Submitted:
31 December 2025
Posted:
01 January 2026
You are already at the latest version
Abstract
The Bangladesh HCW Cohort is a prospective study established to assess the physical and psychological effects of COVID-19 on Bangladeshi HCWs. This paper outlines the study design and baseline characteristics of the cohort participants. The cohort was initiated in February 2021 and enrolled 3,697 HCWs. Baseline demographic, clinical, and occupational risk data were collected through face-to-face interviews. Participants were followed up biweekly to monitor changes in risk factors over time. Validated instruments were used to assess mental health outcomes and infection prevention and control practices. In January 2023, a second phase of the study was initiated to examine breakthrough COVID-19 infections, immune responses by vaccine type, long-term consequences of COVID-19, and booster vaccine uptake. The median age of the HCWs recruited to the cohort was 36 years (IQR: 30-44), and 53.5% were female. Nurses accounted for approximately half of the participants (47.8%), followed by support staff (31.8%) and physicians (20.4%). Nearly half of participants (47%) reported symptomatic COVID-19, most commonly fever (82%) and cough (56%). Additionally, 32% reported hospitalization due to COVID-19.The Bangladesh HCW Cohort provides a prospective platform to evaluate the occupational, physical, and psychological impacts of COVID-19 among HCWs, generating evidence to inform occupational health policy and workforce protection strategies in Bangladesh.
Keywords:
01. Introduction
2. Materials and Methods
2.1. Study site
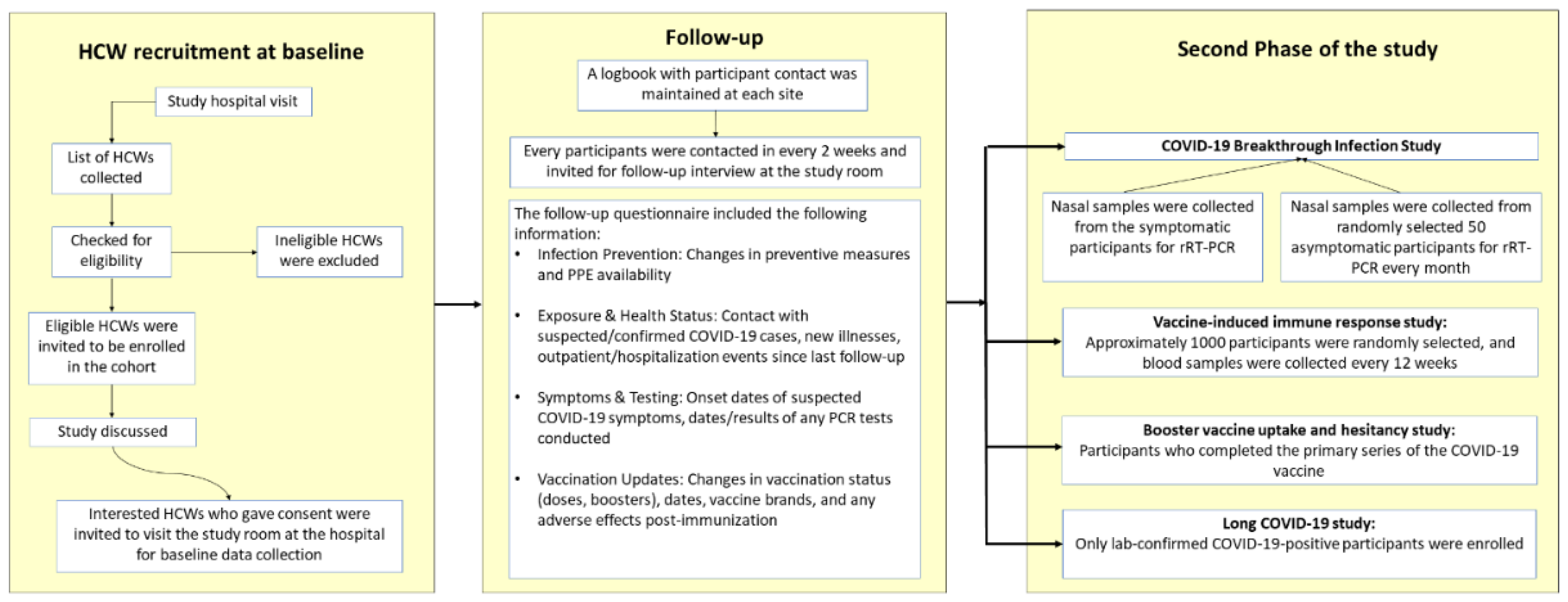
2.2. Participant enrollment
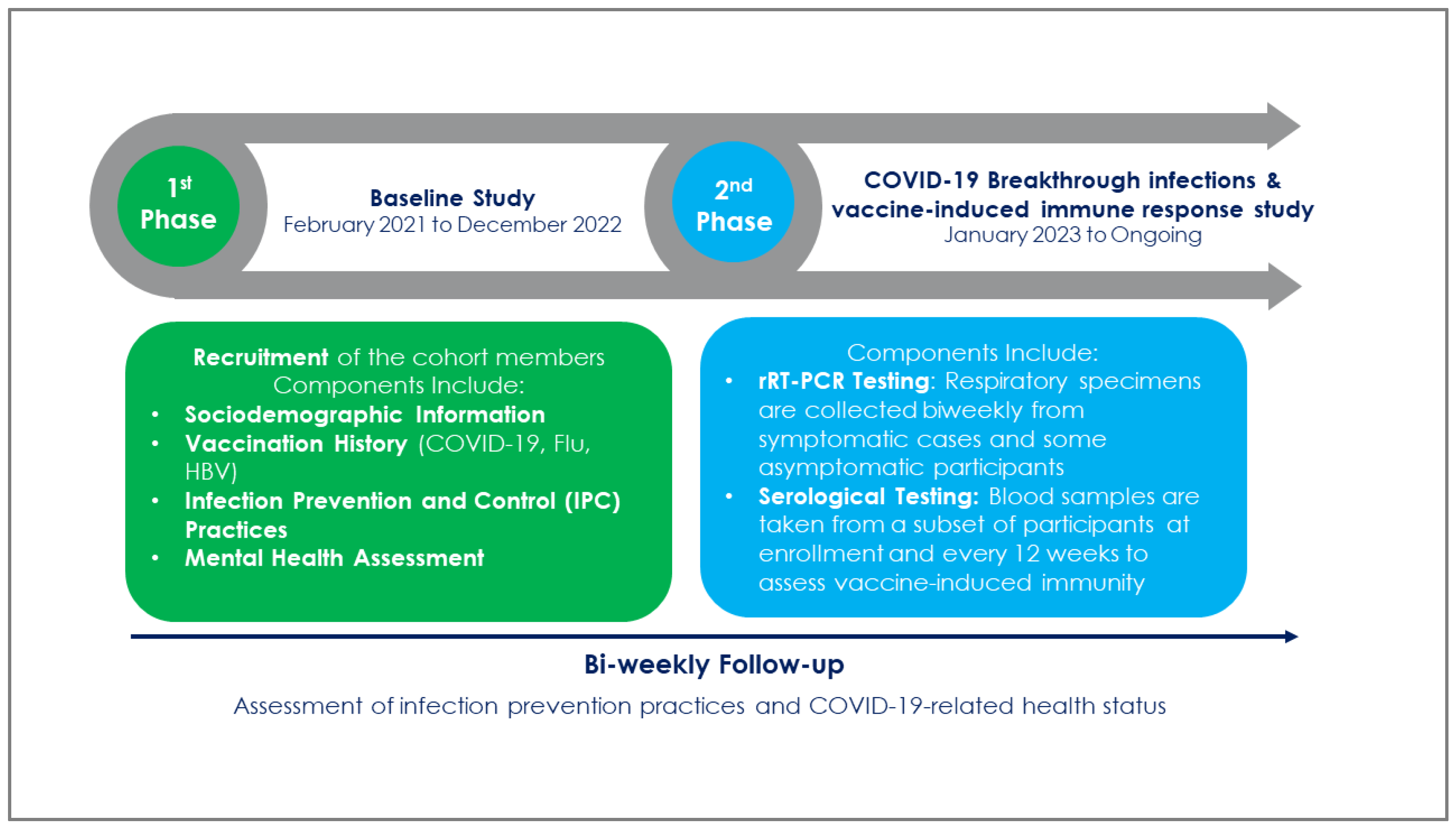
2.3. Phases and timelines of the cohort
2.4. Baseline information collection
2.5. Protocol for follow-up
2.6. Second phase of the study
3. Results
3.1. Characteristics of enrolled participants
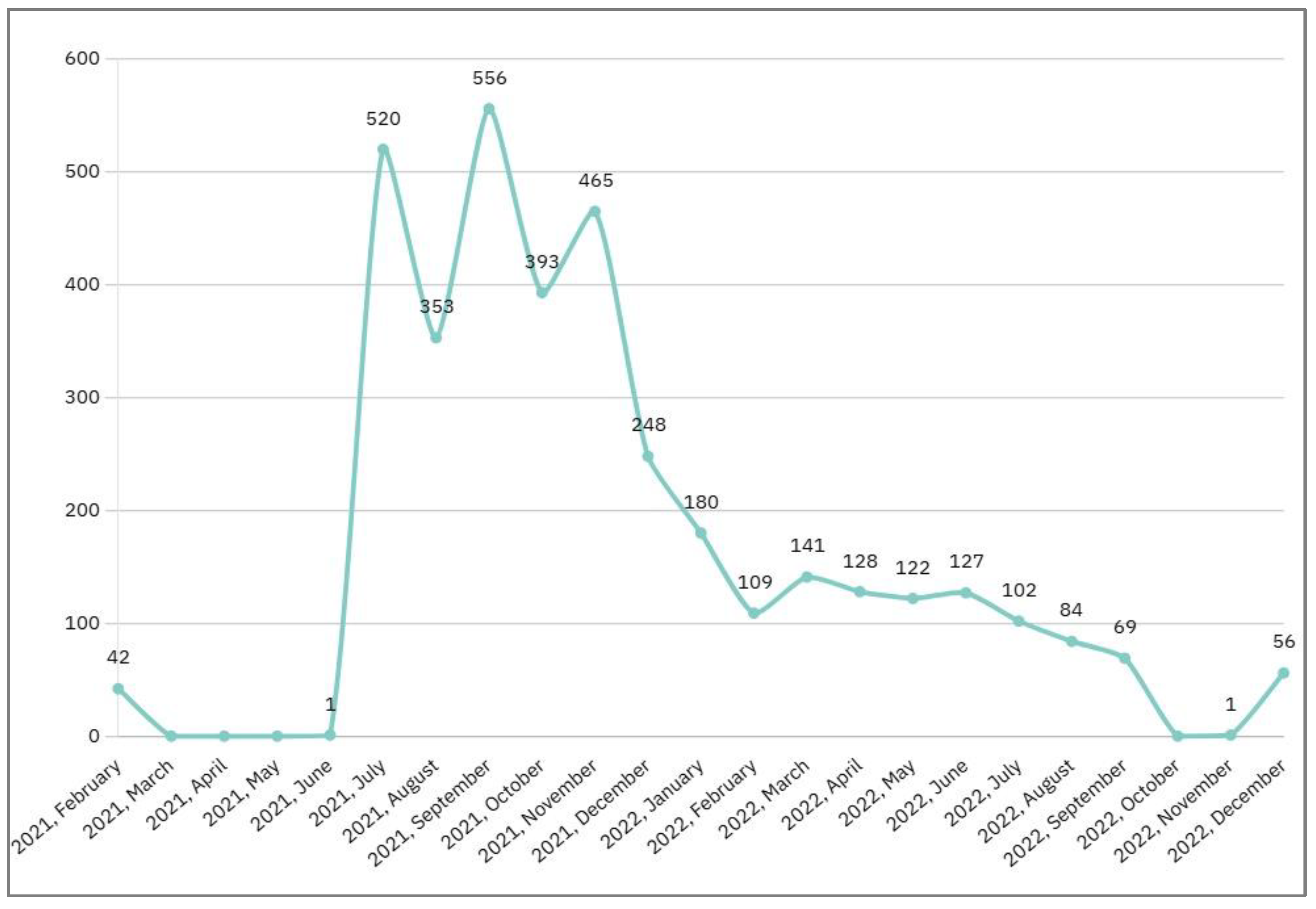
3.2. Follow-up implementation
3.3. COVID-19 illness among HCWs
4. Discussion
4.1. Patient and Public Involvement
4.2. Future research plans
4.3. Strengths and Limitations
4.4. Collaboration
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| HCW | Healthcare Worker |
| WHO | World Health Organization |
| PPE | Personal Protective Equipment |
| rRT-PCR | Real-time Reverse Transcription-Polymerase Chain Reaction. |
References
- WHO SAGE ROADMAP FOR PRIORITIZING USES OF COVID-19 VACCINES IN THE CONTEXT OF LIMITED SUPPLY [Internet]. SAGE Working Group on COVID-19 vaccines. 2020. Available online: https://www.who.int/docs/default-source/immunization/sage/covid/sage-prioritization-roadmap-covid19-vaccines.pdf (accessed on 17 August 2025).
- Wei, XS; Wang, XR; Zhang, JC; Yang, WB; Ma, WL; Yang, BH; et al. A cluster of health care workers with COVID-19 pneumonia caused by SARS-CoV-2. J Microbiol Immunol Infect. 2021, 54(1), 54–60. [Google Scholar] [CrossRef]
- Chew, NWS; Lee, GKH; Tan, BYQ; Jing, M; Goh, Y; Ngiam, NJH; et al. A multinational, multicentre study on the psychological outcomes and associated physical symptoms amongst healthcare workers during COVID-19 outbreak. Brain Behav Immun. 2020, 88, 559–65. [Google Scholar] [CrossRef]
- Preti, E; Di Mattei, V; Perego, G; Ferrari, F; Mazzetti, M; Taranto, P; et al. The Psychological Impact of Epidemic and Pandemic Outbreaks on Healthcare Workers: Rapid Review of the Evidence. Curr Psychiatry Rep. 2020, 22(8), 43. [Google Scholar] [CrossRef]
- Dzinamarira, T; Nkambule, SJ; Hlongwa, M; Mhango, M; Iradukunda, PG; Chitungo, I; et al. Risk Factors for COVID-19 Infection Among Healthcare Workers. A First Report From a Living Systematic Review and meta-Analysis. Saf Health Work. 2022, 13(3), 263–8. [Google Scholar] [CrossRef]
- World Health Organization. Health and Care Worker Deaths during COVID-19 2021. Available online: https://www.who.int/news/item/20-10-2021-health-and-care-worker-deaths-during-covid-19#:~:text=WHO%20estimates%20that%20between%2080,in%20the%20world’s%20pandemic%20response (accessed on 17 August 2025).
- Rahman, A; Abdulla, F; Karimuzzaman, M; Hossain, MM. Burden of COVID-19 on health and wellbeing, education, and economy of Bangladesh. Clinical Case Reports 2022, 10(11), e6639. [Google Scholar] [CrossRef] [PubMed]
- Opu, MH. Over 180 doctors killed due to coronavirus in Bangladesh. Dhaka Tribune. 2021. Available online: https://www.dhakatribune.com/bangladesh/health/256664/over-180-doctors-killed-due-to-coronavirus-in (accessed on 17 August 2025).
- Rahman, MS; Farzana, M; Rahman, T. Occupational Challenges and Physician Deaths During COVID-19 Pandemic. International Journal of Travel Medicine and Global Health 2021, 9(2), 100–1. [Google Scholar] [CrossRef]
- Cousins, S. Bangladesh’s COVID-19 testing criticised. The Lancet 2020, 396(10251), 591. [Google Scholar] [CrossRef]
- Rahaman, KR; Mahmud, MS; Mallick, B. Challenges of Testing COVID-19 Cases in Bangladesh. International Journal of Environmental Research and Public Health 2020, 17(18), 6439. [Google Scholar] [CrossRef]
- Islam, MT; Talukder, AK; Siddiqui, MN; Islam, T. Tackling the COVID-19 pandemic: The Bangladesh perspective. J Public Health Res. 2020, 9(4), 1794. [Google Scholar] [CrossRef] [PubMed]
- Sakib, SN. Bangladesh: Low COVID-19 testing rate raises concerns. Anadolu Agency. 2020. Available online: https://www.aa.com.tr/en/asia-pacific/bangladesh-low-covid-19-testing-rate-raises-concerns/1810132 (accessed on 17 August 2025).
- Chen, X; Huang, Z; Wang, J; Zhao, S; Wong, MC; Chong, KC; et al. Ratio of asymptomatic COVID-19 cases among ascertained SARS-CoV-2 infections in different regions and population groups in 2020: a systematic review and meta-analysis including 130 123 infections from 241 studies. BMJ Open. 2021, 11(12), e049752. [Google Scholar] [PubMed]
- Sah, P; Fitzpatrick, MC; Zimmer, CF; Abdollahi, E; Juden-Kelly, L; Moghadas, SM; et al. Asymptomatic SARS-CoV-2 infection: A systematic review and meta-analysis. Proc Natl Acad Sci U S A 2021, 118(34). [Google Scholar]
- Ma, Q; Liu, J; Liu, Q; Kang, L; Liu, R; Jing, W; et al. Global Percentage of Asymptomatic SARS-CoV-2 Infections Among the Tested Population and Individuals With Confirmed COVID-19 Diagnosis: A Systematic Review and Meta-analysis. JAMA Netw Open. 2021, 4(12), e2137257. [Google Scholar] [CrossRef]
- Syangtan, G; Bista, S; Dawadi, P; Rayamajhee, B; Shrestha, LB; Tuladhar, R; et al. Asymptomatic SARS-CoV-2 Carriers: A Systematic Review and Meta-Analysis. Front Public Health 2020, 8, 587374. [Google Scholar] [CrossRef]
- World Health Organization. WHO SAGE roadmap for prioritizing uses of COVID-19 vaccines: an approach to optimize the global impact of COVID-19 vaccines, based on public health goals, global and national equity, and vaccine access and coverage scenarios, first issued 20 October 2020, updated: 13 November 2020, updated: 16 July 2021, latest update: 21 January 2022; World Health Organization: Geneva, 2022; Contract No.: WHO/2019-nCoV/Vaccines/SAGE/Prioritization/2022.1. [Google Scholar]
- Population-based age-stratified seroepidemiological investigation protocol for coronavirus 2019 (COVID-19) infection [Internet]. 2020. Available online: https://iris.who.int/bitstream/handle/10665/332188/WHO-2019-nCoV-Seroepidemiology-2020.2-eng.pdf?sequence=1 (accessed on 17 August 2025).
- Chen, H; Wang, B; Cheng, Y; Muhammad, B; Li, S; Miao, Z; et al. Prevalence of posttraumatic stress symptoms in health care workers after exposure to patients with COVID-19. Neurobiology of Stress. 2020, 13, 100261. [Google Scholar] [CrossRef]
- Giusti, EM; Pedroli, E; D’Aniello, GE; Stramba Badiale, C; Pietrabissa, G; Manna, C; et al. The Psychological Impact of the COVID-19 Outbreak on Health Professionals: A Cross-Sectional Study. In Frontiers in Psychology; 2020. [Google Scholar]
- Cheng, SKW; Wong, CW; Tsang, J; Wong, KC. Psychological distress and negative appraisals in survivors of severe acute respiratory syndrome (SARS). Psychological Medicine 2004, 34(7), 1187–95. [Google Scholar] [CrossRef]
- Repon, MAU; Pakhe, SA; Quaiyum, S; Das, R; Daria, S; Islam, MR. Effect of COVID-19 pandemic on mental health among Bangladeshi healthcare professionals: A cross-sectional study. Sci Prog. 2021, 104(2), 368504211026409. [Google Scholar] [CrossRef] [PubMed]
- Tasnim, R; Sujan, MSH; Islam, MS; Ritu, AH; Siddique, MAB; Toma, TY; et al. Prevalence and correlates of anxiety and depression in frontline healthcare workers treating people with COVID-19 in Bangladesh. BMC Psychiatry 2021, 21(1), 271. [Google Scholar] [CrossRef] [PubMed]
- Darboe, SMK; Darfour-Oduro, SA; Kpene, GE; Kebbeh, A; Fofana, N; Ndow, M; et al. Factors influencing healthcare workers’ perceived compliance with infection prevention and control standards, North Bank East region, The Gambia, a cross-sectional study. BMC Research Notes 2025, 18(1), 43. [Google Scholar] [CrossRef] [PubMed]
- Alqahtani, N; Elmahboub, R; Al-Qahtani, F; Qahtani, S; Eldeeb, S; Margan, A; et al. Assessment of Healthcare Workers’ Adherence to Infection Prevention and Control Measures in Najran City, Saudi Arabia, in the Post-COVID-19 Pandemic Era. Journal of Pure and Applied Microbiology 2024, 18. [Google Scholar] [CrossRef]
- El-Ghitany, E; Elrewany, E; Omran, E; Farghaly, A; Azzam, N. Self-reported adherence of healthcare workers to infection prevention and control practices during the early waves of the COVID-19 pandemic in Egypt. International Journal of Infection Control 2023. [Google Scholar] [CrossRef]
- Weldetinsae, A; Alemu, ZA; Tefaye, K; Gizaw, M; Alemahyehu, E; Tayachew, A; et al. Adherence to infection prevention and control measures and risk of exposure among health-care workers: A cross-sectional study from the early period of COVID-19 pandemic in Addis Ababa, Ethiopia. Health Sci Rep. 2023, 6(6), e1365. [Google Scholar] [CrossRef]
- Babore, GO; Eyesu, Y; Mengistu, D; Foga, S; Heliso, AZ; Ashine, TM. Adherence to Infection Prevention Practice Standard Protocol and Associated Factors Among Healthcare Workers. Glob J Qual Saf Healthc 2024, 7(2), 50–8. [Google Scholar] [CrossRef] [PubMed]
- Wee, LEI; Conceicao, EP; Tan, JY; Magesparan, KD; Amin, IBM; Ismail, BBS; et al. Unintended consequences of infection prevention and control measures during COVID-19 pandemic. American Journal of Infection Control 2021, 49(4), 469–77. [Google Scholar] [CrossRef]
- World Health Organization. WHO COVID-19 Case definition 2022. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-Surveillance_Case_Definition-2022.1 (accessed on 17 December 2025).
- World Health Organization. Global COVID-19 Clinical Platform Case Report Form (CRF) for Post COVID condition (Post COVID-19 CRF). 2021. [Google Scholar]
- World Health Organization. Delivered by women, led by men: A gender and equity analysis of the global health and social workforce. Human Resources for Health Observer Series No. 24 2019. [Google Scholar]
- International Labour Organization. Care work and care jobs for the future of decent work. 2018. [Google Scholar]
- Lan, FY; Wei, CF; Hsu, YT; Christiani, DC; Kales, SN. Work-related COVID-19 transmission in six Asian countries/areas: A follow-up study. PLoS One 2020, 15(5), e0233588. [Google Scholar] [CrossRef]
- Nguyen, LH; Drew, DA; Graham, MS; Joshi, AD; Guo, CG; Ma, W; et al. Risk of COVID-19 among front-line health-care workers and the general community: a prospective cohort study. Lancet Public Health 2020, 5(9), e475–e83. [Google Scholar] [CrossRef] [PubMed]
- Shanafelt, T; Ripp, J; Trockel, M. Understanding and Addressing Sources of Anxiety Among Health Care Professionals During the COVID-19 Pandemic. JAMA 2020, 323(21), 2133–4. [Google Scholar] [CrossRef] [PubMed]
- Brooks, SK; Webster, RK; Smith, LE; Woodland, L; Wessely, S; Greenberg, N; et al. The psychological impact of quarantine and how to reduce it: rapid review of the evidence. The Lancet 2020, 395(10227), 912–20. [Google Scholar] [CrossRef]
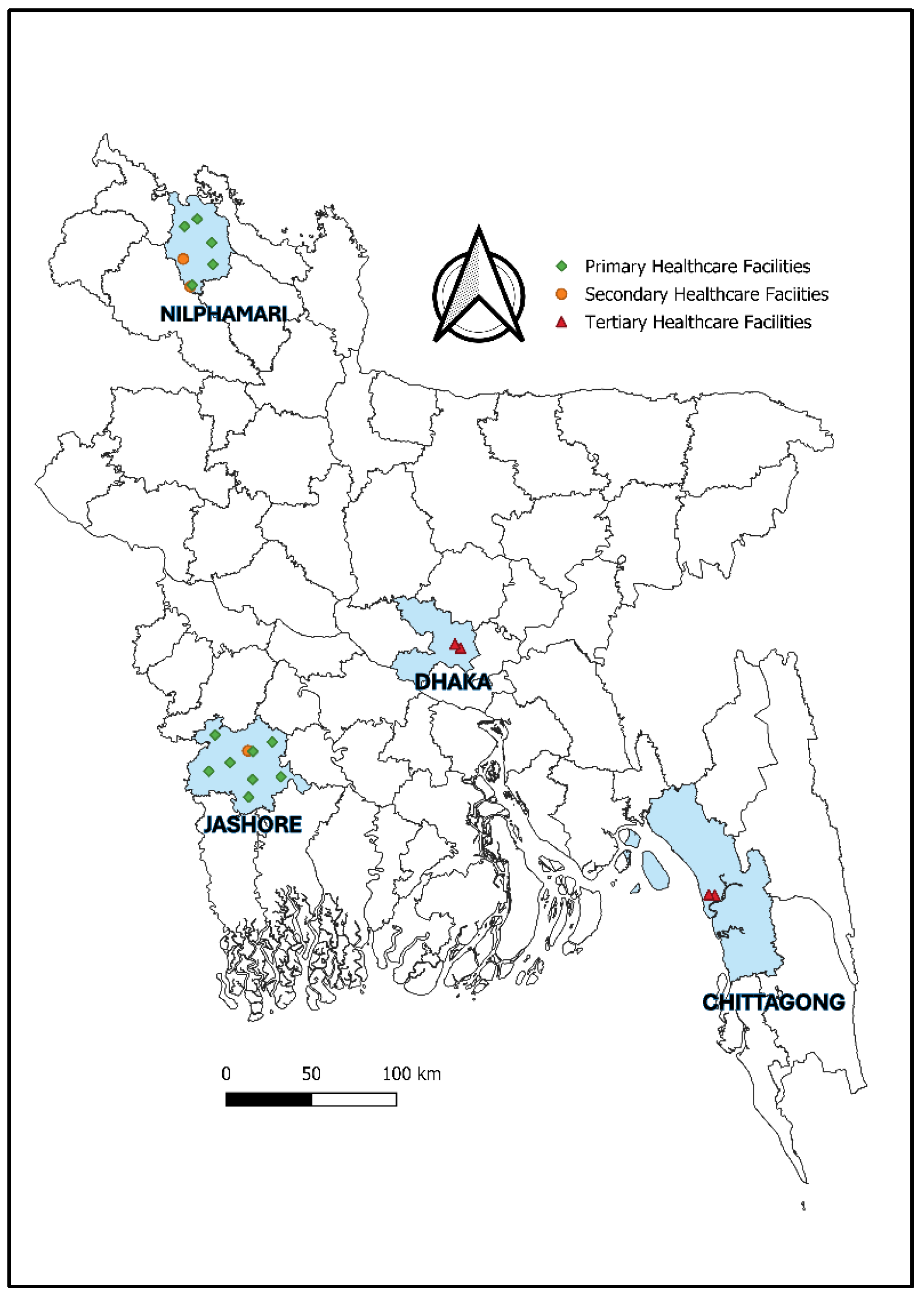
| Administrative division | District | Facility level | Administration | Hospitals/Facilities |
|---|---|---|---|---|
| Dhaka | Dhaka | Tertiary | Public | Shaheed Suhrawardy Medical College Hospital (SMCH) |
| Tertiary | Private | Holy Family Red Crescent Medical College Hospital | ||
| Chittagong | Chittagong | Tertiary | Public | Chittagong Medical College Hospital (CMCH) |
| Tertiary | Private | USTC Bangabandhu Memorial Hospital | ||
| Khulna | Jashore | Secondary | Public | Jashore District Hospital |
| Primary | Public | Seven upazila health complexes in Jashore | ||
| Primary | Public | Seventy community clinics in Jashore | ||
| Rangpur | Nilphamari | Secondary | Public | Nilphamari District Hospital |
| Saidpur 100-Bed Hospital | ||||
| Primary | Public | Five upazila health complexes in Nilphamari | ||
| Primary | Public | Fifty community clinics in Nilphamari |
| Characteristics | Construct | Instruments | Description/Domains assessed |
|---|---|---|---|
| Individual | Sociodemographic characteristics | Semi-structured contextualized questionnaire | Age, sex, ethnicity, religion, marital status, family type and size, education |
| Physical measurements | Blood pressure, anthropometric measurements, blood glucose | ||
| Professional information | HCW type, Type of the healthcare facility, working department, working hours | ||
| Female health | Pregnancy status | ||
| Behavioural information | Tobacco consumption | ||
| Clinical characteristics | Personal medical and drug history, COVID-19-related symptoms, diagnosis, treatment, and hospitalization history | ||
| Occupational information | Exposure to COVID-19 patients, use of PPE | ||
| Vaccination information | Number of doses and date of receipt of the COVID-19 vaccine, side effects following the COVID-19 vaccination, History of vaccination against Influenza and Hepatitis B Virus | ||
| COVID-19 booster vaccine acceptance | Protection Motivation Theory (PMT) scale | Perceived severity, perceived vulnerability, response efficacy, self-efficacy, response costs, intrinsic/extrinsic rewards, | |
| Vaccine Hesitancy (VH) scale | Confidence, complacency, constraints, collective responsibility | ||
| Mental health assessment | Patient Health Questionnaire (PHQ-9) | Assess the severity of depressive symptoms over the past 2 weeks | |
| Generalized Anxiety Disorder (GAD-7) | Assess the severity of generalized anxiety over the past 2 weeks | ||
| Perceived Stress Scale (PSS) | Measure how unpredictable, uncontrollable, and overloaded individuals find their lives | ||
| Pittsburgh Sleep Quality Index (PSQI) | Assess sleep quality and disturbances over a 1-month interval | ||
| 12-Item Short Form Survey (SF-12) | Evaluate physical and mental health status across eight domains (Physical functioning, Role physical, Bodily pain, General health, Vitality, Role emotional, Social functioning, Mental health) | ||
| IPC assessment | WHO hand hygiene observation tools, contextualized observational checklist, structured questionnaire | Assess healthcare workers’ compliance with the “5 Moments for Hand Hygiene” through direct observation, Knowledge, attitude, and practices towards IPC adherence | |
| Long COVID assessment | WHO’s post COVID-19 CRF | Symptoms, clinical history, and functional status in individuals recovering from COVID-19 | |
| Facility level | IPC assessment | WHO facility assessment tool (IPCAF) | Assess IPC practices and capacity at the facility level across eight core components (IPC program, guidelines, education and training, Healthcare-Associated Infection (HAI) Surveillance, Multimodal Strategies, Monitoring/Audit of IPC Practices and Feedback, Workload, Staffing, and Bed Occupancy, Built Environment, and Materials, and Equipment for IPC) |
| Construct | Instruments | Description |
|---|---|---|
| Development of any symptoms of acute illness since the last interview | Semi-structured contextualized questionnaire | No symptoms, Fever, Cough, Difficulty breathing, Sore throat, Runny nose, Chills, Vomiting, Nausea, Diarrhea, Headache, Rash, Conjunctivitis, Muscle aches, Joint ache, Loss of appetite, Loss of smell, Loss of taste, Nose bleed, Fatigue, Seizures, Altered consciousness, Other symptoms, Date of onset of symptom |
| COVID-19 testing for an illness episode | Tested or not for the episode, What type of test (rRT-PCR/Rapid Ag/Serology), Test result | |
| Vaccination status | Number of doses and date of receipt of the COVID-19 vaccine/COVID-19 booster vaccine, side effects following the COVID-19 vaccination | |
| Healthcare seeking for any illness episode | Hospital outpatient/emergency visit since last inteview, data of visit, diagnosis, required hospitalization or not, diagnosis followed by hospitalization, supply of oxygen needed during hospitalization or not, required ICU/CCU, duration of ICU stay (in days), Total hospitalization stay duration (including ICU), developed any complication, what was the complication, outcome of illness followed by hospitalization during last two-week, date of outcome. | |
| Mental health follow-up | Brief mental health symptom screening (PHQ-2, GAD-2), sleep quality, and self-rated health | |
| Occupational information | Exposure to COVID-19 patients, In which ward/setting the HCW got exposed to COVID-19 patients, use of PPE, involvement in aerosol-generating procedure, hand hygiene practice, contact with patients’ body fluids | |
| Professional and Clinical role-related information | HCW type, Type of the healthcare facility, working department, working hours |
| Socio-demographic characteristics | n (%) |
|---|---|
| Total number of HCWs | 3697 |
| Age in years | |
| Median (IQR) | 36 (30-44) |
| Sex | |
| Female | 1980 (53.5) |
| Worker type | |
| Nurse | 1769 (47.8) |
| Doctor | 809 (20.4) |
| Ward Boy/Aya | 440 (11.9) |
| Health Assistant | 229 (6.2) |
| Cleaner | 158 (4.3) |
| CHCP | 125 (3.4) |
| Medical Technologist (Lab) | 79 (2.1) |
| Lab Attendant | 30 (0.8) |
| Medical Technologist (Others) | 29 (0.8) |
| Receptionist | 17 (0.4) |
| Ambulance Driver | 12 (0.3) |
| COVID-19 illness | n (%) |
|---|---|
| Symptomatic COVID-19 | 1725 (47) |
| Single episode | 1474 (40) |
| Two or more episodes | 251 (7) |
| Lab confirmed COVID-19 | 1117 (30) |
| PCR positive | 984 (88) |
| Rapid antigen positive | 180 (16) |
| Common symptoms among lab-confirmed cases (n=1117) | |
| Fever | 913 (82) |
| Cough | 630 (56) |
| Runny nose | 371 (33) |
| Sore throat | 312 (28) |
| Difficulty breathing | 200 (18) |
| Hospitalized (n=1117) | 356 (32) |
| Duration of hospitalization (Median, IQR) | 12 7-14) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




