Submitted:
03 October 2025
Posted:
07 October 2025
You are already at the latest version
Abstract
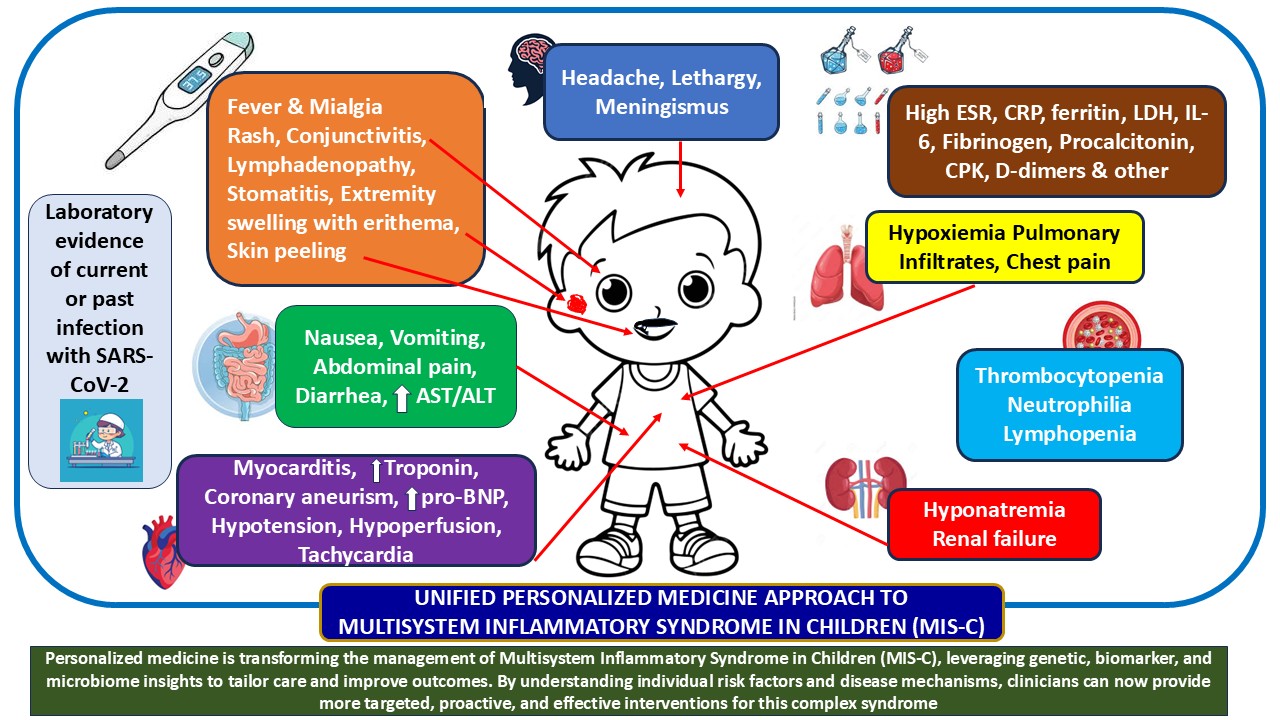
Keywords:
1. Introduction
2. MIS-C Pathophysiology and Proposed Mechanisms
3. Core Principles of Personalized Medicine in MIS-C
4. Genetic Predisposition and Host Susceptibility
5. Biomarkers as Tools for Precision Diagnosis and Risk Stratification
6. Pharmacogenomics and Targeted Immunomodulatory Therapies
7. The Gut Microbiome as a Novel Therapeutic Frontier
8. Clinical Features and Systemic Manifestations
- Cardiovascular Involvement: This is a hallmark of MIS-C and a major determinant of disease severity and prognosis. Patients frequently present with myocardial inflammation and a significantly depressed left ventricular ejection fraction, an abnormality observed in over 45% of patients in one review. Coronary artery dilation or aneurysms are also common and may not be present on initial echocardiograms but can develop over several days. Cardiovascular collapse leading to shock is the most striking and severe clinical manifestation, occurring in 40% to 80% of patients. This prevalence is significantly higher than the rate observed in children with Kawasaki disease, where shock is present in less than 10% of cases. Other common cardiac symptoms include low blood pressure, a very high or irregular heart rate, and chest pain. The high prevalence of shock and profound cardiac dysfunction underscores a more acute and fulminant illness compared to other inflammatory conditions.
- Gastrointestinal Involvement: Gastrointestinal symptoms are highly prevalent in MIS-C, with reports indicating they occur in 60% to 100% of cases. Patients commonly experience severe abdominal pain, vomiting, and diarrhea, with clinical presentations that can sometimes mimic acute appendicitis.
- Dermatologic and Mucocutaneous Signs: While these manifestations are often present, they tend to be less frequent than in Kawasaki disease. They include a variety of rashes (e.g., macules, papules, urticarial-like lesions, and rarely petechial or purpuric skin lesions), conjunctival injection (red or bloodshot eyes), inflamed mucous membranes, cracked lips, and a swollen tongue with a characteristic “strawberry” appearance. Swollen or red hands and feet are also frequently observed.
- Neurologic and Hematologic Involvement: Neurologic symptoms are usually transient, presenting as headaches or an altered mental state. Patients may also experience confusion, neck pain, numbness, or tingling in the hands and feet. However, rare but severe neurologic events such as encephalopathy, stroke, demyelination, and seizures have been documented. Hematologic abnormalities are also common and serve as important differentiating features. Many patients exhibit a low absolute lymphocyte count (lymphopenia) in 37% to 81% of cases and low platelet count (thrombocytopenia) in 11% to 31% of cases, findings that are rare in Kawasaki disease.
- Other Manifestations: Other systemic symptoms can include respiratory issues such as cough and shortness of breath, swollen lymph nodes in the neck, and generalized malaise with fatigue and muscle pain.
9. The Diagnostic and Evaluative Pathway
10. Therapeutic Management and Clinical Care
11. MIS-C and Kawasaki Disease: A Comparative Analysis
12. Emerging Biomarkers and Future Research Directions
13. Conclusions
References
- Demharter, N.S.; Rao, P.; Scalzi, L.V.; Ericson, J.E.; Clarke, S. Prolonged Thrombocytopenia in a Case of MIS-C in a Vaccinated Child. J Investig Med High Impact Case Rep. 2023, 11, 23247096221145104. [Google Scholar] [PubMed]
- Mayo Clinic. Multisystem inflammatory syndrome in children (MIS-C) and COVID-19. Available online: https://www.mayoclinic.org/diseases-conditions/mis-c-in-kids-covid-19/symptoms-causes/syc-20502550#:~:text=Overview,Products%20&%20Services (accessed on 12 September 2025).
- Multisystem inflammatory syndrome in children (MIS-C) associated with coronavirus disease 2019 (COVID-19). Centers for Disease Control and Prevention. Available online: https://emergency.cdc.gov/han/2020/han00432.asp (accessed on 12 September 2025).
- Centers for Disease Control and Prevention. Clinical Overview of Multisystem Inflammatory Syndrome in Children. Available online: https://www.cdc.gov/mis/hcp/clinical-overview/index.html#:~:text=The%20child%20may%20have%20been%20infected%20from,effective%20at%20reducing%20the%20risk%20of%20MIS%2DC (accessed on 12 September 2025).
- Melgar, M.; Lee, E.H.; Miller, A.D.; Lim, S.; Brown, C.M.; Yousaf, A.R.; et al. Council of State and Territorial Epidemiologists/CDC Surveillance Case Definition for Multisystem Inflammatory Syndrome in Children Associated with SARS-CoV-2 Infection—United States. MMWR Recomm Rep. 2022, 71, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Ciortea, D.A. Cardiac Manifestations and Emerging Biomarkers in Multisystem Inflammatory Syndrome in Children (MIS-C): A Systematic Review and Meta-Analysis. Life (Basel). 2025, 15, 805. [Google Scholar] [PubMed]
- Boston Children’s Hospital. Multisystem inflammatory syndrome in children (MIS-C). Available online: https://www.childrenshospital.org/conditions/mis-c (accessed on 12 September 2025).
- Shyong, O. Multisystem Inflammatory Syndrome in Children: A Comprehensive Review over the Past Five Years. J Intensive Care Med. 2025, 8850666251320558. [Google Scholar]
- Children’s Hospital of Philadelphia. Available online: https://www.chop.edu/clinical-pathway/multisystem-inflammatory-syndrome-mis-c-clinical-pathway (accessed on 12 September 2025).
- Ahmed, M.; Advani, S.; Moreira, A.; Zoretic, S.; Martinez, J.; Chorath, K.; et al. Multisystem inflammatory syndrome in children: A systematic review. EClinicalMedicine. 2020, 26, 100527. [Google Scholar] [CrossRef]
- Soczyńska, J. Intestinal Dysbiosis and Immune Activation in Kawasaki Disease and Multisystem Inflammatory Syndrome in Children: A Comparative Review of Mechanisms and Clinical Manifestations. Biomedicines. 2025, 13, 1953. [Google Scholar]
- Lupu, A. Multisystem inflammatory syndrome in children and Kawasaki disease. Front Immunol. 2025, 16, 1554787. [Google Scholar]
- Lee, P.I.; Hsueh, P.R. Multisystem inflammatory syndrome in children: A dysregulated autoimmune disorder following COVID-19. J Microbiol Immunol Infect. 2023, 56, 236–245. [Google Scholar]
- Yale Medicine. Multisystem inflammatory syndrome in children (MIS-C). Available online: https://www.yalemedicine.org/conditions/multisystem-inflammatory-syndrome-in-children-mis-c (accessed on 12 September 2025).
- Children’s Hospital of Philadelphia. Available online: https://www.chop.edu/clinical-pathway/multisystem-inflammatory-syndrome-mis-c-clinical-pathway (accessed on 12 September 2025).
- Ahmed, M.; Advani, S.; Moreira, A.; Zoretic, S.; Martinez, J.; Chorath, K.; et al. Multisystem inflammatory syndrome in children: A systematic review. EClinicalMedicine. 2020, 26, 100527. [Google Scholar] [CrossRef]
- Aronoff, S.C.; Hall, A.; Del Vecchio, M.T. The Natural History of Severe Acute Respiratory Syndrome Coronavirus 2-Related Multisystem Inflammatory Syndrome in Children: A Systematic Review. J Pediatric Infect Dis Soc. 2020, 9, 746–751. [Google Scholar]
- Feldstein, L.R.; Rose, E.B.; Horwitz, S.M.; Collins, J.P.; Newhams, M.M.; Son, M.B.F.; et al. Overcoming COVID-19 Investigators; CDC COVID-19 Response Team. Multisystem Inflammatory Syndrome in U.S. Children and Adolescents. N Engl J Med. 2020, 383, 334–346. [Google Scholar] [PubMed]
- Roarty, C.; Tonry, C.; McGinn, C.; et al. In depth characterisation of the proteome of MIS-C and post COVID-19 infection in children reveals inflammatory pathway activation and evidence of tissue damage. J Transl Med 2025, 23, 929. [Google Scholar] [CrossRef]
- Carzaniga, T.; Calcaterra, V.; Casiraghi, L.; Inzani, T.; Carelli, S.; Del Castillo, G.; Cereda, D.; Zuccotti, G.; Buscaglia, M. Dynamics of Multisystem Inflammatory Syndrome in Children (MIS-C) associated to COVID-19: Steady severity despite declining cases and new SARS-CoV-2 variants-a single-center cohort study. Eur J Pediatr. 2025, 184, 327. [Google Scholar] [CrossRef]
- Dourdouna, M.M.; Tatsi, E.B.; Syriopoulou, V.; Michos, A. Proteomic Signatures of Multisystem Inflammatory Syndrome in Children (MIS-C) Associated with COVID-19: A Narrative Review. Children (Basel). 2024, 11, 1174. [Google Scholar] [CrossRef]
- Bodansky, A.; Mettelman, R.C.; Sabatino, J.J.; Vazquez, S.E.; Chou, J.; Novak, N.; Moffitt, K.L.; et al. Molecular mimicry in multisystem inflammatory syndrome in children. Nature 2024, 632, 622–629. [Google Scholar] [CrossRef]
- Gruber, C.N.; Patel, R.S.; Trachtman, R.; Lepow, L.; Amanat, F.; Krammer, F.; Wilson, K.M.; Onel, K.; Geanon, D.; Tuballes, K.; et al. Mapping systemic inflammation and antibody responses in multisystem inflammatory syndrome in children (MIS-C). Cell 2020, 183, 982–995.e14. [Google Scholar] [CrossRef] [PubMed]
- Bellos, E.; Santillo, D.; Vantourout, P.; Jackson, H.R.; Duret, A.; Hearn, H.; et al. Heterozygous BTNL8 variants in individuals with multisystem inflammatory syndrome in children (MIS-C). J Exp Med. 2024, 221, e920240699. [Google Scholar] [CrossRef]
- Şener, S.; Batu, E.D.; Kaya Akca, Ü.; Atalay, E.; Kasap Cüceoğlu, M.; Balık, Z.; et al. Differentiating Multisystem Inflammatory Syndrome in Children from Kawasaki Disease During the Pandemic. Turk Arch Pediatr. 2024, 59, 150–156. [Google Scholar] [CrossRef] [PubMed]
- Benvenuto, S.; Avcin, T.; Taddio, A. Multisystem inflammatory syndrome in children: A review. Acta Paediatr. 2024, 113, 2011–2023. [Google Scholar] [CrossRef]
- Dashti, M.; AlKandari, H.; Malik, M.Z.; Nizam, R.; John, S.E.; Jacob, S.; Channanath, A.; Othman, F.; Al-Sayed, S.; Al-Hindi, O.; Al-Mutari, M.; Thanaraj, T.A.; Al-Mulla, F. Genetic insights into MIS-C Post-COVID-19 in Kuwaiti children: Investigating monogenic factors. Front Cell Infect Microbiol. 2025, 14, 1444216. [Google Scholar]
- Westphal, A.; Cheng, W.; Yu, J.; Grassl, G.; Krautkrämer, M.; Holst, O.; Föger, N.; Lee, K.H. Lysosomal trafficking regulator Lyst links membrane trafficking to toll-like receptor-mediated inflammatory responses. J Exp Med. 2017, 214, 227–244. [Google Scholar] [CrossRef]
- Chou, J.; Platt, C.D.; Habiballah, S.; Nguyen, A.A.; Elkins, M.; Weeks, S.; et al. Taking on COVID-19 Together Study Investigators. Mechanisms underlying genetic susceptibility to multisystem inflammatory syndrome in children (MIS-C). J Allergy Clin Immunol. 2021, 148, 732–738.e1. [Google Scholar] [CrossRef]
- Santos-Rebouças, C.B.; Piergiorge, R.M.; Dos Santos Ferreira, C.; Seixas Zeitel, R.; Gerber, A.L.; Rodrigues, M.C.F.; et al. Host genetic susceptibility underlying SARS-CoV-2-associated Multisystem Inflammatory Syndrome in Brazilian Children. Mol Med. 2022, 28, 153. [Google Scholar] [CrossRef]
- Gavriilaki, E.; Tsiftsoglou, S.A.; Touloumenidou, T.; Farmaki, E.; Panagopoulou, P.; Michailidou, E.; et al. Targeted Genotyping of MIS-C Patients Reveals a Potential Alternative Pathway Mediated Complement Dysregulation during COVID-19 Infection. Curr Issues Mol Biol. 2022, 44, 2811–2824. [Google Scholar] [CrossRef]
- Abuhammour, W.; Yavuz, L.; Jain, R.; Abu Hammour, K.; Al-Hammouri, G.F.; El Naofal, M.; et al. Genetic and Clinical Characteristics of Patients in the Middle East With Multisystem Inflammatory Syndrome in Children. JAMA Netw Open. 2022, 5, e2214985. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Clinical Treatment of Multisystem Inflammatory Syndrome in Children. Available online: https://www.cdc.gov/mis/hcp/clinical-care-treatment/index.html (accessed on 12 September 2025).
- World Health Organization. Living guidance for clinical management of COVID-19. Available online: https://www.who.int/publications/i/item/WHO-2019-nCoV-clinical-2021-2 (accessed on 12 September 2025).
- Dourdouna, M.-M.; Mpourazani, E.; Tatsi, E.-B.; Tsirogianni, C.; Barbaressou, C.; Dessypris, N.; et al. Clinical and Laboratory Parameters Associated with PICU Admission in Children with Multisystem Inflammatory Syndrome Associated with COVID-19 (MIS-C). Journal of Personalized Medicine. 2024, 14, 1011. [Google Scholar] [CrossRef] [PubMed]
- Constantin, T.; Pék, T.; Horváth, Z.; Garan, D.; Szabó, A.J. Multisystem inflammatory syndrome in children (MIS-C): Implications for long COVID. Inflammopharmacology. 2023, 31, 2221–2236. [Google Scholar] [CrossRef]
- Takia, L.; Angurana, S.K.; Nallasamy, K.; Bansal, A.; Muralidharan, J. Updated Management Protocol for Multisystem Inflammatory Syndrome in Children (MIS-C). J Trop Pediatr. 2021, 67, fmab071. [Google Scholar] [CrossRef] [PubMed]
- American College of Rheumatology: Clinical Guidance for Multisystem Inflammatory Syndrome in Children Associated With SARS–CoV-2 and Hyperinflammation in Pediatric COVID-19: Version 3. Available online: https://acrjournals.onlinelibrary.wiley.com/doi/full/10.1002/art.42062?utm_source=chatgpt.com (accessed on 12 September 2025).
- Peng, Z.; Zhou, G. Progress on diagnosis and treatment of multisystem inflammatory syndrome in children. Front. Immunol. 2025, 16, 1551122. [Google Scholar] [CrossRef] [PubMed]
- Centers for Disease Control and Prevention. How to Protect Yourself and Others. Available online: https://www.cdc.gov/covid/prevention/index.html#:~:text=Wearing%20a%20mask%20and%20putting,spreading%20COVID%2D19%20to%20others (accessed on 12 September 2025).
- Aldawas, A.; Ishfaq, M. COVID-19: Multisystem Inflammatory Syndrome in Children (MIS-C). Cureus. 2022, 14, e21064. [Google Scholar] [CrossRef]
- Gottlieb, M.; Bridwell, R.; Ravera, J.; Long, B. Multisystem inflammatory syndrome in children with COVID-19. Am J Emerg Med. 2021, 49, 148–152. [Google Scholar] [CrossRef] [PubMed]
- Della Paolera, S.; Valencic, E.; Piscianz, E.; Moressa, V.; Raffaella, S.; Tommasini, A.; et al. Front. Pediatr., Sec. Pediatric Immunology. 2020; Volume 8. [CrossRef]
- Multisystem inflammatory syndrome in children (MIS-C) interim guidance. American Academy of Pediatrics. Available online: https://services.aap.org/en/pages/2019-novel-coronavirus-covid-19-infections/clinical-guidance/multisystem-inflammatory-syndrome-in-children-mis-c-interim-guidance (accessed on 12 September 2025).
- Dufort, E.M.; Koumans, E.H.; Chow, E.J.; Rosenthal, E.M.; Muse, A.; Rowlands, J.; et al. New York State and Centers for Disease Control and Prevention Multisystem Inflammatory Syndrome in Children Investigation Team. Multisystem Inflammatory Syndrome in Children in New York State. N Engl J Med. 2020, 383, 347–358. [Google Scholar] [CrossRef]
- Morris, S.B.; Schwartz, N.G.; Patel, P.; Abbo, L.; Beauchamps, L.; Balan, S.; et al. Case Series of Multisystem Inflammatory Syndrome in Adults Associated with SARS-CoV-2 Infection—United Kingdom and United States, March-August 2020. MMWR Morb Mortal Wkly Rep. 2020, 69, 1450–1456. [Google Scholar] [CrossRef]
- Centers for Disease Control and Prevention. Multisystem Inflammatory Syndrome in Children (MIS-C) Associated with SARS-CoV-2 Infection. 2023 Case Definition. Available online: https://ndc.services.cdc.gov/case-definitions/multisystem-inflammatory-syndrome-in-children-mis-c-2023/ (accessed on 12 September 2025).
- Lin, J.; Tong, Q.; Huang, H.; Liu, J.; Kang, Y.; Liu, S.; Wang, W.; Ren, T.; Yuan, Y. Glucocorticoids and immunoglobulin alone or in combination in the treatment of multisystemic inflammatory syndrome in children: A systematic review and network meta-analysis. Front Pediatr. 2025, 13, 1545788. [Google Scholar]
- Dizon, B.L.; Redmond, C.; Gotschlich, E.C.; et al. Clinical outcomes and safety of anakinra in the treatment of multisystem inflammatory syndrome in children: A single center observational study. Pediatr Rheumatol 2023, 21, 76. [Google Scholar] [CrossRef] [PubMed]
- Licciardi, F.; Covizzi, C.; Dellepiane, M.; Olivini, N.; Mastrolia, M.V.; Lo Vecchio, A.; et al. Outcomes of MIS-C patients treated with anakinra: A retrospective multicenter national study. Front Pediatr. 2023, 11, 1137051. [Google Scholar]
- Moraleda, C.; Ludwikowska, K.; Gastesi, I.; Okarska-Napierała, M.; Epalza, C.; Paredes-Carmona, F.; et al. International Working Group on Aneurysms in MIS-C. Both Corticosteroids and Intravenous Immunoglobulin Protect From Aneurysms in Children With Multisystem Inflammatory Syndrome (MIS-C): A Multicenter Ambispective Study. Pediatr Infect Dis J. 2025. [Google Scholar] [CrossRef]
- Kelly, M.S.; Fernandes, N.D.; Carr, A.V.; Beaute, J.I.; Lahoud-Rahme, M.; Cummings, B.M.; et al. Diagnostic Yield of Cardiac Biomarker Testing in Predicting Cardiac Disease and Multisystem Inflammatory Syndrome in Children in the Pandemic Era. Pediatric Emergency Care. 2022, 38, e1584–e1589. [Google Scholar] [CrossRef] [PubMed]
| GENE/LOCUS | PROPOSED ROLE/PATHWAY | ASSOCIATED POPULATION (if specified) |
CLINICAL SIGNIFICANCE |
|---|---|---|---|
| DDX60 | Viral defense, inflammatory pathway | General cohort | Associated with monogenic susceptibility to MIS-C |
| TMEM154 | Immune response, viral defense | General cohort | Associated with monogenic susceptibility to MIS-C |
| TLR3, TLR6 | Innate immune response, viral defense | Middle Eastern cohort | Deleterious heterozygous variants linked to immune dysregulation and inflammation |
| IL22RA2 | Inflammatory pathway | Middle Eastern cohort | Deleterious heterozygous variants linked to immune dysregulation |
| LYST | Lysosomal trafficking, innate immunity | General cohort | Variants associated with abnormal innate immune responses and cytokine heterogeneity |
| BIOMARKER | CLINICAL UTILITY | ROLE IN PERSONALIZED CARE | STATUS |
|---|---|---|---|
| NT-proBNP & Troponin | Cardiac injury, myocardial stress | Risk stratification for cardiac complications; guides ICU admission and monitoring | Established/Robust |
| CRP, Ferritin, D-dimer | Systemic inflammation, coagulopathy |
Assessment of disease severity; monitoring treatment response | Established/Standard |
| CXCL9 | Macrophage activation, immune dysregulation |
Potential for identifying specific inflammatory phenotypes for targeted therapy | Emerging/Requires validation |
| Angiopoietin-2 | Endothelial dysfunction, shock | Potential for identifying risk of vascular collapse and guiding fluid management | Emerging/Requires validation |
| Vitamin D | Immune regulation, disease severity | Potential for identifying individuals with a specific immune profile and risk factor | Emerging/Requires validation |
| CLINICAL CRITERIA | LABORATORY CRITERIA | EPIDEMIOLOGIC LINKAGE CRITERIA |
|---|---|---|
An illness defined by the presence of all of the following features, in the absence of a more likely alternative diagnosis:
Presence of new manifestations in at least two of the following categories: A). Manifestations of cardiac involvement, defined by:
1. Rash or 2. Inflammation of the oral mucosa (ie: mucosal erythema or swelling, drying or fissuring of the lips), or 3. Conjunctival injection or 4. Extremity findings (ie: edema or erythema of the hands or feet) C) Gastrointestinal involvement defined by: 1. Abdominal pain or vomiting or diarrhea D) Hematologic involvement defined by: 1. Platelet count < 150,000 cells/μL or 2. Absolute lymphocyte count (ALC) < 1,000 cells/μL or E) Shock |
Detection of SARS-CoV-2 RNA by a diagnostic molecular amplification test in a clinical specimen collected within 60 days prior to hospitalization, during hospitalization, or from a post-mortem specimen (ie: polymerase chain reaction, PCR) or
|
Close contact with a confirmed or probable case of COVID-19 within 60 days prior to hospitalization |
| PARAMETER | MULTISYSTEM INFLAMMATORY SYNDROME IN CHILDREN (MIS-C) | KAWASAKI DISEASE (KD) |
|---|---|---|
| Median Age | 6-11 years | Almost exclusively under 5 years |
| Predominant Demographics | Children of African, Hispanic, and Latino descent |
Frequent in Children of Asian descent |
| Timing of Onset | Typically, 2-6 weeks after a SARS-CoV-2 infection | Occurs shortly after an infection |
| Etiological Agent | Definitive link to prior SARS-CoV-2 infection |
Unknown pathogen; thought to be an abnormal immune response in predisposed individuals |
| Prevalence of Shock | High (40-80%) | Low (<10%) |
|
Prevalence of Gastrointestinal Symptoms |
Very high (60-100%) | Low (~20%) |
|
Prevalence of Lymphopenia/ Thrombocytopenia |
Common (37-81% / 11-31%) | Rare |
|
Elevated Troponin / NT-proBNP |
Very common (33-95% for troponin) | Rare |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




