1. Introduction
The organizational commitment of physicians has emerged as a fundamental pillar for the stability and excellence of modern healthcare systems. Characterized by a robust emotional attachment and a proactive dedication to institutional goals, this commitment is not merely a psychological state but a critical determinant of professional efficacy and personal accomplishment. In a field intrinsically defined by high-intensity human interaction, maintaining elevated levels of organizational commitment serves as a vital buffer against the deleterious effects of occupational stress, ensuring both job satisfaction and operational efficiency.
Despite its importance, the contemporary hospital environment has become progressively demanding, creating a challenging landscape for medical staff. Recent evidence suggests that a significant proportion of physician’s report symptoms of burnout, often precipitated by unfavorable working conditions and a perceived lack of administrative support. This phenomenon is directly linked to decreased job satisfaction, increased absenteeism, and higher turnover intentions, all of which compromise the overarching quality of patient care and safety.
Current research in the field presents diverging hypotheses regarding the most effective level of intervention. While some scholars emphasize individual resilience-building as a primary solution, a growing body of evidence suggests that without systemic organizational reform, individual-focused strategies yield only transient benefits. This controversy underscores the necessity for a more integrated understanding of how institutional structures influence professional commitment.
The purpose of this scoping review is to systematically map the existing literature to identify the core factors driving physicians' organizational commitment and to evaluate the efficacy of multifaceted interventions in mitigating burnout. By synthesizing data from key publications over the last decade, this study highlights that executive leadership support and proactive organizational culture are the principal catalysts for institutional sustainability. Ultimately, this work concludes that investing in physician well-being is an economically advantageous strategy that fosters a resilient healthcare workforce and enhances the quality-of-care delivery.
2. Materials and Methods
2.1. Methodological Framework and Rigor
This scoping review was conducted in strict accordance with the methodological framework proposed by Arksey and O’Malley and further refined by the Joanna Briggs Institute (JBI). To ensure the highest level of transparency and scientific rigor, the study adheres to the Preferred Reporting Items for Systematic Reviews and Meta-Analyses extension for Scoping Reviews (PRISMA-ScR) guidelines. This systematic approach ensures that the mapping of physicians' organizational commitment is both comprehensive and reproducible.
Furthermore, the protocol for this scoping review has been submitted for registration in the International Prospective Register of Systematic Reviews (PROSPERO). The registration process ensures the transparency of the research and prevents unintended duplication of reviews, reflecting the authors' commitment to high methodological standards.
2.2. Selection Flow and Data Synthesis
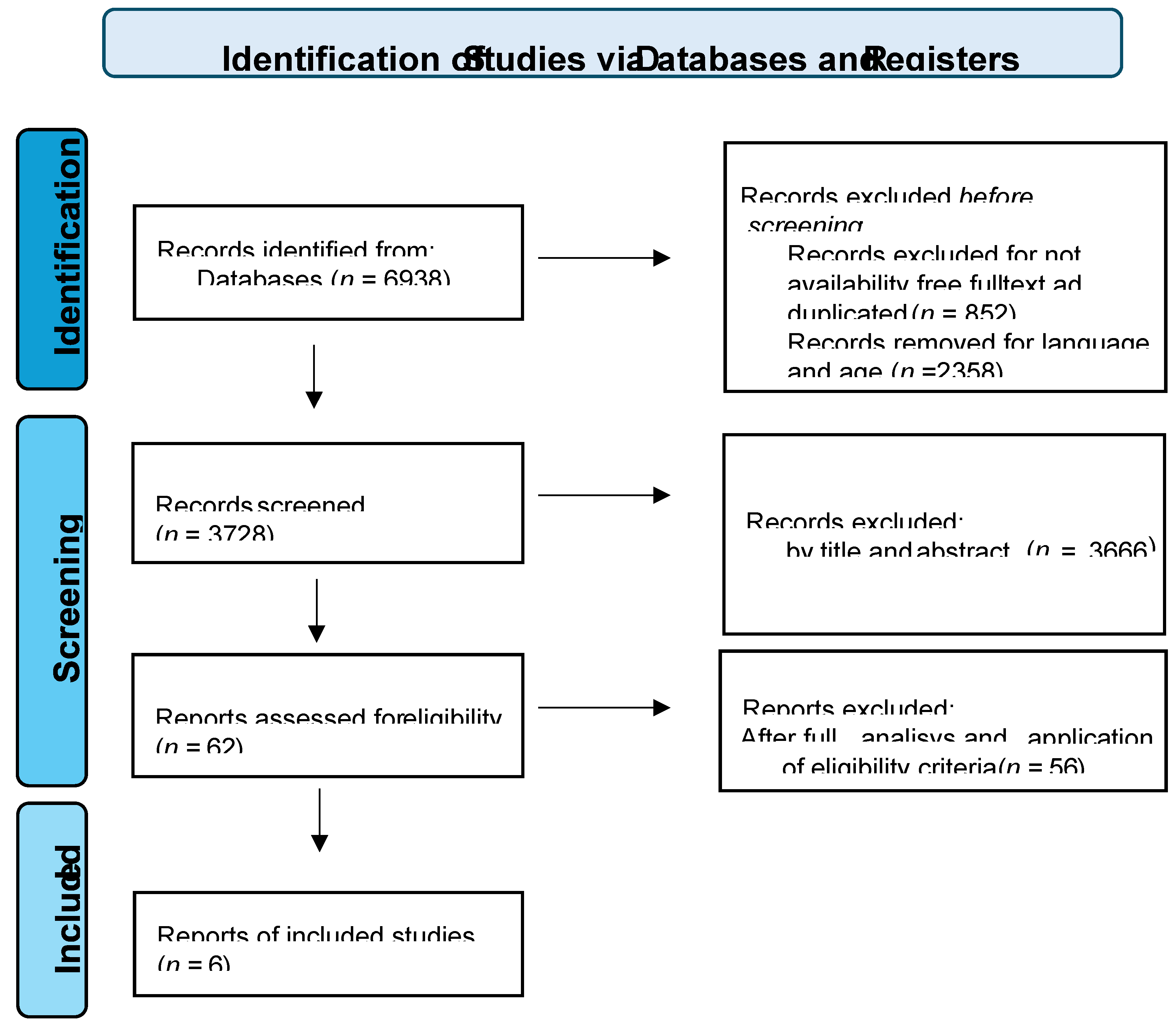
The identification of relevant literature involves a multi-stage process. The initial systematic search across PubMed, CINAHL, and PsycINFO yielded a total of 6,938 records. Following the removal of duplicates and a preliminary screening of titles and abstracts, the remaining articles were subjected to a rigorous full-text evaluation based on the PCC (Population, Concept, and Context) eligibility criteria.
After this exhaustive screening, six primary studies and systematic reviews were selected for qualitative synthesis. These documents were identified as providing critical evidence on the organizational strategies that foster professional commitment and institutional sustainability.
3. Results and Discussion
3.1. Organizational Strategies and Leadership
The qualitative synthesis identified nine pivotal organizational strategies essential for fostering physicians' organizational commitment. A central finding of this review is the paramount importance of clinical leadership characterized by high levels of emotional intelligence. Leaders who possess the ability to recognize, understand, and manage emotions—both their own and those of their subordinates—are significantly more effective in creating a supportive work environment. This leadership style directly influences the professional’s sense of belonging and institutional commitment, serving as a protective factor against the psychological erosion caused by high-pressure clinical settings.
3.2. The Economic Rationale for Commitment
Beyond the ethical and clinical imperatives, this study strengthens the economic argument for investing in physician well-being. The data synthesized indicates that medical turnover represents a staggering financial burden for healthcare institutions. Estimates suggest that the cost of replacing a single physician can reach up to three times their annual salary, factoring in recruitment, onboarding, and the loss of clinical productivity. Therefore, fostering organizational commitment is not merely a human resources initiative but a strategic financial necessity. By reducing turnover rates, institutions can ensure long-term operational cost-effectiveness and maintain the continuity of care.
3.3. Multifaceted Interventions: Structural and Individual Synergy
The discussion further clarifies the hierarchy of interventions aimed at enhancing commitment and mitigating burnout. While individual-focused initiatives, such as mindfulness or resilience training, provide valuable support, they are insufficient when implemented in isolation. This review underscores that professional commitment is most effectively fostered through multifaceted interventions. The synergy between structural changes—such as the optimization of workload and the reduction of administrative burdens—and personalized individual support represents the gold standard for institutional reform. It is the combination of streamlined organizational architecture and a culture of appreciation that truly sustains the physician's commitment to the healthcare mission.
4. Conclusions and Future Directions
The findings of this scoping review underscore that investing in physician well-being and fostering organizational commitment is a paramount strategic necessity rather than a peripheral human resources concern. As healthcare systems face increasing pressure from rising clinical demands and workforce depletion, the stability of medical institutions depends fundamentally on the strength of the bond between the clinician and the organization. This study confirms that a resilient healthcare delivery model is only achievable when institutional leaders prioritize a culture of support, emotional intelligence, and structural reform.
Furthermore, the economic rationale presented herein provides a compelling case for executive intervention. By recognizing that the cost of professional disengagement and subsequent turnover can triple a physician’s annual salary, healthcare administrators must view initiatives that promote commitment as high-yield strategic investments. The transition from fragmented, individual-focused wellness programs to integrated, multifaceted organizational strategies is essential for ensuring long-term institutional viability and the maintenance of high-quality patient care.
Regarding the future research agenda, this review identifies critical gaps that necessitate further academic inquiry. We suggest that priority be given to longitudinal studies designed to evaluate the long-term impact of systemic interventions on physicians' organizational commitment. Additionally, as digital transformation reshapes the clinical landscape, it is imperative to investigate the role of digital health technologies and electronic health records (EHR) in either augmenting or diminishing professional engagement. Future investigations should also explore how diverse cultural and geographic healthcare contexts influence the efficacy of leadership-driven strategies. In conclusion, healthcare organizations must transition from fragmented wellness initiatives toward integrated, leadership-driven strategies. Future research should prioritize longitudinal studies to evaluate the long-term impact of systemic interventions on physicians' organizational commitment, including the role of emerging digital technologies.
References
- Shanafelt, T.D.; Noseworthy, J.H. Executive Leadership and Physician Well-being: Nine Organizational Strategies to Promote Engagement and Reduce Burnout. Mayo Clin. Proc. 2017, 92, 129–146. [Google Scholar] [CrossRef] [PubMed]
- West, C.P.; Dyrbye, L.N.; Sinsky, C.; Trockel, M.; Tutty, M.; Nedelec, L.; Carlasare, L.E.; Shanafelt, T.D. Resilience and Burnout Among Physicians Under the Age of 35 Years in the United States. Mayo Clin. Proc. 2020, 95, 1125–1133. [Google Scholar] [CrossRef]
- Rothenberger, D.A. Physician Burnout and Well-Being: A Systematic Review and Proposals for Solutions. Clin. Colon Rectal Surg. 2017, 30, 123–132. [Google Scholar] [CrossRef]
- Panagioti, M.; Panagopoulou, E.; Bower, P.; Lewith, G.; Kontopantelis, E.; Chew-Graham, C.; Dawson, S.; van Dijk, F.; Geraghty, A.W.; Esmail, A. Controlled Interventions to Reduce Burnout in Physicians: A Systematic Review and Meta-analysis. JAMA Intern. Med. 2017, 177, 195–205. [Google Scholar] [CrossRef] [PubMed]
- Montgomery, A.; van der Doef, M.; Panagopoulou, E.; Leiter, M.P. Connecting Healthcare Worker Well-Being, Patient Safety and Organisational Change: The GOHIS Study; Springer: Cham, Switzerland, 2020; pp. 15–30. [Google Scholar]
- De Hert, S. Burnout in Healthcare Workers is Prevalent in All Specialties: A Case for Individual and Organizational Responsibility. Front. Psychol. 2020, 11, 562932. [Google Scholar] [CrossRef]
- Shanafelt, T.D.; Goh, J.; Sinsky, C. The Business Case for Investing in Physician Well-being. JAMA Intern. Med. 2017, 177, 1826–1832. [Google Scholar] [CrossRef] [PubMed]
- Arksey, H.; O'Malley, L. Scoping Studies: Towards a Methodological Framework. Int. J. Soc. Res. Methodol. 2005, 8, 19–32. [Google Scholar] [CrossRef]
- Peters, M.D.J.; Godfrey, C.; McInerney, P.; Munn, Z.; Trico, A.C.; Khalil, H. Chapter 11: Scoping Reviews. In JBI Manual for Evidence Synthesis; Aromataris, E., Munn, Z., Eds.; JBI: Adelaide, Australia, 2020. [CrossRef]
- Tricco, A.C.; Lillie, E.; Zarin, W.; O'Brien, K.K.; Colquhoun, H.; Levac, D.; Moher, D.; Peters, M.D.; Horsley, T.; Weeks, L.; et al. PRISMA Extension for Scoping Reviews (PRISMA-ScR): Checklist and Explanation. Ann. Intern. Med. 2018, 169, 467–473. [Google Scholar] [CrossRef] [PubMed]
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).