Submitted:
06 November 2025
Posted:
07 November 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Patient Population
2.2. Echocardiographic Assessment
2.3. Biomarker Measurement
2.4. Outcomes
2.5. Statistical Analysis
3. Results
3.1. Baseline Characteristics
3.2. Prognostic Discrimination for In-Hospital Mortality (ROC/AUC Analyses)
Interpretation
3.3. Correlation Between Virtue Index and NT-proBNP
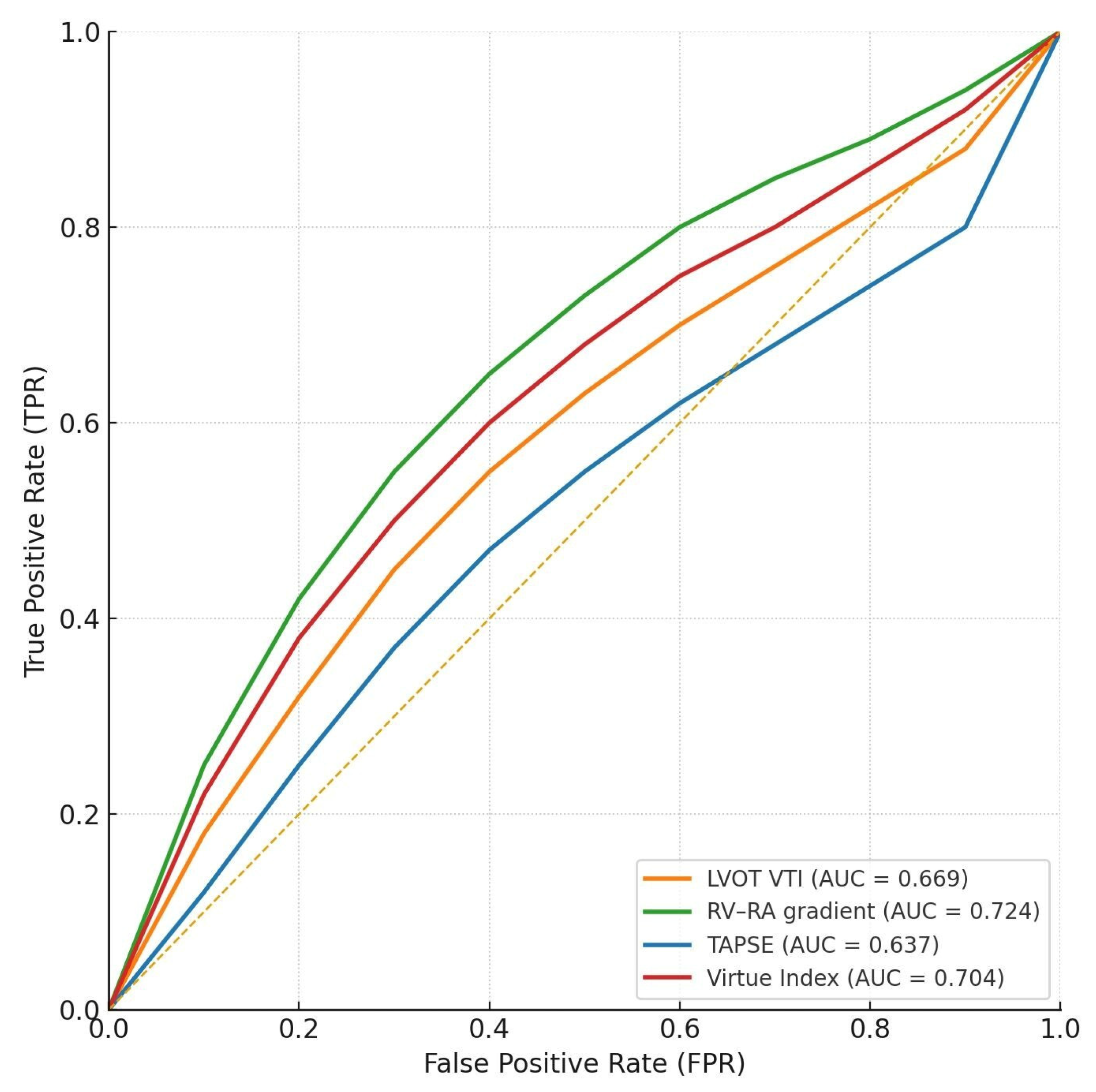
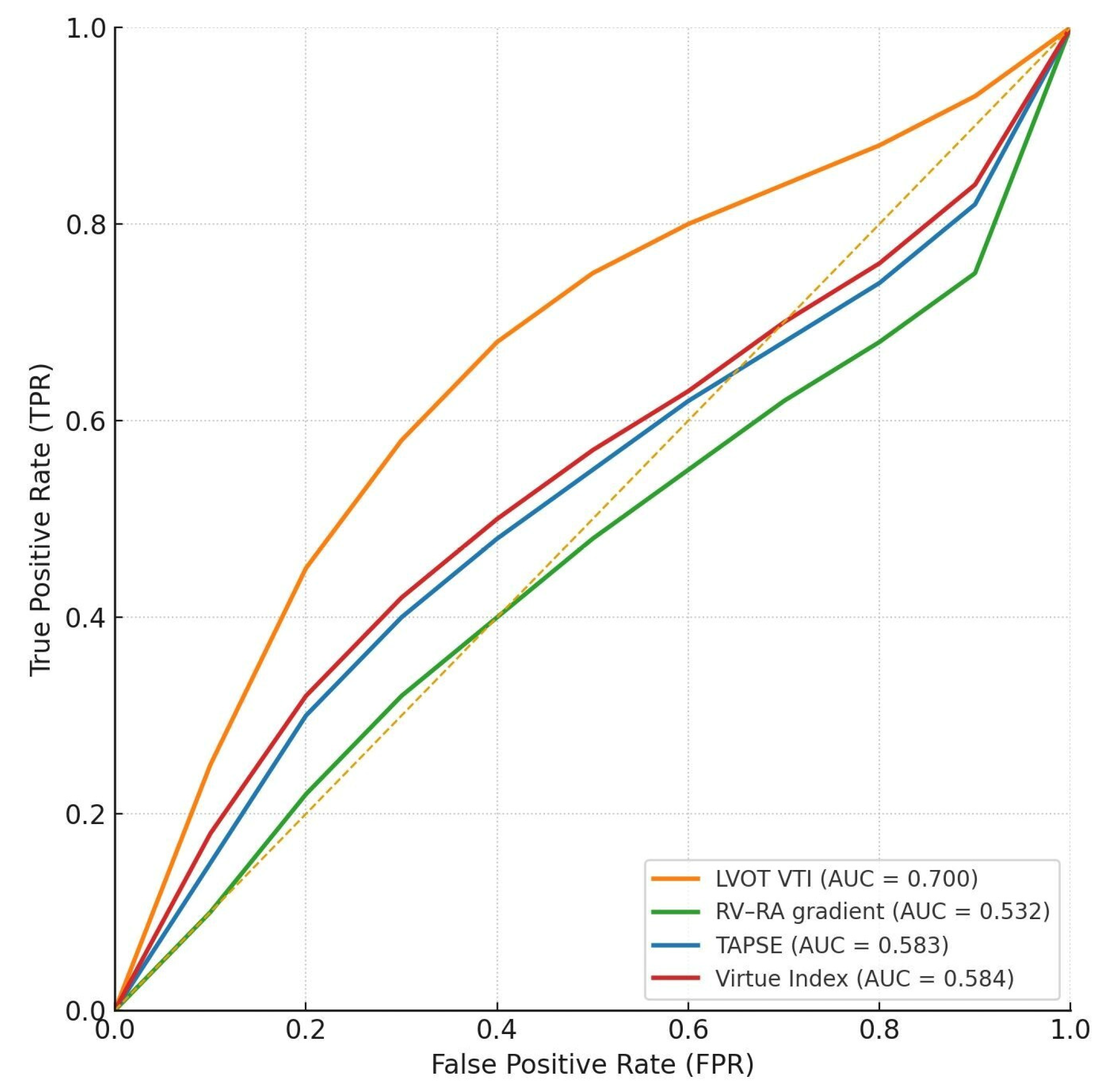
3.4. Pairwise AUC Comparisons Between Virtue and Conventional Parameters
Interpretation
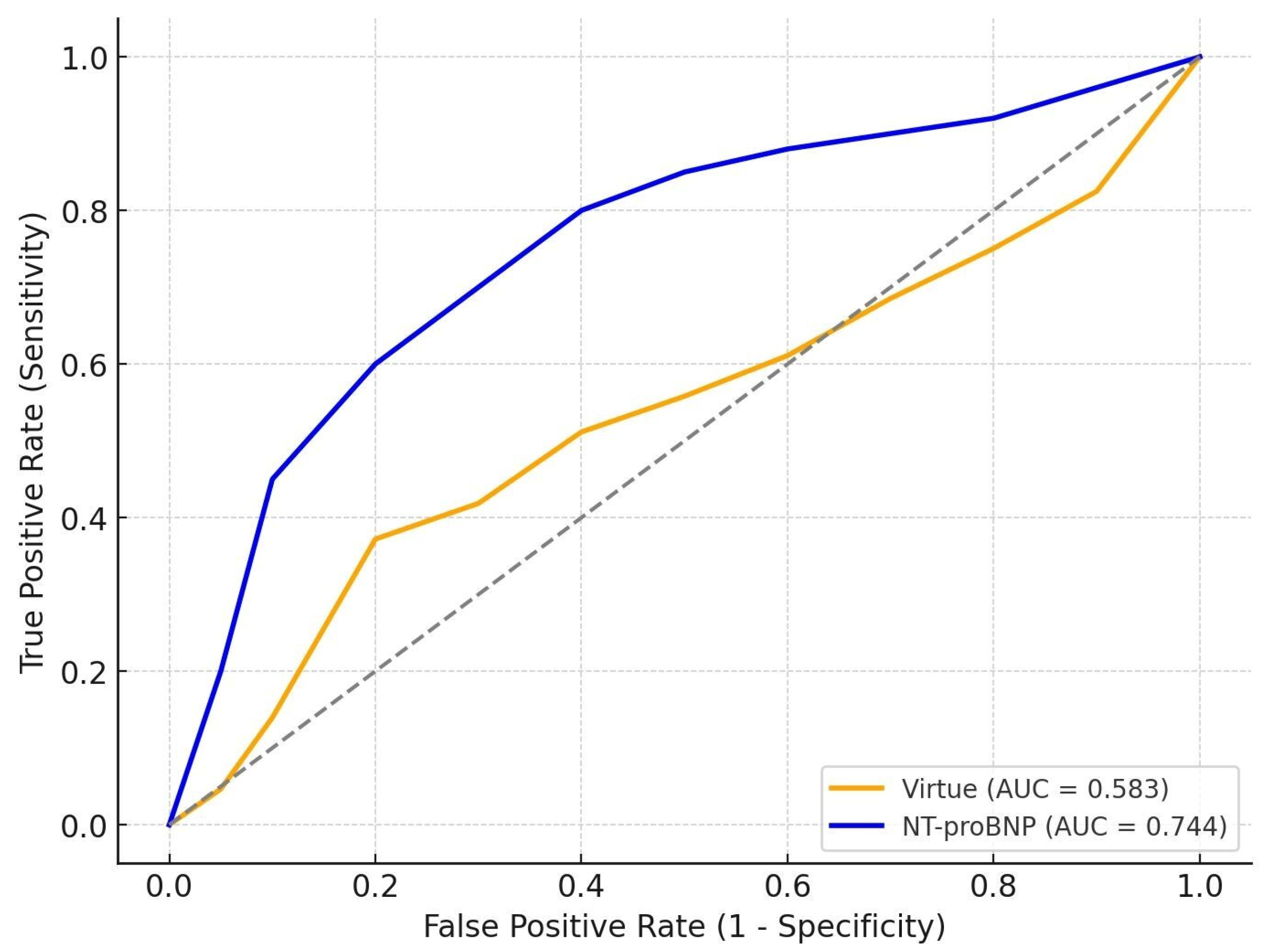
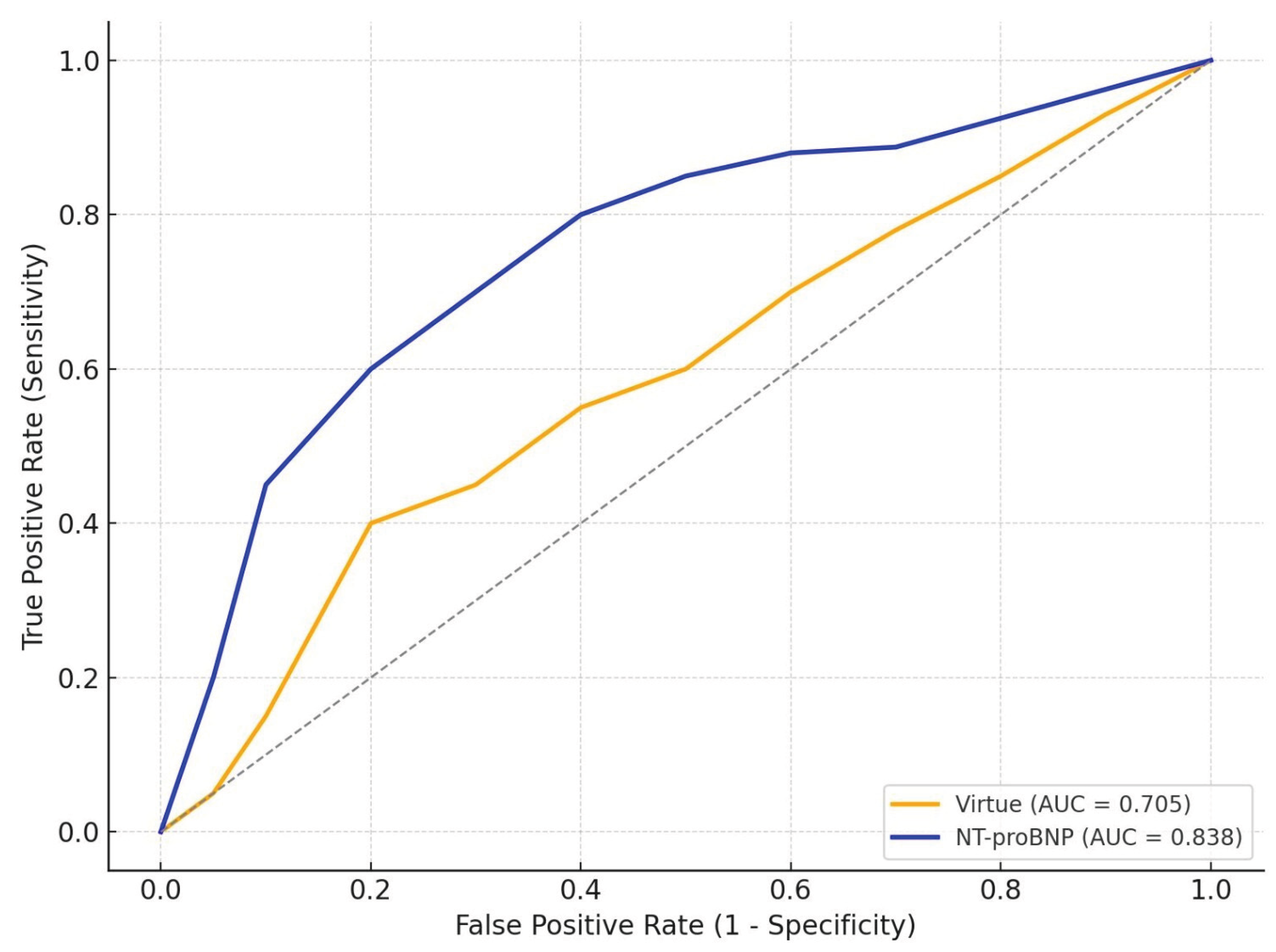
3.5. Comparative Prognostic Performance of Virtue and NT-proBNP
Interpretation
4. Discussion
5. Conclusions
Abbreviations
| AUC | Area Under the Curve |
| AHF | Acute Heart Failure |
| BP | Blood Pressure |
| CAD | Coronary Artery Disease |
| CI | Confidence Interval |
| EF | Ejection Fraction |
| ESC | European Society of Cardiology |
| eGFR | Estimated Glomerular Filtration Rate |
| HFpEF | Heart Failure with Preserved Ejection Fraction |
| HFrEF | Heart Failure with Reduced Ejection Fraction |
| IQR | Interquartile Range |
| LV | Left Ventricle |
| LVEF | Left Ventricular Ejection Fraction |
| LVOT VTI | Left Ventricular Outflow Tract Velocity Time Integral |
| NT-proBNP | N-terminal pro B-type Natriuretic Peptide |
| ROC | Receiver Operating Characteristic |
| RV | Right Ventricle |
| RV- RA gradient | Right Ventricular to Right Atrial Pressure Gradient |
| SD | Standard Deviation |
| TAPSE | Tricuspid Annular Plane Systolic Excursion |
References
- Ambrosy AP, Fonarow GC, Butler J, Chioncel O, Greene SJ, Vaduganathan M, et al. The global health and economic burden of hospitalizations for heart failure: lessons learned from hospitalized heart failure registries. J Am Coll Cardiol. 2014;63(12):1123–33. [CrossRef]
- Chioncel O, Mebazaa A, Harjola VP, Coats AJ, Piepoli MF, Crespo-Leiro MG, et al.; ESC Heart Failure Long-Term Registry Investigators. Clinical phenotypes and outcome of patients hospitalized for acute heart failure: the ESC Heart Failure Long-Term Registry. Eur J Heart Fail. 2017;19(10):1242–54. [CrossRef]
- Gandhi SK, Powers JC, Nomeir AM, Fowle K, Kitzman DW, Rankin KM, et al. The pathogenesis of acute pulmonary edema associated with hypertension. N Engl J Med. 2001;344(1):17–22.
- Gheorghiade M, De Luca L, Fonarow GC, Filippatos G, Metra M, Francis GS. Pathophysiologic targets in the early phase of acute heart failure syndromes. Am J Cardiol. 2005;96(6A):11G–17G. [CrossRef]
- Ponikowski P, Voors AA, Anker SD, Bueno H, Cleland JGF, Coats AJS, et al. 2016 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J. 2016;37(27):2129–200. [CrossRef]
- Shah SJ, Katz DH, Deo RC. Phenotypic spectrum of heart failure with preserved ejection fraction. Heart Fail Clin. 2014;10(3):407–18. [CrossRef]
- Passantino A, Scrutinio D. Risk stratification in acute heart failure: we need a new agenda for clinical research. Int J Cardiol. 2019;293:179–80. [CrossRef]
- McCullough PA, Nowak RM, McCord J, Hollander JE, Herrmann HC, Steg PG, et al. B-type natriuretic peptide and clinical judgment in emergency diagnosis of heart failure: analysis from the Breathing Not Properly Multinational Study. Circulation. 2002;106(4):416–22. [CrossRef]
- Maisel AS, Krishnaswamy P, Nowak RM, McCord J, Hollander JE, Duc P, et al.; Breathing Not Properly Multinational Study Investigators. Rapid measurement of B-type natriuretic peptide in the emergency diagnosis of heart failure. N Engl J Med. 2002;347(3):161–7. [CrossRef]
- Januzzi JL Jr, Camargo CA, Anwaruddin S, Baggish AL, Chen AA, Krauser DG, et al. The N-terminal Pro-BNP investigation of dyspnea in the emergency department (PRIDE) study. Am J Cardiol. 2005;95(8):948–54. [CrossRef]
- Rudski LG, Lai WW, Afilalo J, Hua L, Handschumacher MD, Chandrasekaran K, et al. Guidelines for the echocardiographic assessment of the right heart in adults. J Am Soc Echocardiogr. 2010;23(7):685–713. [CrossRef]
- Obokata M, Reddy YNV, Borlaug BA. The role of echocardiography in heart failure with preserved ejection fraction: what do we want from imaging? Heart Fail Clin. 2019;15(2):241–56. [CrossRef]
- Dini FL, Barletta V, Ballo P, Cioffi G, Pugliese NR, Rossi A, et al. Left ventricular outflow indices in chronic systolic heart failure: thresholds and prognostic value. Echocardiography. 2025;42(2):e70109. [CrossRef]
- Omote K, Nagai T, Iwano H, Tsujinaga S, Kamiya K, Aikawa T, et al. Left ventricular outflow tract velocity time integral in hospitalized heart failure with preserved ejection fraction. ESC Heart Fail. 2020;7(1):167–75. [CrossRef]
- Haddad F, Doyle R, Murphy DJ, Hunt SA. Right ventricular function in cardiovascular disease, part II: pathophysiology, clinical importance, and management of right ventricular failure. Circulation. 2008;117(13):1717–31. [CrossRef]
- Guazzi M, Naeije R, Arena R, Corrà U, Ghio S, Forfia P, et al. Echocardiography of right ventriculoarterial coupling combined with cardiopulmonary exercise testing to predict outcome in heart failure. Chest. 2015;148(1):226–34. [CrossRef]
- Grapsa J, Dawson D, Nihoyannopoulos P. Assessment of right ventricular structure and function in pulmonary hypertension. J Cardiovasc Ultrasound. 2011;19(3):115–25. [CrossRef]
- Wu VC, Takeuchi M. Echocardiographic assessment of right ventricular systolic function. Cardiovasc Diagn Ther. 2018;8(1):70–9. [CrossRef]
- Brener MI, Kanwar MK, Lander MM, Hamid NB, Raina A, Sethi SS, et al. Impact of interventricular interaction on ventricular function: insights from right ventricular pressure–volume analysis. JACC Heart Fail. 2024;12(7):1179–92. [CrossRef]
- Popescu DC, Ciobanu M, Țînț D, Nechita AC. Linking heart function to prognosis: the role of a novel echocardiographic index and NT-proBNP in acute heart failure. Medicina (Kaunas). 2025;61:1412.
- McDonagh TA, Metra M, Adamo M, Gardner RS, Baumbach A, Böhm M, et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur Heart J. 2021;42(36):3599–726. [CrossRef]
- Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L, et al. Recommendations for cardiac chamber quantification by echocardiography in adults. Eur Heart J Cardiovasc Imaging. 2015;16(3):233–70. [CrossRef]
- Nagueh SF, Smiseth OA, Appleton CP, Byrd BF 3rd, Dokainish H, Edvardsen T, et al. Recommendations for the evaluation of left ventricular diastolic function by echocardiography. J Am Soc Echocardiogr. 2016;29(4):277–314. [CrossRef]
- Badano LP, Addetia K, Pontone G, Torlasco C, Lang RM, Parati G, et al. Advanced imaging of right ventricular anatomy and function. Heart. 2020;106(19):1469–76. [CrossRef]
- Pandit K, Mukhopadhyay P, Ghosh S, Chowdhury S. Natriuretic peptides: diagnostic and therapeutic use. Indian J Endocrinol Metab. 2011;15(Suppl 4):S345–53. [CrossRef]
- Tsutsui H, Albert NM, Coats AJS, Anker SD, Bayes-Genis A, Butler J, et al. Natriuretic peptides: role in the diagnosis and management of heart failure. Eur J Heart Fail. 2023;25(5):616–31. [CrossRef]
- Wettersten, N. Biomarkers in acute heart failure: diagnosis, prognosis, and treatment. Int J Heart Fail. 2021;3(2):81–105. [CrossRef]
- Kim, TK. T test as a parametric statistic. Korean J Anesthesiol. 2015;68(6):540–6. [CrossRef]
- Nachar, N. The Mann–Whitney U: a test for assessing whether two independent samples come from the same distribution. Quant Methods Psychol. 2008;4(1):13–20. [CrossRef]
- McDonald, JH. Handbook of Biological Statistics. 3rd ed. Baltimore: Sparky House Publishing; 2014.
- World Medical Association. World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA. 2013;310(20):2191–4. [CrossRef]
- Palazzuoli A, Cartocci A, Pirrotta F, Vannuccini F, Campora A, Martini L, et al. Different right ventricular dysfunction and pulmonary coupling in acute heart failure according to left ventricular ejection fraction. Prog Cardiovasc Dis. 2023;81:89–97. [CrossRef]
- Huttin O, Fraser AG, Lund LH, Donal E, Linde C, Kobayashi M, et al.; MEDIA and KaRen investigators. Risk stratification with echocardiographic biomarkers in heart failure with preserved ejection fraction: the MEDIA Echo Score. ESC Heart Fail. 2021;8(3):1827–39. [CrossRef]
- Melenovsky V, Hwang SJ, Lin G, Redfield MM, Borlaug BA. Right heart dysfunction in heart failure with preserved ejection fraction. Eur Heart J. 2014;35(48):3452–62. [CrossRef]
- Tschöpe C, Birner C, Böhm M, Bruder O, Frantz S, Luchner A, et al. Heart failure with preserved ejection fraction: current management and future strategies. Clin Res Cardiol. 2018;107(1):1–19. [CrossRef]
- Wang J, Li X, Jiang J, Luo Z, Tan X, Ren R, et al. Right ventricular–pulmonary arterial coupling and outcome in heart failure with preserved ejection fraction. Clin Cardiol. 2024;47(7):e24308. [CrossRef]
- Tabima DM, Philip JL, Chesler NC. Right ventricular–pulmonary vascular interactions. Physiology (Bethesda). 2017;32(5):346–56. [CrossRef]
- Núñez J, de la Espriella R, Rossignol P, Voors AA, Mullens W, Metra M, et al. Congestion in heart failure: a circulating biomarker-based perspective. Eur J Heart Fail. 2022;24(10):1751–66. [CrossRef]
- Guazzi M, Villani S, Generati G, Bandera F, et al. Right ventricular contractile reserve and pulmonary circulation uncoupling during exercise challenge in heart failure: pathophysiology and clinical phenotypes. JACC Heart Fail. 2016;4(8):625–35. [CrossRef]
- Troughton RW, Richards AM. B-type natriuretic peptides and echocardiographic measures of cardiac structure and function. JACC Cardiovasc Imaging. 2009;2(2):216–25. [CrossRef]
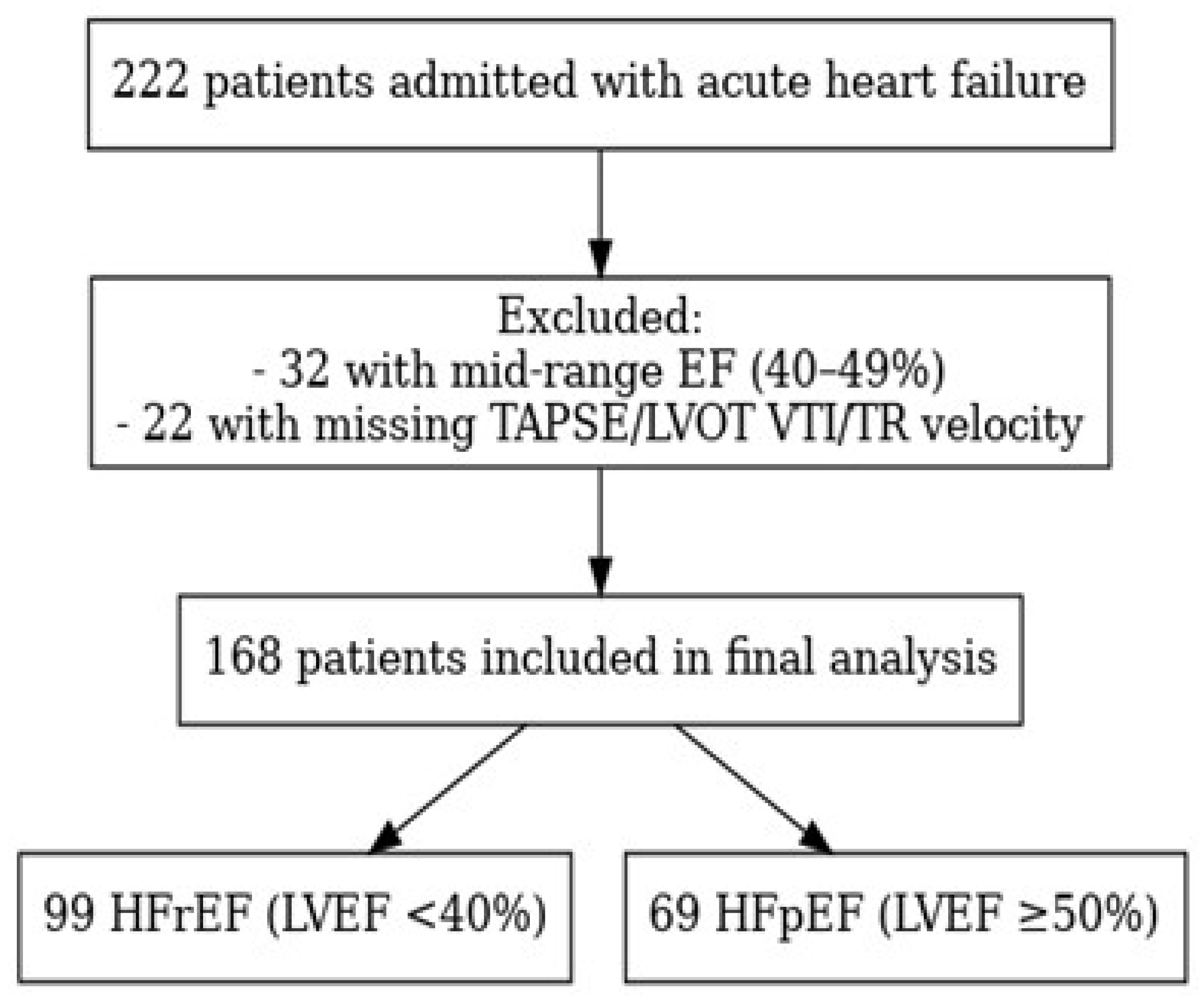
| Variable | Total (n = 168) | HFrEF (n = 99) | HFpEF (n = 69) | p-value |
| Age (years) | 71 ± 14 | 65,9 ± 14,9 | 77.6 ± 9.6 | < 0.001 |
| Male sex, % | 50.6% | 66.7% | 27.5% | < 0.001 |
| Smoking, % | 25.5% | 36.4% | 8.7% | < 0.001 |
| Hypertension, % | 88.1% | 82.8% | 95.7% | 0.017 |
| Dyslipidemia, % | 94.6% | 94.9% | 94.2% | 0.830 |
| Obesity, % | 28.1% | 30.3% | 24.6% | 0.460 |
| Diabetes mellitus, % | 39.9% | 41.4% | 37.7% | 0.630 |
| Valvular heart disease, % | 78.0% | 80.8% | 73.9% | 0.290 |
| Systolic BP (mmHg) | 143 ± 31 | 143 ± 31 | 142 ± 31 | 0.837 |
| Diastolic BP (mmHg) | 85 ± 17 | 87 ± 17 | 81 ± 17 | 0.026 |
| NT-proBNP (pg/mL) | 7830 [3698 – 21764] | 8453 [4957 – 21121] | 6537 [2180 – 24554] | 0.411 |
| RV-RA gradient (mmHg) | 30.0 [22.8 – 40.0] | 17.0 [14.0 – 22.0] | 21.0 [17.0 – 24.0] | < 0.001 |
| TAPSE (mm) | 21 ± 9 | 20 ± 10 | 21 ± 7 | 0.410 |
| LVOT VTI (cm) | 16 ± 5 | 14 ± 4 | 21 ± 7 | < 0.001 |
| LVEF (%) | 41 ± 18 | 28 ± 7 | 60 ± 7 | < 0.001 |
| Atrial fibrillation | 47.0% | 36.4% | 62.3% | 0.002 |
| CAD | 45.8% | 58.6% | 27.5% | < 0.001 |
| eGFR at admission | 60.0 [44.8 – 81.0] | 63.0 [46.0 – 81.5] | 54.0 [44.0 – 80.0] | 0.030 |
| In-hospital mortality | 10.1% | 9.1% | 11.6% | 0.788 |
| Virtue Index | 0.098 [0.057 – 0.190] | 0.135 [0.069 – 0.215] | 0.075 [0.049 – 0.110] | < 0.001 |
| Group | Predictor | N | Events | AUC | CI95 LOWER | CI95 UPPER | p-value |
| HFrEF | Virtue Index | 99 | 9 | 0.584 | 0.364 | 0.791 | 0.441 |
| HFrEF | RV-RA gradient | 105 | 9 | 0.532 | 0.463 | 0.724 | 0.631 |
| HFrEF | TAPSE | 105 | 9 | 0.583 | 0.454 | 0.770 | 0.303 |
| HFrEF | LVOT VTI | 102 | 9 | 0.700 | 0.530 | 0.850 | 0.014 |
| HFpEF | Virtue Index | 69 | 8 | 0.704 | 0.536 | 0.852 | 0.011 |
| HFpEF | RV-RA gradient | 76 | 8 | 0.724 | 0.542 | 0.902 | 0.015 |
| HFpEF | TAPSE | 76 | 8 | 0.637 | 0.457 | 0.891 | 0.216 |
| HFpEF | LVOT VTI | 71 | 8 | 0.669 | 0.456 | 0.861 | 0.102 |
| Group | N_pairs | Spearman_rho | CI95_lower | CI95_upper | p-value |
| HFrEF | 96 | 0.191 | -0.006 | 0.384 | 0.061 |
| HFpEF | 66 | 0.380 | 0.134 | 0.580 | 0.002 |
| Group | Comparison | Delta_AUC(Virtue - X) | Z | p-value | N_common |
| HFrEF | Virtue vs RV–RA gradient | 0.052 | 0.407 | 0.684 | 99 |
| HFrEF | Virtue vs TAPSE | 0.001 | 0.008 | 0.994 | 99 |
| HFrEF | Virtue vs LVOT VTI | -0.116 | -0.894 | 0.372 | 99 |
| HFpEF | Virtue vs RV–RA gradient | -0.020 | -0.186 | 0.852 | 69 |
| HFpEF | Virtue vs TAPSE | 0.067 | 0.504 | 0.614 | 69 |
| HFpEF | Virtue vs LVOT VTI | 0.035 | 0.277 | 0.782 | 69 |
| Group | N | AUC_Virtue | AUC_NTproBNP | p-value |
| HFrEF | 99 | 0.583 | 0.744 | 0.040 |
| HFpEF | 69 | 0.705 | 0.838 | 0.050 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




