Submitted:
02 October 2025
Posted:
02 October 2025
You are already at the latest version
Abstract
Keywords:
Introduction
Methods
Study Design and Population
Variables and Outcome
Statistical Analysis
Descriptive and Inferential Statistics
Multivariable Regression
Machine Learning and Model Evaluation
Visualization and Clustering
Ethics Approval
Results
| Variable | Screening Result: HIGH | Screening Result: LOW | Total | χ² (df) | p-value |
| Age group | 16.61 (5) | 0.005* | |||
| 0–4 yrs | 35 (12%) | 6 (4%) | 41 (9%) | ||
| 5–14 yrs | 70 (24%) | 29 (20%) | 99 (23%) | ||
| 15–24 yrs | 45 (16%) | 30 (20%) | 75 (17%) | ||
| 25–44 yrs | 66 (23%) | 51 (35%) | 117 (27%) | ||
| 45–64 yrs | 46 (16%) | 24 (16%) | 70 (16%) | ||
| 65+ yrs | 27 (9%) | 7 (5%) | 34 (8%) | ||
| Gender | 0.41 (1) | 0.523 | |||
| Female | 145 (50%) | 79 (54%) | 224 (51%) | ||
| Male | 145 (50%) | 68 (46%) | 213 (49%) | ||
| Screened status | 1.54 (1) | 0.215 | |||
| Yes | 290 (100%) | 145 (99%) | 435 (100%) | ||
| No | 0 (0%) | 2 (1%) | 2 (0%) |
Machine Learning Analysis of TB Household Contacts
Discussion
Risk Predictors and Vulnerable Populations
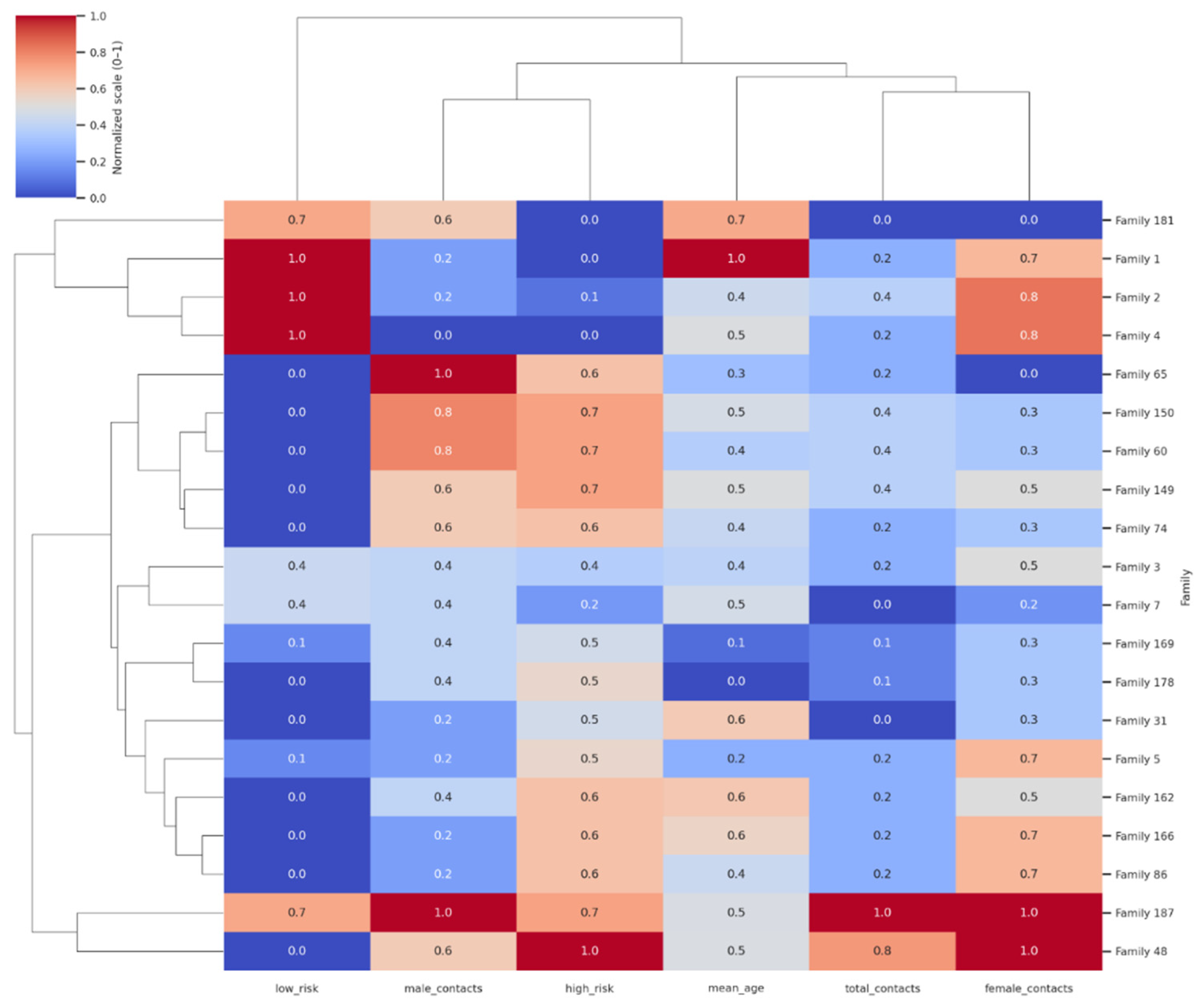
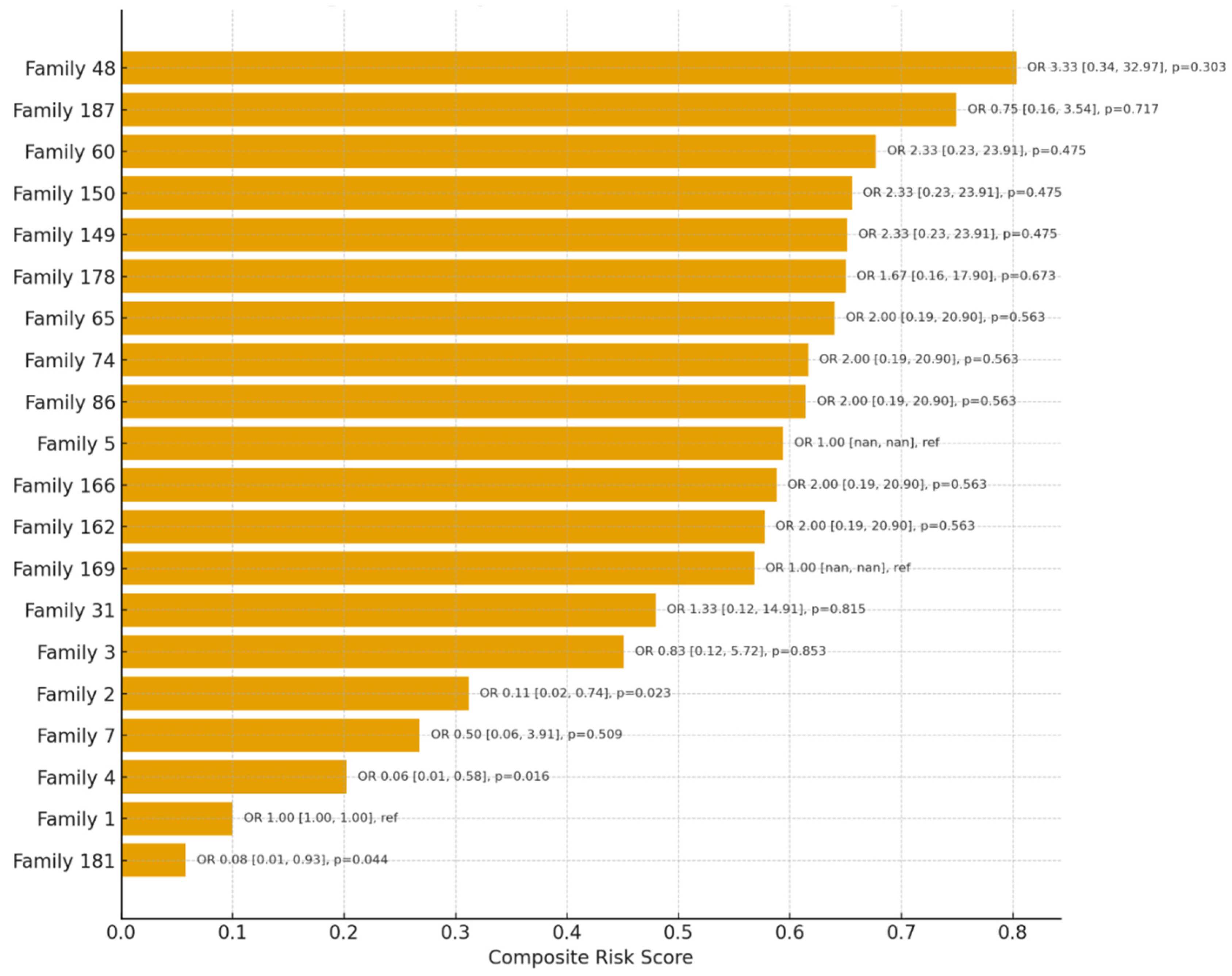
Household Clustering and Prioritization
Clinical and Governance Implications
Alignment with Global Challenges
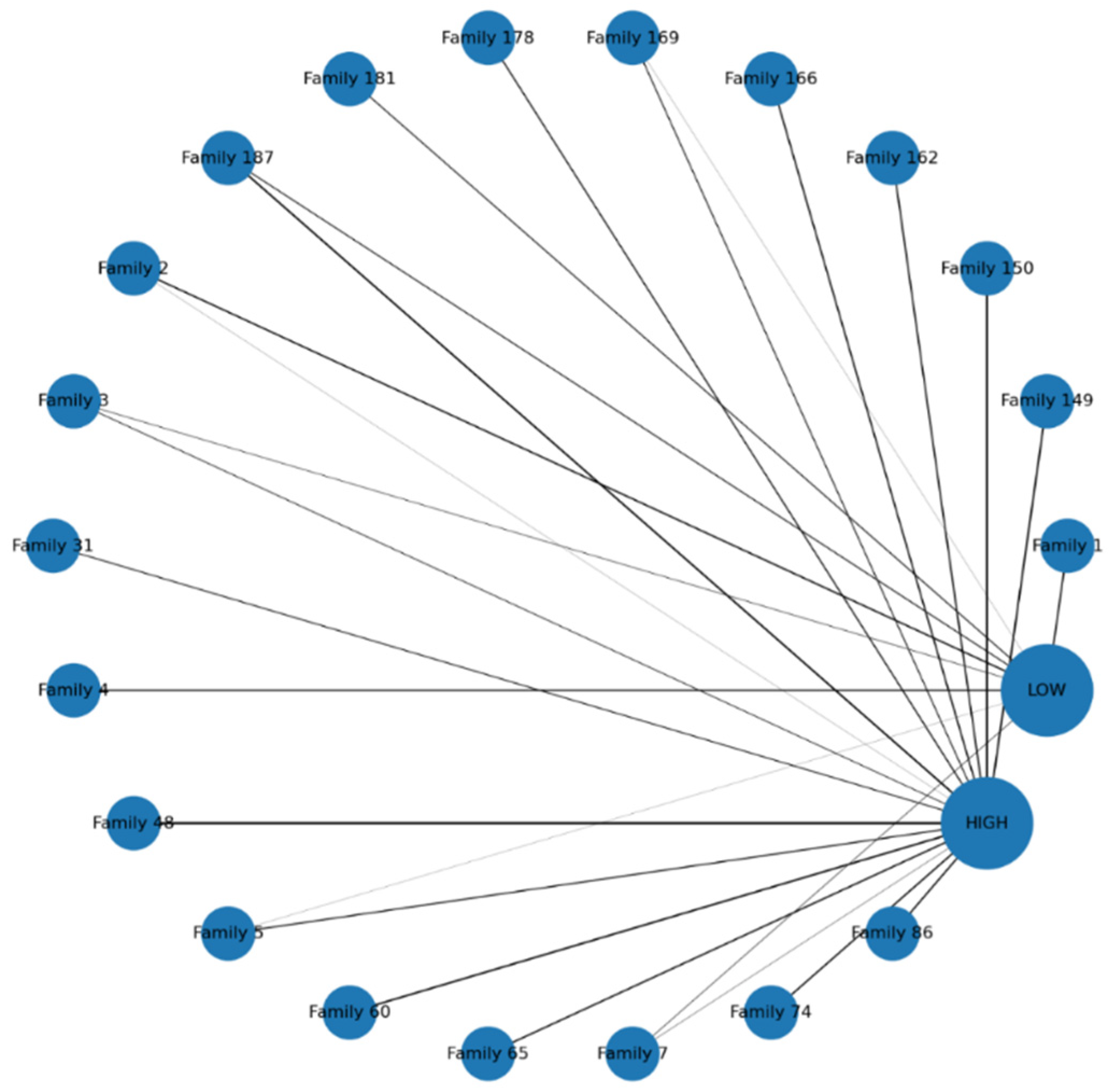
Visualization and the “Hotspot Family” Phenomenon
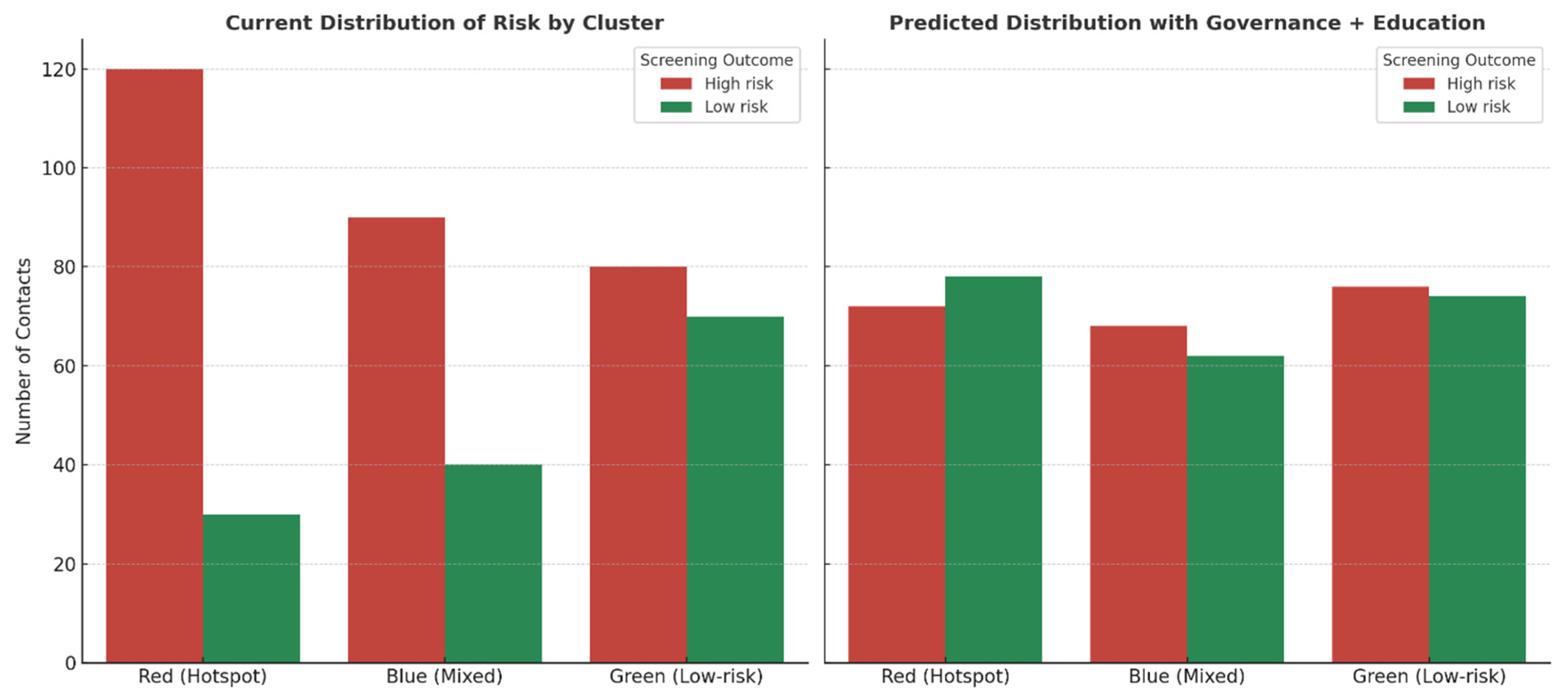
Predictive Analysis and Model Utility
Integrated Strategy for TB Control
Recommendations
- Focus on Hotspot Families: Prioritize households identified through composite risk scoring and clustering visualization (e.g., heatmaps and risk rankings) as having large size, younger age structures, and a high proportion of high-risk contacts.
- Intensified Interventions: For these highest-risk families, allocate resources for intensive contact tracing, provision of TB Preventive Therapy (TPT), and sustained follow-up. This aligns with the WHO family-centered care approach, specifically ensuring TPT for children under five and other vulnerable members.
- Stratified Monitoring: Lower-risk households, characterized by smaller size and older age structures, should receive lighter, routine monitoring, thus maximizing the efficiency of limited resources.
Integration into Governance and Practice
- Data-Driven Governance: Integrate household risk profiles (using tools like risk rankings and heatmaps) into district-level clinical governance systems. This improves decision-making, enhances accountability, and optimizes the efficiency of TB prevention programs.
- Actionable Framework: The study’s framework, which combines traditional statistical analysis, visualization, and predictive modeling, offers a practical guide for implementing this risk-based strategy.
Conclusions
Author Contributions
Funding
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Li, X.; Li, Y.; Guo, L.; Chen, Y.; Wang, G.; Zhang, H. Tuberculosis incidence, deaths and disability-adjusted life years in children and adolescence, 1990–2021: Results from the Global Burden of Disease Study 2021. PloS one. 2025 Mar 10;20(3): e0317880.
- World Health Organization. (2023). Global tuberculosis report 2023. World Health Organization. Retrieved from [Insert URL here, e.g.. https://www.who.int/publications/i/item/9789240083851].
- Velen, K.; Nhung, N.V.; Anh, N.T.; Cuong, P.D.; Hoa, N.B.; Cuong, N.K.; Dung, N.H.; Sy, D.N.; Britton, W.J.; Marks, G.B.; Fox, G.J. Risk factors for tuberculosis (TB) among Household Contacts of patients with smear-positive TB in 8 provinces of Vietnam: a nested case-control study. Clinical Infectious Diseases. 2021 Nov 1;73(9): e3358-64.
- Krishnamoorthy, Y.; Ezhumalai, K.; Murali, S.; Rajaa, S.; Jose, M.; Sathishkumar, A.; Soundappan, G.; Horsburgh, C.; Hochberg, N.; Johnson, W.E.; Knudsen, S. Prevalence and risk factors associated with latent tuberculosis infection among household contacts of smear-positive pulmonary tuberculosis patients in South India. Tropical Medicine & International Health. 2021 Dec;26(12):1645-51.
- Fox, G.J.; Johnston, J.C.; Nguyen, T.A.; Majumdar, S.S.; Denholm, J.T.; Asldurf, H.; Nguyen, C.B.; Marks, G.B.; Velen K. Active case--finding in contacts of people with TB. The International Journal of Tuberculosis and Lung Disease. 2021 Feb 1;25(2):95-105.
- Martinez, L.; Cords, O.; Horsburgh, C.R.; Andrews, J.R.; Acuna-Villaorduna, C.; Ahuja, S.D.; Altet, N.; Augusto, O.; Baliashvili, D.; Basu, S.; Becerra, M. The risk of tuberculosis in children after close exposure: a systematic review and individual-participant meta-analysis. The Lancet. 2020 Mar 21;395(10228):973-84.
- Laycock, K.M.; Enane, L.A.; Steenhoff, A.P. Tuberculosis in adolescents and young adults: emerging data on TB transmission and prevention among vulnerable young people. Tropical Medicine and Infectious Disease. 2021 Aug 5;6(3):148.
- Macharia, E. Uptake of Tuberculosis Preventive Therapy Among Eligible Children Under Five Years in Mombasa County (Doctoral dissertation, UON).
- Chandra, D.K.; Moll, A.P.; Altice, F.L.; Didomizio, E.; Andrews, L.; Shenoi, S.V. Structural barriers to implementing recommended tuberculosis preventive treatment in primary care clinics in rural South Africa. Global public health. 2022 Apr 3;17(4):555-68.
- 10. World Health Organization. (2020). WHO consolidated guidelines on tuberculosis. Module 1: Prevention—Tuberculosis preventive treatment. World Health Organization. https://apps.who.int/iris/handle/10665/331170.
- Aklie, E.N. The Ghanaian War Against Malaria: A Geospatial Approach to Malaria and Healthcare Access in Ghana (Master’s thesis, Jacksonville State University).
- Nhleko, P.N. Mobile Health Technology to Improve Tuberculosis Contact Tracing in Sub-Saharan Africa: A Systematic Review, 2010 to 2021 (Master’s thesis, University of the Witwatersrand, Johannesburg (South Africa)).
- Kerkhoff, A.D.; West, N.S.; del Mar Castro, M.; Branigan, D.; Christopher, D.J.; Denkinger, C.M.; Nhung, N.V.; Theron, G.; Worodria, W.; Yu, C.; Muyoyeta, M. Placing the values and preferences of people most affected by TB at the center of screening and testing: an approach for reaching the unreached. BMC Global and Public Health. 2023 Nov 21;1(1):27.
- Calderwood, C.J.; Timire, C.; Mavodza, C.; Kavenga, F.; Ngwenya, M.; Madziva, K.; Fielding, K.; Dixon, J.; Ferrand, R.A.; Kranzer, K. Beyond tuberculosis: a person-centred and rights-based approach to screening for household contacts. The Lancet Global Health. 2024 Mar 1;12(3): e509-15.
- Hamada, Y. Research to understand multimorbidity in households affected by tuberculosis (Doctoral dissertation, UCL (University College London)).
- Montgomery, R.M. The Multifactorial Determinants of Tuberculosis Mortality: A Global Comprehensive Epidemiological Analysis and Framework for Disease Elimination, 2025.
- Marme, G.; Rutherford, S.; and Harris, N. What tuberculosis infection control measures are effective in resource-constrained primary healthcare facilities? A systematic review of the literature. Rural and remote health, 2023, 23(1), pp.1-15.
- Kilale, A.M.; Makasi, C.; Majaha, M.; Manga, C.D.; Haule, S.; Hilary, P.; Kimbute, O.; Kitua, S.; Jani, B.; Range, N.; Ngowi, B. Implementing tuberculosis patient cost surveys in resource-constrained settings: lessons from Tanzania. BMC Public Health. 2022 Nov 25;22(1):2187.
- Afshari, M.; Dehmardeh, A.; Hoseini, A.; and Moosazadeh, M. Tuberculosis infection among children under six in contact with smear positive cases: A study in a hyper endemic area of Iran. Journal of Clinical Tuberculosis and Other Mycobacterial Diseases, 2023, 30, p.100347.
- Jember, T.; Hailu, G.; and Wassie, G.T. Assessment of family tuberculosis contact screening practice and its associated factors among pulmonary tuberculosis positive patients in South Wollo zone, Amhara region, Ethiopia. International Journal of Public Health, 2023, 68, p.1605815.
- Chawla, S.; Gupta, V.; Gour, N.; Grover, K.; Goel, P.K.; Kaushal, P.; Singh, N.; Ranjan, R. Active case finding of tuberculosis among household contacts of newly diagnosed tuberculosis patients: A community-based study from southern Haryana. Journal of Family Medicine and Primary Care. 2020 Jul 1;9(7):3701-6.
- Imsanguan, W.; Chiyasirinroje, B.; Nedsuwan, S.; Yanai, H.; Tokunaga, K.; Palittapongarnpim, P.; Murray, M.; & Mahasirimongkol, S. Contact tracing for tuberculosis, Thailand. Bulletin of the World Health Organization, 2020, 98(3), 212–218. [CrossRef]
- Khamai, N.; Seangpraw, K.; Ong-Artborirak, P. Using the Health Belief Model to Predict Tuberculosis Preventive Behaviors Among Tuberculosis Patients’ Household Contacts During the COVID-19 Pandemic in the Border Areas of Northern Thailand. Journal of Preventive Medicine and Public Health. 2024 May 1;57(3):223.
- Li, M.; Guo, M.; Peng, Y.; Jiang, Q.; Xia, L.; Zhong, S.; Qiu, Y.; Su, X.; Zhang, S.; Yang, C.; Mijiti, P. High proportion of tuberculosis transmission among social contacts in rural China: a 12-year prospective population-based genomic epidemiological study. Emerging Microbes & Infections. 2022 Dec 31;11(1):2102-11.
- Otero, L.; Battaglioli, T.; Ríos, J.; De la Torre, Z.; Trocones, N.; Ordonezm, C.; Seas, C.; Van der Stuyft, P. Contact evaluation and isoniazid preventive therapy among close and household contacts of tuberculosis patients in Lima, Peru: an analysis of routine data. Tropical Medicine & International Health. 2020 Mar;25(3):346-56.
- Kim, S.; Wu, X.; Hughes, M. D.; Upton, C.; Narunsky, K.; Mendoza-Ticona, A.; Khajenoori, S.; Gonzales, P.; Badal-Faesen, S.; Shenje, J.; Omoz-Oarhe, A.; Rouzier, V.; Garcia-Prats, A. J.; Demers, A. M.; Naini, L.; Smith, E.; Churchyard, G.; Swindells, S.; Shah, N. S.; Gupta, A.; & Hesseling, A. C. High Prevalence of Tuberculosis Infection and Disease in Child Household Contacts of Adults With Rifampin-resistant Tuberculosis. The Pediatric Infectious Disease Journal, 2022, 41(5), e194–e202. [CrossRef]
- Kontturi, A.; Kekomäki, S.; Ruotsalainen, E.; Salo, E. Tuberculosis contact investigation results among paediatric contacts in low-incidence settings in Finland. European journal of paediatrics. 2021 Jul;180(7):2185-92.
- Osman, M.; du Preez, K.; Seddon, J.A.; Claassens, M.M.; Dunbar, R.; Dlamini, S.S.; Welte, A.; Naidoo, P.; Hesseling, A.C. Mortality in South African children and adolescents routinely treated for tuberculosis. Pediatrics. 2021 Apr 1;147(4): e2020032490.
- Teo, A.K.; Morishita, F.; Prem, K.; Eng, S.; An, Y.; Huot, C.Y.; Khun, K.E.; Tieng, S.; Deng, S.; Tuot, S.; Yi, S. Where are the missing people affected by tuberculosis? A programme review of patient-pathway and cascade of care to optimise tuberculosis case-finding, treatment, and prevention in Cambodia. BMJ Global Health. 2023 Mar 15;8(3).
- Cluver, L.; Makangila, G.; Hillis, S.; Ntwali-N’Konzi, J.P.; Flaxman, S.; Unwin, J.; Imai-Eaton, J.W.; Chtimbire, V.; Sherr, L.; Desmond, C.; Toska, E. Protecting Africa’s children from extreme risk: a runway of sustainability for PEPFAR programmes. The Lancet. 2025 May 10;405(10490):1700-12.
- Havumaki, J.; Cohen, T.; Zhai, C.; Miller, J.C.; Guikema, S.D.; Eisenberg, M.C.; Zelner, J. Protective impacts of household-based tuberculosis contact tracing are robust across endemic incidence levels and community contact patterns. PLoS Computational Biology. 2021 Feb 8;17(2): e1008713.
- Coleman, M.; Martinez, L.; Theron, G.; Wood, R.; Marais, B. Mycobacterium tuberculosis transmission in high-incidence settings—new paradigms and insights. Pathogens. 2022 Oct 25;11(11):1228.
- 33. World Health Organization. (2022). Implementing the end TB strategy: The essentials, 2022 update. World Health Organization. https://www.who.int/publications/i/item/9789240065093.
- Boothe, D.B. Tuberculosis Elimination in Arkansas: Modeling Incidence and Evaluation of Screening Strategy (Doctoral dissertation, University of Arkansas for Medical Sciences).
- Rae, J.D.; Landier, J.; Simpson, J.A.; Proux, S.; Devine, A.; Maude, R.J.; Thu, A.M.; Wiladphaingern, J.; Kajeechiwa, L.; Thwin, M.M.; and Tun, S.W. Longitudinal trends in malaria testing rates in the face of elimination in eastern Myanmar: a 7-year observational study. BMC Public Health, 2021, 21(1), p.1725.
- Ntshiqa, T.; Nagudi, J.; Hamada, Y.; Copas, A.; Stender, S.; Sabi, I.; Ntinginya, E.N.; Lalashowi J.; Matete, M.; Ntshamane, K.; Morojele, I.; Ngobeni, M.; Mudzengi, D.; Minja, L.T.; Chirwal, T.; Lönnroth, K.; Dreyer, V.; Niemann, S.; Rangaka, M.; Charalambous, S.; Velen, K. Risk Factors Associated With Tuberculosis Infection Among Household Contacts of Patients With Microbiologically Confirmed Pulmonary Tuberculosis in 3 High Tuberculosis Burden Countries. J Infect Dis. 2025 Sep 15;232(3): e448-e458. [CrossRef]
- van Staden Q. Access to Tuberculosis testing among adolescents living with Human Immunodeficiency Virus in the Eastern Cape, South Africa: social factors and theoretical considerations.
- Konkor, I. Understanding the connections between neighborhood environments and Ghana’s burden of infectious and non-communicable diseases (Doctoral dissertation, University of Toronto, Canada).
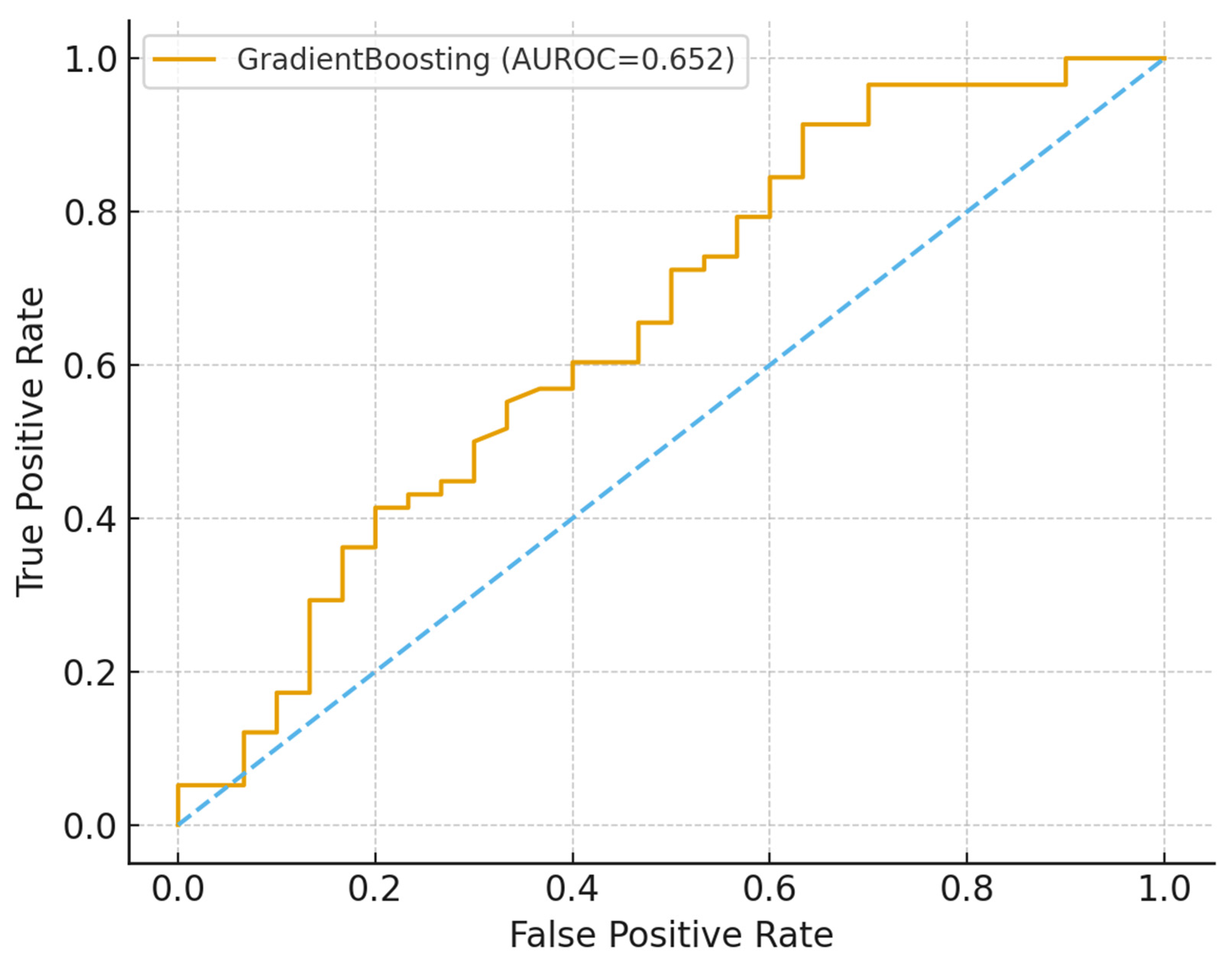
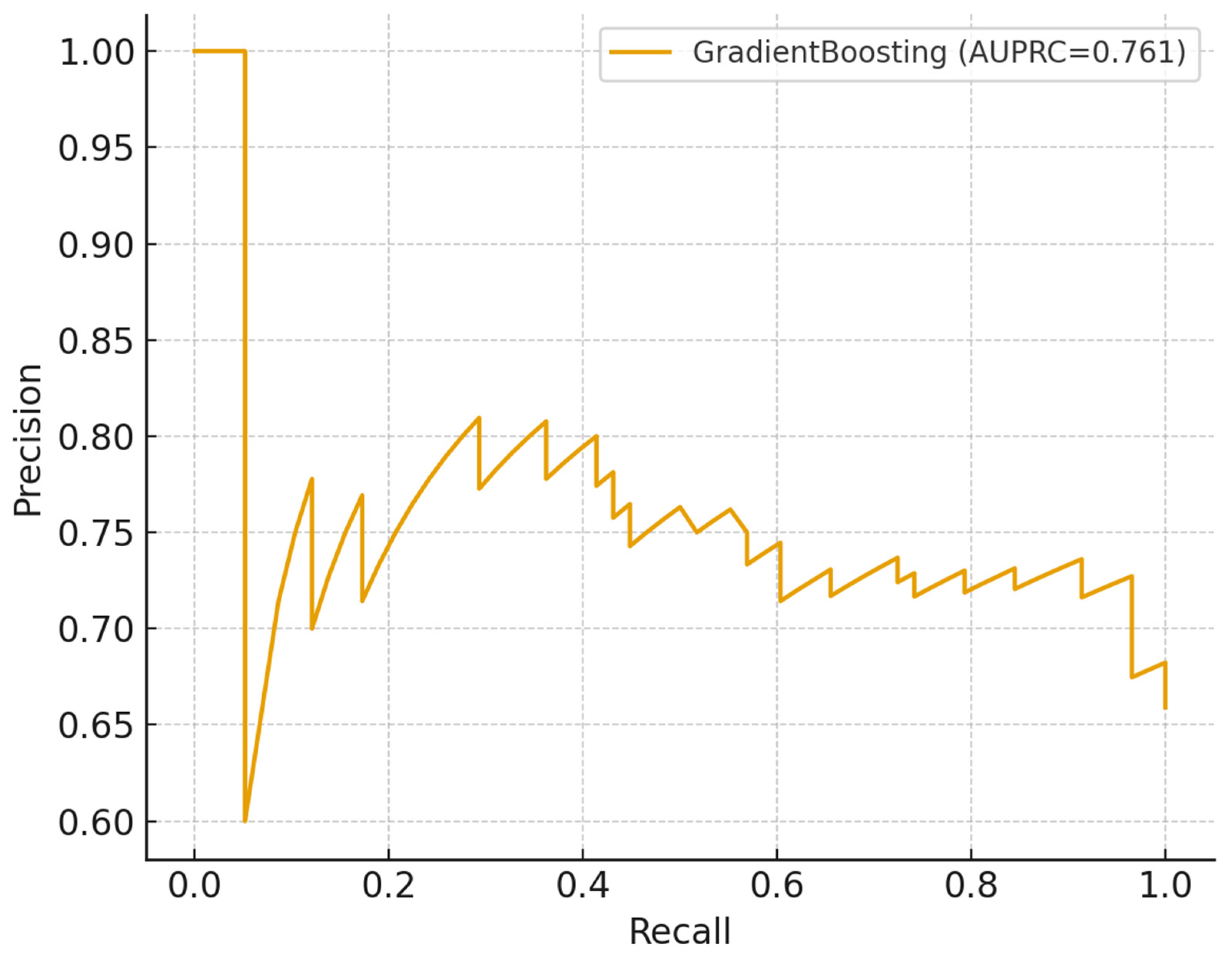
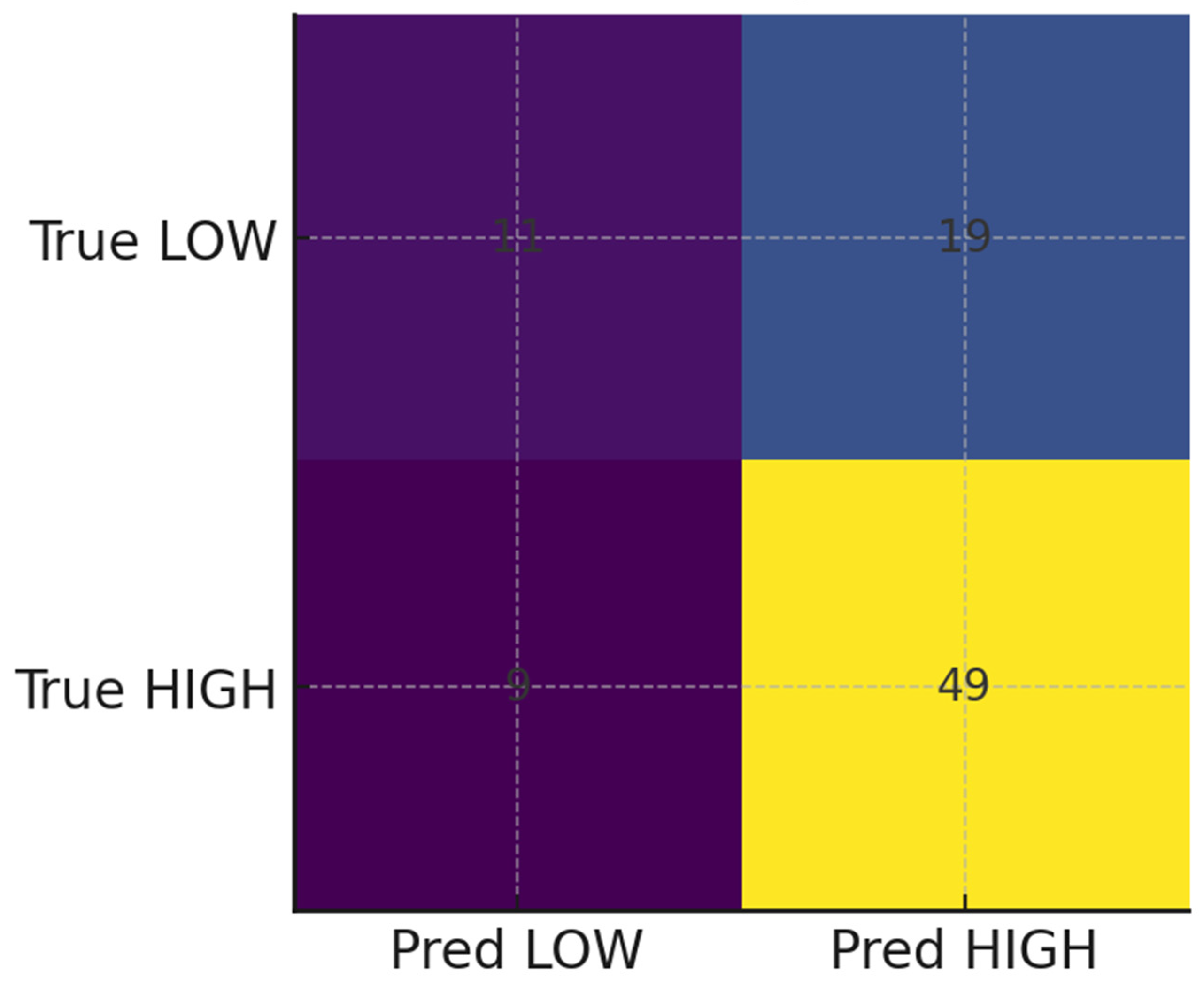
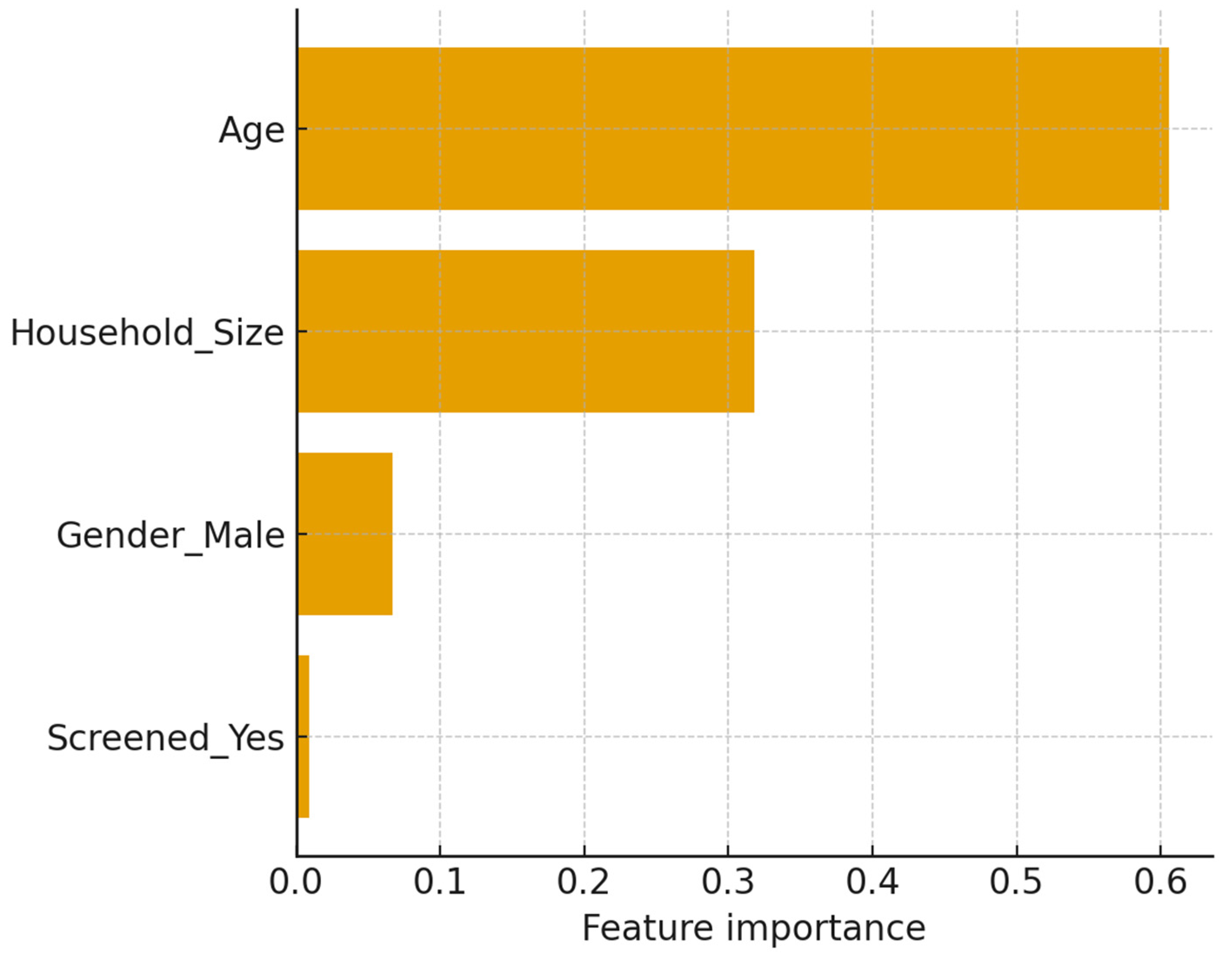
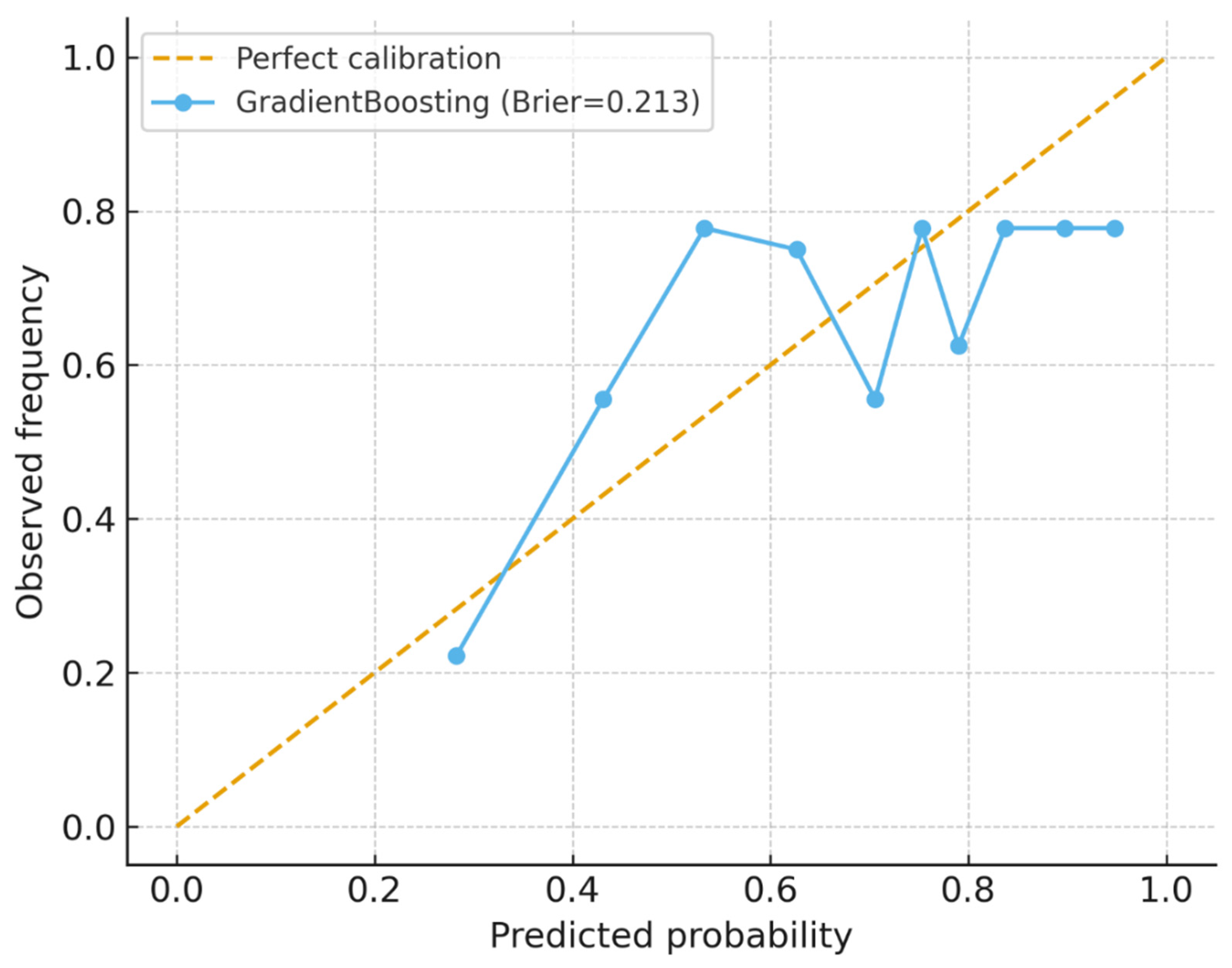
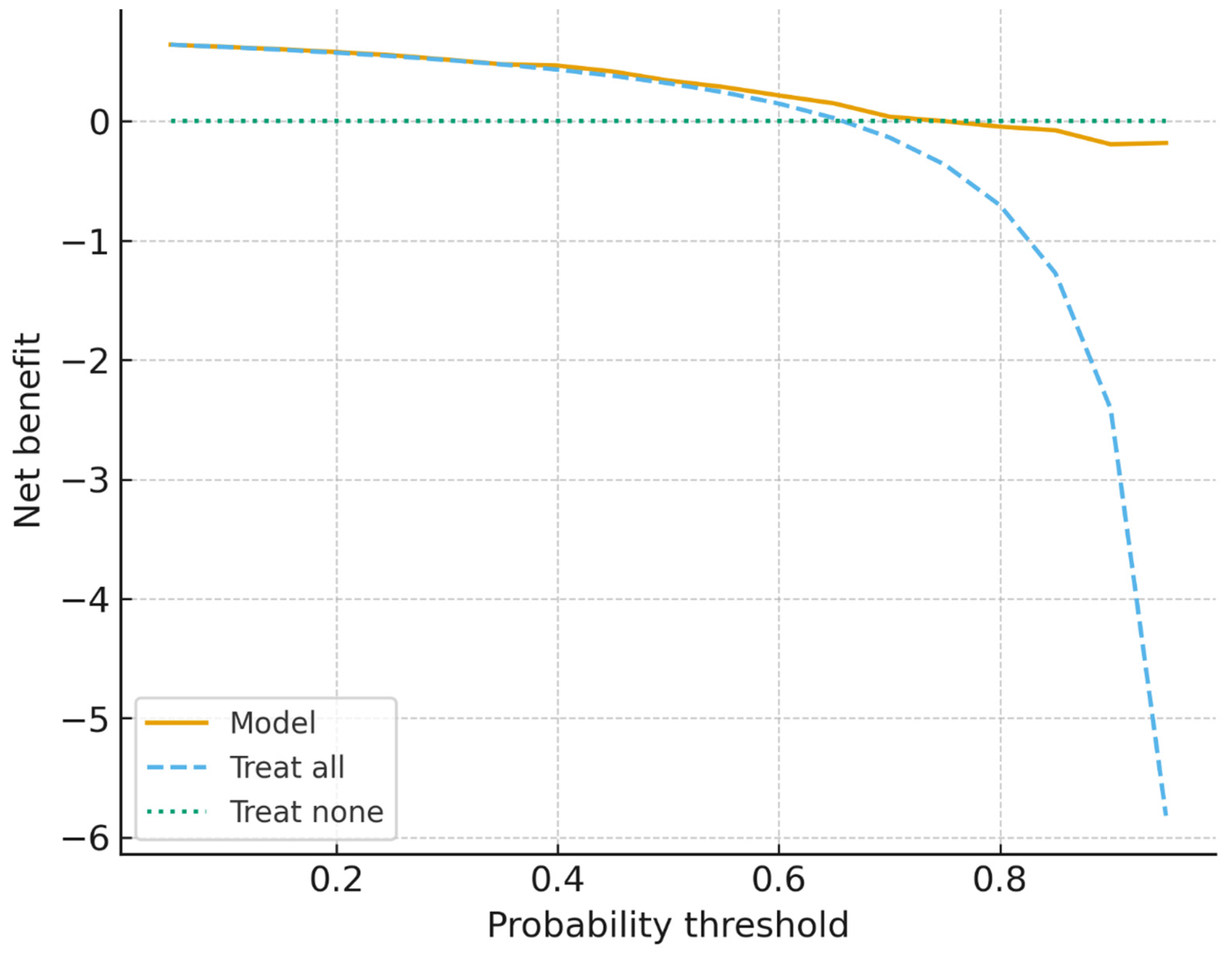
| Model | AUROC (mean±sd) | AUPRC (mean±sd) | Accuracy (mean±sd) | F1 (mean±sd) |
| LogisticRegression | 0.572 ± 0.034 | 0.716 ± 0.040 | 0.666 ± 0.007 | 0.799 ± 0.004 |
| RandomForest | 0.632 ± 0.031 | 0.753 ± 0.018 | 0.634 ± 0.027 | 0.732 ± 0.029 |
| GradientBoosting | 0.657 ± 0.052 | 0.785 ± 0.042 | 0.675 ± 0.026 | 0.776 ± 0.024 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2025 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




