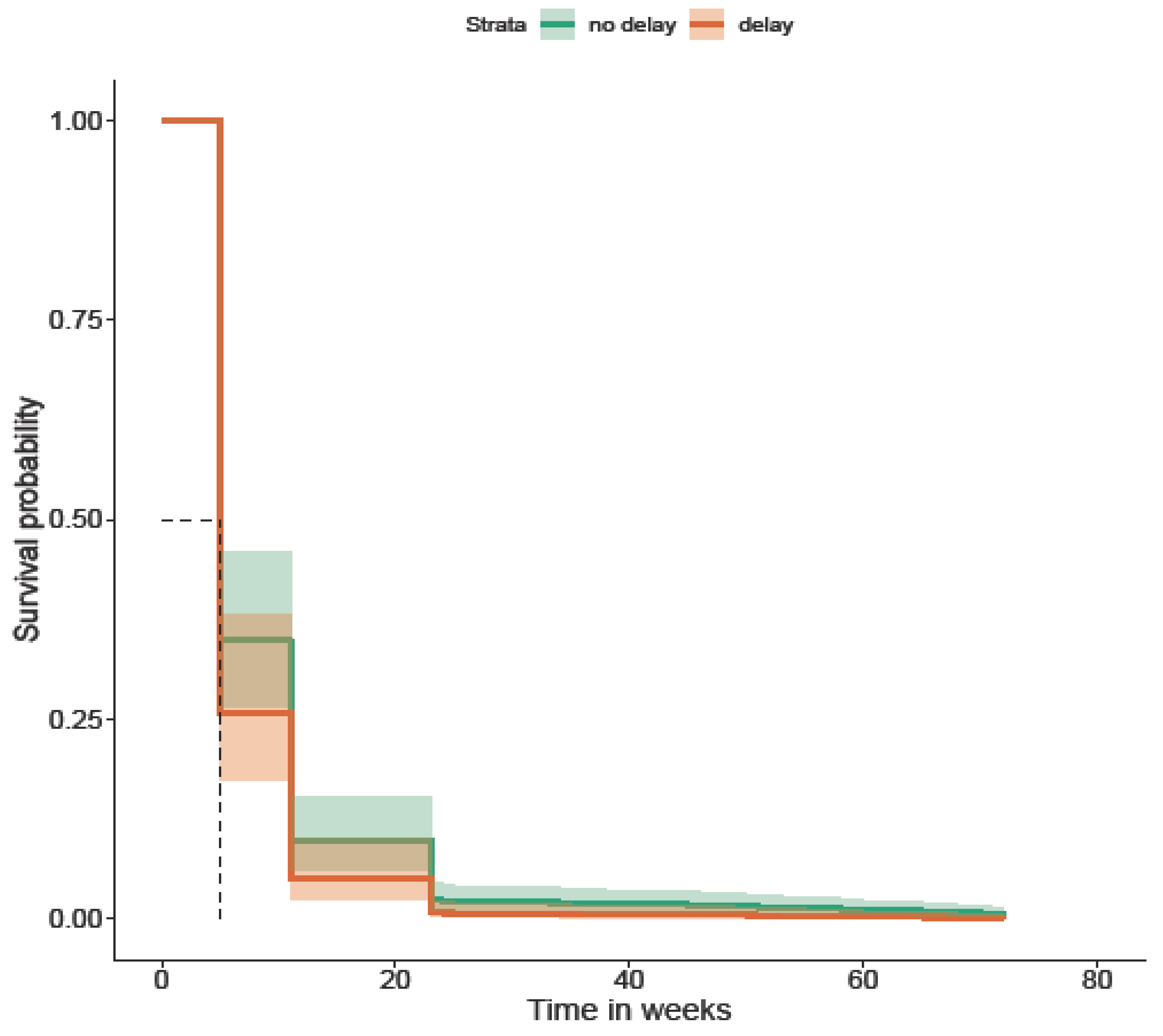
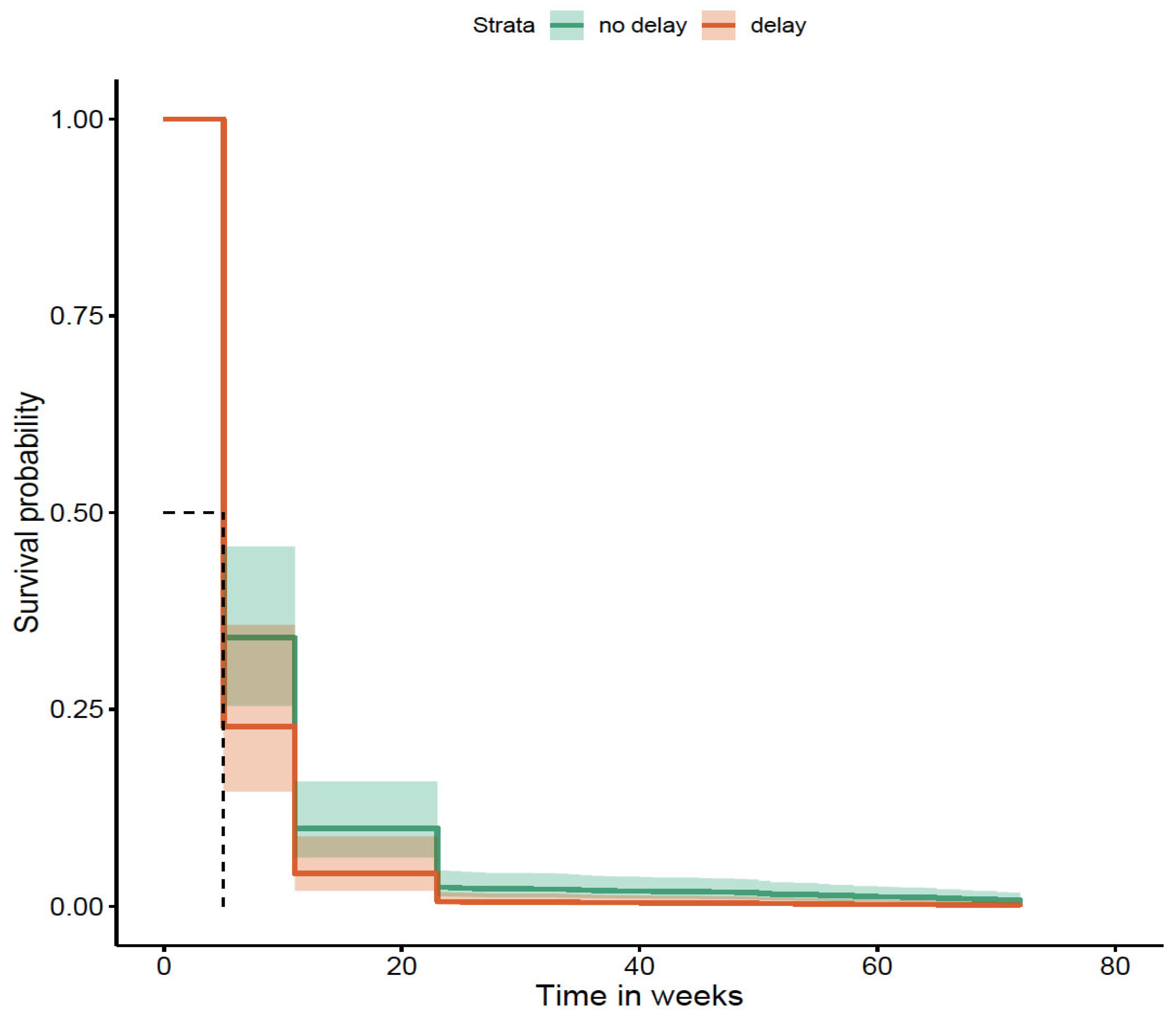
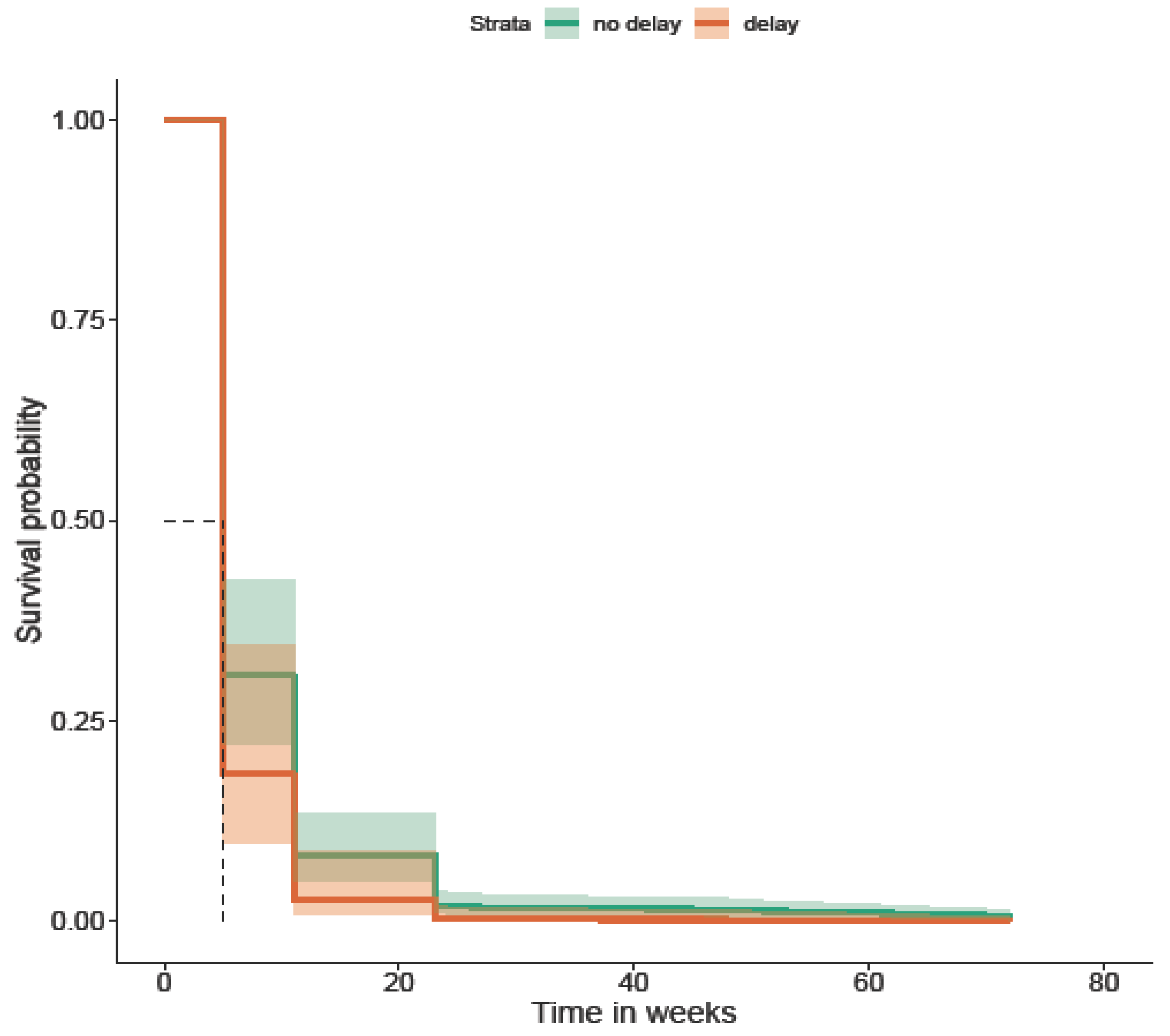
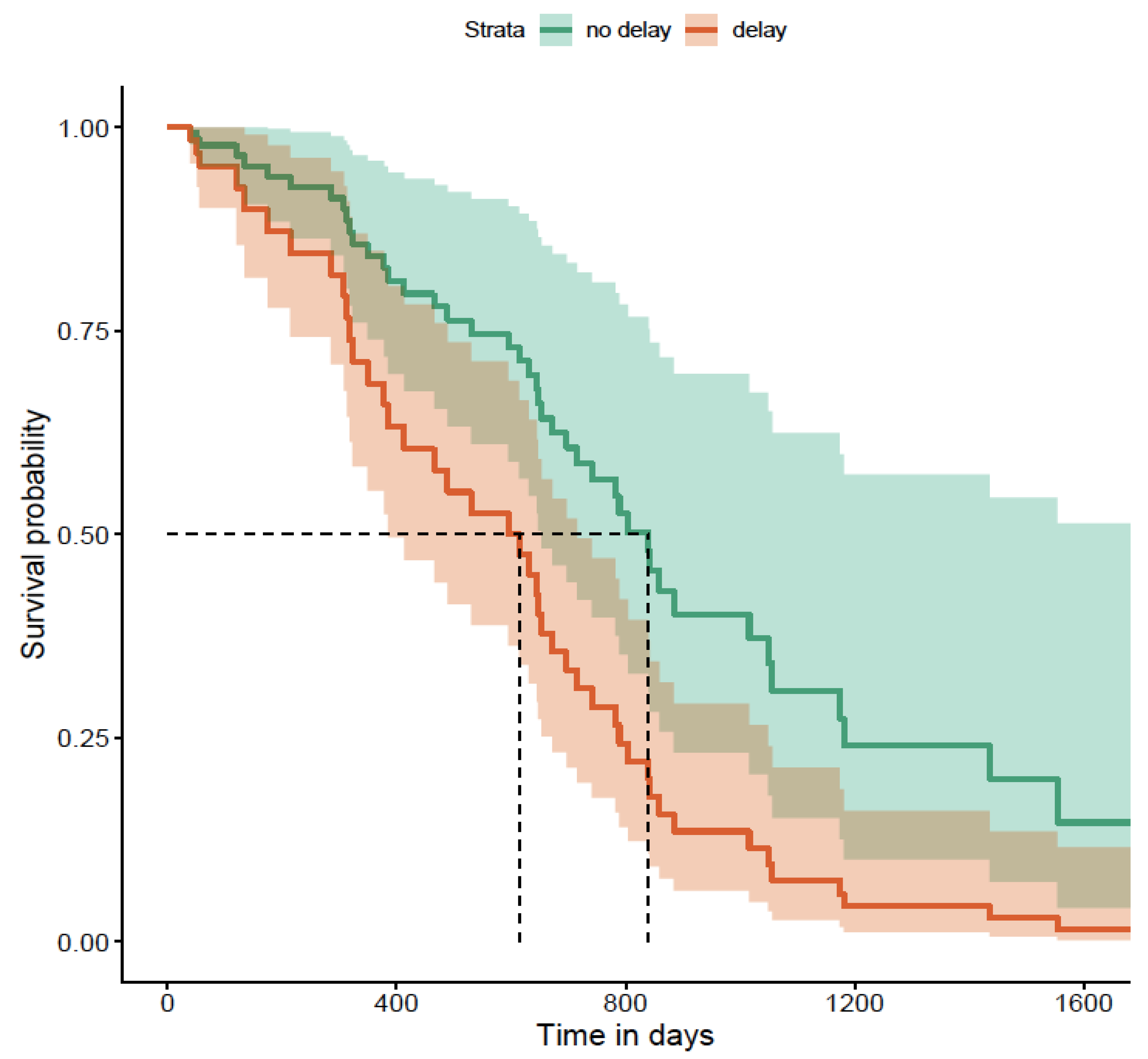
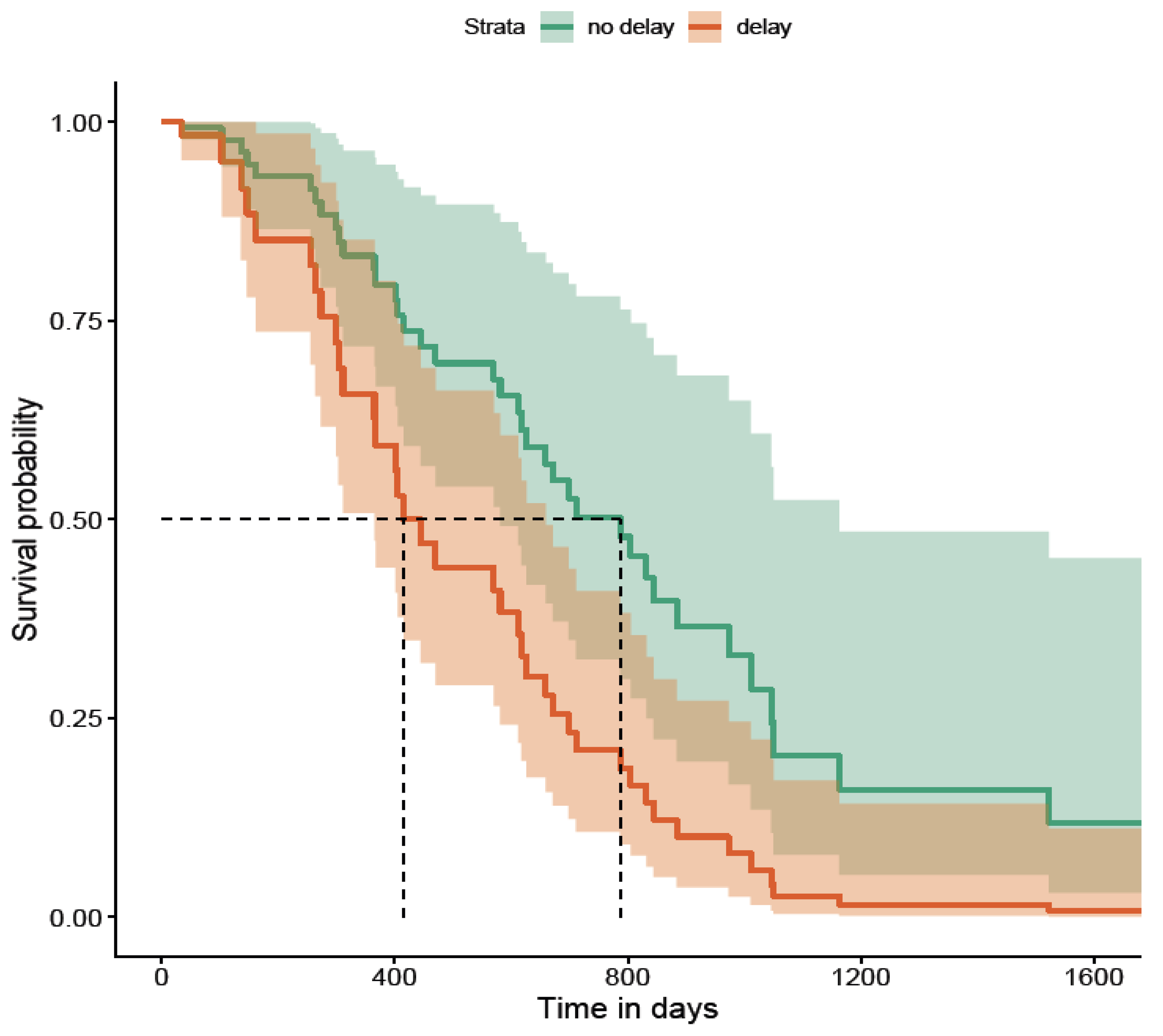
Delays and Biologic Use During Disease Course
5. Discussion
5.1. Delay in Patients Seeking Medical Attention
5.2. Delay Between GP Referral to Gastroenterology Clinic Appointment
5.3. Delay Between First Specialty Review and Index Endoscopy
5.4. Delay Between First Formal Diagnosis to Start of Treatment for IBD
5.5. Strengths and Limitations of the Study
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Data Availability Statement
Conflicts of Interest
References
- Ghosh, S; Mitchell, R. Impact of inflammatory bowel disease on quality of life: Results of the European Federation of Crohn's and Ulcerative Colitis Associations (EFCCA) patient survey. J Crohns Colitis 2007, 1(1), 10–20. [Google Scholar] [CrossRef] [PubMed]
- Burgmann, T; Clara, I; Graff, L; Walker, J; Lix, L; Rawsthorne, P; et al. The Manitoba Inflammatory Bowel Disease Cohort Study: prolonged symptoms before diagnosis--how much is irritable bowel syndrome? Clin Gastroenterol Hepatol. 2006, 4(5), 614–20. [Google Scholar] [CrossRef] [PubMed]
- Vavricka, SR; Spigaglia, SM; Rogler, G; Pittet, V; Michetti, P; Felley, C; et al. Systematic evaluation of risk factors for diagnostic delay in inflammatory bowel disease. Inflamm Bowel Dis. 2012, 18(3), 496–505. [Google Scholar] [CrossRef] [PubMed]
- Moon, CM; Jung, SA; Kim, SE; Song, HJ; Jung, Y; Ye, BD; et al. Clinical Factors and Disease Course Related to Diagnostic Delay in Korean Crohn's Disease Patients: Results from the CONNECT Study. PLoS One 2015, 10(12), e0144390. [Google Scholar] [CrossRef] [PubMed]
- Lee, DW; Koo, JS; Choe, JW; Suh, SJ; Kim, SY; Hyun, JJ; et al. Diagnostic delay in inflammatory bowel disease increases the risk of intestinal surgery. World J Gastroenterol. 2017, 23(35), 6474–81. [Google Scholar] [CrossRef] [PubMed]
- Kang, HS; Koo, JS; Lee, KM; Kim, DB; Lee, JM; Kim, YJ; et al. Two-year delay in ulcerative colitis diagnosis is associated with anti-tumor necrosis factor alpha use. World J Gastroenterol. 2019, 25(8), 989–1001. [Google Scholar] [CrossRef] [PubMed]
- Sainsbury, A; Heatley, RV. Review article: psychosocial factors in the quality of life of patients with inflammatory bowel disease. Aliment Pharmacol Ther. 2005, 21(5), 499–508. [Google Scholar] [CrossRef] [PubMed]
- Jayasooriya, N; Baillie, S; Blackwell, J; Bottle, A; Petersen, I; Creese, H; et al. Systematic review with meta-analysis: Time to diagnosis and the impact of delayed diagnosis on clinical outcomes in inflammatory bowel disease. Aliment Pharmacol Ther. 2023, 57(6), 635–52. [Google Scholar] [CrossRef] [PubMed]
- Hawthorne, AB; Glatter, J; Blackwell, J; Ainley, R; Arnott, I; Barrett, KJ; et al. Inflammatory bowel disease patient-reported quality assessment should drive service improvement: a national survey of UK IBD units and patients. Aliment Pharmacol Ther. 2022, 56(4), 625–45. [Google Scholar] [CrossRef] [PubMed]
- Kaplan, E; Meier, P. Nonparametric Estimation from Incomplete Observations. Journal of the American Statistical Association 1958, 53(282), 457–81. [Google Scholar] [CrossRef]
- Cox, DR. Regression Models and Life-Tables. Journal of the Royal Statistical Society Series B (Methodological 1972, 34(2), 187–220. [Google Scholar] [CrossRef]
- Zaharie, R; Tantau, A; Zaharie, F; Tantau, M; Gheorghe, L; Gheorghe, C; et al. Diagnostic Delay in Romanian Patients with Inflammatory Bowel Disease: Risk Factors and Impact on the Disease Course and Need for Surgery. J Crohns Colitis 2016, 10(3), 306–14. [Google Scholar] [CrossRef] [PubMed]
- Pimentel, M; Chang, M; Chow, EJ; Tabibzadeh, S; Kirit-Kiriak, V; Targan, SR; et al. Identification of a prodromal period in Crohn's disease but not ulcerative colitis. Am J Gastroenterol. 2000, 95(12), 3458–62. [Google Scholar] [CrossRef] [PubMed]
- Tan, M; Holloway, RH; Lange, K; Andrews, JM. General practitioners' knowledge of and attitudes to inflammatory bowel disease. Intern Med J. 2012, 42(7), 801–7. [Google Scholar] [CrossRef] [PubMed]
- Alharbi, R; Almahmudi, F; Makhdoom, Y; Mosli, M. Knowledge and attitudes of primary healthcare physicians toward the diagnosis and management of inflammatory bowel disease following an educational intervention: A comparative analysis. Saudi J Gastroenterol. 2019, 25(5), 277–85. [Google Scholar] [PubMed]
- Iacucci, M; Cannatelli, R; Labarile, N; Mao, R; Panaccione, R; Danese, S; et al. Endoscopy in inflammatory bowel diseases during the COVID-19 pandemic and post-pandemic period. Lancet Gastroenterol Hepatol. 2020, 5(6), 598–606. [Google Scholar] [CrossRef] [PubMed]
- Bodger, K; Bloom, S; Dobson, L; Cummings, F; Grainger, S; Kennedy, N; et al. PMO-37 COVID-19 impact on care and prescribing for inflammatory bowel disease: Data from the IBD Registry. Gut 2021, 70 (Suppl 4), A95–A6. [Google Scholar] [CrossRef]
| Age & gender | N=105 |
|---|---|
| Median age | 32 years (range 21-82 years) |
| Gender | Male=58; Female=47 |
| Race | |
| Caucasian | 65 (62%) |
| Asian | 28 (27%) |
| Afro-Caribbean | 1 (1%) |
| Unknown/Unreported | 11 (10%) |
| Disease type at first diagnosis | |
| Ulcerative colitis | 65 (62%) |
| Crohn’s disease | 27 (26%) |
| IBD-unclassified | 13 (12%) |
| Montreal classification for CD | |
| Age A1 A2 A3 |
2 22 3 |
| Location L1 L2 L3 L4 L3+L4 |
7 6 13 0 1 |
| Behaviour B1 B2 B3 B1+ perianal |
21 3 0 3 |
| Ulcerative colitis extent | |
| E1 E2 E3 |
12 36 17 |
| Symptoms at presentation | Number of patients |
|---|---|
| Abdominal pain | 44 |
| Loose stools | 40 |
| Loose stools with blood in stools | 37 |
| Bleeding per rectum | 33 |
| Weight loss | 16 |
| Vomiting | 5 |
| Medications started at first diagnosis | |
| Oral 5-ASA | 48 |
| Oral Steroids | 33 |
| Rectal 5-ASA | 32 |
| Rectal steroids | 8 |
| 5-ASA and steroids | 6 |
| Thiopurines | 5 |
| Biologics | 5 |
| Details of follow-up | |
| Median follow-up period of cohort | 55 months (range 5-72 months) |
| Patients with first follow-up <6 months | 101 |
| Patients with first follow-up 6-12 months | 2 |
| Patients with first follow-up 12-24 months | 2 |
| Patients with first follow-up >24 months | 0 |
| Type of delay | Risk of biologic use during follow up (OR with CI) |
|---|---|
| Delay in patients seeking medical attention in community | 1.08 (1.03, 1.17) |
|
Delay between GP referral to the point of review in Gastroenterology clinic |
1.10 (1.0, 1.23) |
|
Delay between first specialty review and index endoscopy |
1.09 (1.01, 1.21) |
| Delay between first formal diagnosis to start of treatment for IBD | 1.08 (1.0, 1.21) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




