Submitted:
14 January 2026
Posted:
15 January 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Results
2.1. Study Population and Demographic Characteristics
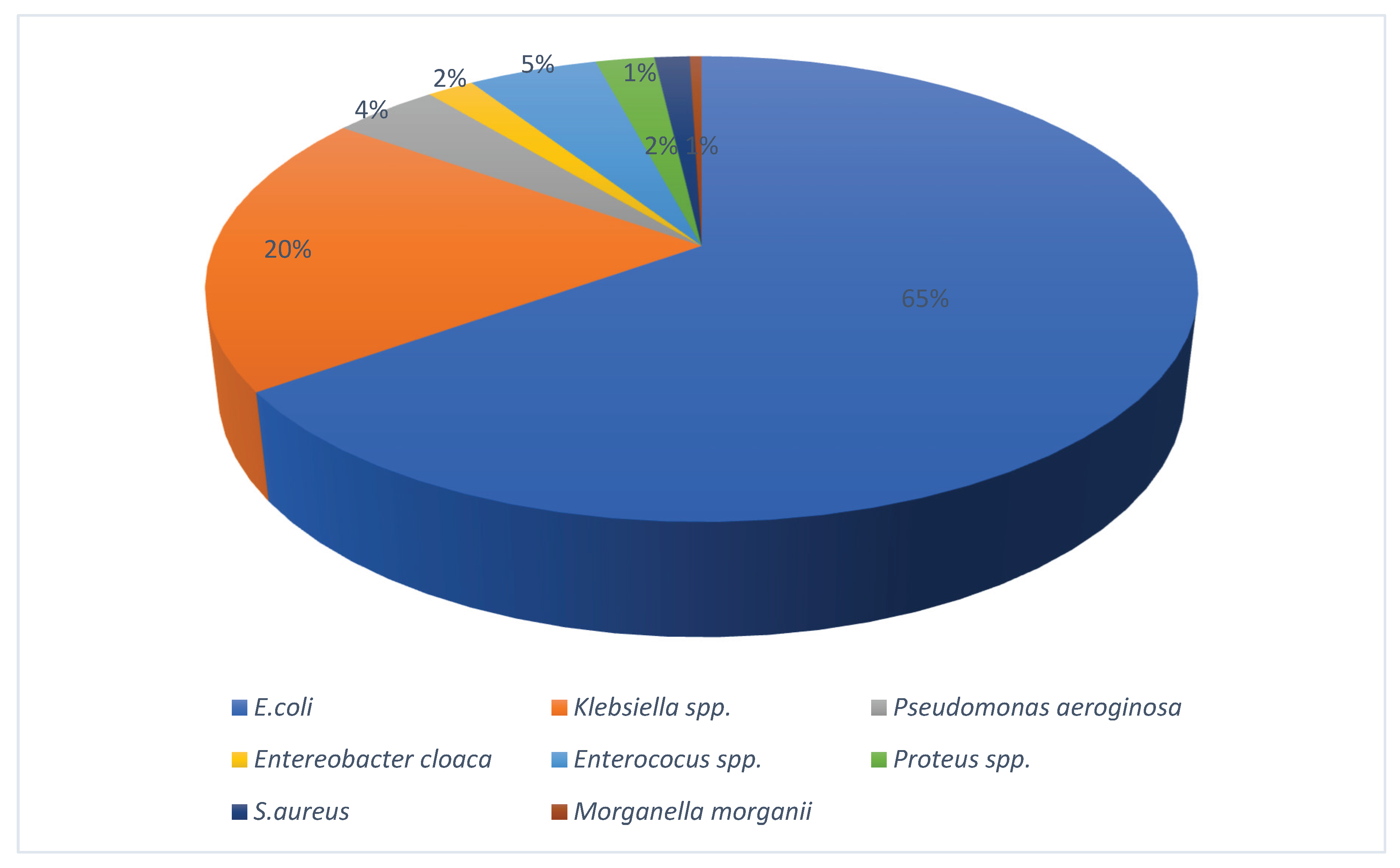
2.2. Microbiological Results
2.3. Distribution of ESBL and Associated Factors
| Variable | ESBL positive n (%) |
ESBL negative n (%) | p value |
|---|---|---|---|
| Hospitalization in the preceding month Yes No |
|||
| 28 (80.0) 67 (46.2) |
7 (20.0) 78 (53.8) |
<0,0011 | |
| Antibiotic exposure in the previous three months Yes No |
47 (67.1) 48 (43.6) |
23 (32.9) 62 (56.4) |
0,0021 |
| History of urinary tract infection within the previous year Yes No |
29 (60.4) 66 (50.0) |
19 (39.6) 66 (50.0) |
0,2161 |
2.4. Antimicrobial Susceptibility Results
| ESBL positive n:91 |
ESBL negative n:78 |
p value | |
|---|---|---|---|
|
Amikacin Resistant Sensitive to high doses Sensitive |
|||
| 5 (5.5) | 0(0) | ||
| 7 (7.7) | 0(0) | 0,0011 | |
| 79 (86.8) | 78 (100.0) | ||
|
Amoxicillin-clavulanic acid Resistant Sensitive |
59 (64.8) 32 (35.2) |
9 (11.5) 69 (88.5) |
<0,0011 |
|
Ciprofloxacin Resistant Sensitive to high doses Sensitive |
58 (65.2) 13 (14.6) 18 (20.2) |
7 (9.0) 0(0) 71 (91.0) |
<0,0011 |
|
Gentamicin Resistant Sensitive |
15 (16.5) 76 (83.5) |
1 (1.3) 77 (98.7) |
0,0011 |
|
Meropenem Resistant Sensitive to high doses Sensitive |
10 (11.0) 2 (2.2) 79 (86.8) |
0 (0) 0(0) 0(0) |
0,0011 |
|
Piperacillin-Tazobactam Resistant Sensitive |
26(28.6) 65 (71.4) |
1 (1.3) 77 (98.7) |
0,0011 |
2.5. Empirical Therapy and Treatment Modifications
| Antibiotic change | n (%) |
|---|---|
|
All treatments Present absent |
|
| 110 (53.9) | |
| 94 (46.1) | |
|
Ceftriaxone Present Absent |
70 (53.8) 60 (46.2) |
|
Piperacillin-Tazobactam Present Absent |
29 (72.5) 11 (27.5) |
|
Ertapenem/Meropenem Present Absent |
7 (35.0) 13 (65.0) |
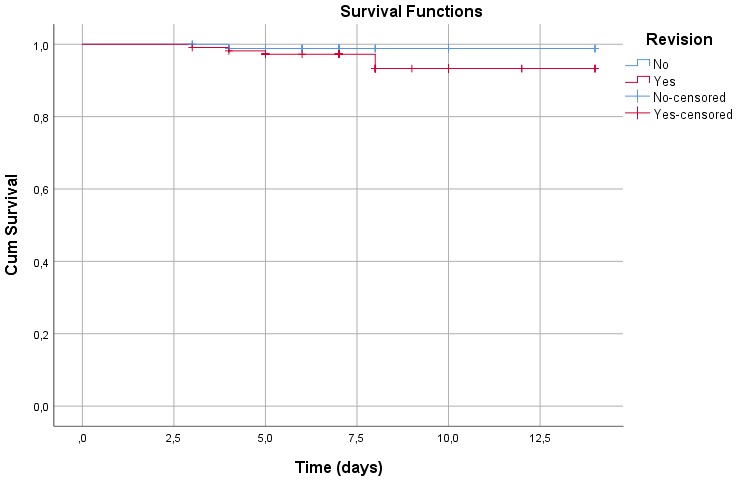
2.6. Clinical Outcomes and Mortality Rates
2.7. Changes in Laboratory Parameters and Imaging Findings
3. Discussion
4. Materials and Methods
4.1. Patient Selection and Study Population
4.2. Data Collection
4.3. Sample Processing and Microbiological Evaluation
4.4. Antimicrobial Susceptibility Testing
4.5. Statistical Analysis
5. Conclusions
Author Contributions
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| ESBL | Extended spectrum beta-lactamases |
| UTI | Urinary tract infection |
| ICU | Intensive care unit |
| DM | Diabetes mellitus |
References
- Trautner, B.W.; Cortés-Penfield, N.W.; Gupta, K.; Hirsch, E.B.; Horstman, M.; Moran, G.J.; Colgan, R.; O’Horo, J.C.; Ashraf, M.S.; Connolly, S.; et al. Complicated urinary tract infections: Treatment and management. Clin. Infect. Dis. 2025, 78, 123–134. [CrossRef]
- Foxman B. The epidemiology of urinary tract infection. Nat. Rev. Urol. 2010, 7, 653–660. [CrossRef]
- Johnson, J.R.; Russo, T.A. Acute pyelonephritis in adults. N. Engl. J. Med. 2018, 378, 48–59. [CrossRef]
- Stapleton, A.E.; Endo, Z.; Blaser, B.S.; Sobel J.D. Urinary tract infections. In: Mandell, Douglas, and Bennett’s Principles and Practice of Infectious Diseases, 10th ed.; Blaser, M.J., Cohen, J.I., Holland, S.M., Eds.; Elsevier: Philadelphia, PA, USA, 2025; pp. 909–929.e5. ISBN 978-0-323-93499-2.
- Larramendy, S.; Deglaire, V.; Dusollier, P.; Fournier, J.P.; Caillon, J.; Beaudeau, F.; Moret, L. Risk factors of extended-spectrum beta-lactamases-producing Escherichia coli community-acquired urinary tract infections: A systematic review. Infect. Drug Resist. 2020, 13, 3945–3955. [CrossRef]
- Flores-Mireles, A.L.; Walker, J.N.; Caparon, M.; Hultgren, S.J. Urinary tract infections: Epidemiology, mechanisms of infection and treatment options. Nat. Rev. Microbiol. 2015, 13, 269–284. [CrossRef]
- Şencan, İ.; Karabay, O.; Altay,F.A.; Yıldız, S.S.; Şimşek, H.; Gözükara, M.G.; Kuzi, S.; Karlıdağ, G.E.; Kaya, Ş.; Kul, G.; el al. Multidrug resistance in pathogens of community-acquired urinary tract infections in Turkey: A multicentre prospective observational study. Turk. J. Med. Sci. 2023, 53, 780–790. [CrossRef]
- Tenney, J.; Hudson, N.; Alnifaidy, H.; Li, J.T.C.; Fung, K.H. Risk factors for acquiring multidrug-resistant organisms in urinary tract infections: A systematic literature review. Saudi Pharm. J. 2018, 26, 678–684. [CrossRef]
- Belyayeva M, Leslie SW, Rout P, et al. Acute Pyelonephritis. [Updated 2024 Feb 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2025 Jan-. Available from: https://www.ncbi.nlm.nih.gov/sites/books/NBK519537.
- Angebault C.; Andremont A. Antimicrobial agent exposure and the emergence and spread of resistant microorganisms: Issues associated with study design. Eur. J. Clin. Microbiol. Infect. Dis. 2013, 32, 581–595. [CrossRef]
- Yıldırım, Ç.; Sarı, S.; Parmaksızoğlu Aydın, A.M.; Kilinç Toker, A.; Turunç Özdemir, A.; Erdem Kıvrak, E.; Mermer, S.; Kahraman, H.; Soysal, O.; Yıldırım, H.Ç.; et al. Extended-Spectrum Beta-Lactamase Production and Carbapenem Resistance in Elderly Urinary Tract Infection Patients: A Multicenter Retrospective Study from Turkey. Antibiotics 2025, 14, 719. [CrossRef]
- Zhou, Y.L.; Long, B.L.; Liu, H.L.; Wu, J.; Xia, H. Risk factors and drug resistance of adult community-onset urinary tract infections caused by Escherichia coli–producing extended-spectrum β-lactamase in the Chongqing region, China: A retrospective case-control study. BMJ Open 2024, 14, e090665. [CrossRef]
- Gupta, K.; Hooton, T.M.; Naber, K.G.; Wullt, B.; Colgan, R.; Miller, L.G.; Moran, G.J.; Nicolle, L.E.; Raz, R.; Schaeffer, A.J.; Soper, D.E. International clinical practice guidelines for the treatment of acute uncomplicated cystitis and pyelonephritis in women: A 2010 update by the Infectious Diseases Society of America and the European Society for Microbiology and Infectious Diseases. Clin. Infect. Dis. 2011, 52, e103–e120. [CrossRef]
- Ince, D.; Fiawoo, S.; Choudhury, R.; Cosgrove, S.E.; Dobrzynski, D.; Gold, H.; Lee, J.H.; Percival, K.M.; Shulder, S.; Sony, D.; Spivak, E.S.; Tamma, P.D.; Nori, P. Epidemiology of Gram-negative bloodstream infections in the United States: Results from a cohort of 24 hospitals. Open Forum Infect. Dis. 2023, 10, ofad265. [CrossRef]
- Zhu, H.; Chen, Y.; Hang, Y.; Luo, H.; Fang, X.; Xiao, Y.; Cao, X.; Zou, S.; Hu, X.; Hu, L.; Zhong, Q. Impact of inappropriate empirical antibiotic treatment on clinical outcomes of urinary tract infections caused by Escherichia coli: A retrospective cohort study. J. Glob. Antimicrob. Resist. 2021, 26, 148–153. [CrossRef]
- Salam, M.A.; Al-Amin, M.Y.; Salam, M.T.; Pawar, J.S.; Akhter, N.; Rabaan, A.A.; Alqumber, M.A.A. Antimicrobial resistance: A growing serious threat for global public health. Healthcare 2023, 11, 1946. [CrossRef]
- Barlam, T.F.; Cosgrove, S.E.; Abbo, L.M.; MacDougall, C.; Schuetz, A.N.; Septimus, E.J.; Srinivasan, A.; Dellit, T.H.; Falck-Ytter, Y.T.; Fishman, N.O.; et al. Implementing an antibiotic stewardship program: Guidelines by the Infectious Diseases Society of America and the Society for Healthcare Epidemiology of America. Clin. Infect. Dis. 2016, 62, e51–e77. [CrossRef]
- Azap, O.K.; Arslan, H.; Serefhanoğlu, K.; Colakoğlu, S.; Erdoğan, H.; Timurkaynak, F.; Senger, S.S. Risk factors for extended-spectrum beta-lactamase positivity in uropathogenic Escherichia coli isolated from community-acquired urinary tract infections. Clin. Microbiol. Infect. 2010, 16, 147–151. [CrossRef]
- Kayaaslan, B.; Oktay, Z.; Hasanoglu, I.; Kalem, A.K.; Eser, F.; Ayhan, M.; Guner, R. Increasing rates of extended-spectrum β-lactamase-producing Escherichia coli and Klebsiella pneumoniae in uncomplicated and complicated acute pyelonephritis and evaluation of empirical treatments based on culture results. Eur. J. Clin. Microbiol. Infect. Dis. 2022, 41, 421–430. [CrossRef]
- Hsu, C.Y.; Fang, H.C.; Chou, K.J.; Chen, C.L.; Lee, P.T.; Chung, H.M. The clinical impact of bacteremia in complicated acute pyelonephritis. Am. J. Med. Sci. 2006, 332, 175–180. [CrossRef]
- Gofron, Z.F.; Aptekorz, M.; Gibas, K.W.; Kabała, M.; Martirosian, G. Retrospective study of the etiology, laboratory findings, and management of patients with urinary tract infections and urosepsis from a urology center in Silesia, southern Poland between 2017 and 2020. Med. Sci. Monit. 2022, 28, e935478. [CrossRef]
- Osthoff, M.; McGuinness, S.L.; Wagen, A.Z.; Eisen, D.P. Urinary tract infections due to extended-spectrum beta-lactamase-producing Gram-negative bacteria: Identification of risk factors and outcome predictors in an Australian tertiary referral hospital. Int. J. Infect. Dis. 2015, 34, 79–83. [CrossRef]
- World Health Organization. WHO Regional Office for Europe Antimicrobial Medicines Consumption (AMC) Network: AMC Data 2023. World Health Organization Regional Office for Europe, Copenhagen, Denmark, 2025. Available online: https://iris.who.int/handle/10665/380848 (accessed on 8 January 2026).
- Zhou, Y.L.; Long, B.L.; Liu, H.L.; Wu, J.; Xia, H. Risk factors and drug resistance of adult community-onset urinary tract infections caused by Escherichia coli-producing extended-spectrum β-lactamase in the Chongqing region, China: A retrospective case-control study. BMJ Open 2024, 14(10), e090665. [CrossRef]
- Muteeb, G.; Rehman, M.T.; Shahwan, M.; Aatif, M. Origin of antibiotics and antibiotic resistance, and their impacts on drug development: A narrative review. Pharmaceuticals 2023, 16(11), 1615. [CrossRef]
- Alshareef, H.; Alfahad, W.; Albaadani, A.; Alyazid, H.; Talib, R.B. Impact of antibiotic de-escalation on hospitalized patients with urinary tract infections: A retrospective cohort single center study. J. Infect. Public Health 2020, 13(7), 985–990. [CrossRef]
- Nelson, Z.; Aslan, A.T.; Beahm, N.P.; Blyth, M.; Cappiello, M.; Casaus, D.; Dominguez, F.; Egbert, S.; Hanretty, A.; Khadem, T.; et al. Guidelines for the prevention, diagnosis, and management of urinary tract infections in pediatrics and adults: A WikiGuidelines Group consensus statement. JAMA Netw. Open 2024, 7(11), e2444495. [CrossRef]
- Francisco, M.Z.; Altmayer, S.; Verma, N.; Watte, G.; Brandao, M.C.; Barros, M.C.; Mohammed, T.L.; Hochhegger, B. Appropriateness of computed tomography and ultrasound for abdominal complaints in the emergency department. Curr. Probl. Diagn. Radiol. 2021, 50(6), 799–802. [CrossRef]
- European Committee on Antimicrobial Susceptibility Testing (EUCAST). Breakpoint tables for interpretation of MICs and zone diameters. Version 19, EUCAST; Växjö, Sweden. Available online: https://www.eucast.org.
| Variable | Yes n(%) | No n(%) |
|---|---|---|
| History of UTI | 54 (26.5) | 150 (73.5) |
| CKD/Dialysis | 27 (13.2) | 177 (86.8) |
| Transurethral catheterization | 24 (11.8) | 180 (88.2) |
| Nephrostomy | 2 (1) | 202 (99) |
| Urethral Stent | 2 (1) | 202 (99) |
| Anatomical defect | 10 (4.9) | 194 (95.1) |
| Neurogenic bladder | 11 (5.4) | 193 (94.6) |
| Vesicoureteral reflux | 2 (1) | 202 (99) |
| BPH | 46 (22.5) | 158 (77.5) |
| Prostatitis | 1 (0.5) | 203 (99.5) |
| Urolithiasis | 28 (13.7) | 176 (86.3) |
| Urinary Intervention | 31 (15.2) | 174 (84.8) |
| Variable | ESBL positive n (%) |
ESBL negative n (%) |
p value |
|---|---|---|---|
| Male | 48 (64.9) | 26 (35.1) | 0,0071 |
| Age (mean ± SD) | 68.2±16.7 | 68.7±18.4 | 0,8312 |
| Uncontrolled DM | 42 (53,8) | 36 (46,2) | 0,8021 |
| Hypertension | 54 (57,4) | 40 (42,6) | 0,1901 |
| Heart Failure | 18 (60,0) | 12 (40,0) | 0,3851 |
| COPD/Asthma | 15 (57,7) | 11 (42,3) | 0,5871 |
| Neurological disease | 29 (52,7) | 26 (47,3) | 0,9931 |
| Malignancy | 11 (55,0) | 9 (45,0) | 0,8331 |
| Immunosuppression | 9 (69,2) | 4 (30,8) | 0,2171 |
| CKD / Dialysis | 15 (60,0) | 10 (40,0) | 0,4361 |
| Variable | ESBL positive n (%) |
ESBL negative n (%) | p value |
|---|---|---|---|
|
Transurethral Catheterization Yes No |
11 (61,1) 84 (51,9) |
7 (38,9) 78 (48,1) |
0,4551 |
|
Nephrostomy / Urethral Stent Yes No |
2 (100,0) 93 (52,2) |
085 (47,8) | 0,4992 |
|
Anatomical Defect Yes No |
5 (71,4) 90 (52,0) |
2 (28,6) 83 (48,0) |
0,4492 |
|
Neurogenic Bladder Yes No |
5 (55,6) 90 (52,6) |
4 (44,4) 81 (47,4) |
1,0002 |
|
Vesicoureteral reflux Yes No |
2 (100,0) 93 (52,2) |
085 (47,8) | 0,4992 |
|
BPH Yes No |
24 (63,2) 71 (50,0) |
14 (36,8) 71 (50,0) |
0,1491 |
|
Prostatitis Yes No |
1 (100,0) 94 (52,5) |
085 (47,5) | 1,0002 |
|
Urolithiasis Yes No |
14 (66,7) 81 (50,9) |
7 (33,3) 78 (49,1) |
0,1751 |
|
Uriner Intervention Yes No |
18 (75,0) 77 (49,4) |
6 (25,0) 79 (50,6) |
0,0191 |
|
Urine Culture E. coli Klebsiella spp. |
74 (52,1) 21 (55,3) |
68 (47,9) 17 (44,7) |
0,7301 |
|
Bacteremia Yes No |
22 (23,2) 73 (76,8) |
22 (25,9) 63 (74,1) |
0,6711 |
|
Hospitalization in the preceding month Yes No |
28 (80.0) 67 (46.2) |
7 (20.0) 78 (53.8) |
<0,0011 |
|
Antibiotic exposure in the previous three months Yes No |
47 (67.1) 48 (43.6) |
23 (32.9) 62 (56.4) |
0,0021 |
| History of urinary tract infection within the previous year Yes No |
29 (60.4) 66 (50.0) |
19 (39.6) 66 (50.0) |
0,2161 |
|
Hospitalization Duration (days) Mean±SD |
7,9 ± 2,5 |
7,3 ± 2,2 |
0,0783 |
| Title 1 | Day of admission | Day 3 of treatment | Day of discharge | p value |
|---|---|---|---|---|
| WBC (mean±SD) | 13,9 ± 6,2 | 9,1 ± 4,4 | 8,6 ± 3,7 | <0,0011 |
| CRP (mean±SD) | 140,7 ± 93,8 | 99,7 ± 76,3 | 29,2 ± 27,1 | <0,0011 |
| PCT (mean±SD) | 5,1 ± 9,0 | 4,0 ± 7,9 | 0,4 ± 0,4 | <0,0011 |
| Creatinin (mean±SD) | 1,5 ± 1,5 | 1,1 ± 0,7 | 1,0 ± 0,8 | <0,0011 |
| GFR (mean±SD) | 59,7 ± 30,9 | 71,0 ± 32,8 | 75,8 ± 31,5 | <0,0011 |
| Complete urine t | 146,3 ± 73,7 | 17,4 ± 42,6 | - | <0,0012 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




