Submitted:
01 October 2025
Posted:
03 October 2025
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Robotic Device
2.3. Robotic Assessments
2.4. Clinical Assessments (Only Stroke)
2.5. Statistical Analysis
3. Results
| Average ± SD | [Min Max] | |
|---|---|---|
| Age | 60 ± 12 | [27 78] |
| Days Post Stroke | 1138 ± 1027 | [201 4085] |
| [25] NIH Stroke Severity Scale [0 42] |
6 ± 3 | [2 16] |
| [26] Lower Extremity Fugl Meyer [0 34] | 20 ± 4 | [12 28] |
| [27]Modified Ashworth Score [0 4] |
1.56 ± 0.46 | [0 2] |
| [28] 6 min walk distance (meters) |
107.9 ± 66.2 | [0.20 298.50] |
| [29] 10 Meter Walk Test (m/s) | 0.36 ± 0.24 | [0 0.76] |
| [30] Montreal Cognitive Assessment [0 30] | 22 ± 6 | [1 30] |
| Ischemic/Hemorrhagic/Both | 16/16/2 | |
| # of Participants | Age [Max Min] | Sex | Dominance | |
| Young | 36 | 25 ± 4 [19 33] | 23M/13F | 34R/2L |
| Older | 26 | 64 ± 10 [50 84] | 10M/16F | 22R/4L |
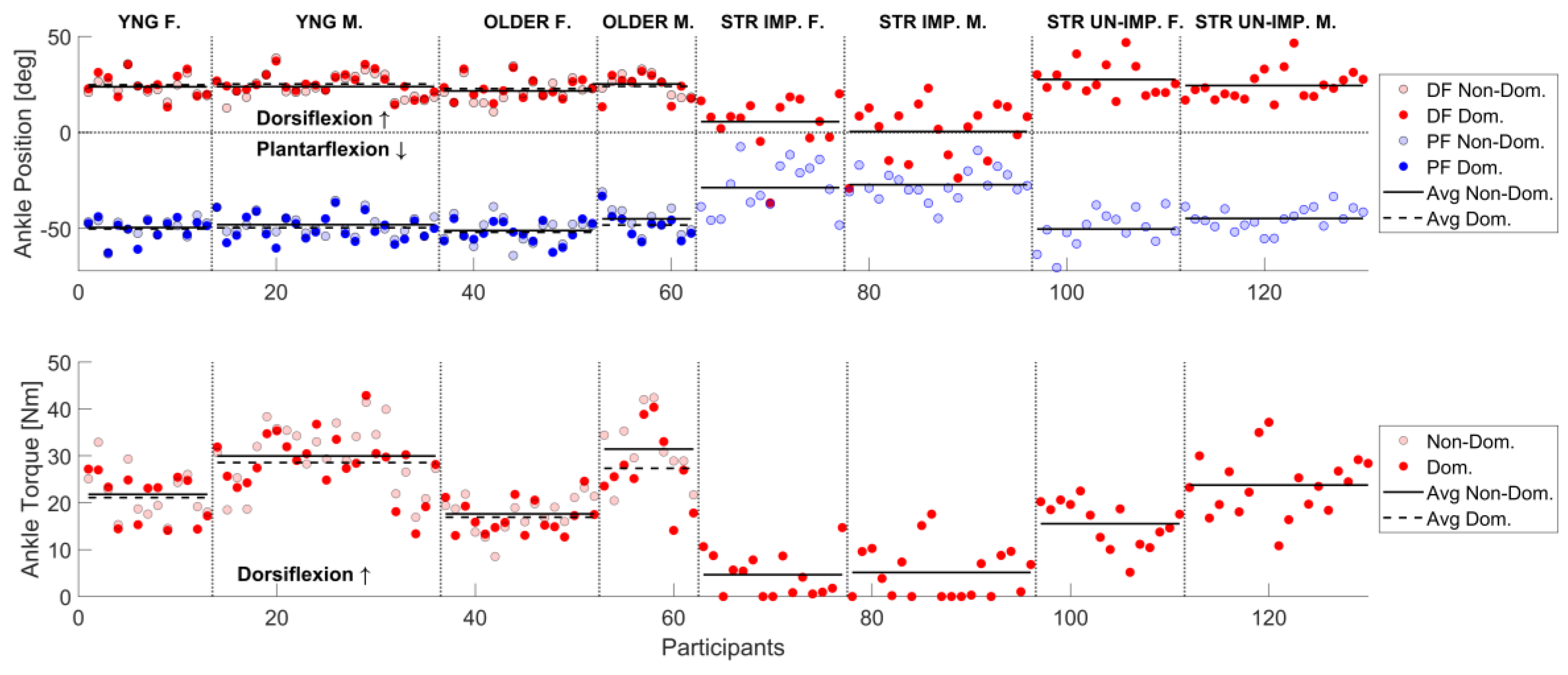
3.1. Overview of Measurements and Effect of Stroke
3.2. Test-Retest Reliability of Robot- and Therapist-Based Measurement of Ankle ROM and MVC
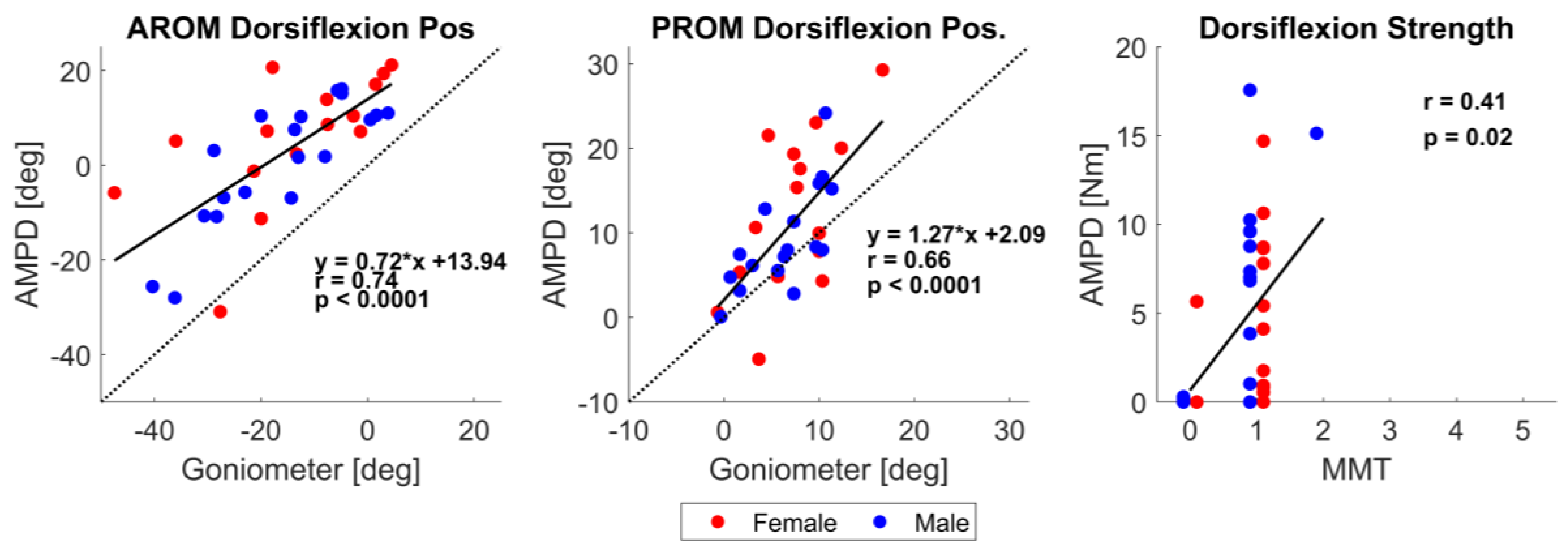
3.3. Validity of Robot-Based Compared to Therapist-Based Measurement
3.4. Reliability of Robotic Measures for Unimpaired Participants
3.5. Comparison of First and Second Session Measurements
3.6. Comparison of Older to Younger Unimpaired Adults and Effect of Leg Dominance
4. Discussion
4.1. Considerations in Using Sensorized, Robotic Platforms as Ankle Assessment Tools
4.2. Limitations and Directions for Future Research
5. Conclusion
References
- E. S. Donkor, “Stroke in the 21st Century: A Snapshot of the Burden, Epidemiology, and Quality of Life,” Stroke Res Treat, vol. 2018, 2018. [CrossRef]
- J. Carod-Artal, J. A. Egido, J. L. González, and E. Varela de Seijas, “Quality of Life Among Stroke Survivors Evaluated 1 Year After Stroke,” Stroke, vol. 31, no. 12, pp. 2995–3000, Dec. 2000. [CrossRef]
- P. Y. Lin, Y. R. Yang, S. J. Cheng, and R. Y. Wang, “The Relation Between Ankle Impairments and Gait Velocity and Symmetry in People With Stroke,” Arch Phys Med Rehabil, vol. 87, no. 4, pp. 562–568, Apr. 2006. [CrossRef]
- S. S. Ng and C. W. Hui-Chan, “Contribution of Ankle Dorsiflexor Strength to Walking Endurance in People With Spastic Hemiplegia After Stroke,” Arch Phys Med Rehabil, vol. 93, 2012. [CrossRef]
- D. Kunkel, J. Potter, and L. Mamode, “A cross-sectional observational study comparing foot and ankle characteristics in people with stroke and healthy controls,” Disabil Rehabil, vol. 39, no. 12, pp. 1149–1154, Jun. 2017. [CrossRef]
- M. Abdalla Alawna, B. H. Unver, and E. O. Yuksel, “The Reliability of a Smartphone Goniometer Application Compared With a Traditional Goniometer for Measuring Ankle Joint Range of Motion,” J Am Podiatr Med Assoc, Jan. 2019. [CrossRef]
- M. Rabelo, G. S. Nunes, N. M. Da Costa Amante, M. De Noronha, and E. Fachin-Martins, “Reliability of muscle strength assessment in chronic post-stroke hemiparesis: a systematic review and meta-analysis,” Top Stroke Rehabil, vol. 23, no. 1, pp. 26–35, 2016. [CrossRef]
- J. Wilken, R. Smita, M. Estin, C. Saltzman, and H. John Yack, “A new device for assessing ankle dorsiflexion motion: reliability and validity,” J Orthop Sports Phys Ther, vol. 41, no. 4, pp. 274–280, 2011. [CrossRef]
- M. M. Konor, S. Morton, J. M. Eckerson, and T. L. Grindstaff, “RELIABILITY OF THREE MEASURES OF ANKLE DORSIFLEXION RANGE OF MOTION,” Int J Sports Phys Ther, vol. 7, no. 3, p. 279, Jun. 2012, Accessed: Mar. 24, 2024. [Online]. Available: /pmc/articles/PMC3362988/.
- S. Y. Cho, Y. Myong, S. Park, M. Cho, and S. Kim, “A portable articulated dynamometer for ankle dorsiflexion and plantar flexion strength measurement: a design, validation, and user experience study,” Sci Rep, vol. 13, no. 1, p. 22221, 2023. [CrossRef]
- F. N. Bittmann, S. Dech, M. Aehle, and L. V. Schaefer, “Manual Muscle Testing—Force Profiles and Their Reproducibility,” Diagnostics, vol. 10, no. 12, Dec. 2020. [CrossRef]
- M. Zhang, T. C. Davies, Y. Zhang, S. Xie, and E. Phd, “Reviewing effectiveness of ankle assessment techniques for use in robot-assisted therapy,” vol. 51, no. 4, pp. 517–534, 2014. [CrossRef]
- O. Lambercy, S. Maggioni, L. Lünenburger, R. Gassert, and M. Bolliger, “Robotic and Wearable Sensor Technologies for Measurements/Clinical Assessments,” 2016, pp. 183–207. [CrossRef]
- J. Mehrholz, S. Thomas, C. Werner, J. Kugler, M. Pohl, and B. Elsner, “Electromechanical-assisted training for walking after stroke,” Cochrane Database Syst Rev, vol. 5, no. 5, May 2017. [CrossRef]
- I. Díaz, J. J. Gil, and E. Sánchez, “Lower-Limb Robotic Rehabilitation: Literature Review and Challenges,” Journal of Robotics, vol. 2011, p. 759764, 2011. [CrossRef]
- S. Maggioni et al., “Robot-aided assessment of lower extremity functions: A review,” Aug. 02, 2016, BioMed Central Ltd. [CrossRef]
- E. A. S. Duncan and J. Murray, “The barriers and facilitators to routine outcome measurement by allied health professionals in practice: A systematic review,” BMC Health Serv Res, vol. 12, no. 1, pp. 1–9, May 2012. [CrossRef]
- P. Biswas et al., “A single-center, assessor-blinded, randomized controlled clinical trial to test the safety and efficacy of a novel brain-computer interface controlled functional electrical stimulation (BCI-FES) intervention for gait rehabilitation in the chronic stroke population,” BMC Neurol, vol. 24, no. 1, p. 200, 2024. [CrossRef]
- N. van Melick, B. M. Meddeler, T. J. Hoogeboom, M. W. G. Nijhuis-van der Sanden, and R. E. H. van Cingel, “How to determine leg dominance: The agreement between self-reported and observed performance in healthy adults,” PLoS One, vol. 12, no. 12, p. e0189876, Dec. 2017. [CrossRef]
- C. A. Johnson, D. S. Reinsdorf, D. J. Reinkensmeyer, and A. J. Farrens, “Robotically quantifying finger and ankle proprioception: Role of range, speed, anticipatory errors, and learning.” Accessed: Nov. 15, 2023. [Online]. Available: https://arinex.com.au/EMBC/pdf/full-paper_1006.pdf.
- R. P. Kleyweg, F. G. A. Van Der Meché, and P. I. M. Schmitz, “Interobserver agreement in the assessment of muscle strength and functional abilities in Guillain-Barré syndrome,” Muscle Nerve, vol. 14, no. 11, pp. 1103–1109, Nov. 1991. [CrossRef]
- T. K. Koo and M. Y. Li, “A Guideline of Selecting and Reporting Intraclass Correlation Coefficients for Reliability Research,” J Chiropr Med, vol. 15, no. 2, p. 155, Jun. 2016. [CrossRef]
- J. P. WEIR, “QUANTIFYING TEST-RETEST RELIABILITY USING THE INTRACLASS CORRELATION COEFFICIENT AND THE SEM,” The Journal of Strength & Conditioning Research, vol. 19, no. 1, 2005, [Online]. Available: https://journals.lww.com/nsca-jscr/fulltext/2005/02000/quantifying_test_retest_reliability_using_the.38.aspx.
- J. Cohen, “Statistical Power Analysis for the Behavioral Sciences,” Statistical Power Analysis for the Behavioral Sciences, May 2013. [CrossRef]
- S. E. Kasner, “Clinical interpretation and use of stroke scales,” Lancet Neurol, vol. 5, no. 7, pp. 603–612, Jul. 2006. [CrossRef]
- S. J. Page, E. Hade, and A. Persch, “Psychometrics of the wrist stability and hand mobility subscales of the Fugl-Meyer assessment in moderately impaired stroke,” Phys Ther, vol. 95, no. 1, pp. 103–108, Jan. 2015. [CrossRef]
- G. Lee, S. An, Y. Lee, D. Lee, and D. S. Park, “Predictive factors of hypertonia in the upper extremity of chronic stroke survivors,” J Phys Ther Sci, vol. 27, no. 8, p. 2545, Aug. 2015. [CrossRef]
- U. B. Flansbjer, A. M. Holmbäck, D. Downham, C. Patten, and J. Lexell, “Reliability of gait performance tests in men and women with hemiparesis after stroke,” J Rehabil Med, vol. 37, no. 2, pp. 75–82, Mar. 2005. [CrossRef]
- K. Severinsen, J. K. Jakobsen, K. Overgaard, and H. Andersen, “Normalized muscle strength, aerobic capacity, and walking performance in chronic stroke: a population-based study on the potential for endurance and resistance training,” Arch Phys Med Rehabil, vol. 92, no. 10, pp. 1663–1668, Oct. 2011. [CrossRef]
- T. B. Cumming, D. Lowe, T. Linden, and J. Bernhardt, “The AVERT MoCA Data: Scoring Reliability in a Large Multicenter Trial,” Assessment, vol. 27, no. 5, pp. 976–981, Jul. 2020. [CrossRef]
- J. A. Saglia, N. G. Tsagarakis, J. S. Dai, and D. G. Caldwell, “Control strategies for patient-assisted training using the ankle rehabilitation robot (ARBOT),” IEEE/ASME Transactions on Mechatronics, vol. 18, no. 6, pp. 1799–1808, 2013. [CrossRef]
- A. B. Farjadian, M. Nabian, A. Hartman, and S.-C. Yen, “Vi-RABT: A Platform-Based Robot for Ankle and Balance Assessment and Training,” J Med Biol Eng, vol. 38, no. 4, pp. 556–572, 2018. [CrossRef]
- Z. Zhou, Y. Zhou, N. Wang, F. Gao, K. Wei, and Q. Wang, “A proprioceptive neuromuscular facilitation integrated robotic ankle–foot system for post stroke rehabilitation,” Rob Auton Syst, vol. 73, pp. 111–122, Nov. 2015. [CrossRef]
- N. A. S. Taylor, R. H. Sanders, E. I. Howick, and S. N. Stanley, “Static and dynamic assessment of the Biodex dynamometer,” Eur J Appl Physiol Occup Physiol, vol. 62, no. 3, pp. 180–188, May 1991. [CrossRef]
- P. Tavares, V. Landsman, and L. Wiltshire, “Intra-examiner reliability of measurements of ankle range of motion using a modified inclinometer: a pilot study.,” J Can Chiropr Assoc, vol. 61, no. 2, pp. 121–127, Aug. 2017.
- I.-G. Jung, I.-Y. Yu, S.-Y. Kim, D.-K. Lee, and J.-S. Oh, “Reliability of ankle dorsiflexion passive range of motion measurements obtained using a hand-held goniometer and Biodex dynamometer in stroke patients,” J Phys Ther Sci, vol. 27, no. 6, pp. 1899–1901, 2015. [CrossRef]
- C. Y. Wang, S. L. Olson, and E. J. Protas, “Test-retest strength reliability: Hand-held dynamometry in community-dwelling elderly fallers,” Arch Phys Med Rehabil, vol. 83, no. 6, pp. 811–815, Jun. 2002. [CrossRef]
- H. B. Menz, A. Tiedemann, M. M.-S. Kwan, M. D. Latt, C. Sherrington, and S. R. Lord, “Reliability of Clinical Tests of Foot and Ankle Characteristics in Older People,” J Am Podiatr Med Assoc, vol. 93, no. 5, pp. 380–387, 2003. [CrossRef]
- J. W. Youdas, C. L. Bogard, and V. J. Suman, “Reliability of goniometric measurements and visual estimates of ankle joint active range of motion obtained in a clinical setting,” Arch Phys Med Rehabil, vol. 74, no. 10, pp. 1113–1118, Oct. 1993. [CrossRef]
- J. T. Choi, J. Lundbye-Jensen, C. Leukel, and J. B. Nielsen, “Cutaneous mechanisms of isometric ankle force control,” Exp Brain Res, vol. 228, no. 3, pp. 377–384, Jul. 2013. [CrossRef]
- N. D. Neckel, N. Blonien, D. Nichols, and J. Hidler, “Abnormal joint torque patterns exhibited by chronic stroke subjects while walking with a prescribed physiological gait pattern,” J Neuroeng Rehabil, vol. 5, no. 1, pp. 1–13, Sep. 2008. [CrossRef]
- S. BRUNNSTROM, “Movement therapy in hemiplegia,” A neurophysiological approach, 1970, Accessed: May 04, 2024. [Online]. Available: https://cir.nii.ac.jp/crid/1574231875545213568.bib?lang=en.
- R. D. Luce and L. Narens, “Measurement Scales on the Continuum,” Science (1979), vol. 236, no. 4808, pp. 1527–1532, Jun. 1987. [CrossRef]
- S. E. Munteanu, A. B. Strawhorn, K. B. Landorf, A. R. Bird, and G. S. Murley, “A weightbearing technique for the measurement of ankle joint dorsiflexion with the knee extended is reliable,” J Sci Med Sport, vol. 12, no. 1, pp. 54–59, 2009. [CrossRef]

| Young | Old | Stroke | ||||
| Dom. | Non-Dom. | Dom. | Non-Dom. | Impaired | Unimpaired | |
| AROM Dorsiflexion Position [°] | ||||||
| Session 1 | A: 25.04°±5.8 F: 24.8°± 6.4° M: 25.2°±5.6° |
A: 23.8°±6.0° F: 23.7° ± 5.2° M: 23.8°±6.5° |
A:23.2°±6.0° F: 22.8°±5.6° M:24.0°±6.7° |
A: 23.0°±6.1 F: 21.6°± 6.3° M: 25.2°±5.4° |
A: 2.7°±7.8° F: 5.6°± 14.2° M: 0.4°± 14.7° |
A:25.8°±8.2 F: 27.6°± 8.6° M: 24.4°± 7.9° |
| Session 2 | A: 26.4°±5.9° F: 25.8°±6.4° M: 26.7°±5.7° |
A: 25.0°±6.4° F: 25.1°± 7.1° M: 24.9°±6.2° |
A:24.7°±7.0° F: 24.9°±7.8° M: 24.3°±5.8° |
A:24.0°±6.7° F: 23.1°±7.0° M: 25.4°±6.3° |
A: 3.3°±13.6° F: 5.6°± 14.6° M: 1.5°± 12.9° |
A:25.5°±7.5° F: 25.7°± 8.4° M: 25.4°± 6.9° |
| Change in mean | A:1.3°±2.7° F: 1.0°±3.5° M: 1.5°±2.2° |
A:1.2 °± 3.7° F: 1.3°±4.7° M: 1.1°± 3.1° |
A: 1.3°± 2.8° F: 2.1°± 2.9° M: 0.4°±1.6° |
A: 1.0°± 2.1° F: 2.1°± 2.9° M: 0.2°±2.5° |
A: 0.6°± 7.8° F: 0.0°± 7.6° M: 1.1°± 8.1° |
A: -0.3°± 2.7° F: -1.9°± 4.2° M: 1.0°± 4.1° |
| AROM Plantarflexion Position [°] | ||||||
| Session 1 | A: -49.8°±6.3° F: -50.2°± 5.9° M: -49.6°±6.6° |
A: -48.5°±5.5° F: -49.5°±5.3° M: -48.0°± 5.7° |
A: -50.5°±6.3° F: -51.9°±5.5° M -48.2°±7.1° |
A: -48.7°±7.6° F: -51.1°± 6.9° M: -45.0°±7.4° |
A: -27.9°±10.5° F: -28.7°± 13.2° M: -27.2°± 8.0° |
A: -47.2°±8.0° F: -50.3°± 9.4° M: -44.8°± 5.8° |
| Session 2 | A: -49.75°±7.0° F: -49.8°± 7.6° M: -49.7°± 6.8° |
A: -48.3°±6.2° F: -49.9°± 6.1° M: -47.4°± 6.2° |
A: -49.2°±5.3° F: -50.3°± 5.3° M: -47.3°±5.0° |
A: -48.6°±6.1° F: 50.1°±6.1° M: -46.2°±5.5° |
A: -28.1°±12.0° F: -27.0°± 15.6° M: -28.9°± 8.5° |
A: -46.8°±8.4° F: -49.4°± 10.3° M: -44.7°± 6.0° |
| Change in mean | A:0.1°±2.8° F: 0.4°±2.9° M: -0.1°± 2.8° |
A:0.2°±3.4° F: -0.4°± 3.0° M: 0.5°±3.6° |
A:1.3°±3.3° F: 1.6°± 3.6° M: 0.9°± 2.9° |
A:0.1°±3.2° F: 1.0°± 3.1° M: -1.2°± 3.0° |
A: -0.2°±6.4° F: 1.7°± 6.8° M: -1.7°± 5.7° |
A:0.4°±3.5° F: 0.8°± 3.3° M: 0.0°± 3.7° |
| Dorsiflexion Maximum Strength [Nm] | ||||||
| Session 1 | A: 25.9±7.0 F: 21.1±5.2 M: 28.6±6.4 |
A: 27.0±7.6 F: 21.8± 5.5 M: 30.0±7.1 |
A: 20.9±7.7 F: 16.9±3.6 M: 27.3±8.3 |
A: 22.9±8.7 F: 17.6±3.9 M: 31.4±7.4 |
A: 4.9±5.1 F: 4.7±4.6 M: 5.1±5.6 |
A: 20.1±7.1 F: 15.5±4.9 M: 23.8±4.6 |
| Session 2 | A: 25.9±7.1 F: 21.7±6.2 M: 28.2±6.6 |
A: 27.1±7.1 F: 22.0±6.1 M: 29.9±6.0 |
A: 21.3±6.9 F: 18.5±4.2 M: 25.9±8.0 |
A: 23.2±8.9 F: 18.9±4.8 M: 30.0±9.8 |
A: 4.3±4.9 F: 4.7±5.4 M: 4.0±4.6 |
A: 19.1±6.9 F: 15.3±4.9 M: 22.1±6.9 |
| Change in mean | A: 0.02±2.7 F: 0.6±2.4 M: -0.3±2.9 |
A: 0.05±3.0 F: 0.2±2.1 M: -0.02±3.5 |
A: 0.4±3.5 F: 1.6±2.8 M: -1.4±3.9 |
A: 0.2±3.9 F: 1.3±2.6 M: -1.4±5.1 |
A: -0.6±3.2 F: 0.1±2.7 M: -1.1±3.5 |
A: -1.0±3.9 F: -0.2±2.7 M: -1.6±4.6 |
| Stroke | |||
|---|---|---|---|
| Trial | ICC [95% CI] | SEM | MDC |
| AROM Dorsiflexion Position (Impaired Ankle) | |||
| Avg of 3 | R: 0.92 [0.84 0.96] T: 0.95 [0.90 0.98] |
R: 2.2° T: 1.3° |
R: 6.2° T: 3.7° |
| Dorsiflexion MVC (Impaired Ankle) | |||
| First | R: 0.89 [0.78 0.94] T: 0.86 [0.72 0.93] |
R: 1.0 Nm T: 0.1 |
R: 2.9 Nm T: 0.3 levels |
| Young | Older | Stroke | ||||||
| ICC [95% CI] | SEM | MDC | ICC [95% CI] | SEM | MDC | ICC [95% CI] | SEM | MDC |
| AROM Dorsiflexion Position | ||||||||
| 0.91 [0.85 0.95] | 0.9 | 2.6 | 0.96 [0.90 0.98] | 0.5 | 1.4 | 0.96 [0.94 0.98] | 1.2 | 3.5 |
| AROM Plantarflexion Position | ||||||||
| 0.94 [0.90 0.96] | 0.6 | 1.8 | 0.93 [0.87 0.96] | 0.9 | 2.5 | 0.96 [0.94 0.98] | 1.0 | 2.7 |
| Dorsiflexion MVC | ||||||||
| 0.96 [0.94 0.98] | 0.6 | 1.6 | 0.95 [0.91 0.97] | 0.9 | 2.4 | 0.96 [0.94 0.98] | 0.7 | 1.8 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




