Submitted:
13 November 2025
Posted:
14 November 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
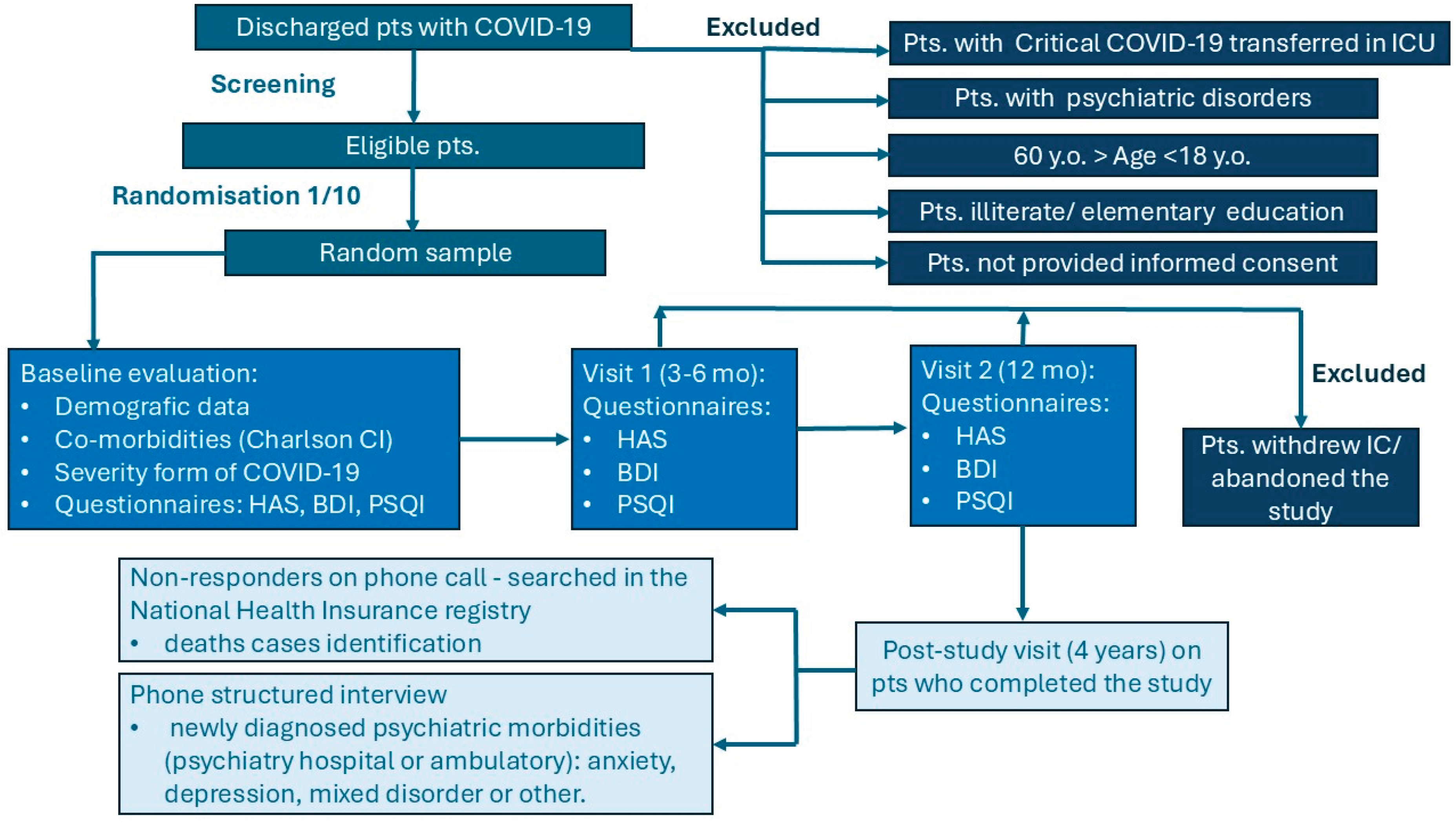
2.1. Study Design
2.2. Study Population
2.3. Data Collected
2.4. Study Questionnaires
2.5. Statistical Analysis
3. Results
3.1. Demographic Data and Severity COVID-19 Episode
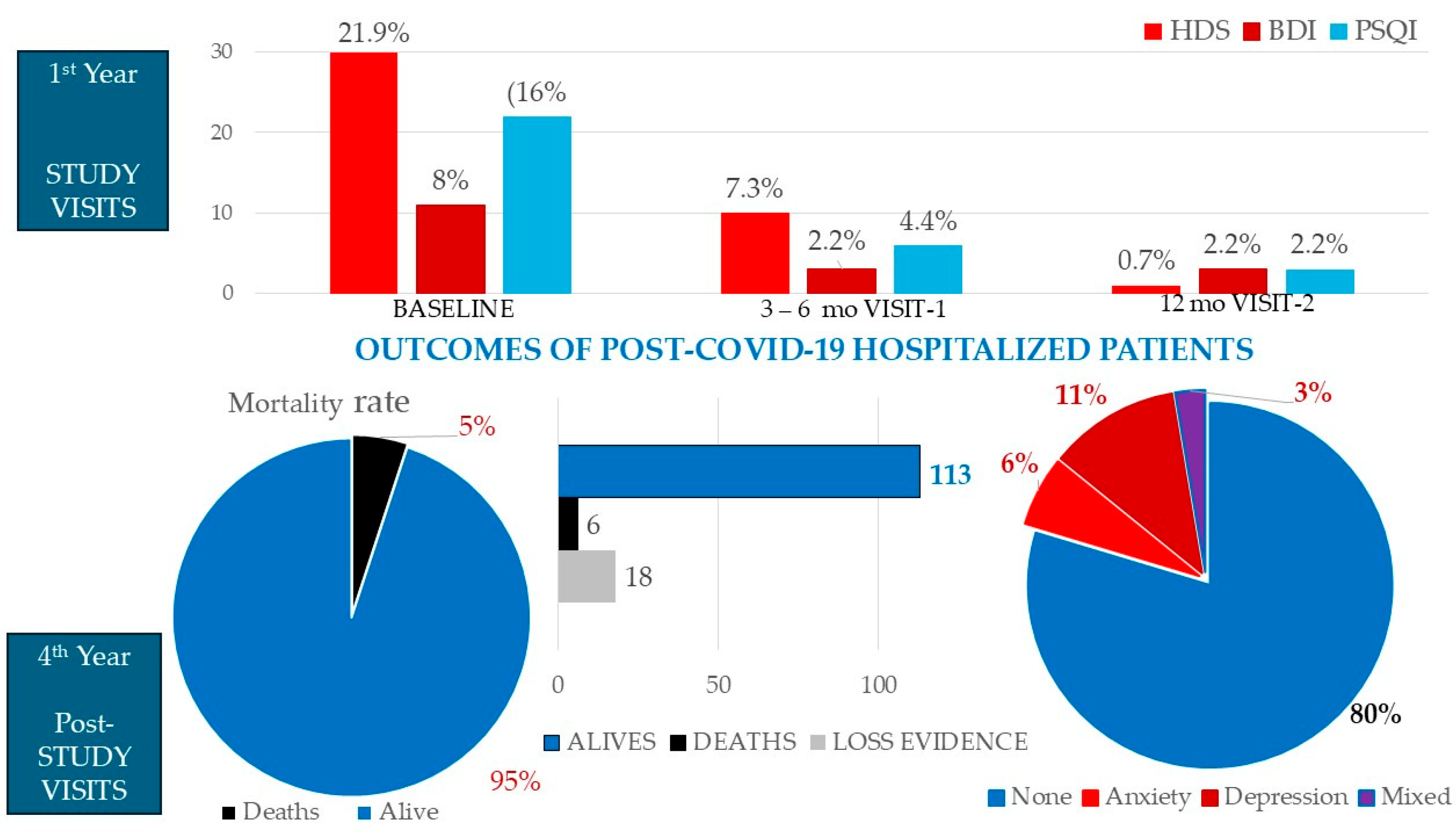
3.2. Anxiety in Patients Hospitalized with COVID-19
3.3. Assessment of Depression in Patients Hospitalized with COVID-19
3.4. Sleapniess Scales in Patients Hospitalized with COVID-19
3.5. Long-Term Post-COVID-Psychiatric Morbidity and Mortalitay
4. Discussion
Limits of Study
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| BDI | Beck Depression Inventory Charlson Comorbidity Index |
| CCI | Charlson Comorbidity Index |
| COVID-19 | Coronaviral Infectious Disease |
| IL | Interleukine |
| HAS | Hamilton Anxiety Scale |
| PSQI | Pittsbourgh Sleep Quality Index |
| PASC | post-acute sequelae of COVID-19 |
| SARS-CoV-2 | Severe Acute Respiratory Syndrome Coronavirus-2 |
| WHO | World Health Organization |
Appendix A
| N | % | P* | ||
| Age | <40 years | 49 | 35.77% | p<0.05 |
| 40-60 years | 88 | 64.23% | ||
| Gender | Male | 63 | 46% | 0.347 |
| Female | 74 | 54% | ||
| Living area | Urban | 91 | 66.42% | p<0.05 |
| Rural | 46 | 33.58% | ||
| Education | Low** | 112 | 81.75% | p<0.05 |
| High*** | 25 | 18.25% | ||
| Smoke | Yes | 25 | 18,25% | p<0.05 |
| No | 112 | 81.75% | ||
| Alcohol | Yes | 18 | 13.14% | p<0.05 |
| No | 119 | 16.86% | ||
| Obesity | Yes | 30 | 21.9% | p<0.05 |
| No | 107 | 78.1% | ||
| Charlson Index | <4 | 135 | 98.54% | p<0.05 |
| ≥4 | 2 | 1.46% | ||
| COVID-19 severity | Mild | 31 | 22.63% | p<0.05 |
| Moderate | 66 | 48.18% | ||
| Severe | 40 | 29.20% | ||
References
- World Health Organization. (2022, March 2). COVID-19 pandemic triggers 25% increase in prevalence of anxiety and depression worldwide; Available: https://www.who.int/news/item/02-03-2022-covid-19-pandemic-triggers-25-increase-in-prevalence-of-anxiety-and-depression-worldwide [Accessed 2.11.2025].
- Mazza, M. G., De Lorenzo, R., Conte, C., Poletti, S., Vai, B., Bollettini, I., Melloni, E. M. T., Furlan, R., Ciceri, F., Rovere-Querini, P., & Benedetti, F. (2020). Anxiety and depression in COVID-19 survivors: Role of inflammatory and clinical predictors. Brain, Behavior, and Immunity, 89, 594–600. [CrossRef]
- Aziz, A. A., Latif, A. A., & Elseesy, S. W. (2025). Cognitive impairment, depressive and anxiety disorders among post-COVID-19 survivors: A follow-up study. Middle East Current Psychiatry, 32(8). [CrossRef]
- Seighali, N., Abdollahi, A., Shafiee, A., et al. (2024). The global prevalence of depression, anxiety, and sleep disorder among patients coping with post COVID-19 syndrome (long COVID): A systematic review and meta-analysis. BMC Psychiatry, 24, 105. [CrossRef]
- Vasile MC, Vasile CI, Arbune AA, Nechifor A, Arbune M (2023). Cognitive Dysfunction in Hospitalized Patient with Moderate-to-Severe COVID-19: A 1-Year Prospective Observational Study. J Multidiscip Healthc., 16:3367-3378. https://doi: 10.2147/JMDH.S432969.
- Burkauskas, J., Branchi, I., Pallanti, S., & Domschke, K. (2023). Anxiety in post-COVID-19 syndrome – prevalence, mechanisms and treatment. Neuroscience Applied, 3, 103932. [CrossRef]
- Benedetti, F., Mazza, M., Cavalli, G., Ciceri, F., Dagna, L., & Rovere-Querini, P. (2021). Can cytokine blocking prevent depression in COVID-19 survivors? Journal of Neuroimmune Pharmacology, 16(1), 1–3. [CrossRef]
- Shetty, P. A., Ayari, L., Madry, J., Betts, C., Robinson, D. M., & Kirmani, B. F. (2023). The relationship between COVID-19 and the development of depression: Implications on mental health. Neuroscience Insights, 18, 26331055231191513. [CrossRef]
- Lorkiewicz, P., & Waszkiewicz, N. (2021). Biomarkers of post-COVID depression. Journal of Clinical Medicine, 10(18), 4142. [CrossRef]
- Batool-Anwar, S., Fashanu, O. S., & Quan, S. F. (2025). Long-term effects of COVID-19 on sleep patterns. Turkish Thoracic Journal, 26(1), 9–16. [CrossRef]
- Batool-Anwar, S., Fashanu, O. S., & Quan, S. F. (2025). Long-term effects of COVID-19 on sleep patterns. Turkish Thoracic Journal, 26(1), 9–16. [CrossRef]
- Yasugaki, S., Okamura, H., Kaneko, A., & Hayashi, Y. (2025). Bidirectional relationship between sleep and depression. Neuroscience Research, 211, 57–64. [CrossRef]
- Ruhrländer, J., Syntila, S., Schieffer, E., & Schieffer, B. (2025). The orexin system and its impact on the autonomic nervous and cardiometabolic system in post-acute sequelae of COVID-19. Biomedicines, 13(3), 545. [CrossRef]
- Ministry of Health of Romania. (2020, March 23). Order no. 487 for the approval of the treatment protocol for SARS-CoV-2 virus infection. Official Gazette no. 242 of March 24, 2020.
- Ministry of Health of Romania. (2020, August 10). Order no. 1418 on the amendment of the annex to the Order of the Minister of Health no. 487/2020 for the approval of the treatment protocol for SARS-CoV-2 virus infection. Official Gazette no. 719 of August 10, 2020.
- Bhimraj, A., Morgan, R. L., Shumaker, A. H., Lavergne, V., Baden, L., Cheng, V. C., Edwards, K. M., Gandhi, R., Muller, W. J., O’Horo, J. C., Shoham, S., Murad, M. H., Mustafa, R. A., Sultan, S., & Falck-Ytter, Y. (2020). Infectious Diseases Society of America guidelines on the treatment and management of patients with COVID-19. Clinical Infectious Diseases. [CrossRef]
- UNESCO Institute for Statistics. (2012). International Standard Classification of Education: ISCED 2011. Montreal: UNESCO-UIS. Available at: https://uis.unesco.org/en/topic/international-standard-classification-education-isced. [Accessed 12.01.2021].
- National Institutes of Health. (1998). Clinical guidelines on the identification, evaluation, and treatment of overweight and obesity in adults—The evidence report. Obesity Research, 6(Suppl 2), 51S–209S.
- Charlson, M., Szatrowski, T. P., Peterson, J., & Gold, J. (1994). Validation of a combined comorbidity index. Journal of Clinical Epidemiology, 47(11), 1245–1251. [CrossRef]
- Charlson, M. E., Pompei, P., Ales, K. L., & MacKenzie, C. R. (1987). A new method of classifying prognostic comorbidity in longitudinal studies: Development and validation. Journal of Chronic Diseases, 40(5), 373–383. [CrossRef]
- Maier, W., Buller, R., Philipp, M., & Heuser, I. (1988). The Hamilton Anxiety Scale: Reliability, validity and sensitivity to change in anxiety and depressive disorders. Journal of Affective Disorders, 14(1), 61–68.. https://doi: 10.1016/0165-0327(88)90072-9.
- Tiwari, K., & Ojha, R. (2024). A study on Hamilton Anxiety Rating Scale among college students. International Journal of Indian Psychology, 10, 1725–1731. [CrossRef]
- Wang, J., Zhu, E., Ai, P., Liu, J., Chen, Z., Wang, F., Chen, F., & Ai, Z. (2022). The potency of psychiatric questionnaires to distinguish major mental disorders in Chinese outpatients. Frontiers in Psychiatry, 13, 1091798. [CrossRef]
- Lee, E.-H., Lee, S.-J., Hwang, S.-T., Hong, S.-H., & Kim, J.-H. (2017). Reliability and validity of the Beck Depression Inventory-II among Korean adolescents. Psychiatry Investigation, 14(1), 30–36. [CrossRef]
- Wang, Y. P., & Gorenstein, C. (2013). Psychometric properties of the Beck Depression Inventory-II: A comprehensive review. Brazilian Journal of Psychiatry, 35(4), 416–431. [CrossRef]
- Wang, Y. P., & Gorenstein, C. (2013). Assessment of depression in medical patients: A systematic review of the utility of the Beck Depression Inventory-II. Clinics (São Paulo), 68(9), 1274–1287. [CrossRef]
- Buysse, D. J., Reynolds, C. F. III, Monk, T. H., Berman, S. R., & Kupfer, D. J. (1989). The Pittsburgh Sleep Quality Index: A new instrument for psychiatric practice and research. Psychiatry Research, 28(2), 193–213. [CrossRef]
- Mollayeva, T., Thurairajah, P., Burton, K., Mollayeva, S., Shapiro, C. M., & Colantonio, A. (2016). The Pittsburgh Sleep Quality Index as a screening tool for sleep dysfunction in clinical and non-clinical samples: A systematic review and meta-analysis. Sleep Medicine Reviews, 25, 52–73. [CrossRef]
- Phelps, C., Bellon, S., Hinkey, M., Nash, A., Boyd, J., Cook, C. E., & Garcia, A. N. (2020). Measurement properties of patient-reported outcome measures used to assess the sleep quality in adults with high-prevalence chronic pain conditions: A systematic review. Sleep Medicine, 74, 315–331. [CrossRef]
- James, B. B., Rengasamy, E. R., Watson, C., et al. (2022). Persistent neuropsychiatric symptoms after COVID-19: A systematic review and meta-analysis. Brain Communications, 4(1), fcab297. [CrossRef]
- Diogo Gonçalves, S., Santos, A. L., Ramos, C., Valente, F., Jesus, L., Pereira, A. J., & Chyczij, F. (2025). Mental health in Europe after COVID-19: A systematic review of depression, anxiety, and stress among adult primary health care users. Psychiatry International, 6(3), 109. [CrossRef]
- Tomasoni D, Bai F, Castoldi R, Barbanotti D, Falcinella C, Mulè G, Mondatore D, Tavelli A, Vegni E, Marchetti G, d'Arminio Monforte A. Anxiety and depression symptoms after virological clearance of COVID-19: A cross-sectional study in Milan, Italy. J Med Virol. 2021; 93(2):1175-1179. doi: 10.1002/jmv.26459..
- Adibi, A., Motahharynia, A., & Adibi, I. (2025). Long-term consequences of COVID-19 on sleep, mental health, fatigue, and cognition: A preliminary study. Discover Mental Health, 5, 66. [CrossRef]
- Popovici, G. C., Georgescu, C. V., Vasile, M. C., Vlase, C. M., Arbune, A. A., & Arbune, M. (2024). Obstructive sleep apnea after COVID-19: An observational study. Life (Basel), 14(8), 1052. [CrossRef]
- Tanriverdi, A., Savci, S., Kahraman, B. O., & Ozpelit, E. (2022). Extrapulmonary features of post-COVID-19 patients: Muscle function, physical activity, mood, and sleep quality. Irish Journal of Medical Science, 191(3), 969–975. [CrossRef]
- Albu, S., Zozaya, N. R., Murillo, N., García-Molina, A., Chacón, C. A. F., & Kumru, H. (2021). What’s going on following acute COVID-19? Clinical characteristics of patients in an out-patient rehabilitation program. NeuroRehabilitation, 48(4), 469–480. [CrossRef]
| Anxiety | Absent | Mild | Moderate | Χ2 Test (p) | |
| Gender | Male | 58 | 2 | 3 | <0.001 |
| Female | 49 | 18 | 7 | ||
| Age | <40 | 51 | 12 | 3 | 0.293 |
| 40-60 | 56 | 8 | 7 | ||
| Living area | Urban | 71 | 15 | 5 | 0.392 |
| Rural | 36 | 5 | 5 | ||
| Education | Low | 19 | 4 | 2 | 0.961 |
| High | 88 | 16 | 8 | ||
| Smoking | Yes | 22 | 2 | 1 | 0.416 |
| No | 85 | 18 | 9 | ||
| Alcohol use | Yes | 18 | 0 | 0 | 0.054 |
| No | 89 | 20 | 10 | ||
| Obesity | Yes | 23 | 3 | 4 | 0.289 |
| No | 84 | 17 | 16 | ||
| COVID-19 severity | Mild | 26 | 5 | 0 | 0.028 |
| Moderate | 51 | 12 | 3 | ||
| Severe | 30 | 3 | 7 |
| Depression | Absent | Mild | Χ2 Test (p) | |
| Gender | Male | 60 | 3 | 0.194 |
| Female | 66 | 8 | ||
| Age | <40 | 43 | 6 | 0.659 |
| 40-60 | 83 | 5 | ||
| Living area | Urban | 86 | 5 | 0.124 |
| Rural | 40 | 6 | ||
| Education | Low | 15 | 2 | 0.640 |
| High | 24 | 1 | ||
| Smoking | Yes | 23 | 2 | 0.995 |
| No | 103 | 9 | ||
| Alcohol use | Yes | 17 | 1 | 0.678 |
| No | 109 | 10 | ||
| Obesity | Yes | 27 | 3 | 0.653 |
| No | 99 | 8 | ||
| Charlson
Index |
<4 | 124 | 2 | 0.673 |
| ≥4 | 11 | 0 | ||
| COVID-19 severity | Mild | 30 | 1 | 0.527 |
| Moderate | 60 | 6 | ||
| Severe | 36 | 4 |
| PSQI score | < 5 | ≥ 5 | Χ2 Test (p) | ||
| Gender | Male | 53 | 10 | 0.956 | |
| Female | 62 | 12 | |||
| Age | <40 | 40 | 9 | 0.582 | |
| 40-60 | 75 | 13 | |||
| Living area | Urban | 76 | 15 | 0.848 | |
| Rural | 39 | 7 | |||
| Education | Low | 28 | 94 | 0.992 | |
| High | 21 | 4 | |||
| Smoking | Yes | 4 | 18 | 0.992 | |
| No | 21 | 94 | |||
| Alcohol | Yes | 13 | 102 | 0.146 | |
| No | 5 | 17 | |||
| Obesity | Yes | 89 | 26 | 0.645 | |
| No | 18 | 4 | |||
| Charlson Index | <4 | 113 | 22 | 0.533 | |
| ≥4 | 2 | 0 | |||
| COVID-19 severity | Mild | 28 | 3 | 0.040 | |
| Moderate | 50 | 16 | |||
| Severe | 37 | 3 | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




