Submitted:
17 November 2025
Posted:
18 November 2025
You are already at the latest version
Abstract
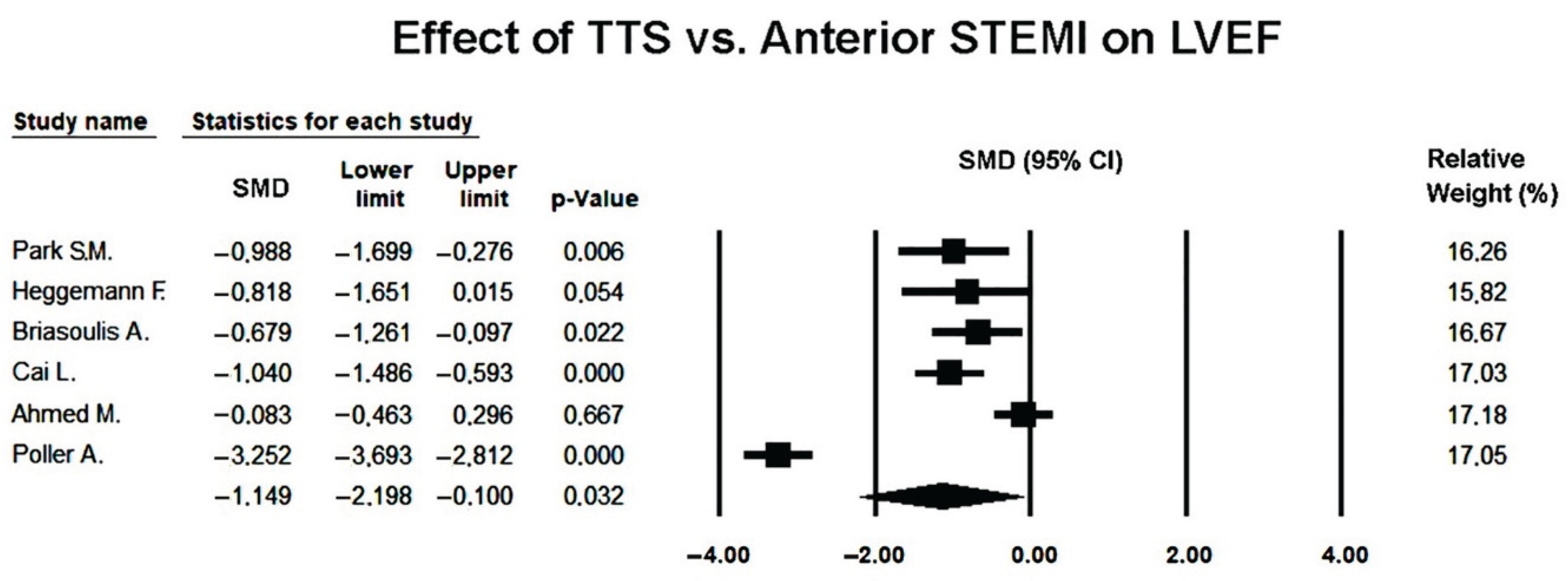
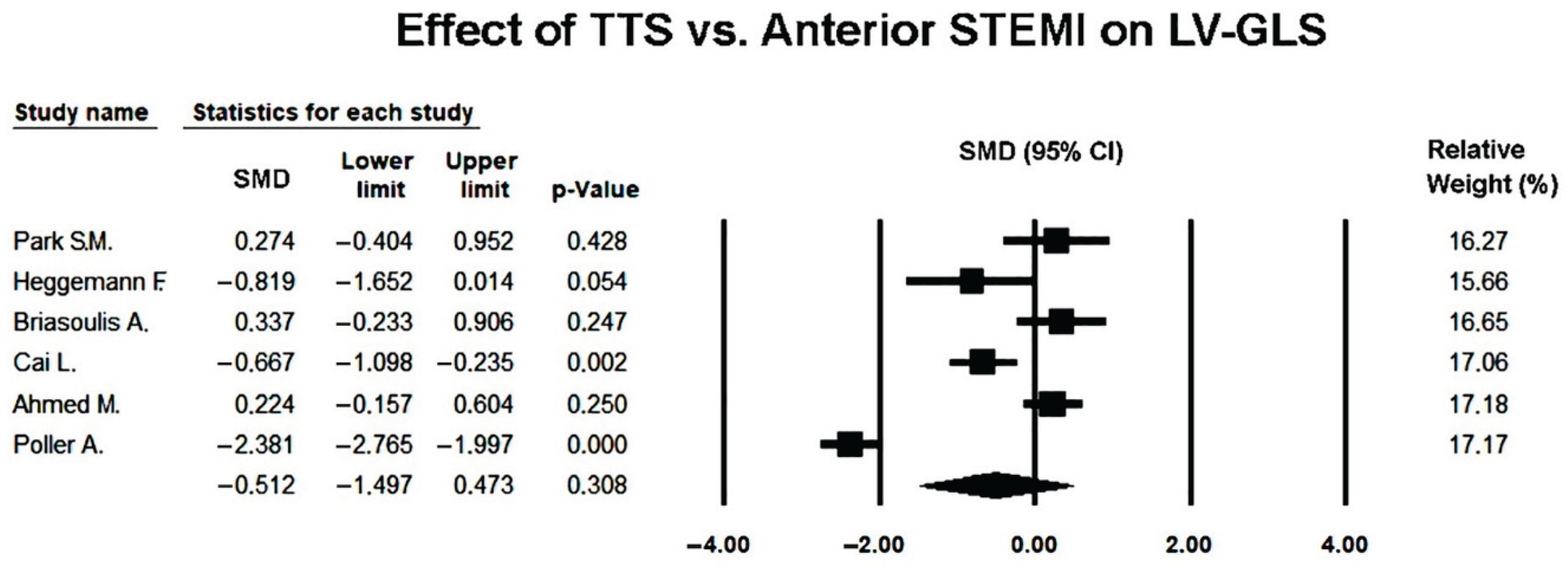
Background: Takotsubo syndrome (TTS) often mimics anterior ST-elevation myocardial infarction (STEMI) caused by left anterior descending (LAD) occlusion, yet the two entities differ fundamentally in pathophysiology and mechanical behavior. Two-dimensional speckle-tracking echocardiography (2D-STE) enables detailed assessment of left ventricular (LV) deformation beyond conventional ejection fraction (LVEF). This meta-analysis compared global and regional LV strain patterns in TTS versus LAD-related anterior STEMI during the acute phase. Methods: A systematic search of PubMed, Embase, and Scopus through October 2025 identified observational case–control studies directly comparing TTS and angiographically confirmed anterior STEMI, with LV mechanics assessed by 2D-STE. Random-effects models were used to pool standardized mean differences (SMDs) for LVEF; global longitudinal strain (GLS); apical, mid-ventricular, and basal longitudinal strain (ALS, MLS, BLS); and global radial strain (GRS). Heterogeneity (I²), publication bias (funnel plots, Egger’s test), meta-regression, and leave-one-out sensitivity analyses were performed. Results: Six studies comprising 221 TTS and 290 anterior STEMI patients met the inclusion criteria. TTS patients were older, predominantly female, and had fewer metabolic risk factors, while LV size was comparable. LVEF was significantly lower in TTS (SMD −1.15; 95% CI −2.20 to −0.10; p = 0.032), with stable findings across sensitivity analyses and no evidence of publication bias. GLS, ALS, MLS, and BLS tended to be more impaired in TTS, although differences were not statistically significant due to marked inter-study heterogeneity. In contrast, GRS was significantly and consistently more reduced in TTS (SMD −1.28; 95% CI −1.59 to −0.98; p < 0.001), indicating more profound global radial dysfunction. Meta-regression showed no significant influence of demographic factors or vendor-specific software on LVEF or GLS differences. Conclusions: Compared with LAD-related anterior STEMI, TTS is characterized by more severely depressed LVEF and markedly impaired radial strain, with a consistent trend toward greater longitudinal dysfunction. This mechanical profile supports the concept of diffuse, stress-induced myocardial stunning in TTS and underscores the value of 2D-STE in differentiating stress cardiomyopathy from ischemic infarction in the acute setting.
Keywords:
1. Introduction
2. Materials and Methods
2.1. Search Strategy
2.2. Eligibility Criteria
2.3. Study Selection and Data Extraction
2.4. Risk of Bias Assessment
2.5. Statistical Analysis
3. Results
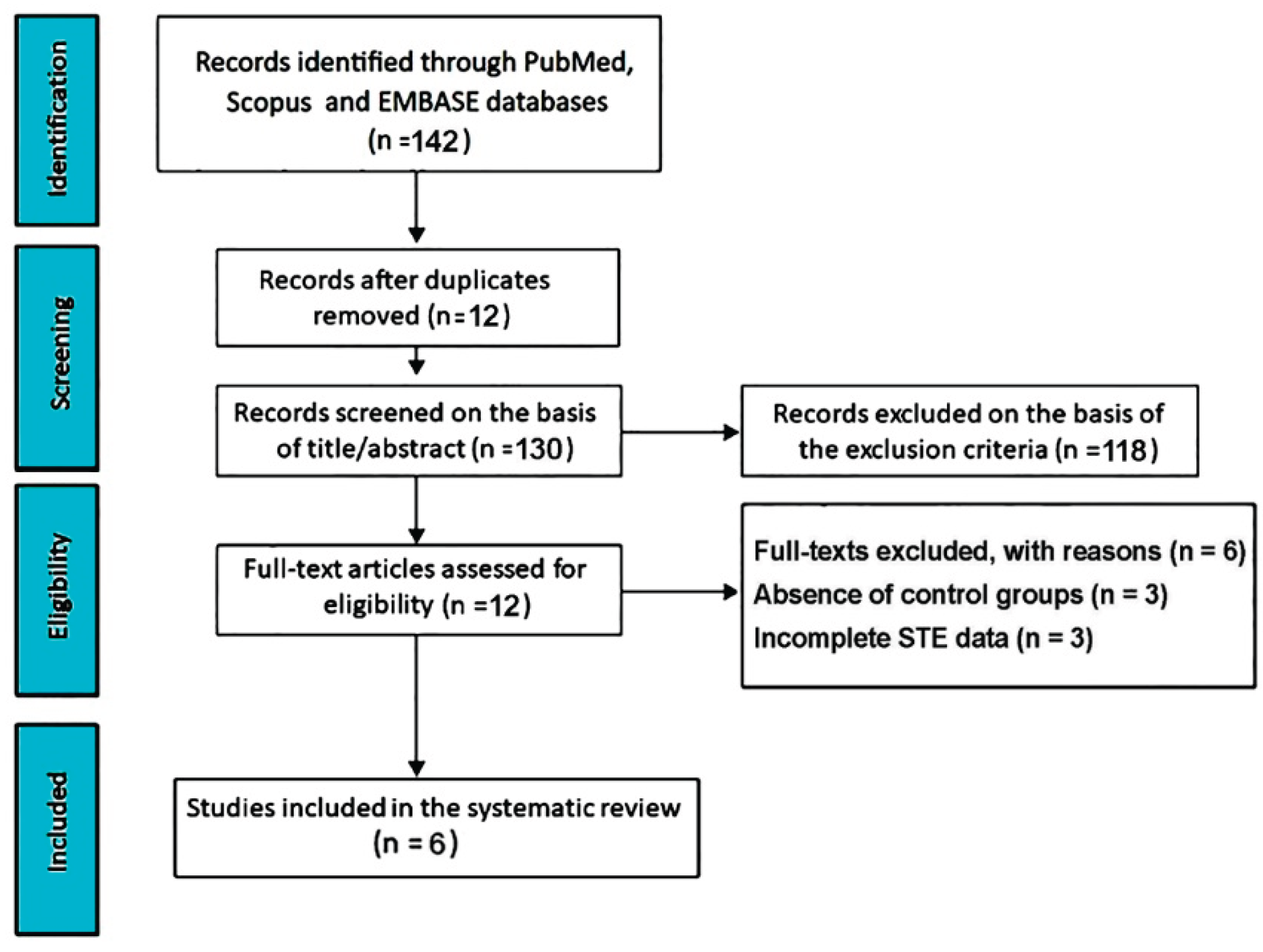
3.1. Study Selection
3.2. Clinical Findings
3.3. Conventional Echocardiographic Findings
3.4. Myocardial Strain Parameters
3.5. Effect of Takotsubo Syndrome versus Anterior STEMI on LVEF
3.6. Effect of Takotsubo Syndrome versus Anterior STEMI on LV-GLS
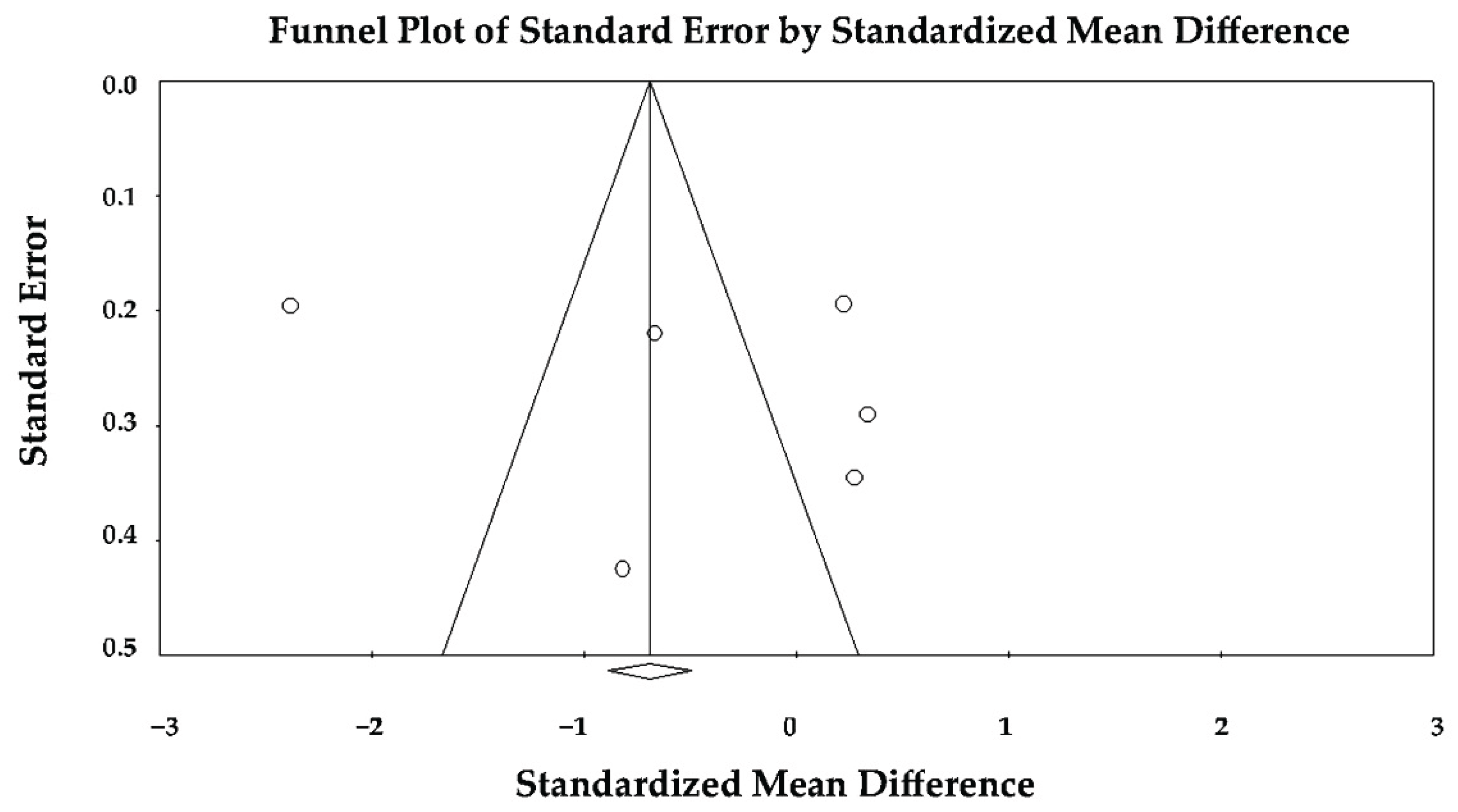
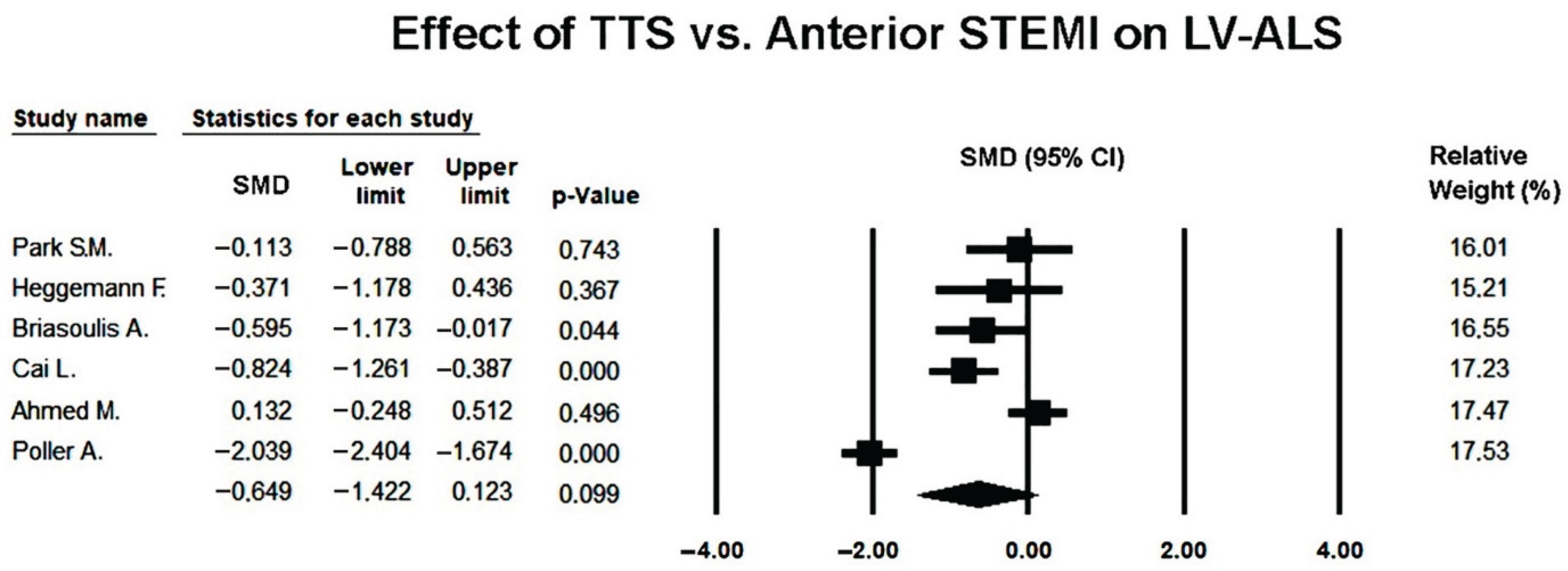
3.7. Effect of Takotsubo Syndrome versus Anterior STEMI on LV-ALS
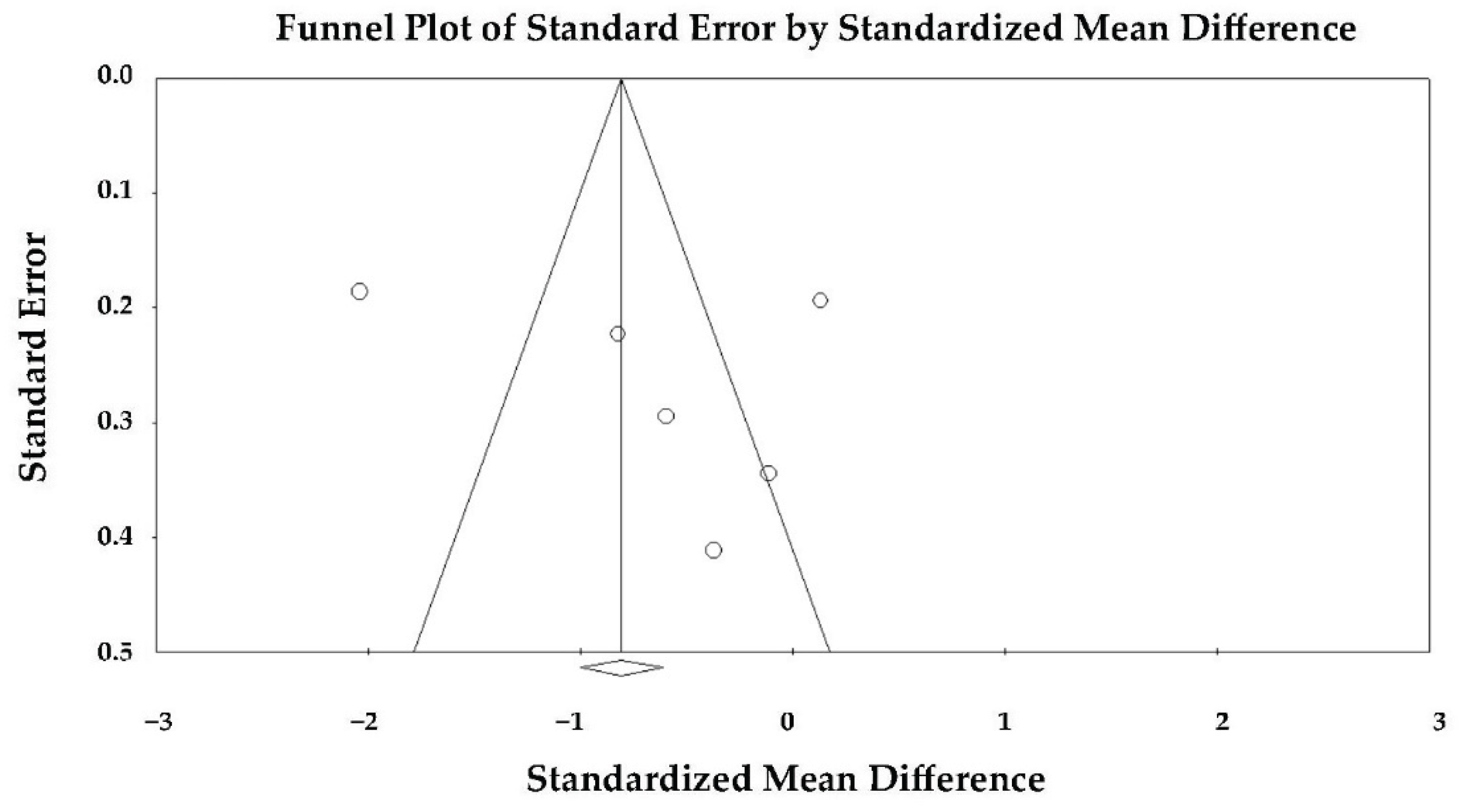
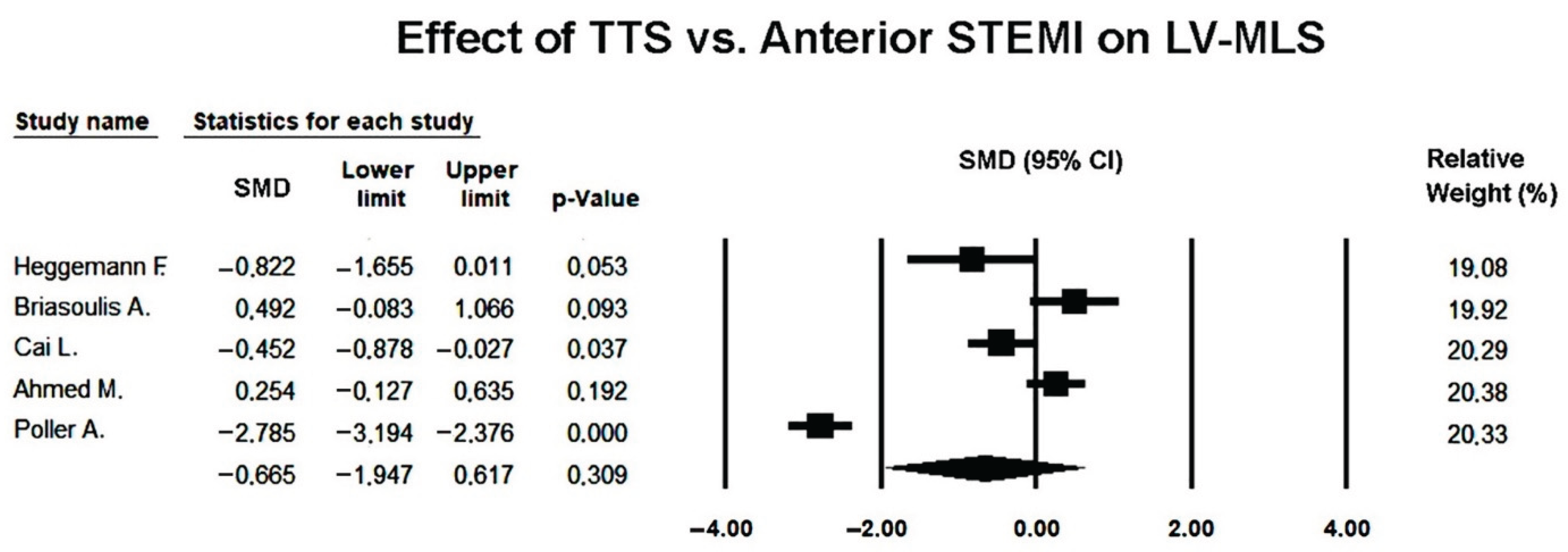
3.8. Effect of Takotsubo Syndrome versus Anterior STEMI on LV-MLS
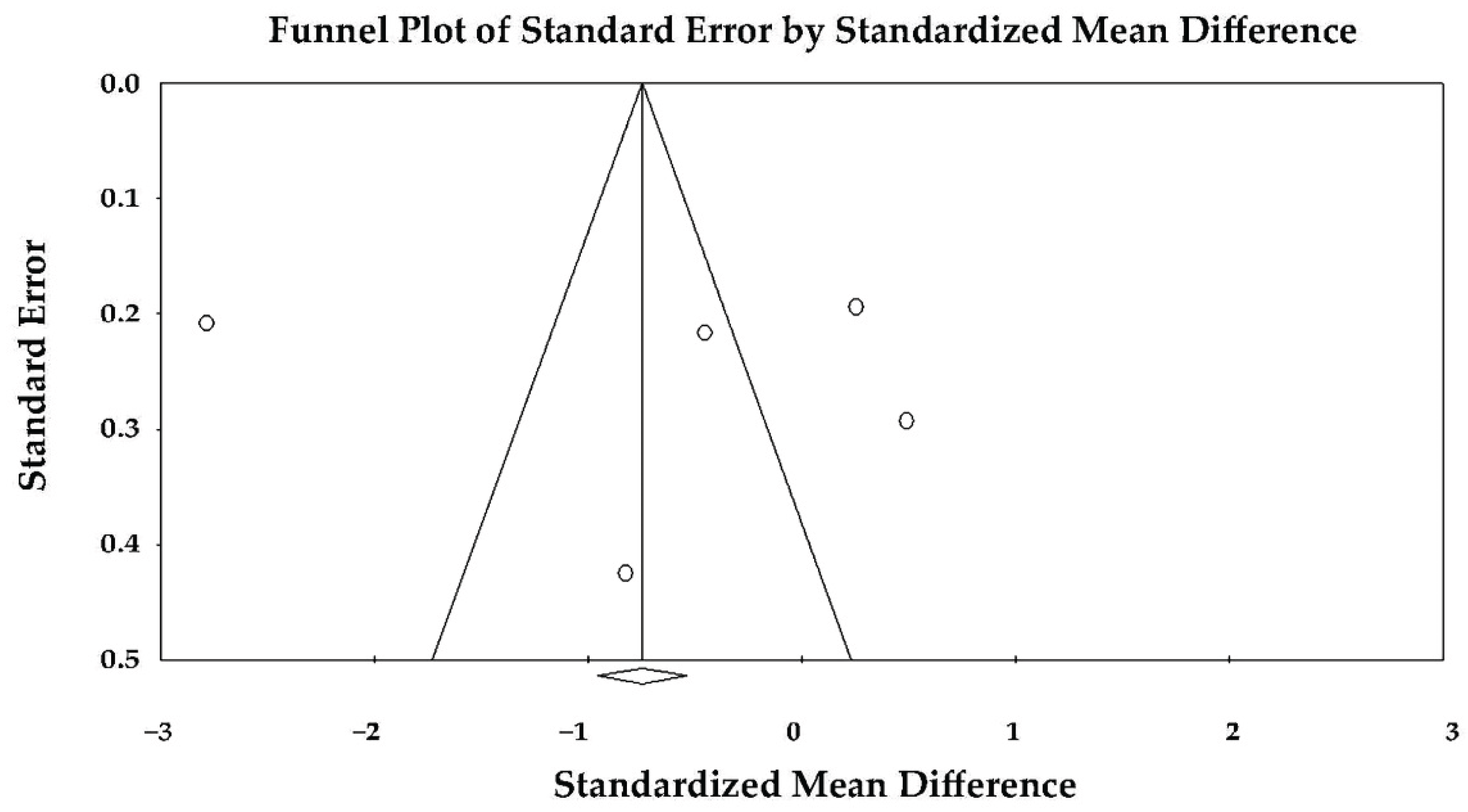
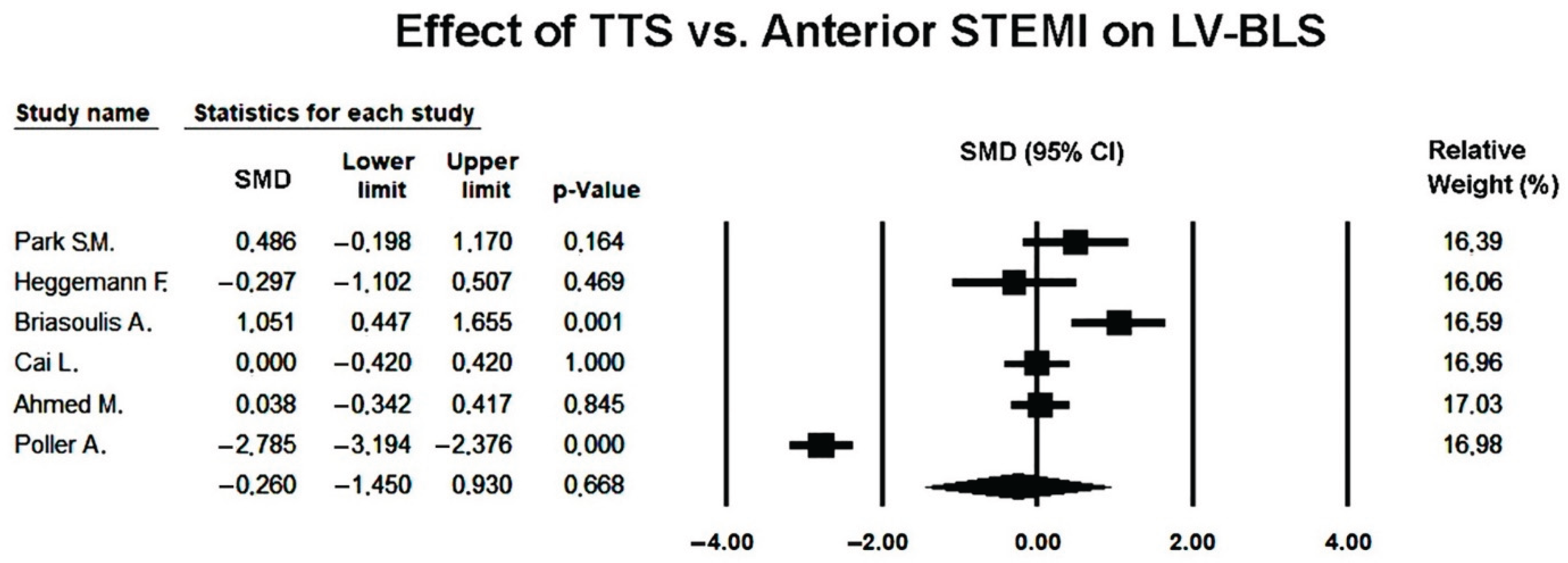
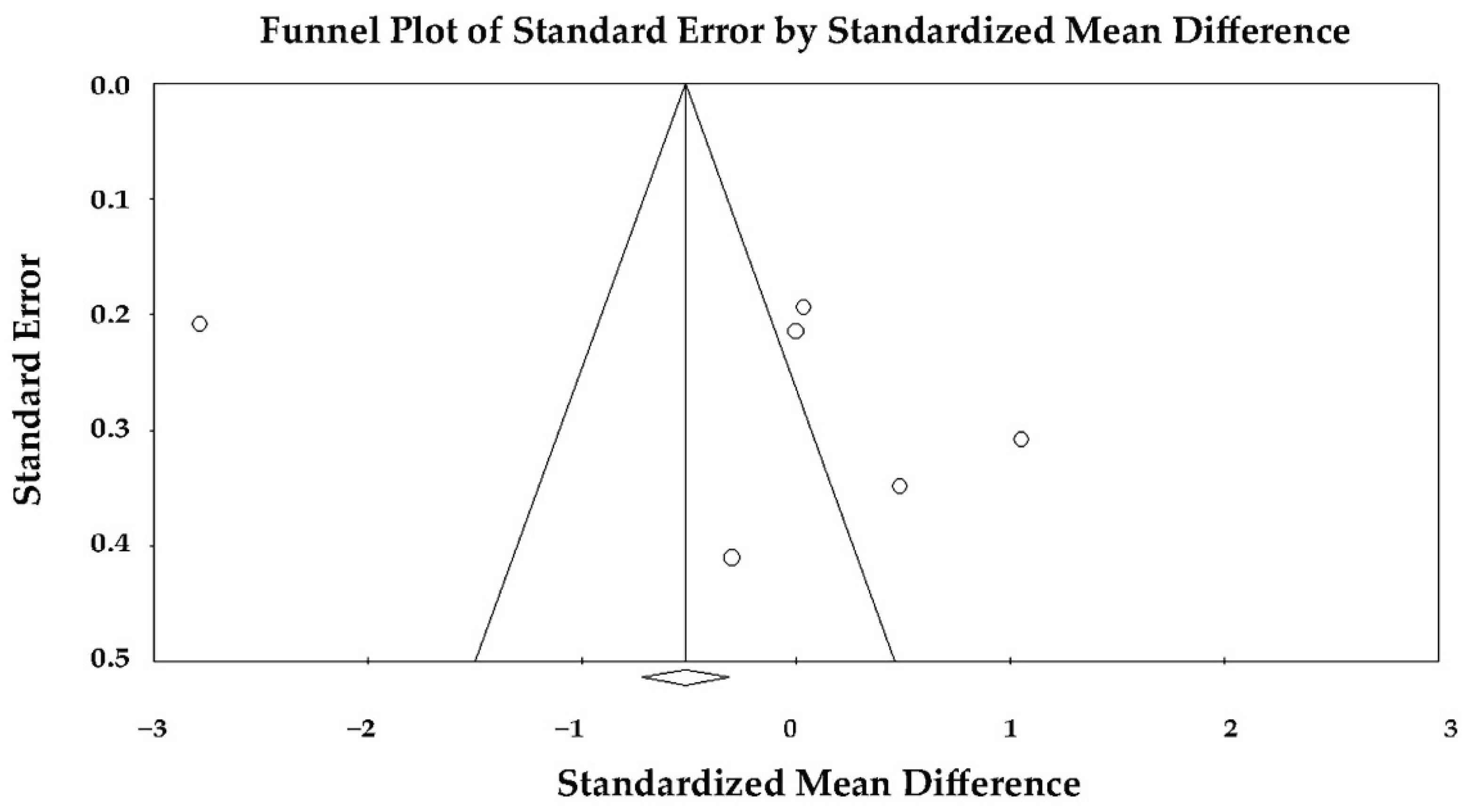
3.9. Effect of Takotsubo Syndrome versus Anterior STEMI on LV-BLS
3.10. Effect of Takotsubo Syndrome versus Anterior STEMI on LV-GRS
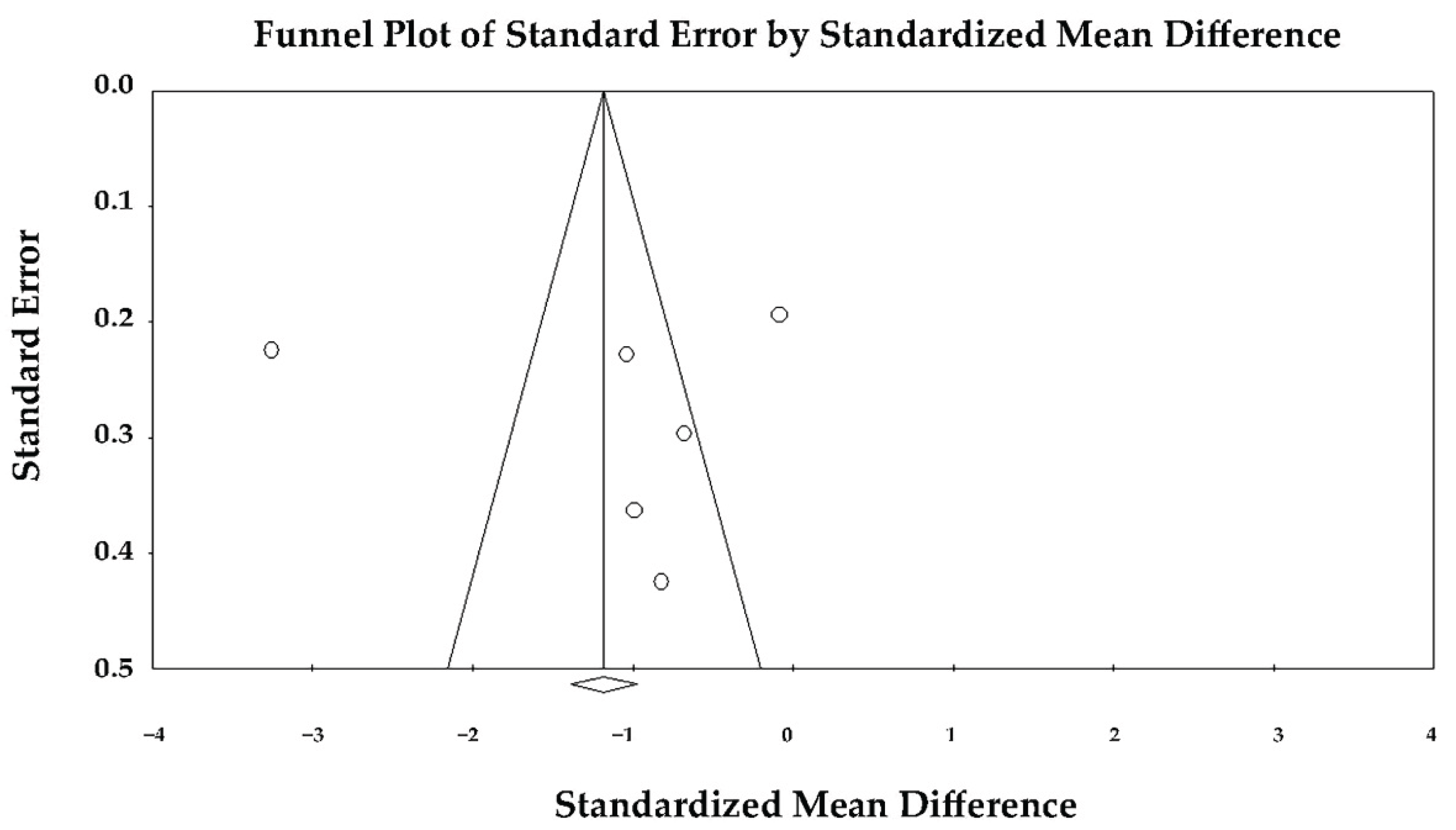
3.11. Publication Bias Assessment
4. Discussion
4.1. Main Findings
4.2. Pathophysiological Mechanisms of LVEF and GLS Impairment in TTS vs. STEMI
4.3. Implications for Clinical Practice
4.4. Limitations of the Included Studies
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Singh, T.; Khan, H.; Gamble, D.T.; Scally, C.; Newby, D.E.; Dawson, D. Takotsubo Syndrome: Pathophysiology, Emerging Concepts, and Clinical Implications. Circulation 2022, 145, 1002–1019. [Google Scholar] [CrossRef]
- Akashi, Y.J.; Goldstein, D.S.; Barbaro, G.; Ueyama, T. Takotsubo cardiomyopathy: A new form of acute, reversible heart failure. Circulation 2008, 118, 2754–2762. [Google Scholar] [CrossRef]
- Templin, C.; Ghadri, J.R.; Diekmann, J.; Napp, L.C.; Bataiosu, D.R.; Jaguszewski, M.; Cammann, V.L.; Sarcon, A.; Geyer, V.; Neumann, C.A.; et al. Clinical Features and Outcomes of Takotsubo (Stress) Cardiomyopathy. N. Engl. J. Med. 2015, 373, 929–938. [Google Scholar] [CrossRef]
- Ghadri, J.R.; Wittstein, I.S.; Prasad, A.; Sharkey, S.; Dote, K.; Akashi, Y.J.; Cammann, V.L.; Crea, F.; Galiuto, L.; Desmet, W.; et al. International Expert Consensus Document on Takotsubo Syndrome (Part I): Clinical Characteristics, Diagnostic Criteria, and Pathophysiology. Eur. Heart J. 2018, 39, 2032–2046. [Google Scholar] [CrossRef] [PubMed]
- Dias, A.; Núñez Gil, I.J.; Santoro, F.; Madias, J.E.; Pelliccia, F.; Brunetti, N.D.; Salmoirago-Blotcher, E.; Sharkey, S.W.; Eitel, I.; Akashi, Y.J.; et al. Takotsubo Syndrome: State-of-the-Art Review by an Expert Panel—Part 1. Cardiovasc. Revasc. Med. 2019, 20, 70–79. [Google Scholar] [CrossRef] [PubMed]
- Kurisu, S.; Kihara, Y. Tako-tsubo cardiomyopathy: Clinical presentation and underlying mechanism. J. Cardiol. 2012, 60, 429–437. [Google Scholar] [CrossRef]
- Wittstein, I.S.; Thiemann, D.R.; Lima, J.A.; Baughman, K.L.; Schulman, S.P.; Gerstenblith, G.; Wu, K.C.; Rade, J.J.; Bivalacqua, T.J.; Champion, H.C. Neurohumoral features of myocardial stunning due to sudden emotional stress. N. Engl. J. Med. 2005, 352, 539–548. [Google Scholar] [CrossRef]
- Lyon, A.R.; Rees, P.S.; Prasad, S.; Poole-Wilson, P.A.; Harding, S.E. Stress (Takotsubo) cardiomyopathy—A novel pathophysiological hypothesis to explain catecholamine-induced acute myocardial stunning. Nat. Clin. Pract. Cardiovasc. Med. 2008, 5, 22–29. [Google Scholar] [CrossRef] [PubMed]
- Cocco, G.; Chu, D. Stress-induced cardiomyopathy: A review. Eur. J. Intern. Med. 2007, 18, 369–379. [Google Scholar] [CrossRef]
- Pelliccia, F.; Kaski, J.C.; Crea, F.; Camici, P.G. Pathophysiology of Takotsubo Syndrome. Circulation 2017, 135, 2426–2441. [Google Scholar] [CrossRef]
- Abdel Mawla, T.S.; Abdel Wanees, W.S.; Abdel Fattah, E.M.; El Khashab, K.A.; Momtaz, O.M. Diagnostic accuracy of global longitudinal strain in prediction of severity and extent of coronary artery stenosis in patients with acute coronary syndrome. Acta Cardiol. 2023, 78, 109–117. [Google Scholar] [CrossRef]
- Bertini, M.; Ng, A.C.; Antoni, M.L.; Nucifora, G.; Ewe, S.H.; Auger, D.; Marsan, N.A.; Schalij, M.J.; Bax, J.J.; Delgado, V. Global longitudinal strain predicts long-term survival in patients with chronic ischemic cardiomyopathy. Circ. Cardiovasc. Imaging 2012, 5, 383–391. [Google Scholar] [CrossRef] [PubMed]
- Bastawy, I.; Ismail, M.; Hanna, H.F.; El Kilany, W. Speckle tracking imaging as a predictor of left ventricular remodeling 6 months after first anterior ST elevation myocardial infarction in patients managed by primary percutaneous coronary intervention. Egypt Heart J. 2018, 70, 343–352. [Google Scholar] [CrossRef]
- Sjögren, H.; Pahlm, U.; Engblom, H.; Erlinge, D.; Heiberg, E.; Arheden, H.; Carlsson, M.; Ostenfeld, E. Anterior STEMI associated with decreased strain in remote cardiac myocardium. Int. J. Cardiovasc. Imaging 2022, 38, 375–387. [Google Scholar] [CrossRef]
- Cau, R.; Muscogiuri, G.; Palmisano, V.; Porcu, M.; Pintus, A.; Montisci, R.; Mannelli, L.; Suri, J.S.; Francone, M.; Saba, L. Base-to-apex gradient pattern assessed by cardiovascular magnetic resonance in Takotsubo cardiomyopathy. J. Thorac. Imaging 2024, 39, 217–223. [Google Scholar] [CrossRef] [PubMed]
- Ghaffar, M.D. Improving reproducibility and pathophysiological understanding in strain imaging: Reflections on Takotsubo syndrome versus STEMI. Int. J. Cardiol. 2025, 440, 133713. [Google Scholar] [CrossRef] [PubMed]
- Kaur, P.; Fatmi, S.S.; Aliabadi, D.; Mandyam, S.; Tosto, S.T. Abnormal longitudinal strain in Takotsubo cardiomyopathy: A case report. Cureus 2022, 14, e24289. [Google Scholar] [CrossRef]
- Moher, D.; Liberati, A.; Tetzlaff, J.; Altman, D.G.; PRISMA Group. Preferred reporting items for systematic reviews and meta-analyses: The PRISMA statement. Open Med. 2009, 3, e123–e130. [Google Scholar]
- Ma, L.L.; Wang, Y.Y.; Yang, Z.H.; Huang, D.; Weng, H.; Zeng, X.T. Methodological quality (risk of bias) assessment tools for primary and secondary medical studies: What are they and which is better? Mil. Med. Res. 2020, 7, 7. [Google Scholar] [CrossRef]
- Luo, D.; Wan, X.; Liu, J.; Tong, T. Optimally estimating the sample mean from the sample size, median, mid-range, and/or mid-quartile range. Stat. Methods Med. Res. 2018, 27, 1785–1805. [Google Scholar] [CrossRef]
- Wan, X.; Wang, W.; Liu, J.; Tong, T. Estimating the sample mean and standard deviation from the sample size, median, range and/or interquartile range. BMC Med. Res. Methodol. 2014, 14, 135. [Google Scholar] [CrossRef] [PubMed]
- Park, S.M.; Prasad, A.; Rihal, C.; Bell, M.R.; Oh, J.K. Left ventricular systolic and diastolic function in patients with apical ballooning syndrome compared with patients with acute anterior ST-segment elevation myocardial infarction: A functional paradox. Mayo Clin. Proc. 2009, 84, 514–521. [Google Scholar] [CrossRef]
- Heggemann, F.; Hamm, K.; Kaelsch, T.; Sueselbeck, T.; Papavassiliu, T.; Borggrefe, M.; Haghi, D. Global and regional myocardial function quantification in Takotsubo cardiomyopathy in comparison to acute anterior myocardial infarction using two-dimensional strain echocardiography. Echocardiography 2011, 28, 715–719. [Google Scholar] [CrossRef]
- Briasoulis, A.; Marinescu, K.; Mocanu, M.; Sattar, A.; Qaqi, O.; Cardozo, S.; Kottam, A.; Afonso, L. Comparison of left ventricular contractile abnormalities in stress-induced cardiomyopathy versus obstructive coronary artery disease using two-dimensional strain imaging. Echocardiography 2016, 33, 863–870. [Google Scholar] [CrossRef]
- Cai, L.; Addetia, K.; Medvedofsky, D.; Spencer, K.T. Myocardial strain may be useful in differentiating Takotsubo cardiomyopathy from left anterior descending coronary artery ischemia. Int. J. Cardiol. 2017, 230, 359–363. [Google Scholar] [CrossRef]
- Ahmed, M.; Sardana, M.; Rasla, S.; Escobar, J.; Bote, J.; Iskandar, A.; Tran, K.V.; Tighe, D.A.; Fitzgibbons, T.P.; Aurigemma, G.P. Comparative left ventricular mechanical deformation in acute apical variant stress cardiomyopathy and acute anterior myocardial infarction utilizing two-dimensional longitudinal strain imaging. Echocardiography 2020, 37, 832–840. [Google Scholar] [CrossRef]
- Poller, A.; Jha, S.; Molander, L.; Espinosa, A.S.; Andersson, E.A.; Simons, K.; Bobbio, E.; Salahuddin, S.; Sevastianova, V.; Thorleifsson, S.J.; et al. Global and segmental longitudinal and radial strain in Takotsubo versus ST-elevation myocardial infarction. Int. J. Cardiol. 2025, 439, 133668. [Google Scholar] [CrossRef] [PubMed]
- Couch, L.S.; Channon, K.; Thum, T. Molecular mechanisms of Takotsubo syndrome. Int. J. Mol. Sci. 2022, 23, 12262. [Google Scholar] [CrossRef]
- Fan, X.; Yang, G.; Kowitz, J.; Akin, I.; Zhou, X.; El-Battrawy, I. Takotsubo syndrome: Translational implications and pathomechanisms. Int. J. Mol. Sci. 2022, 23, 1951. [Google Scholar] [CrossRef]
- Paur, H.; Wright, P.T.; Sikkel, M.B.; Tranter, M.H.; Mansfield, C.; O’Gara, P.; Stuckey, D.J.; Nikolaev, V.O.; Diakonov, I.; Pannell, L.; et al. High levels of circulating epinephrine trigger apical cardiodepression in a β2-adrenergic receptor/Gi-dependent manner: A new model of Takotsubo cardiomyopathy. Circulation 2012, 126, 697–706. [Google Scholar] [CrossRef] [PubMed]
- Rechavia, E.; de Silva, R.; Nihoyannopoulos, P.; Lammertsma, A.A.; Jones, T.; Maseri, A. Hyperdynamic performance of remote myocardium in acute infarction: Correlation between regional contractile function and myocardial perfusion. Eur. Heart J. 1995, 16, 1845–1850. [Google Scholar] [CrossRef]
- Gurudevan, S.V.; Mahmud, E.; Blanchard, D.G.; Strachan, G.M.; Dittrich, T.; Mathews, C.; DeMaria, A.N.; Raisinghani, A.B. Usefulness of compensatory hyperkinesis in the noninfarcted left ventricular wall in separating single from multivessel coronary artery disease in patients with initial ST-elevation acute myocardial infarction. Am. J. Cardiol. 2004, 93, 201–203. [Google Scholar] [CrossRef] [PubMed]
- Caglioni, S.; Mele, D.; Milzi, A.; Bergamaschi, L.; Pavon, A.G.; Landi, A. Impact of coronary microvascular dysfunction in Takotsubo syndrome: Cause, consequence or both? Rev. Cardiovasc. Med. 2024, 25, 163. [Google Scholar] [CrossRef] [PubMed]
- Y-Hassan, S.; Tornvall, P. Epidemiology, pathogenesis, and management of Takotsubo syndrome. Clin. Auton. Res. 2018, 28, 53–65. [Google Scholar] [CrossRef]
- Barmore, W.; Patel, H.; Harrell, S.; Garcia, D.; Calkins, J.B. Jr. Takotsubo cardiomyopathy: A comprehensive review. World J. Cardiol. 2022, 14, 355–362. [Google Scholar] [CrossRef] [PubMed]
- Goto, H.; Kato, K.; Imori, Y.; Wakita, M.; Eguchi, N.; Takaoka, H.; Murakami, T.; Nagatomo, Y.; Isogai, T.; Mitsuhashi, Y.; et al. Time course of left ventricular strain assessment via cardiovascular magnetic resonance myocardial feature tracking in Takotsubo syndrome. J. Clin. Med. 2024, 13, 3238. [Google Scholar] [CrossRef]
- Nishimura, Y.K.; Kubokawa, S.I.; Imai, R.I.; Nakaoka, Y.; Nishida, K.; Seki, S.I.; Kubo, T.; Yamasaki, N.; Kitaoka, H.; Kawai, K.; et al. Takotsubo syndrome in octogenarians and nonagenarians. Circ. Rep. 2021, 3, 724–732. [Google Scholar] [CrossRef]
- Nishimura, Y.K.; Komatsu, J.; Sugane, H.; Hosoda, H.; Imai, R.I.; Nakaoka, Y.; Nishida, K.; Seki, S.I.; Kubo, T.; Kitaoka, H.; et al. Takotsubo syndrome in older men: Clinical characteristics differ by sex and age. Circ. Rep. 2024, 6, 201–208. [Google Scholar] [CrossRef]
- Sonaglioni, A.; Lombardo, M.; Grasso, E.; Nicolosi, G.L.; Foti, N.; Lonati, C.; Harari, S. Presumed Takotsubo syndrome is associated with high in-hospital mortality in very elderly frail females: A case series. Aging Clin. Exp. Res. 2023, 35, 2851–2856. [Google Scholar] [CrossRef]
- El-Battrawy, I.; Santoro, F.; Núñez-Gil, I.J.; Pätz, T.; Arcari, L.; Abumayyaleh, M.; Guerra, F.; Novo, G.; Musumeci, B.; Cacciotti, L.; et al. Age-related differences in Takotsubo syndrome: Results from the multicenter GEIST registry. J. Am. Heart Assoc. 2024, 13, e030623. [Google Scholar] [CrossRef]
- Tawfik, W.; El-Sherif, A.; Bendary, A.; Mahros, M.; Salem, M. Impact of global longitudinal strain on left ventricular remodeling and clinical outcome in patients with ST-segment elevation myocardial infarction (STEMI). Echocardiography 2020, 37, 570–577. [Google Scholar] [CrossRef]
- Wani, A.; Jain, R.; Singsank, Z.; Khandheria, B.K. Trend of global longitudinal strain in Takotsubo cardiomyopathy and clinical predictors of recovery. J. Am. Soc. Echocardiogr. 2021, 34, 452–453. [Google Scholar] [CrossRef]
- Sans-Roselló, J.; Fernández-Peregrina, E.; Duran-Cambra, A.; Carreras-Mora, J.; Sionis, A.; Álvarez-García, J.; Garcia-Garcia, H.M. Incremental prognostic value of global longitudinal strain to the coronary microvascular resistances in Takotsubo patients. Int. J. Cardiovasc. Imaging 2023, 39, 683–693. [Google Scholar] [CrossRef] [PubMed]
- Citro, R.; Okura, H.; Ghadri, J.R.; Izumi, C.; Meimoun, P.; Izumo, M.; Dawson, D.; Kaji, S.; Eitel, I.; Kagiyama, N.; et al. Multimodality imaging in Takotsubo syndrome: A joint consensus document of the EACVI and the Japanese Society of Echocardiography. J. Echocardiogr. 2020, 18, 199–224. [Google Scholar] [CrossRef] [PubMed]
- Farsalinos, K.E.; Daraban, A.M.; Ünlü, S.; Thomas, J.D.; Badano, L.P.; Voigt, J.U. Head-to-head comparison of global longitudinal strain measurements among nine different vendors: The EACVI/ASE inter-vendor comparison study. J. Am. Soc. Echocardiogr. 2015, 28, 1171–1181. [Google Scholar] [CrossRef] [PubMed]
- Rösner, A.; Barbosa, D.; Aarsæther, E.; Kjønås, D.; Schirmer, H.; D’hooge, J. The influence of frame rate on two-dimensional speckle-tracking strain measurements: A study on in-silico models and patient images. Eur. Heart J. Cardiovasc. Imaging 2015, 16, 1137–1147. [Google Scholar] [CrossRef]
- Sonaglioni, A.; Fagiani, V.; Nicolosi, G.L.; Lombardo, M. The influence of pectus excavatum on biventricular mechanics: A systematic review and meta-analysis. Minerva Cardiol. Angiol. 2024, online ahead of print. [CrossRef]

| Study name, year and country | Design | Size (n) |
Mean age (yrs) | Females (%) | STE software | Main findings in TTS vs anterior STEMI |
|---|---|---|---|---|---|---|
| Park S.M. (2009), S. Korea [22] |
Prosp. | TTS = 13 STEMI = 24 |
TTS 70 STEMI = 67 |
TTS = 92 STEMI = 33 |
GE EchoPAC (Vivid 7) | ↓ LVEF; ↓ GLS; ↓ ALS; ↓ MLS; ↓ BLS |
| Heggemann F. (2011), Germany [23] | Prosp. | TTS = 12 STEMI = 12 |
TTS = 72 STEMI = 64 |
TTS = 83 STEMI = 25 |
TomTec 2D CPA | ↓ LVEF; ↓ GLS; ↓ ALS; ↓ MLS; ↓ BLS; ↓ GRS |
| Briasoulis A. (2016), USA [24] | Retrosp. | TTS = 24 STEMI = 24 |
TTS = 68 STEMI = 66 |
TTS = 96 STEMI = 41 |
Philips QLAB (iE33) | ↔ LVEF; ↔ GLS; ↑ BLS; ↔ ALS; ↔ MLS |
| Cai L. (2017), USA [25] |
Retrosp. | TTS = 55 STEMI = 36 |
TTS = 69 STEMI = 64 |
TTS = 88 STEMI = 38 |
GE EchoPAC (Vivid E9) | ↔ LVEF; ↔ GLS; ↓ ALS; ↓ MLS; ↔ BLS |
| Ahmed M. (2020), USA [26] |
Retrosp. | TTS = 60 STEMI = 48 |
TTS = 70 STEMI = 64 |
TTS = 89 STEMI = 42 |
GE EchoPAC (Vivid E9) | ↔ LVEF; ↔ GLS; ↑ ALS/MLS; ↓ BLS |
| Poller A. (2025), Sweden [27] | Prosp. | TTS = 57 STEMI = 146 |
TTS = 71 STEMI = 63 |
TTS = 91 STEMI = 39 |
TomTec Image Arena | ↓ LVEF; ↔ GLS; ↔ ALS; ↔ MLS; ↔ BLS; ↓ GRS |
| TTS (n = 221) |
Anterior STEMI (n = 290) |
P value | |
|---|---|---|---|
| Demographics | |||
| Age (yrs) | 68.8 (62.9-73) | 63.1 (58-66.9) | <0.001 |
| Females (%) | 91.4 (82-100) | 49.2 (28.1-100) | <0.001 |
| Cardiovascular risk factors | |||
| Hypertension (%) | 52.8 (23-72) | 43.3 (33-58) | 0.04 |
| Diabetes (%) | 10.9 (0-23) | 20.8 (12.3-29) | 0.004 |
| Hypercholesterolemia (%) | 21.8 (17.5-25) | 41.4 (15.1-67) | <0.001 |
| Smokers (%) | 18 (14-23) | 29.9 (21-42) | 0.003 |
| Hemodynamics | |||
| Heart rate (bpm) | 87.8 (82-94.3) | 83.1 (79.9-89.6) | 0.002 |
| SBP (mmHg) | 120.4 (98-132.3) | 129.1 (119-136.1) | 0.003 |
| ECG findings | |||
| ST elevation (%) | 48 (32-77) | 98 (92-100) | <0.001 |
| Blood tests | |||
| Peak troponin I (µg/L) | 2.9 (2.3-3.3) | 62.2 (29-93.7) | <0.001 |
| TTS trigger | |||
| Physical stress (%) | 41.4 (28.1-54) | / | / |
| Emotional stress (%) | 36.8 (17-47.3) | / | / |
| Conventional echocardiographic parameters | Number of studies for parameters assessed (n° pts in TTS vs STEMI) |
TTS | Anterior STEMI | P value |
|---|---|---|---|---|
| IVS thickness (mm) | 3 (94 vs. 194) | 9.4 (8.9–10.2) | 10 (9.5–10.3) | 0.03 |
| LV–EDD (mm) | 3 (141 vs. 218) | 46.8 (45–49.1) | 47.1 (45–50.7) | 0.44 |
| LV–ESD (mm) | 3 (141 vs. 218) | 33.3 (29–35.6) | 34.2 (32–36.3) | 0.29 |
| LV–EDVi (ml/m2) | 3 (130 vs. 218) | 62.5 (49.5–80) | 62.7 (45.2–90) | 0.96 |
| LV–ESVi (ml/m2) | 3 (130 vs. 218) | 36.9 (29.6–43) | 35.2 (26.2–51) | 0.61 |
| LVEF (%) | 6 (221 vs. 290) | 34.2 (25.4–39.7) | 41.6 (33.1–48.7) | 0.03 |
| E/A ratio | 2 (70 vs. 170) | 1.0 (0.7–1.3) | 1.15 (1–1.3) | 0.07 |
| E/e’ ratio | 3 (94 vs. 194) | 12.2 (11.4–13) | 12.3 (10.3–16.3) | 0.88 |
| LAVi (ml/m2) | 2 (70 vs. 170) | 30.8 (30.7–30.9) | 31.4 (31.2–31.7) | 0.05 |
| RVIT (mm) | 1 (55 vs. 36) | 37 (37–37) | 36 (36–36) | 0.41 |
| TAPSE (mm) | 1 (55 vs. 36) | 15 (15–15) | 20 (20–20) | 0.004 |
| STE variables | Number of studies for parameters assessed (n° pts in TTS vs STEMI) |
TTS |
Anterior STEMI |
P value |
|---|---|---|---|---|
| LV–GLS (%) | 6 (221 vs. 290) | –9.1 (–3.5,–13) | –10.5 (–6.3,–13) | 0.01 |
| LV–ALS (%) | 6 (221 vs. 290) | –4.4 (–0.5,–9.8) | –6.4 (–3.4,–10) | 0.001 |
| LV–MLS (%) | 5 (208 vs. 266) | –9.9 (–5.8,–13.4) | –11.6 (–5.7,–17.4) | 0.006 |
| LV–BLS (%) | 6 (221 vs. 290) | –14.2 (–11.4,–18.1) | –14.2 (–7.3,–17.4) | 0.03 |
| LV–GRS (%) | 2 (69 vs. 158) | 15.7 (13.9,17.5) | 26.4 (23.8,29.1) | <0.001 |
| Covariate | Coefficient | Standard error | 95% Lower | 95% Upper | P-value |
|---|---|---|---|---|---|
| Intercept | 0.430 | 14.01 | –27.02 | 27.883 | 0.975 |
| Mean age TTS (yrs) | –0.086 | 0.191 | –0.461 | 0.288 | 0.651 |
| %Hypertension TTS | 0.055 | 0.051 | –0.046 | 0.155 | 0.286 |
| %Diabetes TTS | 0.133 | 0.120 | –0.103 | 0.369 | 0.269 |
| Covariate | Coefficient | Standard error | 95% Lower | 95% Upper | P-value |
|---|---|---|---|---|---|
| Intercept | –0.394 | 18.24 | –36.14 | 35.35 | 0.983 |
| Mean age TTS (yrs) | 0.011 | 0.240 | –0.459 | 0.481 | 0.963 |
| %females TTS | –0.015 | 0.088 | –0.189 | 0.158 | 0.864 |
| Software: nonGE | 0.979 | 1.462 | –1.886 | 3.844 | 0.503 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




