Submitted:
13 January 2026
Posted:
14 January 2026
You are already at the latest version
Abstract
Keywords:
Introduction
Methods
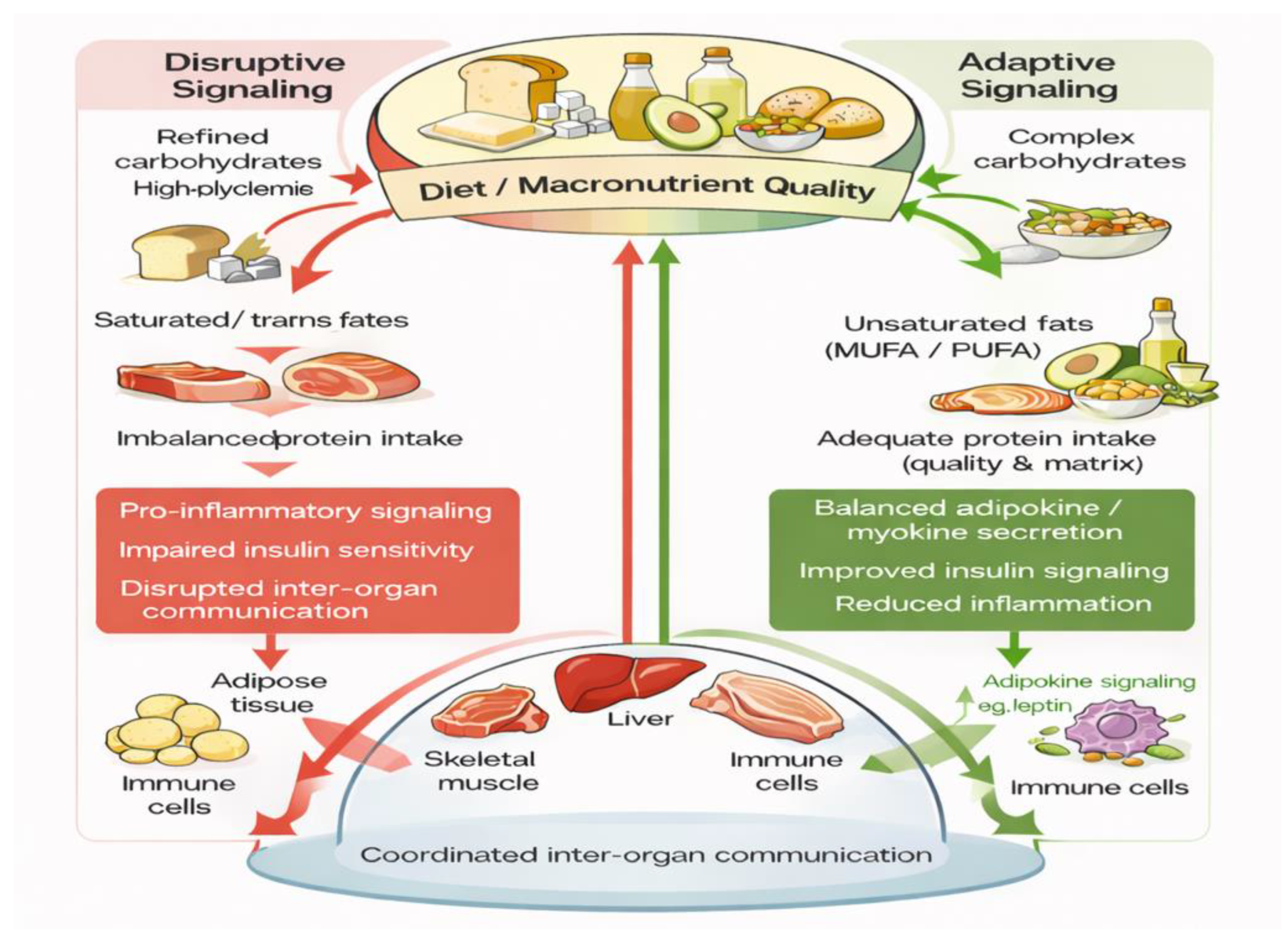
Nutrition as a Modulator of Tissue Crosstalk
Macronutrients and Tissue Communication
Carbohydrate Quality and Metabolic Signaling
Dietary Fat Quality and Inter-Organ Crosstalk
Protein Intake and Metabolic Communication
Conclusion and Future Perspectives
Funding
Acknowledgments
Conflicts of Interest
References
- Hotamisligil, G.S. Inflammation, metaflammation and immunometabolic disorders. Nature 2017, 542, 177–185. [Google Scholar] [CrossRef]
- Oishi, Y.; Manabe, I. Organ system crosstalk in cardiometabolic disease in the age of multimorbidity. Front Cardiovasc Med. 2020, 7, 64. [Google Scholar] [CrossRef]
- Samuel, V.T.; Shulman, G.I. The pathogenesis of insulin resistance: integrating signaling pathways and substrate flux. J Clin Invest. 2016, 126, 12–22. [Google Scholar] [CrossRef] [PubMed]
- Lee, Y.S.; Wollam, J.; Olefsky, J.M. An integrated view of immunometabolism. Cell Metab. 2018, 27, 933–944. [Google Scholar] [CrossRef]
- Bishop, E.L.; Gudgeon, N.; Dimeloe, S. Control of T cell metabolism by cytokines and hormones. Front Immunol. 2021, 12, 653605. [Google Scholar] [CrossRef]
- Tilg, H.; Moschen, A.R. Evolution of inflammation in nonalcoholic fatty liver disease: the multiple parallel hits hypothesis. Hepatology 2010, 52, 1836–1846. [Google Scholar] [CrossRef]
- Katagiri, H. Inter-organ communication involved in metabolic regulation at the whole-body level. Inflamm Regen. 2023, 43, 60. [Google Scholar] [CrossRef]
- Priest, C.; Tontonoz, P. Inter-organ cross-talk in metabolic syndrome. Nat Metab. 2019, 1, 1177–1188. [Google Scholar] [CrossRef] [PubMed]
- Castillo-Armengol, J.; Fajas, L.; Lopez-Mejia, I.C. Inter-organ communication: a gatekeeper for metabolic health. EMBO Rep. 2019, 20, e47903. [Google Scholar] [CrossRef] [PubMed]
- de Oliveira Dos Santos, A.R.; de Oliveira Zanuso, B.; Miola, V.F.B.; et al. Adipokines, myokines, and hepatokines: crosstalk and metabolic repercussions. Int J Mol Sci. 2021, 22, 2639. [Google Scholar] [CrossRef]
- Saponaro, F.; Bertolini, A.; Baragatti, R.; et al. Myokines and microbiota: new perspectives in the endocrine muscle–gut axis. Nutrients 2024, 16, 4032. [Google Scholar] [CrossRef] [PubMed]
- Fan, Y.; Pedersen, O. Gut microbiota in human metabolic health and disease. Nat Rev Microbiol. 2021, 19, 55–71. [Google Scholar] [CrossRef]
- Feng, W.; Liu, J.; Cheng, H.; et al. Dietary compounds in modulation of gut microbiota-derived metabolites. Front Nutr. 2022, 9, 939571. [Google Scholar] [CrossRef]
- Ridlon, J.M.; Kang, D.J.; Hylemon, P.B.; Bajaj, J.S. Bile acids and the gut microbiome. Curr Opin Gastroenterol. 2014, 30, 332–338. [Google Scholar] [CrossRef]
- Agus, A.; Clément, K.; Sokol, H. Gut microbiota-derived metabolites as central regulators in metabolic disorders. Gut 2021, 70, 1174–1182. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Tan, Y.; Cheng, H.; et al. Functions of gut microbiota metabolites: current status and future perspectives. Aging Dis. 2022, 13, 1106–1126. [Google Scholar] [CrossRef]
- Chai, W.; Maskarinec, G.; Lim, U.; et al. Association of habitual intake of probiotic supplements and yogurt with characteristics of the gut microbiome in the multiethnic cohort adiposity phenotype study. Gut Microbiome 2023, 4, e14. [Google Scholar] [CrossRef]
- Thom, G.; Lean, M. Is there an optimal diet for weight management and metabolic health? Gastroenterology 2017, 152, 1739–1751. [Google Scholar] [CrossRef]
- Ludwig, D.S.; Willett, W.C.; Volek, J.S.; Neuhouser, M.L. Dietary fat: from foe to friend? Science 2018, 362, 764–770. [Google Scholar] [CrossRef]
- Farris, K.M.; Senior, A.M.; Sobreira, D.R.; et al. Dietary macronutrient composition impacts gene regulation in adipose tissue. Commun Biol. 2024, 7, 194. [Google Scholar] [CrossRef] [PubMed]
- Ludwig, D.S.; Ebbeling, C.B. The carbohydrate–insulin model of obesity: beyond “calories in, calories out”. JAMA Intern Med. 2018, 178, 1098–1103. [Google Scholar] [CrossRef] [PubMed]
- Mehran, A.E.; Templeman, N.M.; Brigidi, G.S.; et al. Hyperinsulinemia drives diet-induced obesity independently of brain insulin production. Cell Metab. 2012, 16, 723–737. [Google Scholar] [CrossRef]
- Mozaffarian, D. Dietary and policy priorities for cardiovascular disease, diabetes, and obesity. Circulation 2016, 133, 187–225. [Google Scholar] [CrossRef]
- Dimitriadis, G.D.; Maratou, E.; Kountouri, A.; et al. Regulation of postabsorptive and postprandial glucose metabolism. Nutrients 2021, 13, 159. [Google Scholar] [CrossRef]
- Yang, W.; Jiang, W.; Guo, S. Regulation of macronutrients in insulin resistance and glucose homeostasis during type 2 diabetes mellitus. Nutrients 2023, 15, 4671. [Google Scholar] [CrossRef] [PubMed]
- Papakonstantinou, E.; Oikonomou, C.; Nychas, G.; Dimitriadis, G.D. Effects of diet and lifestyle on postprandial glycemia and insulin resistance. Nutrients 2022, 14, 823. [Google Scholar] [CrossRef] [PubMed]
- Wang, Y.; Fan, M.; Qian, H.; et al. Whole grain-derived functional ingredients against hyperglycemia. Crit Rev Food Sci Nutr. 2024, 64, 7268–7289. [Google Scholar] [CrossRef]
- Wu, T.; Rayner, C.K.; Jones, K.; Horowitz, M. Dietary effects on incretin hormone secretion. Vitam Horm. 2010, 84, 81–110. [Google Scholar]
- Nauck, M.A.; Müller, T.D. Incretin hormones and type 2 diabetes. Diabetologia 2023, 66, 1780–1795. [Google Scholar] [CrossRef]
- Park, S.Y.; Gautier, J.F.; Chon, S. Assessment of insulin secretion and insulin resistance in humans. Diabetes Metab J. 2021, 45, 641–654. [Google Scholar] [CrossRef]
- Grosso, G.; Laudisio, D.; Frias-Toral, E.; et al. Anti-inflammatory nutrients and obesity-associated metabolic inflammation. Nutrients 2022, 14, 1137. [Google Scholar] [CrossRef] [PubMed]
- Crick, D.C.P.; Halligan, S.L.; Davey Smith, G.; et al. Polyunsaturated fatty acids and inflammation. Int J Epidemiol. 2025, 54, dyaf065. [Google Scholar] [CrossRef]
- Radzikowska, U.; Rinaldi, A.O.; Çelebi Sözener, Z.; et al. Influence of dietary fatty acids on immune responses. Nutrients 2019, 11, 2990. [Google Scholar] [CrossRef] [PubMed]
- Silva Figueiredo, P.; Inada, A.C.; Marcelino, G.; et al. Fatty acid consumption and obesity-related disorders. Nutrients 2017, 9, 1158. [Google Scholar] [CrossRef]
- Ravaut, G.; Légiot, A.; Bergeron, K.F.; Mounier, C. Monounsaturated fatty acids in obesity-related inflammation. Int J Mol Sci. 2020, 22, 330. [Google Scholar] [CrossRef] [PubMed]
- Khan, I.; Hussain, M.; Jiang, B.; et al. Omega-3 long-chain polyunsaturated fatty acids: metabolism and health implications. J Food Compos Anal. 2023, 114, 104864. [Google Scholar] [CrossRef]
- Djuricic, I.; Calder, P.C. n-3 fatty acids (EPA and DHA) and cardiovascular health. Curr Atheroscler Rep. 2025, 27, 116. [Google Scholar] [CrossRef]
- Saban Güler, M.; Yıldıran, H.; Seymen, C.M. Effect of omega-3 fatty acids on adipose tissue in mice fed a high-fat diet. Sci Rep. 2025, 15, 37179. [Google Scholar] [CrossRef]
- Fernández-Galilea, M.; Félix-Soriano, E.; Colón-Mesa, I.; Moreno-Aliaga, M.J. Omega-3 fatty acids as regulators of brown/beige adipose tissue. J Physiol Biochem. 2020, 76, 251–267. [Google Scholar] [CrossRef]
- Jia, M.; Xu, T.; Xu, Y.J.; Liu, Y. Dietary fatty acids activate or deactivate brown and beige fat. Life Sci. 2023, 330, 121978. [Google Scholar] [CrossRef]
- Negroiu, C.E.; et al. Beyond the cold: activating brown adipose tissue to combat obesity. J Clin Med. 2024, 13, 1973. [Google Scholar] [CrossRef] [PubMed]
- Pahlavani, M.; et al. Eicosapentaenoic acid regulates brown adipose tissue metabolism. J Nutr Biochem. 2017, 39, 101–109. [Google Scholar] [CrossRef] [PubMed]
- Wolfe, R.R.; Church, D.D.; Ferrando, A.A.; Moughan, P.J. Role of protein quality in dietary protein recommendations. Front Nutr. 2024, 11, 1389664. [Google Scholar] [CrossRef]
- Petzke, K.J.; Freudenberg, A.; Klaus, S. Dietary protein beyond amino acids in obesity prevention. Int J Mol Sci. 2014, 15, 1374–1391. [Google Scholar] [CrossRef]
- Lin, Z.; Chang, C.; Zhao, S.; et al. Amino acids shape the metabolic and immunologic landscape in the tumor immune microenvironment. Cancer Biol Med. 2025, 22, 726–746. [Google Scholar]
- Mariotti, F.; Gardner, C.D. Dietary protein and amino acids in vegetarian diets. Nutrients 2019, 11, 2661. [Google Scholar] [CrossRef] [PubMed]
- Kaur, L.; Mao, B.; Beniwal, A.S.; et al. Alternative proteins vs animal proteins: influence of structure and processing. Trends Food Sci Technol. 2022, 122, 275–286. [Google Scholar] [CrossRef]
- Ajomiwe, N.; Boland, M.; Phongthai, S.; et al. Protein nutrition: structure, digestibility, and bioavailability. Foods 2024, 13, 1771. [Google Scholar] [CrossRef]
- Yuzbashian, E.; Fernando, D.N.; Jacobs, R.L.; et al. Effects of milk, yogurt, and cheese on metabolic outcomes in obese mice. Int J Mol Sci. 2025, 26, 5026. [Google Scholar] [CrossRef]
- Mendis, B.I.L.M.; Sarvananda, L.; Jayasinghe, T.N.; et al. Gut microbiota and type 2 diabetes: mechanisms and mediators. Med Microecol. 2025, 26, 100144. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.



