1. Introduction
Pediatric palliative care is a multidisciplinary approach aimed at alleviating the physical, psychological, and social suffering of children with life-limiting conditions and supporting their families[
1]. While pediatric palliative care is well established in high-income countries, services in low- and middle-income settings remain underdeveloped[
2].
In Mexico, leading causes of pediatric mortality include cancer, neurological disorders, and congenital anomalies, with respective rates of 5.0, 3.8, and 3.7 deaths per 100,000 children[
3]. Despite this burden, few hospitals offer structured pediatric palliative care programs. Families in these contexts often face additional socioeconomic and logistical stressors that worsen their quality of life.
Although most pediatric palliative care models are cancer-focused, children with other chronic, disabling conditions may have prolonged disease courses and complex care needs that warrant tailored palliative support.
The aim of this study was to evaluate the effectiveness of a pediatric palliative care program in improving the quality of life trajectories of pediatric patients and their families. Demographic and clinical factors influencing changes in quality of life over time were also examined.
2. Materials and Methods
This prospective cohort study took place at the Hospital Infantil de México Federico Gómez, a tertiary referral center. Children aged 0–18 years with life-limiting or disabling conditions were referred to the pediatric palliative care Unit by their treating physicians. The unit offers integrated medical, psychological, and social care, along with home visits and phone follow-up. Medical equipment is loaned to families in the Mexico City metropolitan area.
Upon enrollment, each family underwent a multidimensional assessment conducted by a pediatrician, psychologist, and social worker. Individualized goals and care plans were developed, focusing on symptom control, caregiver education, and coordination with local health services. Baseline information and demographic data were collected at the hospital for every new patient enrolled between July 1, 2021, and February 28, 2025. Telephone interviews were conducted at 3 and 6 months to assess the quality of life of both patients and their families.
Instruments: Quality of life was assessed using validated Spanish-language instruments: the PedsQL™ 3.0 Cancer Module for children aged 2–18 with cancer, and the
PedsQL™ 2.0 Family Impact Module for caregivers of all patients. Both use a 0–100 scale, with higher scores reflecting better quality of life [
4,
5,
6,
7,
8,
9,
10,
11]. Socioeconomic status was classified using the Mexican Association of Market and Opinion Intelligence (AMAI) index, which categorizes households from D (lowest) to AB (highest) based on education, housing, and access to resources [
12].
Analysis: Repeated measures ANOVA was used to assess changes in quality of life over time. Multilevel mixed-effects models were employed to examine interactions between quality of life trajectories and zone of residence (Mexico City metropolitan area vs. non-metropolitan), socioeconomic status (AMAI D level vs. higher), and diagnostic category (neurologic, oncologic, and others). All statistical analyses and visualizations were conducted using Stata/MP version 14.0 (StataCorp, College Station, TX, USA).
3. Results
A total of 186 patients were enrolled. The median age was 8.8 years (range: 0–18), and 57.5% were male. Most patients (n = 139, 74.7%) had an oncological diagnosis. Other conditions included neurological disorders (n = 24, 12.9%) and cardiopathies (n = 10, 5.4%). Most participants (63.1%) resided in Mexico City or the surrounding metropolitan area. Among those with available socioeconomic data, 73% belonged to the lowest two AMAI categories (D and D+) (
Table S1).
At baseline, the 116 oncological patients who completed the PedsQL Cancer Module had a mean score of 58.9 points. At three and six months, scores increased to 68.4 and 77.9, respectively (p < 0.001), with significant improvements observed across all subscales. The domains showing the greatest improvement were pain, procedural anxiety, and communication.
Table 1; Figure S1.
Participants in the lower socioeconomic strata (AMAI categories D and D+) tended to have lower baseline PedsQL Cancer Module scores than those in higher AMAI categories (mean difference: -8.7 points; p = 0.079). No significant associations were observed between baseline PedsQL Cancer Module scores and sex, age group, neoplasm type, or place of residence.
Caregivers of 166 children completed the PedsQL™ 2.0 Family Impact Module. Total scores improved from 60.1 to 78.8 over a six-month period (p < 0.001), with significant gains in the emotional, cognitive, and family relationship domains.
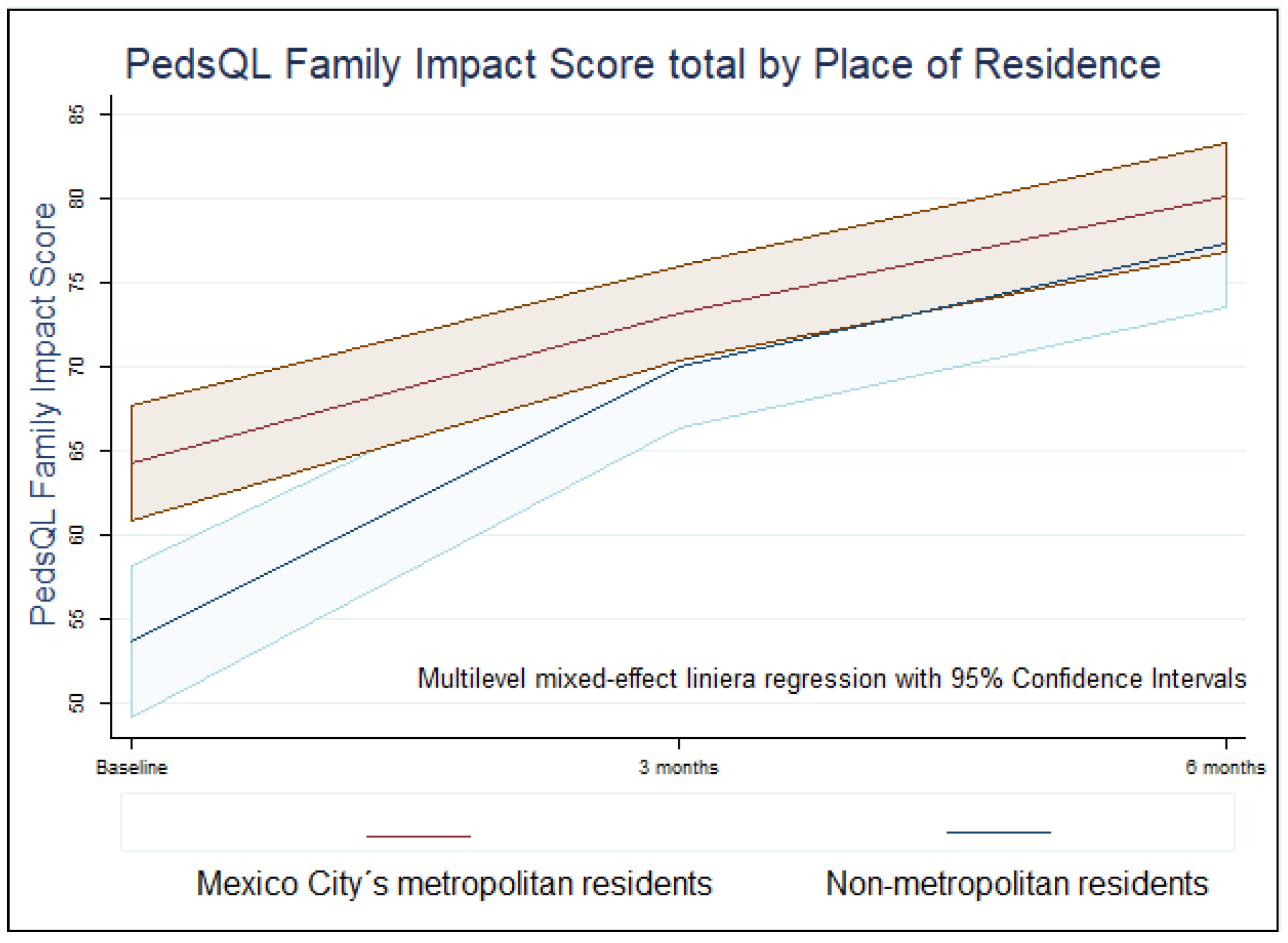
Table S2; Figure S2. Repeated measures ANOVA showed interaction between time and zone of residence (p=0.008) and between time and diagnostic classification (p=0.03). Families living outside the Mexico City metropolitan area had lower baseline scores but showed greater improvements over time.
Figure 1. Similarly, families of children with cancer showed larger quality of life gains than those with neurologic or other chronic conditions.
The median follow-up per participant was 9.3 months (range: 0.03–87.6 months). A total of 70 patients died during the study period, with an overall median survival time of 13.3 months, varying by diagnosis. Patients with non-intracranial neoplasms survived a median of 6.6 months, whereas those with neurological conditions or intracranial neoplasms had a median survival of 39 months.
Figure S3. Most patients (68.7%) died at home, while the remainder died in hospital. No association was found between diagnosis, place of residence, or socioeconomic status and the place of death.
4. Discussion
This study demonstrates that structured pediatric palliative care services can significantly improve quality of life for children and families in a middle-income country. Our findings are consistent with global data showing that early palliative interventions improve symptom management and reduce psychosocial burden.
An unexpected finding of our study was a significantly greater improvement in quality of life among families living outside the Mexico City metropolitan area than among those residing in the same city as the hospital. This may be explained by reduced travel burdens and fewer hospital visits following enrollment in the pediatric palliative care program. These findings support the decentralization of services and suggest a potential role for telehealth and community-based outreach programs in improving access to care. Strategies for delivering palliative care to families living remotely from tertiary care centers have been explored in low- and middle-income countries. Such strategies involve providers from various settings, including volunteers and local health services, and have shown promising outcomes [
13,
14]
Families of children with neurologic or non-oncologic conditions had lower baseline scores and slower improvements. These families often face prolonged caregiving demands without clear prognostic timelines. pediatric palliative care programs should adapt their models to provide sustained, longitudinal support for such populations, beyond the typical oncology-based frameworks.
Consistent with previous reports from high-income settings, our results align with those of Currow et al., who documented improvements in symptom control and patient-reported outcomes following structured, patient-centered palliative care programs [
15]. Similarly, a systematic review by Kaye et al. in pediatric oncology populations identified enhanced symptom control, reduced intensive procedures, increased advanced care planning, and higher family satisfaction as outcomes associated with specialized palliative care services. These international findings underscore the importance of integrating pediatric palliative care services early in the disease course and tailoring them to the needs of both patients and their families, particularly in resource-constrained settings [
16]. A limitation of our study is the loss to follow-up among some participants. Future research should focus on identifying and elucidating modifiable components of palliative care programs that best explain improvements in quality of life, as well as evaluating the program's economic impact from families' perspectives.
Our data highlight the extended survival of a subset of patients, particularly those with neurological disorders. This pattern has important implications for the planning of pediatric palliative care services, as it reflects a growing burden of care associated with long-surviving, non-oncological, severely disabled patients who require sustained multidisciplinary support over an indefinite period. These findings underscore the need for health systems to recognize and adequately resource pediatric palliative care services not solely for terminal oncology care, but also for the growing population of children living with life-limiting conditions of diverse and often prolonged trajectories.
While the study is limited by its single-center design and predominance of cancer cases, the high follow-up rate and use of validated tools enhance its generalizability within similar settings.
5. Conclusions
Pediatric palliative care services significantly enhance the quality of life for seriously ill children and their families, particularly in resource-constrained settings. Programs must ensure sustained, equitable access regardless of diagnosis, geography, or socioeconomic background.
Permission for the use of instruments
PedsQL™, Copyright © 1998 JW Varni, Ph.D. All rights reserved. Request #135535. For permission and access: Mapi Research Trust, Lyon, France
Supplementary Materials
The following supporting information can be downloaded at the website of this paper posted on Preprints.org. Table S1: Characteristics of included participants; Table S2: PedsQL TM 3.0 Family Impact Module; Figure S1: PedsQL Cancer Module subscales over 6 months; Figure S2: PedsQL Family Impact subscales over 6 months. Figure S3: Kaplan-Meier survival function by diagnostic classification.
Author Contributions
Conceptualization, JHGO and MFCP; methodology, MFCP; formal analysis, MFCP; investigation, MGMM, SEBT, PYM, and KMV; resources, JAGO; data curation MFCP, SEBT, and PYM; writing—original draft preparation, MFCP; writing—review and editing, JHGO; project administration JHGO; funding acquisition, JHGO. All authors have read and agreed to the published version of the manuscript.
Funding
The authors disclosed receipt of the following financial support for the research, authorship, and/or publication of this article: This work was supported by the Fundación Gonzalo Rio Arronte.
Institutional Review Board Statement
The study was approved by the Institutional Review Board of the Hospital Infantil de México–Federico Gómez (HIM 2020-013) and conducted in accordance with the Declaration of Helsinki.
Informed Consent Statement
Written informed consent was obtained from all participating caregivers.
Data Availability Statement
The original contributions presented in this study are included in the article and its supplementary material. Further inquiries can be directed to the corresponding author(s).
Acknowledgments
The authors would like to thank the staff of the Hospital Infantil de México Federico Gómez for their support and collaboration, as well as all the voluntary staff who support the Palliative Care Service.
Conflicts of Interest
The authors declare no potential conflicts of interest with respect to the research, authorship, and/or publication of this article.
Abbreviations
The following abbreviations are used in this manuscript:
| AMAI |
Mexican Association of Market and Opinion Intelligence |
References
- al-Lamki, Z. Improving Cancer Care for Children in the Developing World: Challenges and Strategies. Current Pediatric Reviews 2017, 13, 13–23. [CrossRef]
- naul, F.M.; Arreola-Ornelas, H.; Kwete, X.J.; Bhadelia, A.; Rosa, W.E.; Touchton, M.; Méndez-Carniado, O.; Vargas Enciso, V.; Pastrana, T.; Friedman, J.R.; et al. The Evolution of Serious Health-Related Suffering from 1990 to 2021. The Lancet Global Health 2025, 13, e422–e436. [CrossRef]
- Castilla-Peon, M.F.; Rendón, P.L.; Gonzalez-Garcia, N. The Leading Causes of Death in the US and Mexico’s Pediatric Population. Frontiers in Public Health 2024, 12. [CrossRef]
- Robert, R.; Paxton, R.; Palla, S.; Yang, G.; Askins, M.; Joy, S.; Ater, J. Feasibility, Reliability, and Validity of the PedsQL. Pediatric Blood and Cancer 2012, 59, 703–707. [CrossRef]
- Varni, J.W.; Burwinkle, T.M.; Katz, E.R.; Meeske, K. The PedsQL in Pediatric Cancer. Cancer 2002, 94, 2090–2116. [CrossRef]
- Ramírez-Zamora, L.M.; Llamas-Peregrina, N.; Lona-Reyes, J.C.; Sánchez-Zubieta, F.A. Calidad de Vida en Niños con Cáncer. Revista Mexicana de Pediatría 2015, 82, 49–56.
- Varni, J.W.; Sherman, S.A.; Burwinkle, T.M.; Dickinson, P. The PedsQL Family Impact Module. Health and Quality of Life Outcomes 2004, 2, 55. [CrossRef]
- Mano, K.E.; Khan, K.A.; Ladwig, R.J.; Weisman, S.J. Impact of Pediatric Chronic Pain. Journal of Pediatric Psychology 2011, 36, 517–527. [CrossRef]
- Jiang, X.; Sun, L.; Wang, B.; Yang, X.; Shang, L.; Zhang, Y. HRQoL in Recurrent Respiratory Infections. PLoS ONE 2013, 8, e56945. [CrossRef]
- Medrano, G.R.; Berlin, K.S.; Davies, W.H. Utility of the PedsQL Family Impact Module. Quality of Life Research 2013, 22, 2899–2907. [CrossRef]
- Ortega, J.; Vázquez, N.; Caro, A.; Assalone, F. Psychometric Properties of the Spanish PedsQL FIM. Anales de Pediatria 2023, 98, 48-57. [CrossRef]
- Asociación Mexicana de Agencias de Inteligencia de Mercado y Opinión. AMAI 2018. Available online: https://www.amai.org/NSE/ (accessed 30 June 2025).
- Ulloa, Z.G.; García-Quintero, X.; Nakashima-Paniagua, Y.; et al. Community-Based Pediatric Palliative Care in Latin America. Journal of Pain and Symptom Management 2025, 69, e747–e754. [CrossRef]
- Mosha, N.F.V.; Ngulube, P. Implementing Palliative Care in LMICs. Inquiry: The Journal of Health Care Organization, Provision, and Financing 2025, 62. [CrossRef]
- Currow, D.C.; Allingham, S.; Yates, P.; Johnson, C.; Clark, K.; Eagar, K. Improving National Hospice Outcomes. Supportive Care in Cancer 2015, 23, 307–315. [CrossRef]
- Kaye, E.C.; Weaver, M.S.; DeWitt, L.H.; et al. Specialty Palliative Care in Pediatric Oncology. Journal of Pain and Symptom Management 2021, 61, 1060–1079.e2. [CrossRef]
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).