Submitted:
05 November 2025
Posted:
06 November 2025
You are already at the latest version
Abstract
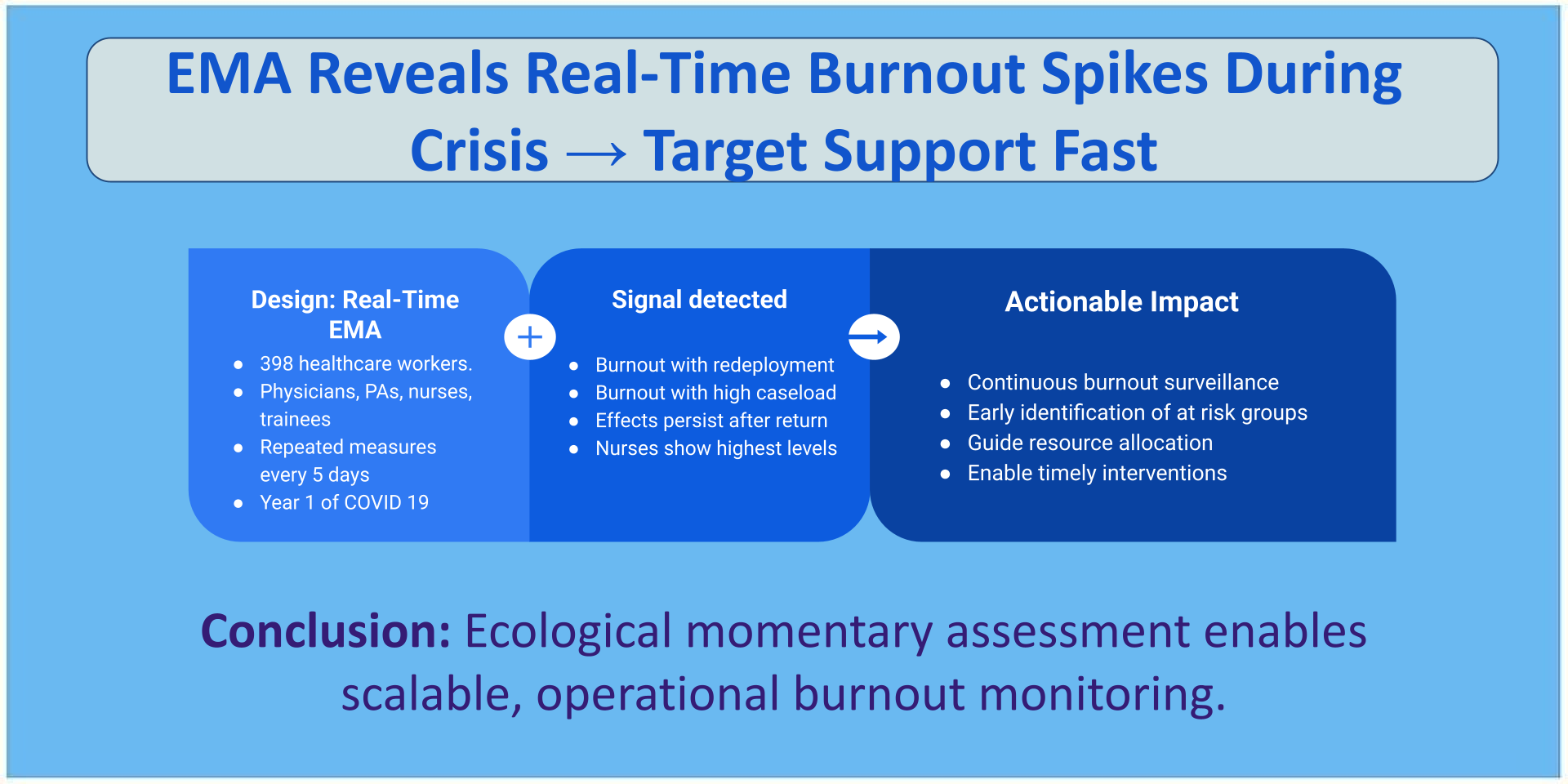
Keywords:
1. Introduction
2. Materials and Methods
2.1. Design
2.2. Data Collection
2.2.1. Demographic and Professional Information
2.2.2. Redeployment
2.2.3. Burnout
2.2.4. Caseload and Case Severity
2.2.5. Participant Comments
2.3. Data Analysis-Survey
2.4. Data Analysis-Comments
3. Results
3.1. Characteristics of the Sample
3.2. Demographic Data
3.3. Redeployment
Redeployment and Burnout
3.4. Analyses
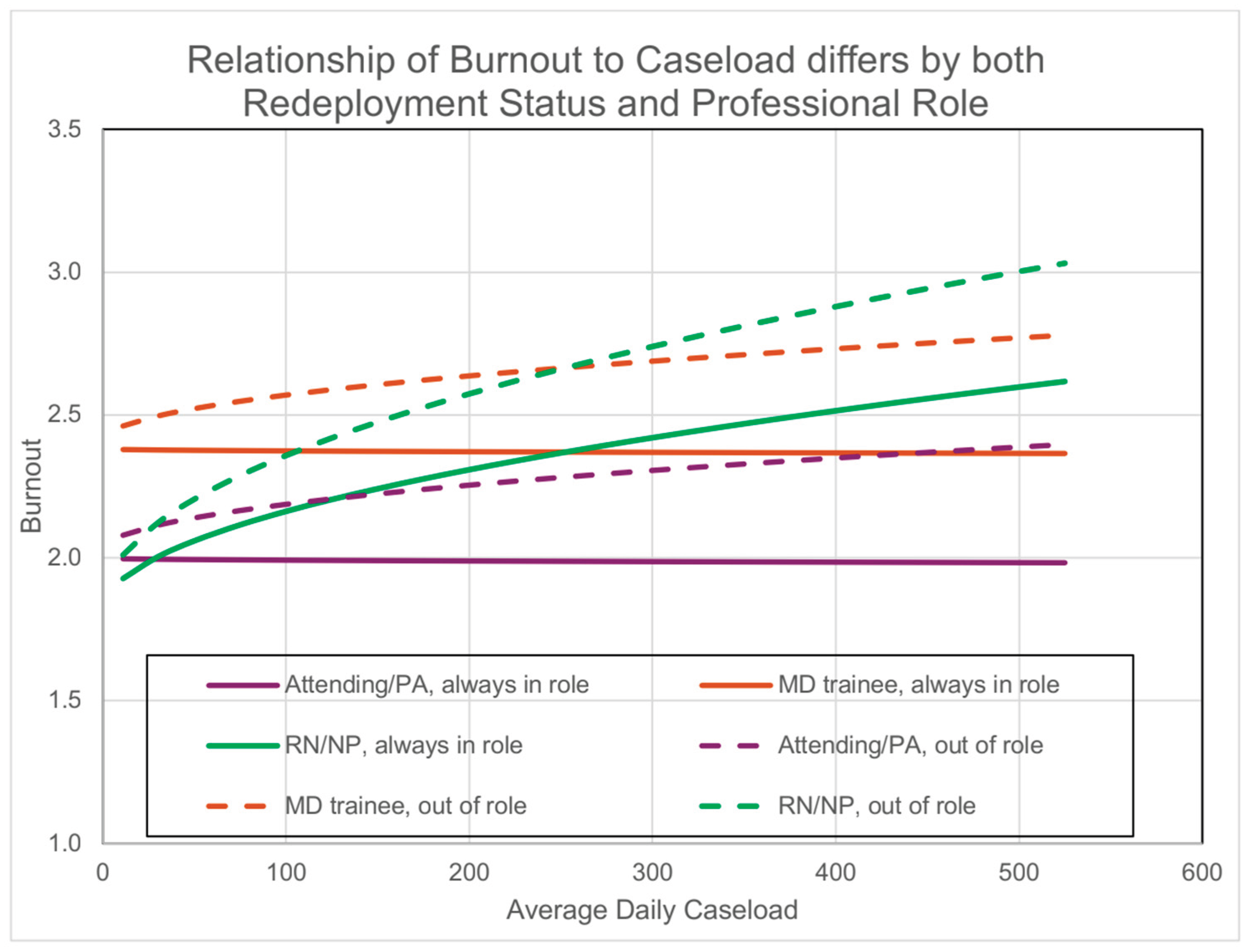
3.4.1. Role-Specific Burnout Trends
3.4.2. Combined Impact of Caseload and Redeployment
3.4.3. Long-Term Burnout Effects of Redeployment
3.5. Analysis of Comments
- Being reassigned to unfamiliar roles with minimal notice.
- Insufficient training for redeployed responsibilities.
- Lack of guidance regarding policies and procedures on new units.
- Concerns about personal safety in less familiar environments.
4. Discussion
5. Conclusions
- Adopt Real-Time Monitoring: Implement EMA or similar tools to continuously track staff well-being and burnout during emergencies. These tools enable the early identification of at-risk individuals and allow for dynamic, data-driven interventions tailored to evolving conditions.
- Develop Redeployment Protocols: Establish structured protocols that include preemptive training, clear role-specific guidance, and organized hand-off processes to reduce the stress of sudden redeployment, allowing for dynamic caseload adjustments during surges.
- Integrate Mental Health and Peer Support Programs: Provide accessible mental health resources and establish peer support networks to address the emotional challenges associated with redeployment and high workloads. These programs should be sustained beyond crises to support long-term workforce well-being.
- Enhance Organizational Communication: Maintain consistent and transparent communication channels to disseminate updates on policies, expectations, and available resources. Clear communication fosters trust and reduces uncertainty during crises.
- Expand Professional Development Opportunities: Offer cross-training and professional development programs to prepare staff for redeployment scenarios. Building skills across roles can ease transitions during emergencies and reduce stress by fostering confidence in diverse responsibilities.
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| EMA | Ecological Momentary Assessment |
| MMLM | Multilevel mixed-effects model |
| REDCap | Research Electronic Data Capture |
| SAS | Statistical Analysis System |
Appendix A
| Effect | Estimate | Standard Error |
DF | t-Value | Pr > |t| | Lower | Upper |
|---|---|---|---|---|---|---|---|
| Intercept | 2.01 | 1.11 | 1253 | 1.81 | 0.07 | -0.1739 | 4.1986 |
| Caseloads x 100 | -0.007 | 0.13 | 1539 | -0.06 | 0.96 | -0.2526 | 0.2385 |
|
Trainee (Resident/Fellow) vs Attending Physicians |
0.38 | 0.13 | 368.5 | 2.87 | 0.0043* | 0.1205 | 0.6445 |
| Nurse/NP vs Attending Physicians | -0.19 | 0.14 | 291.9 | -1.33 | 0.17 | -0.4676 | 0.09122 |
| Caseloads x 100 * Nurse/NP vs. all others | 0.36 | 0.075 | 228.2 | 4.82 | <.0001* | 0.2122 | 0.5061 |
| Sex (Women vs Men) | 0.26 | 0.10 | 351.8 | 2.54 | 0.01 | 0.05794 | 0.4564 |
|
Redeployment Status (Out of role at the time of survey completion) |
-0.099 | 0.063 | 3837 | -1.56 | 0.12 | -0.2227 | 0.02529 |
| Caseloads x 100 * Redeployment Status | 0.17 | 0.049 | 3317 | 3.45 | 0.0006* | 0.07285 | 0.2653 |
|
History of redeployment: Pre vs post periods of redeployment |
0.13 | 0.049 | 2223 | 2.56 | 0.0104* | 0.02944 | 0.2208 |
References
- Tawfik DS, Scheid A, Profit J, et al. Evidence relating health care provider burnout and quality of care: a systematic review and meta-analysis. Ann Intern Med. 2019;171(8):555-567. [CrossRef]
- Montgomery AP, Azuero A, Baernholdt M, et al. Nurse burnout predicts self-reported medication administration errors in acute care hospitals. J Healthc Qual. 2021;43(1):13-23. [CrossRef]
- Shanafelt TD, Hasan O, Dyrbye LN, et al. Changes in burnout and satisfaction with work-life balance in physicians and the general US working population between 2011 and 2014. Mayo Clin Proc. 2015;90(12):1600-1613. [CrossRef]
- Dionisi T, Sestito L, Tarli C, et al. Risk of burnout and stress in physicians working in a COVID team: a longitudinal survey. Int J Clin Pract. 2021;75(11):e14755. [CrossRef]
- Shanafelt TD, Noseworthy JH. Executive leadership and physician well-being: nine organizational strategies to promote engagement and reduce burnout. Mayo Clin Proc. 2017;92(1):129-146. [CrossRef]
- Abate SM, Ahmed Ali S, Mantfardo B, Basu B. Rate of intensive care unit admission and outcomes among patients with coronavirus: a systematic review and meta-analysis. PLoS One. 2020;15(7):e0235653. [CrossRef]
- Satomi E, Souza PMR, Thomé BDC, et al. Fair allocation of scarce medical resources during COVID-19 pandemic: ethical considerations. Einstein (Sao Paulo). 2020;18:eAE5775. [CrossRef]
- Singh V, Young JQ, Malhotra P, et al. Evaluating burnout during the COVID-19 pandemic among physicians in a large health system in New York. Arch Environ Occup Health. 2022;77(10):819-827. [CrossRef]
- Coughlan C, Nafde C, Khodatars S, et al. COVID-19: lessons for junior doctors redeployed to critical care. Postgrad Med J. 2021;97(1145):188-191. [CrossRef]
- Emanuel EJ, Persad G, Upshur R, et al. Fair allocation of scarce medical resources in the time of COVID-19. n Engl J Med. 2020;382(21):2049-2055. [CrossRef]
- Vera San Juan N, Clark SE, Camilleri M, et al. Training and redeployment of healthcare workers to intensive care units during the COVID-19 pandemic: a systematic review. BMJ Open. 2022;12(1):e050038. [CrossRef]
- Denning M, Goh ET, Tan B, et al. Determinants of burnout and other aspects of psychological well-being in healthcare workers during the COVID-19 pandemic: a multinational cross-sectional study. PLoS One. 2021;16(4):e0238666. [CrossRef]
- Ferry AV, Wereski R, Strachan FE, Mills NL. Predictors of UK healthcare worker burnout during the COVID-19 pandemic. QJM. 2021;114(6):374-380. [CrossRef]
- Piercy H, Kelly S, Wills M, Croston M. Psychological impact of caring during the COVID-19 pandemic on HIV nurses. Br J Nurs. 2022;31(1):S10-S15. [CrossRef]
- Kissel KA, Filipek C, Folz E, Jenkins J. The impact of a three-tiered model of nursing redeployment during the COVID-19 pandemic: a cross-sectional study. Intensive Crit Care Nurs. 2023;77:103431. [CrossRef]
- Doherty K, Balaskas A, Doherty G. The design of ecological momentary assessment technologies. Interact Comput. 2020;32(3):257-278. [CrossRef]
- Shiffman S, Stone AA, Hufford MR. Ecological momentary assessment. Annu Rev Clin Psychol. 2008;4:1-32. [CrossRef]
- Pan CX, Crupi R, August P, et al. An intensive longitudinal assessment approach to surveilling trajectories of burnout over the first year of the COVID pandemic. Int J Environ Res Public Health. 2023;20(4):2930. [CrossRef]
- Shea JA, Bellini LM, Desai SV, et al. Exploring residents’ well-being and burnout via qualitative ecological momentary assessment. Acad Med. 2022;97(3):414-419. [CrossRef]
- Mengelkoch S, Moriarity DP, Novak AM, Snyder MP, Slavich GM, Lev-Ari S. Using ecological momentary assessments to study how daily fluctuations in psychological states impact stress, well-being, and health. J Clin Med. 2023;13(1):24. [CrossRef]
- Versluis A, Verkuil B, Spinhoven P, van der Ploeg MM, Brosschot JF. Changing mental health and positive psychological well-being using ecological momentary interventions: a systematic review and meta-analysis. J Med Internet Res. 2016;18(6):e152. [CrossRef]
- Luceño-Moreno L, Talavera-Velasco B, Vázquez-Estévez D, Martín-García J. Mental health, burnout, and resilience in healthcare professionals after the first wave of COVID-19 pandemic in Spain: a longitudinal study. J Occup Environ Med. 2022;64(3):e114-e123. [CrossRef]
- Dolan ED, Mohr D, Lempa M, et al. Using a single item to measure burnout in primary care staff: a psychometric evaluation. J Gen Intern Med. 2015;30(5):582-587. [CrossRef]
- Helfrich CD, Simonetti JA, Clinton WL, et al. The association of team-specific workload and staffing with odds of burnout among VA primary care team members. J Gen Intern Med. 2017;32(7):760-766. [CrossRef]
- Boussat B, Kamalanavin K, François P. The contribution of open comments to understanding the results from the Hospital Survey on Patient Safety Culture (HSOPS): a qualitative study. PLoS One. 2018;13(4):e0196089. [CrossRef]
- Schroeder K, Norful AA, Travers J, Aliyu S. Nursing perspectives on care delivery during the early stages of the COVID-19 pandemic: a qualitative study. Int J Nurs Stud Adv. 2020;2:100006. [CrossRef]
- Norful AA, Rosenfeld A, Schroeder K, Travers JL, Aliyu S. Primary drivers and psychological manifestations of stress in frontline healthcare workforce during the initial COVID-19 outbreak in the United States. Gen Hosp Psychiatry. 2021;69:20-26. [CrossRef]
- Aiken LH, Lasater KB, Sloane DM, et al. Physician and nurse well-being and preferred interventions to address burnout in hospital practice: factors associated with turnover, outcomes, and patient safety. JAMA Health Forum. 2023;4(7):e231809. [CrossRef]
| Theme | Percent of Comments (%) |
|---|---|
| Increased stress | 27.35% |
| Lack of support | 24.63% |
| Poor staffing | 20.87% |
| Discontent with redeployment | 17.75% |
| Feelings of burnout | 13.57% |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




